Abstract
Amputation still considered as primary choice of malignancy treatment in distal tibia. Bone recycling with liquid nitrogen for reconstruction following resection of malignant bone tumours offers many advantages. We presented four patients with osteosarcoma, Ewing sarcoma, adamantinoma and recurrent giant cell tumour over distal tibia. All of the patients underwent wide excision and bone recycling using liquid nitrogen as bone reconstruction. The mean functional Musculoskeletal Tumor Society (MSTS) score was 75% with no infection and local recurrent. The reconstruction provides good local control and functional outcome.
Keywords
Introduction
Amputation still considered as primary choice of malignancy treatment in distal tibia especially if the tumour become extensive. The complexity of distal tibia made the limb salvage treatment difficult to do and patient often has a very limited limb function. 1,2
Improvement in prosthetic and engineering design allow patient treated with amputation to have a very good limb function and capable to participate in daily activities. But, since major advances in diagnostic imaging, neoadjuvant chemotherapy and operative technique development, there was a shift from amputation into limb salvage reconstruction methods such as allograft, microvascular fibula transfer, bone transport, prosthesis or allograft composites prosthesis. 1 –3
In our country, patient with malignant tumour of distal tibia mostly refuse amputation as treatment due to local culture; therefore, we decide to try limb salvage surgery as a treatment for malignant bone tumour of distal tibia.
Various techniques for reconstruction of the bony and soft tissue defect following resection of malignant bone tumours have been described, and one of them use bone recycling with liquid nitrogen. This method provides advantages, such as simplicity, osteoinduction, osteoconduction, a short treatment time, preservation of the cartilage matrix, a perfect fit and sufficient biomechanical strength, less infection rate, eliminate the need for a bone bank, easy attachment of tendons and ligaments and desirable bone stock. 4 –6
Case reports
Patient 1
A 29-year-old male complained of pain and lump on his left leg. Physical examination revealed palpable mass with 4 × 3 cm in size. Range of motion of the ankle was limited (Figure 1(a)). Plain radiograph shows an osteolytic lesion in the metadiaphysis of the distal tibia with soft tissue mass (Figure 1(b)). Histopathology result after open biopsy revealed undifferentiated pleomorphic sarcoma. Neoadjuvant chemotherapy was administered three courses before surgery with doxorubicin and cisplatin regiment.

Patient 1: (a) clinical picture of the left leg showed lump and palpable mass. (b) Preoperative radiograph revealed osteolytic lesion in the metadiaphysis of the distal tibia with soft tissue mass. (c) Excised portion before and after being frozen in liquid nitrogen. (d) Post-operative radiograph. (e) Three-year post-operative radiograph showed bony union process.
Three months later, patient underwent wide excision of distal tibia and fibula. Tumour mass on the distal part of the tibia was curretaged, and the excised portion was frozen in liquid nitrogen for 20 min, thawed at room temperature for 15 min and thawed in distilled water for 10 min (Figure 1(c)). It was used to fill the bone defect followed by fixation by plates and screws. Bone cement was used to enhance the strength of bone for mechanical support, and we performed arthrodesis at the distal part of the ankle with screws (Figure 1(d)). External support was maintained until 4 weeks post-operatively. Adjuvant chemotherapy was administered three courses after surgery with doxorubicin and cisplatin regiment.
Three years later, the functional outcome was 73% using MSTS score without any sign of deep infection and skin necrosis. Follow-up radiograph shows a bony union process of the proximal and distal part of tibia with no sign of recurrence and metastases (Figure 1(e)).
Patient 2
A 6-year-old girl presented with pain and lump on her right leg since 7 months. Patient was unable to walk because of the pain. Physical examination reveals a 4 × 6 cm solid mass with limited ankle active range of motion (Figure 2(a)). Plain radiograph shows a permeative lytic lesion on metadiaphysis of distal tibia with periosteal reaction (Figure 2(b)). The biopsy result was Ewing sarcoma. Neoadjuvant chemotherapy was administered with ifosfamide, mesna and etopuside for three courses before the surgery.

