Abstract
Globally, the number of adolescents and young adults (AYAs) living with human immunodeficiency virus (HIV) has steadily increased; however, retaining them in antiretroviral treatment (ART) remains a challenge. This scoping review identifies and synthesizes research findings on ART adherence of AYAs living with HIV in South Africa. We conducted electronic searches across various databases and identified 20 peer-reviewed articles. Five key themes that characterize the research on ART adherence among AYAs living with HIV emerged. The themes include balancing healthcare and daily activities, desire for HIV status secrecy, psychosocial implications and knowledge of ART. Availability of support was found to enhance ART adherence. ART adherence barriers included treatment and healthcare-specific challenges requiring adjustments from facilities and AYAs. Enhancing ART adherence requires individuals’ knowledge of ART and acceptance of their HIV status. The Healthcare system may need to be flexible to accommodate this group as they navigate between daily activities and ART adherence.
Plain Language Summary Title
Plain Language Summary
The review intends to map and synthesize findings from different research focusing on challenged and motivators to treatment adherence to improve the health and well-being of young people living with HIV.
Introduction
Human immunodeficiency virus (HIV) prevalence among adolescents and young adults (AYAs) remains high, owing to the availability and efficacy of highly active antiretroviral treatment (ART). Globally, ∼1.7 million adolescents aged 10–24 were living with HIV in 2021, representing a critical demographic in the fight against the epidemic. 1 A recent survey in South Africa reported 19 000 new infections among adolescent boys and 19 200 among girls aged 15–24. 2 Indicating the need for early initiation and retention in ART to achieve better health outcomes, including viral load suppression.
As the population of AYAs living with HIV and on treatment continues to grow, reaching optimal treatment adherence becomes a challenge. The 2022 survey also found low viral load suppression rates among AYAs aged 15–24, with rates of 68% for females and 70% for males. 2 While various factors contribute to nonadherence, the majority can be attributed to the significant influence of behavioral, psychosocial and physiological complexities, all of which require management at different levels of care.3–5 This is evident as several studies indicate lower ART adherence rates among individuals aged 15–24 compared to those in older age groups.2,4,5 Interruptions in ART not only hinder efforts to reduce HIV related deaths but also compromise the potential for prolonged life among adolescents.
The transition to adulthood for AYAs introduces many structural and social challenges that can significantly hinder treatment adherence. Due to these complex challenges, it is crucial to conduct a comprehensive analysis to identify the common contributing factors that negatively impact treatment adherence. One significant issue is the side effects and physical challenges associated with treatment, which can complicate identity during this critical developmental stage. 6 Additionally, the challenges and unreadiness for taking the lifelong daily pills can lead to poor self-management decisions, such as pill breaks and interrupting treatment.7,8 These choices can ultimately result in low viremia and, if not addressed, may lead to high viral load.7,8 Understanding these dynamics is essential for developing effective strategies to support AYAs in maintaining their treatment regimens.
As AYAs mature, the complexities of HIV stigma and the need to disclose to families, peers, school teachers, and sexual partners become apparent.6,9 Such disclosure can expose them to stigma, discrimination and rejection, as well as potential violence and abandonment, all of which can significantly affect treatment adherence.9–11 Additionally, socio-economic factors play a crucial role in treatment behaviors, as issues such as transport costs, availability of food and support systems can greatly influence adherence among AYAs living with HIV.7,8
Healthcare services and clinical factors can significantly influence treatment nonadherence among patients. 12 Commonly cited issues include prolonged waiting times, long queues, drug shortages, inflexible appointment schedules, and staff attitudes, all of which contribute to treatment interruption among AYAs.3,6,13 Among these factors, the attitudes of healthcare staff can significantly impact clients’ willingness to ask questions about their treatment and negotiate alternative appointment dates. 13 This scoping review aims to synthesize existing literature on treatment adherence and interruption among AYAs living with HIV in South Africa, while also identifying research and implementation gaps that could inform future interventions to curb frustration and treatment interruptions. By mapping out and analyzing the available evidence, this review aims to provide valuable insights into how healthcare systems can enhance treatment retention strategies for AYAs living with HIV, ultimately improving their health.
Methodology
We conducted a systematic search across multiple databases, including PubMed, Scopus, Web of Science, and Google Scholar, from May 2025 to July 2025. To ensure a comprehensive review, two independent reviewers conducted the literature search across the specified databases for the duration of time. We developed and applied a person, context and content (PCC) framework to guide the search and determine the eligibility criteria for the study to be mapped and included, as summarized in Table 1. 14
PCC Framework.

Abbreviations: PCC, person, context and content; HIV, human immunodeficiency virus.
