Abstract
Background:
There is a paucity of literature regarding the incidence of concussions in facial trauma. Prompt identification of concussion is crucial for patient recovery. The purpose of this retrospective study is to evaluate the relationship between facial trauma and concussion symptoms.
Keywords
Introduction
Concussion is defined as “a temporary disruption in normal brain function after a mechanical impact or transmission which results in transient changes in neurological function, displays no evidence of structural brain damage on computed tomography (CT) of the brain, and may or may not involve loss of consciousness.” 1 The diagnosis of concussion relies solely on history and physical examination, rendering it a diagnosis that can be difficult to identify. However, prompt identification of concussion is crucial for patient recovery. In plastic surgery, facial trauma cases often present and are managed according to the fracture with little regard to subclinical neurological symptoms. Screening craniofacial examinations offer high-level gross examination of neurological function and do not overlap with concussion symptoms. In current literature, there is limited research investigating the incidence of concussions in facial trauma.
Most traumatic brain injuries (TBIs) are classified as mild, demonstrating a post-resuscitation GCS of 13-15. Concussion is a sub-category of mild TBI in which no evidence of structural brain in jury is found on CT. 2 Facial injuries are closely related to concussions as the facial skeleton is in direct continuity with the calvarium. At a UK major trauma center, concussions were reported in one third of patients with facial injuries. 3 While these findings were based on a cohort largely admitted directly from the emergency department (ED), not all facial trauma patients require admission, with a significant number only requiring follow-up in an acute outpatient clinic within the window for any necessary surgical intervention. Current research reports that there is likely an underestimation of acute facial trauma cases with concurrent concussions, as more subtle symptoms such as concentration difficulties and mental fog are not frequently screened. 4 The purpose of this retrospective study is to evaluate the relationship between facial trauma and concussion symptoms and the prevalence of symptoms across the spectrum of facial injuries. The addition of a patient questionnaire for facial trauma patients was introduced as a quality improvement initiative at this clinic in response to the observed presence of concussion in some facial trauma patients. This study also serves a retrospective review of this clinical change of practice.
Methods
We evaluated 74 patients who presented to a facial trauma clinic at a Level 1 trauma center, Royal Columbian Hospital, in British Columbia (2019-2021). Patients with facial trauma were evaluated according to injury type, epidemiological, and demographic characteristics in the context of symptoms indicating clinically significant concussions. Patients that had been admitted to hospital for a closed head injury and then referred to the clinic were excluded. In addition, mandible fractures are outside the scope of practice in this clinic so are not included in this study as a fracture type.
Surveys were given to each patient attending the facial trauma clinic. A change of practice to survey the patients was made due to the observed presence of concussion in some facial trauma patients: a concussion specific questionnaire was introduced to help capture those patients suffering from related symptoms. After a one-year period this was reviewed as part of a clinical quality initiative. Fraser Health Authority (British Columbia) allows for practice review/patient quality of care improvement to be exempt from ethics review.
The objective metrics outlined in the survey include: date of injury, date of facial trauma clinic appointment, type of facial injury/fracture and loss of consciousness. Concussion presentation was captured using sixteen symptom metrics: dizziness, headaches, hearing changes, vision changes, balance changes, nausea and/or vomiting, light sensitivity, noise sensitivity, sleep disturbances, fatigue/tiring more easily, irritability/easily angered, depressed/tearful, anxious/tense, poor memory, poor concentration and mental fogginess. Each of the sixteen symptoms was rated on a Likert scale between 0 (no symptoms) and 3 (most severe) inclusive. The cumulative score out of 48 was deemed to be the concussion score. This was categorized according to mild (0-10), moderate (11-20), and severe (21+) concussion symptoms. Other parameters also investigated included binary responses for whether symptoms were worse with physical activity or worse with thinking/mental activity. Patients also reported if they felt different compared to normal (scale 0 to 10) and provided a written answer for current activity level percentage compared to normal.
Results
At this Level 1 trauma center clinic, 95% of patients presenting with facial injury had a clinically significant concussion symptom that affects quality of life—score greater than 0/48 (Figures 1 and 2). This can be stratified according to mild (0-10), moderate (11-20), and severe (21+) scores for concussion symptoms. Zygoma/zygomatic arch fractures had the highest mean concussion scores (Figure 3). Additionally, in almost all cases, zygoma and zygoma arch fractures have the highest concussion symptom score. Surgery cases with general anesthesia had worse mean concussion scores than no surgery or intervention under local anesthesia cases (Figure 4). For any concussion score, there is a higher proportion of patients with general anesthesia than any other. Local anesthesia has lower scores likely because all the injuries were either nose, upper 1/2, or mid 1/3 (the three injuries with the lowest symptom scores).
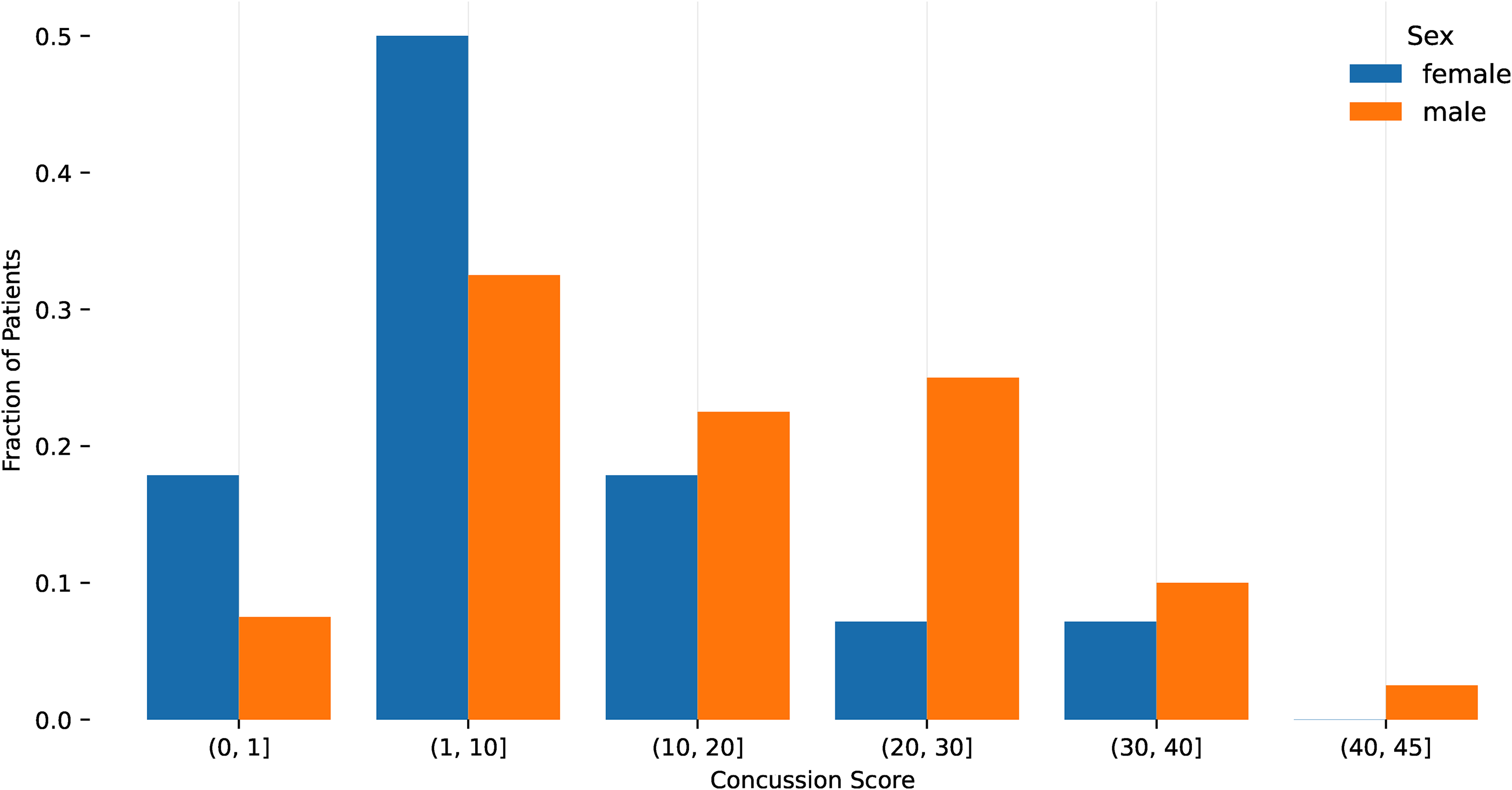
Percentage of patients with facial trauma experiencing concussion symptoms. Bar chart of patients with facial trauma according to their concussion scores.
