Abstract
The coronavirus disease (COVID-19) has spread globally. Dentists, dental specialists, dental assistants, dental staff, and patients are potentially at higher risk of COVID-19 infection during dental treatments. The prosthodontic dental treatment procedures may range from low to very high risk of COVID-19. This article presents necessary recommendations regarding the prosthodontic dental treatment procedures with standards of care and infection control.
Introduction
The coronavirus disease (COVID-19) has spread globally.1,2 The symptoms of COVID-19 include fever, fatigue, dry cough, and dyspnoea. Most infected people show mild to moderate respiratory illness. People with underlying systemic diseases such as diabetes, heart diseases, and respiratory disease are at higher risk of mortality.1,3 COVID-19 has led to stress and anxiety due to the responsibility of family care, future career, and financial burden and crisis. 4 Currently, there are no specific vaccines or other therapies developed for COVID-19 until now. 1 Various clinical trials in various countries are being done along with the evaluation of potential treatments.
COVID-19 has affected dentistry and the dental practice globally. 5 It was found that a high number of dentists, i.e., 284 (70%) were affected by the financial burden and were not receiving a salary during this lockdown. 6 Patients receive dental treatments only from 10% of the dentists. Only 28 (7%) dentists think they should do the regular dental procedures, but 240 (59%) dentists believe they should do emergency dental treatments for COVID-19 infected cases.
Recommended Measures for COVID-19 Prevention in Prosthodontic Dental Practice
Currently, various measures are being taken to limit the spread of COVID-19. In prosthetic dental treatment, the following necessary precautions can be taken. The following are the standard recommendations to be implemented in prosthodontic dental practice.
Prior to Prosthetic Dental Treatment
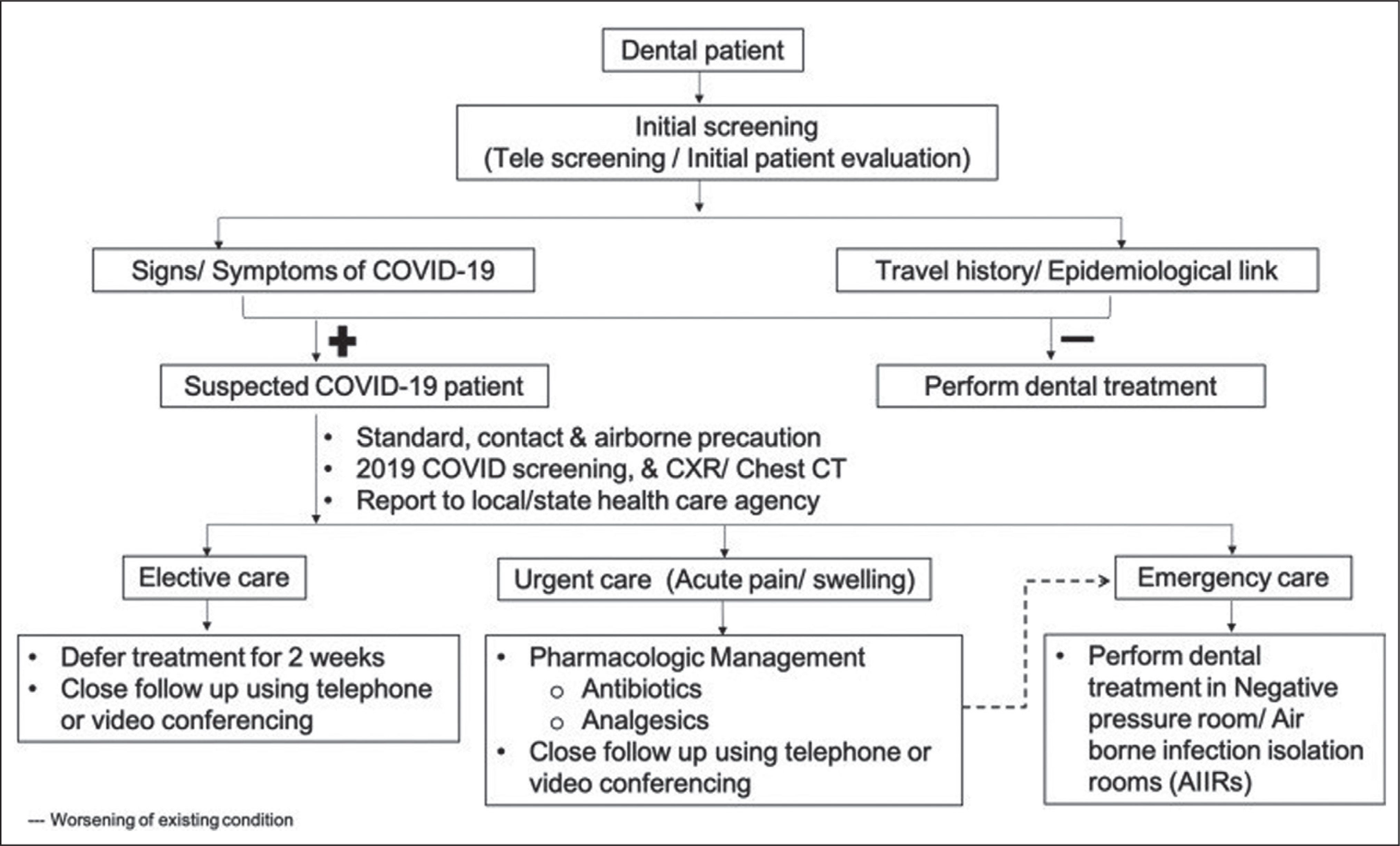
