Abstract
Background:
Total hip arthroplasties (THAs) bearing is one of the most important factors for hip replacement because THA survival depends on it. Metal-on-metal (MoM) bearing has lower wear than metal-on-polyethylene but lot of aseptic loosening decrease utilization. We analyze the survival rate of 28 mm Metasul® bearings after a mean follow-up of 12.9 years.
Methods:
The main objective of this study was to evaluate the survival of the MoM. We evaluate 779 consecutive THAs performed between January 1995 and December 2005 for primary osteoarthritis, congenital dysplasia classified Crowe I, or rheumatoid arthritis. Survival rate was calculated by the Kaplan–Meir method. The association between survival and age, gender, body mass index (BMI), and surface coating was investigated with a proportional odds model. The clinical assessment included Oxford score.
Results:
Six hundred fifty-two THAs were reviewed. Sixty-two revisions (9.5%) were performed including 34 aseptic loosening and 11 deep infections. The survival for prosthesis with any reason at 20 years was 87% (confidence interval (CI) 83–90.2) for aseptic loosening at 20 years was 90.1% (CI 87–93.8). There was no association with age, BMI, and surface coating. Gender was significant with lower aseptic loosening for men, hazard ratio = 0.45, p value = 0.035. Oxford score was 57 ± 6.7 (19–60).
Conclusion:
The survival rate of Metasul was well and seems to be like our clinical finding. However, radiographic aseptic loosening without surgery is not included in the survival rate. The Oxford score was very good with a lot of patients with asymptomatic hip.
Level of Evidence:
Level IV/Retrospective study
Introduction
Over 180,000 hip protheses were performed in 2018 and the projection forecasts a major increase in hip surgeries. 1 The reference bearing is the metal-on-polyethylene (MoP) with its wear problems and osteolysis. 2,3 The most common reason for revision is aseptic loosening with the release of wear products from the bearing surfaces. An alternative to this MoP is a hard–hard metal-to-metal (MoM) or ceramic-on-ceramic (CoC) with both very low wear and debris volume. 4 The MoM was declined as a low-carbon implant with femoral heads often larger than 36 mm in diameter, which showed a high rate of early loosening, 5,6 and high carbon implants with femoral heads less than 36 mm in diameter. Sulzer Medical Technology (Winterthur, Switzerland) developed a second-generation small-head MoM implant, whose high carbon content was designed to minimize wear. In the first clinical studies, 10-year survival was 97.9% to revision for any reason and 100% to aseptic loosening. 7 We found in our clinical practice a low rate of revision of these total hip arthroplasties (THAs). The objective of this retrospective monocentric study was to evaluate the revision rate of Metasul® 28-mm diameter prosthesis, Zimmer® laboratory (Warsaw, Indiana, USA), with a minimum follow-up of 11 years. The high-carbon MoM couple has a correct medium-term survival rate, 8,9 the hypothesis was that this survival rate was good over time.
Materials and methods
This retrospective monocentric study concerned a continuous series of all patients operated between 1995 and 2005 of a THA at the University Hospital of Clermont Ferrand, France. The inclusion criteria were a first-line THA with a Metasul to study the survival of all the MoM implant of our center. The exclusion criteria were a revision of a THA, a history of osteonecrosis of the femoral head, hip infection before surgery, local primary or secondary tumor, traumatic or congenital dislocation of the native hip, cervical, and stage II–IV acetabular dysplasia of the Crowe classification. 10
The Metasul bearing (Zimmer, Warsaw, USA) is the prosthesis with a polyethylene insert with a Metasul metallic sandwich cup, combined with a 28-mm diameter Metasul head. Acetabular implants were either cemented (Metasul Low Profile) or noncemented (Metasul Kappa Insert with metal back Cedior® (Zimmer) or Metal-back CLS Expansion Cup® (Sulzer®) Insert Metasul CLS). The sealed inserts were fixed either directly into the native acetabulum previously milled or via a support ring (M.E. Muller™ original ring (Zimmer)). Femoral implants could be cemented (original M.E. Muller rod, Zimmer) or uncemented (Avenir® Muller rod (Zimmer)). The cement was high viscosity cement with an antibiotic (Palacos® R-40 Gentamycin (Haerus®)) (Figure 1).

