Abstract
Purpose:
Total knee replacement (TKR) is associated with post-operative pain. Femoral nerve block can relieve the pain but also affects the post-operative mobility. Saphenous nerve block (SNB) can improve analgesia without interfering mobilisation. However, there is no consensus on the ideal mode of administration of SNB. We aim to compare the effects of single shot versus continuous SNB on patients undergoing TKR.
Methods:
Patients were randomised into two groups: single shot and continuous SNB groups. Post-operative rehabilitation and mobilisation were assessed by blinded physiotherapists, and preoperative and post-operative American knee scores were recorded by blinded specialised nurse. Post-operative analgesics usage was recorded by blinded pain nurses and anaesthetists.
Results:
Sixty-four patients were recruited; 6 patients withdrew with 29 patients in each group. There is no significant difference in early mobilisation and rehabilitation comparing both groups. The mean of the range gained on day 2 when compared to day 1 in single-shot SNB group was 17.41 ± 19.67° versus continuous SNB group was 23.45 ± 19.18° (p = 0.149). The mean of the range gained on day 3 when compared to day 1 in single-shot group was 27.24 ± 22.66° versus continuous SNB group was 29.31 ± 21.57° (p = 0.6). The mean of maximum flexion achieved by day 3 in single-shot SNB group was 92.41 ± 9.6° versus continuous SNB was 91.90 ± 7.95° (p = 0.84). The day of reaching maximum flexion and the goal of 40 m showed no significant difference. Length of stay (LOS), difference in post-operative American Knee Society knee score at 3 months and analgesics usage showed no significant difference.
Conclusion:
There is no significant difference in comparing the effect on mobilisation, LOS, early clinical outcome, analgesics usage in the single-shot group and the continuous SNB group.
Keywords
Total knee replacement (TKR) is often associated with severe post-operative pain. 1 Traditionally, continuous femoral nerve block (FNB) is considered the gold standard for pain relief after TKR. 2 However, FNB also reduces quadriceps muscle strength and thereby compromises ambulation with potential risk of fall. 3,4
On the other hand, the saphenous nerve is a pure sensory branch of the femoral nerve innervating the anterior part of the knee capsule as well as the medial side of the lower limb. In addition to single-shot nerve block, continuous blockade can be achieved with an insertion of a perineural catheter next to the saphenous nerve in the adductor canal under ultrasound guidance, followed by intermittent bolus injections or continuous infusion of local anaesthetic during post-op period. 5
Recent studies have demonstrated effective analgesia can be delivered by saphenous nerve block (SNB) while preserving motor function thus improving early mobilisation after operation. 5 However, the number of studies is still limited with no consensus on the ideal mode of administration of SNB for post-TKR pain relief. Therefore, we would like to compare the effects of single shot versus continuous SNB on patient outcome. 6– 13
Methods
This randomised controlled trial was approved by the Local Clinical Research Ethics Committee. This is a joint study organised by the Department of Anaesthesia and Intensive Care and Department of Orthopaedic and Traumatology in our hospital. Data will be collected from the same pool of recruited patients but separately analysed by two different principal investigators, focusing on pain control (anaesthesia) and mobilisation/rehabilitation (orthopaedics), respectively. This is a non-commercial trial without any forms of sponsorship.
Written informed consent was obtained from all patients. The data of this study came from patients scheduled for unilateral TKR in our hospital from September 2017 to October 2018.
Inclusion criteria included all patients within the age of 18–80 who undergo primary, unilateral TKR under central neuroaxial block with an American Society of Anaesthesiologists physical status of I–III. Exclusion criteria included secondary osteoarthritis, severe deformity of the knee (varus or valgus more than 20°, severe bone loss more than 10 mm, fixed flexion deformity >30° and collateral laxity), contraindication to Transamin, COX-2 inhibitors, opioid or local anaesthetics, chronic opioid use, operation performed under general anaesthesia, pregnancy and extreme body weights.
The sample size was calculated based on an unpublished retrospective review of previous TKR post-op pain survey while mobilising during rehabilitation period in our hospital. We estimated a mean pain score (numeric rating scale) of 7 during knee flexion (standard deviation = 2) in the placebo group (SNB not administered) with a reduction of 2 to be clinically relevant. With power of 90% and an overall two-sided type I error rate of 0.05, 21 subjects would be required in each group. Nine additional subjects on each arm would be recruited to compensate for dropouts.
Computer-generated random assignment was used, and sealed opaque envelopes were used to randomise patients. It is only revealed to the list anaesthetists who perform the SNB during the operation, all other investigators and administrators as well as patients were blinded.
Standard anaesthesia methods were used. Etoricoxib (Arcoxia; 90 mg) and ondansetron (8 mg) will be given as oral premedication within 1 h prior to surgery. Single-shot spinal anaesthesia or combined spinal-epidural will be provided as surgical anaesthesia with midazolam/propofol sedation given if required. No systemic opioids will be given intraoperatively.
All surgeries were performed with pneumatic tourniquet pressure set at 100 mmHg higher than the systolic blood pressure. Standard medial parapatellar approach and cemented posterior stabilised TKRs were performed. Pericapsular injection of local anaesthetic (40 ml of ropivacaine 3 mg/ml + adrenaline 5 mcg/ml) was given before implantation as a single-dose local infiltration analgesia (LIA). Transamin (30 ml of transamin (1.5 g) + 20 ml of 0.9% normal saline) was given intra-articularly after arthrotomy closure. Low molecular weight heparin (clexane 40 mg Q24H) was given to patients with body mass index ≥27 as prophylaxis to deep vein thrombosis.
The SNB catheter is placed in the operative room immediately after the surgery under ultrasound guidance before the central neuroaxial block wears off in both single shot and continuous SNB group.
Post-operatively, both single shot and continuous SNB groups received a bolus of 4–6 ml of 1% ropivacaine injected via the saphenous nerve catheter in the recovery room by the attending anaesthetist before discharge to orthopaedic wards. Intermittent injection of the study medication (4–6 ml of 0.9% normal saline as placebo for the single-shot group and 4–6 ml of 1% ropivacaine for the continuous group) is then prescribed every 6 h regularly, and 15 min before physiotherapy sessions twice daily.
Standardised multimodal analgesia and adjuncts were provided to all patients including intravenous fentanyl patient-controlled analgesia, oral analgesics and rescue analgesics.
Starting from post-operative day 1, all patients underwent a standard course of training. Range of movement of the knee was recorded and walking distance assessed. Data collection was performed by physiotherapists who were blinded to the study group. Patients were discharged when they were physically fit and able to walk independently with frame. Patients were followed up in 3 months’ interval. Preoperative and post-operative American Knee Society knee scores at 3 months were recorded by specialised nurse who were also blinded to the study group. Analgesics usage was recorded by blinded pain nurses and anaesthetists who were responsible for patient assessment during post-op acute pain rounds.
Primary outcomes include range gained on days 2 and 3 compared to day 1, maximum flexion achieved by day 3, days to reach maximum flexion and walking distance of 40 m. Secondary outcomes include length of stay (LOS), difference in post-operative American Knee Society knee score at 3 months and analgesics usage.
Statistical analysis
Baseline characteristics and outcomes will be compared using t test or Mann–Whitney U test for continuous variables, and Pearson’s χ2 test or Fisher’s exact test for categorical variables, as appropriate. The value of p < 0.05 was considered as statistically significant.
Results
Sixty-four patients were recruited in the study; 6 patients withdrew from the study. One patient underwent unicompartmental knee replacement instead of TKR; one patient requested to stop using patient-controlled analgesia instead of the proposed 3-day duration; two patients had inadvertent slipped out of saphenous nerve catheter before proposed 3-day duration; two patients were prescribed ropivacaine injection instead of study drug A/B by their attending anaesthetists and blinding was lost, so it was regarded as a breach of study protocol.
No actual patient harm or adverse events were reported (Figure 1).