Some essential recommendations for patient appointment in the clinic; requesting the patients to arrive on time for their appointments, rather than too early to reduce the time spent on the dental treatment, scheduling appointments to minimize possible contact with other patients in the waiting room, and removing the materials from the dental clinic (magazines, newspapers, and other objects) to reduce the contamination. 7 Figure 1 shows patient screening flowchart for COVID-19 and prosthetic dental treatment. 8 A detailed medical history of the patients and their family members, including recent travel history, should be asked upon their arrival in the dental clinic. 8
The prosthetic dental treatment procedures can be divided into four categories
9
as shown in Table 1:
Emergency treatments. Urgent conditions:
Managed with minimally invasive procedures without generating aerosol Managed with invasive and/or generating aerosol Nonroutine treatments. Routine treatments.
Common Treatment Urgencies in Prosthodontic Clinical Practice
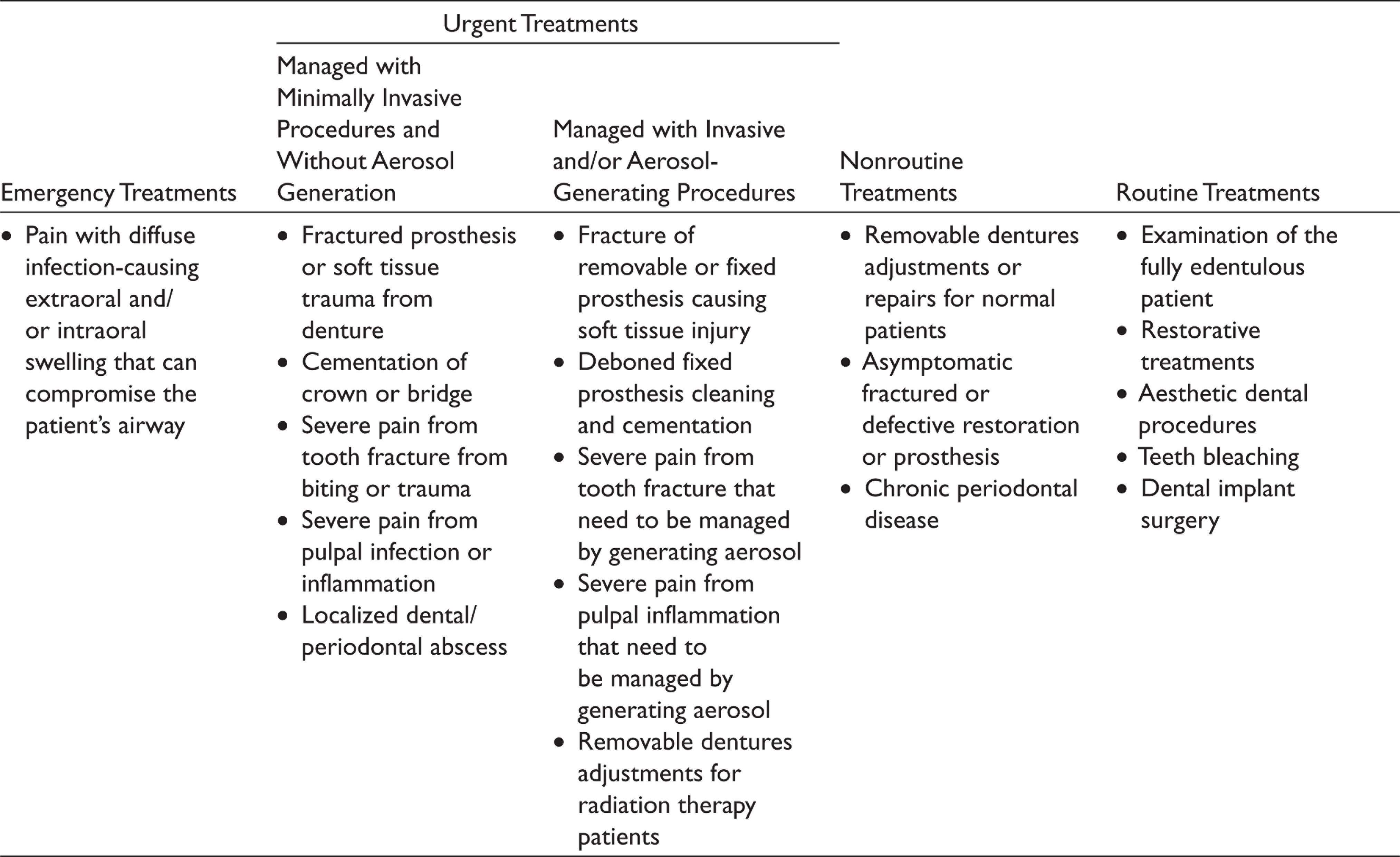
Table 1 shows the common treatment urgencies in prosthodontic clinical practice. Most often, the patient presents symptoms related to prosthetic restoration or dentures. But, usually, the patients may show symptoms of pain from endodontic, periodontic cause also. Such patients can be evaluated initially, and after provisional diagnosis, the patient can be treated by the specialty.
During Prosthetic Dental Treatment
The prosthodontist, dentists, and staffs are at a potentially higher risk of COVID-19 infection due to their close proximity to patients. Hence, proper risk assessments should be carried out of both staff and patients. During prosthetic dental treatment, important considerations should be given for approaches to aerosol-generating exposures, procedural risk mitigation, decontamination, and personal protective equipment.
10
In the prosthodontic dental clinic, the following measures can be taken to prevent the infection from COVID-19:
Whenever possible, use disposable instruments to reduce the risk of cross-infection. Postpone invasive dental treatment and avoid procedures generating aerosols whenever possible.
10
