Abstract
Introduction
The incidence of patellofemoral pain is approximately 2.2%1,2 according to a previous study. There are many factors that can cause patellofemoral (PF) pain, including osteochondral damage, patellar instability, overuse injury, Hoffa disease, and medial plica syndrome.3,4 Isolated PF arthritis is less prevalent than tibiofemoral (TF) joint arthritis and has been reported to be evident in 9% of radiographs of symptomatic knees taken in individuals over the age of 40 years. 5 There is a lack of consensus on the ideal treatment for PF joint cartilage lesions. Common surgical methods include cartilage restoration, lateral retinaculum release, tibial tubercle osteotomy, arthroscopic debridement, and patellofemoral arthroplasty.6,7 PF arthroplasty has been used more commonly in recent years. However, it may induce some complications, such as knee joint catching, patella maltracking, component wear, and periprosthetic infection.5,8–11 Another common treatment is osteotomy of the tibial tuberosity; it was first conceived in the 19th century to improve patellar tracking, but it has also been used to treat chondromalacia patellae.12–15 There are many different methods of performing tibial tubercle osteotomies, including the Hauser, Roux-Goldthwaite, Trillat, and Bandi procedures.16–20 The modified Fulkerson procedure is one of the most promising methods for TTO, some studies have reported improvement in 92% of patients’ symptoms.4,21,22 Also, patients have an excellent rate of return to work after the operation. 15 However, the clinical results of this treatment still vary.23–26 In addition, criteria that have been widely accepted for tibial tubercle osteotomy is lacking. Besides, there was no consensus about preoperative evaluation protocol. We hypothesized that age and femorotibial joint condition may play some roles in tibial tubercle osteotomy. Our goals were to review the mid-term outcomes of the modified Fulkerson osteotomy and suggest a more accurate indication for these patients.
Materials and Methods
This is a retrospectively study in single institution. The approval of the study protocols used to collect clinical data was provided by Institutional Review Board (IRB), Linkou Chang Gung Memorial Hospital, Taiwan (IRB No. 202001831B0). All methods were performed in accordance with the relevant guidelines and regulations. The IRB approves the waiver of the participants’ consent.
All patients who presented with anterior knee pain and were treated by the same senior surgeon between 1998 and 2015 were assessed and treated following a standard protocol. All patients who were considered for inclusion in this study complained of persistent anterior knee pain that was affecting their ability to perform daily activities, for example, walking and climbing stairs. The indications for surgery included symptomatic patellofemoral arthritis, chondrosis, and inferior-lateral facet involvement. Skyline radiographs of the patella in 30° of knee flexion and radiographs during weight bearing in the anteroposterior and lateral views of the knee were taken preoperatively for all patients. The tibiofemoral joint and patella height were evaluated and recorded. The exclusion criteria included the following: concomitant knee ligament injury, episodes of patella dislocation or subluxation), high-grade (III-IV) medial or proximal patellar facet arthrosis, high-grade (III-IV) tibiofemoral joint OA, patellectomy or old patella fracture.
Patients underwent a series of radiographic examinations to determine the severity of patellofemoral arthritis and stability. We primarily focused on chondral damage using the Iwano classification (Figure 1) in the imaging study. In addition, we also used the Merchant view to assess patella tilting/trochlear dysplasia and lateral subluxation.27–29 The lower limbs CT scan or MRI was not available in all the cases, so we did not discuss tibial tubercle–trochlear groove distance (TT–TG) or femoral torsion in this study. In addition, we recorded the Lysholm score and Knee Society score to evaluate the functional outcomes both before and after the operation. During the postoperative follow-up, the anteroposterior and lateral radiographs were used to assess radiological consolidation of the osteotomy. When no radiolucency at the osteotomy site was noted on the serial radiographs and the osteotomy yielded both no pain or movement, union was considered to have occurred. As the long axis view was not complete for all patients, we focused on the anatomic axis while assessing the knee joints. The average follow-up period was 5.9 ± 1.2 years (range 4.1–8.3 years). Failure of the operation was defined as the need for reoperation of the ipsilateral knee or a conversion to total knee arthroplasty. All the radiographic measurements were done by two orthopedists (C.-P. Yang and C.-J. Weng) Iwano classifications showing the roentgenographic stages of patellofemoral osteoarthrosis. (a) Stage 1. Joint-space narrowing is mild. The narrowest part of the joint space is wider than 3 mm. (b) Stage 2. Joint-space narrowing is moderate. The narrowest part of the joint space is narrower than 3 mm, but there is no bony contact. (c) Stage 3. Joint-space narrowing is severe. Partial bony contact below one-quarter of the joint surface is present. (d) Stage 4. Joint-space narrowing is very severe. The bony joint surfaces make full contact.
