Abstract
Objective:
Supramalleolar tibial osteotomy (SMO) for asymmetric ankle osteoarthritis (OA) is known to lead to satisfactory. Here, authors present a preliminary report on SMO surgical treatment in patients with asymmetric ankle arthritis.
Materials and Methods:
We reviewed cases of asymmetric ankle OA treated by modified SMO between January 2011 and October 2015. Clinical assessment was performed with the use of the ankle and hindfoot score of the American Orthopedic Foot and Ankle Society (AOFAS), foot function index, and visual analogue scale (VAS). Patient satisfaction with surgery and postoperative subjective symptoms were examined. Radiographic evaluation included preoperative and postoperative tibial anterior surface angle (TAS angle), talar tilt angle (TT angle), and tibial lateral surface angle (TLS angle). Takakura stage was measured.
Results:
The average follow-up period was 46.3 months. The AOFAS score was 55.7 ± 6.03 preoperatively and 76.0 ± 4.73 postoperatively. Foot function index was 60.7 ± 8.78 preoperatively and 30.8 ± 7.59 postoperatively. VAS was 7.2 ± 0.53 before surgery and 1.9 ± 0.85 after surgery. Clinical evaluations showed statistically significant improvement. The majority of patients reported satisfactory results in the subjective satisfaction evaluation. TAS angle was 84.6 ± 1.82 preoperatively and 94.0 ± 2.79 postoperatively. TLS angle was 78.8 ± 2.11 preoperatively and 81.8 ± 1.80 postoperatively. TT angle was 3.6 ± 1.26 before surgery and 2.1 ± 0.79 after surgery. Thirteen cases showed radiographic improvement of Takakura stage. Complications were not observed.
Conclusion:
Modified SMO is a useful procedure that provides for the union and stability of osteotomy with the advantages of the existing SMO and can be performed without bone graft.
Introduction
Degenerative osteoarthritis (OA) is a disease caused by degeneration of articular cartilage. It is one of the most common human diseases. There are both primary and secondary forms of OA. Degenerative arthritis of the ankle is reported to cause symptoms in about 1% of the world’s adult population, representing a significant economic burden for both patients and the health-care system. 1,2 Ankle joints have an anatomically smaller body area than knee joints and hip joints, and the amount of pressure applied per unit area is relatively larger in ankles than in the other two joint types. Kimizuka et al. reported that when a force of 500 N was applied, the area under the ankle load was 350 mm2, while the analogous value was 1100 mm2 for the hip joint and 1120 m2 for the knee joint. 3 For this reason, arthritis can easily appear when structural anomalies occur. Therefore, secondary OA caused by fractures, chronic ankle ligament injuries or infection, or paralytic deformity is relatively common, while primary degenerative arthritis occurring without trauma or underlying disease is rare. 4
Takakura et al. classified ankle arthritis with the extent of disease progression (Table 1). Conservative treatment for early-stage patients may include ankle joint orthosis or lateral wedge insoles, but for late-stage patients, surgical treatment such as arthroscopic marginal resection of the ankle joint, total ankle joint arthroplasty, or arthrodesis can be performed. 5 However, it is not easy to determine the appropriate treatment for moderate-stage patients because no definite treatment modality has been established. Surgical treatments that can be used in moderate-stage cases include lateral ligament reconstruction, calcaneal osteotomy, and supramalleolar tibial osteotomy (SMO). 6,7 SMO is designed for realigning the weight-bearing axis outward in varus-type OA of the ankle with narrow medial joint space to prevent the progression of arthritis. 8 It is generally known that SMO is effective for preserving the joint in moderate-stage asymmetric ankle arthritis.
Takakura stage of ankle osteoarthritis.

