Abstract
Background:
Ulnar collateral ligament reconstruction (UCLR) is common in the sport of baseball, particularly among pitchers. Postoperative return-to-sport protocols have many players beginning to throw at 4 to 5 months and returning to full competition between 12 and 16 months after surgery. Medial elbow pain during the return-to-throwing period often occurs and can be difficult to manage.
Purpose:
To evaluate the incidence of medial elbow pain and associations with outcomes and revision surgery during the return-to-throwing period after UCLR.
Study Design:
Case-control study; Level of evidence, 3.
Methods:
Between the years of 2002 and 2014, all pitchers who underwent UCLR at a single institution were identified. Charts were reviewed for incidence of medial elbow pain during return to throwing, return to sport, and subsequent operative interventions, including revision ulnar collateral ligament surgery.
Results:
Of a total of 616 pitchers who underwent UCLR during the study period, 317 were included in this study. Medial elbow pain was experienced by 45.1% (143 of 317), with a mean time of complaint of 9.75 months after surgery. The groups with and without pain did not differ statistically with regard to age (pain, 20.6 years; no pain, 20.9 years) or level of competition. Of those who experienced medial elbow pain, 10.5% did not return to sport; 5.6% underwent revision UCLR; and 19.6% underwent other operative procedures at the elbow. Among those who did not experience medial elbow pain when returning to throw, 8.7% did not return to sport, with only 1.7% undergoing revision UCLR and 6.9% undergoing other operative elbow procedures.
Conclusion:
Of the pitchers evaluated in the study, approximately half reported pain during the return-to-throwing phase after UCLR. Those who experienced medial elbow pain had a higher rate of subsequent surgical intervention.
Since the advent of ulnar collateral ligament reconstruction (UCLR) surgery in 1974 by Dr Frank Jobe, many throwing athletes have been able to successfully return to sport after injury to the ulnar collateral ligament. 1,5,8,10,15,17,18 Specifically, baseball players appear to be at highest risk for injury to the ulnar collateral ligament, with the number of those requiring UCLR continuing to rise. For this reason, Conte et al 6 evaluated the prevalence of UCLR in professional baseball and suggested that close to 25% of Major League Baseball pitchers and 15% of minor league players have undergone UCLR.
Despite the high rate of players who undergo UCLR, the literature supports a high return to sport after the procedure, with ranges between 80% and 90%. 2,8,12,14,15,18 Despite a high rate of return, Makhni et al 14 reported that only 67% of established Major League Baseball pitchers returned to the same level of competition postoperatively, and 57% of established players returned to the disabled list because of injuries to the throwing arm. It is important to realize, however, that there are limited data with regard to risk factors for those who do not return to sport or those who later require subsequent throwing arm surgery or revision UCLR.
Rehabilitation protocols that facilitate return to sport after surgery are paramount for adequate healing, optimal outcomes, and successful return to sport. After UCLR, most return-to-sport protocols include abstinence from throwing for the first 4 to 5 months, followed by gradual return to light throwing, with later progression to throwing off the mound, culminating in return to sport anywhere from 12 to 16 months after surgery. Throughout these return-to-sport protocols, players progressively test their reconstructed ligaments in a stepwise fashion, with each step adding increased stress to the medial elbow.
During these progressive rehabilitation phases, there are times when players may experience medial elbow pain, many times requiring them to slow their progression in the return-to-play protocol. We have yet to understand how postoperative medial elbow pain may affect players’ outcome or put them at risk for future injury. The purpose of this study was to evaluate medial elbow pain in the return-to-throwing period after UCLR and to assess if medial elbow pain among these players portends a worse outcome.
Methods
Institutional review board approval was obtained at our institution. All patients who underwent UCLR between 2002 and 2014 at the Kerlan-Jobe Orthopedic Clinic were identified (N = 616). Chart review was performed to establish demographic, clinical, and surgical data. All charts were evaluated for adequate postoperative follow-up through complete return to sport. Only pitchers were evaluated (n = 317) (Figure 1). Pitchers who did not have adequate postoperative follow-up for chart review were excluded. Demographic data included age at time of surgery, level of competition (junior high, high school, college, recreational, or professional) (Table 1), graft type used, and surgical technique performed. Patients’ postoperative notes were then evaluated for patient complaints of medial elbow pain, time from surgery to onset of medial elbow pain, return to sport, subsequent surgery on the throwing arm, and revision UCLR.

Tree plot of patients evaluated. UCLR, ulnar collateral ligament reconstruction.
