Abstract
Purpose:
Supraretinacular endoscopic carpal tunnel release (SRECTR) is a technique in which an endoscope is inserted superficial to the flexor retinaculum through a subcutaneous tunnel. The benefits of this method include a clear view for the surgeon and absence of median nerve compression. Surgeons can operate with a familiar view of the flexor retinaculum and median nerve downward, similar to open surgery. This study aimed to investigate the learning curve for SRECTR, an alternate method for carpal tunnel release, and evaluate its complications and the functional outcomes using a disposable commercial kit.
Methods:
We examined the open conversion rates and complications associated with SRECTR in 200 consecutive patients performed by two surgeons. We compared the operative time operated by a single surgeon. We evaluated outcomes in 191 patients according to Kelly’s grading system. Patients’ mean follow-up period was 12.7 months.
Results:
Nine patients required conversion to open surgery. There were no injuries to the nerves and tendons and no hematoma or incomplete dissection of the flexor retinaculum. The operative times varied between 11 and 34 minutes. We obtained the following results based on Kelly’s grading of outcomes: excellent in 116, good in 59, fair in 13, and poor in 3 patients.
Conclusions:
We found no patients with neurapraxia, major nerve injury, flexor tendon injury, superficial palmar arch injury, and hematoma. Although there was a learning curve associated with SRECTR, we performed 200 consecutive cases without neurovascular complications. This method may be a safe alternative to minimally invasive carpal tunnel surgery.
Keywords
Introduction
Carpal tunnel syndrome (CTS) is a common peripheral nerve disorder, and surgery is required when conservative treatment has failed. 1,2 The endoscopic carpal tunnel release (ECTR) technique has been shown to result in lesser pain, faster return of grip strength, and earlier return to work than the open carpal tunnel release (OCTR) technique. 3 –6 However, the ECTR technique may lead to incomplete release of the flexor retinaculum, neuropraxia, and nerve, flexor tendon, and superficial arch injuries. 1,6 –9
A recent report described an alternative method of CTS surgery using supraretinacular endoscopic carpal tunnel release (SRECTR). 10,11 In this technique, the endoscope is inserted into the subcutaneous tunnel superficial to the flexor retinaculum. This approach facilitates surgical field visualization and avoids median nerve compression, because the endoscope is not inserted into the carpal tunnel. Surgeons can obtain a familiar view of the flexor retinaculum and median nerve downward, similar to open surgery. Ecker et al. used a specific endoscope dissector and reported no major complications. 10 We performed SRECTR using a disposable commercial kit. We hypothesized that SRECTR would be a safe alternative method of minimally invasive carpal tunnel surgery.
Methods
Patients
We obtained institutional review board approval for this study. We performed SRECTR on 200 consecutive patients (59 men and 141 women; 25 had surgery on both hands). Patients’ mean age was 64.5 (range: 33–88) years. To diagnose CTS, we evaluated pain and/or paresthesia in the median nerve territory, nocturnal paresthesia, and thenar muscle atrophy. Tinel’s sign and Phalen’s provocative tests were used to support the diagnosis. Altogether, 105 patients (52.5%) underwent electrophysiological studies.
The inclusion criteria for surgical treatment were neurologic symptoms for >3 months and failure of conservative treatment. Patients were assessed according to the Hamada grading system: grade 1: positive numbness of the distribution of the median nerve with normal thenar prominence and complete opposition; grade 2: positive numbness with some thenar muscles atrophy and complete opposition; and grade 3: positive numbness with significant thenar muscle atrophy and incomplete opposition. 12 We included cases with a history of conservative treatment for distal radius fracture. The exclusion criteria were a recurrence of previous CTS surgery, wrist surgery, such as volar plating, and arteriovenous shunting in the affected side. The demographic details are provided in Table 1. According to the Hamada grading system, 117, 71, and 12 hands had grades 1, 2, and 3, respectively. 12 Most operations were performed under brachial plexus block or general anesthesia, although 32 patients (16%) required local anesthesia use. We did not terminate treatment with anti-platelet agents or anticoagulants in most patients. Other operations were performed concurrently according to the patients’ symptoms (Table 1). Senior surgeon who is an experienced hand specialist performed 154 (77%) operations and junior surgeon who is a less experienced hand specialist performed the remaining 46 operations. 13
Demographic data.

Preparation
The basic hand surgery set included curved 6- to 7-inch scissors with a thin blade, a 4.0-mm 30° angled standard endoscope, and a disposable endoscopic carpal tunnel release kit (CTS Relief Kit®, CONMED, Utica, NY). The CTS Relief Kit® contained two dilators, a cannula, and a knife (Figure 1). The cost of the kit is 13,200 yen in Japan.

