Abstract
Aim:
This in vitro study compared the fatigue resistance of two polymeric materials (Nylon and Polytetrafluoroethylene (PTFE)) used as retentive attachments in implant-retained overdentures after immersion in denture cleansing solution.
Materials and Methods:
A total of 24 samples (N=24), of which 12 capsule-shaped samples of commercially available nylon material from ADIN dental implants, India, and similar sized and shaped 12 PTFE (medical grade) capsules custom fabricated from AAA Industries, Mumbai was obtained. Six samples of each material were immersed in distilled water and six samples in Clinsodent denture cleanser, simulating an 8–h daily immersion of the denture for a period of 2 years. After completion of the immersion protocol, samples were subjected to 2900 fatigue cycles using the Universal Testing Machine (UTM), simulating 4 cycles per day of removal and insertion of the overdenture for a duration of 2 years. Before and after immersion, the wear of the samples was assessed for internal and external diameter changes using the Sipcon Inspection System. The statistical analysis of the obtained results was tested by applying the paired-t test, Fisher analysis of variance, and Tukey’s honest significant difference test, with a probability value less than 0.05 used as statistically significant.
Results:
Statistically significant differences were observed after immersion in denture cleanser for nylon and PTFE. The greatest fatigue for ID, IHL, and IVL was demonstrated in nylon immersed in Clinsodent at p = .000. ED and EHL of PTFE in distilled water showed greater deformation than others (p = .000).
Conclusion:
PTFE attachments have shown better fatigue resistance after immersion in Clinsodent denture cleanser. Nylon material immersed in distilled water as well as in Clinsodent cleanser showed greater deformation after fatigue cycles.
List of Abbreviations
Polytetrafluoroehthylene
Internal diameter
Internal vertical length
External vertical length
Internal horizontal length
External horizontal length
Scanning electron microscope
Null hypothesis
Introduction
The removable denture is commonly used as a prosthesis in edentulous patients, but severely resorbed mandibular ridges pose some problems, like difficulty in obtaining stability with the mandibular prosthesis, poor retention, and discomfort during mastication. The decreased chewing efficiency and altered speech ultimately result in poor health and decreased self-esteem for the patient. 1 Supporting and harmonizing such collapsed dentition using different techniques available at the prosthodontist’s disposal is the key to aesthetic replacement for all losses. 2
Prosthetic rehabilitation of completely edentulous patients with implant-retained overdentures is an excellent, reliable alternative treatment for improved masticatory efficiency, comfort, and patient satisfaction, with considerably high long-term success rates. 3 The conference on overdentures recommended that the choice of prosthesis in the lower jaw with all missing teeth be a removable prosthesis stabilized with two implants. 4
Different attachments, such as studs, bars, and clips, are used to maintain implant overdentures in place. 5 The most popular systems for two implantation cases have been ball or O-ring and locator-type connection systems. 6 O-ring attachments have advantages, including simplicity in design, strong retention, low cost, reduced Candida albicans colonization, ease of maintenance, and the potential elimination of a superstructure bar. As a result, choosing ball attachments for elderly patients is reasonable in light of their benefits. 7
The prognosis of implant prostheses with different attachments is expected to be good, with a success rate of 97%–99%, but failures also occur. 8 Attachments are also associated with mechanical or biological complications. 3 For the longevity and maintenance of prostheses, hygiene maintenance is extremely important. Thorough cleaning of the prosthesis with a combination of chemical and mechanical techniques that allow access to the undercuts areas where biofilm accumulates has yielded satisfactory results due to the simplicity of the technique, greater accessibility, and clinical efficacy.6,9
However, chemical solutions employed in overdenture hygiene can produce harmful changes in soft materials, which are currently used for the manufacture of retentive attachments, resulting in their premature aging and weariness.6,9 Since corrosion of the prosthetic attachments is also exacerbated by immersion in chemical cleaning solutions at night, they often need to be replaced more frequently since they are more likely to deteriorate. 9