However, there has been a continuing debate on the appropriate indications for this surgical treatment. In 2006, Takakura et al. reported that the tibiotalar OA of stage IIIb and above is not an indication for SMO. 8 However, several other studies have reported that SMO improved the clinical outcome even in stage IIIb. Because of these contradictory findings, it is now important to determine the appropriate indications for SMO in the ankle joint and what type of deformation might indicate this treatment. 9 Conventional SMO is medial open-wedge osteotomy to treat varus deformity. However, the cutting plane is often at the upper level of the center of rotation and angulation (CORA). In this state, the distal fragment is inevitably moved to the lateral side. 10 Lee et al. reported subtalar impingement due to lateral displacement of the hindfoot after medial open-wedge osteotomy for varus deformity. 11 In the past, Paley has recommended an Ilizarov’s distraction to simultaneously correct angulation and displacement to address distal movement. 12
The purpose of this study is to introduce a modified step-cut oblique osteotomy which could resolve translational problems of the distal fragment and bone–graft issue after medial open-wedge osteotomy in patients with varus-type OA of ankle and its results.
Materials and methods
This study was analyzed as a case series that includes patients who underwent modified SMO for asymmetric varus-type arthritis in our orthopedic department between January 2011 and October 2015. We only included patients who also had at least 2 years of follow-up. The mean age at the time of surgery was 58.6 years, ranging from 54 to 66 years. Two patients were male and 13 were female. Patients having other operations on the foot and ankle, conventional medial open-wedge osteotomy, and secondary OA such as rheumatoid arthritis or traumatic arthritis were excluded. Thus, 15 patients were available for analysis. This study was approved by the Institutional Review Board of Hanyang University Hospital.
All patients complained of severe pain on the medial side of the ankle during weight bearing. Physical examination revealed tenderness on the medial side of the ankle. Patients were treated with conservative methods such as medication, physical therapy, and wedge insole for at least 6 months but showed no improvement in symptoms. In each case, SMO was then performed. In all cases, there was narrowing or loss of ankle in the medial joint space on the weight-bearing anterior–posterior ankle radiographs. There were 4 cases of Takakura arthritis class II and 11 cases of IIIa (Table 2).
Clinical evaluation of the patients.

Preop.: preoperative; Postop.: postoperative.
Clinical assessment included measurement of the ankle and hindfoot score of the American Orthopedic Foot and Ankle Society (AOFAS), foot function index, and visual analog scale (VAS) both preoperatively and at postoperative follow-up. Patient satisfaction with surgery and postoperative subjective symptoms were also evaluated. Radiological evaluation including standing anteroposterior, standing lateral, and standing hindfoot alignment view was performed before and after the operation and at 6-month intervals postoperatively. At anteroposterior view, tibial anterior surface angle (TAS angle) and talar tilt angle (TT angle) were measured. At lateral view, tibial lateral surface angle (TLS angle) was also measured (Figure 1). The OA stage was assessed using the Takakura classification system as modified by Tanaka et al. both preoperatively and at the last follow-up appointment.

At anteroposterior view, TAS angle and TT angle were measured. At lateral view, TLS angle was measured.
Preoperative and postoperative radiological and clinical evaluations were compared using the Wilcoxon signed-rank test with the nonparametric method in SPSS version 20.0 (IBM Co, Armonk, New York, USA).
Surgical technique and postoperative management
All operations were performed in the supine position by one surgeon under spinal anesthesia or general anesthesia with a tourniquet on the thigh. In the present study, we performed a fibular osteotomy first with a skin incision of 8 cm in length toward the proximal fibula along the longitudinal midline of the fibula. After the exposure of the lateral cortex, temporary fixation on distal tibiofibular syndesmosis was performed with two Kirschner wires. And then an oblique osteotomy was performed from superoanterior to inferoposterior aspect. The midpoint of the fibular osteotomy plane was matched with the planned tibial osteotomy plane. The permanent fixation of the fibula using a locking plate was performed after completing the procedure on the tibia. Next, about 12 cm longitudinally, an incision, started at medial malleolus, was made proximally along the medial aspect of the tibia. After exposure of the medial cortex, supramalleolar osteotomy of tibia was performed. First, a1-cm deep transverse osteotomy on the anterior cortex was made at just proximal of the distal tibiofibular syndesmosis. And then, the oblique osteotomy was performed as posterosuperior direction from the transverse osteotomy site. Finally, the medial open wedge was made. If necessary, translation was done in accordance with heel alignment (Figures 2 and 3). Temporary fixation was performed with Kirschner wires. The amount of wedge was decided to overcorrect 5–6° more than the normal angle of TAS angle, as 89°. Using fluoroscopy, we confirmed that the TAS angle was corrected to the target value. For the osteotomy plane, the anteroposterior lag screw was inserted to compress the oblique osteotomy site and then fixed with a locking plate (Figures 4 and 5). Additional ligament or arthroscopic procedures were not performed. To obtain additional stability, an autogenous bone graft was performed in the open-wedge space using the protruded cortical bone (Figure 6). After the incision site was closed, an operated leg was immobilized with a short-leg splint. Two weeks after the surgery, the splint was changed to removable cast and patients started active range of motion exercise of ankle joint, which maintained from 6 to 10 weeks. And then progressive weight bearing was done.

The internal open wedge was inserted from the distal osteotomy plane.