CTS Relief Kit®. Cannula (white arrow), two dilators (black arrows), and knife.
In the SRECTR procedure, flexor retinaculum resection is performed from the proximal to distal direction. Therefore, it is recommended that a right-handed surgeon sits at the caudal side, and an assistant sits at the cranial side for the patient’s right-hand operation. For a patient’s left-hand operation, a surgeon sits at the cranial side (Figure 2).

Setting of a patient’s right-hand operation. The surgeon sits at the caudal side (white arrow) and the assistant sits at the cranial side (black arrow). The nurse stays next to the surgeon ($). A monitor is placed at the operative side (#).
Surgical technique
A pneumatic tourniquet is necessary to obtain a clear view. The wrist is immobilized in the neutral position with a holder (Figure 3). A transverse line is drawn on the metacarpophalangeal joint of the thumb parallel to the palmar crease. This line serves as a guide for the superficial palmar arch. A longitudinal line between the third and fourth fingers is drawn proximally in the palmar surface. An incision line of approximately 1.5 cm is marked on the wrist crease. The midpoint of the incision is on the line between the third and fourth fingers. If present, the palmaris longus tendon is marked.

Marking on the palm surface. A transverse line serves as a guide for the superficial palmar arch (#). A longitudinal line serves as a guide for the transection of the flexor retinaculum ($). An incision line of approximately 1.5 cm is marked on the wrist crease (white arrow). Palmaris longus (black arrow).
After cutting the skin, subcutaneous tissues are carefully observed, and the palmaris longus is retracted radially to avoid injury to the palmar branch of the median nerve. Then, the subcutaneous tissues are divided, and the fascia is exposed. The vessels are coagulated, if necessary. Scissors are inserted from the incision directing the curved blade toward the flexor retinaculum. The blades are opened to create a space on the flexor retinaculum by dividing the subcutaneous tissues. The plane of dissection is between the palmar aponeurosis and the flexor retinaculum. To obtain a clear view, fat tissues are removed from the flexor retinaculum as much as possible. Dissecting the subcutaneous tissue immediately on the flexor retinaculum is key for fat tissue removal on the flexor retinaculum. The dilators from the CTS Relief Kit® are used to verify the presence of sufficient space. Then, the surgeons insert the canula and endoscope to confirm the flexor retinaculum (Figure 4). The superficial palmar arch in the fat tissues can be seen distal to the flexor retinaculum in most cases. At this time, the surgeon looks for an aberrant motor branch of the median nerve. After gross observation, the cannula is removed once, and the proximal edge of the flexor retinaculum is cut approximately 1 cm under direct vision to easily begin the endoscopic dissection. Then, the surgeon inserts the cannula again and begins the endoscopic dissection. The surgeon holds the cannula and the assistant controls the endoscope (Figure 5). After confirming the absence of adhesion between the flexor retinaculum and median nerve by the reciprocating motion of a raspatory, the proximal part of the flexor retinaculum is cut using scissors (Figure 6). Similar to OCTR, no instrument is necessary to protect the median nerve while cutting the flexor retinaculum. The distal part of the flexor retinaculum is cut using the knife supplied in the kit if the scissors cannot reach it. After complete dissection, the flexor retinaculum stumps are separated in parallel and fat tissues on the median nerve can be confirmed (Figure 7). Finally, the remaining proximal part of the flexor retinaculum is cut approximately 1 cm under direct vision. Similar to conventional OCTR, the surgeon can confirm complete resection of the flexor retinaculum with SRECTR. A drain is used when surgeon suspects hematoma in patients with uncontrolled bleeding or patients who take anti-platelet agents or anticoagulants. However, it is not always needed.

