Abstract
Purpose:
We measured the width of the acetabular labra in, and the clinical outcomes of, patients with borderline hip dysplasia (HD) who underwent arthroscopy.
Methods:
A total of 1436 patients who underwent hip arthroscopy to treat symptomatic, acetabular labral tears were enrolled. From this cohort, we extracted a borderline HD group (162 cases). Lateral labral widths were evaluated using preoperative magnetic resonance imaging scans. Clinical data including the modified Harris hip score (mHHS), non-arthritic hip score (NAHS), hip outcome score–activity of daily living (HOS-ADL) score, visual analog scale (VAS) pain score, and Tönnis grade were collected. In addition, patient satisfaction with arthroscopy outcomes was rated. All complications and reoperations were noted.
Results:
The mean follow-up time was 87.4 months. The lateral labral width was 7.64 mm in those with normal hips and 7.73 mm in borderline HD patients, respectively (p = 0.870). The Tönnis grade progressed mildly from 0.46 to 0.76 (p = 0.227). At the last follow-up, clinical outcome scores (mHHS, NAHS, and HOS-ADL scores) and the VAS score were improved (p < 0.001). The mean patient satisfaction was scored at 8.2. The reoperation rate was higher in those who underwent labral debridement (25.6%) than labral repair (4.1%).
Conclusions:
The lateral labral width did not differ significantly between the borderline HD group and the nondysplastic control group. Arthroscopy relieved the symptoms of painful borderline HD and did not accelerate osteoarthritis. Therefore, if such patients do not respond to conservative treatment, hip arthroscopy can be considered for further treatment.
Introduction
The acetabular labrum is a triangular fibrocartilaginous structure attached to the rim of the acetabulum and facilitates hip joint mechanical stability and lubrication. 1,2 The labrum may increase the depth of the acetabulum, thus extending the coverage provided by the femoral head and increasing joint stability. 3,4 Acetabular labral disorders are associated with various pathogeneses including hip trauma, negative effects of high-level sports activities, degenerative osteoarthritis, femoroacetabular impingement (FAI), and hip dysplasia (HD). 5 –9 In HD patients, the decrease in bony coverage may render the femoral head unstable within the acetabulum, increasing the contact stress on the labrum; any labral changes thus caused may predispose patients to the development of paralabral cysts, disorders of the adjacent articular cartilage, and ultimately osteoarthritis. 10,11 HD is associated with increased labral width in the anterosuperior quadrant. 12 A recent finite element analysis model found that, in HD patients, the labrum supported 4–11% of the total load transferred across the joint, whereas in normal subjects, the figure was 1–2%. 13
The hip stability of borderline HD patients is difficult to determine; instability may be underestimated and treatment thus inappropriate. Historically, hip preservation surgery for HD patients featured open procedures such as periacetabular osteotomies (PAO); these effectively treat symptomatic HD, affording excellent results even in the long term. 14 Over the past decade, hip arthroscopy has become an increasingly common orthopedic procedure, indicated for the treatment of pathologies such as FAI and symptomatic labral tears. 15,16 However, isolated hip arthroscopy in an HD setting has been associated with variable outcomes. Some studies reported good outcomes but emphasized that these correlated principally with the type of intra-articular pathology, not dysplasia status. 17 Other studies described poor outcomes, suggesting that hip arthroscopy was not beneficial in dysplastic patients and that surgery might even accelerate arthritic progression. 18
Here, we retrospectively investigated the utility of isolated hip arthroscopy for borderline HD patients with labral tears; we report the clinical outcomes, lateral labral widths, and progression of joint degeneration/secondary osteoarthritis. Also, we defined labral tear morphology and the associated extents of FAI. This allowed us to define indications and contraindications for arthroscopic treatment of patients with symptomatic borderline HD.
Materials and methods
Patient selection
This study was approved by the institutional review board of our institute (CNUH 2018-08-007). Between May 1996 and April 2013, 1436 patients underwent primary hip arthroscopy in our institution to treat symptomatic and acetabular labral tears. Only cases of Tönnis grade
19
0 or 1, with no other hip abnormality evident either from plain radiography or from magnetic resonance imaging (MRI) were included. We excluded patients with (1) a history of high-energy hip trauma (i.e. a fracture or dislocation); (2) a history of surgery involving the femur or pelvis; (3) Tönnis grade ≥2; (4) any proliferative disease of the hip (i.e. synovial chondromatosis, pigmented villonodular synovitis); and/or (5) the Legg–Calvé–Perthes deformity. We identified 162 borderline HD cases (11.3%) using plain radiographs; the lateral center-edge angle (LCEA) of Wiberg in these cases was
Patient demographics.