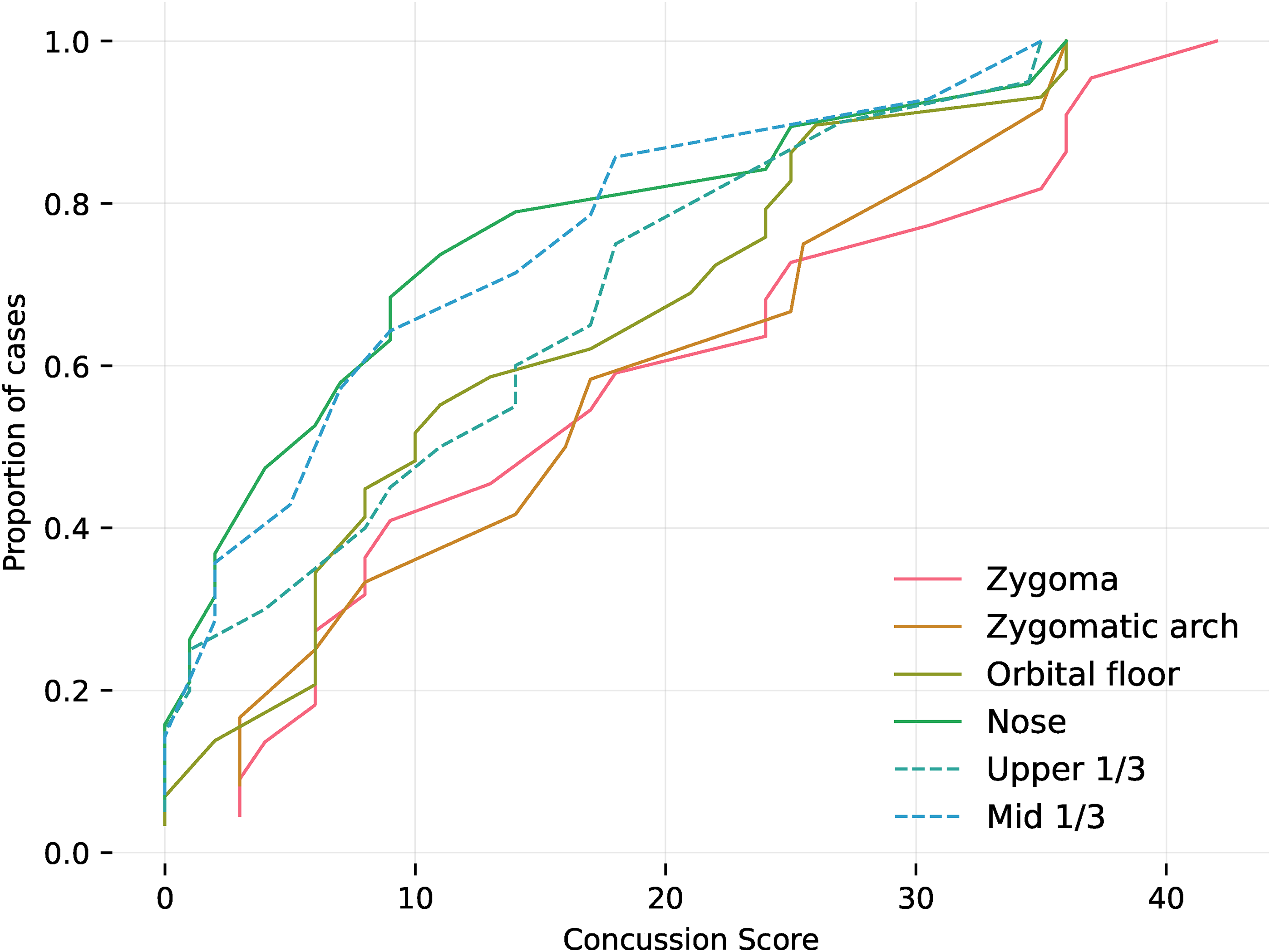
ECDF plot of patients with facial trauma according to their concussion scores.
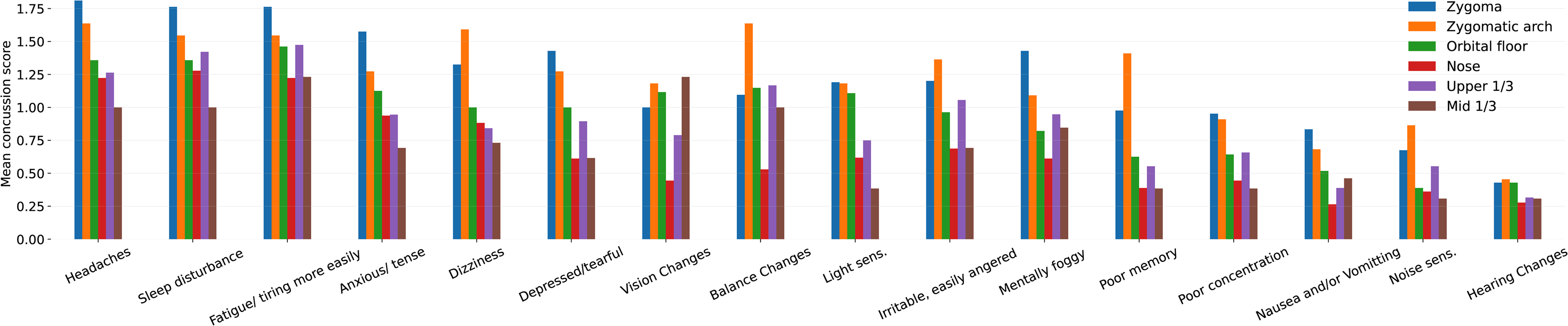
Bar plot of the mean symptom score for each fracture/laceration type (removing types with fewer than 5 patients)—the symptoms and fracture/laceration types are both sorted left to right by mean concussion score.
