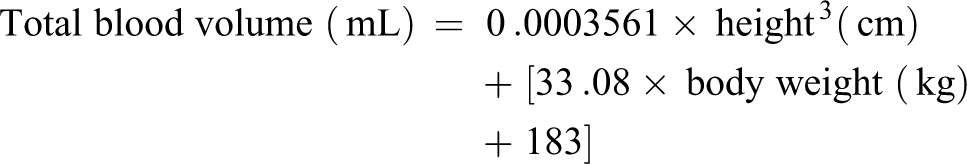Abstract
Purpose:
Concerning the ongoing debate on the effects of continuing aspirin therapy on blood loss in knee arthroplasty, we conducted a retrospective investigation to test the hypothesis that continuation of aspirin prior total knee arthroplasty (TKA) will not cause more blood loss.
Methods:
From a database of patients who underwent unilateral TKA between 2011 and 2016, we identified two groups: the aspirin group (patients continued aspirin during perioperative period) and the nonaspirin group (patients had no current or recent history of aspirin usage). We extracted and compared patient demographic information, comorbidity index, baseline serum hemoglobin (Hb), and creatinine level between the two groups. We also compared our primary outcomes, including the total blood loss, transfusion requirement, and length of hospitalization between the two groups. A multivariate logistic regression for analyzing the risk factors of requiring transfusion was performed.
Results:
We found that apart from preoperative serum creatinine level, there was no difference in the baseline Hb level, perioperative change in Hb, total blood loss, or length of hospitalization between the two groups. The percentage of transfusion utilization was also comparable between the two groups. Our regression analysis shows that the risk of requiring transfusion after TKA is not significantly associated with patients taking aspirin therapy before operation.
Conclusion:
Patients who underwent TKA with continuation of low-dose aspirin did not result in more blood loss. Current blood loss management has provided sufficient reduction of blood loss to accommodate aspirin therapy perioperatively. We suggest that it is safe to continue aspirin prior to TKA.
Introduction
It is widely accepted that total knee arthroplasty (TKA) is associated with significant perioperative bleeding, which may lead to serious complications such as anemia, increased length of stay, hematoma, infection, and even death in rare occasions. 1 As reported in various studies, a total of 1000–2000 mL blood loss, 2 –5 which is composed of visible and hidden blood loss reflected by a change in perioperative hemoglobin (Hb) and transfusion need, during TKA was frequently observed. 4,6 –8 Among various blood-replenish remedies, transfusion of packed red blood cell is commonly utilized when the postoperative serum Hb drops below a critical point, but it is associated with various adverse events such as allergic reactions, acute lung injury, infectious diseases transmission, and immunosuppression. 1,9 –11
Aspirin is commonly used for primary or secondary prevention of cardiovascular diseases, as it inhibits the aggregation of platelet by the irreversible acetylation of cyclooxygenase, thus interfering with the ability of platelet to produce prostaglandin. 12,13 This effect persists across the life span of platelet, which is around 10 days. 14 However, preoperative continuation of aspirin or antiplatelet therapy in general has been found to increase postoperative blood loss and transfusion utilization significantly in patients who underwent elective coronary artery bypass graft surgery. 15 –17 A few studies also reported a significant association between bleeding events (minor or major) and preoperative aspirin continuation. 8,18 On the other hand, acute discontinuation of aspirin therapy can be a problem. Previous studies observed that preoperative aspirin withdrawal was associated with an increase in the risk of arterial and venous thrombotic events because discontinuation of aspirin causes the platelet rebound phenomenon characterized by increased thromboxane and decreased fibrinolysis. 19 –23
The American Academy of Orthopedics Surgeons (AAOS) recommends discontinuation of aspirin before elective knee arthroplasty (moderate recommendation grade). 8 However, this recommendation was developed based on findings of non-arthroplasty clinical trials, 15 –17 because studies directly investigating the effect of preoperative aspirin therapy on postoperative blood loss after knee arthroplasty are scarce in the current literature. 24
Therefore, we conducted a retrospective comparative study of patients who underwent TKA in a tertiary hospital to assess the effects of low-dose aspirin on postoperative blood loss, transfusion utilization, and length of hospitalization after TKA surgery. We hypothesized that continuation of low-dose aspirin is not associated with increased blood loss after TKA surgery.
Materials and methods
Samples
In this study, patients were selected based on the following inclusion/exclusion criteria.
Between May 2011 and March 2016, all patients who were diagnosed with osteoarthritis of the knee and underwent unilateral TKA surgery by the senior author (SJY) at a tertiary hospital were eligible in this study. However, if the patient met any of the exclusion criteria, he/she would be excluded. The exclusion criteria included revision TKA, simultaneous bilateral TKA (BTKA), known history of bleeding disorder, presence of metallic hardware of the same knee joint, diagnosis other than osteoarthritis, and use of other anticoagulants medicine before surgery.
