Abstract
Aim:
To evaluate the microshear bond strength (µSBS) of mineral trioxide aggregate and Biodentine to various resin-based materials using different adhesive strategies.
Materials and Methods:
Three resin-based materials—a self-adhering resin composite with or without acid etching (Vertise flow; Kerr, Orange, CA, USA), a conventional flowable composite with a total-etch adhesive (Filtek Ultimate Flowable; 3M ESPE, St. Paul, MN, USA), and a flowable resin-modified glass ionomer cement (RMGIC) without any surface modification (Ionoseal; VOCO GmbH, Cuxhaven, Germany)—and two calcium-silicate-based materials—Biodentine and BIOfactor mineral trioxide aggregate (MTA)—were tested. A total of 100 cylindrical acrylic molds were prepared. Biodentine and BIOfactor MTA were prepared and placed into the central holes on the molds. Specimens were divided into two main groups according to materials and into five subgroups (n = 10). µSBS were evaluated using a µSBS testing device. The failure modes were examined under a stereomicroscope with magnification. They were categorized as adhesive, cohesive, or mixed. Data were analyzed using two-way analysis of variance (ANOVA) and Tukey test. The significance level was taken as α = 0.05.
Results:
It was observed that both calcium-silicate-based material type and resin-based material type influenced the µSBS significantly according to two-way ANOVA. Biodentine exhibited higher bond strength values than MTA. However, no statistically significant interaction was demonstrated between these factors (P = .396). The µSBS values of intermediate materials to Biodentine and MTA were listed from the lowest to the highest as follows: RMGIC < Acid Etch + RMGIC < SARC (self-adhering resin composite) < FC (flowable composite) < Acid Etch + SARC.
Conclusion:
Self-adhering composites can be used on calcium-silicate-based materials in vital pulp treatments because of their mechanical properties. Acid-etching ensures high µSBS values. Although the µSBS of Biodentine were higher than MTA according to this study’s results, there was no statistically significant difference in µSBS of FC and acid-etched SARC to MTA.
Keywords
Introduction
The restorative treatment of teeth with exposed pulp poses a challenging task for clinicians.1, 2 The preservation of vital pulp is essential to improve the long-term survival rate of restored teeth.2–4 The approach of protecting the exposed vital pulp by covering it, initially using a tiny piece of gold, was introduced by Pfaff in 1756. 5 The main rationale behind pulp capping is the induction of dentin bridge formation and the protection of the pulp tissue against thermal, mechanical, and chemical stimuli. 3 Vital pulp therapy (VPT) is now an essential part of everyday clinical practice and it continues to gain in importance, especially in pediatric dentistry, endodontics, and restorative dentistry. Specific biomaterials produced for VPT release calcium and hydroxyl ions to the surrounding pulp–dentin complex to induce reparative processes. One such biomaterial is calcium hydroxide, the oldest and most well-documented VPT material, which was first introduced as a root canal filling material in the 1920s. 5 However, although the use of calcium hydroxide is popular, this material is known to have some disadvantages, such as its higher solubility and resulting dentin bridge with tunnel defects within the newly formed reparative dentin.6, 7 These shortcomings have spurred researchers to develop optimum VPT material with better durability and superior tissue healing capacity. 8
In the 1990s, MTA—a material containing tricalcium aluminate, dicalcium silicate, tricalcium silicate, tetracalcium aluminoferrite, and bismuth oxide—was introduced. Although MTA has improved durability and bioactivity compared with its predecessor, calcium hydroxide, 9 it also has some drawbacks, such as handling difficulties, long setting time, and tooth discoloration over time. 10 To overcome the disadvantages of MTA, another calcium-silicate-based material called Biodentine (Septodont, St. Maur-des-Fossés, France) was introduced and found to have promising properties. Biodentine has dentin-like mechanical properties and contains tricalcium silicate, dicalcium silicate, calcium carbonate, iron oxide, and zirconium oxide. It has two major superior attributes, which are its faster setting time and higher mechanical strength; these points enable it to be used as a permanent dentin replacement material.11–13 In addition, Biodentine comes in the form of capsules that result in more precise proportions, giving a predictable, reproducible, and homogeneous consistency compared with MTA, which is prepared by hand mixing.