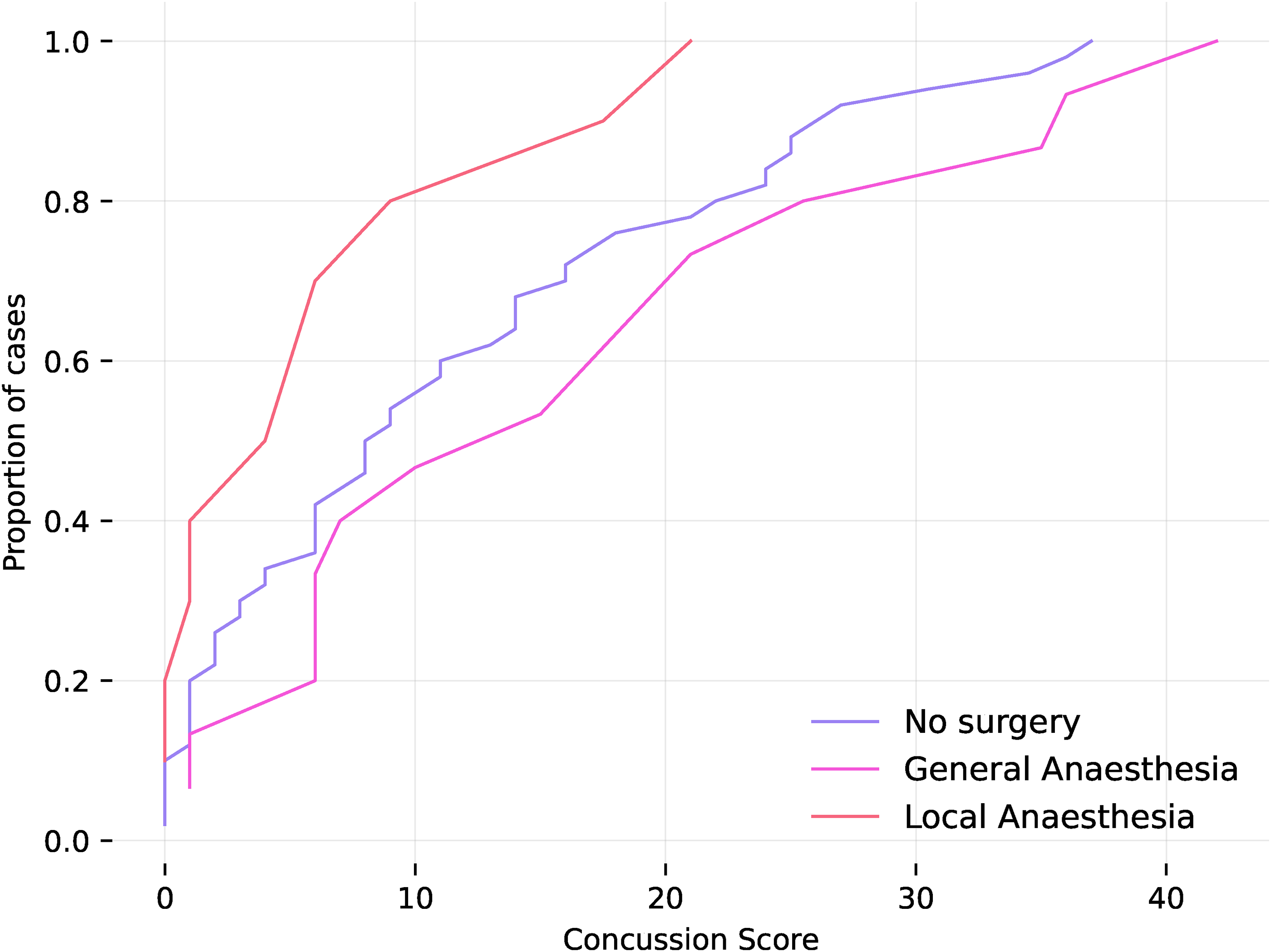
Surgery with general anesthesia has worse mean concussion scores than no surgery or local anesthesia. ECDF (empirical cumulative distribution function) for the concussion scores for no surgery (11.9 mean score, 49/73 cases), local anesthetic (7.2 mean score, 9/73 cases), and general anesthetic (17.6 mean score, 14/73 cases) patients.
Male patients were on average younger than female patients (Figure 5). Male patients are on average younger than female patients. For example, 60% of female patients are older than 60, whereas only 20% of male patients are. There are also more male (44) than female patients (29). Both male and female patients under 30 had higher concussion scores than those over 30 years of age (Figure 6). Male patients also had on average worse symptoms than female patients (Figure 7). Male patients have on average worse symptoms than female patients. For example, only 20% of female patients have a score > 20, whereas 40% of male patients do. The worst concussion score was for the 20-30 years old age range in both males and females (Figure 8). The worst concussion score is for the 20-30 age range in both males and females.
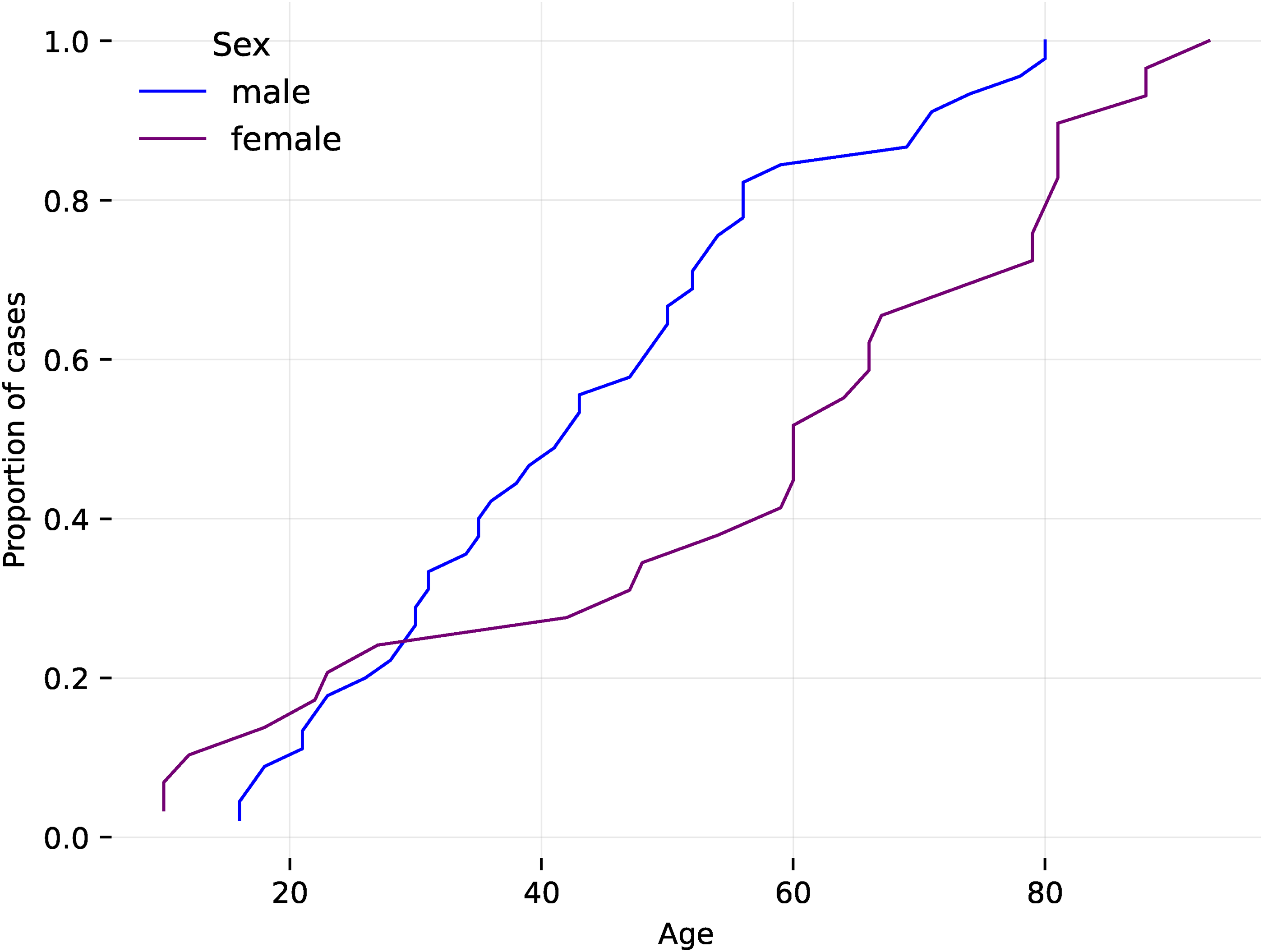
Empirical cumulative distribution function (ECDF) of age of patients by sex.