A medial parapatellar quadriceps splitting approach with patella subluxation was used. The proximal tibia was prepared with an extramedullary guide. The distal femur was prepared with an intramedullary rod and the intramedullary femoral canal was subsequently plugged with the autologous bone graft. To ensure consistent quality of implants, we used the same cruciate-retaining implants and total knee replacement system from the Depuy Synthes PFC Sigma® (Warsaw, Indiana, USA) for all patients. 2,25 From postoperative day 1, 40 mg low-molecular-weight heparin (LMWH) was administrated for venous thromboembolic event prophylaxis.
Multimodal blood management protocol
For all the participants, we performed multimodal blood loss management which included administration of 1.5 g intraarticular tranexamic acid wash and using warming blanket to prevent hypothermia. In addition, the tourniquet was inflated to 300 mmHg 26 before incision and released after skin closure. No surgical drain was used.
Data collection
For all the included patients, medical records were retrieved from the hospital electronic information system and inpatient notes. Patient demographic information including age, gender, and body mass index (BMI) was extracted from medical records. Preoperative comorbidities were assessed by age-adjusted Charlson’s comorbidity index (ACCI). 27 –29 Baseline preoperative serum Hb and creatinine levels measured one day prior to operation were recorded. Additionally, we extracted postoperative Hb one day after operation for both groups.
Data were cross-checked and validated before analysis. Based on the status of preoperative aspirin therapy, patients were divided into two groups: the aspirin group included patients who continued taking low-dose (100 mg) aspirin for prevention of cardiovascular diseases during perioperative phase and the nonaspirin group consisted of patients without history of current or recent aspirin therapy.
Our primary outcomes are (1) difference in preoperative and postoperative Hb level, (2) uncompensated blood loss, (3) total blood loss, (4) percentage of requiring transfusion, and (5) participants’ length of hospitalization after operation.
Total blood loss, which consists of visible and hidden blood loss, was estimated from compensated and uncompensated blood loss using the following formula 30 :
The compensated blood loss was determined by the total volume of blood product transfusion. Our hospital followed the American Association of Blood Banks clinical guideline on transfusion: patients with Hb below 8.0 g/dL were considered for transfusion. 4,31
Additionally, total blood volume was calculated separately for men and women using the following formula:
Men:
Women:
Statistical analysis
The demographic and baseline features of participants were analyzed and compared using descriptive statistics for both groups. To address our study objectives, we compared the primary outcomes between the aspirin group and the nonaspirin group. Normality of all continuous variables was assessed with the Shapiro–Wilk test before the comparison. For nonparametric variables, medians were compared by the Mann–Whitney U-test. Student’s unpaired t-test was used for comparing means of normally distributed continuous variables. Comparison of discrete variables between the two groups was done with Pearson’s χ 2 test.
Additionally, to investigate whether aspirin use is a risk factor for requiring transfusion after TAK, we conducted a multivariable logistic regression analysis to assess the association between the outcome variable (whether patients required transfusion after TKA) and the independent variable of our interests (patient status of under preoperative aspirin therapy), while adjusting for confounders such as age, gender, BMI, preoperative Hb and creatinine level, length of hospitalization, and ACCI. All statistical analysis was performed using STATA 14.1 (StataCorp, College Station, Texas, USA), and a statistical significant level was set at p < 0.05.
Results
Demographic and baseline characteristics
Between 2011 and 2016, a total of 837 patients underwent primary TKA by the senior author (SJY), among which 22 patients who had simultaneous BTKA and 38 patients on other anticoagulant therapy were excluded. The demographic characteristics of the remaining 77 patients on aspirin therapy and the 700 without current or previous history of aspirin therapy are presented in Table 1. There was no significant difference in age, gender, BMI, preoperative serum Hb level, and ACCI score between the two groups. However, the preoperative serum creatinine was higher in the aspirin group than in nonaspirin group by 6 g/dL (p = 0.002).
Demographic and baseline information of study participants.

ACCI: age-adjusted Charlson’s comorbidity index; BMI: body mass index; SD: standard deviation; IQR: interquartile range.
a The value of p < 0.05 is statistically significant.
Primary outcomes
No significant difference was observed between the aspirin and nonaspirin groups in baseline preoperative Hb level, change in perioperative Hb, uncompensated blood loss, total blood loss, or length of hospitalization between the aspirin and nonaspirin groups (Table 2). The percentage of requiring transfusion among the aspirin group was higher than the nonaspirin group by 3%, but no statistical significance was achieved (p = 0.077).
Comparison of primary outcomes between the two groups.

