Abstract
Aim:
The present trend in health care is toward the use of natural products for curing diseases. “Propolis” or bees wax is a natural, nontoxic resinous material collected by bees from exudates and buds of the plant. It has many beneficial biological and pharmacological properties such as antimicrobial, anti-inflammatory, antifungal, antiviral, and anticancer activities. Propolis is widely applied in dentistry as an anticariogenic agent, hypersensitivity reducing agent, and endodontic disinfection to name a few. The diverse phytochemical constituents of propolis are responsible for its valuable properties. Considering its vast potential, propolis has gained the attention of many researchers. The aim of this study is to offer a comprehensive evidence which will enable the readers and researchers to appreciate the prospects of the application of Indian propolis in present-day dentistry.
Material and Methods:
In vitro and in vivo studies on Indian propolis and its application in dentistry searches were performed in PubMed, Scopus, and Cochrane library databases up to December 2020.
Results:
The search identified 31 records; 12 full-text articles which met the eligibility criteria were assessed. Based on the results of in vitro studies, further in vivo studies need to be carried out to prove the feasibility of Indian propolis as an anticariogenic agent, a desensitizing agent, and an intracanal irrigant/medicament in the field of dentistry.
Conclusion:
Indian propolis has shown an immense amount of potentiality which demands for more clinical research to have sufficient evidence-based literature for future usage in oral health care.
Introduction
Numerous medicaments have been incorporated from holistic remedies into contemporary medicine. One such medicament that is becoming popular globally in recent times is propolis: a common ingredient used in apitherapy, i.e., agents derived from bees or bee products. 1
Originating from Greek, pro meaning “in front of” or “at the entrance of,” and polis meaning “city” or “community,” propolis means hive defense substance. 1 In this manner, propolis serves as a means for colonies to maintain the homeostasis of the hive via inhibitory effects on the microorganism, preventing their growth on the walls, averting the uncontrolled airflow into the nest, waterproofing of the hive against moisture, and providing security against external invaders. Therefore, propolis in simple terms means defense of the hive. 2 Propolis (bee glue) is a brownish, sticky, resinous substance that is produced by honey bees from various plant sources such as leaves, flowers, and bud exudates, modified by the addition of bee secretions and wax. 3
A broad analysis reveals approximately 50% resinous compounds and balsam, 30% beeswax, 10% ethereal and aromatic oils, 5% bee pollen, and 5% numerous other organic and inorganic compounds. 3 The chemical composition of propolis includes aromatic acids, flavonoids, esters, ketones, aldehydes, fatty acids, steroids, terpenes, amino acids, alcohols, polysaccharides, hydrocarbon, hydroxy benzene, and several other compounds in trace amounts.3,4
However, the chemical composition may vary according to the source, regional vegetation, climatic condition, bee species, and the season in which it is collected. 2 Propolis samples collected from the temperate region contain flavonoids, chrysin, pinocembrin, cinnamic acid, ferulic acid, and caffeic acid, whereas those collected from the tropical areas are rich in prenylated derivatives of benzophenones, lignans, p-coumaric acid, and diterpenes. 5 Hence, the standardization of propolis is difficult considering the constitutive difficulties associated with the analysis of complex mixtures from different vegetal sources. 2
Current researchers are trying to incorporate the properties of propolis into various fields of contemporary medicine and dentistry. Man, since ancient times, has used propolis for its extensive array of biological properties such as its antimicrobial, antioxidant, and anticancerous properties. 6
