Abstract
Aim:
Early tendon transfer has shown good outcomes in peripheral nerve injuries of upper limb. However, there is lack of knowledge on early tendon transfer for peripheral nerve palsy in lower limb. This study has been designed to study the functional outcomes of early tendon transfer in the lower limb, particularly for foot drop.
Patients and Methods:
We enrolled 30 cases of foot drop due to traumatic sciatic/common peroneal nerve (CPN) palsy between September 2012 and March 2016. We performed nerve exploration with repair and early tendon transfer in all patients. All patients were followed up for a minimum period of 24 months. Functional evaluation was carried out using Stanmore assessment questionnaire.
Results:
At the end of 24 months postoperatively, the Stanmore assessment questionnaire score showed a significant improvement from a mean preoperative score of 17.5 to mean postoperative score of 86.2. All patients were free of ankle–foot orthosis (AFO). All patients were subjectively satisfied. Time to return to original job was 5.2 months on an average. Ankle dorsiflexion of the operated limb was comparable to the normal limb in cases where there was nerve recovery. Planovalgus foot, a known complication of this procedure, was noted in 24 patients. However, it was not disabling to any patient.
Conclusion:
Early tendon transfer in CPN palsy/sciatic nerve palsy has a definite place in the management of the injured patient. The transfer, if appropriately carried out, acts as a helper, an internal splint, a substitute, or perhaps all of the three at varying times in the rehabilitative phase of the patient. Dorsiflexor clearance in swing phase of locomotion was quickly restored in all patients, obviating the need for AFO.
Introduction
Common peroneal nerve (CPN) palsy has been reported as the most frequent lower extremity nerve palsy and the most common cause of foot drop in clinical practice. 1,2 Foot drop leads to functional deficits and devastating consequences such as inability to walk normally, functional limitation of activities, dependence on orthosis, and deformity of the foot. Inability to dorsiflex the foot is the most important functional deficit in foot drop due to CPN or sciatic nerve palsy. The sciatic nerve and CPN recovery after repair in case of palsy is usually unpredictable and delayed because of excessive nerve length, abundance of connective tissue, imbalance between the normal function of plantar flexor muscles and the passively stretched foot and toe extensors, which are inactive because they are paralysed. 3 Excessive contracture of the active muscles and shortening of the heel cord may represent a severe obstacle to re-innervation. Restoration of dorsiflexion of the foot by tendon transfers should be done early as this function allows near normal functional activity in individuals. Considering the fact that gait and foot function is vital to carry out almost all routine activities, it is imperative to stress the need for adopting the concept of early tendon transfer for foot drop. This will not only be helpful in better rehabilitation but also be helpful in achieving a near normal function as early as possible.
Patients and method
The study was conducted in a tertiary level referral and teaching institute between September 2012 and March 2016. The study was prospective including a total of 30 cases of foot drop due to traumatic CPN palsy, who were operated after obtaining a written and informed consent. In all cases, the tibialis posterior (TP) tendon transfer was performed. Nerve exploration and repair of CPN was carried out in all patients. Cases with power less than Medical Research Council (MRC) grade 4 of the muscle to be transferred, ankle and subtalar joint stiffness of the involved side, weakness of gastrocnemius–soleus complex, and significant soft tissue scarring of anterior ankle were excluded from the study.
Preoperative evaluation
Evaluation of gait, functional status, Stanmore assessment, and MRC muscle grading of lower limbs, local condition of foot, musculoskeletal stability, and foot were carried out clinically.
Surgical technique
Under appropriate anesthesia, under tourniquet, after exanguination with an Eschmarch bandage, nerve exploration and repair was carried out using standard approach (Figures 1 and 2). TP tendon transfer was carried out as follows.

CPN exploration. CPN: common peroneal nerve.

End-to-end epineural neurorrhaphy.
The first incision was made on the medial side of the ankle beginning distally at the insertion of the TP tendon and extending proximally over the tendon just posterior to the medial malleolus and from there proximally along the medial border of the tibia for 5 to 7.5 cm. The TP tendon was freed from its insertion on the navicular bone (Figures 3 and 4).

Incision for harvest of tibialis posterior tendon.