Successful completion of the subcutaneous tunnel. The cannula and scope are inserted superficial to the flexor retinaculum.
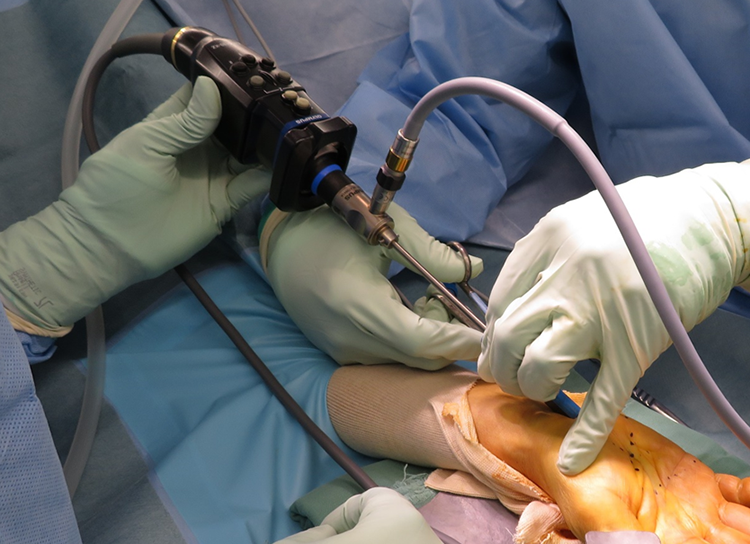
Operation: the surgeon is holding the cannula and the assistant is controlling the endoscope.

Endoscopic view. The flexor retinaculum is cut with scissors.