Patient 2: (a) clinical picture of the left leg showed lump with solid mass. (b) Preoperative radiograph reveals a permeative lytic lesion at distal end of left tibia with periosteal reaction. (c) Excised portion before and after being frozen in liquid nitrogen. (d) Three-year post-operative radiograph showed bony union process.
Three months later, the patient underwent a wide excision of the tibial compartment. All the structures in the anterior and lateral compartment were preserved. After wide excision, the tumour portion was curretaged, and then, it was frozen in liquid nitrogen for 20 min, thawed in room temperature for 15 min and thawed for 10 min in distilled water (Figure 2(c)). It was used to fill the bone defect and fixated using plates and screws, and ankle arthrodesis was performed. Bone cement was used for mechanical support.
Radiotherapy and adjuvant chemotherapy was administered after the surgery until approximately 1 year. Three years after the surgery, the functional outcome was 80% using MSTS score. The radiograph shows a bony union process of the proximal and distal part of the tibia with no sign of recurrence and metastases (Figure 2(d)).
Patient 3
A 51-year-old male complained of pain and lump on his right leg since 3 months. Physical examination revealed palpable mass 5 × 6 cm size on medial part of the leg with limited range of motion of his ankle (Figure 3(a)). Plain radiographs revealed an osteolytic lesion in the metadiaphysis of the distal tibia, geographic type of destruction with eroding cortex and soft tissue mass arising from bone (Figure 3(b)).

Patient 3: (a) clinical picture of the left leg showed lump with palpable mass on medial part of the leg. (b) Preoperative radiograph revealed an osteolytic lesion with geographic type in the metadiaphysis of the distal tibia. (c) Excised portion before and after being frozen in liquid nitrogen. (d) Three-year post-operative radiograph showed bony union process.
The core biopsy result was adamantinoma. One month later, patient underwent wide excision. All the components on the anterior and lateral compartment were preserved. Tumour portion was curettage from the bone; then, it was frozen in liquid nitrogen for 10 min, thawed in room temperature for 15 min and thawed for 10 min in distilled water (Figure 3(c)). Fibular graft was used as inlay graft to gain mechanical support. We performed arthrodesis at the distal part of the ankle using plates and screws.
The histopathology result confirms an adamantinoma. Three years after the surgery, the functional outcome was 75% using MSTS score. Follow-up radiograph shows a bony union process with no sign of recurrence and metastases (Figure 3(d)).
Patient 4
A 20-year-old female complained of pain and lump on her left leg with radiograph showing a geographic type of lytic lesion at distal end of left tibia. An extended curettage was performed and the defect was filled with bone cement followed by fixation using plate and screws. The histopathology result revealed a giant cell tumour. Two years later, the clinical study revealed solid mass 5 × 3 cm in size, located on distal leg with normal ankle movement (Figure 4(a)). The radiograph showed signs of recurrence (Figure 4(b)).
