Abstract
Background:
Bursitis of the snapping scapula is commonly a misdiagnosed problem. Extracorporeal shockwave therapy (ESWT) has been used successfully in the treatment of many chronic inflammatory conditions. The aim of this study was to assess and compare the effectiveness of ESWT in the treatment of scapulothoracic bursitis with the outcome of corticosteroid injection.
Methods:
Using the randomized controlled trials 43 patients with scapulothoracic bursitis were divided into two groups. Group 1 (n = 22) received three sessions of ESWT. Group 2 (n = 21) received a single local injection of 80 mg of methylprednisolone. Visual analogue scale (VAS) scores were recorded at each follow-up, whereas the level of satisfaction was evaluated using the Roles and Maudsley criteria.
Results:
In group 1, the average VAS scores after 1, 2, 3, and 6 months were 39, 30, 27, and 16, respectively, whereas, in group 2, the average VAS scores were 46, 44, 35, and 36, respectively. There was no statistical significance between the two groups in the first and second months. However, after 3 and 6 months, group 1 revealed lower average VAS scores compared to that of the second group with p-values (0.012 and 0.001), respectively. Roles and Maudsley criteria showed that first group patients were 46% excellent, 36% good, 14% acceptable, and 4% had poor results. However, second group patients were 24% excellent, 33% good, 19% acceptable, and 24% had poor results.
Conclusion:
We believe that ESWT is a beneficial and trustable method of treatment and can be strongly recommended in painful cases of scapulothoracic bursitis.
Introduction
Scapulothoracic joint role is so much crucial for the proper functioning of the upper limb; for this reason, any alteration in the scapular gliding movement on the posterior thoracic cage will have a serious detrimental impact on the shoulder girdle function. 1
The articulation of the scapulothoracic anatomy is complex. The osseous, ligamentous, and muscular periscapular relationships are intricate. Although the scapulothoracic pathology is commonly underestimated, 2 a thorough appreciation of the various muscular relationships and bursal planes is very crucial while evaluating scapulothoracic disorders. 2,3
Several bursae have been described to be located in areas with increased friction. Bursae are virtual spaces filled by a synovial membrane. Kuhn et al. had described two major and four minor bursae around the scapula. One of the major bursae is located between the serratus anterior muscle and the chest wall (the scapulothoracic bursa or infraserratus bursa), while the second major bursa is located between subscapularis and the serratus anterior muscles (subscapularis bursa or supraserratus bursa) (Figure 1). Biomechanical dysfunction of the scapulothoracic joint may lead to a symptomatic painful inflammation of these bursae. 4

An anatomical diagram, showing the major periscapular bursae.
Bursitis and crepitus of the scapulothoracic joint were described first by Boinet in 1867. 5 Milch modified the concept by specifying two different forms of scapulothoracic crepitus. 6 The osseous crepitus type, which is caused by an osseous pathology at the superomedial angle of the scapula, such as an osteochondroma in the scapulothoracic space, was named as the “snapping scapula” by Milch. The other form is less severe than the osseous form and has a soft tissue component, such as bursitis. But, nowadays, it is well recognized by clinicians that painful scapulothoracic bursitis is present most of the time without associated crepitus. 4
Radiological examination of the scapulothoracic bursitis includes plain radiographs, ultrasonography, and magnetic resonance imaging (MRI). Plain radiographs including a true anteroposterior and tangential trans-scapular (Y) views to help in identifying any skeletal abnormalities, scapular osteochondromas, a Luschka tubercle, and rib abnormalities. Ultrasonography was used to identify the bursal tissue dynamically; however, dynamic ultrasonography was not sensitive in detecting small bursal tissues in many cases. MRI was the gold standard imaging tool in identifying small fluid-filled bursal tissues. 7
Diagnosis of scapulothoracic bursitis and crepitus is still mainly clinical. 8 Most of the time, patients present with a history of pain during overhead activities or after a repetitive overuse of the shoulder. Most patients describe an audible crepitus with shoulder movements. Although the audible crepitus can be painless during overhead movements, pain can be severe enough to limit many daily activities. Physicians can feel crepitus and feel the snapping of the scapula most of the time. Pain is usually present at the superomedial angle of the scapula and radiating to the levator scapulae, trapezius, and rhomboid muscles. 8 –10