Tibialis posterior tendon harvested.
The second skin incision anteriorly was given distally 5–7 cm proximal to the ankle joint, and extended proximally for 7.5 cm just lateral to the tibialis anterior tendon. The TP tendon was freed from its sheath up to the musculotendinous junction and delivered proximally.
The third skin incision was made laterally beginning 5–7 cm proximal to the lateral malleolus and extending proximally for another 6–7 cm (Figure 5). The dissection was carried deep between the tendons of the tibialis anterior and the extensor hallucis longus (EHL), carefully preserving the neurovascular bundle. The interosseous membrane was exposed (Figure 6) and a window was made in the interosseous membrane.

Incision for tendon transfer.

Interosseous membrane.
The TP tendon was passed through the window between the bones, ensuring that it was not kinked, twisted, or constricted, and that the vessels and nerves to the muscle were not damaged (Figure 7).
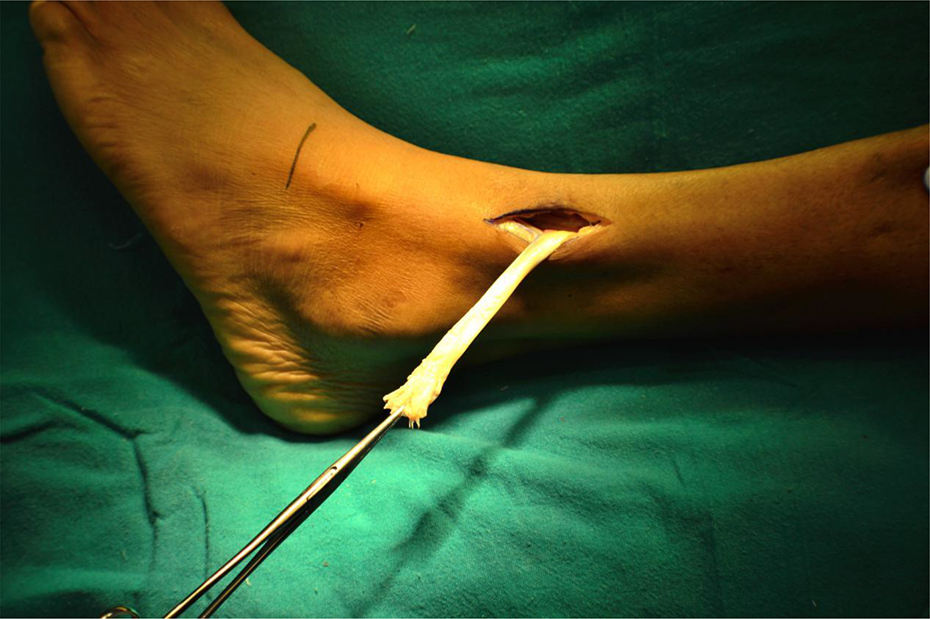
Tendon delivered through the interosseous membrane.
The fourth skin incision was made which exposed the third cuneiform or the base of the third metatarsal or the second metatarsal through a longitudinal incision 2.5 cm long. The extensor tendons were retracted and the periosteum was sharply incised over the bone in a cruciate fashion (Figure 8), and the osteo-periosteal flaps were folded back. A drill hole was made through the bone, that is, the second or the third metatarsal base or the medial cuneiform in line with the tendon and large enough to receive it and anchored it in the bone with either a pullout wire which was fixed with a button on the plantar surface of the foot or with a 3.5 mm cancellous screws with a figure of eight anchoring sutures around the screw. The insertion was modified according to the power of peronei muscles. The incision was closed, and a plaster cast to hold the foot in neutral position was applied.