Surgical procedure
All surgeries were performed by the same senior surgeon (Y.-S. Cheng). Prophylactic antibiotics were administered routinely. We performed diagnostic arthroscopy before performing the tibial tubercle osteotomy. Patients with chondromalacia patellae were graded by using the Outerbridge system. Lateral release was performed routinely to improve patellar mobility. The tibiofemoral joint cartilage was assessed closely. If a small osteochondral lesion was present, microfracture awl was performed. Patients with advanced tibiofemoral joint arthritis would not receive the tibial tubercle osteotomy.
After the arthroscopy procedure, we did a standard modified Fulkerson osteotomy;12,30–32 a longitudinal incision was made from the lower pole of the patella, extending to the base of the tibial tuberosity. The patellar tendon was isolated by sharp dissection along its medial and lateral borders. An osteotomy was made using a microsagittal saw from the medial and lateral sides of the tuberosity and was extended distally for 10 cm, leaving the distal bony pedicle intact. Two 3.2-mm drill holes were made at the medial and lateral aspects of the distal attachment of the bone shingle to allow elevation without creating a cortical fracture distally in the tibia. The tuberosity was slowly elevated over a period of 4–5 min to a height of 10–15 mm using an osteotome, and medialization measuring 10 mm was performed while an intact periosteal sleeve was maintained. A pyramidal block of the femoral head allograft was fashioned and wedged beneath the elevated tubercle to maintain its position. Intravenous antibiotics were administered for 24 h postoperatively, and the drains were removed on the morning following surgery. Figure 2 is a typical postoperative image. Postoperative picture of the Fulkerson osteotomy. The A-P view is shown on the left, and the lateral view is shown on the right. We used two cancellous screws for fixation.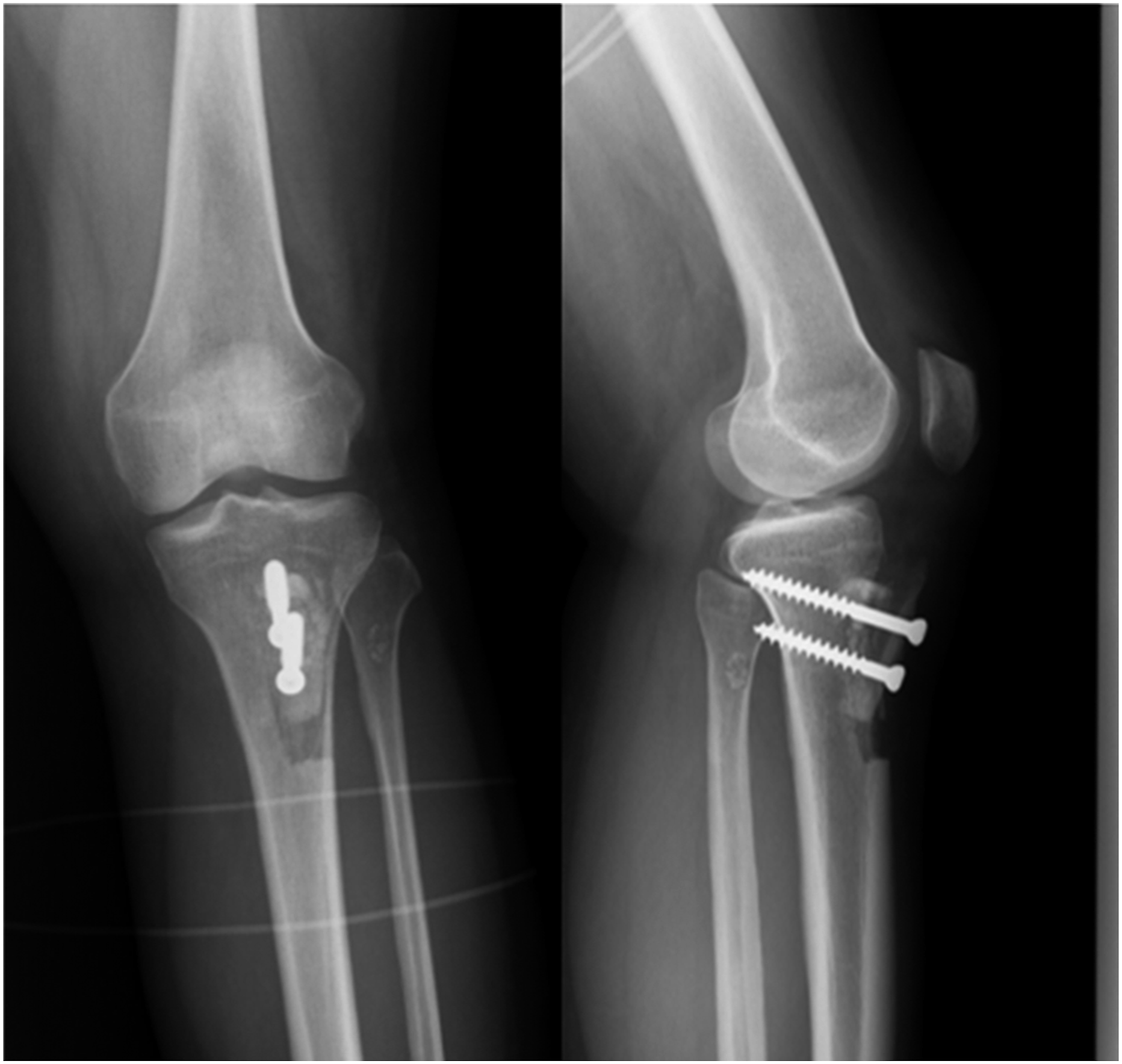
Rehabilitation protocol
The operated knee was protected in a knee brace for the initial 6 weeks postoperatively. The range of motion was limited to 30° of flexion during the first 2 weeks, and an additional 30° of flexion was allowed every 2 weeks until full flexion was reached. Partial weight bearing, as tolerated, was allowed. The patients were discharged on the first postoperative day. After this initial