Abstract
Background:
Adolescent spasmodic valgus foot is usually associated with resistant pain and deformity. It shows controversy regarding its incidence, etiology, and treatment. Our study aimed to evaluate the functional outcome after the nonsurgical treatment for such condition.
Methods:
This study included 50 planovalgus feet secondary to peroneal or peroneo-extensor spasm in 33 adolescents with a mean age of 14 ± 2.8 years. The procedure included foot manipulation under general anesthesia, sinus tarsi injection with corticosteroids, and a walking cast in the neutral position. Patients were evaluated functionally (using the American Orthopedic Foot and Ankle Society (AOFAS)) and radiologically before the procedure, after cast removal, and 3, 9, and 18 months later with special attention given for recurrence during the follow-up period with a mean duration of 22.5 ± 3.5 months.
Results:
Once general anesthesia had been conducted, the deformity was corrected without any manipulation, and full passive inversion could be easily obtained in 26 feet, the deformity was corrected only after manipulation, and full passive inversion had been obtained in 14 feet, while 10 feet remained stiff even after manipulation. The mean AOFAS score was significantly improved (p < 0.001) from 40.9 ± 3.5 at presentation to 73.56 ± 5.2 at the last follow-up in which 12 feet was painless and freely mobile and 24 feet had partial relapse, while 14 feet had complete relapse.
Conclusion:
The nonsurgical treatment for adolescent spasmodic valgus foot could be a simple and effective treatment. Apart from limited complete recurrence, the overall functional outcome was satisfactory. Level of evidence: type IV case series.
Keywords
Introduction
Sir Robert Jones has described that the acquired deformity of peroneal spastic planovalgus foot has no consensus regarding its incidence, etiology, and mechanism with wide divergence of treatment opinions. 1,2 Although many of arthritic and neuromuscular conditions can cause peroneal spastic planovalgus foot, it is commonly associated with tarsal coalition with calcaneonavicular or talocalcaneal bridge. Whenever no cause could have been found, the condition has been termed idiopathic peroneal spastic flatfoot or idiopathic spasmodic planovalgus foot. 3,4
Adequate assessment of peroneal spastic flatfoot depends on proper clinical and radiographic evaluation. 5,6 The initial treatment for such condition should be conservative, while surgical intervention should be restricted to those who fail to respond to nonoperative measures. 3,4
This study aimed to evaluate the functional outcome after the nonsurgical treatment for adolescent spasmodic valgus foot. The planned procedure included foot manipulation under general anesthesia, sinus tarsi injection with long-acting steroids, and a walking cast in the neutral position. This work studied the relation between different radiographic findings and patients’ symptoms and tried also to highlight different factors affecting the outcome and recurrence in such condition.
Patients and methods
This prospective, case series study was conducted between October 2013 and January 2016 after approval from the Research Ethics Committee of the university. Any adolescent with unilateral or bilateral spasmodic valgus feet with resistant foot pain and stiff planovalgus deformity with peroneal or peroneo-extensor spasm and radiographic signs of flatfoot (with or without intertarsal anomalies) was included in this study. Cases with neuromuscular disorders, hysterical conditions, cases with generalized intertarsal arthritis, or inflammatory arthritis and cases with frank intertarsal bony bars were initially excluded from our study. This study included 50 feet with symptomatic spasmodic planovalgus deformity in 33 adolescents not responding to nonsteroidal anti-inflammatory drugs and activity modifications.
A detailed history was obtained regarding the age and general health, a recent weight gain, the standard level of activity, and whether there is a recent involvement in strenuous activities, a recent or repetitive foot or ankle trauma, mode of onset, and duration of symptoms. Physical assessment (Figure 1) had been done to evaluate the gait, foot posture, and state of the arch during weight-bearing and non–weight-bearing; the site of tenderness; the forefoot/hindfoot relationship; and the range of motion of the ankle, hindfoot, midfoot, and forefoot. The American Orthopedic Foot and Ankle Society (AOFAS) Ankle–Hind foot scale was used for scoring patients’ condition. Complete blood picture, erythrocyte sedimentation rate, and antistreptolysin O titer have been evaluated in all cases.