In dentistry, propolis can be used as lozenges, topical creams, mouth rinses, and toothpastes. It has shown antiplaque, cariostatic effect, dentinal hypersentitivity reduction, improvement of periodontal health, and in minimal invasive dentistry. 6 Many researchers have studied the biochemical and phytochemical constituents of propolis from all around the world, including Brazil, Turkey, Iraq, Mexico, Egypt, Iran, Ethiopia, China, and Bulgaria. Compared to its global counterparts, Indian propolis has been less studied and researched. 7
Beekeeping is a dateless tradition and practice in India. India ranks 1st and 7thglobally in beeswax and honey production, respectively. 8 In spite of India having such high rankings, research on propolis is almost neglected owing to the lack of awareness about its quality, therapeutic levels, and market potential. 9
India is one of the biggest countries in terms of cultural and environmental biodiversity, inhabiting large number of flora and fauna. Conditions and the various climate and seasonal variation mostly impact the chemical composition and biological activity of propolis. In the Indian context, the literature offered concerning the utilization of Indian propolis is restricted and solely a few Indian analysis clusters have worked on their biological activity and chemical composition. 10
Ramnath et al 10 identified 93 compounds by gas chromotography mass spectrometry in six Indian propolis collected from various regions of India (Karnal from Haryana State, Hamirpur from Himachal Pradesh, Sarangpur from Uttaranchal, Palladam from Tamil Nadu, Hubli from Karnataka, and Sultanbatteri from Kerala). The major components were carboxylic acid (20.4%), terpenoids (15.0%), steroids (11.5%), hydrocarbons (9.6%), sugars (6.4%), alkaloids (6.4%), flavonoids (4.3%), phenols (3.2%), ketones (2.1%), amino acid (2.1%), vitamins (2.1%), and other compounds (15.0%).
The studies have shown that antibacterial activity of propolis is evidenced in two levels. First, it acts directly on the microorganisms, and the other with stimulation of the immune system which results in activation of natural defenses of the organism. Propolis effects on the permeability of the cellular membrane by disrupting the membrane potential and affecting the production of adenosine triphosphate by decreasing the bacterial mobility of microorganisms. 11
The study on Indian propolis has just started. Only a handful of studies have been reported on the chemical constituent of Indian propolis and its medicinal attributes, such as the antimicrobial, anti-inflammatory, antioxidant, antiatherosclerotic, anticancer, antiplatelet, and pro-oral health activities. 12 Even though propolis, specifically Indian propolis, may have a great potential against oral pathogens, data for this is still scarce. The aim of this study is to offer comprehensive evidence which will enable the readers and researchers to appreciate the prospects of the application of propolis in present-day dentistry. The present review focuses on the potential applications of Indian propolis in dentistry.
Materials and Methods
In order to conduct a review, the following electronic databases: PubMed, Scopus, and Cochran library were used to find published articles on Indian propolis since the inception of database till December 2020. Only studies written in English were included. The databases were searched using keywords and medical subject headings (MeSH) terms in titles as follows: (“Indian propolis” AND “phytoconstituents,” “Indian propolis” AND “antimicrobial activity,” “Indian propolis” AND “application in dentistry,” “oral pathogens” AND “Indian propolis,” “in vitro” OR “in vivo” studies on Indian propolis, etc. Original full-text articles were reviewed and articles published in other languages, abstracts, conference proceedings, review articles, and animal studies were excluded. No authors were contacted for articles.