The quality of the bond between VPT material and definitive restorative material is decisive for the prognosis of VPT. Moreover, a leak-proof restoration with a balanced stress distribution ensures long-term success. 8 For these reasons, an intermediate material is usually placed on the VPT material under final restoration. To provide optimum sealing, resin-modified glass ionomer cement (RMGIC), flowable resin composite (FC), and SARC are usually applied as an intermediate material over calcium-silicates using the sandwich technique instead of direct application of the definitive restoration. 14 RMGICs combine the properties of conventional glass ionomer cements and resin composites. Their setting mechanism is initiated with an acid–base reaction and continues with photoinitiated polymerization. These materials can also chemically adhere to dental tissues and provide fluoride release, as do conventional glass ionomer cements. In contrast, resin composites are continually being developed with various properties and in various forms. 15 Resin composites are classified as packable and flowable according to their viscosity; briefly, flowable resin composites are conventional resin composites with a reduced filler loading in a volume of 37%–53% compared with packable resin composites. 16 SARC (Vertise flow; Kerr, Orange, CA, USA) does not require an adhesive application protocol owing to the functional monomers in its composition. Therefore, they involve fewer application steps, reduced chair time, and a minimum risk of handling mistakes. 17 SARCs can be used for the restoration of small occlusal cavities or noncarious cervical lesions; alternatively, they can be used as a liner under definitive restorative material. 18 As a result of their favorable properties, SARCs can also be used as intermediate materials in VPT.