Example of implants at 15 years. (a) and (b) Acetabular component CLS® with Metasul®, (c) and (d) acetabular component Cedior® with Metasul, (e) cemented stem M.E. Muller™.
The procedure was planned using template on frontal pelvis radiographs to determine the size of the implants, the length of the cut, and the offset of the THA. All patients were operated in lateral decubitus at 45° with an external anterolateral approach of Hardinge.
The main objective of this study was to evaluate the survival of the MoM. The main criterion of judgment was the surgical revision. After an analysis of the medical files and the consultation reports, telephone interviews were carried out to contact the patients directly or, failing that, their immediate family (spouse or child) or their attending physician to find out if their patients had revision. In case of revision, the date, reason, and name of the surgeon performing the revision were recorded to confirm the cause and the type of procedure performed (cleaning, unipolar, or bipolar revision). These interviews used a standardized questionnaire, and it was performed by three of the authors (RE, GV, and SM). During the interview with the patient and in the absence of revision, the Oxford functional score (Appendix 1) 11,12 was collected. The scores ranged from 60 to 12 points for an asymptomatic hip to a very painful hip with a major functional impairment.
From 1995 to 2005, 893 patients were operated with 980 THA with MoM bearing, 806 unilateral and 87 bilateral, with an average follow-up of 12.9 ± 4.5 years. Two hundred one patients were excluded after analysis of their file because they met the exclusion criteria. Population is shown in Figure 2. The mean age of the intervention was 63.2 ± 9.3 years with a minimum of 29 years and a maximum of 88 years. There were 160 patients (20.6%) who died since surgery and 127 patients (16.3%) lost to follow-up. There was no significant difference between the lost and the group assessed. None of the deaths listed was linked to a complication of THA. In the case of the surgical indications of the patients included, 679 THAs (87.1%) were performed for idiopathic osteoarthritis hip, 32 (4.1%) secondary to chronic inflammatory arthritis (inflammatory arthritis, ankylosing spondyloarthropathy, and lupus), and 69 (8.9%) dysplastic.
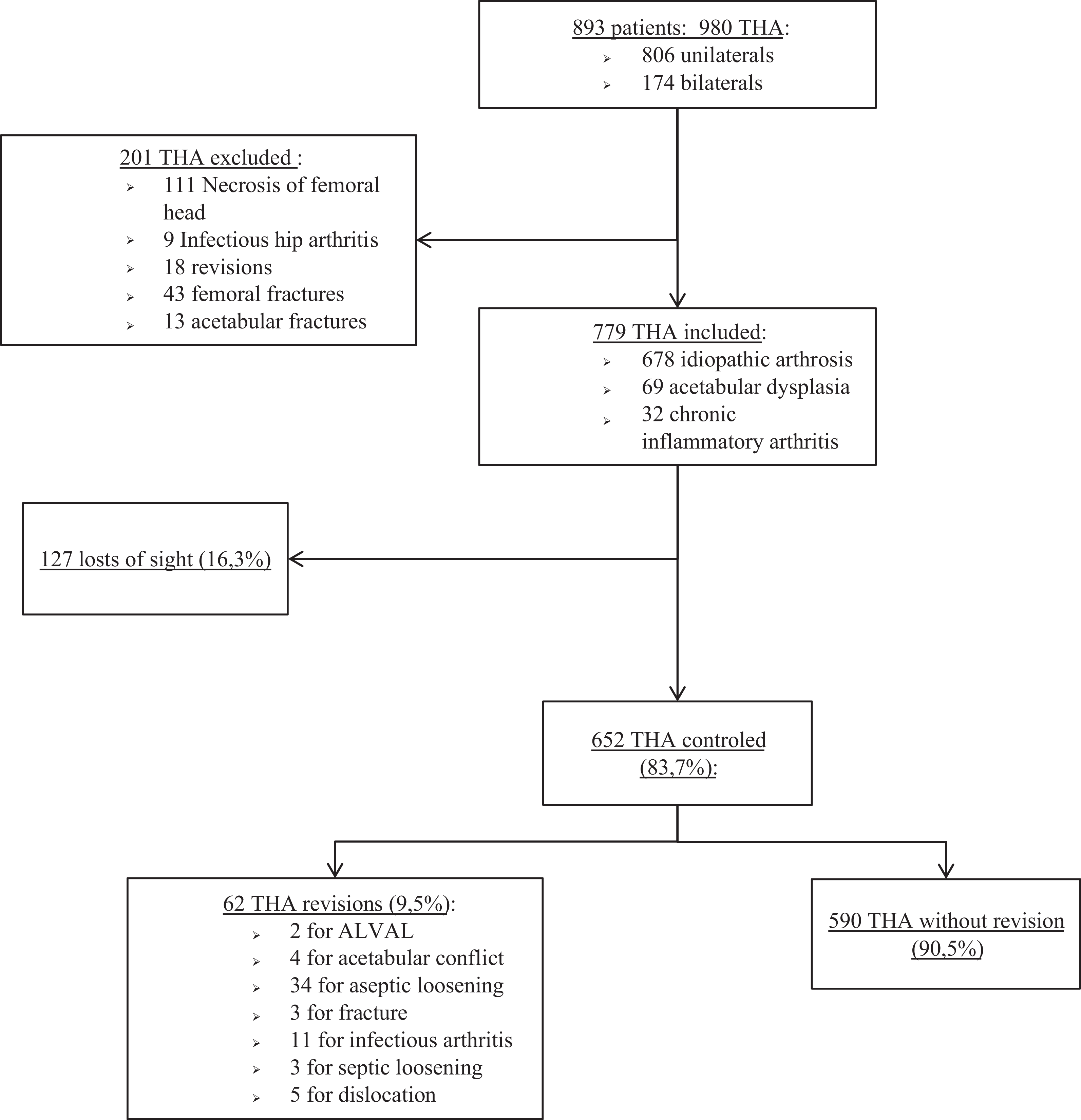
Flowchart.