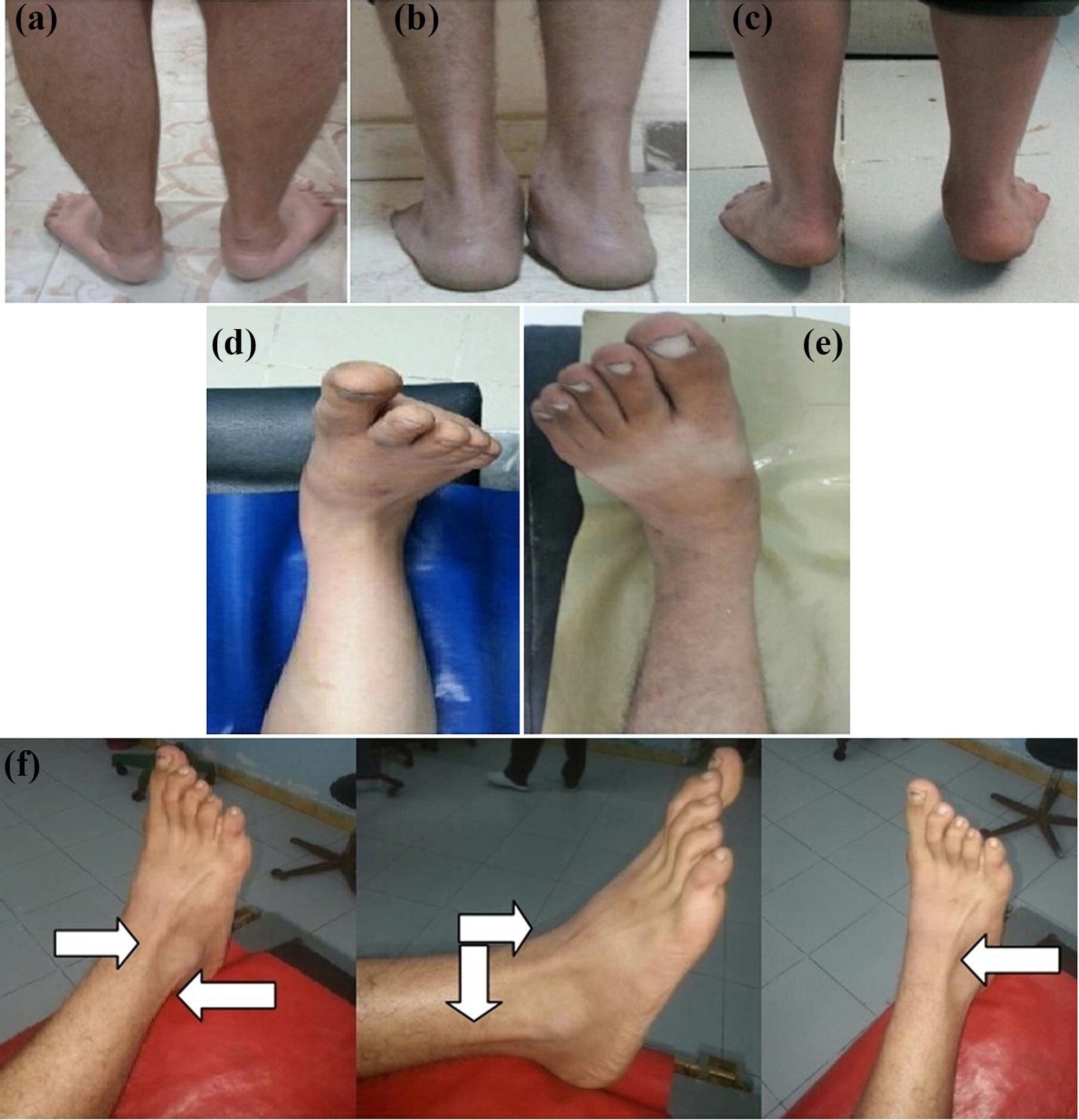
(a) to (f). Clinical findings in some of the studied cases. (a) to (c): Foot attitude during weight-bearing showing (a) bilateral and (b) unilateral involvement, and (c) persistence of the deformed foot attitude with tiptoeing denoting rigid deformity. (d) and (e): Foot attitude during non weight-bearing showing (d) planovalgus foot with spasmodic extensors and (e) planovalgus foot without spasmodic extensors. (f) The characteristic peroneo-extensor spasm (white arrows) with rigid planovalgus foot and extended four lateral toes.
