Abstract
Acute hemorrhagic edema of infancy (AHEI) is a cutaneous leukocytoclastic vasculitis presenting with purpura, ecchymosis, fever, and edema. Pediatricians must effectively differentiate AHEI from other diseases that have similar presentations but are more severe in order to treat appropriately without overutilizing expensive, unnecessary diagnostic tests. In this article, we describe a case of a 6-month-old previously well male who presented to our institution with a worsening rash and fever. In this case, the patient’s age and benign clinical manifestations without systemic involvement favored the diagnosis of AHEI over more serious conditions. This case is a valuable example of the clinical findings of AHEI and the effectiveness of conservative therapy once a diagnosis is made for pediatricians, especially emergency and urgent care physicians.
Keywords
Introduction
Acute hemorrhagic edema of infancy (AHEI) is a benign leukocytoclastic vasculitis that has previously had many names including Finkelstein’s disease, Seidlmayer’s disease, and postinfectious cockade purpura.1,2 It is a benign process that presents with localized purpura, which is frequently associated with fever and edema. It usually resolves within a few weeks without intervention. 3 We are presenting a 6-month-old male with AHEI who presented with rash and edema in the lower extremities.
Case Report
A 6-month-old previously well male presented to our institution with a worsening rash. His illness began 3 days prior with cough, rhinorrhea, decreased appetite, and he was moderately febrile with a maximum rectal temperature of 38.3 °C. The fever disappeared within 24 hours. Parents gave a dose of natural cough medication during the illness, otherwise he had not taken any other medications. There was no vomiting, diarrhea, change in behavior, recent vaccinations, and no known sick contacts. Past medical history and family history were unremarkable. He received his 2- and 4-month vaccinations and was scheduled to receive his 6-month vaccines the following week.
At initial presentation in the emergency room, he was afebrile (98.6 °F [37 °C]) with a heart rate of 140 beats/min, respiratory rate of 30 breaths/min, blood pressure of 84/62 mm Hg, and an oxygen saturation of 100% in room air.
On examination, he was active, well developed, and nontoxic appearing. His neck was supple, he had mild rhinorrhea and erythema of the oropharynx without exudates or vesicles. His skin had various sized erythematous macules and plaques extending from the soles of his feet to his thighs. The diameter of the lesions varied from a few millimeters to several centimeters (Figure 1).

Erythematous macular rash on patient’s feet with edema.
There was mild scrotal edema. Nontender and nonpitting edema of his bilateral ankles and feet were present but he had normal range of motion of all joints. No rash was noted on the face, chest, back or arms. His abdominal examination was soft, nontender without palpable organomegaly. The rest of the physical examination was unremarkable.
Laboratory studies revealed a mildly elevated erythrocyte sedimentation rate (24 mm/h, reference = 0-15 mm/h) with a mild thrombocytosis (415 × 103/µL, reference = 150-400 × 103/µL) and absence of leukocytosis. A complete metabolic panel, coagulation panel (includes prothrombin time/partial thromboplastin time and international normalized ratio), C-reactive protein, and urinalysis were all unremarkable.
Over his 3-hour stay in the emergency department, he remained afebrile and well appearing, though some areas on his feet and legs became purpuric. He also developed purpura on the dorsal sides of his feet and his lower legs (Figures 2 and 3).

Nonblanching purpura on the dorsal sides of patient’s feet with pedal edema.
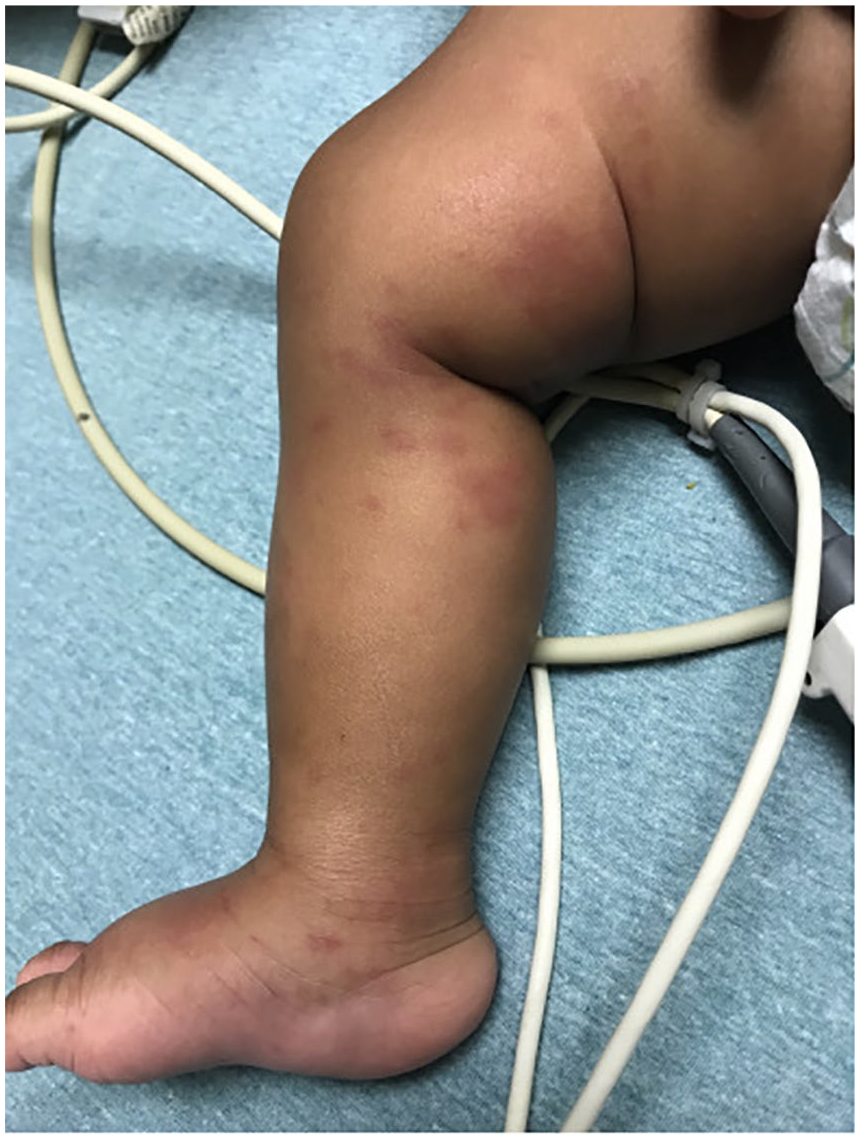
Nonblanching purpura extending from feet to upper thigh.
