Abstract
Background:
Traditional anteromedial incision for pilon fractures would further increase the damage to the subcutaneous tissues anterior and medial to tibia. In this study, we retrospectively evaluated the method and the outcomes of lateral approach for surgical treatment of Gustilo type-I and type-II open pilon fractures with medial soft tissue injuries.
Methods:
From May 2014 to September 2017, 35 patients with Gustilo type-I and type-II open pilon fractures were treated with standard protocol using a lateral approach. The initial wound debridement and application of a spanning external fixator or traction of calcaneal tubercle were performed within 24 h and a definitive fixation was performed when the wound was healed. The mean time from primary surgery to definite surgery was 11.8 (range: 8–16) days. Postoperative radiographs, complications, bone union, and American Orthopedic Foot and Ankle Society (AOFAS) ankle/hind foot score were recorded.
Results:
The mean follow-up period was 17 months (range: 13–23). The average time to bone union was 22 weeks (range: 18–25). In 35 patients, 2 patients had a superficial wound infection and another 1 patient showed limitation of ankle joint motion. No cases of deep infection, skin necrosis, and symptomatic implant reported. The mean AOFAS score was 89.8 (range: 84–95). On final outcome, 25 patients come under excellent and 10 patients had good result.
Conclusion:
From the results of this study, we can conclude that the lateral approach to treat Gustilo type-I and type-II open pilon fractures was a safe option with a low complication rate. On the other hand, it provides sufficient exposure to restore anatomic articulation, which is worthy of clinical recommendation.
Introduction
Traditional anteromedial approach is popular in the surgical treatment of pilon fractures. This approach provides access to the medial malleolus, the medial and middle thirds of the anterior tibiotalar joint. 1 However, pilon fractures are generally a result of high-energy trauma and significant soft tissue injury is frequently present. As the skin on the medial side of tibia is thin, so an open wound is usually found on the medial side. 2 Anteromedial approach would further damage the blood supply of the medial skin flap. The incidence of wound complications and deep infections of anteromedial approach has been reported as high as 55%. 3
In many cases, external fixation is chosen for open fractures. However, the incidence of post-traumatic arthritis and joint stiffness remains high and functional recovery is poor. 4,5 Selection of a suitable operative approach can provide rigid internal fixation and early functional rehabilitation for open pilon fractures with severe medial soft tissue injuries. An anterolateral incision for pilon fractures has been previously described and this approach has excellent visualization of articular surface without intervention to the soft tissue medial to tibial. 6 However, when the fixation of fibular fracture is needed, another incision along the fibular is made. Two approaches can lead to more soft tissue damage, followed by a high rate of infection and necrosis. 7,8 In recent years, many authors reported the treatment of open distal tibia and fibula fractures by single lateral incision and achieved good clinical results. Good visualization of the distal tibial joint surface and fixation of both the tibia and fibula could be obtained through a single lateral incision. 9,10 However, there were few reports for application of this approach in open pilon fractures associated with medial soft tissue injuries. Thus, in this study, we retrospectively analyzed the treatment results of 35 patients with Gustilo type-I and type-II open pilon fractures treated with open reduction and internal fixation using a lateral approach.
Patients and methods
The patients treated in our hospital from May 2014 to September 2017 for Gustilo type-I and type-II open pilon fractures with severe medial soft tissue injuries (medial open wound did not exceed the posterior edge of the tibia) at the same level were included in the present study. We excluded pediatric patients; patients with diabetes and severe vascular disease; patients with Gustilo type-III open fractures; patients with medial comminution, medial crush with impaction at the medial shoulder of the joint, or varus deformity; and patients with anterolateral tibia soft tissue injury. For pilon fractures with medial comminution, an anteromedial approach was performed and a buttress plate was placed on the medial side of tibial.
Ethics approval and informed consent
This study was conducted in accordance with the declaration of Helsinki. This study was conducted with approval from the Ethics Committee of the Second Affiliated Hospital of Anhui Medical University. Written informed consent was obtained from all participants.
Initial management
The initial wound lavage, debridement, and external fixation or traction of calcaneal tubercle were performed within 24 h. After the wound healing with no sign of infection, open reduction and internal fixation was performed. The mean time from primary surgery to definite surgery was 11.8 (range: 8–16) days. Prior to surgery, three-dimensional computed tomography scanning reconstruction around the ankle joint and the order of surgical reduction were designed.