Radiological assessment included both resting and weight-bearing plain X-ray (anteroposterior (AP) and lateral radiographs, oblique tarsal views) and computed tomography with axial, coronal, and sagittal cuts (Figure 2). The standard radiographical parameters were checked including the talonavicular coverage angle, the AP and lateral CYMA line, the AP talar-first metatarsal angle, the AP talocalcaneal angle, and the calcaneal pitch angle. Moreover, the intertarsal radiological abnormalities suggesting developmental tarsal anomalies (hindfoot attitude and clarity of the subtalar joint, the presence of accessory navicular bone, prolongation of anterior process of calcaneous and talonavicular peaking) were checked.

(a) to (f) Radiological findings in some of the studied cases. (a) Plain X-ray AP view foot bilateral involvement with valgus attitude. (b) Plain X-ray AP view foot showing accessory navicular. (c) Lateral view ankle X-rays showing narrowing of the posterior facet of the subtalar joint with loss of subtalar joint clarity with talonavicular joint beaking. (d) Oblique views to exclude arthritis and coalition. (e) and (f) CT ankle showing narrowing of subtalar joint with no bony bar ((e) coronal; (f) sagittal). AP: anteroposterior.
Three groups of patients were identified after induction of G/A. In group I, the foot assumed a neutral position without any manipulation, and full inversion could be easily obtained. In group II, the neutral position and full inversion had been obtained only by manipulation, whereas in group III, the feet were still stiff and remained in the preanesthetic valgus position even after a trial of manipulation.
In all the cases of the three groups, the sinus tarsi was injected with long-acting corticosteroids combined with a local anesthetic. In groups I and II cases, a walking plaster cast was applied with the foot in neutral position and retained for 3 weeks. For group III cases, the cast was applied with the foot inverted as far as possible to near-neutral position and retained for 6 weeks.
Once the patient is fully conscious after awakening from general anesthesia, the first clinical sign of improvement that could be detected was the ability to do painless, complete active planter flexion of the toes due to relief of the extensor spasm. Patients were advised for early full weight-bearing from the first day as tolerated by pain.
Post-manipulation X-rays were done to assess changes in the radiographic parameters compared with pre-manipulation values. After cast removal, active and passive movements of the ankle and foot (mainly the subtalar joint in the form of eversion and inversion) were encouraged. Patients were functionally assessed (using the AOFAS Ankle–Hindfoot scale) with special attention to the relapse of the condition at 3, 9, and 18 months after the procedure.
Ethical standards
The procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2000 and 2008. All patients’ parents gave informed consent before inclusion in the study; the study was authorized by the institutional review board.
Statistical analysis
Statistical analysis was performed using IBM SPSS Statistics for Windows, Version 22.0 (IBM Corp., Armonk, New York, USA). Statistical analysis was done using a two-tailed Student’s t-test, and the value of p < 0.05 was considered statistically significant.
Results
This study included 50 feet with symptomatic planovalgus feet secondary to peroneal or peroneo-extensor spasm in 33 adolescents with a mean age of 14 ± 2.8 years (ranged from 11 years to 18 years). The condition was bilateral in 17 patients, while 16 patients had unilateral affection. The study comprised 5 females (15.2%) and 28 males (84.8%), and patients were followed up for duration ranged from 18 months to 30 months with a mean duration of 22.5 ± 3.5 months. Most of the patients (27 of the 33 patients) reported recent involvement in strenuous activity and began to complain after the age of 13.