Patients diagnosed with FAI and arthroscopic procedures for painful borderline hip dysplasia.

FAI: femoroacetabular impingement
Clinical and radiologic evaluations
Clinical and radiographic outcomes were evaluated at a minimum of 5 years (average 87.4 months) postoperatively. Patients who did not attend regularly scheduled visits were contacted by telephone. Clinical evaluations featured calculation of the modified Harris hip score (mHHS), non-arthritic hip score (NAHS), hip outcome score–activities of daily living (HOS-ADL) subscale, and visual analog scale (VAS) score evaluating pain. Patient satisfaction with arthroscopy outcomes was rated on a scale of 1 to 10 (1 = complete dissatisfaction; 10 = complete satisfaction). The radiographs analyzed included anteroposterior views of the pelvis, frog-leg lateral views, and cross-table lateral views of the hip. The Tönnis classification 19 was used to grade degenerative radiographic changes. Computed tomography scan was also performed preoperatively to assess other bony abnormalities of the hip joint. Preoperative MRI scans were employed to measure labral widths and identify intra-articular pathologies. The lateral width of the acetabular labrum was measured at the level of the central coronal MRI scan, cross-referenced to the sagittal and axial planes (Figure 1). 20 During operations, the labral tear morphology was noted. We divided all patients into two types by tear morphology: type 1 patients exhibited tears commencing at the chondrolabral junction and extending down the inner side of the acetabular subchondral bone and type 2 patients exhibited tears at the base or body of the labrum without the extension described above (Figure 2). All complications and reoperations were noted.

Lateral labral width was measured by lateral labrum at the level of the central coronal MRI scan cross referenced to the sagittal and axial planes. MRI: magnetic resonance imaging.

Location of labral tears. (a) type 1: labral tears at chondrolabral junction with labrum extended down to the inner side of acetabular subchondral bone and (b) type 2: labral tears at the base or body of labrum without labrum extended into the inner side of the acetabular subchondral bone.
Surgical technique and postoperative care
All operations were performed by a single senior surgeon (DSH), with all patients under general anesthesia. All patients were placed supine on a standard traction table, and the operative extremity was positioned in slight hip flexion, abducted relative to the pelvis, at 15–20° of hip internal rotation established by applying traction of 8–10 mm. The contralateral extremity was positioned in extension and in neutral rotation, with the foot placed in a support to apply a counterbalancing traction. Countertraction, lateralized toward the operative hip, was established in the perineal region. The procedure usually commenced in the central compartment. A guidewire was inserted into the joint via an anterolateral portal using a puncture needle and a C-arm image intensifier. The portal was dilated, and a 70° scope was inserted. A mid-anterior portal was established under direct outside-in visualization. Sometimes, we created additional portals. After portal setup, diagnostic arthroscopy was performed, and any pathology of the labrum, impingement, and chondral damage or ligamentum teres tears were documented. We sought to preserve as much of the native labrum as possible, using the standard arthroscopic repair technique to this end. If the labrum was found to be incompetent, debridement was performed. Decompression of pincer FAI was minimized to preserve the acetabular cover; decompression of subspinal impingement was performed as required. Thermal shrinkage was performed if a degenerative partial tear of the ligamentum teres was identified. The cartilage of the acetabulum and femoral head was thoroughly assessed, and any pathology treated. Microfracture was performed if a discrete Outerbridge grade IV chondral lesion was identified. After central compartment manipulation, the traction was removed, and the hip was flexed approximately to 40°. We then focused our attention on the peripheral compartment, using a 30° arthroscope to this end. Cam FAI was treated via femoral head-and-neck femoroplasty. Iliopsoas tendon release was performed if internal hip snapping was evident. The operation was completed without capsular closure or plication.
All patients were permitted to engage in partial weight-bearing ambulation using the affected leg for a minimum of 4 weeks; this was extended to 6 weeks in those who experienced microfractures. We also encouraged pendulum exercise and continuous passive motion to avoid postoperative capsulolabral adhesions. A soft hip brace was worn to prevent hip extension and rotation while walking. To control pain and heterotopic ossification, NSAIDs were prescribed for 3–4 weeks.