Surgical technique
All patients were in supine position, and the ankle joint line, lateral malleolus fracture line, and anterior border of the fibula were marked on the skin. Surgical incision was made 4 cm proximal to the lateral malleolus fracture and extended along the anterior border of the fibula to the fourth metatarsal base (Figures 3(b) and 5(a)). Once the incision was made, superficial peroneal nerve should be identified and protected especially at the proximal side of the incision. The incision curved at different level according to the level of lateral malleolus fracture line. For Denis–Weber type-B and type-C lateral malleolus fracture, in which fibular fracture line was above or through the level of the tibiofibular ligament, incision curved at the level of the ankle joint. For type-A lateral malleolus fracture, in which fibular fracture line was below the level of the tibiofibular ligament, the incision curved at 1 cm distal to the level of ankle joint for conveniently exposing the distal of lateral malleolus and reducing the skin tension that causes skin necrosis.
The superficial fascia was opened and then the extensor retinaculum was cut at lateral tibial margin. The tibia was visualized between the distal tibial extensor muscle and interosseous membrane, and a submuscular tunnel was created using a large elevator or finger. The peroneal artery was identified and ligated. Then the extensor muscles and the skin were retracted to the medial side with a Hoffman retractor and the articular surface was visualized after opening the articular capsule from the lateral to medial malleolus. Kirschner pins were placed at the talus and the proximal of tibia fracture; later, a retractor was used to maintain the length and alignment of the foreleg and to facilitate the reduction of the tibia.
According to the traditional reduction sequence of pilon fractures, the lateral malleolus fracture was fixed firstly. Fixation of tibia fracture was based on fracture type. For Ruedi–Allgower type-I and type-II pilon fractures, the tibia was fixated with an anterolateral tibial locking plate through the above lateral approach. For type-III pilon fractures, however, it was difficult for reduction of the posterior and medial fragment through lateral approach. Thus, we put the affected limb to the “figure of 4” position and made a small incision along the posterior edge of the tibia for reduction and temporary fixation of the posterior and medial fragment using Kirschner wire (Figure 1). Then, we dealt with the anterior fragment and the articular surface was restored under the direct view. The plate was placed through the anterolateral incision after the reduction of anterior fragment (typical cases in Figures 2 to 5)

With the patient in supine position, the affected limb was placed in the “figure of 4” front position for performing posteromedial approach.

A 45-year-old man sustained a left open pilon fracture and fibular fracture and a length of 4 cm wound exited around the medial side of ankle (Ruedi–Allgower type III and Gustilo–Anderson type II). Thorough debridement and traction of calcaneal tubercle were applied within 24 h.

(a) The wound in Figure 2 healed 2 weeks after initial management and further definitive fixation was performed. (b) Skin incision for the anterolateral approach. Surgical incision is made 4 cm proximal to the lateral malleolus fracture and extended along the anterior border of the fibula to the fourth metatarsal base. (c) The superficial fascia was opened without separating superficial peroneal nerve. (d) The extensor retinaculum was cut at lateral tibia margin level, then the tibia fracture line was visualized between the distal tibia extensor muscle and interosseous membrane. (e) With the assistant of the distractor, the entire articular surface could be visualized. (f) Definitive fixation for both tibia and fibula could be performed in a lateral approach. Postoperative AP (g) and lateral radiographs (h) showed satisfactory reduction of articular surface and fixation of tibia and fibula. AP (i) and lateral radiographs (j) at 1-year follow-up showed fracture healing. (k) and (l) Satisfactory function of affected ankle joint at 1-year follow-up. AP: anteroposterior.

A 38-year-old man sustained a left open pilon fracture and fibular fracture and a length of 4 cm wound exited around the medial side of ankle (Ruedi–Allgower type III and Gustilo–Anderson type II). Thorough debridement and ankle-spanning bridge external fixator were applied within 24 h.