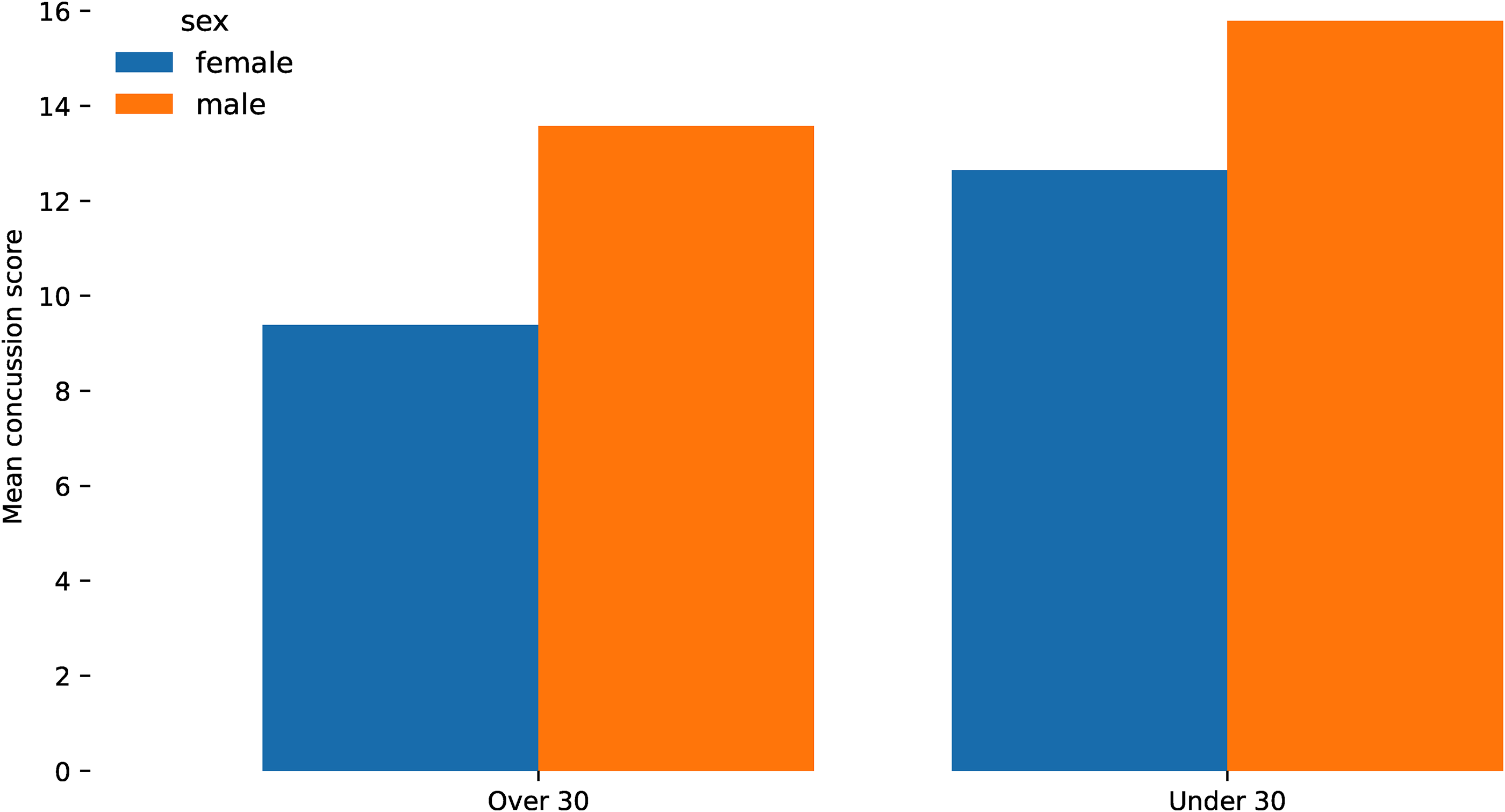
Mean concussion scores for males and females over 30 years of age and under 30 years of age.
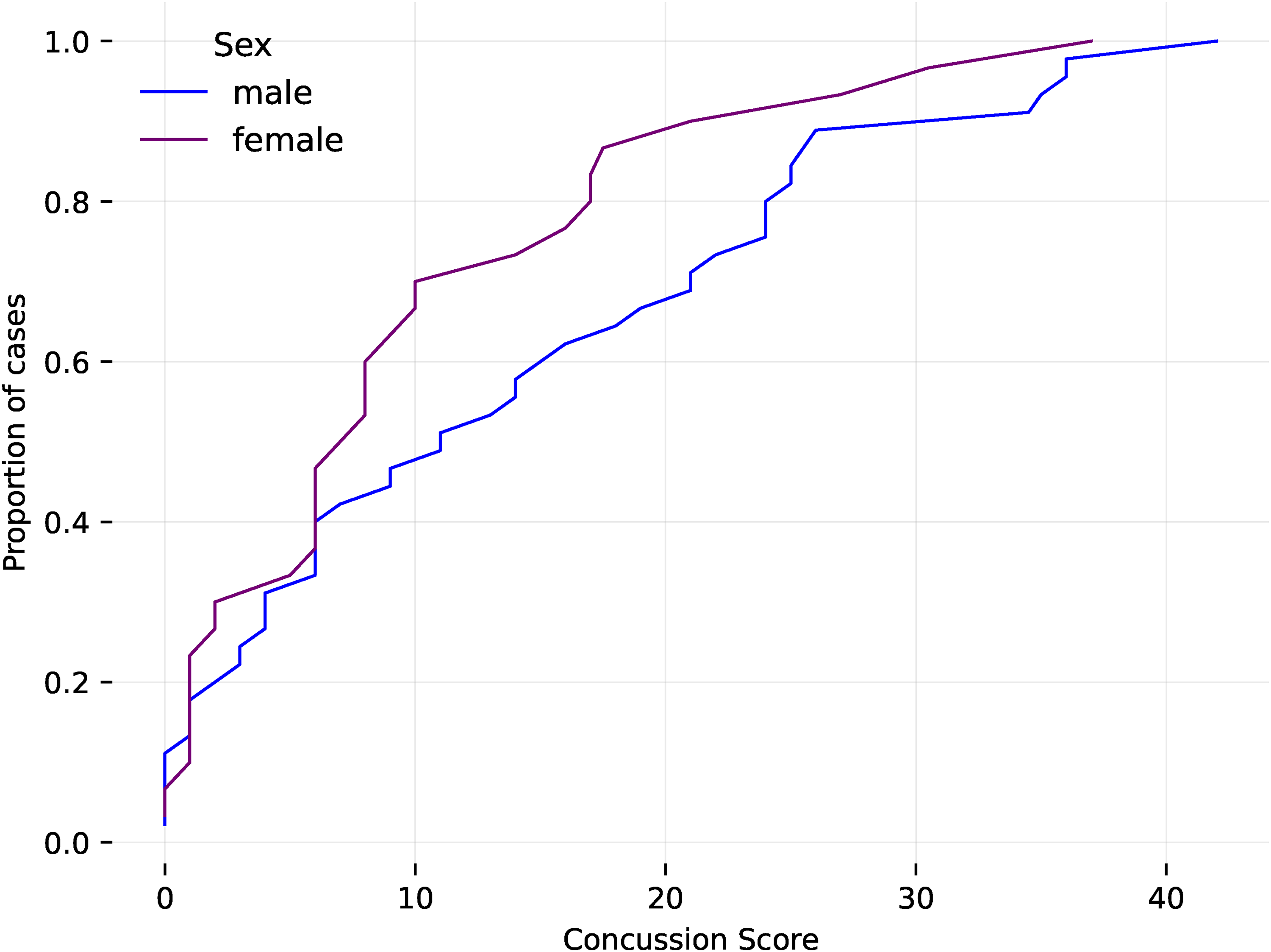
Empirical cumulative distribution function (ECDF) of concussion score of patients by sex.