We used 477 (61.2%) uncemented acetabular implants, including 343 (45.4%) for the Cedior/Insert Metasul Kappa couple and 123 (15.8%) for the CLS® Expansion Cup/Metasul CLS Insert. There were 302 (38.8%) Metasul Low Profile cemented inserts, of which 69 (9.2% of the total THA) were on a support ring. For the femoral stems, 768 (98.6%) were cemented against 10 (1.4%) uncemented. Population description is provided in Table 1.
Population description.

Statistics were computed with Stata v12 (Stata Corp., College Station, Texas, USA). Results are expressed as frequency and percentage for categorical data and as mean ± standard deviation for continuous data. The cause of revision was analyzed using Fisher’s exact test for categorical data and using Kruskal–Wallis test for continuous data. Prothesis survival was analyzed using Kaplan–Meier curves, considering revision as the event and time from initial operation to revision for reoperated patient or to latest news (=censor). Date of death is considered as latest news, and prosthesis is considered still functional at this date. Survival rates and their 95% confidence interval are given at 5, 10, 15, and 20 years. Log-rank tests (univariate) and Cox models (multivariable) were used to analyze factors related to prosthesis survival. Results are shown as adjusted hazard ratio (HR) and their 95% confidence interval. All tests were two-sided and a p-value <5% was considered statistically significant.
Results
The survival curves are shown in Figures 3 and 4. The survival rate was 93.6% at 10 years and 87.0% at 20 years.

Survival curve for all causes of revision with a survival at 20 years of 87%, CI 95% [0.830–0.902].

Survival curve for revision for aseptic loosening with a survival at 20 years of 90.1%, CI 95% [0.870–0.938].
Table 2 presents the distribution of causes of surgical revision, most of them due to aseptic loosening.
Causes of surgical revisions.

ALVAL: aseptic lymphocyte vasculitis associated lesions.
a p < 0.05.
The multivariate analyses are presented in Table 3.
Details of multivariate analysis of risk factors for surgical recovery.

THA: total hip arthroplasty; BMI: body mass index.
The Oxford score average was 57.8 ± 6.7 points out of 60 with a minimum of 19 points and a maximum of 60 points (Figure 5). Multivariate analysis did not find any significant difference in the risk of revision, either for age, sex, weight, or acetabular fixation. There was no significant difference between the group of patients with 60 points and those with 30–59 points or less than 30 points.

Oxford score.