Statistical analyses
All statistical analyses were performed using IBM SPSS Statistics software (ver. 23.0; IBM Corporation, Armonk, NY, USA). Age, sex, and BMI were compared between the borderline HD patients and the nondysplastic control groups using the independent-samples t-test and χ 2 test. Differences between preoperative and final follow-up clinical features and Tönnis grades were compared using the paired t-test. The lateral labral widths of the borderline HD patients and nondysplastic control groups were compared using the independent-samples t-test. Differences were considered statistically significant if p < 0.05.
Results
Clinical results
From the preoperative stage to the final follow-up, mean mHHS score increased from 62.6 (SD = 7.7, range 37.5–82.0) to 87.4 (SD = 5.3, range 60.0–94.6), mean NAHS score increased from 59.6 (SD = 7.9, range 19–87) to 85.5 (SD = 5.4, range 59–95), and mean HOS-ADL score increased from 60.4% (SD = 4.8%, range 20–80%) to 81.6% (SD = 7.4%, range 45–95%). By contrast, mean VAS score decreased from 6.7 (SD = 0.7, range 3–10) to 2.1 (SD = 1.1, range 0–7). All scores exhibited statistically significant improvements (p < 0.001). At the final follow-up, mHHS scores were >80 (satisfied or very satisfied) in 129 cases (79.6%) and <70 (dissatisfied) in 12 cases (6.7%). Overall, mean patient satisfaction with arthroscopy outcomes was scored at 8.2 (SD = 1.6, scale 1–10) at the final follow-up (Table 3).
Comparison between the preoperative and postoperative latest follow-up clinical outcomes (mean ± SD).
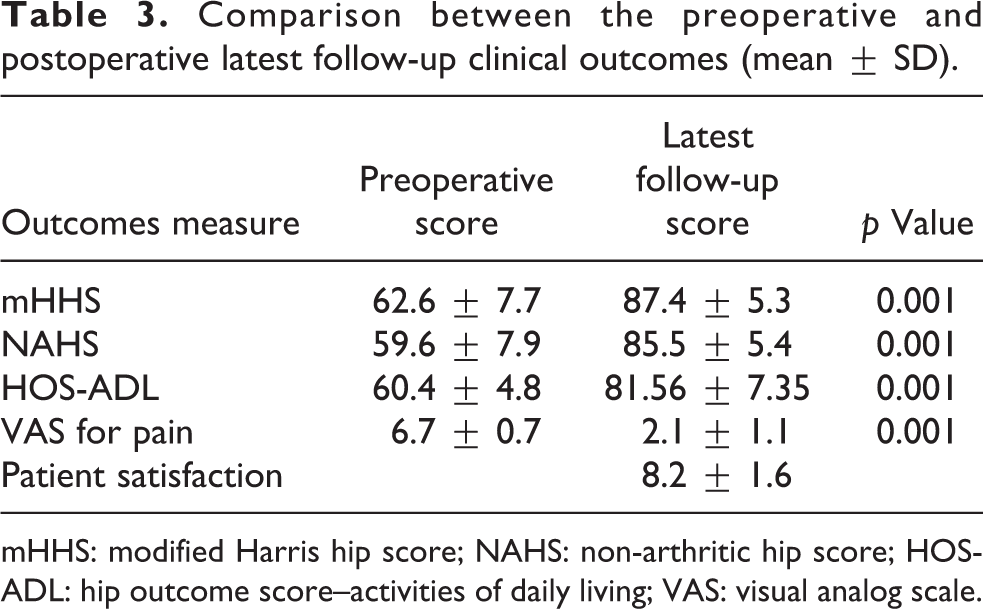
mHHS: modified Harris hip score; NAHS: non-arthritic hip score; HOS-ADL: hip outcome score–activities of daily living; VAS: visual analog scale.
