Abstract
The incidence of anterior cruciate ligament reconstruction (ACLR) is continuously increasing. As a result so has the need for revision ACLR, which unfortunately has worse functional outcomes and rate of return to sport. Revision ACLR can be performed as a single stage or in two stages. The latter is recommended in the presence of enlarged and/or malpositioned tunnels. We describe our surgical technique, experience and outcome of our first 19 patients in whom we used allograft bone dowels in the first stage of revision ACLR.
Introduction
The incidence of anterior cruciate ligament (ACL) tears in the United States is over 250,000, 1 of which around 65% proceeds to ACL reconstruction (ACLR). 2 The recommended management for ACL tears in young active patients with functional instability following an ACL tear is ACLR. Patients with ACL tears who continue to play high-level pivoting and cutting sports are at high risk of developing osteoarthritis, 3 especially of the lateral tibiofemoral and patellofemoral joints. 4 Some patients despite an intact graft complain of functional instability following ACLR which limits their ability to return to sport. The increasing incidence of ACLR has resulted in an increasing number of revision ACLRs. Risk of ACL graft failure has been reported to be 2–6% 5,6 at <5 years and 3–10% at 5–10 years, 7,8 and peaks around 1–2 years postoperatively mostly due to sport injuries. 9
Current literature shows that approximately 1.7–7.7% of primary ACLR will be revised. 10 –14 Primary ACLR failure can be attributed to surgical technique error, graft failure, trauma and failure to address other ligamentous injury. 15 The main determining factors are the position and size of the original tunnels and the presence of infection. Rerupture rate following revision ACLR varies between 3.5% and 33%. 9,12,16 Patients should be made aware that revision ACLR has inherently a worse outcome than primary ACLR in terms of functional scores, quality of life and return to high level sport. 9,12,17
Several techniques have been described for dealing with bony defects in staged revision ACLR, including autograft such as from the iliac crest and allograft chips, struts, as well as bone dowels. 18 –22 Although allograft bone dowels are easy to use and avoid donor site morbidity, 15,22 several concerns have been raised for fragmentation and failure to effectively plug the defect due to the tunnel shape irregularity and the lack of malleability of the bone dowels. 20
The aim of the present study was to investigate the practicality and radiological integration of the allograft bone dowels used in the first stage of revision ACLR, which would then allow for a solid bony bed to place anatomical ACL tunnels, and to review the clinical outcomes using this two-stage technique in revision ACLR.
Methods
We retrospectively looked at all the patients who needed a revision ACLR and were operated on by the senior author between January 2015 and July 2018. Our centre is a tertiary referral centre and as such receives a wide spectrum of soft tissue knee pathologies. We chose to analyse the approach and outcomes of this procedure by a single surgeon so as to minimize the variables that could impact the outcome. The clinical and surgical management of patients requiring two stage revision ACLR is outlined below.
Patient assessment
Following history and clinical examination of the patient, anteroposterior and lateral radiographs are taken to determine the ACL tunnel position and location of hardware and ideally comparison with previous radiographs is made. If there is suspicion of tunnel dilation or malposition, computed tomography scan is obtained to elucidate further tunnel diameters and location. ACL tunnels which were of acceptable size (<10 mm), or located in an acceptable position which could be reused or located so far out of position which meant that we could insert the tunnels through intact native bone could proceed to single stage revision. Only in cases when the tunnels were dilated or when the existing tunnels were partially out of position and therefore encroaching into where we would insert the new tunnels, we proceeded to two-stage revision ACLR so as to plug the tunnels first with allograft bone dowels, allow time for incorporation, and upon CT scan confirmation of bony integration around 3–4 months after the first stage, second stage ACLR would be proceeded.
Figure 1 shows an example of preoperative CT scan showing tibial tunnel widening. Magnetic resonance imaging is also performed to elucidate other soft tissue pathology such as other ligamentous injury, meniscal and articular pathology. Patient is counselled for a two-stage revision ACLR and extended rehabilitation time and the use of allograft bone dowels. The required bone dowel dimensions are ordered based on and matching the tunnel dimensions from the CT scan.