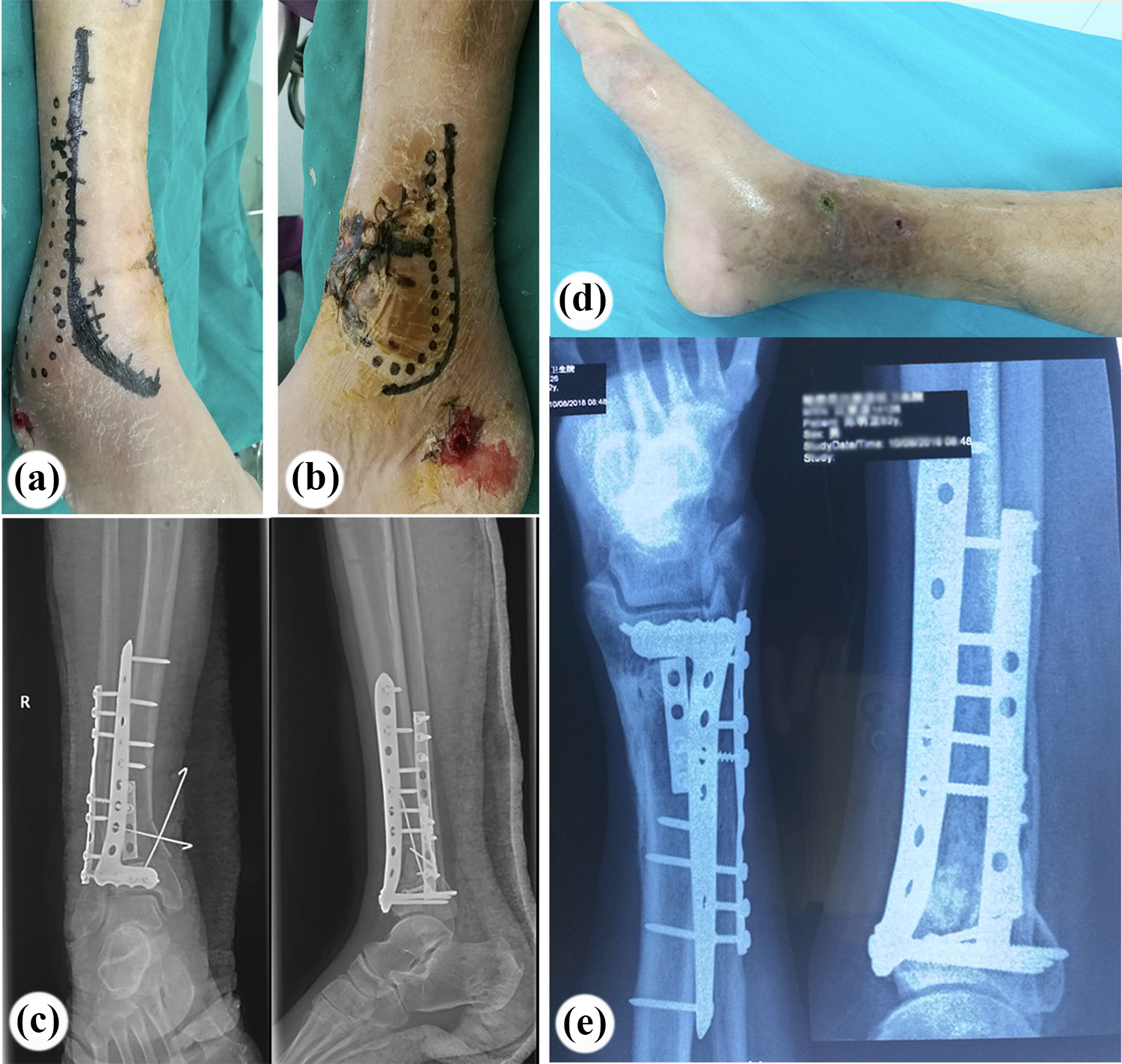
When the wound of patient in Figure 4 healed with no sign of infection after 14 days, pilon fracture was treated with open reduction and internal fixation through anterolateral approach combined with posteromedial approach. (a) Skin incision for the anterolateral approach. (b) Skin incision for the posteromedial approach. Avoiding the area of medial soft tissue injury, the incision was made along the posterior edge of the tibia for reduction and fixation of the posterior and medial fragment. (c) AP and lateral radiograph after fixation of plates. (d) Medial incision healed with no infection at first month follow-up after operation. (e) The bone healed at 1-year follow-up after operation. AP: anteroposterior.
