Abstract
Aim:
To evaluate the shear bond strength (SBS) of 3 fissure sealants used alone and with ozone and laser pretreatment.
Materials and Methods:
For the SBS test, the flattened enamel surfaces of 90 healthy third molars were randomly divided into nine groups (n = 10 for each groups), based on different sealants (BeautiSealant, Fuji Triage, and Grandio Seal) and pretreatment conditions (no pretreatment, pretreatment with ozone, and pretreatment with neodymium-doped yttrium aluminum garnet [Nd:YAG laser]). Ozone was applied for 30 s in caries superficial mode, and Nd:YAG laser was applied for 60 s. After the pretreatment procedures, sealants were placed inside a mold on the enamel surface. SBS was measured with a universal testing machine. Data were analyzed using analysis of variance. Tukey’s multiple comparison tests were applied to determine the difference between the groups (α = 0.05).
Results:
The lowest SBS was observed in the Fuji triage group. Nd:YAG laser and ozone did not affect the SBS of BeautiSealant. However, significant differences were determined in the Fuji triage and Grandio Seal groups after pretreatment procedures (P < .05).
Conclusion:
Ozone and laser can be employed to disinfect fissures before BeautiSealant application.
Introduction
Pits and fissures are prone to dental caries because they provide suitable conditions for plaque accumulation. 1 Fissure sealant placement creates a physical barrier preventing the growth of biofilm and fissure caries. 2 These materials are usually applied as soon as possible after eruption. However, difficulty in isolating oral fluids and the aprismatic and highly mineralized enamel surface of newly erupted teeth is the main limitation of using fissure sealants.3,4 These factors can cause an insufficient acid etch and result in sealant leakage and loss. 5 The occlusal pit and fissures are too narrow (only 0.1 mm wide) for effective cleaning by toothbrush or saliva, and bacteria and food can therefore easily adhere to the tooth structure. 6 Acid etching removes microorganisms from the enamel surface, although some studies have reported various quantities of remaining bacteria even after acid etching. 7 Different pretreatment procedures involving ozone, laser, and chemical agents have been employed for disinfection.8,9
Treatment with lasers has been extensively used in operative dentistry. Neodymium-doped yttrium aluminum garnet (Nd:YAG) laser is a pulsed infrared laser with a wavelength of 1064 nm, which is highly absorbable in pigmented tissues, and which causes liquefaction, and recrystallization in laser-irradiated enamel and dentin surfaces.8,10 This laser can be used in the remineralization of incipient caries, cavity disinfection, debridement, and alteration of pits and fissures, and in the treatment of dentin hypersensitivity.8,11 However, there is still no consensus regarding the ability of laser-treated enamel or dentin to provide suitable bonding.
Ozone is a triatomic molecule of oxygen that exhibits antibacterial properties because of its powerful oxidizing activity.12,13 Both aqueous and gaseous forms have been used for various therapeutic purposes in dentistry, such as disinfection of cavities and root canals, control of early caries lesions, management of inflammation and wound healing in periodontal tissue, and promotion of hemostasis.12,14,15 Ozone enters cells by breaking down the bacterial cell wall and membrane and provokes the destruction of microorganisms’ intracellular components. 14 Remineralization of the tooth structure and elimination of acidogenic bacteria have been reported with ozone therapy and its use before the application of fissure sealant is therefore recommended.16,17 However, the oxidizing potential of ozone may affect the polymerization of resin materials and the bonding of materials to enamel. 17 The aim of this study was to determine the effects of surface disinfection on the shear bond strength (SBS) of giomer, glass ionomer, and resin-based fissure sealants. The null hypothesis tested in this study was that the laser and ozone pretreatment of the enamel surface for disinfection would have no effect on the SBS of fissure sealants.