Initial Diagnosis and Outcome
Our patient’s presentation with a nontoxic appearance, purpuric rash with impressive edema of the feet, legs, and scrotum in the setting of a mild upper respiratory tract infection is consistent with a diagnosis of AHEI due to the patient’s age and relatively normal laboratory results without systemic findings. A decision was made not to admit the child and to avoid cutaneous biopsy since a well-defined diagnosis was made clinically.
He was discharged home with his parents to follow-up with his pediatrician the next day. We followed-up with parents via phone the following week and his mother informed us that his vitals at the pediatrician’s office were normal and repeat laboratory results and urinalysis remained unremarkable. Per his mother, his rash and swelling completely resolved by 5 days.
Discussion
Autoimmune hemolytic edema of infancy is a rare cutaneous leukocytoclastic small-vessel vasculitis that affects children ages 4 to 24 months. 4 AHEI presents as a purpuric, targetoid rash with accompanying tender and nonpitting edema of the face and extremities. 2 These symptoms often present in the setting of a mild upper respiratory illness or other prodromal illness that causes mild fever.1,3 Symptoms of AHEI are usually limited to the skin. In addition to the symptoms listed above, general edema including scrotal edema and auricular edema are common. 3
Acute hemorrhagic edema of infancy is a benign condition that self-resolves after 1 to 3 weeks. 5 There is only a 5% to 10% chance of recurrence of symptoms for these patients. 3 Its presentation is similar to other more systemic and dangerous diseases, including Henoch-Schönlein purpura (HSP), meningococcemia, Kawasaki disease, erythema multiforme, and acquired coagulopathy, so it is important for primary care, urgent care, and emergency care physicians to be able to recognize and differentiate AHEI from these other conditions.
Laboratory findings for AHEI are nonspecific and nondiagnostic, but may include mild leukocytosis, lymphocytosis, thrombocytosis, or elevated inflammatory markers. 2 Coagulation studies, liver function tests, and kidney function tests remain normal. 1 Skin biopsy studies demonstrate leukocytoclastic vasculitis of the small blood vessels in the dermis layer of the skin. Immunoglobulin A (IgA) deposition is found in <25% of biopsy samples of children with AHEI. 5
Systemic involvement is rare (<10% of children with AHEI), which differentiates AHEI from HSP, which usually presents with nausea, vomiting, abdominal pain, as well as renal involvement.4,5 Some have argued that HSP and AHEI are not distinct diseases but are rather on a disease spectrum. However, HSP is an IgA-mediated disorder and biopsies of HSP lesions demonstrate IgA deposition, which, as mentioned above, is only seen in a quarter of AHEI biopsies.5,6 HSP presents at an older age, has systemic findings, and has predominance of purpura on the buttock and lower extremities compared with AHEI.1,6
Meningococcemia patients present with toxic appearance, fever, and a petechial rash, which are diagnostic pearls that can help differentiate these much sicker patients from AHEI patients. 1 Similarly, AHEI can be differentiated from Kawasaki and other common vasculitis by young age of onset, nontoxic appearance, absence of nonexudative conjunctivitis or lymphadenopathy, presence of edema, and complete resolution of symptoms within 3 weeks.1,6
There is no specific treatment for AHEI and the condition usually self resolves between 1 and 3 weeks.5,7 Systemic corticosteroids, anti-inflammatory drugs, and antihistamines are often prescribed but do not change the course of the illness. 1 Patients may receive antibiotics for presumed concurrent bacterial infections due to prodromal illness but these have not been found to affect the cutaneous manifestations of AHEI.1,5
Conclusion
Acute hemorrhagic edema of infancy is an often underrecognized and rare disorder that results in cutaneous lesions and edema in an otherwise well appearing child. The patient’s appearance, age, lack of systemic findings, and benign laboratory findings can quickly differentiate AHEI from other more severe disorders and help pediatricians avoid unnecessary, expensive, and invasive workups.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics Approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed Consent
Written informed consent was obtained from a legally authorized representative(s) for anonymized patient information to be published in this article.