Fixation of tendon to base of second metatarsal.
In cases where there was only deep peroneal nerve injury, the transferred tendon was fixed to medial cuneiform juxta position to the base of second metarsal (n = 6). In cases where the peronei were nonfunctional, the tendon was fixed to base of third metatarsal to allow eversion along with dorsiflexion.
Postoperative regimen
An above knee plaster cast with knee in 90° flexion was applied in patients where nerve repair with end-to-end anastomosis was carried out. A below knee plaster cast was applied in patients where nerve repair was not carried out. At the end of the second postoperative week, a window was made in the cast in all the cases for removal of the sutures. In cases where an above knee cast was applied, a window was made in the posterior aspect of the knee and the knee was progressively extended by 10° and the cast was reinforced at weekly interval. At the end of the sixth postoperative week, the circular above knee cast was converted to a below knee cast, and bivalve of the cast at the foot extending from ankle up to the toes was carried out to allow the training of the ankle dorsiflexion. At the end of the eighth postoperative week, the cast was removed and replaced by an ankle and foot orthosis in neutral position, which was continued for another 4 weeks. The active dorsiflexion of the ankle was initiated with retraining of the transferred muscle, and the plantar flexion of the ankle was not allowed during this time. Gait training was also given to prevent the disordered gait from interfering with the use of the tendon transfer.
At the end of the third postoperative month, the patient was allowed to apply full load on the affected limb.
Pre- and postoperative evaluation using Stanmore system was carried out (Table 1; Figure 9).
Stanmore assessment questionnaire.


Stanmore score distribution in all cases.
Results
Total number of patients included was 30 (n = 30); 60% (n = 18) of the patients belonged to second and third decade of life. There was a mean delay of 6 months from time of onset of foot drop to surgical intervention (Table 2). All patients showed a grade 0 power in tibialis anterior and EHL. TP had a grade 5 power in all cases.
Details of cases.

The Stanmore assessment questionnaire components showed a significant improvement in all parameters. All patients were free of ankle–foot orthosis (AFO) postoperatively (22 cases at the end of third postoperative month, six cases at the end of sixth postoperative month, and two cases at the end of seventh postoperative month). In the long-term follow-up of cases (n = 12) with a follow-up period of at least 48 months, there was a significant improvement in functional status of all cases, with increase in Stanmore score. All patients were able to return to their job early (mean 5.2 months) and satisfactorily carry out all routine activities.
There was valgus deformity and flat foot noted in 24 cases (Figure 10). Plantar flexion was also restricted (Figure 11). These were the known complications of the procedure. However, neither of the complication was disabling to the patients. Twenty-two cases showed neurological recovery. Ankle dorsiflexion of the operated limb was comparable to normal limb in cases where there was nerve recovery.

Restricion of plantar flexion after transfer.

Planovalgus deformity.
Discussion
With the acclaimed success of the early tendon transfer surgery for peripheral nerve injuries of the upper extremity, it was but natural for us to consider that a similar approach for nerve injuries of the lower extremity, predominantly the sciatic and the CPN injuries would also be able to restore function quickly. With this premise, an early TP tendon transfer was performed in cases of foot drop along with peripheral nerve reconstruction wherever indicated.
In our study, there were 30 traumatic cases of foot drop, of which 24 cases were associated with open wounds and 6 cases due to closed injuries. One steadily rising cause of nerve injuries in our society is road traffic accidents. It is important to note that most of the nerve injuries can be prevented through proper education. Also, nerve injuries should be carefully excluded in every patient with an acute extremity injury. Equal diligence should be applied in evaluation after surgery, manipulation, casting, and recovery from skeletal injury to detect secondary neural injury.
Wood in his study on surgical repair of peroneal nerve in 11 patients reported excellent or good results in 54.5% patients 3 . Garozzo et al. in their study on 62 patients of CPN palsy, where nerve repair with or without tendon transfer was carried out, reported that nerve repair associated with tibialis tendon transfer dramatically improved the postoperative outcome and at 2-year follow-up, neural regeneration was demonstrated in 90% of the patients 4 . Surgical outcome depends on the causative mechanisms of the lesion: sharp injuries and severe dislocations of the knee had an excellent recovery, while in crush injuries and gunshot wounds good recovery was less common. 5 –8 In our study, all patients had a minimum of 2-year follow-up, with 73.3% (n = 22) showing neurological recovery (Table 3).
Comparison of results of studies on CPN repair with/without tendon transfer.