Perform extraoral radiographs and restrict the use of intraoral radiographs to minimize the salivation and gag reflex. Use mouthwash (0.23% povidone-iodine or 0.5%–1% hydrogen peroxide) for at least 15 seconds before the prosthetic dental procedure.11,12 Whenever possible, use rubber dam while doing restorative treatment on teeth (inlay, onlay, or fillings) as it significantly reduces the spread of micro-organisms.
13
Post Dental Treatment
After treatment, an important consideration should be given to the procedures to protect the patients and staff. Hands should be washed properly, and the use of hand sanitizer should be considered. 14 The appropriate follow-up should be done for the patients. It is necessary to do the risk assessments for COVID-19 for all clinic staff. All staff should be monitored if they feel unwell. 10
Finally, a multidisciplinary clinical approach, including dentistry, is needed in the treatment for this condition through a clinical practice supported by scientific knowledge. 15 Psychological intervention and mental health support are required to reduce anxiety and stress. Psychological counseling is also required to reduce anxiety and stress in severe cases.
Conclusion
Dentists, dental assistants, dental staffs, and patients are potentially higher risk of COVID-19 infection during prosthetic dental treatments. The prosthetic dental treatment procedures may range from low to very high risk for COVID-19. Hence, the prosthodontic/prosthetic dental treatment procedures should be done with standards of care and infection control following high standard guidelines and recommendations for COVID-19.
Footnotes
Clinical Recommendation
The prosthodontic treatments should be done with high standards of care and infection control following standard guidelines and recommendations for COVID-19.
Acknowledgements
The author acknowledges Walailak University International College of Dentistry for the support for this work.
Declaration of Conflicting Interests
The author declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author received no financial support for the research, authorship, and/or publication of this article.
