Abstract
Drug-induced thrombotic microangiopathy (DITMA) is a secondary cause of thrombotic microangiopathy and a potentially fatal inflammatory disease. DITMA has been attributed to a variety of drugs, particularly chemotherapeutic and immunosuppressive agents. Prompt diagnosis is critical for survival and treatment necessitates withdrawal of the offending drug; however, many cases require further treatment including plasmapheresis, immunosuppression, and anticoagulation. In this article, we report a cutaneous biopsy-proven case of tacrolimus-induced DITMA, which was successfully treated with eculizumab after failing the conventional standard of care.
Introduction
Drug-induced thrombotic microangiopathy (DITMA) can be challenging to diagnose given its rarity and difficulty in isolating the offending agent; however, early recognition is vital due to significant morbidity and mortality associated with it. DITMA has been associated with a variety of medications, herbal supplements, vaccines, toxins, and other substances. 1 The mechanism of action is not fully known; however, it can cause thrombotic changes in small blood vessels leading to eventual ischemia and multisystem end-organ damage. 2 DITMA can be divided into immune-mediated and direct toxicity reactions. 1 Immune-mediated reactions involve antibody formation against a particular drug causing endothelial damage leading to TMA. Dose-related toxicity reactions are dose-dependent and result from direct toxic effects of the drug on the microvasculature causing endothelial damage. 3 The diagnosis of DITMA is clinical and based on findings of microangiopathic hemolytic anemia, thrombocytopenia, history of drug exposure, the absence of severe ADAMTS13 deficiency, and histological findings of the affected tissue. 4 Treatment involves immediate withdrawal of the offending agent along with supportive care. Here we report a case of effective therapeutic response to eculizumab in a patient with tacrolimus-induced TMA who failed to show hematologic and renal function improvement with standard care.
Case Presentation
A 67-year-old Caucasian male with a past medical history significant for a liver transplant on prednisone and tacrolimus, heart failure with preserved ejection fraction, atrial fibrillation on apixaban, hypertension, and type 2 diabetes mellitus was admitted to an outside hospital 4 months prior to presenting to our hospital with a chief complaint of painful and necrotic ulcerations of the left first metatarsal and fifth toes. During this hospitalization, he was diagnosed with bilateral pulmonary emboli, subclavian clots, and thrombocytopenia. Skin biopsy was performed due to worsening necrotic ulcers, which showed intravascular clots and shaggy perivascular deposits of C4d. He was diagnosed with tacrolimus-induced TMA and was treated with 7 sessions of plasmapheresis with resultant improvement in thrombocytopenia and some of his lower extremity ulcerations; however, he did require amputation of his left great toe. Due to concern for tacrolimus-induced TMA but concomitant need for immunosuppression, he was switched to cyclosporine and later to everolimus due to thrombocytopenia associated with cyclosporine. Two weeks later, the patient was admitted to our hospital with worsening necrotic lesions and ulcerations of the left first metatarsal and fifth toes with significant spread to his bilateral lower extremities.
On examination, the patient was in mild distress. His temperate was 99.3 °F, the blood pressure was 103/73 mm Hg, the pulse rate was 117 beats per minute, and the oxygen saturation was 94% on 6 liters of O2 via nasal cannula. Jugular vein dilatation was noted. Effort and breath sounds were normal with no wheezes. No murmurs were appreciated. There was no abdominal tenderness or organomegaly. He had bilateral lower extremity edema. The left foot was cool and dusky with edema and the first left great toe was amputated-pulses present (Figure 1A and B). The amputation site was dry and black and the tip of the third toe was black (Figure 1A). Large open wounds were present on bilateral shins (Figure 1C and D). The left lateral leg ulcer measured 8 × 3 cm with an unknown true depth (Figure 1C). The wound base was moist, yellow, and black with no drainage. The right medial leg had an ulcer measuring 6.5 × 5.5 cm at the skin level with a dry and black wound base with no drainage or odor (Figure 1E-H). Bilateral arms had ecchymosis with a left arm ulcer measuring 3 × 1.5 × 0.2 cm (not shown). The wound base was moist and yellow with scant discharge.