Radiographic results
The mean Wiberg LCEA was 22.3° (SD = 2.0°, range 20.0–24.9°). The mean Tönnis osteoarthritis grade determined using the final and follow-up simple radiograph was 0.76 (SD = 0.39, range 0–3); this did not differ significantly from the mean preoperative grade of 0.46 (SD = 0.21, range 0–1; p = 0.227). The mean lateral labral width measured using MRI scans was 7.73 mm (SD = 1.39 mm) in the borderline HD group and 7.64 mm (SD = 1.49 mm) in the nondysplastic control group; this difference was not significant (p = 0.870). Intraoperatively, type 1 labral tears were observed in 37 cases (22.8%) and type 2 tears in 125 cases (77.2%).
Complications
Although we encountered no significant complications such as infection, deep venous thrombosis, fluid extravasation, or permanent nerve injury, five cases of transient neuropraxia (three at the pudendal nerve and two at the lateral femoral cutaneous nerve) occurred, but all cases were resolved uneventfully within the first week to 6 months after surgery. Fifteen patients (9.26%) underwent revision arthroscopy or conversion to total hip arthroplasty (THA). The labral debridement group (10 of 39 patients, 25.6%) exhibited a higher reoperation rate than the repair group (5 of 123 patients, 5.1%). In the latter group, three patients underwent revision arthroscopy—two cases of labral retearing and one case of incomplete femoroplasty—and two patients underwent conversion to THA because of advanced arthritis. In the debridement group, seven patients underwent revision arthroscopy—four cases of capsulolabral adhesions, two cases of incomplete femoroplasty, and one case of heterotopic ossification—and three patients underwent conversion to THA because of advanced arthritis. Data on all revision arthroscopies and THA conversions are summarized in Table 4.
Revisional arthroscopic procedure and conversion to THA.

THA: total hip arthroplasty.
Discussion
The principal findings of our study are the following: (1) hip arthroscopy is useful for patients with painful borderline HD; (2) the labrum should be maximally preserved (although debridement may be required) to maintain its role as a suction seal, facilitating hip joint stabilization and preventing early joint degeneration; and (3) lateral labral width did not differ between the borderline HD patients and the nondysplastic control groups.
HD is a common congenital condition; it is more common in females than males and is often associated with a family history of hip arthritis. The main feature of HD is a shallow, abnormally shaped, or improperly oriented socket. These anatomical configurations may render the femoral head unstable within the acetabulum. Also, various alterations in femoral shape and orientation are now thought to contribute to hip instability, defined as excessive joint mobility that can cause labral tearing and deterioration of joint articular cartilage. If left untreated, hip instability causes pain, discomfort when walking, progressive hip joint deterioration, and accelerated osteoarthritis. Borderline HD patients with labral tears pose challenges in terms of definitive treatment. Namely, the choice between arthroscopy and periacetabular osteotomy (PAO) is difficult. Patients with limited cartilage damage and spherical hip joints are PAO candidates. PAO reorientates the hip socket, stabilizes the femoral head within the acetabulum, normalizes forces within the hip joint, prevents or dramatically slows joint deterioration, and improves hip symptoms and function. 21,22 However, in patients exhibiting FAI, PAO may exacerbate the condition and is associated with risks of secondary impingement or overcorrection, leading to poor outcomes. 23 –25
Over the past decade, hip arthroscopy has been increasingly used to manage hip pathologies such as FAI and symptomatic labral tears. 15,16 Satisfactory surgical outcomes have been achieved. However, the indications for and outcomes of hip arthroscopy in HD or borderline HD patients have been both inconclusive and controversial. 17,18 Arthroscopy was rapidly adopted to treat HD patients with FAIs and labral injuries, but, in earlier treatments, failure rates were high and pain relief inadequate; also, the procedure may trigger progressive osteoarthritis and/or exacerbate instability symptoms. 26 –28 Parvizi et al. 18 reported the outcomes of 34 patients with symptomatic acetabular dysplasia who underwent hip arthroscopic labral debridement to manage labral tears. Of these, 24 patients (70.6%) experienced failures in terms of pain relief (which was incomplete), and 14 patients also exhibited accelerated arthritis, suggesting that patients with abnormal hip morphologies may not benefit from hip arthroscopy and labral treatment alone. Also, 16 patients required second surgery. Similarly, many studies reported significantly poorer clinical outcomes and increased rates of revision arthroscopy and THA conversion in dysplastic patients compared to nondysplastic patients. 28 –30