Patients frequently maintain dentures in liquids such as water, NaOCl, and other liquids using effervescent tablets. 10 Reviewing several pieces of literature, it is shown that NaOCl causes retention loss and bleaches the acrylic. There is no agreement regarding the best recommended overdenture cleanser because different studies have produced different findings. The most frequent (33%) prosthodontic problem among all implant restorations has been recognized as the wear of overdenture retentive systems. 11 In a half-decade prospective in vivo study, Winkler et al. and Naert et al. stated that O-ring attachment retained onlay dentures needed the replacement of 29 O-rings, but bar-attachment overdentures only required the replacement of two clips. 11
O-rings gradually lose their retention as they age and need to be replaced. Increased O-ring wear is seen due to the lack of parallelism of implants and creates a weak spot that increases the chance of abutment neck fracture. 7 Inadequate laboratory practice, an improper O-ring size, and resulting damage during insertion and removal can all make these problems more complicated. Therefore, it has become necessary in dentistry to adopt an alternative biocompatible material with higher mechanical qualities and longer clinical longevity and understand how these various materials interact. 9
This study incorporated new overdenture attachments using polytetrafluoroethylene (PTFE) material and compared the deformation of this material with that of a commercially available nylon capsular attachment after immersion in denture cleansing solution using a fatigue resistance test. The H0 considered was that the various types of attachments after immersion in denture cleansing solution would not show wear effects after subjecting them to cyclic fatigue.
Materials and Methods
The study was approved by the ethical committee of Dr. D.Y. Patil Dental College and Hospital (reference no: DPU/484/8/2021).
Preparation of Specimen
A total of 24 samples (N=24), of which 12 capsule-shaped samples of commercially available nylon material from ADIN dental implants, India, and similar sized and shaped 12 PTFE (medical grade) capsules custom fabricated from AAA Industries, Mumbai was obtained.
Two rectangular blocks with the dimensions of 4×3×3 cm were fabricated with modeling wax (Deepti modeling wax sheets, India), which were flasked and processed in heat-cured acrylic resin (Triplex by Ivoclar Vivadent). To insert implant analogs with dimensions 3.75×10 mm, two implant sockets 22 mm apart were made in one resin block using a surgical drill (ADIN dental implants, India). To align implant analog orientation troughs apace with one another and perpendicular to the horizontal plane, a dental surveyor was employed. The implant analogs were placed in the sockets and filled with auto-polymerizing resin (DPI, India). Ball abutments were fitted onto the implants after polymerization (Figure 1A), and metal housings holding the retentive samples were secured to the respective abutments.
A dental parallelometer was used to prepare the location for female housings in the upper block. A cold-cured resin was applied to secure female housings that contained the retentive samples, simulating a direct method, that is, the clinical pick-up procedure (Figure 1B). Proper coupling was achieved between the ball abutment in the lower block and the metal housing with retentive samples in the upper block.
(A) Lab Analogues with Ball Abutments Secured within Acrylic Block Using Cold Cure Acrylic Resin Parallel to Each Other with the Help of Surveyor at a Distance of 22 mm. (B) Metal Housings Picked Up in Another Acrylic Block and Sealed with Cold Cure Acrylic Resin. (C) The Opposing Surface of an Acrylic Block with Metal Housings Held with a Metal Loop for Lab Testing Purpose.

A metallic eyelet was attached at the upper portion and midpoint of the upper block to perform the test (Figure 1C). All 24 polymeric samples of PTFE (n = 12) (Figure 2A) and nylon (n = 12) (Figure 2B) were tested on the same model.
(A) 12 Samples of Retentive Capsules of PTFE Material. (B) 12 Samples of Retentive Capsules of Nylon Material. (C) Nylon and PTFE Capsules Immersed in Distilled Water (Control Group) and Clinsodent Denture Cleansing Solution (Test Group), Which Was Replaced Daily 8 h. (D) An Acrylic Block Having Metal Housings with Capsules Attached Over Another Acrylic Block with Lab Analogues, Secured in Position Using a Firm Platform for Cyclic Loading using UTM for 2900 Fatigue Cycles.

