Abstract
Superficial perivascular dermatitis with tissue eosinophils is a histopathologic finding associated with various dermatologic conditions, including urticarial dermatitis, drug reactions, autoimmune processes, and infectious etiologies. Diagnosis often requires correlation of clinical findings, laboratory evaluations, and histopathologic examination. We present a case of a 24-year-old female with urticarial dermatitis-like symptoms, whose final diagnosis of superficial perivascular dermatitis with tissue eosinophils was established 2 weeks postdischarge. The case highlights the importance of maintaining a broad differential diagnosis, employing a structured diagnostic approach, and implementing strategic follow-up when histopathologic findings are delayed. This delay highlights the importance of a thorough differential diagnosis, a structured diagnostic approach, and strategic follow-up to guide management and allow for appropriate treatment options. Potential etiologies are explored, including medication-induced reactions, and a diagnostic approach is proposed for future cases.
Keywords
Introduction
Superficial perivascular dermatitis is a histopathologic pattern characterized by perivascular inflammation in the superficial dermis. Granulocytes, such as eosinophils and neutrophils, cluster around blood vessels and can invade the vessel walls, leading to localized tissue damage. 1 The finding of tissue eosinophils is a nonspecific histologic finding seen in a broad range of hypersensitivity reactions including urticarial dermatitis, insect bites, drug reactions, autoimmune diseases, and infections.2,3
Cutaneous disorders that lack pathognomonic histologic findings and instead present with nonspecific microscopic findings require methodical clinical correlation to establish an accurate diagnosis. This case describes a young woman who presented with a rash and edema suggestive of urticaria but whose definitive diagnosis, superficial perivascular dermatitis with eosinophils, was delayed due to a 2-week turnaround on biopsy results. The case underscores the importance of maintaining a broad differential and initiating empiric treatment when pathology is not immediately available.
Case Presentation
A 24-year-old female presented to the emergency department with a 3-day history of diffuse pruritic rash and swelling of the lips and hands. She denied fever, respiratory symptoms, gastrointestinal complaints, or systemic manifestations. Her past medical history included rheumatoid arthritis, treated with methotrexate, and epilepsy managed with ethosuximide. She denied any recent medication changes, new foods, or environmental exposures. Notably, she had experienced a prior dermatologic issue diagnosed as contact dermatitis, which had responded well to clobetasol.
On examination, she was afebrile and hemodynamically stable. As shown in Figures 1 to 5, cutaneous findings included erythematous, edematous, and pruritic plaques on the arms, trunk, and legs. The lesions were annular and circular, blanching with pressure, and lacked central clearing. Subcutaneous nodules were also present. There was no mucosal involvement, no urticating papules (as seen in cutaneous mastocytosis), and no systemic signs of hypotension or flushing.

Photograph of abdomen with urticarial rashes.

Photograph of the anterior view of lower extremities showing maculopapular rashes.
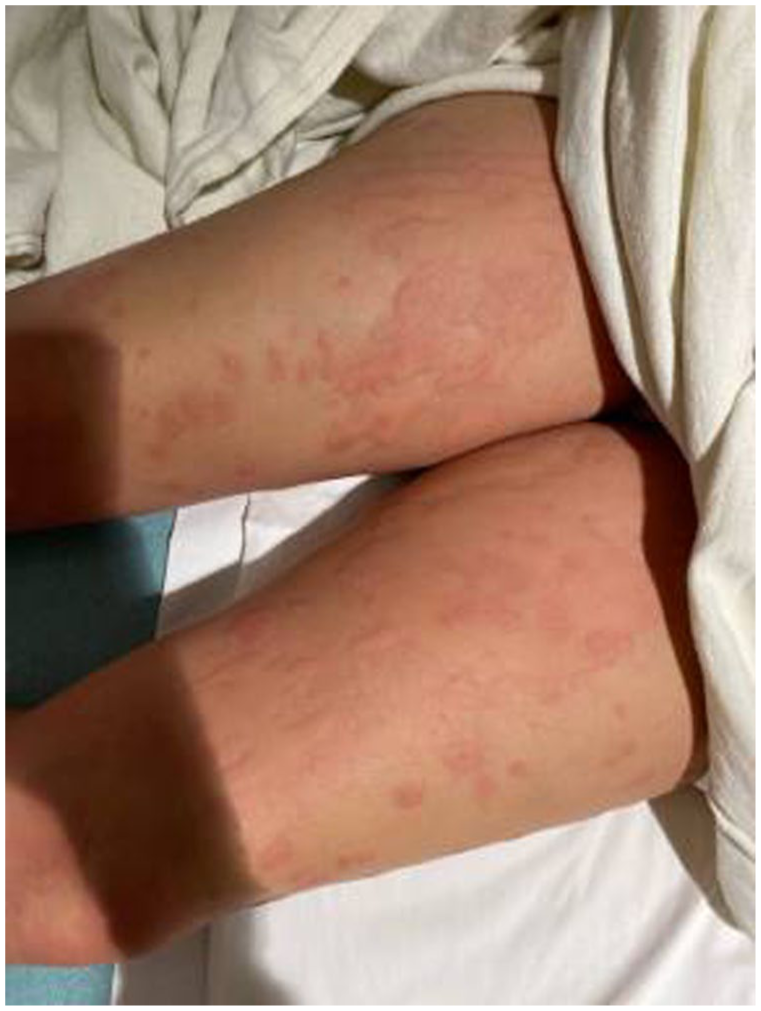
Photograph of the posterior view of lower extremities showing maculopapular rashes.