Discussion
Our study found a survival of 87% at more than 12 years for revision for all causes and 90.1% for revision for aseptic loosening. The main limitation of our study is its clinical analysis without radiological analysis at the last review. Indeed, the absence of a radiographic study of these prostheses does not make it possible to detect the THAs which have a loosening which could require a surgical resumption, which could alter the survival rate. At the time of inclusion, we decided not to retain some causes of hip osteoarthritis, such as a history of hip dislocation, fracture of the coxofemoral joint, or aseptic osteonecrosis of the femoral head to homogenize our population and to make our results more reproducible because the THAs performed for these secondary arthritis have a higher revision rate 13,14 and are not representative of the majority of cases. We did not include all the THA of our center because we aimed to estimate the survival rate of only the MoM implants since this data is controversial. That is why we included both cemented and cementless implant, the main material studied is the bearing MoM.
Our results are consistent with the literature, which reports an average 10-year survival rate between 90% and 98% (Table 4) for MoM THA. Survival of MoM is equivalent to the other bearing studied regardless of the causes of revision 4,32 –35 or for only revisions for aseptic loosening. 21 However, these studies, when analyzed, often take into account as a survival event the presence of radiological loosening as a failure of THA, which decreases their survival rate. Different types of bearing in the same study often give slightly lower results in terms of survival compared to the others. 30,36
A literature review of the survival rate of the MoM couple with an average follow-up of more than 5 years.
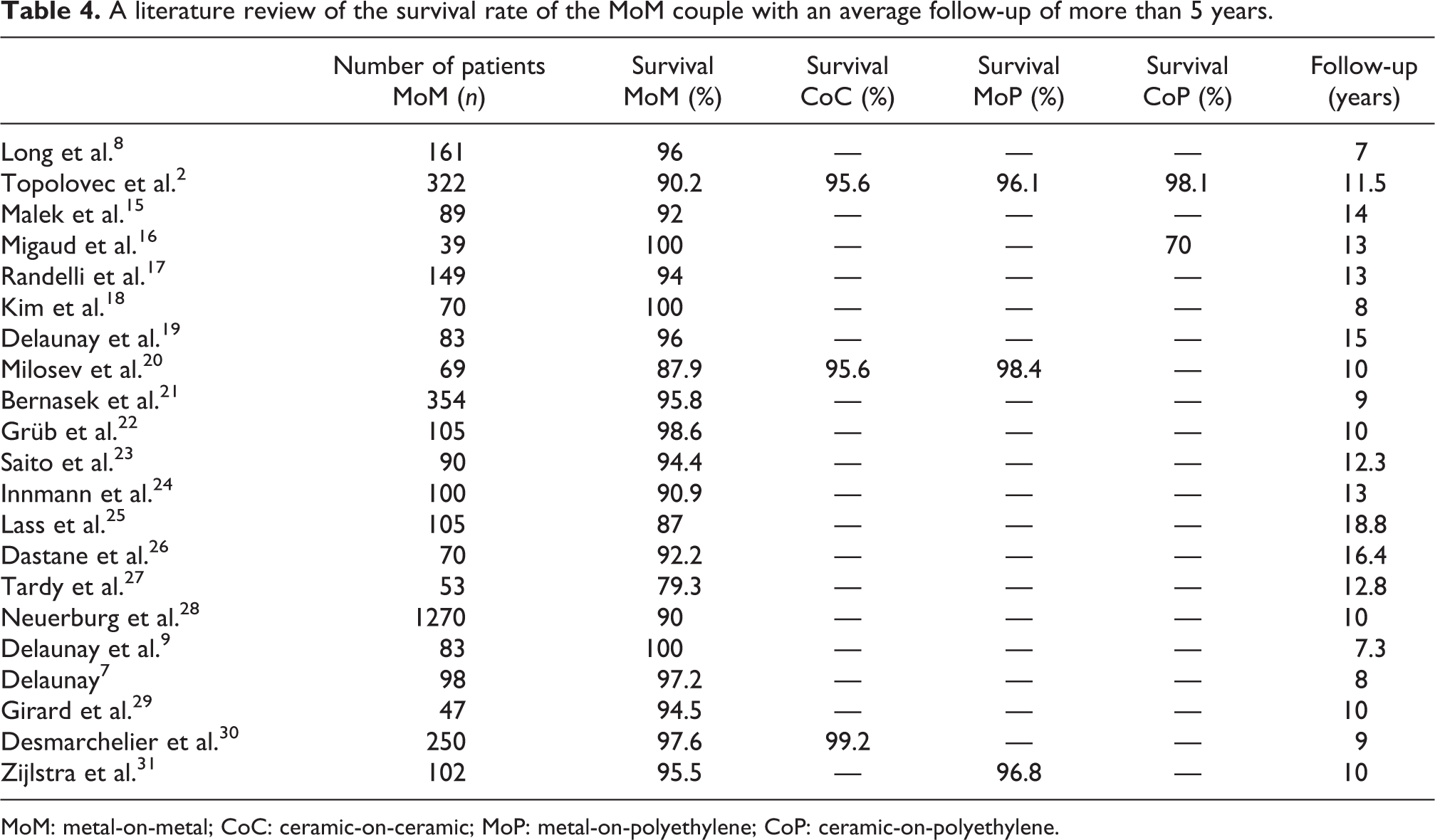
MoM: metal-on-metal; CoC: ceramic-on-ceramic; MoP: metal-on-polyethylene; CoP: ceramic-on-polyethylene.