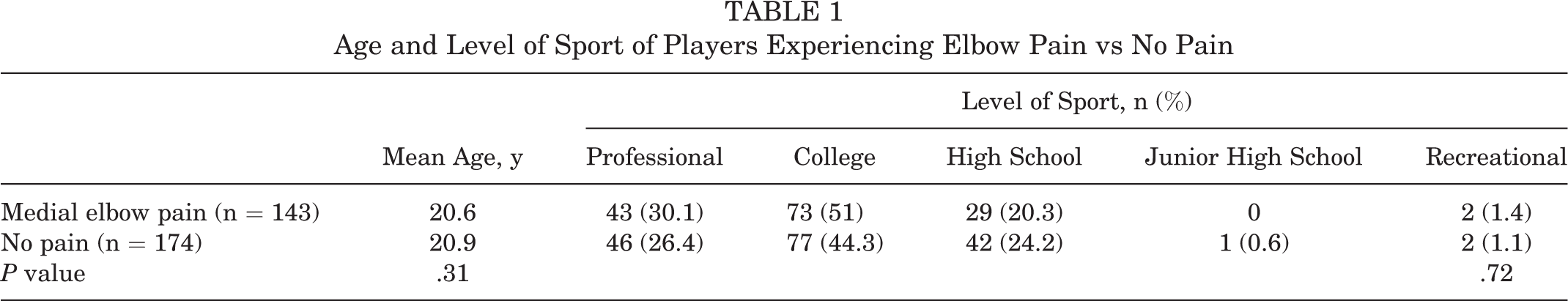
Age and Level of Sport of Players Experiencing Elbow Pain vs No Pain
To assess for differences in demographics and outcomes, players who developed medial elbow pain during the return-to-throw protocol were then compared with players who did not have medial elbow pain. Specifically, differences were evaluated in terms of return to sport, reoperation of the throwing arm, and revision UCLR. Continuous variable data were reported as weighted means, and categorical variable data as frequencies with percentages. Categorical data was compared between groups with chi-square analysis, with significance set at P < .05.
Results
Of the 317 pitchers evaluated, 143 (45.1%) experienced medial elbow pain and 174 (54.9%) did not. For those who experienced medial elbow pain, the mean time of complaint was 9.75 months (range, 4-16 months) after surgery. In comparing the 2 groups with the data available, we did not observe a statistically significant difference with regard to age (pain, 20.6 years; no pain, 20.9 years; P = .31) or level of competition (pain: n = 43 professional, 73 college, 29 high school, and 2 recreational; no pain: n = 46 professional, 77 college, 42 high school, 1 junior high school, and 2 recreational; P = .72) (Table 1). Also, with the numbers available, we identified no significant differences in the incidence of medial elbow pain based on graft type for reconstruction (Table 2).
Surgical Procedure, Graft Type, and Ulnar Nerve Transposition of Players Experiencing Elbow Pain vs No Pain a

a Results are reported as n (%).
In comparing outcomes after UCLR, medial elbow pain during the return-to-throwing period did not have a significant effect on the likelihood of return to sport (pain, 10.5%; no pain, 8.7%; P = .630). A significantly higher percentage of pitchers who experienced pain required other elbow operative interventions (pain, 19.6%; no pain, 6.9%; P < .01). In the pain group, these procedures consisted of 12 ulnar nerve decompressions/transpositions, 6 elbow arthroscopies, 1 removal of medial heterotopic ossification, 1 excision of medial antebrachial nerve neuroma, and 8 revision UCLR, compared with 3 ulnar nerve transpositions, 6 elbow arthroscopies, and 3 revision UCLR in the no-pain group. Medial elbow pain showed a trend toward a higher rate of subsequent revision UCLR (5.6% vs 1.7%), but the trend was not significant (P = .06) (Table 3).
Post-UCLR Elbow Surgery Performed Among Players Experiencing Elbow Pain vs No Pain a

a Bolded P value indicates statistically significant difference between pain and no pain groups (P < .05). UCLR, ulnar collateral ligament reconstruction.
b Decompression/transposition.
c Loose body removal and decompression.
d Miscellaneous included 1 removal of medial heterotopic ossification and 1 excision of medial antebrachial nerve neuroma.
Those who did not have medial elbow pain showed a trend toward more post-UCLR shoulder surgery as compared with those who did experience medial elbow pain (pain: 2.1%, n = 3; no pain: 6.4%, n = 11; P = .06), but the trend did not reach significance. These shoulder surgical procedures included 10 SLAP (superior labral anterior and posterior) repairs and 1 rotator cuff debridement in the no-pain group versus 3 SLAP repairs in the pain group.
Discussion
As the number of UCLR procedures continues to rise, it is important to evaluate potential risk factors that may lead to inferior outcomes. The findings of this study suggest that medial elbow pain during the return-to-throwing phase of recovery after UCLR may be associated with worse outcomes after surgery, including increased risk of subsequent elbow surgical procedures.