Protocol for Immersion in Cleansing Solutions
Six samples of each material were immersed in distilled water, and 6 samples of each material were immersed in Clinsodent denture cleanser (sodium perborate monohydrate, 480 mg). The immersion protocol was to simulate 8 h per day of immersion for a period of 2 years (24 months = 720 days) (Table 1).
Distribution of Samples among Groups and Immersion Protocol for Simulated Duration.

This immersion protocol was to simulate 8 h of overnight immersion of dentures. According to the recommendations of the manufacturer, Clinsodent solution was made. To keep the samples from floating on the surface of the water, they were placed inside a tiny perforated plastic bag filled with glass beads. Plastic bags were immersed in 150-ml beakers containing distilled water and denture cleansing solution, respectively (Figure 2C).
After 8 h, the samples within the perforated bags were removed and rinsed under tap water for 15 s. Distilled water and Clinsodent solution in the beaker were renewed with a new solution to mimic the daily change of solutions after every 8 h as per the post-denture insertion instructions.
Testing Procedure
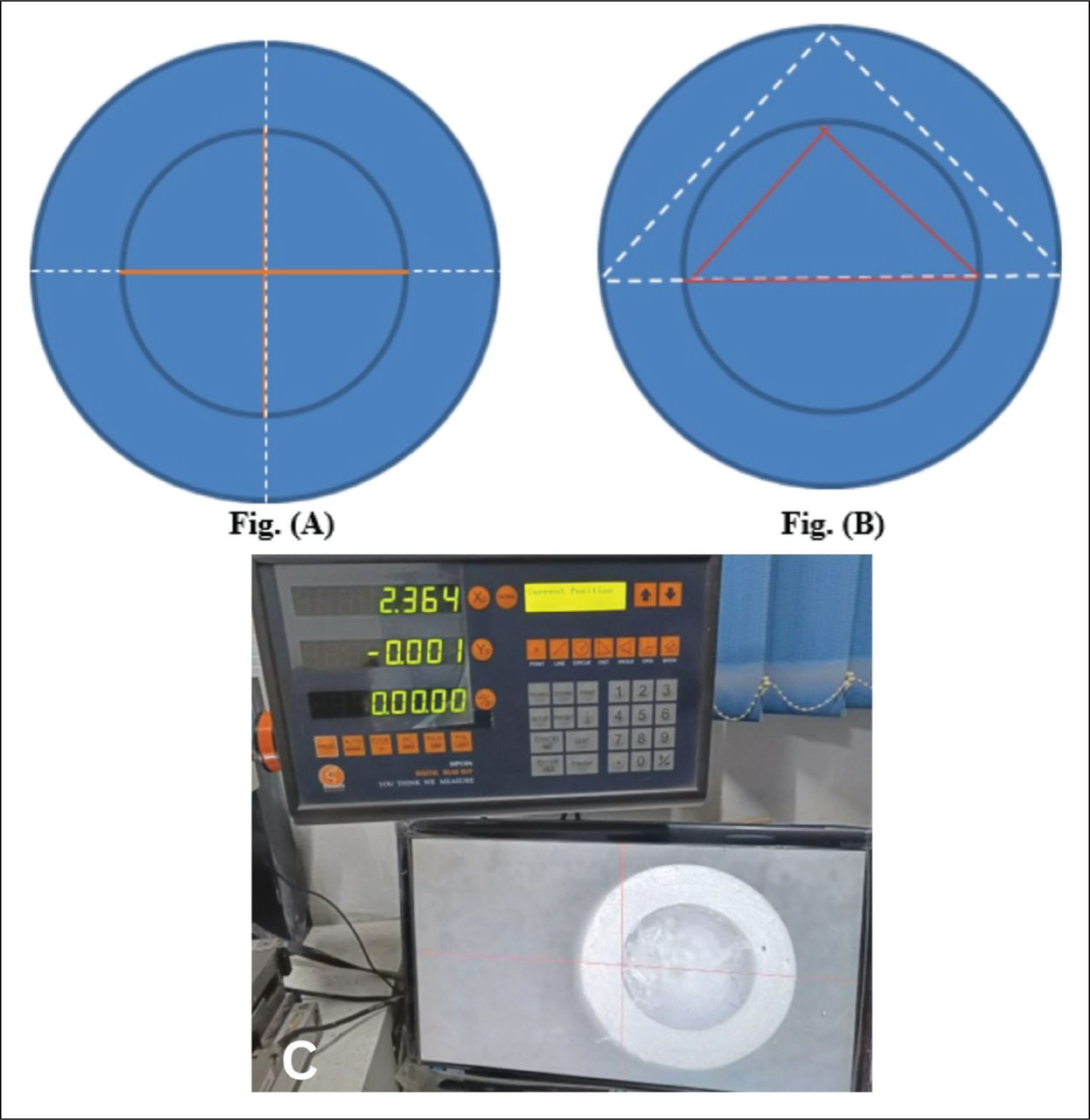
After completion of the equivalent time of immersion, samples of each material were inserted one after another into the intaglio surface of metal housings, which are inserted into one resin block. Metal housings were fitted onto the ball abutments screwed to the implant analogs inserted in another resin block, ensuring proper coupling between the two resin blocks. The fatigue resistance of samples was assessed using a universal testing machine (UTM) (Figure 2D). Before subjecting the samples to fatigue testing, the quantitative assessment of the samples of each material was done by two methods. First, measurements of internal and external horizontal lengths as well as internal and external vertical lengths were obtained by choosing two points (Figure 3A). In the second method, internal and external diameters were assessed using three points, as shown in Figure 3B. The Vision Inspection System (Sipcon Measuring Systems, India) was used for this assessment (Figure 3C).
(A) Internal (Continuous Line) and External (Dotted Line) Horizontal and Vertical Length. (B) Internal Diameter and External Diameter. (C) Vision Inspection System Showing Measurement of Internal Diameter of Nylon Attachment.