Photograph of the posterior view of upper extremities showing maculopapular rashes.
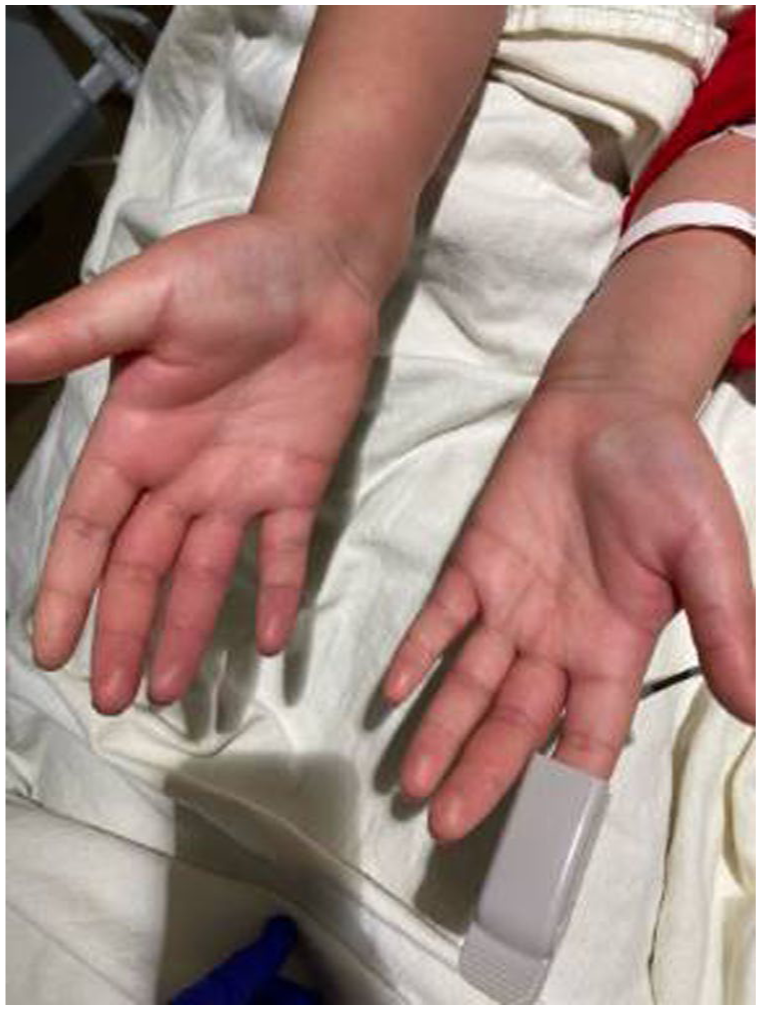
Photograph of the anterior view of upper extremities showing maculopapular rashes.
Initial labs revealed an elevated C-reactive protein, an elevated tryptase level of 11.7 µg/L, and a positive Rapid Strep A screen. Autoimmune work up, including anti-nuclear antibody, rheumatoid factor, anti-dsDNA, anti neutrophil cytoplasmic antibodies, and complement levels was unremarkable.
Given her known autoimmune history and current findings, the differential diagnosis included urticarial vasculitis, rheumatoid arthritis-associated vasculitis, a delayed drug reaction, and a postinfectious hypersensitivity response. A punch biopsy of a lesion on the right thigh was performed prior to discharge to further evaluate the etiology. She was empirically treated with a single dose of IV methylprednisolone 125 mg, followed by prednisone 10 mg orally daily for 10 days. The patient experienced rapid symptom improvement, with notable reduction in rash and edema within 24 hours. Due to the patient flying back home, she was instructed to follow-up with their primary care physician.
The patient was discharged from the hospital but contacted the treatment team 2 days later reporting that her rash had persisted despite taking the prednisone that she was prescribed at discharge. Hydroxyzine 25 mg tablets were then prescribed 3 times a day for 1 month to alleviate her symptoms. Two weeks later, the skin biopsy results became available and revealed superficial perivascular dermatitis with tissue eosinophils, consistent with an allergic or hypersensitivity process. 4
Discussion
The histopathologic finding of superficial perivascular dermatitis with eosinophils warrants a comprehensive differential diagnosis, particularly when biopsy results are delayed. The potential causes include
• Urticarial Dermatitis: The patient’s clinical presentation, pruritic, edematous plaques without mucosal involvement or systemic instability, was highly suggestive of urticarial dermatitis. Her prompt response to corticosteroids further supports an inflammatory etiology consistent with this diagnosis. 2 The annular appearance and widespread distribution are also typical of urticarial eruptions.