Radiographically, calcaneonavicular developmental anomalies with prolongation of anterior process of calcaneous of variable degrees were present in 16 feet, talocalcaneal developmental anomalies with narrowing of the posterior facet of the subtalar joint with loss of subtalar joint clarity, talonavicular joint beaking, flattening of the lateral talar process in 8 feet, and accessory navicular in 2 feet, while there were no detectable developmental tarsal anomalies in the remaining 24 feet.
After induction of anesthesia, 26 feet (52%) assumed a neutral position without any manipulation, and full inversion could be easily obtained (group I cases). In 14 feet (28%), the neutral position and full inversion had been obtained only by manipulation (group II cases). In 10 feet (20%), the foot remained in the preanesthetic valgus position even after a trial of manipulation (group III cases).
The pre-manipulation radiographic data were evaluated with regard to the attained foot posture and subtalar mobility post-manipulation under G/A: in group I, 18 feet showed no detectable developmental tarsal anomalies, 6 feet had calcaneonavicular anomalies, and 2 feet had talocalcaneal anomalies. In group II, 6 feet showed no detectable developmental tarsal anomalies, 4 feet had calcaneonavicular anomalies, 2 feet had talocalcaneal anomaly, and 2 feet had an accessory navicular bone. In group III, 6 feet showed calcaneonavicular anomalies and 4 feet showed talocalcaneal anomalies.
Pain was dramatically improved in all patients, while their feet were rested in cast. The post-manipulation X-rays (Figure 3) showed marked improvement (p < 0.001) of the AP talus-first metatarsal, the AP talocalcaneal angles, and the calcaneal pitch angle compared to the initial radiographic parameters in 40 cases (80%; groups I and II; Table 1), while the remaining 10 cases (20%; group III) showed no improvement in the radiographic parameters.

(a) to (e) Radiological results in some of the studied cases. (a) Lateral view X-rays comparing the calcaneal pitch angle and clarity of the subtalar joint before and after the procedure showing marked improvement. (b) Plain X-rays AP view foot comparing the valgus attitude of the foot and forefoot abduction before and after the procedure showing marked improvement. (c) Plain X-rays AP view comparing forefoot abduction, eversion, and the leg–foot relationship (before and after the procedure showing marked improvement. (d) Plain X-rays AP view foot comparing the AP talocalcaneal angle and the talar-first metatarsal angle before and after the procedure showing marked improvement. (e) Lateral view X-rays comparing the calcaneal pitch angle and clarity of the subtalar joint before and after the procedure showing almost no improvement. AP: anteroposterior.
Radiological parameters pre- and post-manipulation (mean ± SD).

SD: standard deviation; AP: anteroposterior; LAT: lateral.
Immediately after cast removal, active and passive movements of the ankle and foot (mainly the subtalar joint in the form of eversion and inversion) were restored both actively and passively and progressively increased. With tiptoeing, normal inversion of the subtalar joint with heel varus is present in cases of groups I and II (Figure 4).

Functional outcome immediately after cast removal of a bilaterally affected patient showing full active plantar flexion and dorsiflexion of the ankle and toes with full passive inversion on the subtalar level bilaterally and improved foot attitude during tiptoeing with the heels went into varus.
During the later follow-up, the condition of the foot was almost one of the following: Normal foot: Corrected, painless, and freely mobile foot. Improvement with partial relapse: Infrequent pain with no deformity, full passive inversion but limited active inversion or limited both active and passive inversion. Complete relapse: Deformed, painful, and stiff foot. Complete relapse with deterioration: Deformed, painful, and stiff foot with progressive partial or complete intertarsal arthritis.