The fatigue resistance was analyzed by clamping the resin blocks tightly to the UTM (ACME engineers, India). Samples were subjected to a tensile force of 5–7 N on the center of the upper block, which was fixed to the UTM. As given by Lehmann and Arnim, attachment retention forces ranging from 5 to 7 N have been reported to be the force required to stabilize overdentures. 6 Testing was done by performing 20 cycles/min with a constant speed of 35.79 mm/s and load cell of 100 kg. A total of 2900 cycles were performed on the samples of each material, simulating 4 cycles per day of removal and insertion of the overdenture for a duration of 2 years (24 months).
Post-fatigue cycles of the 2900, the measurements of the samples of each material were remeasured as mentioned before using the Vision Inspection System (Sipcon Measuring Systems, India) (Figure 3A and B).
Statistical Analysis
Statistical software (SPSS Version 23; Chicago Inc., IL, USA) was used to carry out statistical analysis of the obtained results. Variables were compared using mean values and standard deviations. The difference in the mean of fatigue cycles in individual groups before and after immersion was tested by applying a paired “t” test. The means of different readings for fatigue cycles were compared using the analysis of variance test. Tukey’s Honest Significant Difference Test was applied to find significant differences between pairs. p < .05 was considered to be statistically significant.
Results
ANOVA statistical analysis of our study demonstrated significant differences in internal vertical length, internal horizontal length, and internal diameter of nylon and PTFE material immersed in Clinsodent denture cleanser at p = .000. As shown in Table 2, when compared between before and after fatigue cycles using a paired “t” test, internal diameter readings showed the greatest fatigue in nylon of the Clinsodent group with a mean of 9.3857 ± 0.04532, which was significant at p = .000. This finding was confirmed when nylon in Clinsodent group showed statistically significant differences for IVL with a mean of 7.3372 ± 1.01712 at p = .024 and IHL at a mean of 6.2563 ± 0.3036 at p = .000 exhibiting the greatest deformation among all.
Demonstrating the Mean Scores of Different Variables of Individual Group before and after Immersion.