By contrast, Domb et al. 31 found that hip arthroscopy effectively treated the labral lesions of borderline HD patients. The injuries were repaired, and capsular plications were performed at the interportal capsulotomy, to reduce the later incidence of iatrogenic instability. Patient-reported mHHS, NAHS, HOS-SSS, and HOS-ADL scores improved significantly, and overall patient satisfaction was rated as good or excellent (77%). Two patients (9%) required revision arthroscopy. Thus, borderline HD patients could be successfully managed via hip arthroscopy when a consistent surgical approach—including both labral repair and capsular plication—was applied. Similarly, Byrd and Jones 17 reported on a series of 48 patients with either dysplasia (16) or borderline dysplasia (32); all patients exhibited labral injuries and underwent arthroscopy, minimal debridement, and/or maximal labral preservation. The mHHS scores improved significantly for all patients, with 79% (38 patients) reporting improvements of ≥10 points. Only two patients underwent conversion to THA. Thus, arthroscopic success rate depended on the underlying intra-articular pathology and not on acetabular dysplasia status. We did not perform capsular closure or plication, but patient outcomes improved significantly nonetheless. This was likely because we performed minimal interportal capsulotomy without T-capsulotomy. Also, to stabilize soft tissues around the hip joint, we placed a soft hip brace to prevent hip joint extension and rotation and permitted only partial weight-bearing for 4–6 weeks. Another possible explanation of our good clinical outcomes is that healthy labra were maximally repaired and other intra-articular hip pathologies treated during arthroscopy. However, isolated hip arthroscopy may require caution for dysplastic hips. For example, Ricciardi et al. 32 reported that failure of hip arthroscopic surgery prior to PAO to treat symptomatic HD was associated with poorer hip-specific functional outcomes.
Labral enlargement in HD patients is evident both in MRI scans 12,20,33 –35 and during surgery. 18,36,37 Mild forms of HD may not develop until adulthood. However, in such patients, the labrum imparts crucial stability to a borderline HD; labral arthroscopic debridement or resection can therefore trigger fulminant (thus, very negative) clinical outcomes. 18,31,36 Labral enlargement may afford better joint surface congruence and deepen the acetabular fossa, contributing to hip joint stability. 2,4,18 Both we and others found that labral debridement patients (25.6%) required more revision arthroscopies and underwent more THA conversions than labral repair patients (5.1%). However, lateral labral width measured using MRI scans did not differ significantly between the borderline HD patients (7.73 ± 1.39 mm) and the nondysplastic control group (7.64 ± 1.49 mm; p = 0.870), probably because the labra of former patients did not contribute greatly to acetabular hip stabilization (in contrast to patients with severe dysplasia). The constraints imposed by various soft tissues also afforded adequate hip stability. Additionally, in unstable, borderline HD patients, the labrum may extend to the inner side of the acetabular subchondral bone—thus, reducing hip stress—and may become injured at the point where the chondrolabral junction extends into the hip joint because of low bony coverage in this region and increased contact stress. We identified 37 cases (22.8%) of type 1 labral tears; these were probably borderline HD patients with unstable hips. Future work should explore labral morphological and injury patterns in patients with severe HD.
A limitation of our study is that all cases were treated by a single surgeon for a broad duration of time. Our results may thus not apply to all hip arthroscopic series of borderline HD patients, due to selection and performance biases. Second, we did not perform a prospective cohort study; retrospective studies often suffer from data inaccuracies or absences. Third, assessing HD is complex and requires multiple radiographic measurements. Our study focused on only LCEA to assess borderline HD, it can mischaracterize or underdiagnose the acetabular morphology and hip instability. Fourth, the radiological evaluations of borderline HD status and lateral labral widths were subjective. However, to enhance objectivity, all evaluations were performed by a single radiologist and two board-certified orthopedic surgeons. Despite these limitations, our patient numbers were relatively large and our follow-up period is the longest reported to date. Also, to the best of our knowledge, this is the first work to show that the lateral labral width does not differ between the borderline HD and the nondysplastic patients. Future, well-controlled prospective studies are required to further explore the prognostic implications of our findings.
Conclusions
The lateral labral width did not differ significantly between the borderline HD group and the nondysplastic control group. Arthroscopic treatment relieved symptoms and did not accelerate osteoarthritis development in those with painful borderline HD. Therefore, if patients with painful borderline HD do not respond to conservative treatment, hip arthroscopy is a useful option.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