Search and Identification of Literature
To streamline our search and ensure relevance, we employed a set of targeted keywords such as “adolescents living with HIV,” “young adults living with HIV,” “HIV treatment,” “Treatment adherence,” “Treatment compliance,” “HIV treatment default,” “HIV treatment support,” and “family support.” We included studies published between 2000 and June 2025 that specifically addressed treatment adherence challenges among AYAs living with HIV.
We conducted a systematic search for articles published in peer-reviewed journals that presented original research on studies conducted in South Africa. The selection criteria included articles published in English and classified as original research and specifically addressing ART adherence of adolescents and young adults aged 10–30 living with HIV.
The Preferred Reporting Items for Systematic Reviews and Meta-Analysis extension for Scoping Reviews (PRISMA-ScR) guidelines were applied to conduct and report this scoping review.15,16 Following the scoping review methodology and PRISMA-ScR guidelines, no critical appraisal of included studies was performed. Initially, we identified 213 articles, of which 147 met the preselection criteria. The excluded articles primarily consisted of reviews, unpublished preprints, and studies with a different age range and conducted outside of South Africa. The selected articles were imported into the reference manager, EndNote 20. 17
The 147 articles were imported to a shared electronic platform for reviews, Rayyan, a software application designed for systematic and scoping reviews. 18 This platform facilitated a preliminary cleaning process to identify duplicates, resulting in the identification of 24 duplicate entries. Following deduplication, 12 duplicates were removed, resulting in a total of 135 articles for screening based on the determined inclusion criteria. This screening process resulted in the selection of 45 articles for full-text screening. On completion of full text review, 22 articles were deemed eligible by both reviewers, while four were selected by only one reviewer. Discrepancies regarding these four articles were resolved through discussion among reviewers, with articles included only upon mutual agreement; a consensus was ultimately reached on two of the articles. In total, 20 articles were identified for data extraction and analysis.
Data Extraction and Analysis
Inductive and deductive data extraction approach were applied following the PCC framework and the agreed terms of reference, utilizing a standardized extraction tool for data capturing. 14 The reviewers collaboratively created a codebook, which was subsequently used to conduct qualitative content analysis to identify common codes and themes across studies. This initial analysis was followed by a team discussion to reach a consensus on the final themes, enhancing the reliability and validity of the thematic analysis. A six-step coding reliability thematic approach guided further analysis, beginning with open coding and grouping codes which were based on the review objectives. Subsequently, the codes were categorized to facilitate effective clustering of the extracted text segments, highlighting emergent themes by selecting illustrative quotes with consideration of both explicit and implicit meanings.
Results
The studies that were identified and deemed eligible during the selection process are listed in detail in Table 2. Our search included research conducted in South Africa from 2000 to June 2025. Among the 20 identified studies, 12 applied qualitative approaches, and nine applied quantitative approaches. Based on this search, eligible manuscripts were of studies conducted in six of the nine provinces. Even of the studies were conducted in the Western Cape, followed by Gauteng with five studies, KwaZulu-Natal had two studies, with Limpopo and Northwest having one study each and one study recruited participants in both KwaZulu-Natal and Gauteng provinces.
Summary of Aims, Methods, Participants, and Key Findings of Studies Included in the Review.
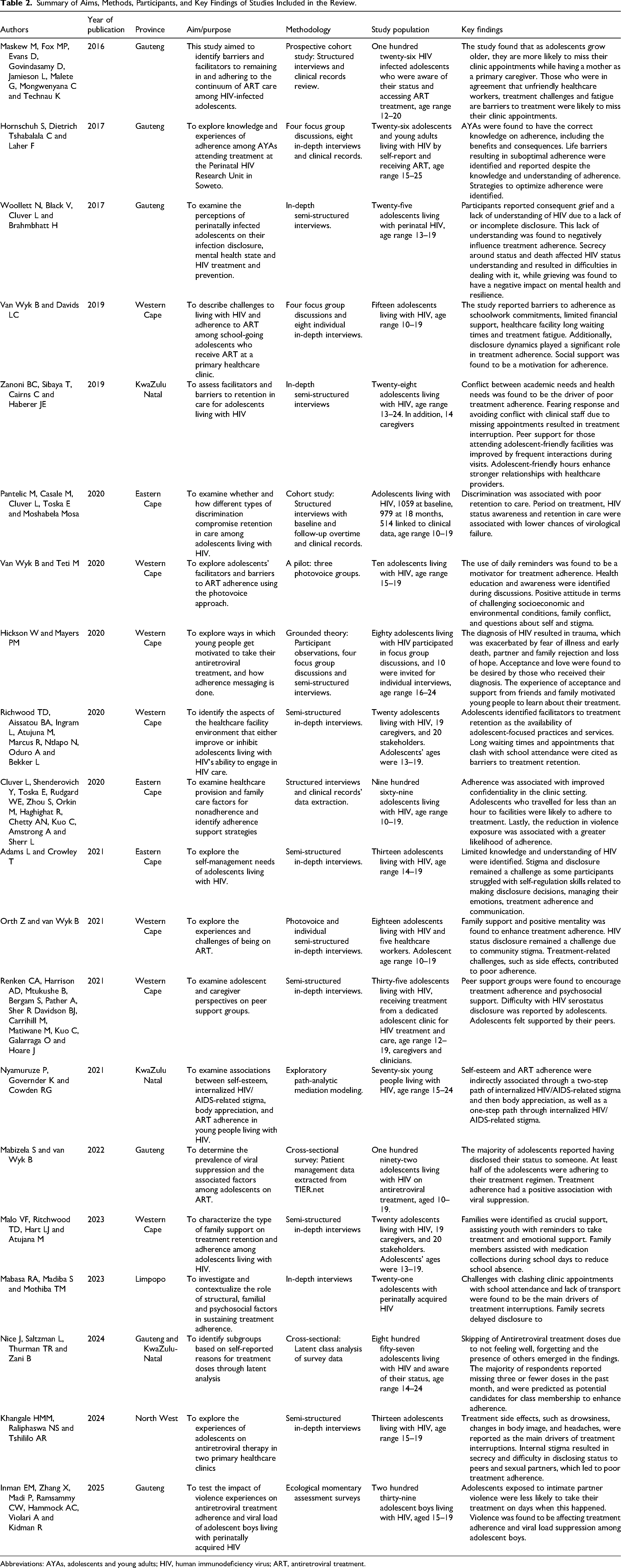
Abbreviations: AYAs, adolescents and young adults; HIV, human immunodeficiency virus; ART, antiretroviral treatment.
The analysis of this review identified five themes that characterized both barriers and facilitators of treatment adherence for AYAs living with HIV. Under barriers to treatment adherence, four themes were identified as balancing healthcare and daily activities demands, desire for HIV status secrecy, mental health impact and knowledge and understanding of ART and adherence. Availability of support was found as an aching theme for facilitators of ART adherence.