Image obtained after complete transection of the flexor retinaculum.
Methods of assessment
To investigate the learning curve associated with SRECTR, we compared the operative time and open conversion rate among the 154 patients who were operated by the senior surgeon. We divided the patients into groups A (initial 52 patients), B (next 51 patients), and C (last 51 patients). We assessed the rate of conversion to OCTR and the reasons of conversion. We evaluated the complications including nerve, tendon, and superficial palmar arch injuries, and hematoma. Patients’ outcomes were evaluated using the Kelly grading, which were as follows: excellent, complete relief of symptoms; good, persistence of occasional minor symptoms; fair, some constant or annoying symptoms; and poor, symptoms unchanged or worsened. 14 We planned to follow-up the patients for at least 3 months and were able to examine 168 patients till the final follow-up. We sent questionnaires to the patients who did not return for the final follow-up and 23 patients replied. We evaluated final outcomes in 191 patients. The patients’ mean follow-up period was 12.7 (range 3–40) months.
Statistical analysis
The Kruskal–Wallis with Dunn’s test was used to compare the operative times among groups A, B, and C. P values <0.05 indicated statistical significance.
Results
The mean operative times for groups A, B, and C were 21.7, 18.8, and 17.1 min, respectively (range: 11–34). Groups B (
None of the patients had neurapraxia, major nerve, flexor tendon, and superficial palmar arch injuries, and hematoma.
At the follow-up timepoint, 118 hands had excellent, 57 had good, 13 had fair, and 3 had poor results. Approximately one-third of the patients experienced pillar pain in the palm when holding an object or cutting a hard object with a kitchen knife.
Discussion
Our findings suggest that SRECTR would be a safe alternative to minimally invasive carpal tunnel surgery. Its principal advantages are as follows: it is safe and complications rarely occur due to the improved visualization without median nerve compression. 10 Surgeons can complete the operation with an assurance of complete resection of the flexor retinaculum. Generally, the incomplete release of the flexor retinaculum can only be identified through a re-operation. However, reconfirmation of intraoperative photographs can be alternative means. Therefore, another surgeon evaluated the intraoperative photographs of patients with fair and poor results, and another group of 30 patients were randomly selected. In this investigation, complete resection was confirmed in all photographs.
Until the twentieth century, several authors reported nerve injuries after conventional ECTR. 1,7,8,14,15 Although recent reports mentioned fewer nerve symptoms in ECTR than previous reports, nerve injuries remain an important issue. 6,9 For the SRECTR procedure, there were no reports of nerve injury or neurapraxia, 10,11 and we achieved similar results. The anatomic variations of the carpal tunnel structures, such as recurrent motor branch of the median nerve penetrating the flexor retinaculum, were reported. 2 Ecker et al. successfully performed endoscopic dissection of this anatomic variation in their SRECTR procedure. 10 The overlying muscle on the distal transverse carpal ligament has been reported as an anatomic variation and occurs in 13–36% of cases. 16,17 Jegal et al. mentioned that the presence of this overlying muscle indicated that the thenar motor branch originated from not only the radial side but also the anterior or ulnar side. 17 They warned of the possibility of thenar motor branch injury during transverse carpal ligament transection. 16,17 In our experience, we did not observe the thenar motor branch in the overlying muscle during separation. However, surgeons should be aware of the possibility of encountering a thenar motor branch. When the overlying muscle is thick, this muscle should be transfected first; then, the transverse carpal ligament is resected. Stepwise resection would be a safe management for cases with an overlying muscle.
There is a learning curve associated with SRECTR. The senior and junior surgeons had no experience with ECTR procedures before starting SRECTR. The junior surgeon served as the senior surgeon’s assistant several times before starting to perform SRECTR. We consider that SRECTR can be performed without experience with ECTR if the surgeon can perform OCTR capably. Success and safety of SRECTR depend on the surgeon’s experience with OCTR.
In this series, the middle and latter groups had shorter operative times than the initial group. Among the seven open conversions performed by the senior surgeon, four cases were performed in the initial group. The open conversion rate of ECTR was reported to be 2.5% by Agee et al., 7 14% by Kelly et al., 14 and 4.1% by Palmer et al. 15 Our series had a 4.5% open conversion rate. In SRECTR, open conversion is preferred if the surgical field cannot be clearly visualized, not if the endoscope was difficult to insert. Therefore, the surgeon can decide to perform open conversion before excessive median nerve compression occurs, which may sometimes occur with ECTR. One of the factors of unclear vision is local anesthesia. After injecting local anesthetics around the flexor retinaculum, swollen fat tissues could cover the surgical field and remove the benefit of the clear view. In our series, we used local anesthesia in 32 patients and 4 needed open conversion. Although SRECTR can be performed under local anesthesia, open conversion rate might be higher with local anesthesia than with a brachial block. We recommend performing SRECTR, which provides a clear vision under a brachial block if surgeons need detailed information of the carpal tunnel or are in the process of learning. We do not recommend the use of intravenous regional anesthesia because it may lead to unclear vision if there is bleeding from the vessel filled with local anesthetic. Once bleeding starts, the surgical field is covered with blood and a clear endoscopic view is difficult to obtain.
In this series, 16 hands in 13 patients had fair or poor results. Regarding the preoperative Hamada grades, 8 and 5 hands had grades 2 and 3, respectively. Three patients had diabetes mellitus and one patient had depression. We believe that the relatively higher grade and patient’s condition would influence the operative outcomes.
Although a rare complication, one disadvantage of the SRECTR is wound redness or scar formation. 10,11 Fat tissue dissection, skin elevation, and skin scratches could be possible factors related to complications. To minimize scar formation, we used a surgical tape on the proximal part of the incision to prevent skin scratches.
Apart from open procedures, ECTR can also cause pillar pains. Guo et al. reported that the occurrence rates of pillar pain were 7–61% for open surgery and 28% for ECTR. 18 Wong et al. reported that radial and ulnar pillar pains can occur after ECTR and OCTR. 5 In this report, all 30 patients who underwent ECTR had pillar pain. 5 Given that the definition of pillar pain differs depending on the physician, its cause or etiology remains controversial issue. 3,6,18 In this series, we defined pillar pain as the pain in the palm between the thenar and hypothenar regions. In SRECTR, pillar pain would be caused not only by the release of the transverse retinacular ligament but also by making the subcutaneous tunnel. The subcutaneous tunnel, formed to divide the flexor retinaculum and palmar aponeurosis, destroys structures around the palm and could cause pillar pain. Further investigation is necessary to compare ECTR and SRECTR.
The cost of OCTR performed under local anesthesia for outpatients is about 4,100 yen in Japan. The costs of SRECTR performed under general anesthesia for hospitalized patients and under brachial block for outpatients are about 104,000 yen and 24,000 yen, respectively. Therefore, SRECTR performed under brachial block may be acceptable.
There are several limitations in this study. First, we were unable to confirm the safety of the subcutaneous tunnel before endoscope insertion. An aberrant motor branch or abnormal variation of the vessels could be damaged during soft tissue dissection. Thus, preoperative ultrasound examination may be useful to identify an aberrant motor branch. 19 Second, the operation around the wrist could damage the palmar branch of the median nerve. The palmar branch runs between the flexor carpi radialis tendon and palmaris longus tendon. 20,21 Therefore, we retracted the palmaris longus to the radial side to avoid palmar branch damage. However, traction could cause the damage, and a palmar branch with an aberrant course could also be injured. 21 Third, we did not investigate the patient’s satisfaction and time taken to return to work. Further investigation on this is necessary. Finally, the final follow-up time point varied with different patients. This influenced the recovery rating in patients.
Conclusion
In our SRECTR technique, we used the basic hand surgery set, a 4.0-mm 30°-angled standard endoscope, and a disposable endoscopic carpal tunnel release kit (CTS Relief Kit®). Although some patients experienced pillar pain after the procedure, SRECTR is relatively safe and severe complications are rare due to the improved surgical field visualization. SRECTR would be a safe alternative to minimally invasive carpal tunnel surgery.
Footnotes
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