Some previous studies have investigated the bond strength of resin composites and various restorative materials to calcium-silicate-based cements, but there is a scarcity of studies evaluating the bonding quality of FC and SARCs to calcium-silicates—namely, MTA and Biodentine. It is important to develop knowledge on which material or adhesive strategy provides a better bond as an intermediate material between definitive restoration and calcium-silicate-based materials for the improvement of the VPT prognosis. Therefore, the aim of this in vitro investigation was to evaluate the μSBS of two calcium-silicates to intermediate materials with different adhesive strategies. The tested null hypotheses were as follows: (a) There is no difference between μSBS of calcium-silicates and intermediate materials and (b) μSBS value is not influenced by acid-etching.
Methods
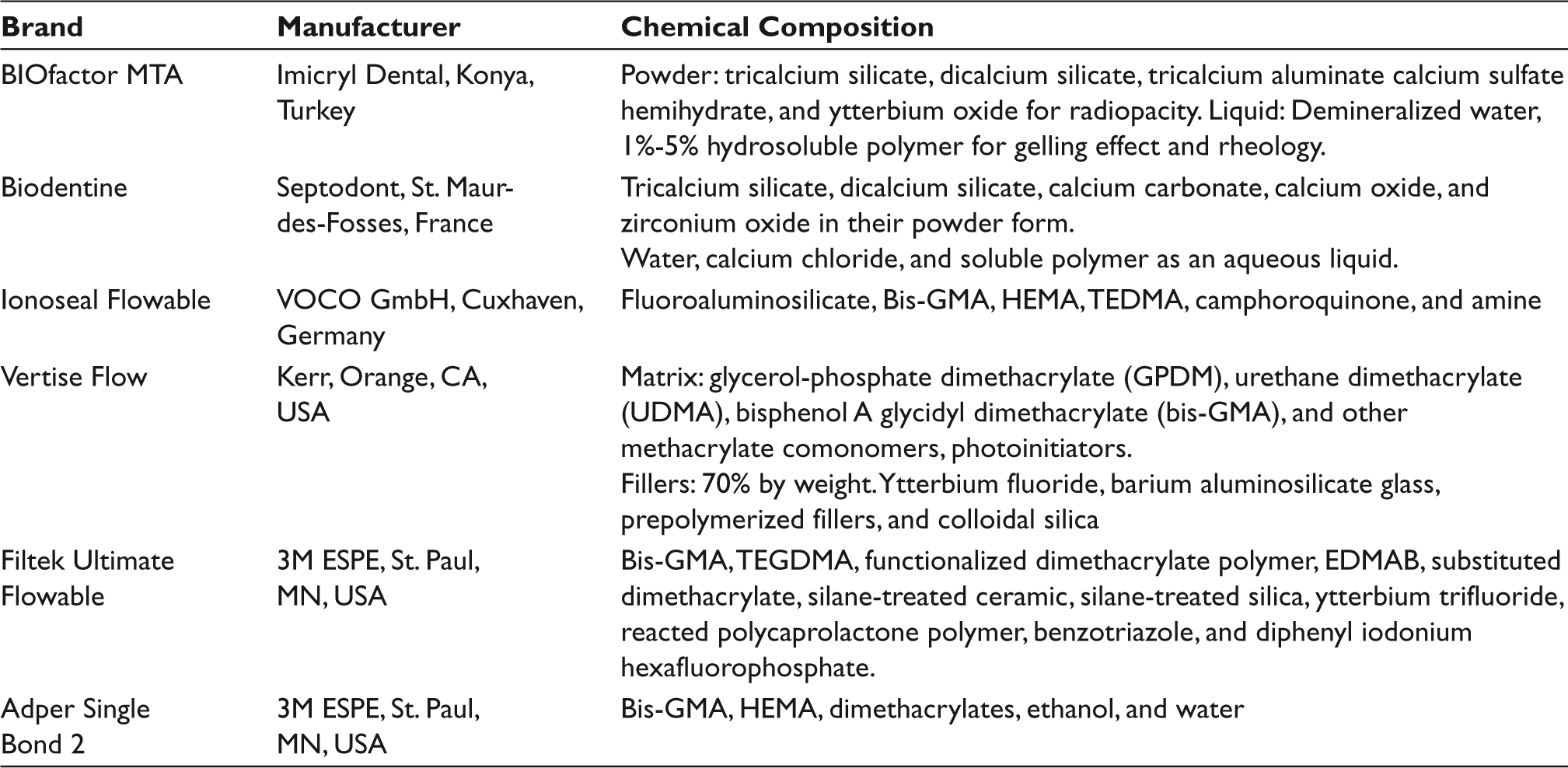
Three different types of material—namely, a SARC (Vertise flow; Kerr, Orange, CA, USA), a conventional FC (Filtek Ultimate Flowable; 3M ESPE, St. Paul, MN, USA), and a flowable RMGIC (Ionoseal; VOCO GmbH, Cuxhaven, Germany)—were tested as intermediate materials. In addition, two calcium-silicate-based materials were used—BIOfactor MTA (Imicryl Dental, Konya, Turkey) and Biodentine (Septodont, St. Maur-des-Fosses, France). Information about the manufacturer and chemical composition of the tested materials is presented in Table 1.19–26
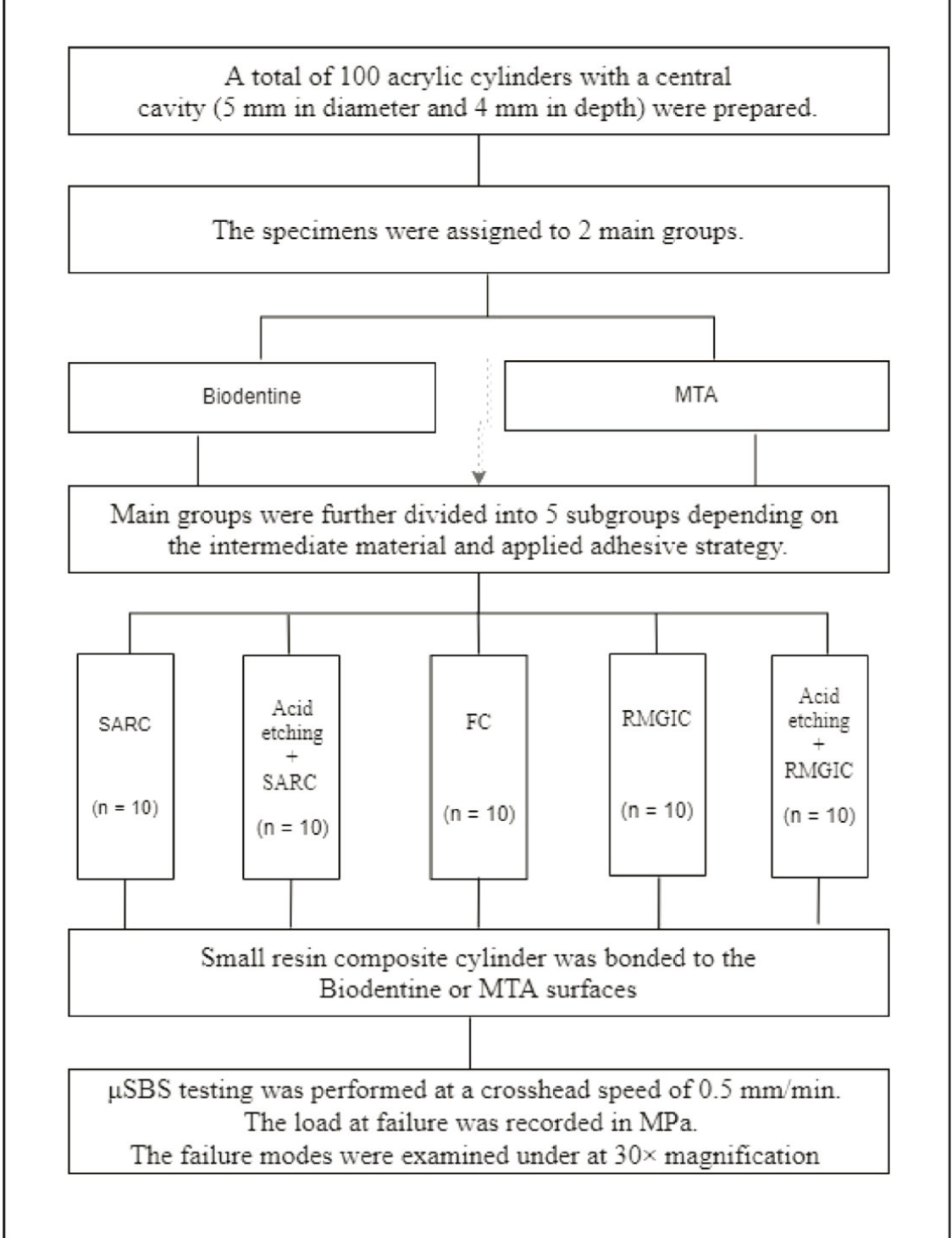
