Abstract
Locus minoris resistentiae refers to a region of decreased resistance within the body. This occurs from changes to the microenvironment secondary to previous trauma and results in increased vulnerability. As a result, infection, inflammatory processes, and malignancy may localize to this area. In this article, we describe 2 unique cases of malignancy, primary prostate carcinoma and serous carcinoma of the ovary, both of which disseminated to sites of prior trauma. We review the available literature, discuss proposed pathophysiology, and highlight the need for further investigations along with increased clinician awareness.
Keywords
Introduction
Locus minoris resistentiae refers to a region of decreased resistance within the body. This occurs from changes to the microenvironment secondary to previous trauma and results in increased vulnerability. As a result, infection, inflammatory processes, and malignancy may localize to this area. Locus minoris is well described in the medical literature by various case reports from several different subspecialties. One widely recognized example is that of a damaged heart valve being more susceptible to infection. 1 Another example is the skin, which can act as a site of locus minoris, most notably known as the Koebner phenomenon. 2 In oncology, well-established examples include the development of hepatocellular carcinoma in a cirrhotic liver, lung cancer within a tuberculosis scar, or osteosarcoma at the site of chronic osteomyelitis. 1
Despite the ubiquitous nature of this phenomenon, the medical literature of cases exploring malignant spread to susceptible sites of prior injury is uncommon. This lack of literature regarding cancer seeding to areas of locus minoris is unlikely an indicator of the rarity of the pathogenic process, but rather a result of underrecognition. In this article, we describe cases of malignant metastasis of 2 distinct forms of cancer, primary ovarian cancer and prostate cancer, which on review of literature, have not been previously associated with locus minoris. Specifically, we describe these 2 unique cases of malignancy, both of which disseminated to sites of prior trauma. We also explore some of the proposed mechanisms of action of the coupling of metastasis and localization to susceptible areas.
Methods
Kern Medical Institutional Review Board approval. Review of the patients’ records.
Case Reports
Case 1
A 64-year-old G4P3 (gravida 4 para 3) female with past medical history of gastric bypass and bilateral brachioplasty presented with abdominal and pelvic pain, ascites, and a left ovarian mass. She was diagnosed with ovarian carcinoma. She subsequently underwent posterior exenteration, coloproctostomy, right pelvic lymphadenopathy, left aortic node biopsy, and omentectomy for stage IVA serous carcinoma of the ovary (pT3c, pN1) in 2017. She then received 7 cycles of adjuvant chemotherapy with carboplatin and paclitaxel followed by maintenance bevacizumab for 1 year. She was then found to have an increasing CA-125 tumor marker, and the chemotherapy regimen was changed to liposomal doxorubicin and bevacizumab for 7 cycles, after which the tumor marker normalized. The patient then developed an erythematous rash and nodules in the left axillary region, overlying the site of prior brachioplasty (see Figure 1a and b).

(a, b) Case 1 lesions of the left axillary region overlying the site of a prior brachioplasty.
She was initially treated for presumed herpes zoster with acyclovir for 10 days without improvement. Subsequent biopsy revealed malignant cells consistent with ovarian primary and repeat CA-125 antigen was also elevated at this time.
Case 2
A 59-year-old man with a history of an L4-5 vertebral fracture from a fall 10 years prior presented to medical attention for mild urinary symptoms and was found to have an elevated prostate-specific antigen. Prostate biopsy was obtained, which revealed malignant cells consistent with primary prostate carcinoma with a Gleason score of 8. He was clinical stage 2 and was treated with primary radiation to the prostate gland and surrounding tissue. He remained stable for 4 years, at which time he was noted to have an increasing prostate-specific antigen. Positron emission tomography scan demonstrated fluorodeoxyglucose-avid uptake to the L4-5 vertebral region corresponding to the same site of his prior vertebral fracture (see Figure 2).

Case 2: positron-emission tomography scan demonstrating fluorodeoxyglucose-avid uptake to the L4-5 vertebral region at the site of prior vertebral fracture.
A magnetic resonance imaging also showed vertebral metastasis and a mass at L4-5 vertebral body with mild spinal cord impingement (see Figure 3). He was subsequently treated with hormonal therapy and radiation therapy.
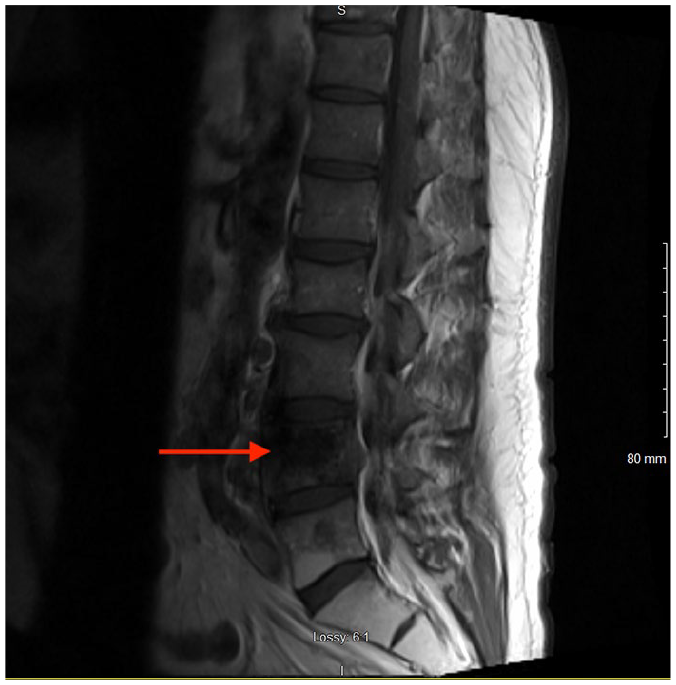
Case 2: magnetic resonance imaging demonstrating vertebral metastasis and mass at L4-5 vertebral body with mild spinal cord impingement.