Balancing Healthcare Access and Daily Activities
Denial about the need for lifelong treatment, forgetfulness (memory lapses) and treatment fatigue were identified as significant factors contributing to missed doses and treatment interruptions.19–22 Additionally, structural and socioeconomic factors such as household dynamics, lack of food and financial resources to cover the transport costs were identified as barriers to treatment adherence, as those living in poverty often face challenges in consistently taking their treatment and keeping healthcare facility appointments.20,23–26
Long distances to healthcare facilities, along with high costs and travel times, significantly impact treatment adherence as AYAs prefer healthcare facilities that are closer and more accessible.20,25,27 AYAs constantly have to choose between attending school and keeping healthcare facility appointments, often prioritizing school attendance to avoid an impact on their academic performance.19,28,29 On days when they prioritize healthcare appointments, the lack of adolescent-focused services and prolonged waiting times results in missing the entire day of schooling.19,20,26,28–30 Furthermore, experiences of poor treatment within healthcare facilities and perceptions of healthcare providers as unfriendly and unapproachable, especially those transitioning from pediatric services, are usually more pronounced among AYAs.20,30,31
Desire for HIV Status Secrecy
Receiving assistance for treatment collections and getting additional lessons from teachers is often impractical, as they continue to struggle with stigma and the need for disclosure to peers, caregivers and even teachers, resulting in superficial relationships.24,26,28 The desire for HIV status secrecy and concerns about being seen by other students and peers while collecting treatment contribute to feelings of embarrassment, which in turn negatively impacts treatment adherence as AYAs grappled with the burden of the diagnoses and treatment without adequate support.20,22,26–28,31–34 Additionally, the presence of others at home and shared living space led to skipping of doses and eventually altered adherence based on circumstances. Some AYAs managed to make means of privately excusing themselves to go and take their treatment, while others struggled to manage their circumstances.21,22,30
Mental Health Impact
The findings from the reviewed studies indicate that emotional wellness significantly influences ART adherence. Orphaned adolescents struggle with complex grief and loss, adversely affecting their mental health and ART adherence. 35 For some adolescents, the trauma associated with learning their HIV status, upon receiving results or having their caregivers disclose to them, resulted in difficulty coping and eventually struggling with ART adherence.33,35,36 Moreover, mental health disorders and lack of peer support and counselling services were associated with a higher risk of ART nonadherence. 20 The exposure to stigma, discrimination and experiences of diagnoses and disclosure may lead to internalized stigma, resulting in feelings of shame and guilt that compromise their ability to engage and remain in care.24,29,31,37,38 Additionally, repeated exposure to violence and acute traumatic incidents may contribute to long-term mental health issues such as depression, which in turn affects their treatment adherence, while removal of exposure was associated with a greater likelihood adherence.25,38
Knowledge and Understanding of ART Adherence
Five studies examined the understanding and knowledge of treatment adherence among adolescents and young adults. The shared findings indicate a strong awareness of the importance of treatment adherence and the consequences associated with nonadherence.22,33 Among adolescents with perinatal HIV, a lack of understanding regarding the biological rationale of their infection, diagnosis and treatment was identified. 24 Positive interactions and various sources of information about ART, including insights from healthcare providers and family members, were identified as factors that enhanced understanding and motivated adherence among AYAs.22,26,34
Facilitators of Treatment Adherence: Availability of Support
Across studies, adolescents expressed a strong desire to live healthy lives and achieve personal goals, which served as a motivation for adhering to treatment regimens.22,27 Family support emerged as a crucial factor, not only providing shelter, but also emotional encouragement and reminders for medication and healthcare visits for AYAs living with HIV. Those who receive family support demonstrated higher levels of treatment adherence, as this support often included setting alarms, assisting with treatment collection and accompaniment to appointments.22,26,29,30,33,35,39