• Drug-Induced Hypersensitivity: Drug reactions are a common cause of eosinophilic skin infiltrates. While the patient had no new medications, methotrexate can, on rare occasions, cause delayed hypersensitivity even after long-term use. 5 Sertraline, also on her medication list, has been associated with skin reactions. However, in the absence of a new or recently adjusted medication, this remained a less likely but plausible consideration. Evaluation typically includes a detailed medication history, possible drug cessation, and consideration of patch testing if clinically indicated.
• Post-Infectious Hypersensitivity: The patient had a positive Rapid Strep A screen at presentation to the hospital. Group A Streptococcus has been linked to delayed immune-mediated skin responses (eg, psoriasis). 6 Identifying active infection or colonization of the upper respiratory tract can help determine whether Streptococcal focused treatment can play a role in treating a patient’s rash. Because the patient did not present with other systemic signs of infection (ie, she was afebrile, lacked throat soreness, was not tachycardic and normotensive) a confirmatory throat culture was not performed. In a case like hers where Streptococcal infection is a possible or probable cause for a persistent rash, it is very helpful to perform a throat culture to guide management. 3 While antistreptolysin O antibody screening tests are sometimes ordered for this purpose, they are less preferred as an ASO test detects antibodies against Streptococcus and can remain positive for months after an infection as passed.
• Insect Bites and Parasitic Infections: These conditions can cause localized or diffuse eosinophilic inflammation. However, the patient had no known insect exposures, no travel history, and no clinical findings suggestive of parasitic infection. Serologic testing for parasitic antigens or eosinophil-stimulating infections was not indicated.
• Autoimmune Conditions: Although autoimmune disease was strongly considered due to her history of rheumatoid arthritis, screening serologic testing did not support an active autoimmune flare or an overlapping autoimmune condition. Specifically, urticarial vasculitis and connective tissue diseases were considered but deemed less likely in light of negative ANA, ANCA, RF, anti-dsDNA, and normal complement levels. 7
• Mast Cell Activation Syndromes (MCAS): The elevated tryptase level of 11.7 µg/L (normal <11 µg/L) prompted consideration of MCAS or systemic mastocytosis.8,9 Elevated tryptase level numbers can be seen in patients experiencing activation of mast cells, expected in patients with urticarial eruptions. However, the patient lacked other cardinal features—such as flushing, hypotension, or recurrent anaphylactoid symptoms. Furthermore, the acute and self-limited course of symptoms following corticosteroid treatment suggested a transient process rather than a chronic mast cell disorder. Serial tryptase levels or bone marrow biopsy could be considered in the future if symptoms recur or persist. In the situation in which the patient did present with flushing, hypotension, or recurrent anaphylactoid symptoms, her elevated tryptase levels would need to be followed with repeated testing. If a patient were found to have transiently elevated tryptase that returned to normal after she was treated and her rash resolved, then further work up may not be needed. If her tryptase remained elevated after her treatment, then she may require a work-up for systemic mastocytosis.
• Idiopathic or Allergic Causes: In the absence of a clear trigger, idiopathic hypersensitivity reactions remain a diagnosis of exclusion. Environmental allergens or undiagnosed food sensitivities could contribute to such presentations. Further allergist evaluation and additional testing could be pursued if symptoms recur. Empiric corticosteroid therapy is appropriate while awaiting workup. 10
Conclusion
This case illustrates the diagnostic challenge posed by superficial perivascular dermatitis with eosinophils in the absence of immediate biopsy results. When presented with a patient with a history of autoimmune disease and nonspecific cutaneous findings, clinicians must consider a wide differential that includes urticaria, drug reactions, infections, autoimmune processes, and mast cell disorders.
In this case, the absence of recent new medications, systemic involvement, infectious symptoms or signs, and the patient’s rapid response to corticosteroid treatment supports an autoimmune or hypersensitivity etiology for her dermatitic reaction. The prolonged time to receive the results of the histologic examination of the skin biopsy delayed reaching a final diagnosis for the patient. While in our case the clinician’s clinical judgment, history taking, and a structured diagnostic result led to a rapid resolution of the patient’s symptoms, having immediate access to dermatopathologic consultation would have reduced the risk of an extensive and prolonged work up for the patient.
Footnotes
Ethical Considerations
Our institution does not require ethical approval for reporting individual cases or case studies.
Consent for Publication
Verbal informed consent was obtained from the patient for their anonymized information to be published in this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