Discussion
Locus minoris resistentiae is an area of increased vulnerability resulting in the localized spread of infection, inflammatory conditions, and malignancy. The phenomenon has been recognized for centuries in medicine, and the concept of locus minoris resistentiae presents across multiple specialties. 3 Early documented experiments involved the controlled introduction of foreign substances and observation of their spread to locus minoris.4-6 This phenomenon was investigated by Chesney et al at Johns Hopkins in 1928. 4 They found that when rabbits with wounds on their backs are inoculated with either intratesticular or intravenous Treponema pallidum, syphilitic lesions consistently developed in the wounds. 4 In another study, Sager et al demonstrated that subcutaneous injection of silver nitrate in rabbits caused sterile abscesses. 5 After intravenous injection of streptococci, these organisms were recovered from the abscesses in some rabbits. 5 These results prompted further investigation into the pathophysiology driving localization to areas of inflammation.
Menkin et al built on the widely accepted theory of increased capillary permeability, allowing substances to diffuse to an area of locus minoris through a series of experiments. 6 Reproducing the mechanism of a traditional infection, the experimenters introduced foreign substances into the micro-ecosystem of a locus minoris. 6 They suggested that in addition to increased capillary permeability, these substances cannot escape from the site of inflammation because of a fine network of fibrin and thrombosed lymphatics. 6 Other such experiments and case reports suggest that the specifics of pathogenic signaling differ in each respective microenvironment of inflammatory conditions, infection, and malignancy.3,7-11
The locus minoris phenomenon is well described in bacterial and mycobacterium infection yet less frequently appreciated in fungal infections, including coccidioidomycosis. 3 There is an available case series that describes 2 patients with active pulmonary coccidioidomycosis with osseous dissemination and localization to the site of prior injury, supporting the theory of hematogenous dissemination. 3 In addition to changes that facilitate pathogens honing to an area of prior trauma, the environment is primed further. Prostaglandins from damaged leukocytes at the site of injury have been shown to stimulate the formation of the spherule-endospore phase of Coccidioides immitis.3,8 Furthermore, the neutrophil response is unable to ingest mature spherules.3,12 This sophisticated interface between the organism, the modified environment, and the immune response all guide the deposition and growth of the infection.
In inflammatory conditions such as psoriasis, systemic sarcoidosis, and systemic lupus erythematosus, the locus minoris phenomenon has been observed both as the initial manifestation of the disease or accentuation of an existing disorder. 9 Sarcoidosis is described as having a known tropism for scars and areas of previous trauma. 9 There continues to be unusual presentations added to the literature, including a case of the initial manifestation of systemic sarcoidosis presenting in only the black dye of a tattoo. 9 Highlighting the possibility of the black ink’s specific microenvironment within the entire tattoo functions as a more inviting anchor for the condition.
Regarding malignancy, reports of “inflammatory onchotaxis,” the phenomenon in which mechanically injured tissues are predisposed to metastases, 11 may be underestimated. The pathogenesis of metastasis is a sophisticated process and not random cellular anarchy but, instead, quite selective. 10 The critical players that modulate metastasis are the properties of metastatic cells and the host environment, which influences this process. 13 Apart from the environment’s influence, it has been suggested that cancer cells acquire specialized functions to invade target organs in metastasis. 14 Experiments show the expression of genes involved in an intricate latent metastatic cascade in breast cancer cells, enhancing their adhesion to brain endothelial cells and their passage through the blood-brain barrier. 14 It appears that target organs become metastatic sites through an interplay between tumor gene expression and alterations in the environment.
Tumors have been designated as wounds that will not heal. 15 Parallels have been drawn between signaling molecules that regulate tumor microenvironment with those of the microenvironment of wound repair. In vitro and animal experiments revealed interleukin 6, interleukin 8, chemokine (C-X-C motif) ligand 1, galectin-1, and selected proteins of the extracellular matrix (eg, fibronectin) do have similar regulation during wound healing and tumor growth. 10 The continued identification of the intersection of signaling molecules responsible for tumor and wound microenvironments can have significant implications in targeted and immunotherapy modalities.