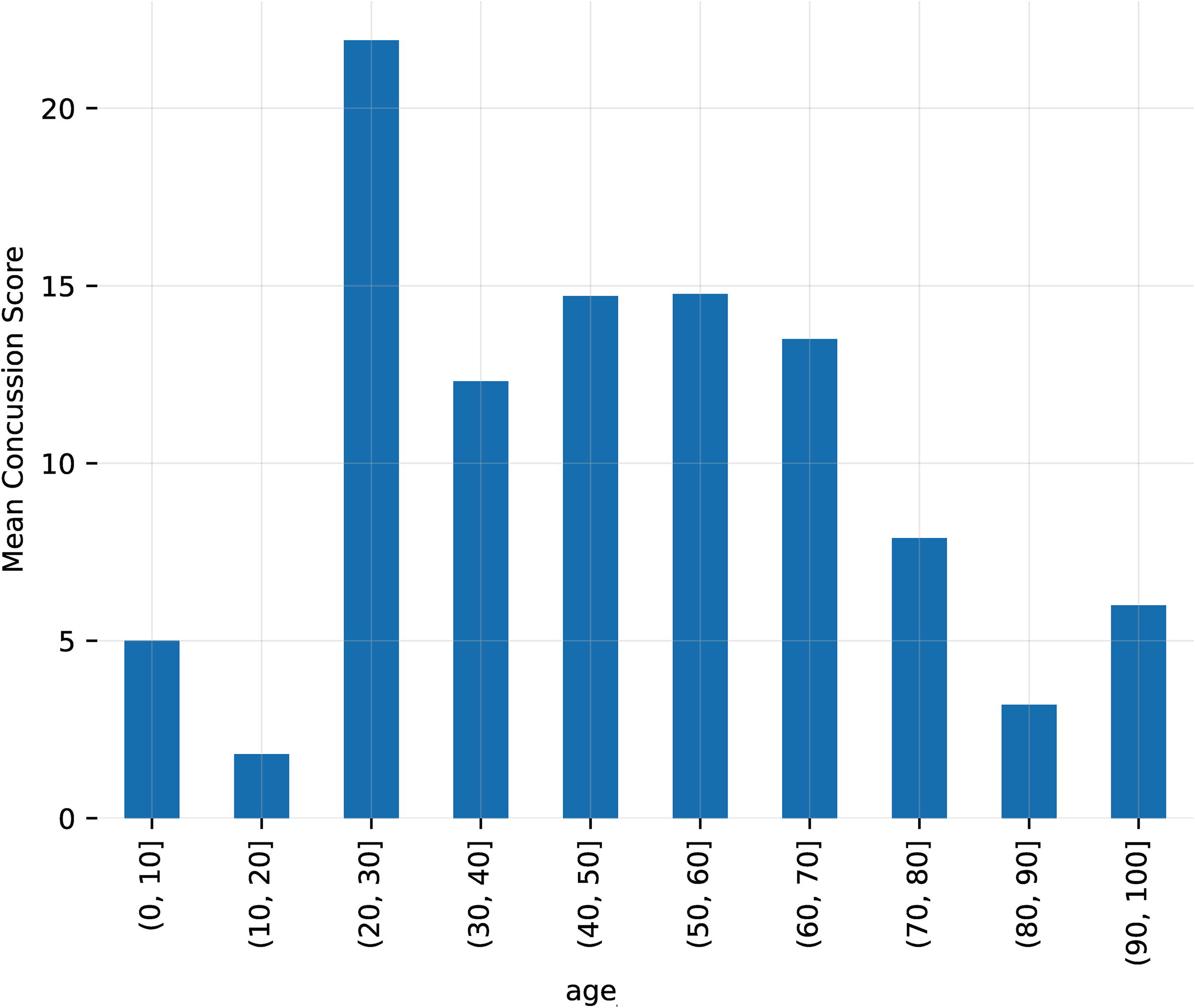
Bar plot of the concussion scores according to patient age.
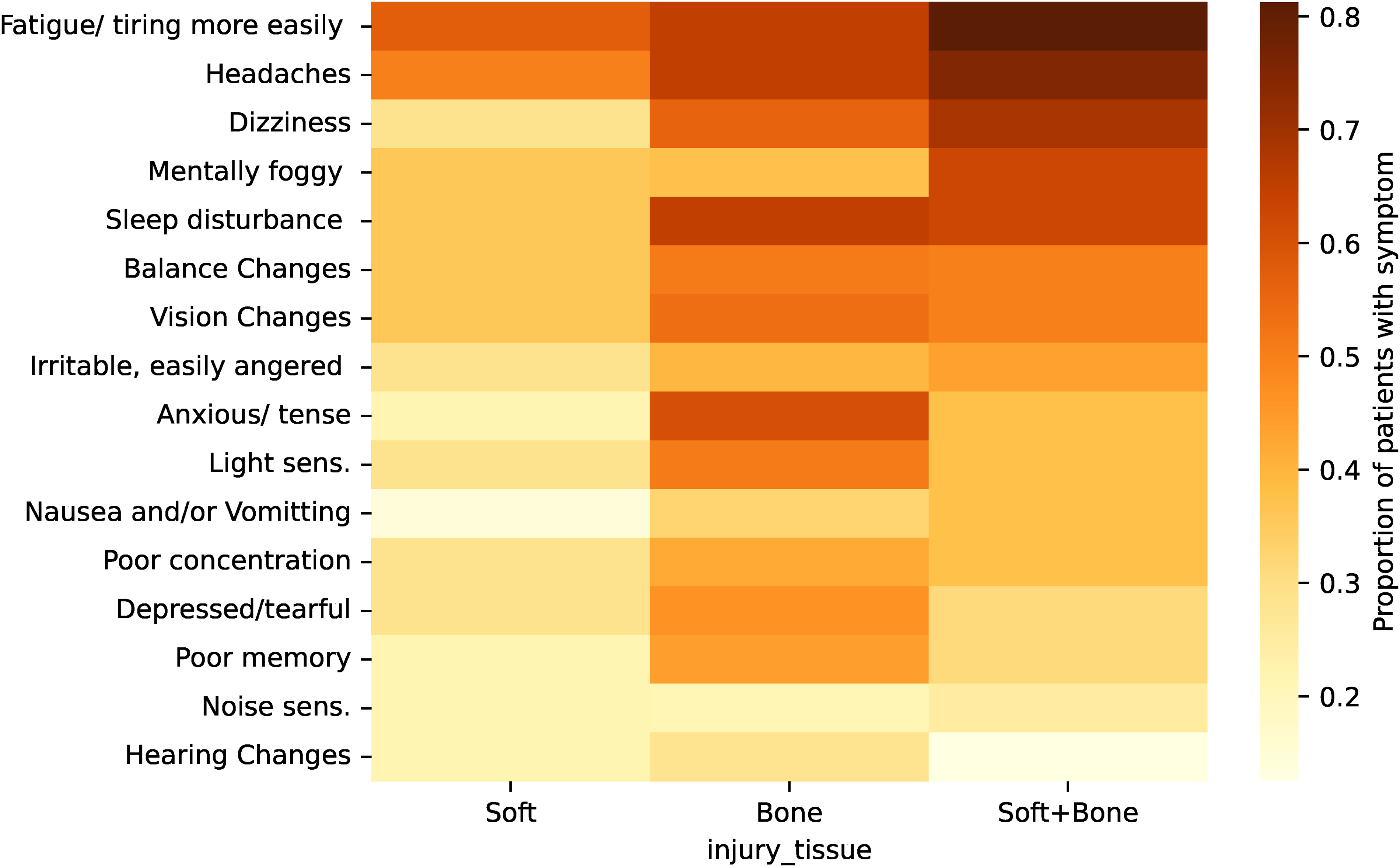
Figure 7 shows the proportion of patients with each symptom given the injury tissue. The most common symptoms were fatigue/tiring more easily and headaches, and these were the two most common symptoms across all the injury types when stratifying according to soft tissue versus bony injury (Figures 9, 10, and 11). Similarly, these two symptoms were the most reported in both males and females when the data was stratified according to gender (Figure 12). Fatigue/tiring more easily and headaches were also the most common symptoms reported in both groups of patients when stratified according to age: less than and greater than 30 years old (Figure 13).
