Abstract
Background:
Lateral discoid meniscus (LDM) should be treated and preserved with saucerization and/or suture repair. However, repair of the meniscal hoop structure is sometimes difficult due to displacement or large defects. In this study, we aimed to examine tear patterns based on the Ahn classification in those requiring meniscal repair and those undergoing subtotal meniscectomy.
Methods:
Twenty-three patients were evaluated (mean age, 27.4 years; mean follow-up period, 2.5 years). The following were evaluated: displacement morphology based on the Ahn classification, site of tear under arthroscopy, morphology, surgical procedure, Lysholm score at final postoperative follow-up, and clinical outcome of meniscus using Barrett’s criteria.
Result:
There were 16 knees without displacement (saucerization with suture repair, 13 knees; subtotal meniscectomy, 3 knees) and 10 knees with displacement (reduction with suture repair, 3 knees; subtotal meniscectomy, 7 knees). Subtotal meniscectomy was performed more often in cases with dislocation, especially in the central shift type as defined by the Ahn classification. The mean Lysholm score was 65.0 points preoperatively and 95.3 points postoperatively. Twenty-three knees (88%) were postoperatively categorized under the Barrett’s criteria as healing and 3 knees (12%) were categorized as non-healing. The number of non-healing cases that underwent subtotal meniscectomy was relatively small (1 of 10 knees), and the short-term results were not poor.
Conclusion:
Localized peripheral longitudinal tears tended to be repairable even with displacement, while peripheral tears covering the entire meniscus or with severe defects/tears in the body of the meniscus tended to be difficult to repair, leading to subtotal meniscectomy.
Introduction
Subtotal and total meniscectomy have been performed for treating lateral discoid meniscus (LDM) 1 –3 ; however, risks for developing arthritic changes and osteochondritis dissecans (OCD) over a long-term observation period have been reported. 4,5 Recent progress in treatment have aimed to preserve the meniscus as much as possible with good results reported for saucerization to reshape the meniscus to a normal width and, if needed, additional suture repair. 6,7 Despite the success of these recent developments in treatment options, LDM is complicated by various damage and displacement morphologies, and the meniscal abnormality often requires some degree of resourcefulness in terms of determining the appropriate surgical technique. In particular, some cases are difficult to repair the meniscal hoop structure. As with subtotal and total meniscectomy, the disruption of meniscal hoop strength with inadequate function and meniscal extrusion can result in osteoarthritic changes and OCD over the long term.