Materials and Methods
Settings and Design
This in vitro comparative study was performed in the laboratory of Atatürk University Dentistry Faculty. After a receipt of approval from Atatürk University Dentistry Faculty Ethical Committee, Turkey (approval number: 28/2018), freshly extracted impacted human third molars were collected from the patients who applied to the clinic in August to September, 2017. Sample size analysis was calculated using the website
Specimen Preparation
Following crown-root sectioning, the coronal parts of the teeth were sectioned in a buccolingual direction using a low-speed diamond saw (Isomet 1.000, Buehler Ltd, Lake Bluff, IL, USA) with water cooling. The prepared mesial and distal enamel surfaces were then flattened with 4000-grit polishing paper, and the enamel specimens were embedded in acrylic resin. Specimens were finally randomly and equally divided into three treatment groups.
Laser Group
The following Nd:YAG laser (Deka Laser, Florence, Italy) parameters were used, based on the manufacturer’s instructions and previous studies: an output power of 1.4 W, an energy level of 70 mJ, a frequency of 20 Hz, in noncontact mode, and a distance of 1 mm from the surface for 60 s (n = 30).
Ozone Group
The ozone gas was applied using an ozonytron XP (Biozonmylius, GmbH Mymed, Germany) device in accordance with the manufacturer’s protocol in caries superficial mode, CR/CA for 30 s (n = 30).
Control Group
No pretreatment procedures were applied to the enamel surfaces (n = 30).
After the pretreatment procedures, specimens were divided into three subgroups depending on the type of fissure sealant applied. Materials were applied according to the manufacturers’ instructions, and the sealants used in the study are shown in Table 1. A silicone mold 3 mm in diameter and 2 mm in height was placed on the enamel surfaces, and the sealants were then placed in the mold.
Composition of Fissure Sealant Tested in the Study

BeautiSealant
Self-etching primer was applied for 5 s. This was then air-dried for 5 s, after which the sealant was placed into a silicone mold and polymerized with an LED light device (Elipar Freelight II, 3 M-ESPE, St. Paul, MN, USA) for 10 s.
Fuji Triage
20% polyacrylic acid was applied to the enamel surface for 10 s according to the manufacturer’s instructions. This was followed by rinsing with water and drying under a gentle stream of air for 5 s. The GC Fuji Triage was then mixed and placed into a silicone mold and light-cured for 40 s using an LED light device.
Grandio Seal
Etching gel (35% phosphoric acid) was applied for 30 s. After rinsing and drying, the sealant was placed into a silicone mold and light-cured for 20 s using an LED light device.
Shear Bond Strength Test
All specimens were kept in distilled water at 37 ºC for 24 h and were subjected to SBS testing with a universal testing machine (Instron 3344, Instron Corp., Wilmington, USA) using a special blade applied to the adhesive interface at a crosshead speed of 1 mm/min. Specimens were exposed to stress until failure occurred, and the load per area was expressed in MPa.
Statistical Analysis
Because the SBS values were normally distributed, analysis of variance and Tukey’s post hoc test were used to investigate statistical differences. The level of significance was set at P < .05 for all analyses.
Results
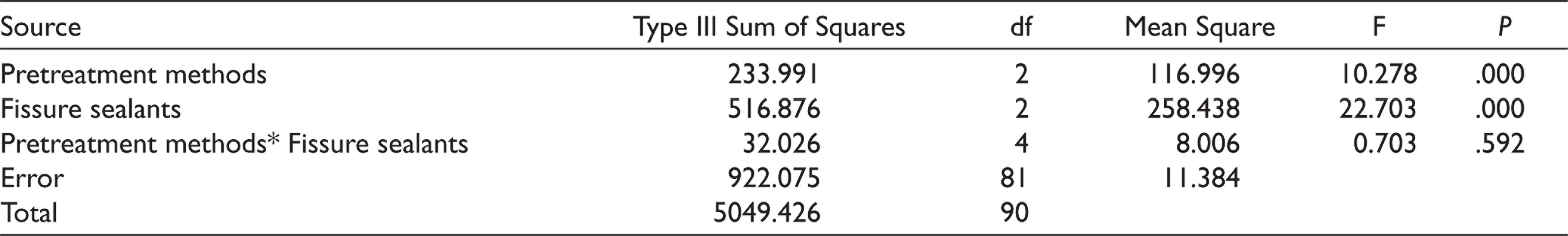
The mean SBS values and standard deviations for the tested sealants are shown in Table 2. SBS was significantly higher in the Grandio Seal group with no pretreatment, while Fuji Triage values differed significantly from the other sealants (P = .00). Laser and ozone pretreatment reduced SBS significantly in all sealant groups except for BeautiSealant (P < .05). Fuji Triage SBS values decreased significantly when pretreated with laser and ozone (P < .05). There was no significant difference between laser and ozone applications (P > .05; Tables 3, 4A, and 4B).