At 3-month follow-up
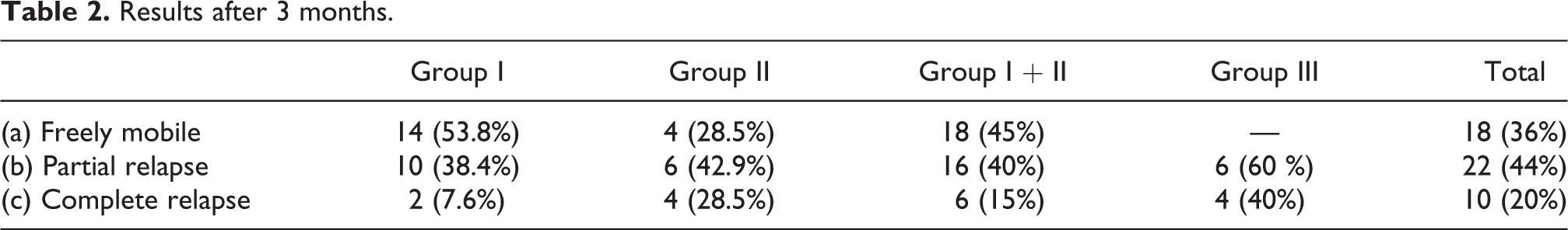
In group I cases, 14 feet was still painless and had a full range of active inversion (completely mobile feet); 10 feet had full passive inversion, limited active inversion, and return of slight pain (partial relapse); and 2 feet completely relapsed with the same pain and deformity before the procedure (Table 2). In group II cases, 4 feet was freely mobile and 6 feet had a lack of full active and passive inversion (2 feet with slight pain and the other 4 feet were painless (partial relapse), while complete relapse occurred in 4 feet. In group III cases, 6 feet was slightly better than before (less pain than before) and 4 feet was unchanged by the procedure. The overall functional results at 3-month follow-up were as follows: 18 feet (36%) was freely mobile; 22 feet (44%) had partial relapse, and 10 feet (20%) had a complete relapse.
Results after 3 months.
At 9-month follow-up
In group I cases, 4 feet of 14 freely mobile feet developed recurrence of symptoms; 3 feet had loss of some inversion with slight pain (partial relapse) and 1 foot returned to the same painful deformity as before (complete relapse; Table 3). In group II cases, 1 foot of the 4 freely mobile feet had a partial relapse. In group III cases, 1 foot of 6 (that were slightly improved) developed a complete relapse.
Results after 9 months.

At 18-month follow-up
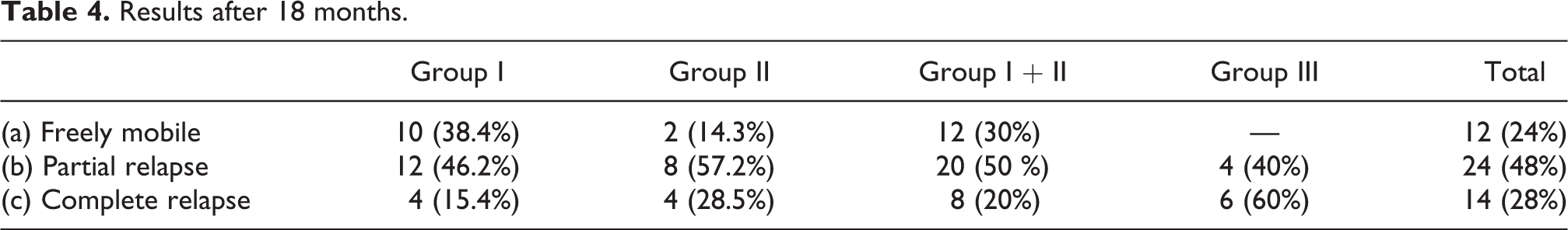
In group I cases, of the 13 feet which had a partial relapse, 1 foot returned to the same painful deformity as before (Table 4). In group II cases, 1 foot of the 3 freely mobile feet had a partial relapse. In group III cases, 1 foot of 5 (that were slightly improved) developed a complete relapse. Table 5 outlines the outcome correlation between tarsal anomalies and resolution of symptoms at the final follow-up.