period, weight bearing, as tolerated, was encouraged. From the first postoperative day, exercises focused on patellar tendon mobilization, extension mobilization, and quadriceps and hamstring muscle reactivation were encouraged, as tolerated. After the first 6 weeks, the use of a stationary bicycle without resistance was encouraged for both limbs. The use of a stationary bicycle with progressive resistance was initiated at week 12, and other exercises such as treadmill walking and swimming were also encouraged. At week 24, the patients were allowed to return to all activities and sports without limitations on each patient’s individual schedule.
Statistical analysis
We used the Statistical Package for the Social Sciences (SPSS) and Microsoft Office Excel. All categorical data were analyzed using Fisher’s exact test. Radiographic outcomes comparison between the survival and non-survival groups were analyzed using the two-tailed Mann–Whitney U test or unpaired t-test. Results were considered statistically significant at a p value <0.05.
Results
Demographics and preoperative alignment.

Radiographic outcomes-Patellofemoral joint
Radiographic parameters.

aStatistically significant result.
Radiographic outcomes-Femorotibial joint
Arthroscopic findings.

aAll the cartilage injuries were small (<1 cm2), and patients with larger lesions were excluded from the study.
Clinical results
The mean preoperative Lysholm score was 56.12, and the Knee Society score was 60.52. At the final follow-up, these scores improved to 88.75 and 86.49, respectively. There was a statistically significant difference between the values according to the Wilcoxon test with a continuity correction (p < 0.001).
Complication and survival
No cases of patellofemoral symptom recurrence, nonunion, or wound infection were observed. However, 22 (55%) patients underwent cortical screws removal. Among these patients, 12 (54.5%) had implant irritation and difficulty kneeling, and 10 patients elected to undergo this operation.
For the survival rate, eight patients (20%) underwent total knee arthroplasty in the follow-up period, five of whom underwent the operation within 5 years. However, none of these patients suffered from patellofemoral arthritis progression. The indication for total joint arthroplasty was advanced femorotibial osteoarthritis. The survival analysis is shown in Figure 3. The survival analysis.