Angulation and translation were implemented as needed.
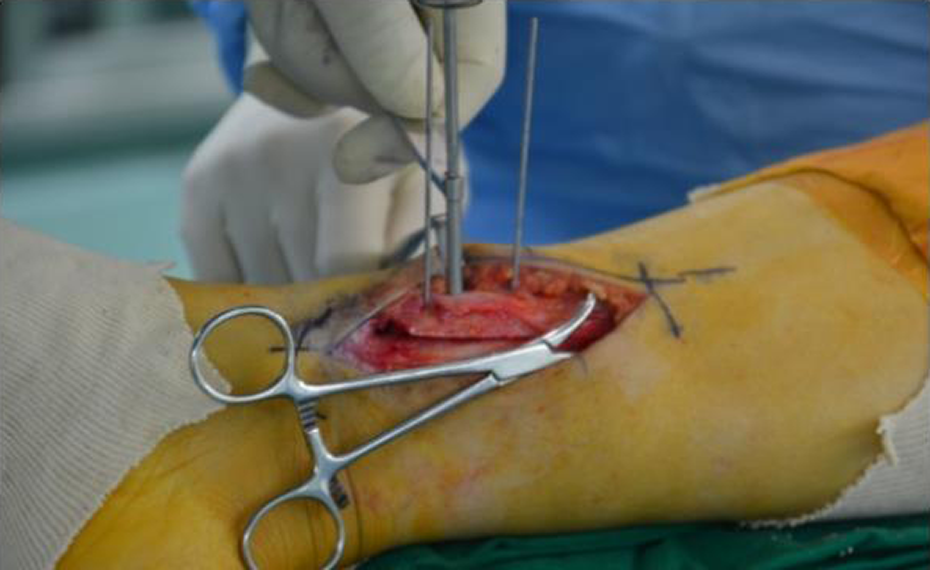
For the osteotomy plane, a cancellous cannulated screw or lag screw was inserted to compress the interfragmentary space.

The interfragmentary space was fixed with a locking plate.
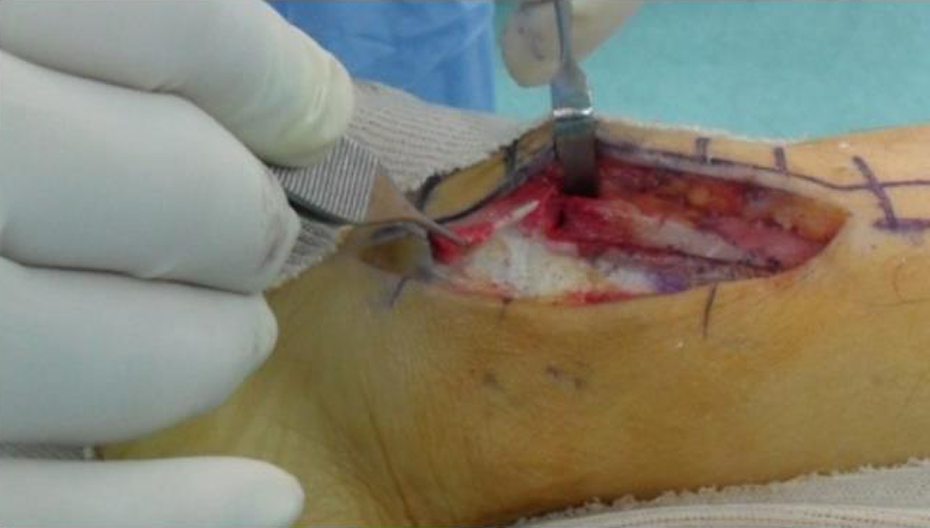
An autogenous bone graft was performed in the open-wedge space using the protruded distal medial cortical bone from the proximal fragment.
Results
All cases showed fusion at the osteotomy site within the postoperative follow-up period (average 46.3 months). Clinical assessment indicated patient improvement. The mean AOFAS score was 55.7 ± 6.0 (standard deviation) preoperatively and 76.0 ± 4.73 postoperatively. The mean foot function index was 60.7 ± 8.78 preoperatively and 30.8 ± 7.59 postoperatively. The mean VAS for pain was 7.2 ± 0.53 preoperatively and 1.9 ± 0.85 postoperatively. In all cases, the clinical evaluation scale did not deteriorate, and all clinical evaluation items showed a statistically significant improvement after the operation (Table 2). Patients reported a satisfaction level of “very satisfactory” in nine cases, “satisfactory” in four cases, and “moderate” in two cases, meaning that 86% of all patients (15 cases) were satisfied or very satisfied with postoperative results. Postoperative pain was not observed in the lateral part of the ankle joint during follow-up.
All radiological evaluation showed statistically significant improvement. The TAS angle changed from 84.6° ± 1.82 preoperatively to 94.0° ± 2.79 postoperatively. TT angle was 3.6 ± 1.26 before surgery and 2.1 ± 0.79 after surgery. The TLS angle was 78.8 ± 2.11 preoperatively and 81.8 ± 1.80 postoperatively.
The Takakura stage of our patient’s arthritis improved in 13 cases: an improvement from preoperative grade IIIa to grade II was achieved in 11 patients, and an improvement from grade II to grade I occurred in two patients. There were no changes in two of the cases (Table 3), but there were also no cases in which the Takakura stage deteriorated. Clinical results were correlated with radiological results in most cases. In one case, there was a radiological improvement from stage IIIa to stage II, but it was not matched by clinical improvement. In that case, the preoperative VAS score was 8 and then 4 postoperatively. The AOFAS score changed from 53 points preoperatively to 69 points postoperatively. The patient reported that their postoperative pain did not change significantly, and the satisfaction with surgery was moderate. There were no reports of complications such as infection, skin necrosis, nonunion, or nerve injury at the last follow-up of the SMO. There were no cases of conversion to ankle arthrodesis or artificial ankle arthroplasty due to progression of postoperative arthritis or persistent ankle pain.
Radiological evaluation of the patients.