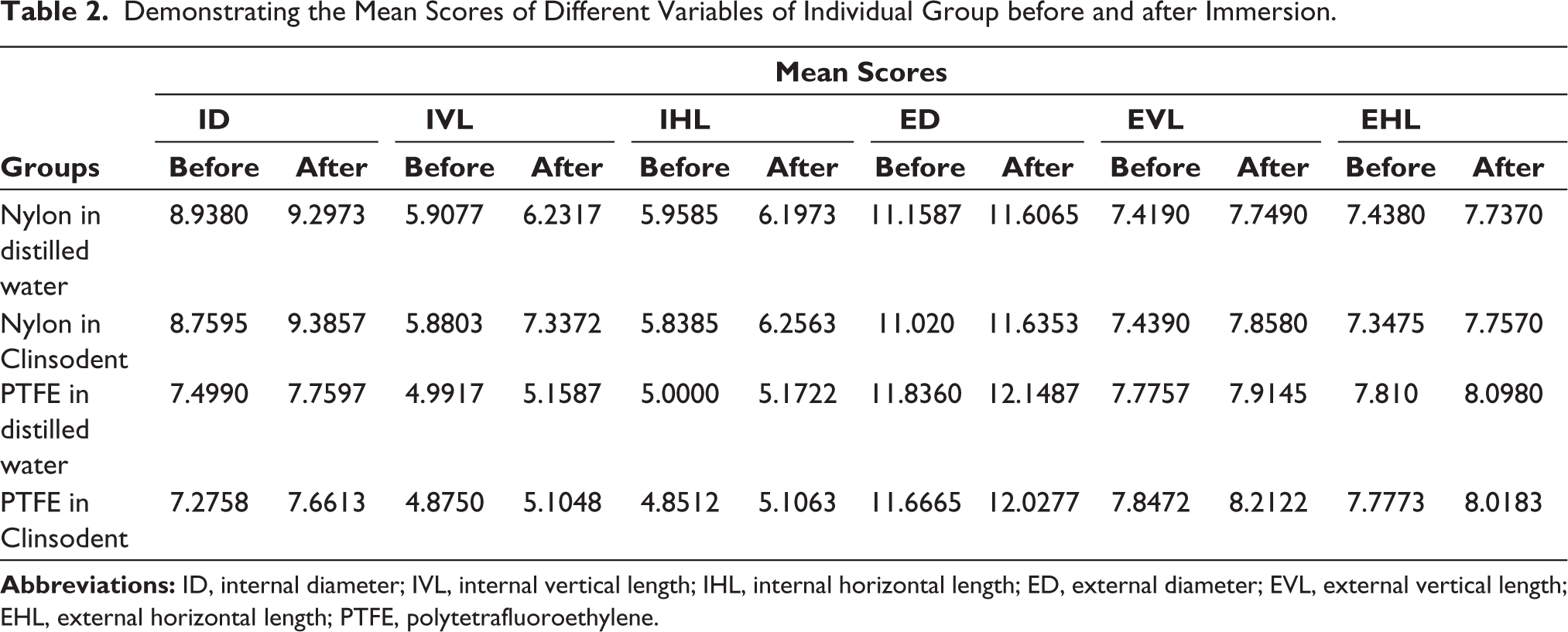
On Tukey’s post hoc analysis between pairs as presented in Table 3 for IHL assessment, the greatest mean difference was noted between Nylon in Clinsodent vs. PTFE in Clinsodent at 1.15000, which was significant at p = .000. Significant differences were also noted between the groups of nylon in distilled water vs. PTFE in distilled water, as seen in Table 3.
Post hoc Assessment of Fatigue Resistance of Different Variables between Groups (after Immersion).