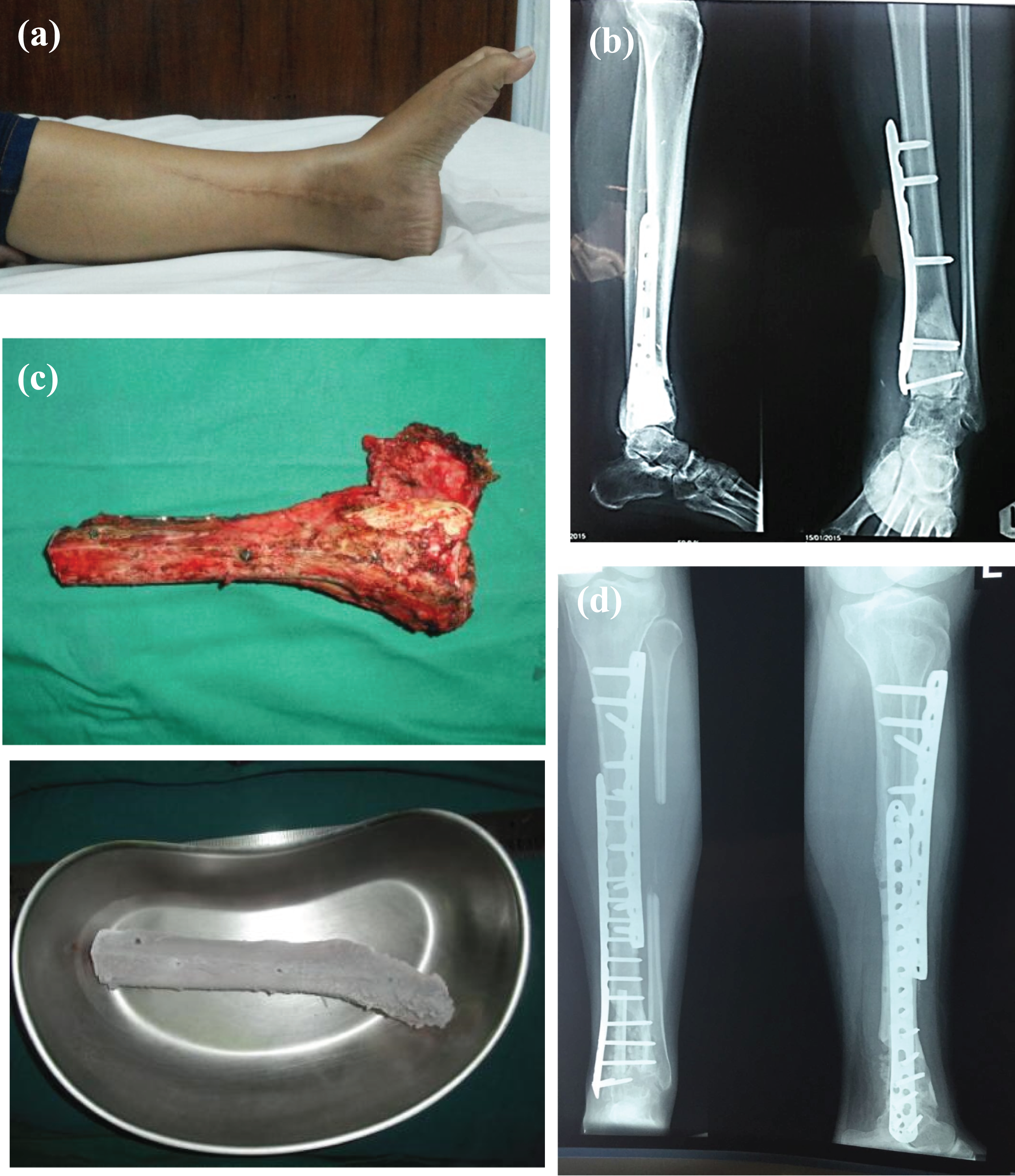
Patient 4: (a) clinical picture of the left leg showed recurrence pain and swelling over the distal aspect of the leg. (b) Radiograph revealed recurrence of giant cell tumour. (c) Excised portion before and after being frozen in liquid nitrogen. (d) Three-year post-operative radiograph imaging showed bony union process.
A wide excision and ankle arthrodesis were performed. The remaining excised bone was frozen in liquid nitrogen for 20 min, thawed at room temperature for 15 min and thawed in distilled water for 10 min (Figure 4(c)). Fibular graft was used as inlay graft to enhance the mechanical support. We performed arthrodesis at the distal part of the ankle using plates and screws.
Follow-up after 3 years revealed 75% functional outcome using MSTS score, and radiograph result shows a bony union process with no sign of recurrence and metastases (Figure 4(d)).