Results
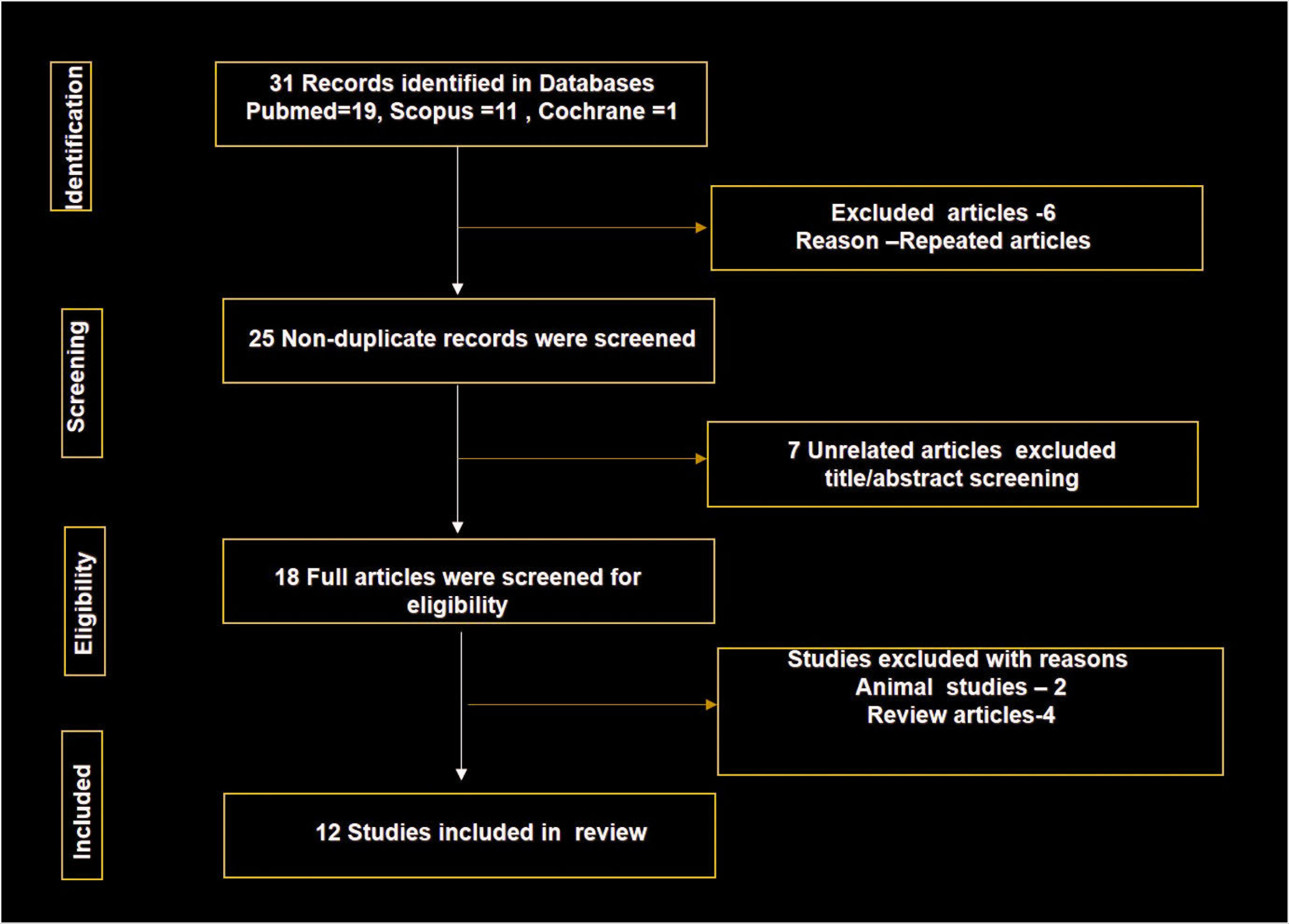
After the search using appropriate keywords and MeSH terms, a total of 31 articles were obtained from online databases. After duplicate removal, 25 articles were screened, and then, seven articles were excluded after title/abstract screening as propolis was not procured from India and not related to application in dentistry. Eighteen full-text articles were further screened, animal studies and review articles were excluded based on the eligibility criteria. Finally, 12 articles, five in vitro and seven in vivo studies on Indian propolis were available for assessment. Figure 1 shows the flow diagram of a number of studies identified screened assessed for eligibility. Table 1 represents the in vitro studies demonstrating the uses of Indian propolis in dentistry.
In Vitro Studies Demonstrating the Uses of Indian Propolis in Dentistry

Discussion
Applications of Indian Propolis in Dentistry
Propolis has shown a lot of potential in the form of numerous applications in the field of dentistry. Propolis possess antimicrobial characteristics against oral diseases; because of its strong anti-infective activity, propolis has often been referred to as a “natural antibiotic.” Below are a few aspects that prove the same and that are based on studies conducted by various researchers specifically on Indian propolis.