Study groups are listed in Figure 1 in relation to the materials.
Preparation of Specimens
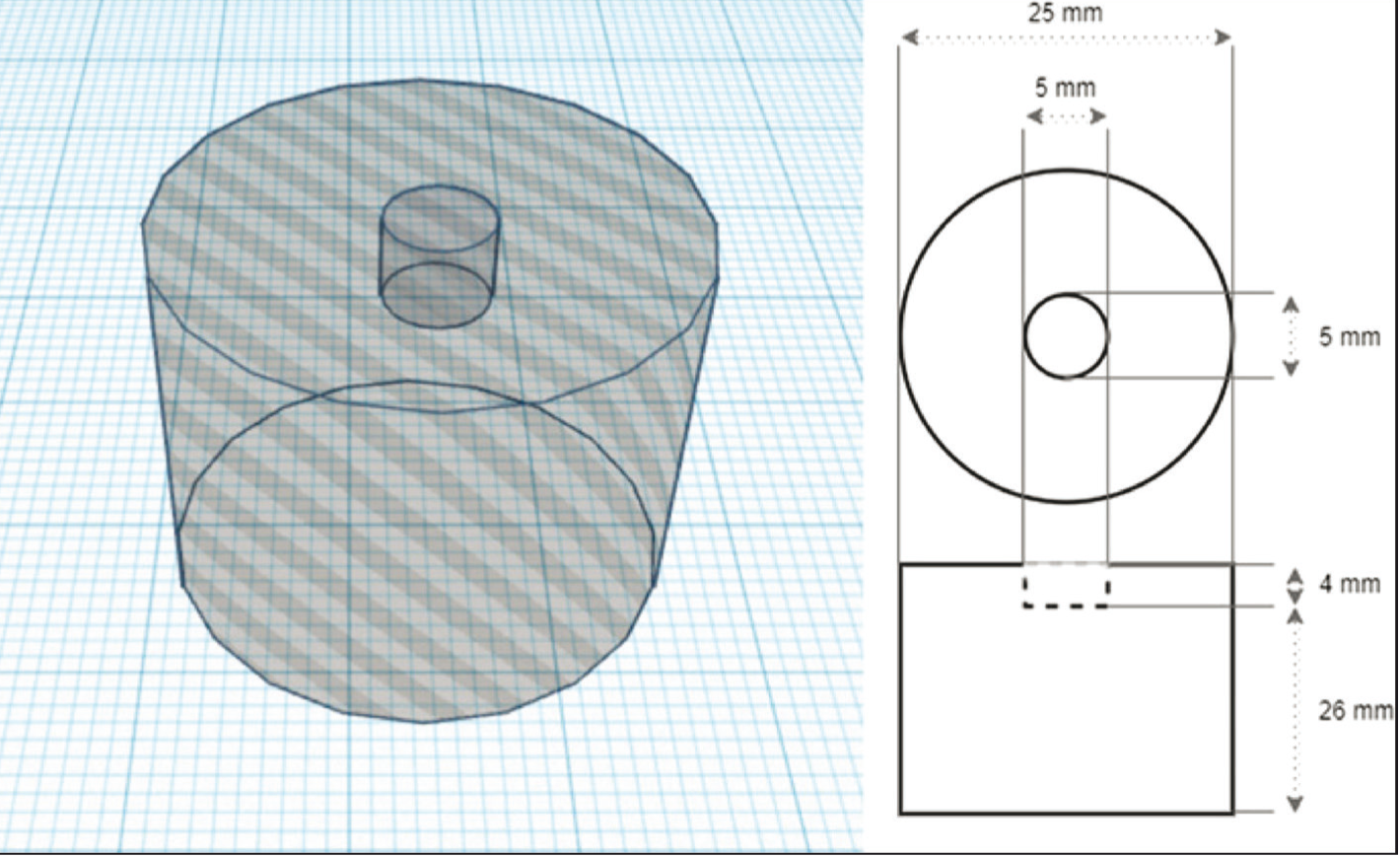
A total of 100 cylindrical acrylic molds (Imicryl Dental, Konya, Turkey) with a central hole (5 mm in diameter and 4 mm in depth) were fabricated (Figure 2). Biodentine and BIOfactor MTA were prepared in accordance with the manufacturer’s instructions and placed into the central holes on the molds (n = 50). Specimen surfaces were covered with wet cotton pellets and they were stored at 37 °C in 100% relative humidity for 72 h to ensure complete setting. 1 The specimen surfaces were wet-polished with 600-, 800-, and 1000-grit silicon carbide papers at room temperature using minimum hand pressure and under water cooling to provide smooth surfaces.27, 28 The polished specimens were rinsed gently with distilled water and then air-dried.
A small transparent polyvinyl tube (D&N, Orlab, Istanbul, Turkey) with an inner diameter of 1 mm and a height of 0.5 mm was used to prepare resin microtubules. The microtubules were carefully cut from the polyvinyl tube with an aid of a gauge to provide parallel ends. The specimens were divided into five subgroups according to the intermediate material application protocol. Each specimen surface received one resin microtubule (n = 10, in each subgroup; Figure 1).
Preparation of Cylindrical Acrylic Mold
SARC: The SARC was applied on a flat specimen surface without conditioning using microtubules. After application, the SARC was light-cured using an LED curing unit (Valo Grand; 1000 mW/cm 2 , Ultradent, South Jordan, UT, USA) according to the manufacturer’s recommendations. The light intensity of the