Kim et al. in his study reported that all patients operated with tibialis tendon transfer were free of the kick up brace and walked with a near normal gait. 10 In our study, all patients were of AFO by a mean of 3.9 months. Gait was analyzed at 4 months when most patients were off AFO. Gait was comparable to contralateral limb.
Vigasio et al.
9
in their study on new tendon transfer for correction of foot drop had a mean delay of 33.3 months from the time of initial trauma to surgery. This delay contraindicated any attempt at microsurgical reconstruction. The Stanmore score at the mean of 65.12 months was as follows. Excellent: 56.25% Good: 25% Fair: 6.25% Poor: 12.5%
In our study, there was a mean delay of 6 months from the time of initial trauma to surgery. Hence, exploration of nerve and early tendon transfer was found to be more beneficial. The Stanmore score at the mean of 30 months in our study was as follows: Excellent: 70% Good: 30% Fair: 0% Poor: 0%
All cases were followed up for more than 24 months duration. There was a significant improvement in all parameters of Stanmore assessment questionnaire score. Valgus and flat foot deformity was observed in 24 cases which are also the known complications.
Garozzo et al., in their study on surgical treatment of common peroneal injuries, stated that among the several factors advocated to explain the poor outcome following surgery, it has been suggested that re-innervation might be obstacled by the force imbalance between the functioning flexors and the paralyzed extensors that eventually results in the fixed equinism of the foot, due to the excessive contracture of the active muscles and the shortening of the heel cord. Therefore, the early correction of these forces might favor nerve regeneration. Following such hypothesis, the authors treated irreversible CPN injuries performing a one-stage procedure of nerve repair and tibialis tendon transfer. Outcome of nerve repair only was highly disappointing with poor recovery. Nerve repair associated with tibialis tendon transfer dramatically improved the postoperative outcome. At 2-year follow-up, neural regeneration was demonstrated in 90% of the patients.
According to their experience, the association of a transfer procedure to nerve repair enhances neural regeneration, dramatically improving the surgical outcome of the CPN injuries.
In our study, we have performed early tendon transfer in all the cases. This included CPN exploration with repair and TP tendon transfer carried out in all cases. There was a dramatical improvement in surgical outcome of 22 patients who had neurological recovery. This correlated with the earlier study which states that a transfer procedure to nerve repair enhances neural regeneration.
Valgus deformity of foot and flat foot were the complications noted in long-term follow-up cases. Valgus deformity of foot was due to the loss of inversion as a result of TP tendon transfer and/or recovery of nerve palsy, that is, the peronei muscle action. Flat foot deformity was due to the loss of one of the prime stabilizer (TP tendon due to tendon transfer) of medial arch of the foot.
Neither of the complications was disabling to the patients and all patients had a very good functional status.
Flexor digitorum longus (FDL) transfer is a well-established substitute to the function of TP. There were no functional disability noticed by any patient due to loss of TP function and the planovalgus deformity was observed by the surgical team on follow-up. No further reconstruction, including FDL tendon transfer, was therefore considered in our cases.
Conclusion
Early tendon transfer in CPN palsy/sciatic nerve palsy has a definite place in the management of the injured patient. The transfer, if appropriately carried out, may act as a helper, an internal splint, a substitute, or perhaps all of the three at varying times in the rehabilitative effort of the patient. The transfer aids in early restoration of the foot function, prevents contractures at the same time and does not compromise the ultimate result if significant motor recovery occurs following neurorrhaphy, and allows the patient to be splint free during the period of axon regrowth. Early transfer also helps in reducing the time off work. The TP tendon transfer is considered the gold standard for correction of foot drop. The concept of early tendon transfer for foot drop gives very good results objectively and very good subjective satisfaction and improvement in functional status.
Keeping in mind, the long distance to be covered by the newly regenerating axons, in axonotmetic injuries and following nerve repair surgery in neurotmetic lesions, it makes all the more sense to combine early tendon transfer with nerve reconstruction surgery. Although it has been proposed that tendon transfer surgery has the capability of improving neuronal regeneration, this needs to be backed up by scientific evidence at present. This would therefore be a subject of future studies.
The fear that neurological recovery in future may result in a deformity has been the prime deterrent to early tendon transfer in the past. Tendon transfer having been reserved only for cases in which recovery failed to occur. A valgus deformity in this study did occur but did not cause any significant functional compromise. The fact that neurological recovery was observed in 22 cases of CPN palsy around 1 year, early tendon transfer significantly shortened the period of external splintage in these cases.
This study strongly supports the performance of early tendon transfer for all foot drop cases.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