Emotional and appraisal support from families was also noted, as they encouraged AYAs to view their treatment as a pathway to a healthy future, thereby normalizing their HIV status.26,27,29 Peer support groups were identified as another essential layer of support, providing a sense of community, encouragement and shared experiences with homogenous others, which further motivated treatment adherence.28,34,36 Additionally, adolescent-friendly services were recognized as important facilitators of treatment adherence for AYAs living with HIV, with interactions with the healthcare professionals being critical, as they were reported to offer encouragement and education about HIV.28,29,34
Discussion
The review synthesized existing literature elucidating the treatment adherence of AYAs living with HIV in South Africa. Despite the presence of numerous studies conducted on AYAs living with HIV in sub-Saharan Africa, this review aimed to focus on mapping the available evidence on treatment adherence in South Africa. Through this analysis, the available literature focused on both barriers to ART and facilitators of the same. Through the coding exercise, the subthemes emerged under the two main themes. The findings from the review underscore critical gaps to be closed and existing opportunities available to enhance treatment, management and empowerment of AYAs living with HIV.
The review findings highlight the daily challenges faced by AYAs on ART. Three studies emphasized the complexities associated with the expectation of managing chronic, lifelong treatment at a young age, emphasizing the need for accurate knowledge and skills to effectively self-manage and develop treatment adherence competencies.40,41 Barriers to treatment adherence included forgetfulness, pill breaks, fatigue and side effects, which made taking ART uncomfortable and led to voluntary pill breaks and interruptions.42,43 These behavioral patterns often resulted from balancing multiple social and family activities.44–48 To mitigate forgetfulness, reminders such as alarms and personal diaries can be beneficial. 41 Healthcare providers should leverage their observation and counselling skills to identify individual behaviors and provide tailored support. Enhanced adherence counselling should be considered for all adolescents, offering opportunities to educate them on pill timing and integrating treatment into daily routines. 49
AYAs living with HIV are expected to lead productive lives, which presents various socioeconomic challenges and demands. Caregivers are often faced with the reality of living on short-term and task-based employment to make ends meet. 50 The costs associated with travelling to healthcare facilities introduce an additional burden for AYAs and their guardians, who must also manage expenses related to food, school, work, and other daily necessities. These factors highlight the complex social issues faced by AYAs, with some of them being orphaned. 51 Similar to their peers, AYAs living with HIV prioritize school attendance over healthcare visits, viewing education as a pathway to overcoming socioeconomic difficulties. The findings emphasize the need for multisectoral collaboration to develop interventions and policy guidance clearly outlining the management and support for AYAs with diverse needs.
Receiving positive HIV test results and subsequent disclosure by caregivers or self-discovery present psychological and emotional challenges for AYAs. In most cases, judging the timing of disclosure becomes challenging for healthcare providers and caregivers. 52 Following disclosure, the intense feelings of hopelessness may lead to self-questioning and self-stigmatization, compromising the willingness to continue with treatment. 51 While grappling with these different feelings, some AYAs do not receive adequate support. The desire for secrecy surrounding their status can disrupt relationships with families, peers, and teachers, limiting their ability to seek support. 53 While disclosure enhances treatment adherence,46,54 the stress of maintaining secrecy negatively impacts daily lives and treatment routines. At times, leading to AYAs changing their appointment dates to avoid encountering people they know. 49 Effective bi-referral systems for psychosocial support must be established, including the disclosure and stigma mitigation guidance.