curing unit was checked with a radiometer periodically (Hilux Radiometer, Curing Radiometer, Benlioğlu Dental, Ankara, Turkey). The light was positioned parallel and as close as possible to the material surface during the polymerization. The application tip of the light device was centered over the sample being cured. Specimens were polymerized by using an LED unit with an output irradiance of 1200 mW/cm 2 .
Acid-etching + SARC: The specimen surfaces were etched with 37% phosphoric acid (Scotchbond Etchant; 3M ESPE, St. Paul, MN, USA) for 20 s, rinsed thoroughly with distilled water for 15 s, and gently air-dried for 5 s. Then, the SARC was applied to the specimen surface as previously described.
FC: After acid-etching with 37% phosphoric acid for 20 s, a two-step, total-etch adhesive (Adper Single Bond 2; 3M ESPE, St. Paul, MN, USA) was applied using a microbrush for 20 s, followed by gentle air-drying for 5 s. The adhesive was light-cured for 10 s. Following the adhesive application, FC was gently placed into the microtubule and was photopolymerized using the same LED curing unit as described before.
RMGIC: The RMGIC was applied on a flat specimen surface without surface treatment. Each microtubule was adjusted over the substrate surface, and RMGIC was gently injected into the microtube. RMGIC was light-cured using the same LED curing unit for 20 s according to the manufacturer’s recommendations.
Acid-etching + RMGIC: The specimen surfaces were etched with 37% phosphoric acid for 20 s, rinsed thoroughly with distilled water for 15 s, followed by gentle air-drying for 5 s. Then, RMGIC was applied on the specimen surface as previously described.