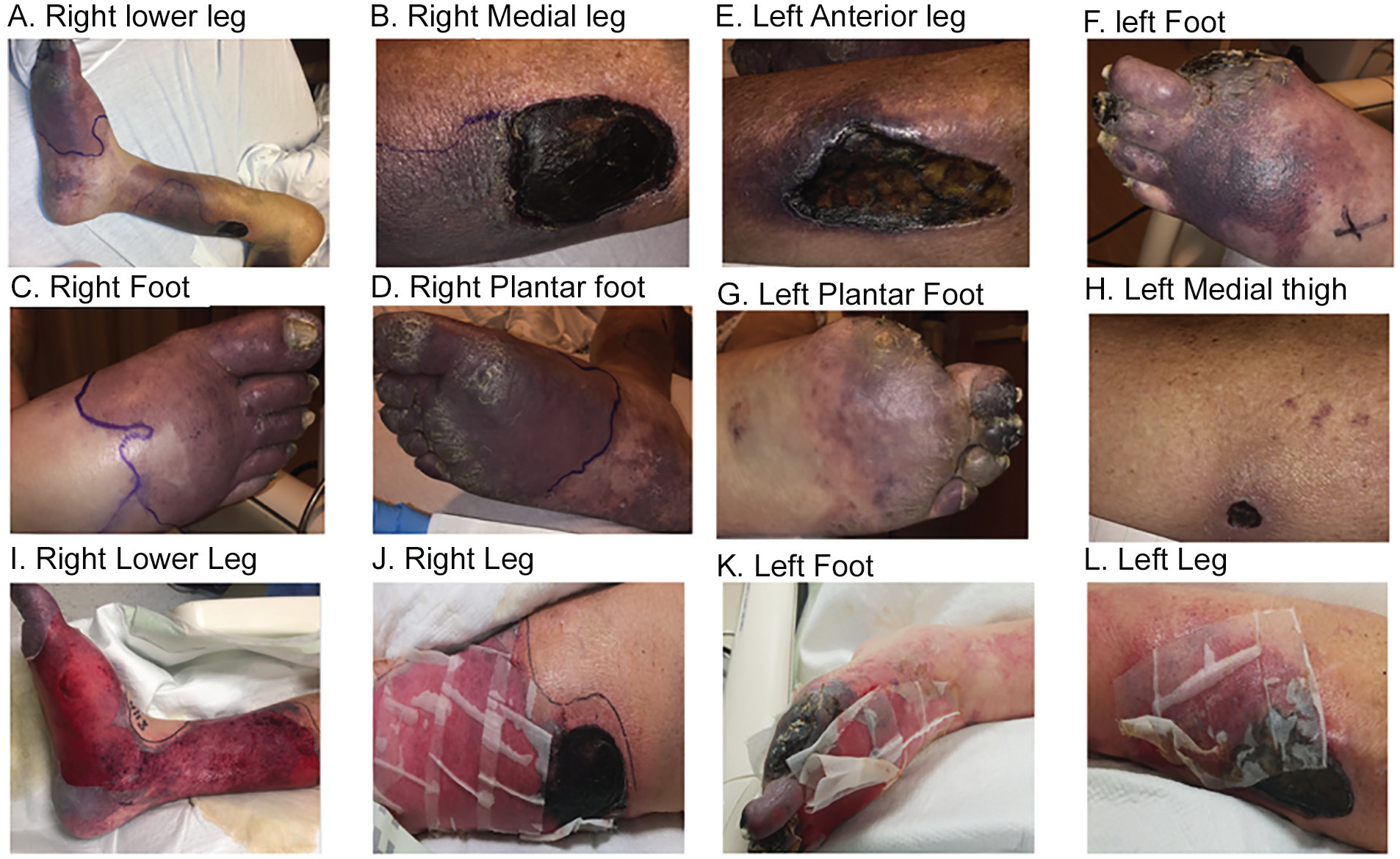
Shows patients lower extremity images before and after eculizumab therapy. Images A to H show the patient’s right and left lower extremity prior to eculizumab therapy. Images I to L show the patients right and left lower extremity 48 hours after eculizumab therapy.