Although Watanabe’s classification is widely accepted for the categorization of LDM, 8 its use has fallen out of favor in recent years, as the classification system does not account for the degree of meniscal damage or stability. LDM is often associated with instability due to rupture of the margin, in which the hoop function of the meniscus may not be maintained and may affect long-term results. A newer classification based on preoperative MRI described by Ahn et al. 9 is believed to be useful to determine the degree of meniscal damage with a specific focus on the rupture site of joint capsule site of the lateral meniscus, the presence or absence of instability, and the classification of dislocation morphology into 4 groups comprising of the no shift, antero-central, postero-central, and central shift types. The purpose of this study is to examine the tear patterns, surgical procedure, and short-term clinical results based on the Ahn classification in LDM injury refractory to repair, defined as those requiring meniscal repair and those undergoing subtotal meniscectomy that could not be treated by saucerization alone.
Materials and methods
From 2016 to 2019, patients who underwent suture repair after saucerization of LDM and irreparable cases that underwent subtotal meniscectomy at our department were evaluated. Cases with a postoperative course of less than 1 year were excluded. Subtotal meniscectomy was defined as cases with a residual meniscal width of 5 mm or less under arthroscopy. A total of 23 patients and 26 knees (14 males, 12 females) were included. The mean age was 27.4 (13–45) years, and the mean follow-up period was 2.5 (1.2–3.4) years. The following criteria were evaluated: displacement morphology assessed by simple MRI images based on the Ahn classification (Figure 1), 9 site of tear under arthroscopy, morphology, surgical procedure, Lysholm score at final postoperative follow-up and clinical outcome of meniscus using Barrett’s criteria (Figure 2). 10 Barrett’s criteria was comprised of three objective parameters for clinical evaluation of meniscal healing after meniscal repair. We categorized the case as “healing” if all three items were negative. Approval for this study was given by the institutional review board (IRB), and informed consent was obtained from each patient or candidate. For statistical analysis, the Lysholm score was expressed as mean, standard deviation, and range. In addition, data were analyzed using a paired t-test and Wilcoxon signed-rank test between pre- and postoperative scores. The Mann-Whitney U test was used between the saucerization and suture group and the subtotal meniscectomy group. A p value of <0.01 was considered statistically significant. Analyses were performed using SPSS statistics ver. 22.0 (IBM Japan, Ltd., Tokyo, Japan).
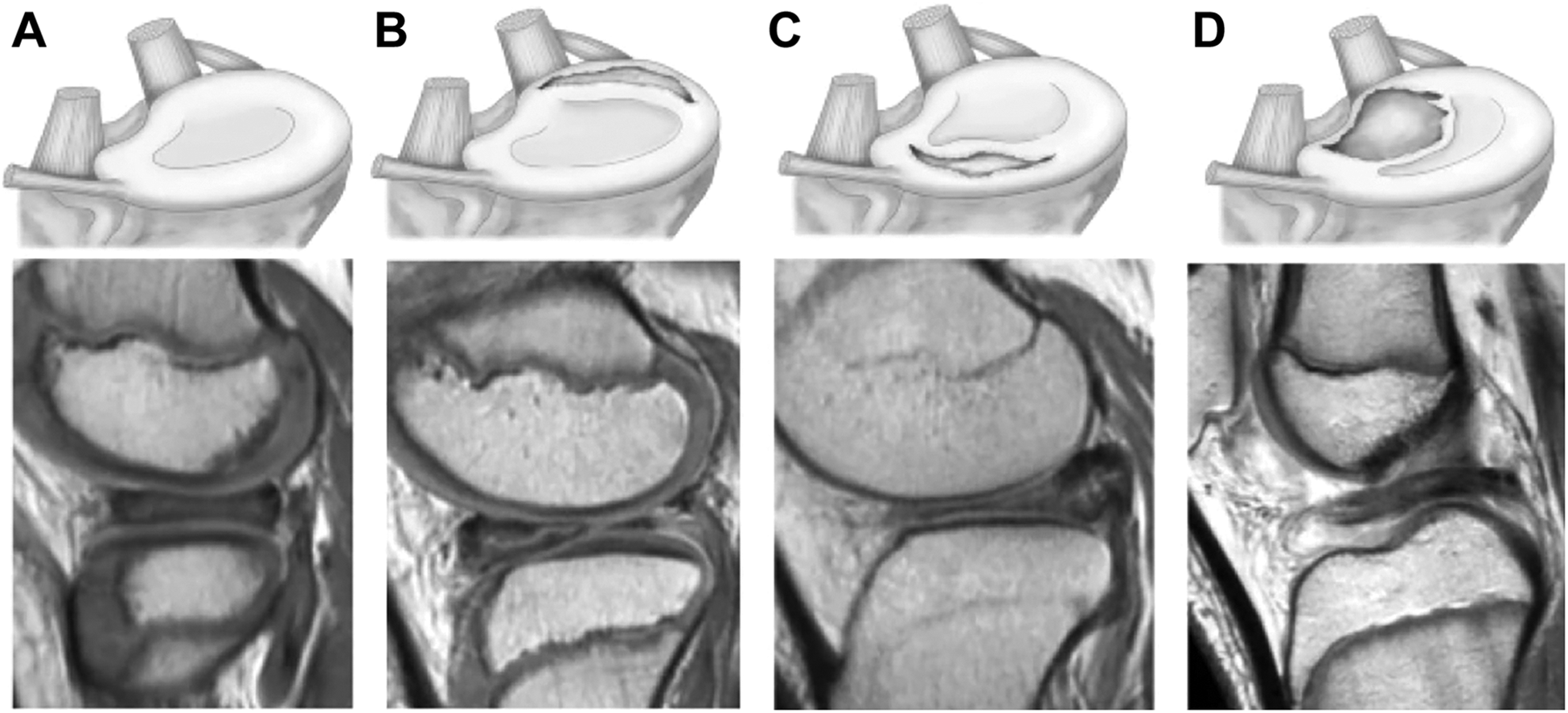
Ahn classification based on MRI. Magnetic resonance imaging classification of the discoid lateral meniscus (DLM) based on peripheral detachment. (A) No shift, (B) anterocentral shifting corresponding to a longitudinal tear in the posterior horn, (C) posterocentral shifting corresponding to a longitudinal tear in the anterior horn, and (D) central shifting corresponding to posterolateral corner loss.