Microshear Bond Strength Testing
After the sample was stored for 24 h at 100% humidity, the polyvinyl microtubule around the resin was gently removed using a sharp scalpel. A shear force was applied to the adhesive interface at a crosshead speed of 0.5 mm/min using a μSBS testing device (Esetron Smart Robotechnologies, Ankara, Turkey). The failure load was recorded in MPa by dividing the failure load (N) by the area of the adhesive interface (mm 2 ). The failure modes were examined under a stereomicroscope with magnification, and they were categorized as follows: adhesive (A; failure at the repair-substrate-bonded interfaces), cohesive (C; failure at least parts of the substrate or the repair composite), or mixed (M; A + C). 17
Statistical Analysis
The μSBS data were analyzed using two-way ANOVA to determine the effects of calcium-silicate-based cement and different intermediate material applications, and the interaction of these factors on µSBS values. According to the Kolmogorov–Smirnov (P = .30) and Shapiro–Wilk (P = .18) tests, data were normally distributed, and therefore, parametric tests were performed. Pairwise analyzes were performed using Tukey HSD test. Data were analyzed using GraphPad Prism (GraphPad Software, Inc., San Diego, CA, USA) statistical software. The level of significance was set at 0.05.
Results
The μSBS (MPa ± SD) values of different intermediate materials to calcium-silicate-based VPT materials are presented in Table 2. It was observed that both calcium-silicate-based material type and intermediate material type influenced the μSBS significantly according to two-way ANOVA. However, no statistically significant interaction was demonstrated between these factors (P = .396).
Conditioning both Biodentine and MTA surfaces with acid-etching prior to intermediate material application increased the bond strength values considerably. Statistically significant benefit was found only between SARC and Acid etch + SARC for BIOfactor MTA (P > .05). According to the bond strength data of this study, Biodentine exhibited higher bond strength values than MTA. This difference in favor of Biodentine was found to be statistically insignificant for FC and SARC applications to the acid-etched surface (P > .05). The highest μSBS values were observed for SARC bonded to acid-etched Biodentine (11.2 MPa), whereas the lowest μSBS values were observed for RMGIC bonded to BIOfactor MTA (4.1 MPa). Although RMGIC performed better bond strength values to the acid-etched surfaces, the increase in bond strength was not observed at a significant level (P > .05). The μSBS values of intermediate materials to Biodentine and MTA were listed from the lowest to the highest as follows: RMGIC < Acid Etch + RMGIC < SARC < FC < Acid Etch + SARC (Table 2).
Microshear Bond Strength (MPa ± SD) Values and the Failure Distribution
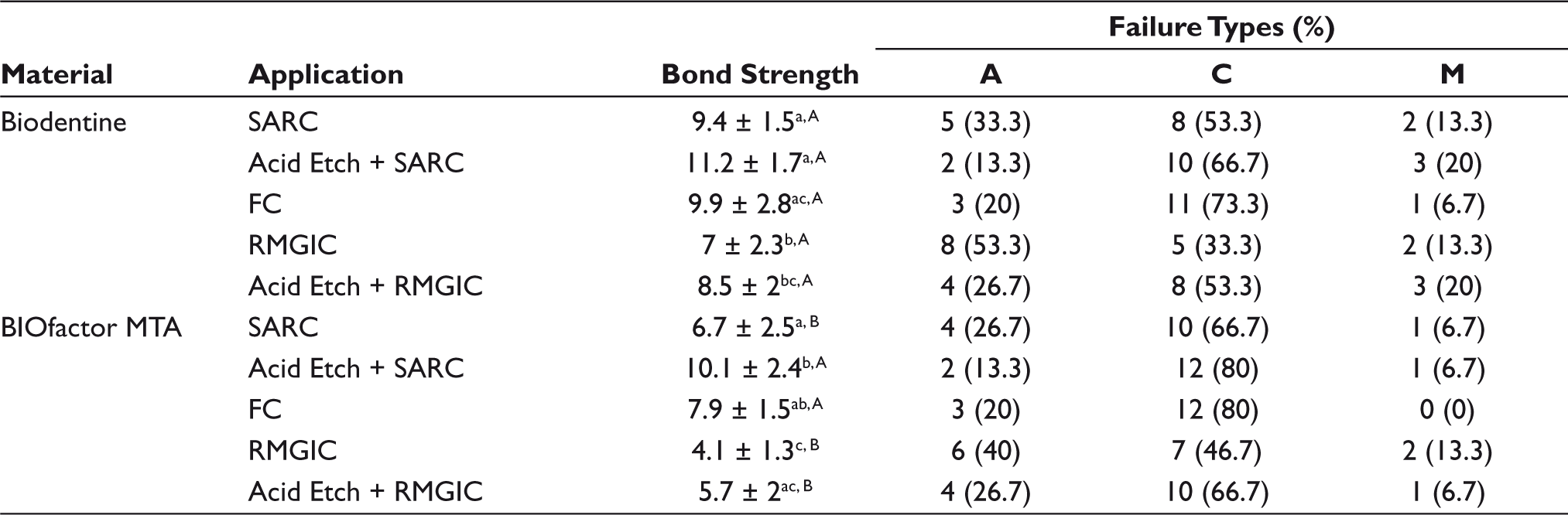
The failure mode distributions resulting from the μSBS test are shown in Table 2. No pretest failure was observed for all groups. There was no cohesive failure within the intermediate materials. For the calcium-based materials, the predominant failure mode was cohesive type, especially in FC and Acid etch + SARC. Cohesive failures markedly increased in groups where calcium-silicate surfaces are acid etched. The mixed failure mode was the least common failure mode among all groups. A slight increase in cohesive failure mode was noted for MTA compared to Biodentine.