Flow Chart of study selection
Demographics were compared between two groups of patients and showed no significant differences. (Table 1)
Demographic data.a

SNB: saphenous nerve block.
a Data are expressed in counts or mean.
The mean of the range gained on day 2 when compared to day 1 in the single-shot SNB group was 17.41 ± 19.67° and in the continuous SNB group was 23.45° ± 19.18° (p = 0.149). The mean of the range gained on day 3 when compared to day 1 in the single-shot group was 27.24° ± 22.66° and in the continuous SNB group was 29.31° ± 21.57° (p = 0.6). The mean of maximum flexion achieved by day 3 in the single-shot SNB group was 92.41° + 9.6°and in continuous SNB was 91.90° ± 7.95° (p = 0.84; Table 2).
Post-operative range.a

SNB: saphenous nerve block.
a Data are expressed in mean.
In the single-shot SNB group, 3 patients reached maximum flexion in day 1, 9 patients reached maximum flexion in day 2, and 17 patients reached maximum flexion in day 3. In continuous shot SNB group, 2 patients reached maximum flexion in day 1, 16 patients reached maximum flexion in day 2, 11 patients reached maximum flexion in day 3 (p = 0.168; Table 3).
Days to reach maximum flexion.a,b

SNB: saphenous nerve block.
ap = 0.168.
b Data are expressed in counts.
For the goal to reach walking for 40 m, in the single-shot SNB group 11patients were able to do so in day 1, 12 in day 2, 4 in day 3 and 2 required more than 3 days. In the continuous SNB group, 15 patients can reach the goal in day 1, 9 in day 2, 4 in day 3 and 1 required more than 3 days (p = 1.513; Table 4).
The day to reaching walking 40 m.a,b

SNB: saphenous nerve block.
ap = 1.513.
b Data are expressed in counts.
The mean LOS in the single-shot SNB group is 7.17 ± 1.47 days. The mean LOS in the continuous SNB group is 6.69 ± 2.22 days (p = 0.111). The mean of the differences in post-operative knee score in 3 months in the single-shot SNB group is 26.97 ± 25.10. The mean of the differences in post-operative knee score in 3 months in the continuous SNB group is 22.31 ± 24.2 (p = 0.63; Table 5).
Secondary outcomes.a