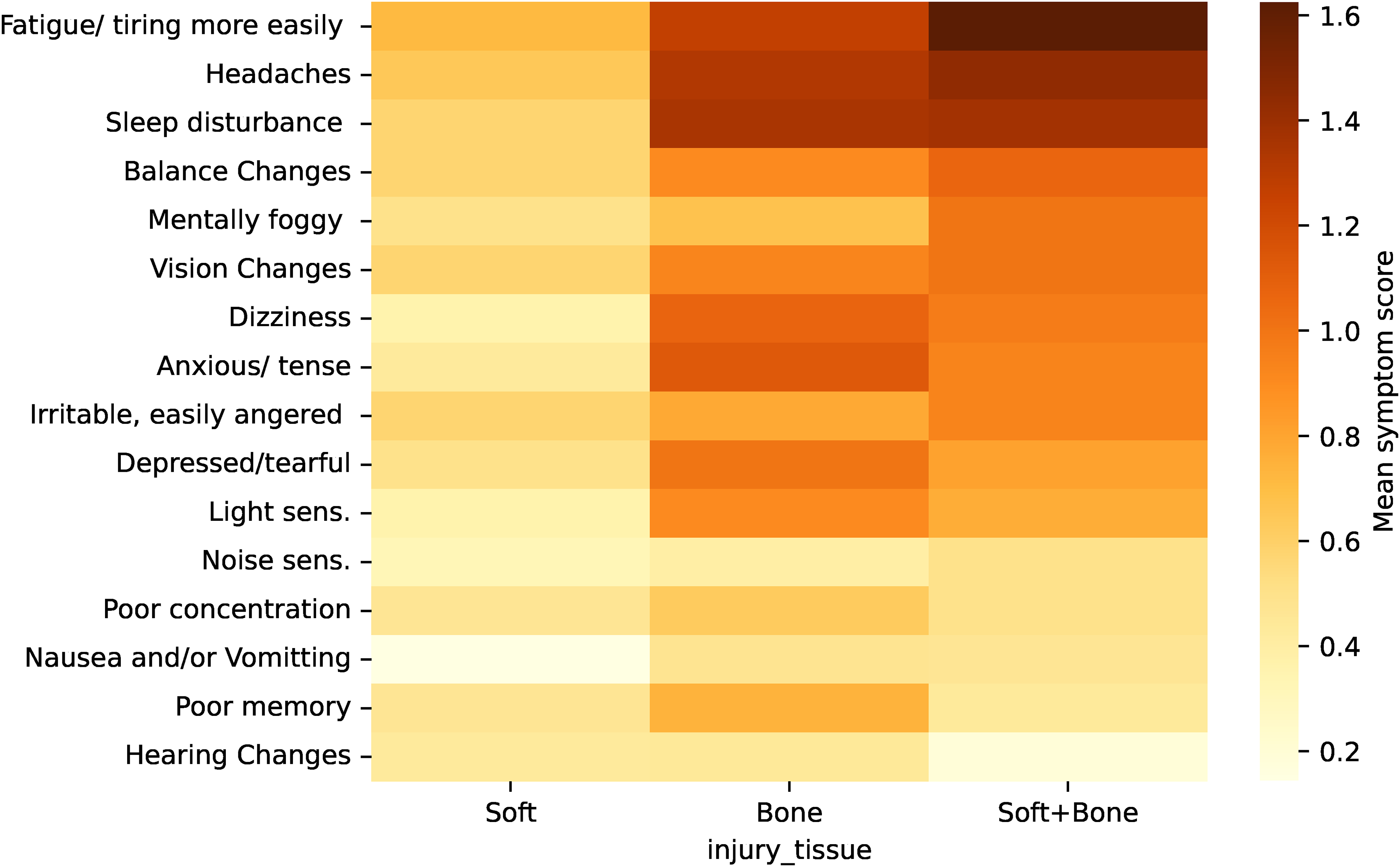
Relative risk of concussion symptoms in soft tissue only versus bone injury versus soft tissue and bone injury.
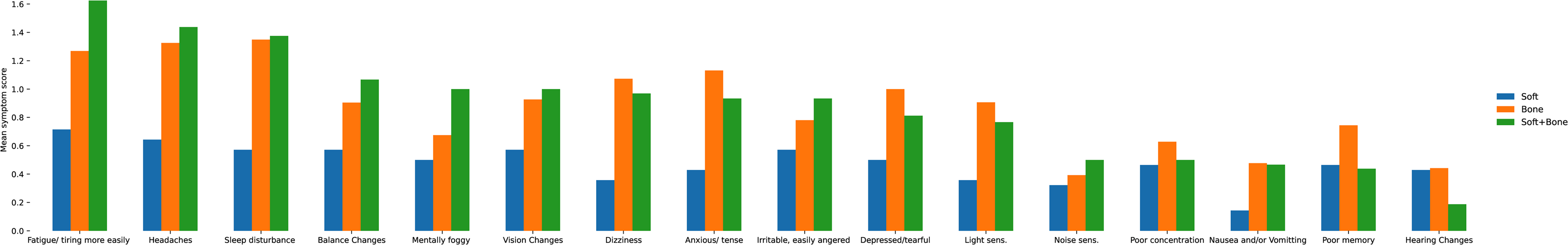
Mean concussion symptom scores in soft tissue versus bone versus soft tissue + bone injury.
Most common symptoms reported subdivided by type of injury: soft tissue, bone, or soft tissue and bone injury.