Discussion
VPT is indicated for teeth with reversible pulpitis caused by caries progression, mechanical pulp exposure during caries removal, or dental trauma.4, 27 The main objective of pulp capping, which is one of the most frequently used VPTs, is to preserve the vitality of the pulp. To achieve this goal, many pulp-capping materials have been introduced thus far. 28 MTA and Biodentine, known for various indications, such as indirect and direct pulp capping, perforation repair, treatment of internal root resorption, furcation repair, apical plug procedures, and pulpotomy, are the most popular of these materials considering their bioactivity, biocompatibility, and ability to repair hard tissues. 1 Apart from these properties, the bond strength of pulp-capping medicaments to the restorative materials is highly important because the sealing of the restoration plays a crucial role in the VPT’s success. 29
Placing an intermediate material over a calcium-silicate-based material in deep cavities reduces polymerization shrinkage and prevents microleakage.30, 31 A stable bonding between the pulp-capping medicament and the intermediate material provides a high adhesive strength, which evenly distributes stress on the lining–filling interface and plays a crucial role in the restoration’s integrity.32, 33 Various intermediate materials can be applied to calcium-silicate-based materials to provide hermetic sealing and to ensure durable restorations.
This study aimed to evaluate the μSBS of MTA (BIOfactor MTA) and Biodentine to SARC, FC, and RMGIC used as intermediate materials. The first null hypothesis, that “no difference would be detected between μSBS of calcium-silicates to intermediate materials,” was partially rejected because not all the groups showed statistically significant differences. The second null hypothesis, that “μSBS value would not be influenced by acid-etching,” was also partially rejected because the difference was found between only SARC and Acid etch + SARC.
Different bond strength values can be observed between the calcium-silicate-based materials and the intermediate materials used with them. There are studies in the literature with different results regarding the μSBS of FC to Biodentine and MTA.1, 34–36 Although the μSBS values for Biodentine were higher than those for MTA according to this study’s results, there was no statistically significant difference in the μSBS of FC and acid-etched SARC to BIOfactor MTA. In a study that aimed to evaluate the SBS of a SARC and FC to MTA, Biodentine, and a calcium-enriched mixture (CEM), researchers found that the SBS values for MTA were higher than those for Biodentine, and the difference between these materials was statistically insignificant. 1 Similarly, in another study that compared the SBS values of resin composite, compomer, and RMGIC to Biodentine and MTA, it was reported that the SBS values when using MTA with compomer and composite restorations were better than the values for restorations using Biodentine. 34 On the contrary, other studies have reported higher SBS values for Biodentine than for MTA.35, 36
In this study, Biodentine had the highest μSBS values in all adhesive strategies. The differences in μSBS were attributed values to the different characteristics of the materials and acid-etching applications. Because of the absence of resin monomers in MTA and Biodentine, these pulp-capping materials bond to the intermediate material solely micromechanically. 37 In the acid-etching groups, phosphoric acid created deeper and more retentive microporosities and provided higher μSBS values.
μSBS values may be affected by the setting time of the material. MTA has a slow setting time and is considered to be unstable when the tooth is restored before the calcium-silicate-based material’s complete setting. 38 It was suggested that 72 h is needed after mixing to allow the material to accomplish its optimum sealing ability.39, 40 According to the product manual, Biodentine has an initial setting time of 12 min. However, several studies suggested that the optimum strength of Biodentine was achieved approximately two weeks later.41, 42 In a study in which the shear bond strength (SBS) of different restorative materials to MTA and Biodentine was investigated, the specimens were stored for 72 h after the placement of calcium-silicate-based material. 24 Similarly, in a study that represented the effect of intracoronal bleaching agents on μSBS of MTA cements to resin composite, MTA cements were stored for 72 h to ensure complete setting. 33 Because there is no definite consensus, it was thought that this specified time interval was sufficient for complete setting and necessary for standardization. Thus, MTA and Biodentine were kept at 37°C and 100% relative humidity for 72 h to provide ideal hardening in this study.