Rehabilitation following UCLR is a fairly long process. The senior author’s (N.S.E.) current protocol for return to sport consists of beginning short toss at 3 and 4 months post-UCLR, followed by slow progression of increasing distance to a maximum of 150 ft between 4 and 7 months. Players then transition to throwing off the mound at one-half to three-quarter speed between 8 and 10 months, followed by full-speed pitching after 10 months, with the goal to condition the arm to return to sport between 12 and 16 months. In our cohort, those who experienced medial elbow pain did so around the 10-month time frame. This is the point at which most pitchers begin throwing at normal speeds off the mound for the first time after surgery. This also represents the time when the new ligament experiences the full stresses of pitching. Medial elbow pain during this period may be an indication that a pitcher’s throwing arm is not entirely ready to withstand the full effort of pitching. Under these circumstances, plausible causes of medial elbow pain may be due to a lack of strength or endurance or to improper mechanics, or the reconstructed ligament may not have matured enough to withstand full pitching effort off the mound. For any of these reasons, the rehabilitating thrower should be observed very closely and progression even delayed to this advanced level of play and stress to the throwing arm.
Several studies have evaluated return to sport after UCLR, suggesting that 80% to 90% of those who undergo the procedure return to play. 2,8,12,14,15,18 However, there is limited literature to suggest which pitchers are at risk of being unable to return to sport. Dines and colleagues 7 reported on a cohort of 15 patients who underwent revision reconstruction, and they stated that the main reason for a compromised result was pain, with 8 of the 15 having chronic medial pain following return to sport. To our knowledge, no other studies have evaluated postoperative clinical symptoms or findings suggesting that a player is at risk for not returning to his or her previous level of sport. The current study’s results suggest that players who experience medial elbow pain while returning to the mound during their return-to-throw protocol may be at higher risk than those without pain with respect to returning to sport after UCLR.
Following successful return to sport after UCLR, a player is still at risk for reinjury to his or her throwing elbow. Osbahr et al 16 reported data at 10-year follow-up on a group of 313 baseball players who had undergone UCLR, citing a reoperation rate of 19%. Separate data from the same group—on a cohort of 942 patients with a mean follow-up of 38 months—revealed an elbow reoperation rate of 5.8%. 2 Of those who had UCLR in our cohort, 12.6% later required reoperation. However, pitchers who experienced medial elbow pain during the return-to-throw protocol showed an even higher risk for reoperation, at 19.6%.
As the incidence of primary UCLR continues to rise, so too does that of revision UCLR. Several studies have tried to elucidate risk factors for revision reconstruction. Some have suggested that relative workload changes and age at primary reconstruction, as well as percentage of fastballs pitched, may be risk factors for revision surgery. 11 Others correlated pitch velocity with risk for revision reconstruction and evaluated the stresses of different pitches. 3,4,9,13 However, limited evidence has been reported on pitchers who may be at risk during the return-to-throwing phase of rehabilitation. Our study found that medial elbow pain, most commonly 10 months after surgery, may be a risk factor leading to revision reconstruction, as 5.6% of patients with pain underwent revision UCLR versus 1.7% in the group without pain, but this trend did not reach significance.
There are several limitations to this study. This was a retrospective review of previous operative reports and clinical data. A prospectively designed study is needed to completely analyze a player’s risk of experiencing pain after UCLR. We did not have complete records or follow-up for approximately half of the patients who underwent UCLR during our study period, so we cannot draw inferences about the risk of pain after UCLR; nevertheless, this is by far the largest cohort of patients undergoing UCLR that has been used to evaluate medial elbow pain after reconstruction. The data collected were also subjective, based on patients noting medially based elbow pain during return to throwing. This can be perceived as a vague complaint at times. However, pitchers have become quite familiar with noting pain at the medial elbow, and this complaint is much less vague than other subjective measures.
Conclusion
Medial elbow pain during the return-to-throwing period after UCLR is not uncommon, with up to half of pitchers potentially experiencing pain. Our results suggest that those who experience medial elbow pain are at increased risk for further surgical intervention. Medial elbow pain during the return-to-throwing period is an important complaint and requires further study to determine its incidence and to optimize treatment for patients undergoing UCLR.
Footnotes
One or more of the authors has declared the following potential conflict of interest or source of funding: R.A.K. has received educational support from Zimmer Biomet, Arthrex, Smith & Nephew, and DJO. O.L. is a consultant for Arthrex and receives royalties from ConMed Linvatec. A.F.D. has received educational support from Arthrex, Smith & Nephew, and DJO. M.B. is a paid speaker/presenter for Arthrex, has received educational support from Mako Surgical, and is a consultant for Stryker. N.S.E. receives royalties from Arthrex and Wolters Kluwer Health–Lippincott Williams & Wilkins and is a paid speaker/presenter for Arthrex. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
Ethical approval for this study was obtained from the Cedar Sinai Hospital Institutional Review Board.