Comparison of the survival and non-survival groups
Comparison between the survival and non-survival groups.

aStatistically significant result.
Progression of femorotibial osteoarthritis was the main reason for TKA. The condition of the cartilage at the index surgeries seemed to have no correlation with femorotibial osteoarthritis progression. No difference was found in the incidence of meniscal injury. In the survival group, there were 21 cases of no meniscal injuries, 6 cases of medial meniscus fraying, and 4 cases of lateral meniscal lesions. In the non-survival group, there were five cases of medial meniscal injuries and one case of a lateral meniscus lesion, and two patients had no meniscus injury.
Discussion
Fulkerson osteotomy yields promising outcomes, in terms of both pain relief and function, for patients suffering from PF joint cartilage lesions. In our study, the mean Lysholm scores improved from 56.12 (poor) to 88.75 (good), and the Knee Society score improved from 60.52 (poo-fair) to 86.49 (excellent). Atkinson et al. reviewed 48 knees undergoing tibial tubercle advancement osteotomy due to patellofemoral arthritis between January 1993 and April 2015. They followed a protocol with the standard amount of elevation, 10–15 mm. If patellar maltracking was present, the patients also underwent medialization of the tibial tubercle (6–12 mm). Femoral head bone allograft blocks were used in all cases. In their study, the overall clinical outcomes were rated as excellent/good in 77%, fair in 35%, and poor in 8% of the knees. 12 The modified Fulkerson procedure seems to be an appropriate treatment for overloading around the patella. Because the patella engages in the trochlear groove at approximately 30°–90° of knee flexion, anteriorization of the tibial tubercle may decrease the patellofemoral contact pressure in this functional range.
No patients had recurrent PF symptoms during the follow-up period in our study. It is widely accepted that central trochlear lesions, medial patellar lesions, and workers’ compensation issues are related to less favorable outcomes. 33 However, there was an unacceptable rate of TKA conversion in our study. Among the patients who underwent conversion, five underwent a second operation in 5 years. A total of eight patients underwent ipsilateral TKA during the follow-up period. All of the patients had deteriorated femorotibial joints, especially of the medial compartment. The coronal knee alignment was significantly more varus prior to TTO in this group (survival: 6.4° ± 4.5°; non-survival: 1.8° ± 4.9°, p = 0.08). Besides, the mean age was significantly different between the survival and non-survival groups (48.3 ± 11.1 vs 57.8 ± 8.7 p = 0.03). Age had not been a contraindication for TTO before. Klinge et al. followed 15 patients underwent TTO due to lateral and/or distal patellar chondrosis for more than 15 years and found satisfactory results in 94% of knees (16 of 17). 22 No cases had conversion to knee arthroplasty. The mean age at surgery was 29.5 years in their series. Different from their study, the patients in our group were much older. Further study should focus on the impact of age on TTO and establish an age threshold for this kind of surgery.
There is little evidence on the effects of TTO on the femorotibial joint and the criteria of the meniscal condition before TTO. Atkinson et al. reviewed 50 patients who underwent TTO due to symptomatic patellofemoral arthritis. Two (4%) knees developed progressive medial compartment osteoarthritis in the medial knee compartment; one underwent TKA at 8 years; and the other underwent a high tibial osteotomy at 4 years.
12
However, the authors did not provide sufficient information on the lower limb alignment or meniscal condition. A finite element study performed in 2006 used a 3D finite element model of the entire knee to investigate the effect of tubercle elevations on the biomechanics of the entire knee joint (1.25 cm and 2.5 cm). According to the findings by Shirazi-Adl et al., the PCL and TF contact forces at larger flexion angles significantly increase after tibial tubercle elevation due to changes in the lever arm.
34
However, this study only focused on the Maquet procedure and did not consider the effect of medialization. Using a simple mathematic model (Figure 4), we determined that medialization may affect the lever arm of the medial TF compartment. Therefore, there is an urgent need for a knee joint kinematic study on tibial tubercle osteotomies. In addition, thorough preoperative planning before TTO is needed, including the estimation of the medial TF pressure after the operation. Illustrative picture of the vectors of the knee joint. We hypothesized that as the tibial tuberosity was moved medially, the vector of the loading force from the patella tendon and quadriceps in the coronal plane may shift from the lateral side to the medial side. (Q: quadriceps muscle force vector; M: medial femorotibial compartment; L: lateral femorotibial compartment).