Once stable and anatomic reduction was obtained, the wound was thoroughly irrigated. Wounds were closed over a drain. The joint capsule and the extensor retinaculum were first closed to prevent the occurrence of the string effect.
Postoperatively, a posterior splint was applied to the ankle joint in the neutral position for 2 days. A full range of movement of ankle joint was allowed 3–5 days after surgery. Four to six weeks after surgery, partial weight-bearing was encouraged depending on reconstruction stability. Radiographic evaluation was performed using anteroposterior and lateral radiographs at the time of patient admission, immediately postoperatively and after at least 1–12 months of follow-up. We evaluated time to union, range of motion of the ankle, wound healing, complications, and American Orthopedic Foot and Ankle Society (AOFAS) ankle–hind foot score.
Results
For the 35 patients meeting the eligibility criteria, the mean age was 45 (range: 25–64) years and 4 were females. The cause of the fracture was as follows: 16 cases were from traffic accidents, 17 were a fall from height, and 2 were from machine stretch/contusion injuries. Twenty-two patients had an associated fibular fracture. According to the Ruedi–Allgower classification for pilon fractures, 8 cases were classified as type I, 12 cases as type II, and 15 cases as type III. Accordance with the Gustilo–Anderson classification for open injuries, 15 cases were classified as type I and 20 cases as type II. The mean follow-up period was 17 (range: 13–23) months. Bone union was achieved in all cases. The average time to bone union was 22 (range: 18–25) weeks.
All patients in this group successfully got wound healing, and no cases of deep infection, skin necrosis, and symptomatic implant. In 35 patients, 2 patients had a superficial wound infection and another 1 patient showed limitation of ankle joint motion.
The mean AOFAS foot and ankle score was 89.8 (range: 84–95). On final outcome, 25 patients come under excellent and 10 patients with good result. No patient showed evidence of neurovascular injury or shortening of the tibia. No cases of varus/varus deformity were found.
Discussion
Pilon fracture is a common fracture in trauma orthopedics and most of them are high-energy injury involving the distal tibial joint surface accompanied by fibular fractures and severe soft tissue injuries. 11,12 The treatment effects are often not satisfactory. The main postoperative complications include incision infection, skin necrosis, traumatic arthritis, and varus deformity. 13,14 Especially when soft tissue injuries are in the medial side of the tibia, treatment is more challenging. 15,16 From the perspective of soft tissue preservation, some scholars suggested the external fixation as the ultimate treatment for open pilon fractures and practice has proved that external fixation was a safe and effective treatment. However, problems such as the limitation of joint activities, post ankylosis, pin tract infection, and inconvenience of patient care were hard to be solved. 17,18 Thus, choosing a safe approach for open reduction and internal fixation of open pilon fractures is beneficial to the recovery of the patient’s function. This study we performed a retrospective review of 35 patients treated with Open Reduction and Internal Fixation (ORIF) of Gustilo type-I and type-II pilon fracture that were operated through a lateral approach. All cases achieved bony union with an average period of 22 weeks, and mean AOFAS ankle–hind foot score was 89.8. A lateral approach in the treatment of pilon fracture with the medial open injury provides accurate reduction of articular facets with less intervention of medial soft tissue.
The traditional anteromedial approach for pilon fractures mainly exposes the internal fragment of the distal tibia fracture and part of the medial malleolus fracture. 19 However, the subcutaneous soft tissue on the medial side of the distal tibia is thin, and it is close to periosteal bone, because of this, soft tissue complications are common when performing this approach. In particular, when medial plate was used for open pilon fracture with medial side wound and extensive soft tissue injury, the complications like skin necrosis and plate exposure would occur. 15 In addition, through the anteromedial incision, it is difficult to expose lateral column and therefore requires excessive traction on the fragile soft tissues to adequately visualize and reduce the Chaput fragment to perform the lateral plating; hence, it is not suitable for such fractures. 20 Furthermore, if fibular fracture is present, then a second lateral incision is needed accompanying with the anteromedial approach.