Nonoperative measures consisting of rest, systemic nonsteroidal antiinflammatory drugs (NSAIDs), local corticosteroid injection, modification of upper extremity-related activity, and physical rehabilitation should be the initial treatment of scapulothoracic bursitis. 11,12
Many patients respond well to conservative treatment, while others don’t. For those who don’t respond to nonoperative measures, operative interventions like partial open scapulectomy and arthroscopic bursectomy are a choice. 13
Extracorporeal shockwave therapy (ESWT) healing effect has been studied by many researchers in treating inflammatory conditions. Some investigators have demonstrated its efficacy in the treatment of many chronic inflammatory conditions around the heel, elbow, and the shoulder joint, 14,15 while other studies claimed that ESWT provides little or no benefit in terms of pain and function for tennis elbow and rotator calf pathologies. 16,17
A prospective randomized controlled study was conducted to assess the effectiveness of ESWT for the treatment of scapulothoracic bursitis (snapping scapula; soft tissue type) and to compare its outcome with that of corticosteroid injection of the scapulothoracic bursa. Till date, searching the Medline did not reveal any study showing the effectiveness of ESWT application on the scapulothoracic bursitis.
Patients and methods
Institutional ethical approval was granted by the Shifa University Hospital ethics of research committee under the reference number 346-90. A prospective study comprised of 43 patients diagnosed with scapulothoracic bursitis, divided into two groups. Demographic data related to the involved patients is demonstrated in Table 1.
Demographic data of the patients involved in the study.

ESWT: extracorporeal shock wave therapy.
Patients who did not have scapular osseous lesions, any previous surgery around the scapula, and any spinal congenital anatomies were included in this study, whereas patients with the history of neck discopathy or generalized neurological abnormality, nerve entrapment pathology of the upper limb, pregnancy, infection, tumors, a clotting disorder and who were on anticoagulant therapy, or had a heart pacemaker were excluded from this study.
Initially conservative treatment such as specific physiotherapy program (muscle strengthening and traction), rest, modification of shoulder activities, and antiinflammatory drugs had been attempted for at least 1 month in all patients before conducting the study in both groups. 9,11
An explanation of the purpose and the nature of the study was made for all patients before signing a consent form. During and after the follow-up periods, all patients were asked to quantify the pain according to the visual analogue scale (VAS), which is considered as a valid measure of acute pain with a good construct validity.
18
Whereas, after 6 months, all patients were asked to determine the level of satisfaction according to Roles and Maudsley criteria. The Roles and Maudsley scale is a subjective four-point rating scale that has been used by many investigators when reporting the results of shock wave therapy,
19
–21
which depends on measuring the residual pain compared to the pain before starting the treatment. It is composed mainly of four satisfactory conditions: Excellent: Patient has no pain with full movement and full activity. Good: Patient has occasional discomfort with full movement and full activity. Acceptable: Patient has some discomfort after prolonged activities. Poor: Patient has a pain-limiting activity.
Fifty-two patients had common complaints of pain during overhead activities and repetitive shoulder movements. Twelve patients described an audible crepitus associated with severe pain at the superomedial angle of the scapula radiating to the levator scapulae muscle, whereas the remaining patients did not recognize audible crepitus, but often referred history of pain around the superomedial scapular angle during repetitive shoulder activities. Physical examination revealed a crepitus in most of the patients accentuated with compression of the superomedial angle of the scapula against the chest wall during abduction and pain is decreased with crossing the arm to lift the scapula from the posterior chest wall.