Laboratory studies showed low hemoglobin at 9.0 g/dL (reference range: 13.5-18 g/dL; reference range is provided in the parenthesis in the following laboratory studies), platelet count at 30,000/µL (150 000-400 00/µL). Creatinine 1.33 mg/dL (0.66-1.25 mg/dL), prothrombin time 17.9 (9.9-13.1 seconds), international normalized ratio 1.6 (0.8-1.2), partial thromboplastin time was 27.2 (25.6-38 seconds), haptoglobin 463 mg/dL (30-200 mg/dL), and lactate dehydrogenase (LDH) 407 U/L (122-225 U/L). Autoimmune, vasculitic, and antiphospholipid antibody syndrome workup was negative. Hexagonal phase phospholipid and platelet neutralization phase were elevated but could not be interpreted as positive due to anticoagulation use. Inflammatory markers C-reactive protein 192.7 mg/L (<8.0 mg/L) and sedimentation rate 49 mm/h (<20 mm/h) were elevated.
On admission, the patient was continued on oral prednisone 30 mg twice daily along with everolimus 1 mg by mouth twice daily. Computed tomography angiogram of the bilateral lower extremities revealed <50% stenosis in tibioperoneal artery on the right side, suggesting that his ulcerative lesions were unlikely to be due to major vessel pathology and more likely due to small vessel disease. Skin biopsy from his left lower extremity wound showed tissue hemorrhage (Figure 2A and B) and fibrin thrombi (Figure 2C and D) with immunofluorescence showing antibodies against immunoglobulin (Ig) G, IgM, IgA, C3, and fibrin, suggestive of immune-mediated vascular injury. His hospital course was complicated by acute hypoxic respiratory failure requiring mechanical ventilation secondary to cytomegalovirus (CMV) and

Hematoxylin-eosin (H&E) sections from skin over the left foot shows extensive dermal hemorrhage (A and B) and rare fibrin thrombi in small vessels. H&E sections of skin and subcutaneous tissue from the right leg (C and D) show numerous fibrin thrombi within small vessels.
Workup for thrombocytopenia and normocytic anemia with peripheral blood smear showed rare schistocytes. LDH and haptoglobin were elevated and not indicative for overt hemolysis and direct coombs test was negative. ADAMTS13 activity level was normal at 94% and did not support the diagnosis of thrombotic thrombocytopenic purpura. His prothrombin time, partial thromboplastin time, and international normalized ratio were within normal limits and not suggestive of disseminated intravascular coagulation. Due to his ulcerative cutaneous lesions, thrombocytopenia, and prior improvement of his skin lesions at the outside hospital with plasmapheresis, he received 4 more sessions of plasmapheresis. There was initial concern for the possibility of antiphospholipid syndrome and his steroids were increased to IV solumedrol 125 mg daily and he was started on a heparin drip. While on high-dose steroids, his platelet counts only increased from 30 000 µL to 57 000 µL; however, there was no improvement in his lower extremity ulcerations.
Given his overall worsening necrotic low extremity skin lesions suspected to be secondary to small vessel ischemia, significant thrombocytopenia, and acute kidney injury, there was concern for DITMA secondary to tacrolimus. Due to limited improvement with drug withdrawal, steroids, and plasma exchange, he was given IV eculizumab, 900 mg 2 times 7 days apart. The patient had significant improvement in several of his lower extremity ulcerations (Figure 1I-L) and had a sustained creatinine within normal limits. His platelets showed dramatic response and quickly normalized after just one infusion and LDH and haptoglobin levels both normalized.
Prior to eculizumab infusion, the patient was offered below knee amputation of his left leg and transtarsal amputation of his right foot due to the extent of his necrotic lesions. The patient was interested in a second opinion for potential amputation and was transferred to an outside hospital. His total hospital stay was 22 days.