Previous series suggested that lateral or anterolateral approach did not allow access to posterior fragments and did not allow for visualization of the articular surface. 21 However, an anterolateral incision centered between the tibia and fibula was described and detailed in reduction strategies by Mehta et al. in 2011 for exposure and fixation of Association of Internal Fixation (AO)/Orthopaedic Trauma Association (OTA) type-B and type-C pilon fractures. 6 They suggested the contrary that an extensile anterolateral exposure with a defined reduction strategy allowed for accurate reduction of the entire tibia plafond with the exception of impaction at the medial shoulder of the distal tibia. With the assistant of the universal retractor and intraoperative imaging, the entire articular surface could be visualized, reduced, and stabilized. Compared to above anterolateral approach, a direct lateral approach over the anterior edge of fibula was performed in our study for open pilon fractures with medial soft tissue injuries. Both approaches got access to the distal tibia fracture and Chaput fragment through the gap of anterolateral tibia extensor and tibia periosteal exposure without overstretch of soft tissue. When addressing the medial or posterior fragment, we used a small posteromedial approach to reduce and fix these fractures. In difference with above anterolateral approach, the direct lateral approach can be used as a single incision technique, permitting access to the fibula and anterocentral and anterolateral tibial plafond without a second incision over the posterior edge of fibula.
This direct lateral approach was first applied in pilon fractures by David et al. with the goal of creating a single, more robust flap for fixation of both the fibula and tibia. 22 Here, 44 cases of pilon fractures were surgically treated with a direct lateral approach. An anatomic or good fracture reduction was achieved in 41 fractures (93%) and a low rate of wound complications happened with a wound dehiscence in 2 cases (2/44, 4.5%) and a deep infection in 2 cases (2/44, 4.5%). Consider the advantage of this approach in managing soft tissue issues, we further applied this approach for treatment of Gustilo type-I and type-II open pilon fractures with medial soft tissue injuries in 35 cases. All patients got a mean follow-up of 17 (range: 13–23) months. No cases of infection, skin necrosis, or the symptomatic implants occurred at the last follow-up. These results were comparable to previous reports using different approaches. 23 Besides, we further detailed the distal extension of this lateral approach for convenient exposure and fixation of the lateral malleolus fracture. We suggested that this incision curved at the level of the ankle joint for Denis–Weber type-B and type-C lateral malleolus fracture, while it curved at the level of 1 cm distal to the level of ankle joint for type-A lateral malleolus fracture.
In this study, we suggested that a “figure of 4” position of affected limb with a posteromedial approach was convenient for reduction and fixation of the posterior and medial fragment. Traditionally, floating position was required when performing anteromedial approach combined with posterior lateral approach for treatment of Ruedi–Allgower type-III pilon fractures. 24 Reduction of lateral malleolus and posterior fracture was firstly performed through lateral position and then medial fragments were displaced through supine position. However, if the reduction of lateral malleolus and posterior fracture was not satisfied, patient position was changed to lateral position again to adjust reduction. Repeated transformation of the patient’s position would increase operation time and infection risk. Besides, of patients with spinal fractures or thoracoabdominal injuries or pelvic cavity injuries, intraoperative conversion of the body position would increase the risk of secondary damage. This problem could be easily resolved with a simple a “figure of 4” position of affected limb without changing of body position.
However, open wound extending over the posterior edge of the tibia is not suitable for posteromedial approach and anterolateral tibia soft tissue injury is not suitable for lateral approach. In addition, this method is not suitable in fractures with medial comminution, medial crush with impaction at the medial shoulder of the joint, or varus deformity. Other limitations include a small sample size for a short follow-up and a retrospective study design. Although several limitations exist in our study, we believe that type-I and type-II open pilon fractures gain proper management, and clinical outcomes are satisfactory.
In conclusion, though multiple approaches are viable for pilon fractures, a lateral approach allows for excellent restoration of anatomical structure of articular with less medial soft tissue damage and lead to low complication rate. Thus, this approach is safe for type-I and type-II open pilon fractures especially with medial soft tissue injuries.
Footnotes
Author contributions
Chuanzhen Hu and Weiyi Zhu contributed to this work equally as first author. HCZ, JJH, and Gang Wang conceived and designed the study and drafted the manuscript. All the operations were performed by ZJF. ZN, FW, and ZWY collected the data and performed the statistical analysis. All of the authors read and approved the final manuscript.
Availability of data and materials
The data sets supporting the conclusions of the article are included within the article.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported in part by grants from the National Nature Science Foundation of China (no. 81802840).