(a) Pre first-stage revision ACLR – coronal CT scan of knee showing tibial tunnel ellipsoid dilatation. (b) Pre first-stage revision ACLR – sagittal CT scan showing dilated tibial tunnel. ACLR: anterior cruciate ligament reconstruction; CT: computed tomography.
Bone dowels
All bone dowels used were unicortical pre-shaped allograft comprising of dense cancellous bone with partial cannulation for ease of implantation. 23 They are available in diameters of 8–18 mm and length of 15–35 mm. They are freeze-dried and sterilized with their own developed BioCleanse sterilization process which achieves a sterility assurance level of one in a million. 24 Company claims that with over 5 million BioCleanse sterilized allografts there have been zero implant-related infections. The cost of the dowels vary from £455 to £628 based on their diameter.
Patient positioning
Examination under anaesthesia is performed on both knees in supine position to confirm degree of anterior tibial translation, anterolateral rotatory instability, other concomitant ligamentous instability and range of motion. A high thigh tourniquet is placed as well as a side support and two foot rest posts one at 90° flexion and another at maximal flexion.
Operative technique
Diagnostic arthroscopy is initially carried out via high anterolateral portal and anteromedial portals and, if necessary, an accessory anteromedial portal. The insufficient/torn ACL graft is debrided, tunnels are visualized and debrided with a shaver. The tunnels are reamed over a 2.4-mm guide wire to achieve a concentric tunnel with bleeding cancellous bone visible at all aspects. The final diameter is determined by the final reamer. The dowels are inserted using a 5 ml syringe with its end cut off, threaded over a 2.4 mm guide wire and impacted into the tunnels.
Postoperative plan
Postoperatively a check X-ray of the knee is taken before discharge (Figure 2). Patients are allowed to fully weight bear postoperatively and continue with physiotherapy to ensure good range of movement is maintained and muscle bulk is improved ready for the second stage revision ACLR. At 3 months postoperatively patients are seen in clinic again and a CT scan is booked to ensure osteointegration of the allograft bone dowels at the 4 months stage. A typical example is shown in Figure 3. Osteointegration at this stage was found in all our patients although we are aware it could take a bit longer.
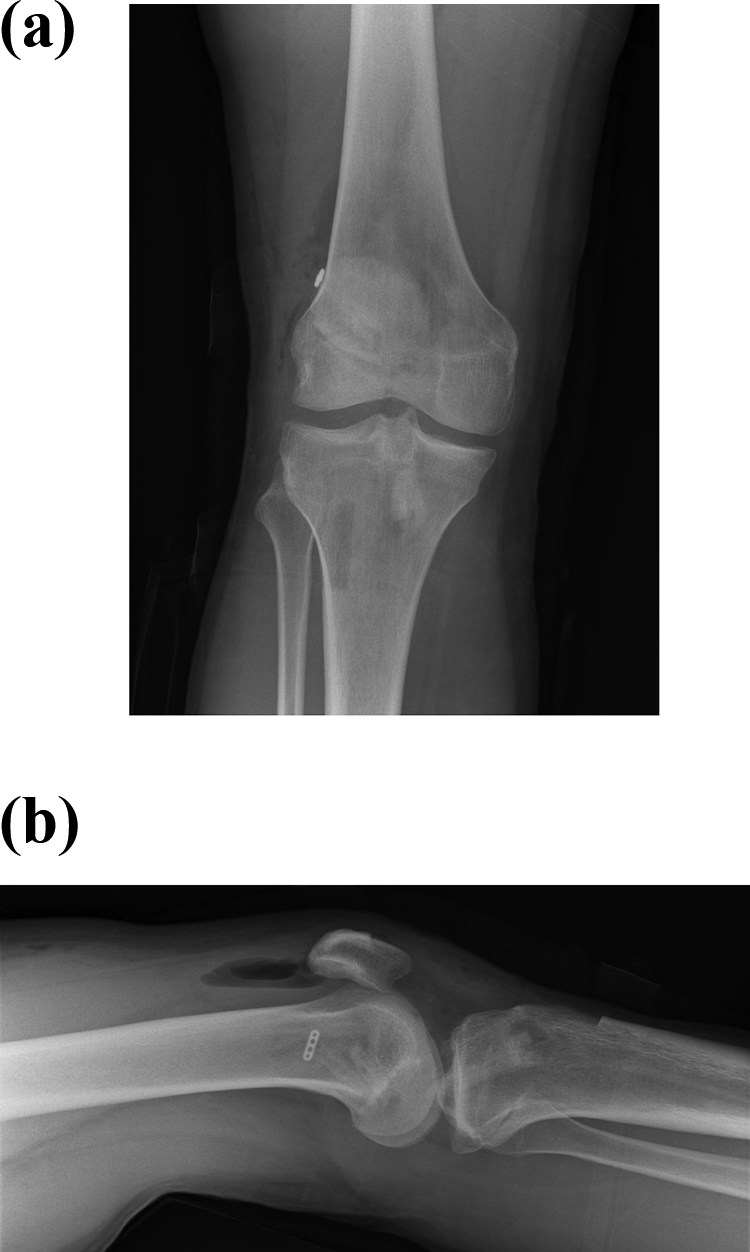
(a) Postoperative AP radiograph of knee. (b) Postoperative lateral radiograph of the knee. AP: anteroposterior.

(a) Coronal CT scan of knee 3 months postoperatively showing incorporation of tibial tunnel allograft bone dowel. (b) Sagittal CT scan of knee 3 months postoperatively showing incorporation of tibial tunnel allograft bone dowel. CT: computed tomography.
Clinical and radiological evaluation
All patients were seen routinely in clinic at 6 weeks, 3 months post first stage revision ACLR. At the 3-month clinic appointment an outpatient CT scan was booked to elucidate the degree of bone dowel incorporation and confirm that the bony bed was satisfactory to proceed with the second stage revision ACLR. The CT scan was reviewed with the patient at a follow-up clinic appointment and the patient consented and listed for the operation.
Results
There were 19 patients (16 males and 3 females) who were eligible for a two-stage revision ACLR (Table 1). The average age at the original injury was 25.2 years (16–34 years). All patients were assessed and operated on by a high volume soft tissue knee surgeon (ORW). Three of the original operations were performed in our trust and the rest at other regional hospitals. Two patients had already undergone a revision ACLR elsewhere and presented to our clinic with instability. Causes for primary ACLR failure were 12 twisting injuries in sport (seven football, three rugby, two American football), two patients had inadequate attendance to physiotherapy, two patients had poorly placed tunnels and three patients reported that they never felt their knee to be stable.
Patient demographics.

Aw: awaiting operation/scan; allog: allograft; BH: bucket handle; BPTB: bone-patellar tendon-bone graft; DBM: demineralized bone matrix; HS: hamstrings; MM: medial meniscus; LM: lateral meniscus; LFC: lateral femoral condyle; PLCR: posterolateral corner reconstruction; P: patient; post-op: post-operative.
aTime lapse between the first and second stage of revision in months.
bThere were two cases that had already a revision ACLR performed elsewhere which failed and we proceeded to second revision in our trust.
11 out of 19 (57.8%) patients had meniscal pathology of which five had both menisci involved and three had a meniscal root tear. Four patients had chondral damage requiring chondroplasty and one patient had microfracture to the lateral femoral condyle. Following thorough evaluation all 19 patients were booked for the first of a two-stage revision ACLR by using bone dowels. The mean time from primary ACLR to being seen in clinic and planning for first stage revision ACLR was 1.6 years.
In our series graft integration was classified as complete/excellent (100%), very good >75%, good 50–75%, poor <50% and absent (Table 1), based on trabecular remodelling crossing the graft-host interface utilizing plain radiographs and CT scans. The grading system has been utilized with good effect in other studies such as in revision hip arthroplasty surgery 25 and was found to be suitable for our study.