Barrett’s criteria. Barrett’s criteria consisted of three objective parameters for clinical evaluation of meniscal healing after meniscal repair. We determined whether three items are positive or negative, and we evaluated as “healing” if all three items were negative.
Results
Detailed arthroscopic findings and operative interventions are shown in Table 1. The arthroscopic findings and operative intervention were assessed for each displacement type according to the Ahn classification based on preoperative MRI images. There were 16 knees without displacement and 13 knees that underwent suture repair due to residual tear in the remaining meniscus after saucerization, and 3 knees underwent subtotal meniscectomy due to difficulty in suturing. Suture repair according to tear type were performed as follows: horizontal tear, 5 knees; transverse tear, 3 knees; peripheral longitudinal tear, 1 knee. Fibrin clot augmentation was performed in 3 knees with horizontal tear and 1 knee with transverse tear.
Arthroscopic finding and operative intervention.

Ahn classification based on preoperative MRI. There were more subtotal menisectomy with shift. †Fibrin clot augmentation was performed in 3 knees; ‡Fibrin clot augmentation was performed in 1 knee.
The number of subtotal meniscectomy by shift type is shown in Table 2. The three knees that were refractory to repair and underwent subtotal meniscectomy were all complicated by a defect in the meniscal body or severe degenerative tear. Tears with displacement were observed in 10 knees, and 3 knees underwent reduction that required additional suture repair for their peripheral longitudinal tears, and 7 knees underwent subtotal meniscectomy due to difficulty in reduction or suturing. Subtotal meniscectomy was performed more often in cases with dislocation, especially with those exhibiting central shift as defined by Ahn et al. 9
Number of subtotal meniscectomy by shift type.

Those without meniscal displacement underwent subtotal meniscectomy in 3 of 16 knees, while those with displacement underwent subtotal meniscectomy in 7 of 10 knees. Among those with meniscal displacement, those with central displacement underwent subtotal meniscectomy in all cases.
Pre- and postoperative clinical outcomes are shown in Table 3. The mean preoparative Lysholm score was 65.4 ± 7.6 points in all cases, 65.3 ± 7.6 points in the saucerization and suture group, and 65.6 ± 8.0 points in the subtotal meniscectomy group. There were no statistical differences between each group. Furthermore, the mean postoperative Lysholm score was 95.2 ± 4.1 points in all cases, 95.0 ± 5.3 in the saucerization and suture group, and 95.3 ± 3.4 points in the subtotal meniscectomy group. There was also no statistical difference between each group. However, there were statistical differences between the mean pre- and postoperative scores in all groups. Barrett’s criteria was categorized as healing for 23 knees (88%) for and non-healing for 3 knees (12%). In all non-healing cases, residual joint edema was observed. In addition, the number of non-healing cases that underwent subtotal meniscectomy was relatively small (1 of 10 knees), and the short-term results were not poor.
Pre- and postoperative clinical outcomes.