Preop.: preoperative; Postop.: postoperative.
Discussion
The purpose of SMO is to reduce pain and mitigate the effects of varus-type ankle arthritis by shifting previously concentrated weight bearing from the medial side of the ankle to the lateral side. 13 Several studies have reported that unequal pressure on the articular surface can cause degenerative changes in cartilage and that redistribution of pressure through osteotomy can be an effective treatment. 14,15 Cadaveric studies demonstrated that changes in the angle of the distal tibia can change the weight distribution of the ankle joints, 16 and it has been demonstrated that weight load can be moved outward by changing the varus ankle joint surface angle to neutral or slightly valgus using osteotomy. 17 Takakura et al. reported that more than 80% of patients with moderate ankle joint degenerative arthritis with varus deformity had satisfactory results after osteotomy. 7 Cheng et al. also reported that osteotomy in patients with primary and secondary moderate arthritis showed good clinical results. 15 To date, there have been many studies on the indication of osteotomy, biomechanical studies, and surgical techniques as well as good clinical outcomes with SMO. This study also showed satisfactory clinical outcomes with SMO in patients with moderate OA as in other studies.
The radiological and clinical outcomes reported hereafter a modified SMO were similar or superior to those after conventional SMO. With an exception of one case, most cases showed clinical and radiological improvements. There are several advantages of the modified SMO technique used in this study. First, there were no patient complaints of subfibular pain after surgery. In case that subfibular impingement due to excessive lateral translation may be expected at the time of correction for varus deformity, the varus can be corrected, while simultaneously distal fragment can be translated inward as freely as the operator wants. Therefore, the excessive lateral displacement of the distal fragment, potentially caused by correction of severe varus deformity, can be prevented by medial translation of the distal fragment or repositioning CORA. Second, recurvatum ankle deformity with a decreased TLS angle was corrected using a wider open wedge on the anteromedial side than used in the conventional SMO. In this procedure, sagittal plane deformity correction is feasible by reducing or increasing the angle of obliquity. Third, there is no donor site morbidity by harvesting autogenous iliac bone. We performed a minimal bone graft using a protruded local bone fragment after correction. Fourth, while the intrinsic stability may be lower than that of a structural bone graft, the use of interfragmentary fixation over a larger contact surface between the fragments and the additional fixation with a locking compression plate improves stability and the union of the osteotomy site. Therefore, we believe that stability of a modified SMO approach is not necessarily lower than that of an open wedge with a cancellous bone graft.
Recent studies have reported positive outcomes of total ankle arthroplasty in the treatment of late-stage ankle arthritis, but relatively high failure rates have been reported compared to other joint arthroplasty techniques. The SMO technique reported here is likely a useful joint-preserving treatment for patients with moderate ankle arthritis. The technique may delay or halt progression to late stage in which total arthroplasty or arthrodesis is required. The slightly valgus alignment in radiological parameters improved clinical outcomes in this study.
This study has several limitations. First, the cohort of this study is the small number of cases included in its retrospective analysis. Second, the relatively short follow-up period of 2 years is also likely to affect the interpretation of results.
Conclusion
The modified SMO described in this study improved clinical and radiological results for Takakura II or IIIa varus ankle OA in short-term follow-up. This step-cut oblique osteotomy technique has a benefit to achieve an intended alignment of distal tibia and fibula as well as the heel by controlling position of the distal fragment. Another benefit is that the necessity of iliac bone graft can be excluded. Therefore, this technique is regarded as a useful joint preserving technique in the treatment of varus ankle OA.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