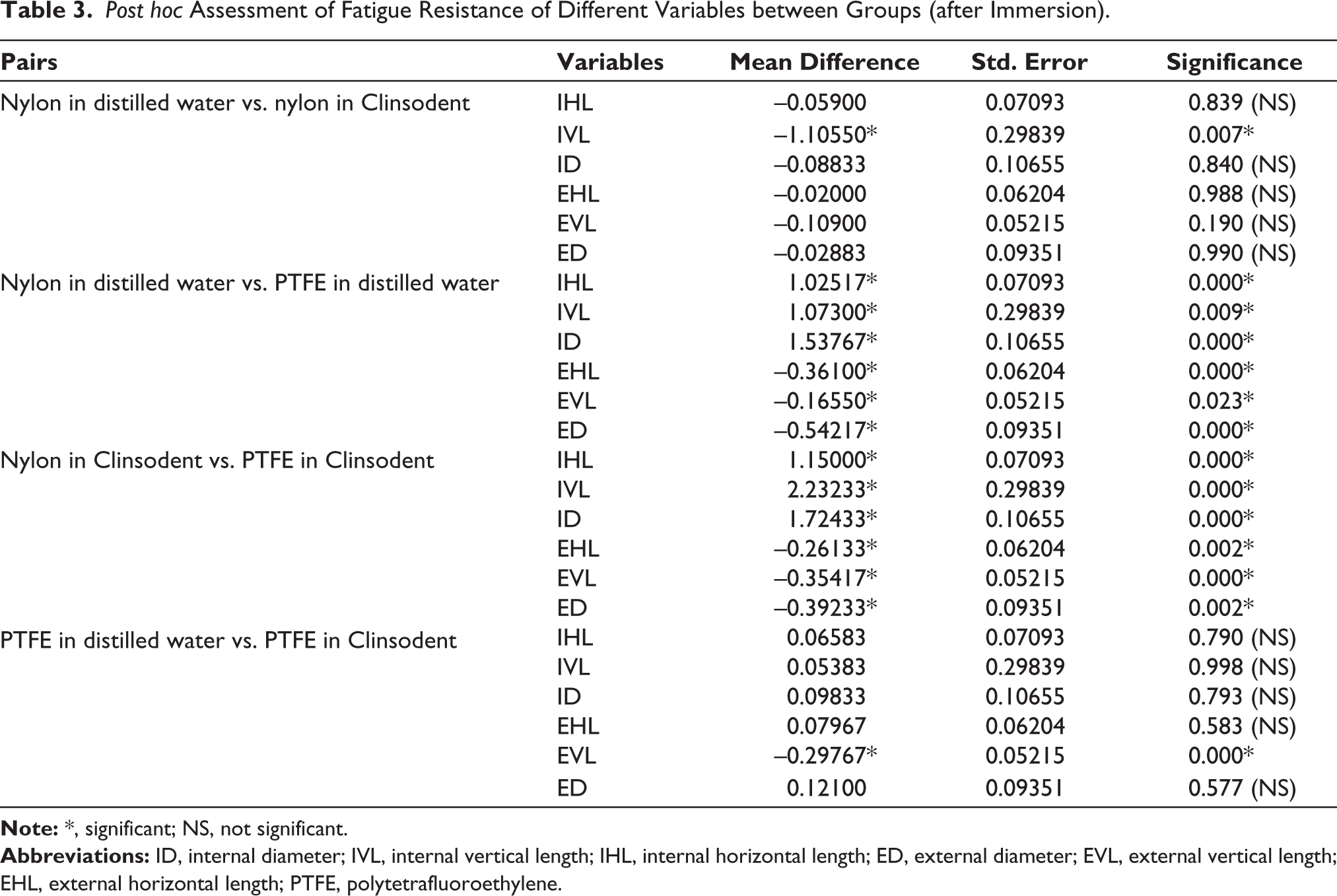
In addition, post hoc analysis of IVL between groups (after immersion) showed the greatest mean difference was noted between Nylon in Clinsodent vs. PTFE in Clinsodent 2.2323, which was significant at p = .000. Significant differences were also noted between the groups of nylon in distilled water vs. nylon in Clinsodent and nylon in distilled water vs. PTFE in distilled water, as seen in Table 3.
Post hoc assessment of ID between groups (after immersion), nylon in distilled water vs. PTFE in distilled water and nylon in Clinsodent vs. PTFE in Clinsodent have shown statistically significant differences in the internal diameter post fatigue cycles (Table 3).