Mean Values and Standard Deviations of Shear Bond Strength Obtained in This Study

Statistical Analysis of Analysis of Variance
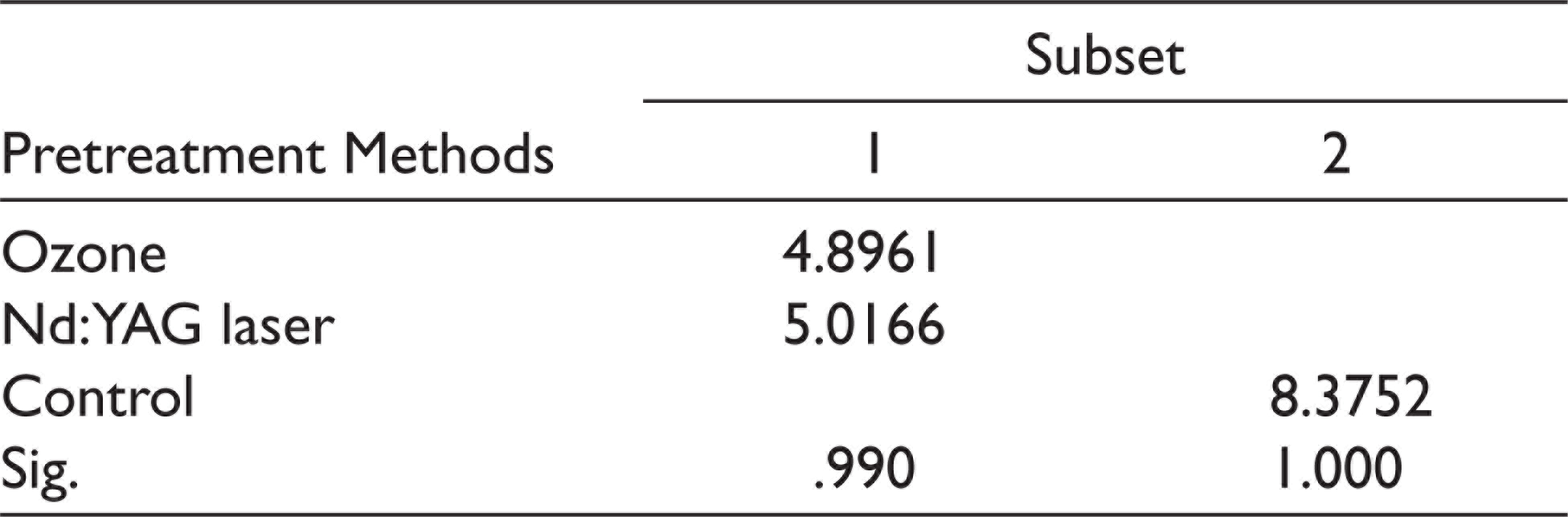
Tukey HSD Post Hoc Multiple Comparison Tests for Pretreatment Methods
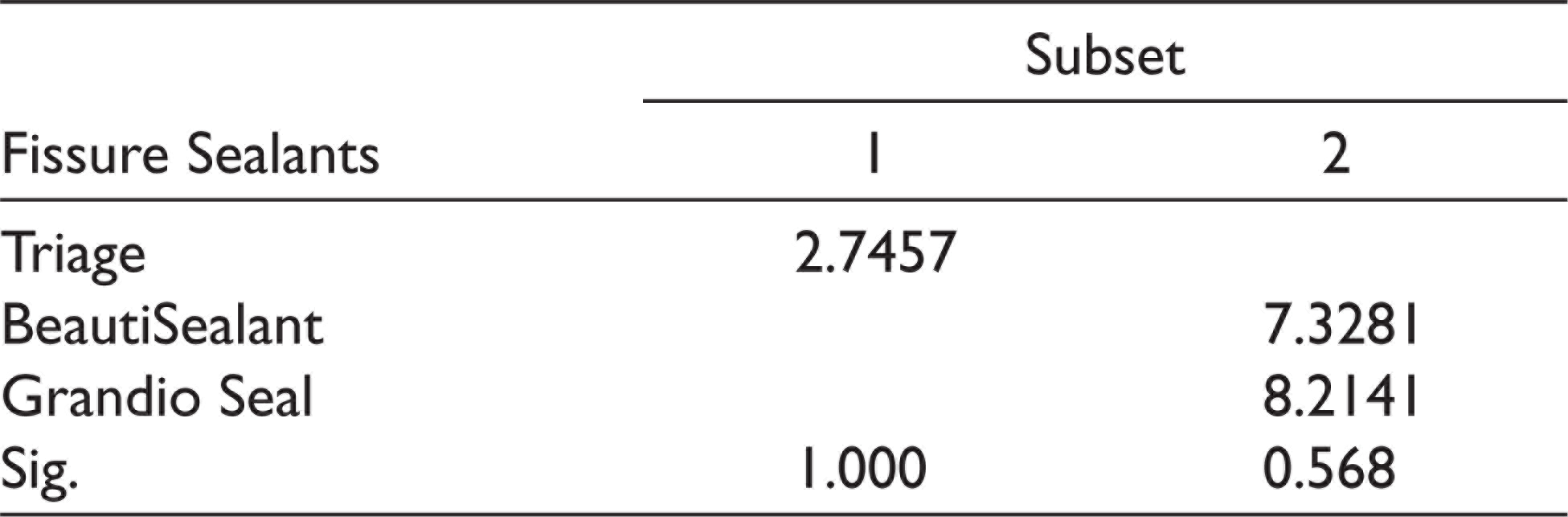
Tukey HSD Post Hoc Multiple Comparison Tests for Fissure Sealants Type
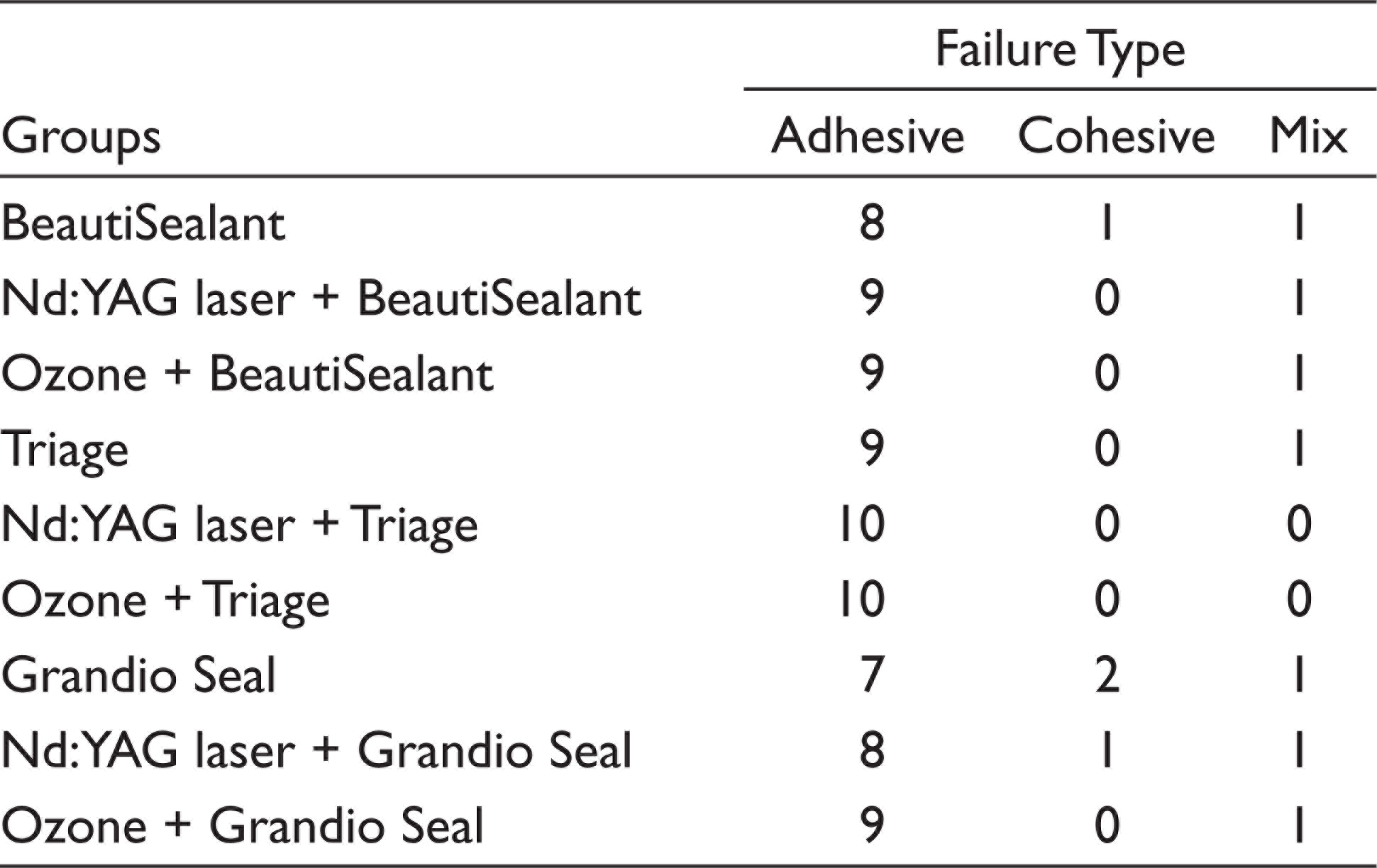
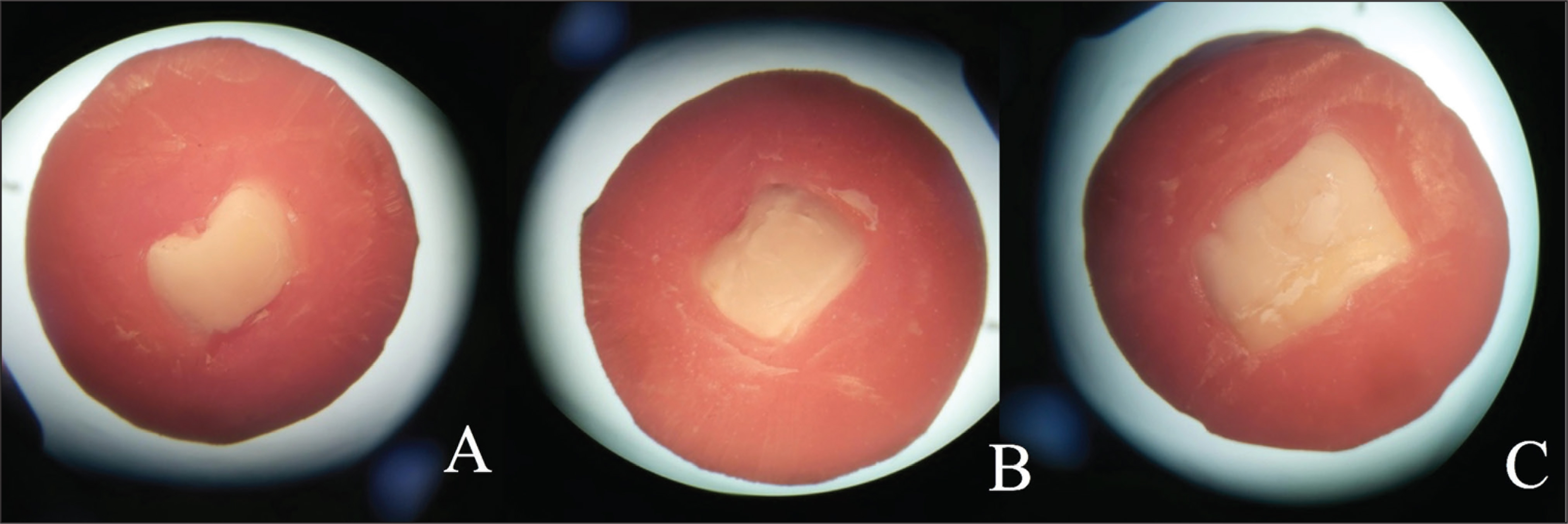
The enamel specimen surfaces were examined under a stereomicroscope (SZ-PT Olympus, Japan). Failure types were classified based on the amount of fissure sealant remaining on the enamel surface (<20% of remaining sealant representing adhesive failure, 20% to 80% representing mixed failure, and > 80% representing cohesive failure). Failure types are shown in Table 5 and Figure 1. The predominant failure type was adhesive in all groups.