Through the lens of locus minoris, Walter et al propose the pathogenesis may predispose to metastasis through 2 distinct, yet not necessarily exclusive mechanisms. 11 The first, physical trauma, induces tissue damage and local inflammation, creating a favorable environment that is permissive for seeding of metastatic cells from distant sites. 11 The second, micrometastatic foci, are already present at the time of trauma, initiates changes in the microenvironment that stimulate the proliferation of the metastatic cells. 11 During trauma or scar formation, a balance between proangiogenic (eg, interluekin-8 and transforming growth factor-β), antiangiogenic (L-10) cytokines, and chemokines is likely more important than the absolute levels in tumor angiogenesis. 11 Further understanding of the network’s intricacies may lead to potential ways of undermining the priming process and preventing seeding of disease.
Identification of the details involved in an inflammatory onchotaxis microenvironment is further complicated by the unusual alterations in the behavior of respective cancers, unpredictable timing, location, and span of histological phenotypes.3,9-11,16,17 Reports describe not only distant metastasis but also unexpected local invasion. 11 Regarding squamous cell carcinoma specifically, there have been case reports that describe metastasis to sites of trauma without locally invasive disease, which is unusual behavior for squamous cell carcinoma of the lung. 11 Additionally, one of the patients had localized liver metastases from the lung cancer, which more commonly is randomly dispersed. 11
Furthermore, reports illustrate the unpredictable timing of metastasis to areas of prior trauma, ranging from weeks to several years.11,17 A case report discusses a case of rapid metastasis of squamous cell carcinoma of the lung to the right knee that had been injured only 6 weeks earlier. 11 Two additional cases are available of squamous cell carcinoma at sites of old maxillary fractures that had occurred years before. 17 Most cases of observed locus minoris describe metastasis to a site of injury from previously recognized disease. Nevertheless, others describe prior sites of injury as unusual initial presentations of cancer. One such case report describes hepatocellular carcinoma at the site of skull fracture as the first presenting symptom, even though hepatocellular carcinoma rarely metastasizes to the skull. 18 The tumor cells in this case were found to be positive for vascular endothelial growth factor and basic fibrous growth factor on histopathology. 18 This suggests that processes involved in bone healing modified the microenvironment and likely caused skull metastasis from the primary tumor. 18 Case reports have identified sources of locus minoris as cutaneous and internal scar tissue, 19 fractures of multiple subtypes of bone,17,18 and blunt trauma of internal organs, 11 among others. The intersection of each unique atmosphere’s wound healing mechanism is likely where the fundamental mechanism of locus minoris lies.
The available literature also illustrates the need for further attention to the implications of inflammatory onchotaxis on treatment. Huang et al describe 42 cases of isolated squamous cell metastasis at percutaneous endoscopic gastrostomy (PEG) insertion sites at the skin. 16 They assert modifications in the PEG technique or timing of adjunctive therapies are possible areas for further research. 16 These data are of substantial importance given that PEG tubes are often a significant part of treatment efforts for head and neck squamous cell carcinoma. 16 Huang et al suggest that PEG site metastatic disease portends a poor prognosis and that early detection and aggressive therapy is critical. 16 Despite the integral role surgery plays in cancer treatment strategies, clinicians do not often recognize this surgery can trigger the growth of dormant micrometastasis. 20 Therefore, it has been suggested that perioperative chemotherapy may also limit the emergence of any dormant malignant cells associated with surgical trauma-associated inflammation. 11
There is limited literature regarding malignancy in association with locus minoris but a high prevalence of metastasis in general; therefore, this phenomenon may be underdetected and, in turn, underreported. Surprisingly, the available literature for prostate cancer metastasis to bone at the site of previous fractures is lacking given prostate cancer metastasis has a near-total tropism for bone. 21 Therefore, inflammatory onchotaxis metastasis to sites of prior fractures may often go unrecognized as typical metastasis. Bone metastasis leads to bone pain, skeletal fracture, and increased mortality. 21 If primary care clinicians, oncologists, and surgeons become aware of metastatic predilection to areas of trauma, thresholds for diagnostic and therapeutic interventions may change, and in turn, the incidence of misdiagnoses decreased.
Conclusion
Locus minoris resistentiae is associated with a variety of disease states and is well described in the literature. Theories and experiments have begun to delineate a network of signaling far more complicated than simply decreased resistance. Despite all of the advances in understanding of the mechanisms of action, there remains outstanding research questions. The possibilities of unexpected presentations span phenotype, location, and variations in presentation timing; they continue to broaden as the literature documents.
Clinicians should be aware of the possibility of malignant spread to surgical sites or sites of prior trauma, especially in the setting of elevated tumor markers or new symptomology onset. Surgery to resect cancer is frequently a mainstay of treatment, and perioperative chemotherapy might be beneficial in certain instances. Early recognition of the pathophysiology of a locus minoris environment favoring metastasis has important implications in patient care and patient outcomes by allowing for prompt initiation of additional interventions to prevent disease progression and evolution.
Footnotes
Authors’ Note
This work was presented as an oral presentation at the Western Medical Research Conference, Carmel, CA, on January 23, 2020.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics Approval
Ethical approval to report this case was obtained from the Kern Medical Institutional Review Board (Approval ID: 19085).
Informed Consent
Informed consents for patient information to be published in this article were waived as patients were lost to follow-up.