Results after 18 months.
Outcome correlation between tarsal anomalies and resolution of symptoms at the final follow-up.

Although there was a progressive decrease in the AOFAS score through the three-recorded evaluations at 3, 9, and 18 months post-procedure, there was an overall statistically significant improvement (p < 0.001) in the score when the mean AOFAS score was improved from 40.9 ± 3.5 at presentation to 73.56 ± 5.2 at the last follow-up (Table 6). At the last follow-up, 12 feet was painless and freely mobile; 24 feet had partial relapse, while 14 feet had complete relapse. So, satisfactory results were obtained (Figure 5) with complete or partial improvement in 36 feet (72%) and unsatisfactory results with complete relapse in 14 feet (28%). Between the 14 feet with complete relapse, 5 feet developed arthritic changes with deterioration of their conditions and were treated by triple arthrodesis.
The mean AOFAS score pre-manipulation, immediately after cast removal, and 3, 9, and 18 months post-manipulation.

AOFAS: American Orthopedic Foot and Ankle Society; SD: standard deviation.
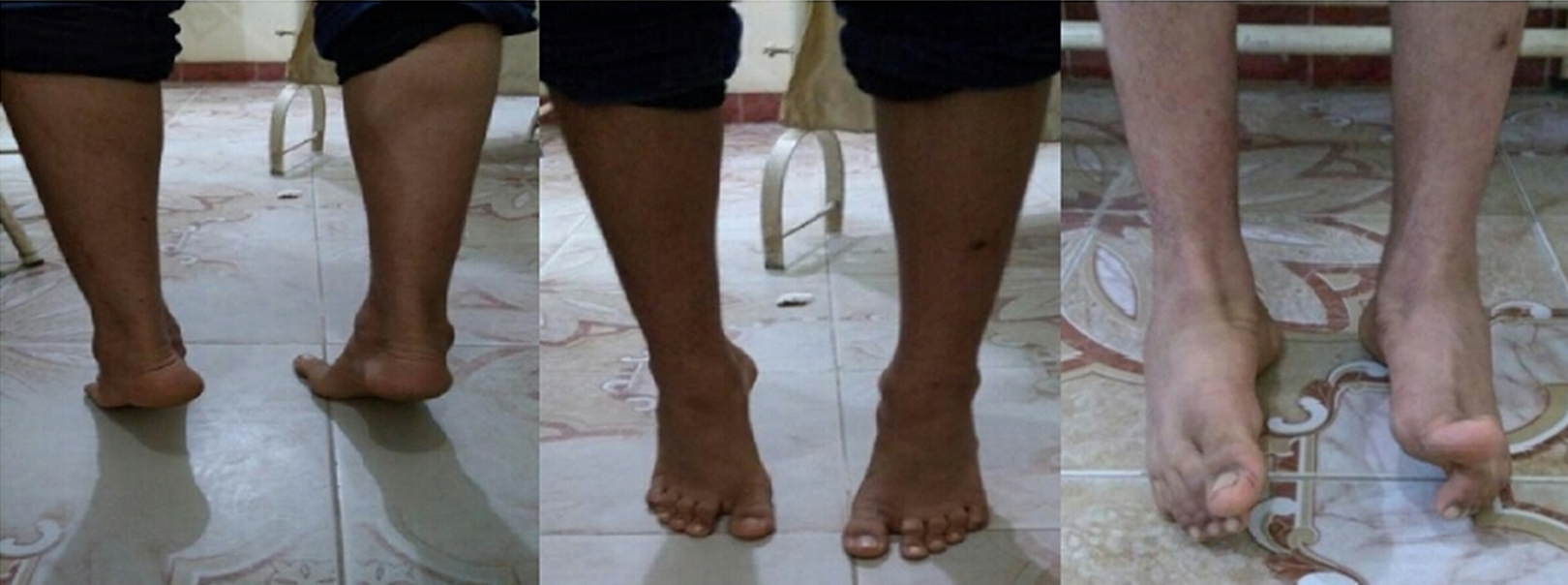
Very satisfactory clinical results after 18-month follow-up.