Failure Types of the Experimental Groups After SBS Testing
The three images which were obtained under ×30 magnification of the stereomicroscope showed (A) adhesive failure, (B) cohesive failure, and (C) mixed failure modes
Discussion
The study findings demonstrate that the in vitro application of Nd:YAG laser and ozone caused significant decreases in SBS, with the exception of BeautiSealant, which is a surface prereacted glass material. Therefore, the null hypothesis was partially rejected.
Resin, glass ionomer, polyacid-modified resin, and more recently giomer-based fissure sealants are the material groups capable of use for sealing.18,19 The clinical success of sealants depends on the materials’ ability to adhere to the enamel surface. The sealant adhesion ability can be measured using the SBS test. 20 Studies assessing the success of fissure sealants have reported a lower retention rate for glass ionomer-based sealants than for resin-based sealants.21–23 Consistent with other studies, glass ionomer-based fissure sealant exhibited lower SBS compared to the giomer and resin sealant. Acid etching increases the surface energy, thus enhancing the wettability of the materials, and creates a morphologically porous enamel layer. The sealants are able to penetrate to a depth of 25–50 µm, thus providing a resistant and effective bond between the sealant and enamel.24,25 Polyacrylic acid etching provides good wetting of the tooth surface and produces a chemical interaction between the glass ionomer and the mineral phase of the enamel. 24 20% polyacrylic acid was used to condition the tooth surface before sealant application. 20% polyacrylic acid application has also been reported to provide good SBS. 23 Alonso et al. 25 showed that conventional glass ionomer sealant exhibited lower bond strength than resin and resin-modified glass ionomer sealants. They also reported that interaction between calcium from enamel and carboxylic groups from polyacid is responsible for low bond strength. Giomer-based sealant, consisting of methacrylate-based composite and surface prereacted glass ionomer, has become the preferred material for high-risk pediatric patients. 26 Our results showed that giomer-based BeautiSealant has a similar bond strength as that of resin-based sealant. Quader et al. 27 reported that giomer possessed greater compressive strength and toughness than glass ionomer. The majority of previous studies have assessed the F-releasing, penetration depth, and microleakage values of the giomer-based fissure sealant,19,28 and very few have evaluated its SBS.