In addition to clinical improvement, the radiographic parameters also showed persistent changes during the postoperative follow-up. During the preoperative evaluation, the patellofemoral angle was 1.1° ± 14.5°, and the congruence angle was 28.0° ± 27.8°. At the last follow-up, the values were 6.6° ± 11.9° and 15.5° ± 28.5°, respectively, and both measures showed significant and persistent improvement. Indeed, many researchers have questioned the validity of PF alignment parameters. In a systemic review published in 2019, Hochreiter B et al. reported highly variable patellofemoral alignment in healthy patients, including the sulcus angle (SA), femoral trochlear depth (FTD), patellar tilt angle (PTA), lateral patellofemoral angle (LPFA), lateral femoral trochlear inclination (LFTI), and tibial tubercle–trochlear groove distance (TT–TG). 35 However, a good radiographic protocol that can be used to evaluate chondromalacia of the knee is still lacking. The study by Mattila et al. showed that the severity of articular cartilage lesions of the patella, as determined by a grading system, arthroscopy, and MRI, had a weak correlation with the clinical symptoms of anterior knee pain.36,37 As a result, we could not conclude that the improvement in patellofemoral alignment was related to the relief of knee pain.
Studies have revealed different complications of TTO, including delayed wound healing, infections, skin necrosis over the tuberosity, tuberosity fractures, proximal tibial fractures, delayed union of the osteotomy, and the need for later hardware removal.21,30,31,38–40 Generally, the Maquet procedure has higher complication rates (up to 8.2%) due to excessive anteriorization and the resultant soft tissue tension.18,19,24,38 On the basis of this concept, we limited the extent of correction and preserved the periosteum around the osteotomy site. In our study, no patients had delayed wound healing or infection. Having an intact periosteum can also prevent nonunion following Fulkerson’s osteotomies. Luhmann et al. 41 reported an overall bony complication rate of 5.9, which decreased to 0% when an intact periosteum was left around the distal portion of the osteotomy site. Akkie et al. used a V-shaped TTO, which the tibial tuber is completely detached on three sides, and reveal lower risk for tibial fracture (0.75%) and nonunion (0.37%). 42 The most common complication that occurred in our study was irritation around the bicortical screws. A total of 55% of patients underwent the removal of implants after bone union. Shelbourne KD et al. suggested that only one 4.0 mm cancellous screw directed proximally toward the posterior tibia is used to avoid hardware tenderness if a stable, flat osteotomy cut has been obtained. 31 However, two screw fixations are still commonly used in these kinds of surgeries. Zonnenberg CB et al. used only absorbable suture fixation while performing TTO with revision total knee arthroplasty (TKA). In 18 out of 23 patients, immediate weight bearing was allowed with a knee extension splint. The rates of radiological consolidation and migration (>90%) with this technique were at least as good as those with other fixation techniques. 43 According to these studies, 44 the development of a less invasive fixation device is necessary to improve patient satisfaction in the future.
There are several limitations of this study. It is a relatively small retrospective study. Additionally, we did not arrange routine preoperative CT or MRI studies. Because the major symptoms of our patients included anterior knee pain due to patellofemoral arthritis, rather than patella instability, CT and MRI scans were not commonly recommended preoperatively. In addition, MRI has poor sensitivity in detecting early-stage patellar chondromalacia. Third, TTO and other treatments for PF arthritis, such as cartilage restoration and PF arthroplasty, could not be compared, as a comparison group was not included in our study.
Conclusion
The modified Fulkerson osteotomy is a reliable treatment for PF arthritis. Wound complications can be avoided with limited correction and preservation of the periosteum. However, we found that patients with older age and those with varus alignment have an increased risk of deteriorated medial femorotibial cartilage. Therefore, studies on the effects of the modified Fulkerson osteotomy on the TF compartment and the age threshold for TTO should be conducted in the future. Moreover, surgeons must take the whole knee joint into account during the preoperative evaluation.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