Concerns about being seen taking their treatment can be exacerbated by living in shared spaces, such as boarding school, hosting visitors at home, which interferes with treatment times and raises fear of stigma.43,49,51 In contrast, a study in Limpopo found no direct association between stigma and nonadherence, however, it noted that some individuals resorted to alcohol as a means of coping with stigma, leading to treatment interruptions.4,7 Additionally, exposure to violence can lead to long-term mental health issues that further interfere with treatment adherence, with studies linking neglect, abuse, and bullying to nonadherence.42,47,55 This highlights the need for contextualized and individualized interventions when addressing ART adherence, with high consideration of backgrounds and social circumstances.
Across studies, the desire to live a healthy, long life remained the motivator for treatment adherence. The hope for their future life and desire to even have children motivated adherence.54,56 Support from families, peers, and teachers is essential for AYAs to manage treatment demands and daily activities effectively. Good relationships and communication with caregivers and healthcare providers were found to reduce depressive symptoms and motivated adherence.54,57 Pairing support with appropriate health education for AYAs and caregivers could be a valuable tool to enhance ART adherence. This education, along with tools like text appointment reminders and operating on weekends, can further support adherence.45,58,59 While adolescent-friendly facilities offer safe spaces for AYAs, further evaluation is needed to ensure they meet the specific needs of those living with HIV.
Review Limitations
The scoping review has several limitations that were identified during the process. Firstly, the review was limited to studies conducted within a single country context, which limits the ability to draw comparisons with findings from other countries. Despite the efforts to conduct a comprehensive search, relevant studies published in nonindexed journals, unpublished works and articles in languages outside the inclusion criteria may have been missed, potentially introducing selection bias. Additionally, the data charting was primarily narrative, which may have introduced an element of subjectivity. Although the reviewers aimed to ensure the quality of the scoping review analysis by applying a six-step coding reliability thematic approach during analysis and adhering to PRISMA-ScR guideline for reporting, is important to note that, consistent with the scoping review methodology, a critical appraisal of the included studies was not conducted, Consequently, the quality and risk of bias of the included studies could not be assessed.
Conclusion
This review highlights several barriers to ART adherence among AYAs living with HIV. Key challenges include long distances to healthcare facilities, transport costs and long waiting times for scheduled appointments. Additionally, financial difficulties were identified as an additional concern, particularly for AYAs who are still in school, orphaned, or living with unemployed caregivers. The review also highlights the impact of HIV stigma on treatment adherence, emphasizing the need for ongoing support and counselling to help AYAs in navigating the complexities of living with HIV. The findings demonstrate the advantages of multifaceted support systems that enable young individuals to manage both daily life and treatment demands. Such support systems may include family assistance, school and teacher support and flexible healthcare services with supportive providers. Therefore, the strategies to enhance ART adherence should be flexible and more contextualized to meet the diverse needs of AYAs living with HIV for improved treatment outcomes.
Footnotes
Author Note
The authors, Dr Bandile Ernest Ndlazi and Prof David Ditaba Mphuthi, declare that the views expressed in this article are the researchers’ and not an official position of any institution mentioned in this document.
Acknowledgements
The author sincerely appreciates all those who contributed to the completion of this scoping review. I am especially thankful to Prof David Mphuthi for his invaluable guidance and support throughout my academic growth. A heartfelt appreciation goes to the late academic mother and mentor, Prof Thembekile Masango. Lastly, the University of South Africa's Department of Health Studies for making this work possible.
Ethical Considerations
This scoping review examined existing literature on antiretroviral treatment adherence among adolescents and young adults in South Africa. The review was conducted in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analysis extension for Scoping Reviews (PRISMA-ScR) guidelines and ethical standards for studies using publicly available data. Considering that the review did not involve human participants, personal data or interventions, Institutional Review Board's ethical approval was not required. All the sources and materials included in this review were publicly available. The authors ensured the ethical integrity of the review by adhering to principles of transparency, integrity and responsible scholarship.
Author Contributions
Authors BN and DM conceived the initial idea for the review. BN created the review profile on Rayyan for article selection, while both authors collaborated on the literature search. All authors participated in discussions to agree on the selected articles and conducted the analysis. BN drafted the initial manuscript, and sections were subsequently distributed among authors for contributions, culminating in the final version of the manuscript.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The University of South Africa M&D bursaries supported this work.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The review was conducted using the published literature.