The application of ozone to enamel is an effective method of disinfection in several situations, such as before fissure sealant use or orthodontic bracket adhesion.29,30 Ozone neutralizes bacteria and organic components on fissure and enamel surfaces because of its high activity and oxidation properties. It has therefore been suggested that some physical properties of enamel and the retention of restorative materials may affect ozone application.31,32 Ozone is a powerful antioxidant agent that reacts with all organic materials, and there is a possibility that collagen components may also be transformed. 33 Previous studies have reported that ozone application exhibited no adverse effect on sealant penetration and did not change the SBS of dental adhesives to bovine enamel and dentin tissue.34,35 Similarly, Pires et al. 29 reported that 20 s ozone application had no effect on the SBS of dental adhesives. However, Dalkılıç et al. 36 showed that ozone reduced the bond resistance of self-etch adhesives. Rodrigues et al. 37 reported that ozone applied for 40 s caused a significant reduction in the μTBS of restorative materials. In the current study, ozone pretreatment reduced the SBS of resin, and glass ionomer-based sealants to the enamel surface. The differences among the results may be because of the length of application, the type of ozone equipment used, or the type of dental substrate.
The disinfecting ability of Nd:YAG, Diode, Er:YAG, and Er, Cr:YSGG lasers has been evaluated from several aspects. It has been reported that the bactericidal activity and penetration ability of Nd:YAG laser is high. 8 In the present study, the effect of Ng:YAG laser on SBS of fissure sealants was evaluated. The findings of the study showed that laser application significantly reduced the bond strength of resin- and glass-ionomer-based fissure sealants. Alkhudhairy et al. 38 identified the energy level and output power of the laser as important factors affecting bond strength. The use of Nd:YAG lasers has been reported to cause chemical and morphological changes in the dental structure, to increase the distribution of oxygen, calcium, and phosphorus in the enamel; to present fewer soluble compounds; and to enhance acid resistance.39–41 Recent studies have shown that laser treatment of the enamel surface at energy levels of 60 mJ or lower causes the formation of a glass-like surface, while treatment at higher energy levels results in craters and cracks.42,43 According to Barcellos et al., 44 Nd:YAG laser irradiation significantly reduced the bond strength in bovine incisor enamel. Rattanacharoenthum et al. 45 showed that the bond strength of sealant to laser-irradiated enamel was significantly lower than that of phosphoric acid-etched enamel. In contrast, other studies have reported enhanced bond strength or no effect on enamel bond strength with the use of laser technology.46,47 This is possibly because of the use of different energy levels and application modes.
Failure types are usually reported as being between the adhesive and substrate (adhesive), within the restorative material or substrate (cohesive), or mixed. Triage, BeautiSealant and Grandio Seal showed a tendency to adhesive failure after ozone and laser treatment. This suggests that the adhesive–enamel interface was weakened by ozone and Nd:YAG treatment compared to control groups. There was a 100% rate of adhesive failure in Triage groups after ozone and laser treatment.
The present study gives important knowledge about the SBS of fissure sealant in the selection of materials after disinfection methods. The use of single type laser and the evaluation of the bond strength only on permanent teeth are the limitations of the present study. Further studies are needed to be undertaken using different disinfection protocols and different laser types on both primary and permanent teeth.
Conclusion
Within the limitations of this study, it can be concluded that disinfection of enamel with ozone and laser did not affect the bond strength of giomer-based fissure sealant.
Clinical Significance
Laser and ozone pretreatment did not affect the enamel bond strength of a giomer-based fissure sealant.
Footnotes
Acknowledgements
This research was presented at the International Congress on Preventive Dentistry Erzurum, Turkey, on March 5–8, 2018.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