In a post hoc analysis of EHL assessment, nylon in distilled water vs. PTFE in distilled water demonstrated the greatest mean difference at -0.36100, which was significant at p = .000. No significant difference was found between the groups of Nylon in distilled water vs. Nylon in Clinsodent and PTFE in distilled water vs. PTFE in Clinsodent (Table 3).
For EVL, nylon in Clinsodent vs. PFTE in Clinsodent showed the greatest mean difference significant at p = .000 between pair comparisons. For ED, on post hoc analysis, nylon in Clinsodent vs. PTFE in Clinsodent showed the greatest statistically significant differences (–0.39233) followed by nylon in distilled water vs. PTFE in distilled water (–0.54217) post fatigue cycles (Table 3).
Discussion
In the era of 21st century, modern restorative dentistry has allowed the transformation of structurally malformed, malposed, and discolored teeth into a particularly appealing form. 13 This is because a wide variety of materials and procedures have been developed, which has resulted in a significant improvement in aesthetics. 14 The conventional complete denture fabrication process basically includes working with different impression materials along with their clinical or laboratory techniques. 15 Especially for markedly resorbed mandibular alveolar ridges, implants can provide more stability. But it also poses a few difficulties, like the patient’s systemic problems, financial constraints, or his psychological state. 16 For such cases, implant-retained overdentures with ball-type retentive attachments have proven to be a successful and affordable oral rehabilitation approach.17,18
Overdenture attachments have benefits such as easy insertion and removal, hygiene maintenance, and minimal cost; however, they are subjected to complex three-dimensional movements as a consequence of masticatory loading, insertion, and removal. This may alter the physical-mechanical properties of attachment components. 19 Reduced retention caused by degradation, wear, and the eventual breakage of attachment components with time is the mechanical problem with implant-supported overdentures. Functional stresses, the trajectory of inserting and removing the prostheses, the angle of the implants, and parafunctional habits all contribute to surface fatigue, with a consequent decrease in retention. That often happens within the first 12 months of use, necessitating more frequent maintenance. 20
As time progressed from 1980, implants were modified in design as well as texture. 8 Similarly, for prosthetic materials, the adoption of alternate biomimetic materials with higher mechanical qualities and clinical longevity has become a demand in the dental field. Synthetic biomaterials like PTFE have significant advantages. Branchi et al. have stated that PTFE is a self-lubricating material, which leads to less wear. 21 It is chemically inert and does not absorb water, resulting in excellent dimensional stability. Any changes in its retention are therefore more gradual when compared to materials with greater frictional coefficients. Due to its excellent chemical resistance and minimal cell adhesion, this material is less likely to degrade when exposed to denture cleaning solutions. 19
For hygiene maintenance and longevity of prostheses, chemical denture cleansing solutions are advised along with mechanical methods because they are more effective. 20 Chemicals like effervescent tablets contain sodium perborate and sodium bicarbonate, and the resulting peroxide solution mechanically eliminates debris by releasing oxygen. Despite their efficacy, denture cleansers have been reported to cause deleterious effects on prosthetic materials. 5 Certain denture cleansers such as Corega tablets and sodium hypochlorite cause retention loss, as suggested by the findings of Derafshi et al., 22 due to the acidic and oxidizing nature of Corega and the corrosive properties of sodium hypochlorite. Studies have mentioned that NaOCl produced cracks and porosities and altered the surface morphology of nylon, which was observed under SEM. 10 Similar findings about decreased retention of locator attachments due to NaOCl were observed by Nguyen et al. 18 Hence, our study compared the effect of denture cleansers on nylon and a newer biocompatible polymeric material, PTFE, to overcome the drawbacks of nylon material using fatigue resistance tests.