Standard plain radiographies including anteroposterior and tangential views were obtained for all patients to exclude any skeletal abnormalities or any scapula-related tumoral conditions. A minimal form of dorsal scoliosis was detected in two patients who were excluded from the study. Dynamic ultrasonography was used to identify any bursal lesion around the scapulothoracic joint and the superomedial angle of the scapula; however, dynamic ultrasonography was not helpful in detecting fluid-filled small bursal tissues around the scapular bone. A cervical, dorsal, and scapular MRI protocol was used for all patients to exclude cervical or dorsal lesions that may cause periscapular pain and to evaluate the periscapular fluid-filled bursal tissues. Three patients, whose complaints were associated with cervical radicular discopathy, were excluded from this study.
In this study, the diagnosis of scapulothoracic burisitis was mainly related to the clinical presentation of the patients after excluding any other mimicking lesions in parallel to other studies in the literature. 22,23
All patients had increased pain with overhead activities and 12 of them had an audible crepitus with motion of the scapula. Most of patients had moderate-to-severe pain at the superomedial angle of the scapula and some of them even experienced severe pain even at rest. To confirm the clinical diagnosis, 3 cc of local anesthetic (1% lidocaine) was injected below the superomedial angle of the scapula; when it is followed by partial or complete pain relief, it is considered that patient’s pain is related to the inflamed bursal tissue. 23
After excluding 5 patients from the 52 patients included in this study, 47 patients remained. Of the 47 patients, 43 patients fulfilled the treatment protocols, and were divided into two groups.
Patients in this study were randomized using the close envelope technique to form two groups.
Group 1 patients (n = 22) composed of 14 females and 8 males with an average age of 43.2 ± 5.6 years, received three sessions of ESWT of 7–10 min depending on the patient’s tolerance without the application of local anesthesia, using the portable ESWT (BTL Industries Ltd, UK), 1 per week for 3 weeks. In each session, 1500 pulses of 0.1 to 0.15 MJ/mm2 and 2500 pulses of 1.4 to 2.1 bars were applied depending on the participant’s tolerance of pain. This power setting was defined as a low-energy treatment protocol. 24,25
The ESWT was applied to the area of the superomedial angle of the scapula with the patient’s arm in extension, adduction, and internal rotation trying to reach for the opposite scapula while the patient is prone (Figure 2).
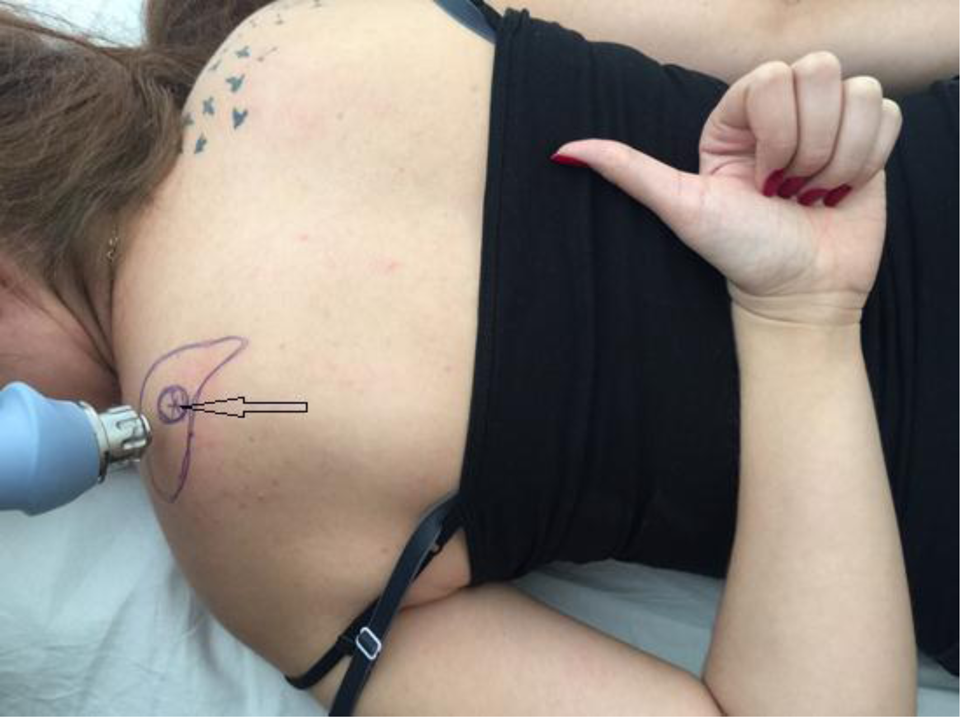
ESWT application at the scapulothoracic bursa area, while the arm in extension, adduction, and internal rotation pointing to the other scapula. The black arrow pointing at the point of the maximum tenderness on the superomedial scapular angle. ESWT: extracorporeal shock wave therapy.