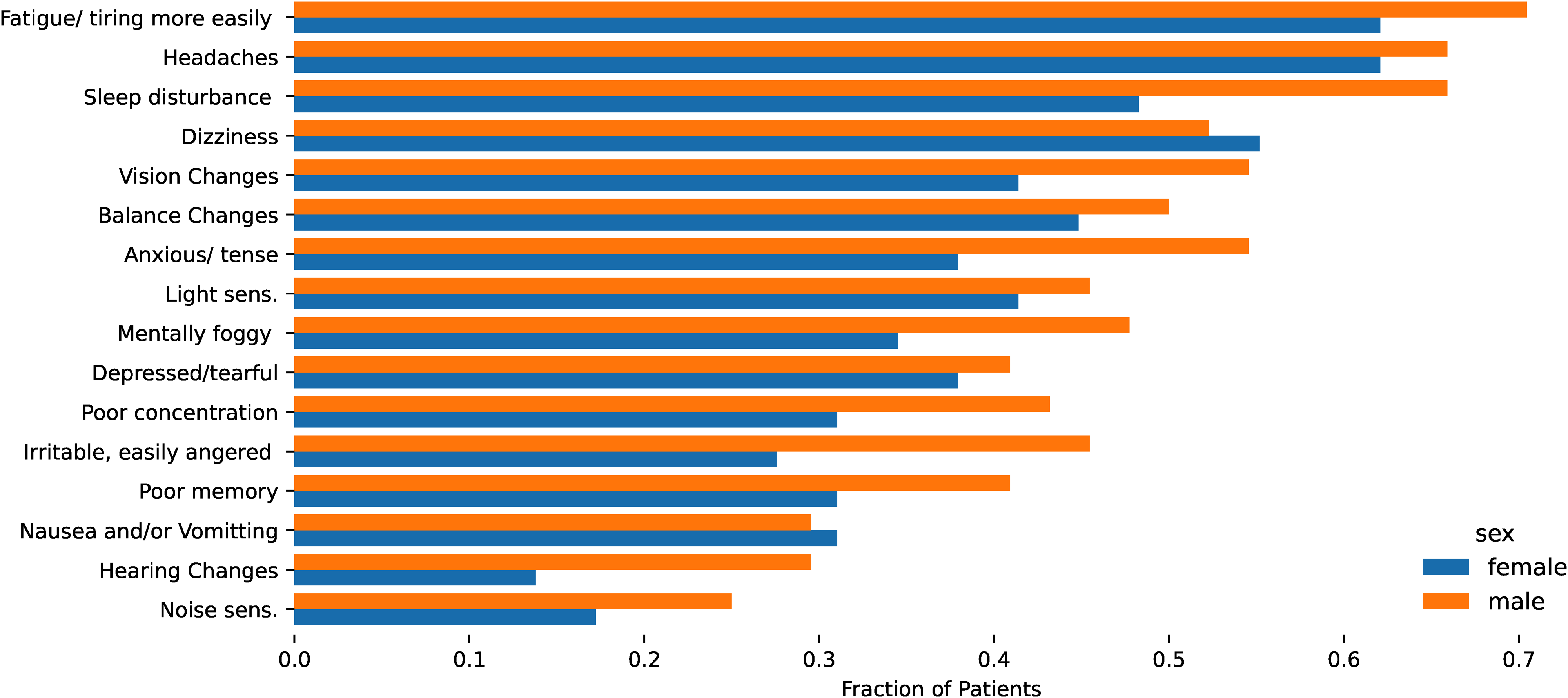
Most common symptoms reported subdivided into male and female.
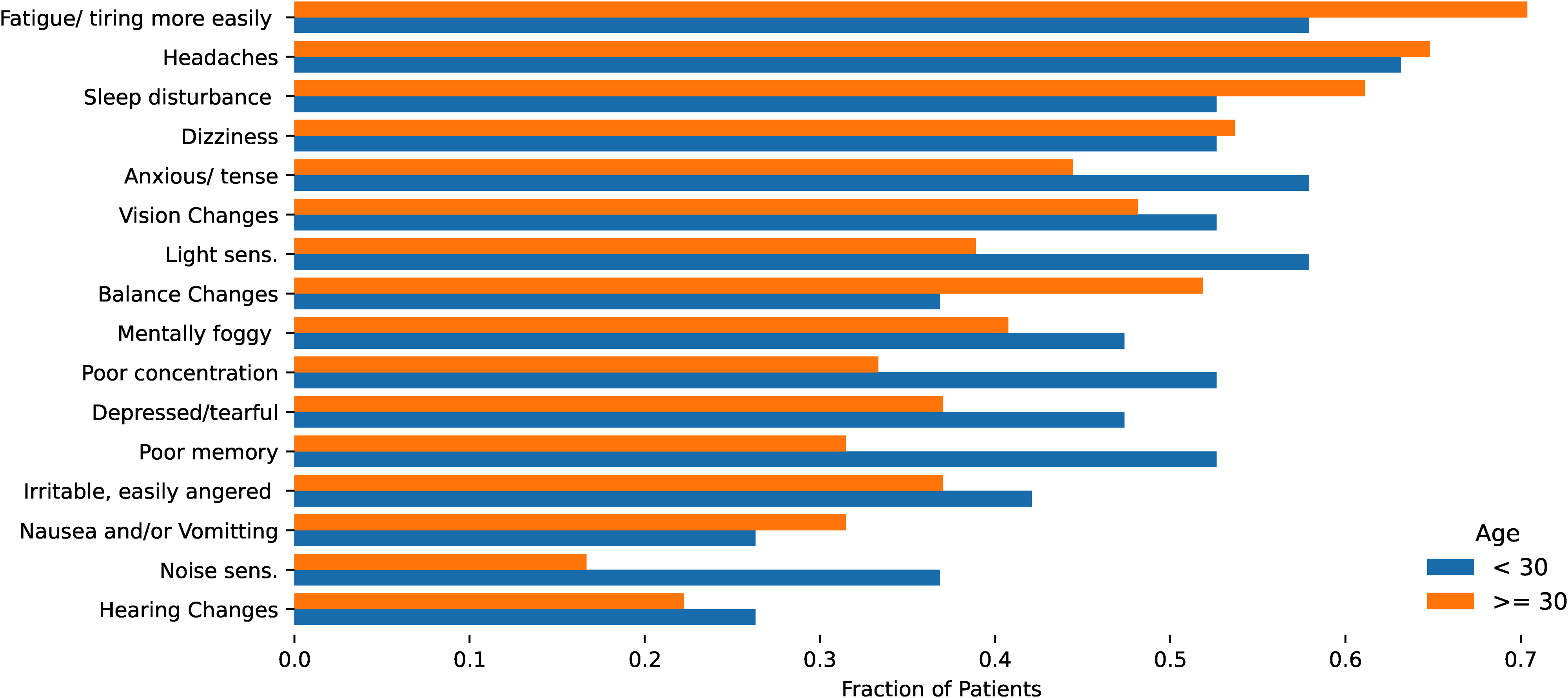
Most common symptoms reported subdivided into less than 30yo and greater than 30yo.
Of any symptom, knowing the “irritable” symptom score was the biggest predictor of concussion score, followed by “anxiousness” (Figure 14). These were the two most predictive factors using the model of a simple two-layer decision tree, common in machine learning. The assumption under this model is that if you could only measure two symptoms, the best two to estimate the total concussion score would be irritability and anxiousness. Interestingly, the more subjective symptoms appear to be more powerful predictors of concussion scores. The more subjective symptoms appear to be more powerful predictors of concussion scores. When determining the most predictive symptoms of concussion score, a simple two-layer decision tree model was used with that premise that only two symptoms could be measured to estimate total concussion score. Thus, the best two symptoms that estimate the total concussion score were found to be irritability and anxiousness.