The Lysholm score improved from a mean of 65.4 points preoperatively to 95.2 points postoperatively in all cases. Similarly, the saucerization and suture group and the subtotal meniscectomy group improved from a mean of 65.3 and 65.6 points preoperatively to 95.0 and 95.3 points postoperatively, respectively, and statistical differences were observed in each group. However, no statistical difference between the saucerization and suture group and the subtotal meniscectomy group was observed. Twenty-three knees (88%) were healed and 3 knees (12%) were not healed according to Barrett’s Criteria; moreover, residual joint edema was the only applicable criteria in all unhealed cases.
 : no statistical difference (p ≒ 0.95).
: no statistical difference (p ≒ 0.95).
 : statistical difference (p < 0.01).
: statistical difference (p < 0.01).
 : no statistical difference (p ≒ 0.93).
: no statistical difference (p ≒ 0.93).
Report of a representative case
17-year-old female. The preoperative MRI image shows that the LDM was displaced anterocenterally and was subsequently categorized as an antero-central shift under the Ahn classification (Figure 3). Intraoperative arthroscopic findings showed a 3-cm long longitudinal tear on the joint capsule side of the posterior segment, and a partial longitudinal tear on the capsule side of the anterior segment with central meniscal shift except for a section of the anterior horn (Figure 4). Although reduction was initially attempted, saucerization was performed first due to the difficult of reduction. Reduction was reattempted, and reduction of the posterior segment was achieved; however, the reduction of the middle to anterior segment was unachievable. The posterior segment was reduced and sutured using the all-inside technique, and only the synovial tissue remained with no meniscal tissue of the anterior to middle segment (Figure 5).

Preoperative MRI. Preoperative MRI T2 star coronal view (A); Preoperative MRI T2 star sagittal view (B). The lateral meniscus exhibits an antero-central displacement according to the Ahn classification system.

Interoperative arthroscopic findings. Longitudinal tear on the joint capsule side of the posterior segment (block arrow) and a similar longitudinal tear of the anterior segment with a meniscal displacement toward the center except for a section of the anterior horn (double block arrow).

Interoperative reduction and technique. Saucerization was performed first because temporary reduction was unachievable. Only the posterior segment achieved reduction when reattempted. The posterior segment was sutured using the all-inside technique. Only synovial tissue remained with no meniscal tissue of the anterior to middle segment.
Discussion
Peripheral longitudinal tear of lateral meniscus starts from the popliteal hiatus due to its poor connection with the meniscus and extends to the anterior or posterior horn. 11 Therefore, when there is a considerable defect in the popliteal hiatus of the DLM and reduction with a probe is unachievable, subtotal menisectomy is considered as a viable option, albeit with reluctance. 12 In addition, those with displacement are prone to require subtotal meniscectomy than those without displacement, and among those with displacement, the central shift type has been reported to most commonly require subtotal menisctomy. 9 In this study, when the meniscal body was difficult to reduce or if there were concurrent defects of the meniscal body or severe degeneration, the hoop function of the meniscus was also difficult to repair. Depending the displacement morphology of the meniscus, a temporary fixation should be performed with sutures, followed by a partial meniscectomy. Furthermore, the use of fibrin clot augmentation has been described in the literature, particularly in cases exhibiting concurrence of horizontal or transverse tear. 12 In this study, even if meniscal displacement was observed, localized peripheral longitudinal tears tended to be repairable, while those with peripheral tears covering the entire meniscus and those with severe defects or tears in the body of the meniscus tended to be difficult to repair. In terms of postoperative outcomes, in addition to subtotal meniscectomy, those with residual peripheral rim of 5 mm width or less and those that cannot maintain the hoop function of the meniscus have been reported to show predisposition to concurrent degenerative changes or OCD. 13,14 The merger rate of osteochondritis dissecans of the lateral femoral condyle (OCD) is highest in those with central shift as described by the Ahn classification. The remaining volume of the mid to posterior horn showed a negative correlation with OCD. 15 Although the short-term postoperative outcomes in this study were relatively good for cases wherein the hoop function was difficult to maintain, an assessment of long-term outcomes should be examined in future studies.
We investigated LDM cases that were refractory to meniscal repair and subtotal meniscectomy at our hospital. Even if meniscal displacement was observed, cases with less severe peripheral tears and defects tended to be repairable after saucerization. However, it is difficult to repair the hoop function of the meniscus in cases with peripheral tears, severe tears of the meniscal body, or defects. We believe that further improvements in surgical techniques are warranted for better results in those refractory to conventional methods.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