The study rejected the null hypothesis as retentive attachments of different materials behaved differently and showed wear after immersion in denture cleansers and post-fatigue cycles. In the available literature, no study was found where PTFE attachments were subjected to denture cleansing solutions. Valente et al. 23 evaluated the retention and deformation of PTFE, polyacetal, and traditional silicone O-rings after subjecting them to 3625 fatigue cycles. They found that polyacetal and PTFE had greater internal deformation than the traditional O-rings. The polyacetal attachments demonstrated the highest retention despite the fact that they underwent the most deformation. 23 However, in that particular study, attachments were not immersed in denture cleansing solution. In contrast, ANOVA statistical analysis of our study demonstrated significant differences in internal vertical length, internal horizontal length, and internal diameter of nylon and PTFE material immersed in Clinsodent denture cleanser at p = .000. Evaluation for internal diameter before and after fatigue cycles seemed to increase in every group, suggesting that a certain amount of wear occurred in all, the greatest being in the nylon attachment (Table 2).
Similar to our findings, Kim et al.’s study found that after 2500 cycles of insertion and removal, SEM analysis of the attachments showed noticeable deformation and deterioration in the surface morphology of the rubber matrix of the O-ring and the nylon matrix of Kerator, but no noticeable change in the ceramic ball. 24 In contrast with the outer ring area, he discovered that the nylon matrix underwent significant deformation and degeneration, mostly in the center core. Thus, these results support our study findings that IVL, IHL, and ID of nylon material showed consistent deformation when compared to PTFE. Thus, our study also supports the idea that the material of attachment is one of the factors that influence wear patterns.
In our study, when compared between the groups for IHL, ID, and IVL, the greatest wear due to fatigue was seen in nylon in the Clinsodent group and the least noted in PTFE in Clinsodent. In comparison to the distilled water group, nylon has shown more statistically significant differences and the greatest fatigue. But for EVL, PTFE was found to have more deformation in contrast to the findings of Valente et al., 23 and statistically significant differences were seen with the samples of nylon in Clinsodent. This was similar to the ED group’s findings. However, this external deformation of attachments has no effect on retention loss. 23 This dissimilarity the with previous study may be due to the inappropriate removal of PTFE samples through housings after fatigue tests or any other unknown reason. As the complex mechanism of wear involving surface fatigue, corrosive, adhesive, and abrasive components is essentially unknown, more research could be done further. 22
Limitations
In support of our study, as literature suggests that PTFE is inert to microorganisms and not influenced by denture cleansing solutions, 9 it can be further evaluated with a greater number of samples since our study tested only six samples per group. Saliva composition, amount and qualitative type of saliva, and thermal behavior were not simulated in this study. Samples were continuously soaked in the cleansers for 8 months, so more changes might appear after a longer period of immersion time. Horizontal and oblique forces were not simulated in this study, which occur clinically, as do masticatory and parafunctional forces. Testing of physical-mechanical properties of PTFE materials such as surface roughness, hardness, and the assessment of retention forces was not performed.
Future Implications
Further research considering longer fatigue cycles can be performed. The in vitro results of this research should be clinically validated.
Conclusion
Within the limitations of our study, we can conclude that PTFE attachments have shown better fatigue resistance after immersion in Clinsodent denture cleanser. Nylon has less fatigue resistance as it has shown more wear and deformation when compared to PTFE, and immersion in denture cleanser solution has aggravated the same. Also, nylon material immersed in distilled water and nylon immersed in Clinsodent cleanser showed greater deformation after fatigue cycles. Thus, an alternative material used as a retentive attachment may offer a longer life span, prolong the time interval between periodic replacements, and benefit patients with improved quality of life.
Footnotes
Authors’ Contributions
Conceptualization, methodology, data curation, investigation, writing and preparing the original draft was done by Dr. Akanksha Shinde along with Dr. Nilesh Bulbule. Dr. Varun Bhatt and Dr. Balachandran Gayathri helped in data curation and editing of original draft. Dr. Amit Jagtap contributed in visualization, supervision and made the resources available.
Data Availability Statement
The data incorporated in study cannot be made available.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
The study was approved by the ethical committee of Dr. D.Y. Patil Dental College and Hospital (reference no: DPU/484/8/2021).
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Informed Consent
Not applicable