Hb: hemoglobin; IQR: interquartile range.
Risk of requiring transfusion after TKA between patients with and without aspirin
In the multivariate logistic regression analyses (Table 3), we observed that the risk of patients requiring postoperative transfusion was not significantly different between the aspirin and nonaspirin groups (adjusted odds ratio (OR) 1.833; 95% confidence interval (CI) 0.327, 10.285) after adjusting for other confounders. Additionally, patients with higher ACCI score tended to have significantly higher risk of transfusion (adjusted OR 1.686; 95% CI 1.112, 2.557). Age, female gender, low preoperative Hb, and high preoperative creatinine concentration were not significant risk factors for transfusion after TKA.
Risk of requiring transfusion after TKA surgery.

TKA: total knee arthroplasty; BMI: body mass index; ACCI: age-adjusted Charlson’s comorbidity index; Preop Hb: preoperative hemoglobin level; Preop creatinine: preoperative serum creatinine level; OR: odds ratio; CI: confidence interval.
a The value of p < 0.05 is statistically significant.
Discussion
To date, our study is the largest single surgeon series that investigated the effect of aspirin therapy on blood loss and transfusion requirement in patients who underwent TKA. Align with our hypothesis, we found that no differences between patients on aspirin therapy and those without current or history of aspirin therapy in terms of total and uncompensated blood loss, transfusion requirement, and length of hospitalization were observed.
The current AAOS guidelines on preoperative aspirin use were developed based on three non-arthroplasty studies, where preoperative aspirin use was found with more perioperative blood loss. 8,15 –17 However, the strength of evidence supporting this recommendation was “moderate” due to the limitations in the studies; therefore, the applicability of this recommendation is still controversial and further research is needed to strengthen the evidence base for recommendations on preoperative aspirin use. 8
Unlike the three non-arthroplasty studies referenced in the guidelines, we examined the effects of preoperative aspirin use among TKA surgical patients, therefore providing additional evidence to the existing knowledge. Furthermore, our results are supported by a similar study conducted by Schwab et al., 24 which also observed nonsignificant differences in total blood loss, length of hospitalization, and transfusion requirement between the aspirin and nonaspirin groups. However, unlike Schwab’s study that included mixed cases of TKA and unicompartmental knee arthroplasty, we only selected patients underwent TKA surgery and a low-dose (100 mg) aspirin was taken by all the included patients. Additionally, Schwab el al. 24 only analyzed the absolute number of patients who were transfused, rather than the ratio of transfusion as we did in our study.
Similar to other major operations, TKA is associated with both the risks of bleeding and thromboembolic events. 32 Current available guidelines recognize and emphasize the risk of bleeding and recommend withdrawing aspirin 1 week prior to TKA 8,32 ; however, sudden discontinuation of aspirin therapy may lead to abrupt aggregation of platelets and thromboembolic events. Based on the findings from our study, we believe that low-dose aspirin therapy for prevention of thromboembolic events can be continued during the perioperative period of TKA with modern multimodal blood management, including minimally invasive surgical approach, intraarticular tranexamic acid wash, and use of warming blanket and tourniquet.
There are a few limitations of this study. Firstly, this is a retrospective study and the strength of evidence is limited by the nature of the study. Findings of this study need to be confirmed with future prospective trials with higher level of evidence. Secondly, there are inherent selection and observer biases as patients recruited are from a single hospital. Future multicentered trials will be required to reduce these biases. In addition, all patients received deep vein thrombosis prophylactic agent: LMWH. Despite taking LMWH, there was no difference noted in postoperative blood loss between the aspirin and nonaspirin groups. Another limitation was that we did not analyze the postoperative complications other than blood loss and transfusion requirement, as all patients were admitted for elective TKA and only came in when the preoperative conditions were optimized. In our analysis, the ACCI assessing preoperative comorbidity was comparable between the two groups. Previous study did not report any difference in terms of postoperative complications between aspirin and nonaspirin groups. 24
All patients on aspirin were taking the same dosage of aspirin for prevention of thromboembolic events. The postoperative Hb level was uniformly measured at postoperation day 1, which was sufficient for Hb equilibration after acute blood loss, transfusion, and fluid infusion. 33 Another strength of our study was that the Hb balance method took into account of both explicit and hidden blood loss and has been validated in TKA and other orthopedic surgeries. 33
Conclusion
With the advancement of modern multimodal blood management in TKA, continuing low-dose aspirin therapy prior to surgery does not significantly increase blood loss and the risk for requiring transfusion after operation. Therefore, we recommend that current clinical guidelines should reconsider the decision on the use of aspirin prior to TKA surgery.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
The study was approved by our hospital’s ethics committee and conducted in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki.