Abstract
Introduction and purpose:
Patellar tendinopathy is a disease affecting particularly athletes. Platelet-rich plasma (PRP) injections have gained increasing interest for their potential benefits. Anyway, a tendon disease longer than 6 months should be considered as an indication for surgery. The aim of our study was to evaluate the efficacy of PRP in athletes with a severe chronic patellar tendinopathy longer than 6 months when surgery should be chosen.
Methods:
We enrolled 17 sport practitioners (19 patellar tendons) who did not want to undergo surgery and who are nonresponders to other conservative treatments. We treated them with PRP and calculated the results using the visual analog scale (VAS), the Victorian Institute of Sport Assessment-Patellar (VISA-P) score, and Tegner Activity Scale. Every test has been conducted at T0, T1 (4 months), and T2 (12 months).
Results:
We found a poor improvement at T1 and a clinical worsening at T2 through VAS. VISA-P showed a medium improvement both at T1 and T2. Tegner scale did not show improvements.
Conclusions:
Our study was not able to remove the doubts about the benefits of PRP in patellar tendinopathy, confirming ambiguous certainties. Further investigations are needed to assess its effectiveness.
Introduction
Patellar tendinopathy is a common disease mainly affecting athletes. It is generally characterized by pain at the proximal insertion of the tendon. Pain is firstly felt as a simple discomfort. It is insidious and tends to be engraving leading to a limitation of physical activity. As a disease of considerable severity, it leads athletes to stop sporting activities for long periods. In the most serious cases, it forces the complete abandonment of physical activity. 1
Patellar tendinopathy predominantly affects professional volleyball players (45%) or basketball ones (32%). 2 In these sports, the tendon is very stressed for the many jumps and landings. There are also other professional categories at risk. Some authors have shown that patellar tendinosis can also affect nonprofessional athletes who are forced to spend most of their job-time sitting or who have to go up and down the stairs repeatedly. 3
Unfortunately, lots of elite athletes do not respond to conservative treatment and after a prolonged period of persisting symptoms, generally 6 months, surgery is indicated.
In recent decades, infiltrative treatments involving the use of platelet-rich plasma (PRP) or autologous blood have gained increasing interest in the scientific community. 4
PRP is a concentrate of autologous platelets suspended in a small volume of plasma. Its therapeutic effects result from the presence of high growth factor concentrations (transforming growth factor (TGF)-beta1, TGF-beta2, platelet-derived growth factor, insulin-like growth factor-1, epidermal growth factor, hepatocyte growth factor); these are contained in platelet secretion granules capable of accelerating the repair of damaged structures following a trauma. 5,6 The first standardized application of PRP began in the mid-1990s in the dermatological and plastic-reconstructive field to speedup the recovery of surgical wounds. 7 –10 The encouraging results gave rise to various other orthopedic applications in the 2000s, initially concerning bone trauma, then also regarding a number of other pathologies such as osteoarthritis and musculoskeletal diseases. 11 –13 Currently, the validity of PRP is being tested in noninvasive treatments of chronic tendon diseases. The first study on the application of PRP in chronic tendinopathy was in 2007: Volpi et al. proposed a prospective cohort study analyzing the response of eight subjects after a single infiltration with PRP in a rehab protocol. After 120 days of treatment, seven patients reported a clear improvement in symptoms, and magnetic resonance imaging (RMN/MRI) images showed a significant reduction in signal heterogeneity compared to the images before the treatment. 14
Several other studies have followed showing important results in pain reduction and concerning recovery time for knee mobility and sport activities. 15 –25 Despite studies demonstrating the importance of PRP in chronic tendinopathies, few randomized studies of strong impact exist in the current scientific literature, and scholars are looking for further evidence.
The purpose of our study was to evaluate the efficacy of PRP in cases where surgery has become the particular treatment for diseases longer than 6 months and not sensible to any other conservative treatment.
We aimed to evaluate the progression of clinical symptoms in patients treated with PRP at 4 months and 12 months through a clinical subjective evaluation. The clinical evaluation was followed by an echographic evaluation of tendon tissue.
Materials and methods
Seventeen patients were selected for the study (12 males and 5 females); for two patients, both knees were treated, leading to a total amount of 19 knees. They had an average age of 30.6 years ranging from 19 years to 45 years.
The average body mass index (BMI) was 24.3 kg/m2; no patient had contraindications to treatment.
An observational study was conducted through a clinical evaluation at 0, 4, and 12 months after PRP treatment. In some patients, we succeeded in conducting an echographic evaluation. The patients were all sportsperson who had performed several conservative approaches that had not led to any important benefits. Treatment options included oral medications and topical nonsteroidal anti-inlammatory drugs (FANS/NSAIDs), tendon supplements, and physiotherapy treatment.
After 6 months since the beginning of the conservative treatments, the patients refused surgery; therefore, we proposed PRP injection as an alternative attempt. They spontaneously decided not to be operated and to be treated with PRP injections.
All patients had to submit an informed consent before the treatment.
Exclusion criteria left out patients who had undergone surgery, patients over 45 years of age, degenerative articular disorders, contraindications to the use of PRP, and patients who had undergone previous infiltration with PRP. We included in the study young patients, patients practicing amateur agonist sports, and nonresponders to other conservative treatments.
The first step involved medical history reconstruction and visit. Visit has been repeated at T0, T1, and T2, with the collection of clinical data for our study: visual analog scale (VAS) score, Tegner activity scale, and the Victorian Institute of Sport Assessment–Patellar (VISA-P). 22
The VAS score was rated from 1 to 10, indicating the degrees of pain reported by the patients during the treatment and thus representing the subjective measure of the pain experienced.
In our study, we applied VAS score to a series of six gestures typically able to evoke pain in the patient suffering from chronic tendinopathy: Sitting without feeling pain. Going downstairs. Extending the leg. Bending the leg keeping the weight on it. Crouching down. Jumping 10 times on the affected leg.
The VISA score measures the ability to practice sports activities by means of a 0–100 score, in which the highest score represents full activity.
Tegner activity scale scores a sports activity level between 0 and 10, where 0 is the disability and 10 is the participation in competitive or extreme sports. 23
Assessment of PRP
The blood withdrawal (50 mL in a 1:10 ratio of gluconate calcium and entire blood) was processed using the Gravitational Platelet Concentration System ® (GPS) II Platelet Concentration System.
After separation by centrifugation, we managed to obtain a concentration about 10 times lower, reaching a total amount of PRP of about 5 mL.
A small amount (50 μL) of sodium bicarbonate solution was added to reestablish the physiological pH in the infiltration site and to allow platelet degranulation in the collagen. 24 The obtained PRP was stored in 5 cm3 tubes and stored at −30°C.
After the disinfection of the infiltration site by iodate solution, a sterile field was set up.
Through ultrasound (US) guide, after an injection of 0.5 mL of lidocaine (local anesthetic), a 22-gauge needle was inserted perpendicular to the affected tendon.
We injected the PRP into small doses by repositioning the needle five to six times in the pathological tissue.
After infiltrating all the volume of PRP (5 cm3), the needle was removed and the infiltration site was disinfected again. 25
Finally, we applied a compression bandage and invited the patient to remain in a supine position for 30 min.
Patients were discharged after about an hour from PRP injection.
We performed three injections in 15 days, for all patients. Then we assigned them the rehabilitation protocol.
The patients were required to keep the affected limb at rest for at least 7 days, to start walking and to apply ice on the infiltration site twice a day for 15 min.
Between 7 and 21 days after treatment, patients started to walk into the water and swim at moderate and controlled speeds.
At 5 weeks from infiltration, patients began eccentric training of quadriceps and concentric exercises for leg flexors gradually increasing the effort up to 7 weeks after treatment.
At 9 weeks, they started specific sports exercises, with a return to normal sports activity at 12 weeks after PRP therapy.
Statistical analysis
The data obtained were collected and organized into a database. We calculated mean, median, and standard deviation of the obtained values. The normality of the distribution of the different variables was evaluated by Shapiro–Wilk test. As the non-normal distribution was applied, Mann–Whitney’s nonparametric test has been used to evaluate the existence of a statistically significant difference in the clinical evaluations.
Results
In our study, 23 patients have been recruited for the application of 24 PRP infiltrations between January 2015 and August 2016. However, only 17 of these patients carried out the complete cycle of three distant 10-day infiltrations at T0 and have been reevaluated at 4 and 12 months at the clinical–functional level. The other six people did not complete the cycle because they decided to suspend sports activity before the 12 months follow-up and were therefore excluded from the analysis.
Table 1 presents the average scores of VAS of five patients calculated from the six questions mentioned.
Values of VAS for every question.
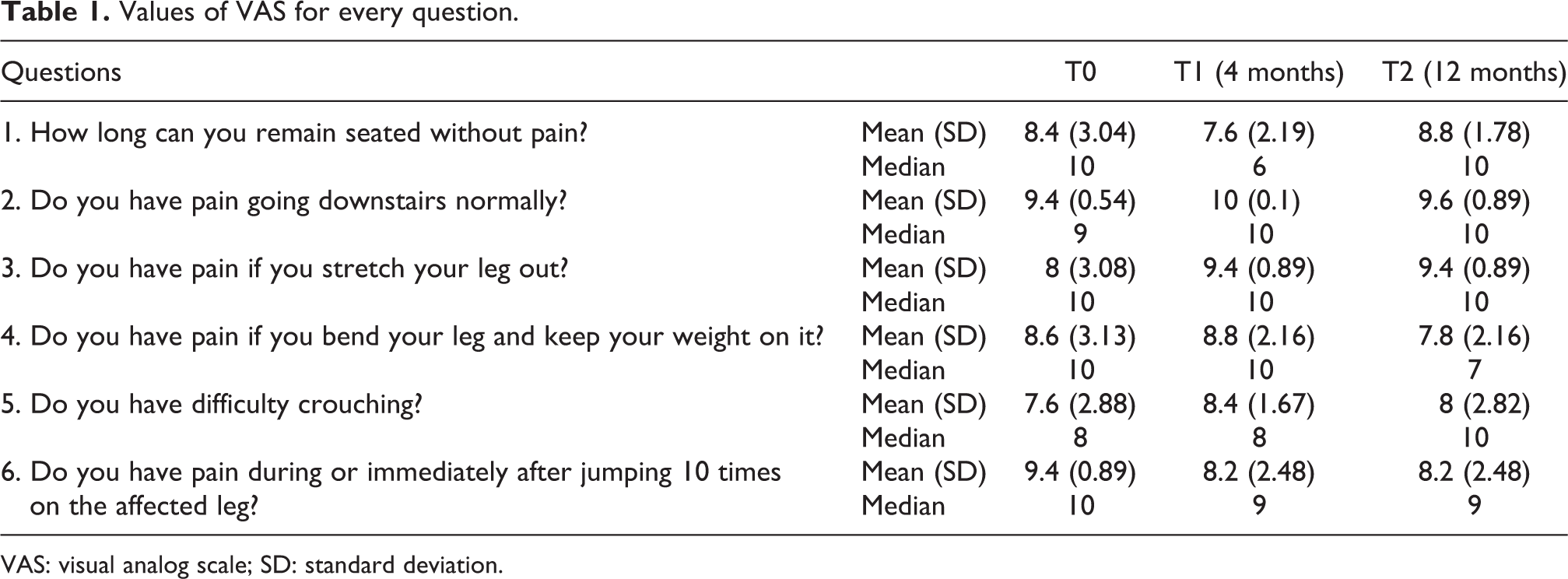
VAS: visual analog scale; SD: standard deviation.
The mean VAS for all patients at T0 was 8.8. Mean VAS at T1 was 7.18, while at T2 it was 8.
From the Mann–Whitney test, it was a correct p > 0.05, so there was no significant difference in results at 4 and 12 months compared to T0 (Table 2).
Values of averages and medians VAS for every evaluation.

VAS: visual analog scale.
The VISA score showed a relative enhancement, with an average pretreatment score of 46.7 ± 11.8, an average value at T1 of 56.7 ± 8.2, and a final average value of 61.5 ± 9.5 (p > 0.05).
It has been noted that no correspondence between mean values of VAS and VISA-P was observed. (Figure 1).

Correlation between VAS and VISA. VAS: visual analog scale; VISA: the Victorian Institute of Sport Assessment.
Both for VAS and for VISA-P, from the Mann–Whitney test, we obtained a correct p > 0.05, so there was no significant difference in results at 4 and 12 months compared to T0.
Tegner’s Activity scale started from an average value of 8.2, it was still 8.2 at T1, while it was 8.0 at T2.
Only 13 of the 17 patients were evaluated through an echographic test at T0 and at the end of the follow-up. Four patients (35%) reported an almost complete recovery of the echographic defects. (Figures 2(a) and (b) and 3(a) and (b)).

(a) and (b) Transversal and linear projections of patellar tendinopathy at T0.

(a) and (b) Linear and transversal projection of patellar tendon at T2 in the same patient of Figure 2.
Three patients showed calcific deposits on the proximal insertion of tendon and they reported the same features at 12 months.
A patient had to be reoperated since pain persisted in the first week. In this patient, the unsatisfactory outcome of the therapy has also been related to tendinopathy chronicity more than 5 years long.
Even more unsatisfactory results were reported with a 45-year-old patient who suffered non-absorption of the infiltration: in this case, tendon pain became worse due to the persistence of PRP and has led to the interruption of sports activities (volleyball).
We found a steady improvement in a 20-year-old patient with particularly serious start-up symptoms that led to a total resolution of the symptoms just 4 months after the treatment. The patient scrupulously followed the post-infiltration protocol and has been followed by a physiotherapist with specific exercises; he performed personalized training before returning to sports too.
The other patients had an improvement especially in the first 6 months of the treatment, but symptoms did not improve in the further 12 months.
Discussion
Despite the promising preclinical premises, the literature on the clinical application of PRP for patellar tendinopathies presents controversial findings.
The study we have proposed is in line with other studies with similar goals and methods, in particular Filardo’s study of 2013. Filardo evaluated the effects of PRP therapy after a medium-term follow-up period: They enrolled 43 patients (average age 30.6 years, mean BMI, 24.7 kg/m2, 42 men and 1 woman) with chronic tendinopathy. Eleven patients suffering from bilateral tendinopathy have been subjected to three intra-tendinous injections with 5 mL of PRP. At first, patients have been evaluated prospectively, then after 2 months, 6 months, up to a minimum of 3 years. The evaluation used included VISA-P, EQ-VAS questionnaires, overall patient satisfaction, and time to return to sports. High scores were documented at time over, and 80% of patients declared they were satisfied and managed to return to sports. Significantly, worse results were obtained in patients with a history of long-lasting painful symptoms and bilateral lesions. No correlation between US and clinical outcomes was found. In accordance with our results, we found an appreciable improvement at medium term (4 months) with normalization of long-term outcome evaluated on VAS, and a clinical deterioration of the patients with long-lasting tendinopathy. 16
The 2015 Kaux’s study has focused on the objective of turning back to sports after treatment, and its results are comparable to ours for those who have scrupulously followed the proposed rehab program. Recovery was almost total, both from the force developed by the articulation and the movements before the development of the pathology. Twenty subjects with chronic proximal circular tendinopathy benefited from a PRP infiltration coupled with standardized rehabilitation programs through eccentric exercises. The follow-up (up to 1 year) was evaluated by a VAS, International Knee Documentation Committee, and VISA-P. Seventy percent of patients reported a favorable evolution of symptomatology with pain decreasing and returned to sports activities. Progressively, all scores have improved significantly. This recent study confirms that a local PRP injection with an eccentric rehabilitation program improves symptoms and knee functionalities in chronic patellar tendinopathy up to 1 year after injection. 17
In 2009, Kon et al. reported a steady improvement with a sample of 20 male athletes with chronic patellar tendinosis. For this study, 20 consecutive cases were treated and prospectively clinically evaluated at a minimum 6 months follow-up. Participants were all men, with a mean age of 25.5 years (range 18–47 years). All the patients had a chronic condition, with a mean history of 20.7 months pain (range 3–60 months) and had tried rest as treatment without any success. PRP injections were carried out in three different moments. Tegner score and VAS were used for clinical evaluation prior to treatment and in the follow-up. Complications, functional recovery, and patient satisfaction were also documented. A statistically significant improvement was observed in all sportsmen following PRP injections. A further improvement has been observed 6 months later, following the physiotherapy treatment. These clinical results have proved encouraging, indicating that PRP injections have the potential to determine a satisfactory outcome, even in severe cases of refractory tendinopathy. 18
Another important aspect that we have to consider is that PRP is not always the same product. In fact, the exact definition of PRP has not been clearly established and includes a range of formulations. Different applications and formulations of PRP present different properties: Some of them might produce good results, while others might be ineffective or even dangerous.
The concentrations could vary in the number of platelets supplied to the lesion, leading to a variety of amount of growth factors (GFs): Even small variations in their concentrations can produce very different effects. 26 Moreover, the appropriate dose, timing, and length of intervention are important aspects requiring further investigation: The chronological activation of molecular signaling should be appropriately coordinated to the temporal presence of cells. 27
Other controversial aspects regard cells that are into the formulation. Platelets are not the lonely cells, but also leukocytes, monocytes, macrophages, and mast cells might be contained and play a role. 28
The method and timing of activation may play a role in this variability. In fact, the amount and speed of GFs release and activation may differ from the activation time. 16,26,27,29
The contradictory findings along the age, about effectiveness of PRP, could be justified by all these kinds of differences.
In our study, athletes who did not benefited from other conservative treatments have been enrolled. PRP infiltration had then been supplemented with specific rehabilitation protocols, and the effects have been evaluated on the VAS, VISA-P, and Tegner activity scale. Results have not been encouraging at mid-term follow-up. A poor improvement of clinical conditions has been revealed at 4 months. No satisfactory results were recorded 12 months after the infiltration. Both for VAS and for VISA-P, from the Mann–Whitney test, we obtained a correct p > 0.05, so there was no significant difference in results at 4 and 12 months compared to T0.
Echographic evaluations, as in correspondence with clinical features, have shown no significant improvements.
According to our results, the treatment for chronic patellar tendinopathies with PRP infiltrations would seem not to guarantee a good clinical outcome.
We believe that our clinical results are quite different with respect to most of the other studies and provide a good opposition in the literature. In fact, they seem a contrary to what is supported by recent optimistic studies in literature.
This study is not with limitations. First, the sample size is less with small number of patients; second, there is a lack of uniformity in sample collection, particularly because of the broad age range (19–45 years) and the nonuniform BMI; third, the currentshort follow-up (12 months) period is insufficient to determine the longevity of the treatment; and finally, a control group of investigation is missing.
Unfortunately we did not succeed in evaluating all patients with an echographic (US) test; only some of them have been evaluated both at T0 and in the follow-up, and no objective standardized criteria have been used in the evaluation, according to some scientifically recognized research items.
Then further instrumental investigations, such as functional knee-specific biomechanical tests, may be needed to evaluate the effectiveness of the treatment.
Conclusions
The purpose of our study is to propose a preliminary study on the use of PRP infiltrations in chronic patellar tendinopathies with a surgical indication, evaluating whether it is a viable alternative to surgery. The results have been largely in line with the latest literature in a context still open. There are doubts about the real benefits of PRP in chronic tendinopathy despite its important use in health-care facilities.
Our study has not been able to address these doubts, probably due to methodological limits, but also because the tendency of its excessive use is superior to its proven evidence-based effectiveness.
In conclusion, further investigations and analyses are needed to improve the efficacy of the treatment, to reduce the incidence of complications, and to evaluate the actual efficacy of PRP as a valid alternative to surgery.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