Propolis as a Desensitizing Agent
Dentin hypersensitivity (DH) can be defined as a sharp, sudden, short pain arising from thermal, tactile, osmotic, or other stimuli from exposed dentin. Flavonoids, a component of propolis, is one of the main active and reactive agents capable of stimulating reparative dentin formation. This is one of the main factors that enables propolis to reduce dentin permeability efficiently.
Torwane et al. 13 conducted randomized, double blind, split mouth, controlled clinical trial to evaluate the effect 30% ethanolic extract of Indian propolis and Recaldent (casein phosphopeptide-amorphous calcium phosphate) on reduction of DH. Thirteen patients having at least three teeth with DH were divided randomly into three groups and allotted for 30% ethanolic extract of Indian propolis, Recaldent, or sterile water.
Verbal rating scale was used to determine the hypersensitivity predicted by air blast and tactile stimuli. The study was conducted for 21 days and concluded that both Indian propolis and Recaldent showed significant reduction in the DH. Recaldent was a superior agent in the reduction of DH as compared to propolis and sterile water. 13
Purra et al. 14 carried out a study to assess the efficacy of saturated ethanolic solution of propolis in comparison with 5% potassium nitrate and distilled water for the DH treatment. This was a three-month, randomized, double blind study on 10 patients aged between 20 and 40 years. Patients were evaluated at intervals of 1 week, 2 weeks, and 4 weeks after the application of the agent. The final re-evaluation was done post three months from the first application. Propolis group and the potassium nitrate group showed no significant difference in the immediate posttreatment period. However, the results were significant at the end of the first and the second weeks. At four weeks and three months period, groups did not show any significant difference, and authors concluded that propolis was more effective than 5% potassium nitrate in reducing DH and produced an immediate and sustained effect.
Propolis as Mouthwash
Mouthwashes are antiseptics and can be used as a home remedy to improve oral hygiene. Therapeutic mouthwashes reduce bacterial counts, produce antiplaque effects, have an astringent effect, and help in reducing gingivitis and caries.
A study conducted by Dodwad et al. 15 aimed to test the effectiveness of a propolis-containing mouth rinse in plaque formation inhibition and gingival health improvement. Study was single blind three-group parallel study of five-day de novo plaque formation. Three groups of 10 subjects each either received a propolis-containing mouth rinse, or a negative control (saline) or a positive control (chlorhexidine 0.2%). The evaluation of plaque and Gingival index at baseline and at a five-day interval was carried out. Chlorhexidine mouthwash was concluded to be a better agent than propolis and saline in inhibiting plaque formation. Gingival scores obtained using propolis were only marginally better than those obtained by chlorhexidine. The study concluded that propolis can be used as a natural alternative to chemical mouthwash. Moreover, long-term trials are necessary and required for more accurate data and conclusive evidences. 15
Propolis as an Anticariogenic Agent
Dental caries is one of the biggest public health issues among the world population. There are many methods to prevent the occurrence of caries, ranging from brushing techniques to diet to mouthwashes to fluoride applications. Chewing sugar-free gum has shown potentiality in benefitting the oral health.
Tulsani et al., 16 did a study with the aim of evaluating and comparing the anticariogenic action of two commercial chewing gums, propolis and xylitol, on the salivary S. mutans count in a group of children. Two groups of children were given xylitol and propolis chewing gums, respectively. Saliva was tested just after spitting and post 1 hour. The result showed that there was a substantial decrease in the number of colonies in children who used propolis gum when compared to xylitol. However, xylitol gum was more preferred by children. The author suggested propolis chewing gum can be employed as an anticariogenic agent in children. 16
Propolis as a Cavity Disinfectant and in Minimally Invasive Dentistry
Restorative dentistry was conventionally based on the concept that the infected dentin must and should be treated by operative intervention. However, the more recent concepts that follow the principle of minimally invasive dentistry (MID) stress upon creating an environment that results in arresting the caries progression with minimal operative intervention. The drawbacks of minimally invasive dentistry are limited accessibility and fatigue of hand and wrists, increased risk of incomplete excavation, thus permitting cariogenic bacteria to survive incarceration under adhesive restorations. Even in conventional restorative techniques, residual or secondary caries is one of the major reasons for restoration failure.