All cases used standard protocol for liquid nitrogen freezing at −196°C for 20 min as hypothermia method to treat the bone containing the tumour. The polymethyl methacrylate (PMMA) without antibiotic was used in addition to mechanical support.
The bony union takes an average time of 9 months, and it is the same on both ends of the autograft. Bone grafting was undertaken to enhance bony union in all cases. An external support with back slab was maintained until the post-operative wound healed and then continued with circular cast for 3 months to allow protection post reconstruction. The patients were not allowed to weight bear for at least 6 months.
The MSTS scores revealed more than 75% functional outcome. This scoring system was based on pain status, functional restriction, emotional status, usage of supports, walking limitation and gait.
Discussion
Although various biological and nonbiological options are available, there is no gold standard technique for reconstruction after tumour resection of malignant and recurrent benign aggressive bone tumour of distal tibia. Currently, amputation still considered as primary choice for malignancy treatment in distal tibia especially if the tumour become extensive. 1 –3 A shifting treatment option for limb salvage was considered by some reasons to achieve optimal psychological and functional outcome over survival and local recurrence rates.
A retrospective study conducted by Mavrogenis et al. comparing the outcome of limb salvage over amputation for distal tibia malignancy found 84% survival rate for limb salvage as compared to amputation with survival rate 74%. 1 The local recurrent in limb salvage was 13% compared to amputation with no local recurrent. The limb salvage also showed higher MSTS score of 76% compared with amputation which showed a score of 71%. Although the survival, local recurrence and complications were similar, the functional outcome for limb salvage showed better and achievable result than amputation. 1 This result showed similar results with our study which revealed 75% functional outcome after 3 years follow-up. But in our cases, signs of local recurrence and metastases were not found.
Two important factors must be considered in choosing amputation or limb salvage for malignant and recurrent benign aggressive bone tumour of distal tibia: survival rates should not be worse than amputation and the reconstruction must provide satisfactory limb function. 3 Improved advances in reconstructive surgery supported by a good to excellent MSTS score ensure that the limb salvage procedure is acceptable in such condition when compared with amputation.
The limb preservation procedure can be done by several techniques, such as, allograft, autograft with microvascular fibula transfer, bone transport, bone recycling with pasteurization or liquid nitrogen, prosthesis or composites. 3 A research by Brien et al. showed that patient with malignant and benign aggressive tumour of tibia who underwent endoprosthetic reconstruction had prosthetic loosening and infection. 7 Another study by Natarajan et al. assessed oncological and functional results of limb salvage surgery using custom-made endoprosthetic replacement for distal tibia osteosarcoma. 8 The functional score was 81% but local recurrent and infection were reported (33%) during the follow-up. 8 –10 These data showed the possibility of prosthetic limb salvage use rather than amputation in spite of some complications.
A study conducted by Jeon et al. and Liu et al. showed that the use of pasteurized bone graft for primary malignant bone tumours of distal tibia indicated a satisfactory outcome with functional score of 74.3% and 86.7%, respectively. 9,10 But some complications occurred during the follow-up period. Jeon et al. reported infection (33%), nonunion (22%) and refracture (22%), whereas Liu et al. only reported infection (20%). 9,10 This technique is considered an accessible and economical alternative of high efficiency for reconstructive modalities but did not resolve complications that occurred.
In our study, using reconstruction technique with tumour-bearing massive frozen autograft/bone recycling treated by liquid nitrogen provides an excellent survival and functional score with MSTS score 75% with no complications (infection, nonunion or fracture) and also no local recurrent compared than below knees amputation nor another limb salvage procedure in 3 years of follow-up. A study conducted by Rahman et al. using reimplantation of resected tumour-bearing segment after recycling using liquid nitrogen for knee osteosarcoma gave a functional score of 82.4% over 4–5 years of follow-up with no local or systemic recurrence. 11 Paholpak et al. reviewed clinical results of primary malignant musculoskeletal tumour of tibia treated by wide resection and recycling autograft reconstruction using liquid nitrogen. 6 In 32 months of follow-up period, the functional score was excellent (79%) with 50% failures. About 33% were infected and 8% develop local recurrence but with good union rate. 6 These research are in line with our study that the reconstruction technique using tumour-bearing massive frozen autograft/bone recycling treated by liquid nitrogen offers an excellent survival and functional outcome without any complications and local or systemic recurrence.