Group 2 patients (n = 21) composed of 10 females and 11 males with an average age of 41.7 ± 2.3 years, received a single local injection comprised of 80 mg of methylprednisolone mixed with 3 cc of 1% lidocaine as a local anesthetic agent. Using an aseptic technique, the application of the local injection at the superomedial bursa of the scapula was done while the patient is lying in prone position with the shoulder in extension, internal rotation, and adduction, where the hand lies behind the back (the chicken-wing) position. The needle (1.5-inch 22–25 gauge) is angled 45° going from the proximal to the distal, entering just below the superomedial angle of the scapula taking care not to penetrate so deep as to cause a pneumothorax (Figure 3). 10 , 23

The corticosteroid injection was done while the arm in extension, adduction, and internal rotation pointing to the other scapula to prevent penetration of the scapula. The black arrow pointing at the point of the maximum tenderness on the superomedial scapular angle.
NSAIDs were not allowed during the study period. Patients in both groups were advised to rest and decrease the level of their activities to avoid aggravation of their symptoms.
All patients were assessed clinically at 1, 2, 3, and 6 months after the end of the treatment. The VAS scores were recorded at each follow-up, whereas the level of satisfaction was evaluated for all patients using the Roles and Maudsley criteria at the end of the follow-up.
For statistical analysis the Mann–Whitney U-test was used. The level of significance was set as p < 0.05.
Results
Patients in both groups were evaluated by the VAS system 1, 2, 3, and 6 months after completing the treatment protocol, whereas all patients’ satisfaction levels were evaluated at the end of the follow-up period using the Roles and Maudsley criteria (Table 2).
Pretreatment and posttreatment values of the VAS scores and the Roles and Maudsley criteria measuring the patient’s satisfaction level.

VAS: visual analogue scale; ESWT: extracorporeal shock wave therapy.
In the pretreatment period, the average VAS of the first group was 76, whereas it was 73 in the second group. No statistical significance was detected between both groups in the pretreatment period with a p-value of 0.18.
In the first group (ESWT group), after three sessions of ESWT application, the average VAS scores after 1, 2, 3, and 6 months were 39, 30, 27, and 16, respectively. Whereas, in the second group (corticosteroid group), the average VAS scores after 1, 2, 3, and 6 months were 46, 44, 35, and 36, respectively.
There was no statistical significance between the study arms after 1 and 2 months of the follow-up periods with p-values (0.34, 0.62), respectively. However, 3 and 6 months after treatment, the first group (ESWT group) revealed a lower average VAS scores compared to that of the second group (corticosteroid group) with a significant statistical difference, p-values (0.012, 0.001), respectively.
Roles and Maudsley criteria were employed for all patients at the last follow-up session, 6 months after completing both treatment protocols. In the first group, of 22 patients, 10 (46%) had excellent, 8 (36%) had good, 3 (14%) had acceptable, and 1 (4%) had poor results. However in the second group, of 21 patients, 5 (24%) had excellent, 7 (33%) had good, 4 (19%) had acceptable, and 5 (24%) had poor results.