Discussion
Adolescent symptomatic flatfoot is not uncommon 7 ; patients usually present with vague complaints of pain and/or stiffness of the foot and ankle with recent altered foot shape, muscle spasm, and gait abnormalities. Symptoms usually start insidiously and could be precipitated by minor trauma or change in activity, and if not properly addressed and managed could have disabling and debilitating consequences. 7
Peroneal spastic flatfoot is a term used to describe symptomatic rigid planovalgus foot deformity resulting from widely different etiologies. 7 Tarsal coalitions are the most common cause but not the only causative factor for this condition. Unfortunately, little was written in the literature about peroneal spastic flatfoot. 7
Every effort should be directed toward the nonoperative treatment for such condition affecting mainly younger patients and adolescents, and it is very important to clearly define treatment goals with both the patient and the parent, since resuming all activities may not be possible.
Thirty to ninety percent of patients have been reported to respond to nonoperative treatment for spasmodic valgus foot even with those having tarsal coalitions. 8 However, recurrence of the symptoms may occur at any time and may necessitate either repeated immobilization or surgical intervention. 9 The surgical outcome of tarsal coalition was evaluated by many clinical studies with few reports of nonsurgical treatment outcome. 10 Jayakumar and Cowell reported that approximately 25–30% of their patients improved with casting. 6 In the study by Blockey on 30 rigid flatfeet, 2 the results after 2-year follow-up were 2 feet (6.6%) complete cure, 16 feet (53.4%) partial relapse, and 12 feet (40%) complete relapse.
The functional outcome in our study was superior to the previously discussed studies due to multiple factors. 2,6 Firstly, our procedure was done under G/A that had an important effect in relieving muscle spasm in most of the patients, while previous studies used nerve block instead of G/A for their patients. Secondly, others did casting without manipulation, while we did manipulation before casting. Thirdly, local injection of a long-acting steroids and local anesthesia in the sinus tarsi was done in all patients who had an anti-inflammatory action, improving the pain and stiffness. Lastly, 48% of our patients had no significant radiographic anomalies.
Luhmann et al. had examined 13 patients under anesthesia 11 ; 9 had significant improvement regarding the subtalar motion (in whom casting with subtalar steroid injection was done), and 4 had some improvement (in whom peroneal fractional lengthening was done). Only two patients required surgical interventions. Fifty percent of their patients at the final follow-up had pain relief and unlimited activity. Varner and Michelson evaluated 33 feet in 27 adults with tarsal coalition. 12 They found that the nonoperative treatment in the form of activity modification and anti-inflammatory medications was successful in most of their patients. Only 5 of the 33 feet required surgical intervention.
In the current study, the mean AOFAS score was significantly improved from 40.9 at presentation to 73.56 at the last follow-up. Satisfactory and encouraging results (with complete or partial improvement) had been obtained in 36 feet (72%) and unsatisfactory results with complete relapse occurred in only 14 feet (28%).
The radiographic parameters were not totally restored to the normal anatomical values, but most of them were improved compared to the pre-manipulation values in 40 cases as a nonsurgical method without any bony procedure—like calcaneal osteotomy or arthrodesis—was used to treat this condition.
All the studied patients were adolescents with symptomatic peroneal or peroneo-extensor spasm; but neither the foot condition regarding severity of deformity and rigidity nor the radiographic characteristics were alike in all patients. Moreover, the foot condition under anesthesia and the potential for deformity correction were dissimilar. Despite the presence of pain, foot spasm, and deformity, frank bony coalition was not detected in any of the studied 50 feet, giving a conclusion that symptoms could occur in the absence of frank bony tarsal coalition. No significant radiographic tarsal anomalies were detected in 24 feet, whereas 16 feet had a calcaneonavicular anomalies and 8 feet showed talocalcaneal anomalies with variable degrees, while 2 feet had accessory tarsal navicular. So, peroneal spastic flatfoot could occur with or without the presence of developmental tarsal anomalies.