Concerning the risk of recovery by age, our study found two trends: a higher risk of revision for the patient younger than 40 but with few patients, it is found for several bearings. 37 The second trend found a good survival of our implants in the 40–55 age group with a revision risk identical to the age group of 65–75 years (HR = 1.28 and p = 0.46), results that find other studies. Despite the risk of increased revision in young patients, the MoM seems to give good results. This could be explained by a lower risk of implant breakage than for the CoC couple as well as a lower debris production than the polyethylene-based bearings. 38 A recent meta-analysis found that studies with follow-up of greater than 10 years seem to suggest an increased risk of mortality in MoM THA compared to non-MoM THA. 33
We did not find any difference in survival between men and women for all the causes of revision. However, there is a nearly twice as high risk of loosening in women compared with men for revision for aseptic loosening (HR = 0.45 and p = 0.035), which is confirmed by the literature. 39 We did not find any explanation in the literature or with our study.
We found no difference in BMI, but with an average of 27.6 and only 32 patients with a BMI greater than 35, our obese patient population is surely too small to show a significant difference. The analysis of the literature reflects this problem with a significantly increased risk of revision for BMI >40 40,41 but appears to remain weaker or not seen in cases of BMI <40. 37
In the case of acetabular implants fixation, there was no difference in survival between noncemented and cemented implants (HR = 0.82, p = 0.44), even when using support rings (HR = 1.55, p = 0.66). The comparison with the literature reports divergent results regarding the superiority of one or the other mode of fixation. 22,42 –45 The use of support ring seems to give a good result with a HR of 1.56, p = 0.29 between implants sealed directly and via a ring regarding revision risk. These satisfactory results concerning survival are found in the literature. 29
During the interviews, we have sometimes encountered problems in the elderly patients: many pains limiting the patient but not specifically affecting the hip, low stress on their hip can hide a normally symptomatic THA, or pain difficult to relate to the joint involved (lumbar spine, sciatica, cruralgia, and gonalgia). These difficulties can explain the significant difference in the results concerning this score with those found in the literature, 27,46 concerning the MoM couple. This study has other limitations. In this retrospective review of medical files and phone interviews, the radiological parameters and other complications were not analyzed. Moreover, the concern of metal ion toxicity and adverse local reactions with MoM was not investigated.
Moreover, our study does not find any difference according to age, weight, or sex, probably due to a plateau effect because many patients have the maximum score.
Conclusion
Despite a reputation tarnished by a high rate of early loosening for low-carbon cast implants, the Metasul forged metal–metal with 28 mm heads gives good results over time with a satisfactory survival rate although slightly lower than the other bearings. The MoM couple can be an alternative in young subjects for which MoP poses the problem of the wear of the acetabular insert. CoC is most often preferred because ceramic breakage has become rare. Implantation in young subjects of a MoM couple poses the problem of the monitoring and long-term effects of high blood levels of chromium–cobalt, which over long periods of exposure could increase their toxicity to the body.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
This article was accepted by ethical committee.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Informed consent was obtained from all individual participants included in the study.