Discussion
ESWT had been introduced for the treatment of kidney stones. Many studies demonstrated the beneficial effect of ESWT in the treatment of musculoskeletal disorders. 26 Some animal trials demonstrated the potential of ESWT in accelerating soft tissue healing and reducing the associated pain through inhibition of the afferent pain receptor function and thus improving tissue angiogenesis by increasing tissue blood flow, 27 while other investigators claimed that ESWT provides little or no benefit in terms of pain and function for lateral elbow pain and rotator calf pathologies. 13 ,28
The wave energy protocol used for ESWT application around the shoulder joint varies widely in previously reported studies. However, in general, the trials conducted to the superficial soft tissue structures such as plantar fasciitis, lateral epicondylitis, and calcific tendonitis of the rotator calf muscles mostly used 1500–3000 shocks of a low-energy protocol applied to the site of maximum tenderness. It is usually applied at weekly intervals for three to five sessions. 25
Nonoperative treatment modalities should be the first line of treatment in scapulothoracic bursitis; however, in the case of failed conservative treatment, arthroscopic and open procedures maybe considered. 13,28
Ciullo et al. had applied iontophoresis and ultrasound to the undersurface of the superomedial border of the scapula to treat scapulothoracic painful bursitis and they have obtained fair-to-good results. 22
Percy et al. had described the application of ethyl chloride to the trigger area of the superomedial scapular angle; however, the results were not satisfactory. 23
Corticosteroid injections had been suggested by some researchers to be used for therapeutic and diagnostic purposes of scapulothoracic bursitis. For the injection to be safe and reduce the risk of pleural penetration and pneumothorax formation, they advised that the injection be performed while patient’s arm is in a position of extension, adduction, and internal rotation. 11,23
ESWT is considered by many patients as a painful and unpleasant treatment modality. For that reason, some investigators advised using local anesthesia before ESWT application, while others deny local anesthetic application of ESWT, since it had been reported to alter the soft tissue response to wave therapy. 19,29,30 In this study, local anesthesia had not been employed before ESWT application.
Till date, ESWT has never been employed in the treatment of painful scapulothoracic bursitis in snapping scapula. To our knowledge, this is the first study documenting the effectiveness of ESWT in the treatment of painful scapulothoracic bursitis in snapping scapula.
Besides being a noninvasive modality of treatment, ESWT doesn’t carry the risk of serious complications like pleural penetration, which maybe encountered by corticosteroid injections and arthroscopic procedures. 23,28
During our study, no major side effects were encountered; only four patients in the ESWT group developed myalgia but recovered within a few days. Two patients in the corticosteroid group developed severe burning at the injection site for 2–3 days, which gradually disappeared within a week.
Our study demonstrates clearly that, the effectiveness of ESWT starts to increase gradually after application in a steady status, which in turn reflects the potential soft tissue healing effect of the wave therapy. However, in the corticosteroid group, the VAS dropped at the early follow-up and rose up again at the end of the follow-up period.
At the end of the follow-up period, we reported four patients in the ESWT group with acceptable results. Out of the four patients, three patients accepted to have an extra two ESWT sessions, whereas one patient refused the offer. One patient’s pain level improved from an acceptable level to a good level, whereas the remaining two patients’ pain levels did not change.
One patient of the ESWT group demonstrated a poor result even after applying two extra ESWT sessions. Corticosteroid injection had been tried for him, but no improvement was seen.
However, this study has several weaknesses. The patient population was small, the follow-up period was short, and a single ESWT protocol (low-energy protocol) was applied in this study. Further studies should be conducted on a larger patient population with different ESWT protocols.
Conclusion
Both ESWT and corticosteroid injection groups demonstrated comparable results regarding the reduction of pain level and overall condition of the satisfaction rate. We believe that ESWT is a beneficial and trustable method of treatment and can be strongly recommended in painful cases of scapulothoracic bursitis.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