Results
The dowel sizes used in the femur were 10 × 35 mm2 in 12 cases, 8 × 35 mm2 in three cases and 12 × 35 mm2 in one case. In one patient two smaller 10 × 15 mm2 and 10 × 17 mm2 bone dowels were used. In two cases, the old femoral tunnel was ignored as it did not interfere with the new tunnel. For the tibia, two dowels were used in all cases to make up for the length. The most commonly used diameter was 12 and 14 mm2 dowels. Then, 10 × 35 mm2 dowels were used in seven cases, 11 × 35 mm2 dowel in one case, 12 × 35 mm2 dowels in nine cases, 13 × 35 mm2 dowel in one case and 14 × 35 mm2 dowel in one case as well. It was noted that in most cases the tunnel aperture in the tibia varied along its length, being larger in the middle and smaller at the apertures. Hence, the dowels used in eight patients varied in diameter to try and match this variance in the diameter of the tibial tunnel. In our series we used demineralized bone matrix (DBM) in two cases, due to the severity of ballooning of the tibia tunnel in its midportion.
All patients had CT scans on average of 3.6 months (range 3–11 months) following first-stage revision ACLR and in all, except one case, and all patients were reviewed again in clinic 1 week after the scan. A typical example is shown in Figure 3. In 11 cases the bone dowel integration was found to be very good (>75%) and in the remaining five cases excellent (100%). While we are aware that satisfactory osteointegration could take longer than our intended time frame of obtaining CT scans 3 months postoperatively, it was reassuring that satisfactory osteointegration was found in all our patients. One patient, who happened to be our first patient, had fragmentation of the distal part of the tibial bone dowel.
There were two postoperative complications, one major and one minor. The major complication was a case of a 34-year-old patient who presented 3 days postoperatively with pneumonia and non-fatal pulmonary embolism (PE). The patient has recovered fully but remains sceptical about proceeding to the second stage. Non-fatal PE is a rare but a well-described complication following arthroscopic procedures. 26,27 The minor complication was that of a stitch abscess which settled with a course of oral antibiotics.
At the time of write up of the paper 14 of the 19 patients had their second-stage revision at a mean time of 13.6 months (range 4.5–31 months) from the first stage. One patient is sceptical to proceed to the second-stage revision ACLR as they recovered from a PE following their first-stage procedure. Another patient has been listed for the operation but has not had it yet. Nine patients who underwent the second-stage procedure had ipsilateral bone-patellar tendon-bone (BPTB) ACLR, one needed contralateral BPTB graft as the ipsilateral one had already been used, one contralateral hamstrings graft and in three cases a BPTB allograft was required as a result of multiple revisions. Finally, in two cases a posterolateral corner (PLC) reconstruction was performed (Larsen technique) using either Achilles tendon or peroneus longus tendon allograft (Table 1). The BPTB graft was secured in the femur using RIGIDFIX pins (DePuy Synthes) and BIOSURE PK screws (Smith and Nephew) in the tibia. When quadruple hamstring graft was used they were secured in the femur with an endobutton and in the tibia with a BIOSURE PK screw. At a mean follow up of 7 weeks (range 6–30 weeks), some quads wasting was noted early on which was recovered at the 3 months follow-up. Two patients had lost 5–10° hyperextension which physiotherapy helped to regain.
Discussion
While there is no universally accepted definition for ACLR failure, Johnson and Fu. 28 defined it as recurrent instability or stiff and painful knee with restricted range of motion from 10° to 120° of flexion. ACL laxity can be objectively measured using commercially available instruments such as the KT1000/2000 arthrometer (MEDmetric, San Diego, California, USA), which measures antero-posterior tibial translation. A disparity of >3 mm is considered significant for ACL failure. 29 Moreover, static and dynamic clinical tests used to assess knee stability correlate poorly with patient’s perception of instability. 30
The causes of ACLR failure can be categorized into trauma, technical errors and failure of graft incorporation. The Danish knee ligament reconstruction registry showed that trauma was a cause of ACLR failure in 36.2%, knee instability of unknown cause in 25.6% and suboptimal femoral tunnel placement in 21.5%. 31 The Multicentre ACL Revision Study (MARS) showed the reasons for ACLR failure to be trauma in 32%, technical in 24%, graft incorporation in 7%, combination of all three in 37% and infection in <1%. 32 The MARS study further showed that femoral tunnel malposition was the commonest technical error followed by tibial tunnel malposition.