We prefer the reconstruction technique using tumour-bearing massive frozen autograft treated with liquid nitrogen; as it provides several advantages, namely simplicity, osteoinduction, osteoconduction, a short treatment time, preservation of the cartilage matrix, a perfect fit, sufficient biomechanical strength, no infection, eliminate the need for bone bank, easy attachment of tendons and ligaments and desirable bone stock. 4 –6 The disadvantages are degeneration of the cartilage over time, the impossibility of histological analysis of the whole specimen and related complications similar to allograft implantation. Biomechanical testing showed no significant difference in compression strength between intact bone and the bone treated with liquid nitrogen, whereas in autoclaved bone, the strength was decreased. 4
The functional results are comparable with other methods of reconstruction, and once incorporated by the host, frozen autografts provide the advantage of incorporation bone stock and with soft tissue attachments, unlike metal implants. For osteoinduction, the activities of proteins and enzymes are preserved in bones treated in liquid nitrogen. Freezing with liquid nitrogen is widely used to measure and analyse tumour and healthy tissues in biomedical research. 5 Tumour-bearing autograft treated by liquid nitrogen is a simple and effective option for biological reconstructions. It is best used for osteoblastic tumours while prosthetic or allograft reconstruction should be used for osteolytic lesions. 12
Allografts used to reconstruct the bony defects after resection of a tumour offer many advantages, including reconstruction of the joint and incorporation of the graft to the host bone. However, the high incidence of complications makes the outcome unpredictable. Fracture is one of the common complications and is thought to result from revascularization of the allograft cortex. Chemotherapy increases the rate of fracture at the allograft junction. This phenomenon may be due to an allogenic immune response. Other complications include graft resorption, recurrence and nonunion. 5
Frozen autografts contain autogenous proteins, growth factors and cytokines and does not elicit an immune reaction. They have the advantages of early bony union and low risk of bone resorption in spite of some complications similar to allografts, such as infection, fracture, nonunion or graft failure, which was resulted from the use of dead bone. 5
Another important aspect of treatment by liquid nitrogen is cryoimmunology. It is possible that tissue proteins released from the frozen lesions have antigenic properties, which initiate an immune response directed against the tumour. There have been reports that metastatic tumour shave regressed after freezing of the primary tumour. Cryoablation of tumour tissue induces inhibition of secondary growth of the tumour and causes release of cytokines. Therefore, tumour-bearing massive frozen autograft may play a role in reducing local recurrence and lung metastasis by its cryoimmunological function. 5,13
Cartilage frozen with liquid nitrogen will progress to osteoarthritic change in time as it seen in osteochondral allografts. 14 Nevertheless, as bioengineering evolves, the ability to restore or repair cartilage may become a practical proposition. Recovery of chondrocytes has been observed in cryopreserved porcine articular cartilage by drilling a hole through the subchondral bone to the base of the cartilage. 4,5,14
Reconstruction with tumour-bearing massive frozen autograft treated with liquid nitrogen in malignant bone and soft tissue tumours is a simple and effective method of biological reconstruction. Long-term follow-up studies will provide more useful information and clarify the effectiveness of this study.
Conclusion
We conclude that the bone reconstruction procedure in malignant and recurrent benign aggressive bone tumour of distal tibia with bone recycling using liquid nitrogen is an excellent reconstruction option compared to amputation hence providing good local control and functional outcome without local recurrence and metastases.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflict of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