SNB: saphenous nerve block.
a Data are expressed in mean.
The mean of total fentanyl usage in the single-shot SNB group was 1395.21 ± 672.34 mcg versus the continuous SNB group was 1362.69 ± 775.37mcg (p = 0.576). The mean of total rescue tramadol in the single-shot SNB group was 5.17 ± 20.46 mg versus the continuous SNB group was 0 ± 0 mg (p = 0.154; Table 6).
Total analgesics used.a
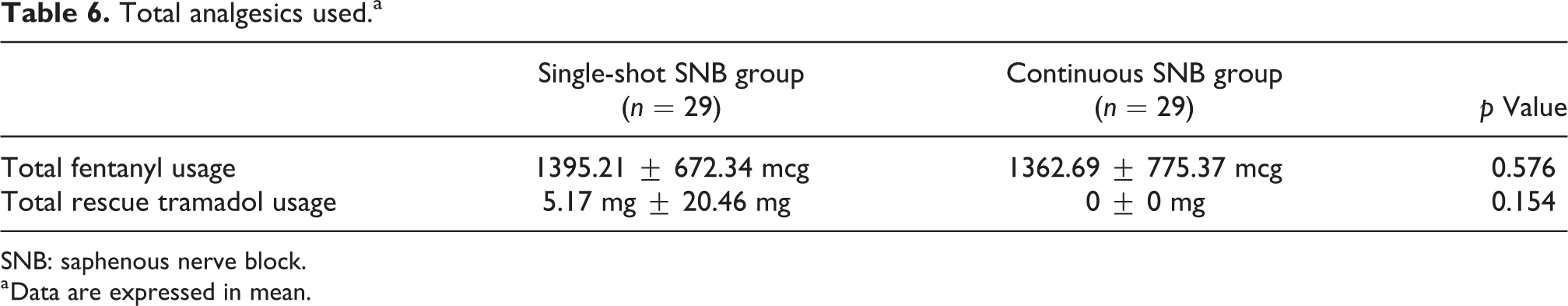
SNB: saphenous nerve block.
a Data are expressed in mean.
Discussion
Our focus was the effect of single-shot SNB versus continuous SNB on post-operative mobilisation and rehabilitation in patients receiving TKR. Both primary and secondary outcomes in our study showed no statistical differences. Primary outcomes including range gained on days 2 and 3 compared to day 1, maximum flexion achieved by day 3 and the day reaching the walking distance of 40 m. Secondary outcomes include LOS, differences in post-operative American Knee Society knee score at 3 months and the usage of analgesics.
This is the first study in our locality comparing single-shot SNB versus continuous SNB on post-operative mobilisation. Literatures had been reviewed showing that single-shot SNB versus continuous SNB on post-operative mobilisation and rehabilitation showed no statistical differences. Benefits had been shown in some studies that continuous SNB had better pain control when compared with single-shot SNB but it was not unanimous. Therefore, there is still no consensus on the best mode of administration of SNB post-operative patients with TKR done.
It is hoped that our study will contribute to the process of reaching a consensus on the optimal mode of administration of SNB for patients undergoing major knee surgeries in future.
According to Turner et al. 10 , they stated that single-injection SNB provided a similar analgesia effect as continuous SNB for up to 36 h after block placement in patients who underwent total knee arthroplasty. However, at 42 h and after, the continuous SNB was more favourable. They also showed that post-operative mobilisation and rehabilitation such as ability to straight leg raise, patient satisfaction and LOS were statistically insignificant in both groups. Shah et al. 11 stated that continuous SNB was superior to single-shot SNB in terms of pain control but was similar for early functional recovery. Min et al. 12 showed that continuous SNB provided superior analgesia and fewer side effects without any significant motor deficit than the intravenous patient controlled analgesia with a single-shot SNB. Svava et al. 13 indicated no benefit of continuous infusion SNB added to a single-dose LIA compared with LIA alone on pain while ambulating on post-operative days 1 and 2. SNB showed no superiority in ambulation ability on the two post-operative days.
Limitations of our study included that the pre-procedure ambulation aid requirements were not taken into account as the study was not powered for such analysis. Social factors were also not explored which could affect LOS.
With no adverse effects reported in this study and previous studies, it could reassure the safety of SNB.
In conclusion, our results indicate no benefit of continuous SNB compared with single-shot SNB in post-TKR early functional recovery. With further studies to support that single-shot SNB is not inferior to continuous SNB extra costs for catheters and pumps and manpower for the care of continuous infusion or bolus injection needed could be reduced.
Footnotes
Acknowledgements
The authors would like to acknowledge the invaluable assistance of Dr Chan Chin Chin, Dr Vansie Kwok of the Department of Anaesthesia and Intensive Care, Ms Wong Tai Fong (Advanced Practice Nurse), Ms Ho Mei Yee (Registered Nurse), Ms Tse Yan Kei (Registered Nurse), Ms Ho Sze Man (BSc(Hons) Physiotherapy), all nursing staff and physiotherapists in Orthopaedic wards and all members of staff at the operating and recovery room at Pok Oi Hospital, Hong Kong SAR.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