When evaluating patients, detailed history of the initial injury and primary ACLR should be taken as well as the rehabilitation that followed. Time elapsed between ACLR and failure can suggest the cause. Typically, ACLR failures within 6 months are more likely to be due to technical errors or over aggressive rehabilitation or early return to sport in particular those involving cutting and pivoting prior to achieving adequate neuromuscular control. 33 Late failure is commonly due to trauma. 34 While in our series none of the ACLR failed due to over aggressive rehabilitation, three patients had inadequate physiotherapy. One of them who was a self-employed labourer and could not afford the time off for his rehabilitation. Another patient claimed expensive transportation costs to have their physiotherapy and in the last case the patient failed to attend multiple physiotherapy appointments.
Revision ACLR has worse outcome scores and higher graft failure than primary ACLR. 9,12,35,36 Return to sport has also been documented to be lower (62–74%) following revision ACLR. 37 It is important patients are counselled for these lower outcomes so as to adjust their expectations. Increasing evidence has come about to show the risk of contralateral ACL injury. In a prospective multicentre study, it was found that the risk of contralateral ACL tear was the same at 3.0% to graft failure within 2 years of the ACLR. 6 However, in a systematic review it was shown that over 5 years post ACLR that the risk of ACL tear in the contralateral knee (11.8%) was double that of the ipsilateral knee (5.8%). 38 In a recent systematic review of studies with minimum follow-up of 10 years it was found that the risk of ACL graft tear was 7.9% and of the contralateral ACL 12.5%, and the risk of a contralateral tear was 1.63 times that of a graft tear. 39 On the other hand, a multicentre prospective study 11 showed similar results of ipsilateral and contralateral ACL tears at 6 years (7.7% vs. 6.4% respectively). They also found that younger age at the index operation and use of allograft to be risk factors for further surgery but revision ACLR, female sex, body mass index and surgical exposure were not. This fits with our series where the mean age was just under 20 years at the index operation. None of our patients had allograft as part of their index operation. The risk of subsequent injury to either knee within the first 5 years after ACLR was reported as 17% for those <18 years old, 7% for those between 18 years and 25 years and 4% for those >25 years. 40 None of the patients in our series suffered contralateral knee injuries, but these risks are important to bear in mind when treating these patients.
Revision can be performed as single stage or two stages. The two primary reasons to perform a two stage revision to bone graft the tunnels are for tunnel malposition or widening. This is supported by our series whereby all our patients had tunnel widening in the tibia and two had malpositioned tibial tunnels. Other causes of two stage revision ACLR are infection, arthrofibrosis, malalignment, focal chondral lesions, meniscal deficiency and other ligamentous injury. 41 The MARS study group reported that bone grafting of dilated tunnels was performed in 3% for tibia and 3% for femur at the time of revision operation and a two stage-approach was required in 9% for tibia and 8% for femur. 32
Confirmation of osteointegration of the bone dowels is a prerequisite in our practice prior to proceeding with the second stage revision ACLR. Our results show that we managed to obtain CT scans at an average of 3.6 months postoperatively. In 11 cases of our series the integration was found to be very good >75% and in the remaining five cases complete (100%). Although our grading system is practical, it is only an estimation of bone dowel integration. A recent prospective study assessing iliac crest bone graft incorporation in the tibia by CT scan prior to revision ACL reconstruction showed higher occupying ratios, union ratios, and bone mineral density scores at 24 weeks than at the 12 weeks point postoperatively. 42 In another study the use of iliac crest autograft has been described to fill bone defects and requires an average of 5.8 months for incorporation to show on CT scans. 18 The time lapse between the first- and the second-stage revision ACLR in our series was on average 13.6 months (range from 4.5 months to 31 months). Taking into consideration that the widest tibial tunnel drilled was 14 mm in our series, whereas Uchida et al. 42 reported bigger defects (the enlargement of the tibial tunnel aperture was 20 mm in diameter), we feel that our results are in line with the published literature.