Discussion
The terminal complement-inhibitor, eculizumab, is currently food and drug administration–approved for paroxysmal nocturnal hemoglobinuria, atypical hemolytic uremic syndrome, generalized myasthenia gravis, and neuromyelitis optica spectrum disorder. It is not approved for patients with persistently positive antiphospholipid antibodies, refractory catastrophic antiphospholipid syndrome, or TMA, although there are many case reports and case series with successful outcomes. Like other monoclonal antibody therapies, eculizumab is a potent immunosuppressant and all patients must receive meningococcal vaccine at least 2 weeks prior to treatment or receive antibacterial prophylaxis. Our patient had already received the meningococcal vaccine; however, given his immunocompromised state, precautionary measures were taken with antibiotic use and close monitoring.
Our patient presented with severe skin involvement and thrombocytopenia secondary to DITMA; he did not present with the classic findings of TMA such as macroangiopathic hemolytic anemia and severe renal failure. Skin involvement has not classically been reported in cases of DITMA although it has been reported in thrombotic thrombocytopenic purpura and atypical hemolytic uremic syndrome. The most commonly affected organ system in complement-mediated TMA are the kidneys; however, up to 20% of patients experience extra-renal manifestations affecting the central nervous system, lungs, skin, skeletal muscle, and gastrointestinal tract.5,6 Our patient did show evidence of kidney injury with elevated creatinine and evidence of proteinuria at 5.7 g per 24 hours, which improved after eculizumab treatment.
Some cases of tacrolimus DITMA have successfully been treated on discontinuing therapy along with plasma exchange. Switching immunosuppression from tacrolimus to cyclosporine has been associated with initial resolution of TMA, but in some cases, TMA can recur. 7 Our patient was initially switched to cyclosporine without improvement, which prompted the switch to everolimus. There has been no strong evidence linking the use of everolimus with DITMA, as most cases of DITMA were related to tacrolimus, quinine, and cyclosporine. 1 Immediate drug discontinuation in the case of suspected DITMA is the mainstay of management. Other treatment modalities such as plasma exchange have been used with variable success rates. In gemcitabine-induced TMA, about 50% of patients progressed to end-stage renal disease despite plasma exchange.7,8 In some cases where withdrawal of the offending agent and plasma exchange were unsuccessful, eculizumab resulted in resolution of renal failure.2,8-10
In our patient, stopping the offending agent was not enough. He was tried on the standard of care for general TMA with steroids and plasma exchange but with only minimal benefit. De novo TMA has been reported, mostly in renal transplant patients, and can occur months to year’s post-transplant. Risk factors include use of immunosuppressive drugs, malignancy, and infections. 11 CMV as a potential trigger for posttransplant TMA has only been reported in a few cases. It has been shown that CMV infection can damage endothelial cells and induce platelet adherence and aggregation leading to microvascular thrombosis and TMA. 12 In most cases, patients were treated with IV ganciclovir, in one case, the patient was treated with eculizumab with complete recovery. 13
The significant clinical and laboratory response of our patient to eculizumab strongly suggest a dysregulation within the complement system in the pathophysiology of DITMA. There have been many case reports of DITMA attributed to chemotherapeutic agents such as gemcitabine and mitomycin-C in cancer patients that resolved with the treatment of eculizumab.8,14 There have been a few reported cases of drug-induced transplant-associated thrombotic microangiopathy as a rare but serious complication with the most common offending drug being tacrolimus and sirolimus.15-19 These previous cases involved the transplanted organ, which was unaffected in our patient.
Conclusion
In summary, we reported a patient with a case of DITMA with severe skin and musculoskeletal involvement that responded to eculizumab therapy. We therefore suggest that further studies address the therapeutic potential of drugs that target C5 and other potential components of the complement activation cascade in patients with DITMA who fail to improve on drug withdrawal and conventional therapy alone.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics Approval
We confirm that ethical committee approval was sought where necessary.
Informed Consent
We confirm that guidelines on patient consent have been met.