In a study done by Prabhakar et al., 17 using ethanolic extracts of naturally available Aloe vera and propolis for disinfecting the cavities before restoration, dentinal samples were collected at the stages of preexcavation, postexcavation, and postdisinfection, and were later submitted for microbiological analyzes. Cavities treated with A. vera and propolis extracts showed a substantial decrease in bacterial counts when compared to the control group. Both propolis and A. vera extracts can be used as potential natural disinfecting agents, hence backing up the concept of phytotherapy in minimum intervention dentistry. 17
Action of Propolis in Periodontal Health
Propolis has anti-inflammatory effects. The mechanism of action of propolos is by “cytokines and inflammatory mediators” modulation, such as inhibition in the production of prostaglandins, histamine, and transforming growth factor beta (TGF-β). The anti-inflammatory effect of propolis can be found by the results of the use of it on the severity of gingival and bleeding indices scores.
The study done by Sanghani et al. 18 aimed at evaluating the clinical and microbiological efficacy of Indian propolis extract that is delivered sublingually as an adjunct to scaling and root planning (SRP) in the treatment of periodontitis. Control sites were treated with SRP alone and test sites with SRP and propolis. The sites were clinically assessed and microbiologically assessed for periodontal pathogens. There was a substantial improvement in the clinical and microbiological parameters in the test sites when compared to the control sites.
The author concluded that subgingival delivery of propolis has a huge potential to be used as an adjunct to SRP in patients with chronic periodontitis when assessed by clinical and microbiological parameters. 18
Propolis as a Root Canal Filling Material in Primary Teeth
Pulp therapy is a routine procedure performed in children to treat pulpal and periapical lesions. The success of this treatment depends mainly on effective instrumentation and obturation. Thus, it is very important to select the right obturating material for better prognosis. Zinc oxide eugenol (ZOE) has always been the go-to material for obturating in children, but it does have its limitations in the form of irritation and limited antimicrobial activity.
Roja Ramya et al. 19 conducted an in vivo study to compare the effectiveness of zinc oxide- propolis mixture and ZOE as a root filling material in nonvital primary molars. Children aged 4 to 8 years who required pulpectomy treatment in primary molars were randomly allocated into two groups: control group (zinc oxide-propolis mixture) and ZOE (control group). All the pulpectomy treated teeth were restored with stainless steel crowns, and followed up at 6, 12, and 24 months for postoperative clinical and radiographic evaluation.
The results showed success rates of pulpectomy with zinc oxide-propolis mixture to be at 95% and ZOE at 70%. Zinc oxide-propolis mixture showed a 90 to 70 cm success rate of 100% at 6 months and 95% at 12- and 24-months follow-up, whereas ZOE showed 80% success rate at 6 and 12 months, and it reduced to 70% at 24-month follow-up. Zinc oxide-propolis mixture was more effective and showed better results clinically and radiographically. 19
Limitation of the Review
Direct comparison of the studies was not possible because of the presence of very limited data on Indian propolis and its application in dentistry.
Conclusion
In this review, various in vivo and in vitro studies carried out on Indian propolis have been enumerated and elaborated upon. Based on the results of in vitro studies further in vivo studies need to be carried out to prove the potential application of propolis in the field of dentistry. In vivo studies which have been conducted so far have shown that Indian propolis can be used as a desensitizing agent, mouthwash, chewing gum with anticariogenic effect, local drug delivery for chronic periodontal disease, and a varnish for dentine hypersensitivity. With this limited data, Indian propolis has shown an immense amount of potentiality and demands for more clinical research to have sufficient evidence-based literature for future usage in oral health care.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