Following the confirmation of bone dowel integration, patients were listed promptly for the second stage revision ACLR. Delays in proceeding to the second stage had to do more with social and work-related reasons rather than medical conditions and bone dowel integration. The bone quality during drilling of the new tunnels, and the rigidity of fixation, were positively reassuring that a sound bony bed was present. Although bone dowels are easy to use and avoid donor site morbidity 15,22 several concerns have been raised for fragmentation and failure of the bone graft due to tunnel irregularity. 20 The overall radiological integration was very good. In situations where the bone tunnels are irregular, different sized cylindrical dowels could be used at different tunnel depths based on measurements from preoperative CT scans. Alternatively, they could be used in conjunction with other grafts, such as DBM, to avoid over drilling the tibia in trying to achieve a uniform width. In our series, we have used DBM in two cases in combination with the bone dowels with very good results. Regarding the raised concerns about the ability of the graft to heal within the tunnel when these dowels are large, we have three patients in our series that had bone dowels in tibia of 12 and 14 mm and had excellent clinical and radiological results.
Intra-articular findings in primary and revision ACLR were reported using the Multicentre Orthopaedics Outcomes Network and MARS study groups 43 were reported to show a significant risk of chondral damage in the medial and lateral compartments following respective menisectomies. However even when controlling for meniscal injury, there was an increased odds ratio in revision compared to primary ACLR of lateral and patellofemoral compartment chondral injury but not in the medial compartment. A 2-year follow-up study of 442 revision ACLRs from the Danish registry reported meniscal damage in 26% and chondral damage in 31%. 31 In our series, which is small in comparison, we had a similar proportion of patients with chondral damage requiring either chondroplasty or microfracture (26.3%) but just over double the rate of meniscal damage (57.8%).
Most studies cite age as the main predictor for revision ACLR. Other predictors include participation in sports involving jumping, cutting and pivoting 44 and smoking. 45 In a 2-year follow-up study of almost 17,000 patients from the Swedish registry, it was found that adolescents and football players had a 1.5 and 2.5 higher risk of revision ACLR, respectively, and those individuals with both of these predictors had three fold higher risk. 41 Our findings are in keeping with the literature as all our patients suffered their index ACL injury secondary to cutting and pivoting sports and had a mean age of just under 20 years.
Revision ACLR is often compounded by bone defect problems secondary to malpositioned tunnels, hardware removal or tunnel enlargement. Various ways to fill the bone defect have been reported each with their own pros and cons. The use of iliac crest autograft has been described to fill bone defects and require an average of 5.8 months for incorporation to show on CT. 18 Structural iliac crest bone graft has been harvested using osteochondral autologous transfer system but is limited to maximum dimensions of 10 mm diameter and 25 mm length. 19 The morbidity of harvesting iliac crest bone graft can be overcome with the use of allograft.
Single-stage ACLR with the use of allograft has been described for malpositioned femoral tunnels although this is limited to the ability to place the new tunnel in the anatomical but different orientation and as long as the old tunnel was not too posterior that would compromise its integrity. 15 However, drilling along the axis of the existing tunnel could lead to allograft fragmentation and failure.
Advantages and limitations
The advantages in our study are that we used the same management plan and surgical approach for patients requiring two-stage revision reconstruction ACLR, the operations were performed by a single consultant soft tissue knee surgeon, and we confirmed with CT scans osteointegration of the allografts for all patients prior to second-stage revision ACLR. Limitations include lack of objective clinical outcome measures and statistical testing, retrospective study, lack of a control group and comparison testing to confirm superiority of this technique over another. We would advocate further testing of this technique by other centres to confirm its applicability, ease of use and reliability as well as long term patient outcomes. Table 2 summarises the advantages and limitations of two stage revision ACLR using allograft bone dowels.
Advantages and limitations of two-stage revision ACLR using allograft bone dowels.

ACLR: anterior cruciate ligament reconstruction.
Conclusion
Although one-stage revision ACLR is preferable, we recommend a two-stage approach in selected cases, when existing tunnels are excessively dilated or when malpositioned to an extent that they are encroaching the desired tunnel path. By allowing time for the bone to incorporate, it ensures complete freedom in placement and orientation of the new tunnels without compromise similar to a primary ACLR. Use of allograft avoids the need for autograft harvesting which may be limited in the amount when taken locally or has additional comorbidities when taken from the iliac crest. It is a relatively simple and quick technique that gives the opportunity to address concomitant pathology. To the best of our knowledge this is the first attempt to associate the radiologic and clinical findings following a two stage ACLR using bone dowels (Table 1A).
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