The chemical hardening mechanisms and acid-etching applications of the materials also affected SBS. The RMGIC demonstrated lower SBS values in both the Biodentine and the MTA groups in this study. These results are similar to those reported by Tulumbaci et al. and Ajami et al.34, 37 The lower bond strength can be associated mostly with the chemical bonding between the RMGIC and the tested pulp-capping agents because micromechanical retention has a negligible effect on those groups. 34 This result is also supported by the type of failure in Biodentine to RMGIC, which is mostly adhesive. Furthermore, it should be noted that cohesive failure is the most common type of failure in all acid-etching groups of SARC and RMGIC compared to those without acid-etching. This implies that the bond strength between RMGIC and pulp-capping agents becomes higher than the substrates’ cohesive strengths when specimen surfaces are etched with 37% phosphoric acid.
The application method and the materials’ characteristics may also affect SBS values. In a study aimed to evaluate the SBS of SARC and bulk-fill flowable composites to MTA Plus, Dycal, Biodentine, and TheraCal LC, the researchers found statistically significant differences among materials. 44 Biodentine’s SBS was higher than that of MTA, which is consistent with our study’s findings. In that same study, the researchers specified that, compared to MTA, Biodentine’s smaller particle size might increase its micromechanical bonding, resulting in higher SBS values. Additionally, the researchers suggested that the presence of calcium chloride in Biodentine increased its bond strength because of calcium chloride’s resistance to removal. Additionally, pH levels may affect SBS values. It was stated that the pH results were independent of the mixing method used and revealed an alkaline pH in a study indicating that alkaline pH and calcium ion release are properties of tricalcium-silicate-based materials related to biological activity and repair induction. 45 Studies have shown that the microhardness and compressive strength values of tricalcium silicate materials are significantly higher in a neutral or alkaline pH environment compared to those in acidic conditions. An acidic environment may lead to more porous structural changes in these materials, and this may adversely affect the repair capacity of the calcium-silicate materials in vital pulp treatments.26, 46–48
In this study, a conventional flowable composite (Filtek Ultimate Flowable, 3M ESPE, St. Paul, MN, USA), a SARC material (Vertise Flow [VF], Kerr, Orange, CA, USA), and an RMGIC material (Ionoseal Flowable, VOCO GmbH, Cuxhaven, Germany) were used as intermediate materials. According to the manufacturer’s recommendations, VF-SARC material does not require any adhesive application. However, research has demonstrated that etching and rinsing can improve VF’s adhesion to tricalcium silicate-based cements. 49 In a recent study investigating the effectiveness of SARC and various surface treatments for aged nanofilled resin composites with microtensile bond strength, researchers reported that VF can be used in the repair of old nanofilled composites. Furthermore, they concluded that the acid-etching procedure can be applied for a better repair ability in clinical practice. 50 In this study, the bond strength is tried to be increased by making surface modifications with reference to other studies.51, 52 There are also newly introduced self-adhesive bulkfill composites that can eliminate the need for an intermediate material and can be used as a one-piece restoration alternative.53, 54
In another recent study, researchers found that acid etching significantly increased SARC bond strength at different time intervals, whereas using a self-etch adhesive decreased it. 49 Although the RMGIC used in this study did not require acid etching according to the manufacturer’s recommendations, acid etching was applied to one of the RMGIC groups, which resulted in increased μSBS values. This was an important finding because no previous studies in the literature have used this methodology to improve the bond strength of intermediate materials to calcium-silicate-based materials.
The limitations of this in vitro study are that it was not performed with dentin tissue and the artificial aging procedure. Despite the clinical conditions providing proximity to the dentin tissue with the materials used, it was not performed such as mentioned in this study to standardize the bond strength of the resin composite and MTA. Further studies on dentin involving the aging process are needed.
Conclusion
Within the limitations of this study, the highest μSBS values were found in Biodentine to acid-etched SARC. It can be concluded that acid-etching increased the μSBS values in both SARC and RMGIC groups. Even though there were numerical differences between μSBS values, no statistically significant difference was found between μSBS of intermediate materials to calcium-silicate materials. Self-adhering composites can be applied over the calcium-silicate-based materials in VPTs because of their mechanical properties.
Footnotes
Authors’ Contribution
Data Availability Statement
The publication contains all of the data supporting the current study. There is no extra information available.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.