This coincides with what was reported by Blockey who did a study on 30 abnormal feet 2 ; 9 feet showed calcaneonavicular anomalies, 4 showed talocalcaneal bridge, 1 foot had a bony ridge on the superior surface of navicular near its articulation with the talus, 1 foot had an abnormal joint between two bony prominences below the lateral malleolus, 2 feet showed an accessory navicular bone, 2 feet showed vertical talus, and 2 feet had a marked osteoporosis, while 9 feet showed no radiographic tarsal anomalies. In another study by Harris and Beath, 13 they examined 17 feet and found that 12 feet had a talocalcaneal bridge, 3 feet had calcaneonavicular bar, and 2 feet had tarsal rheumatoid arthritis.
In the present study, most of the patients started complaining after the age of 13, and most patients reported a recent involvement in strenuous activities or foot trauma. This coincides with what was reported by Seddon who suggested that although tarsal anomalies are developmental, 14 clinical symptoms only appear in late childhood as the interference in smooth action of mid tarsal joints was compensated for by their cartilaginous coverage which is lost at the age of 12–14 and Blockey who found that the symptoms had appeared in late adolescents or in patients who had recently acquired more heavy activities. 2 Pauk and Ezerskiy highlighted the importance of controlling body weight, 15 physical activity to reduce complications, and the consequences of flatfeet. However, the relationship between a patient’s body weight and pes planus (and the associated effects on pain and function) are inconclusive. 16
Although the best improvement was reported in patients in whom full inversion could be achieved under anesthesia, full inversion could not assure or guarantee the absence of relapse. In groups I and II, there was 70% rate of relapse (partial and complete) at the last follow-up, while cases that couldn’t be manipulated with persistent loss of inversion showed less satisfactory functional outcome with higher rates of recurrence at the last follow-up.
We can conclude that mobility of foot under general anesthesia does not necessarily mean absence of tarsal anomalies and on the other hand, the presence of tarsal anomalies does not necessarily mean that the foot will be rigid under general anesthesia. On the other hand, radiographic findings denoting tarsal anomalies have a significant correlation with the occurrence of partial or complete relapse in the studied cases during the follow-up period. Partial relapse had occurred in cases with or without radiographic tarsal anomalies, while complete relapse had not occurred in cases with no radiographic tarsal anomalies.
Compared to the body weight and activity level, mobility of the feet under G/A and the severity of the radiographic abnormalities are the most important factors that could affect the outcome of the treatment and the rate of recurrence. Mobility of foot under general anesthesia markedly affects improvement and patients’ satisfaction, while the severity of the radiological abnormalities markedly affects the rate of recurrence.
The relatively small number of cases in this study with a relatively short-term follow-up period and the absence of a control group with another method of treatment represent the limitations of this study; however, these limitations do not undermine the results achieved by this study.
Conclusions
Symptomatic spasmodic valgus foot could occur without the presence of a frank bony tarsal coalition. Manipulating the deformed foot under general anesthesia combined with sinus tarsi injection with steroids with a protective cast in the neutral position could be an easy, simple, and reliable nonsurgical treatment for adolescent rigid planovalgus foot secondary to peroneal or peroneo-extensor spasm. Apart from limited recurrence, the overall clinical results were very satisfactory and encouraging. Mobility of foot under general anesthesia does not necessarily mean the absence of radiographic tarsal anomalies and the presence of the radiographic tarsal anomalies does not necessarily mean that the foot will be completely and permanently rigid. The degree of the foot mobility under general anesthesia and the radiographic tarsal anomalies were the main factors predicting the clinical results and recurrence of symptoms. Mobility of foot under general anesthesia markedly affects improvement and patients’ satisfaction, while the severity of the radiological abnormalities markedly affects the rate and type of recurrence. Partial relapse could occur with or without the presence of radiographic tarsal anomalies, while complete relapse did not occur in cases with no radiographic tarsal anomalies.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