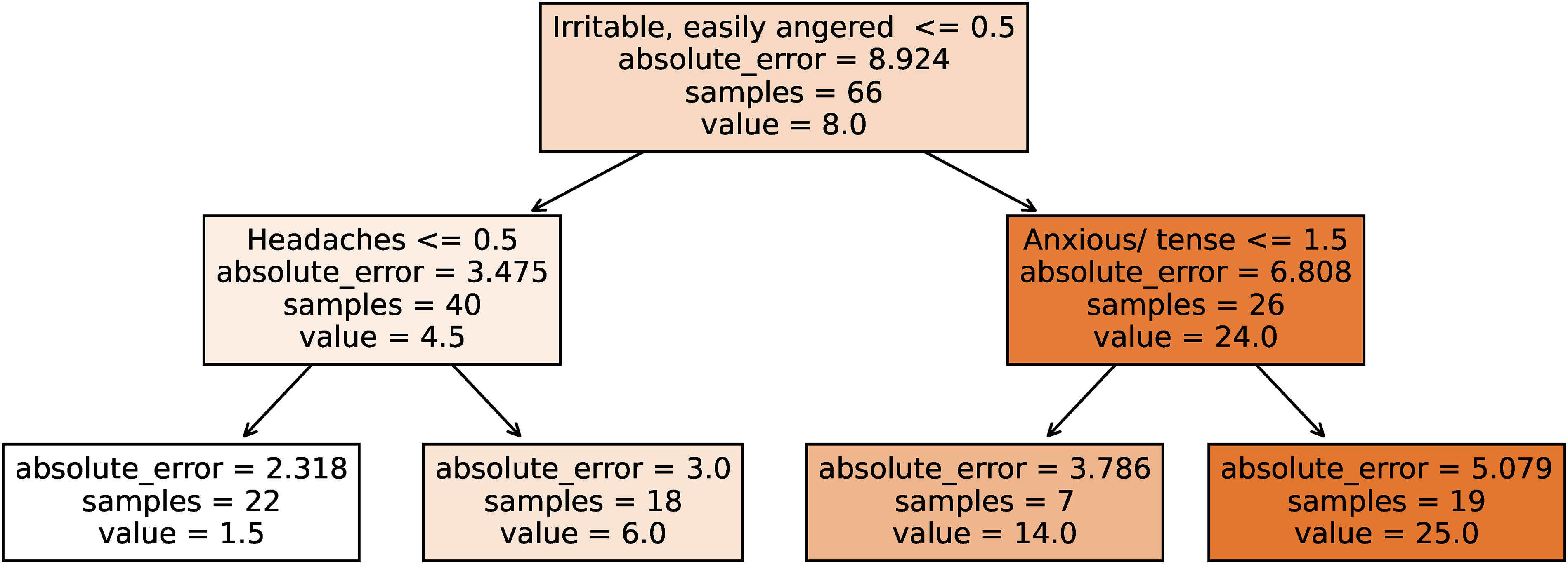
A two-layer decision tree model showing that irritability/anxiousness are the top two predictors for concussion score.
Discussion
Early recognition with subsequent appropriate management of concussion symptoms is important because of the wide-reaching functional consequences of concussions. 3 While studies have shown that concussive symptoms often resolve within 10 days in 80%-90% of patients, the remaining may require a longer recovery period developing post-concussion syndrome (PCS). 5 Zygoma/zygomatic arch fracture was the facial injury type that had the highest mean concussion scores. This finding aligns with literature reports that zygoma fractures have been found to be closely associated to post-traumatic headaches. 6
Interestingly, there appears to be a strong predictive value of GA cases with regards to the severity of the fracture (Figure 3). General anesthesia cases were associated with higher concussion scores compared to local anesthesia cases. This is of significance because all patients in this study were tested before their surgeries, so this speaks to the severity of fracture versus risk, highlighting the strong predictive value of GA for the severity of the fracture type.
Conducting concussion screenings in plastic surgery trauma clinics could result in a higher detection rate for concussions and provide an opportunity for early intervention. While all patients with risks of concussions are ideally identified in the ED at the time of their facial trauma, the plastic surgery trauma clinic offers an additional opportunity to identify concussions that may have been overlooked due to concurrent facial injuries. Thus, screening in this subsequent outpatient setting may serve as a safety net, especially if concussive symptoms are delayed, and would provide further direction for longitudinal care by the patient's family physician.
Interestingly, 95% of patients presenting to the plastic surgery trauma clinic experienced a clinically significant concussion symptom that was not formally diagnosed. Several hypotheses could explain this lack of management for concussions in facial trauma cases. Firstly, facial injuries may distract from assessing or discussing concussions, with the focus shifting towards managing the facial injury. Secondly, there may be the assumption that the plastic surgery team will manage the concussion once the patient is seen in the facial trauma clinic. The current guidelines for head injuries as per the Canadian CT head rules, 7 as well as the those from the National Institute for Health and Care Excellence 8 focus on recognizing neurological red flags for imaging. However, they both lack detailed guidance on self-care, occupational advice, and accessing further help if concussion symptoms persist. Identifying patients experiencing concussion symptoms in the plastic surgery trauma clinic would offer an opportunity to provide more comprehensive advice, including resources such as the Parachute Guidelines for Concussions in Sport. 9
Currently, there is no national guidance for the follow-up of patients with concussion, and there is a wide spectrum of symptoms leading to considerable variation in management. Follow-up for patients is logistically challenging due to the high number of concussion cases. Furthermore, as evidenced in this study with almost all patients presenting with unmanaged concussion symptoms, is the lack of clear ownership for ongoing care. This second touchpoint offers an additional chance to identify concussions that are resulting in a functional impairment and help direct further management by the primary care physician.
Diagnosing concussions is challenging due to the absence of an objective diagnostic test. Previous studies have shown that only a small percentage of patients with facial injuries resulting in concussive symptoms in the ED receive a formal diagnosis. 3 In the absence of biomarkers for concussions, implementing structured symptom screening tools for all at-risk patients in both the ED and facial trauma clinic settings could be beneficial.
While this study is the first of its kind in Canada, it has limitations, including its retrospective nature and lack of statistical power. The study's retrospective nature limits causative conclusions and may introduce bias in data interpretation. A larger sample size may be needed to detect significant differences in assessed facial injury types. With 74 patients, the statistical power does not cater to drawing definitive conclusions about trends across all facial trauma types; however, it provides insight for future prospective studies. Differences in concussion symptoms were analyzed using descriptive statistics. Additional analysis with a greater sample size would allow for inferential statistics to predict concussion scores in a population and would help build an infrastructure to triage injuries by concussion severity. With a larger sample size, future efforts could be directed towards comparing symptom severity based on fracture complexity (simple vs comminuted). 10 A larger sample size would also allow for investigation of the link between surgical management outcomes and the relationship with concussive symptoms.
As well, the days between the office visit and the injury were not standardized between the patients which may contribute to a variance in the degree of symptom severity. Variability in between injury and clinic visit is a potential limiting factor for concussion score interpretability. Assuming severity is manifested in both duration and intensity of symptoms, while an earlier clinic visit may show higher concussion scores than a later clinic visit, the injury severity would also manifest in a greater number of symptoms that persist for a longer timeline, which would still be captured in the dataset.
Additionally, the absence of ED notes limits insights into the initial diagnosis and management of concussions. Thus, it is unclear whether patients may have received any head injury advice from their referring hospitals.
The trauma clinic does not follow mandible fractures and the relationship between these injuries and concussion would need to be evaluated. Recognizing that mandible fractures are a subset of facial fractures that are excluded from this study as they are not seen in this clinic, their inclusion in future studies may have demonstrate a greater power score for the difference between soft tissue versus bony injury.
Demographic information apart from age and sex was not collected for the sample. Socioeconomic or cultural factors could influence the likelihood of reporting concussion symptoms. Current literature has studied this on a large scale in student athletes and have found knowledge and attitude influence concussion reporting. 10
Implementation of a structured concussion screen protocol would be a multi-layered approach to ensure ease of uptake with a reliable yet simple triaging tool. Given that irritability and anxiousness were strong predictors of concussion scores, targeted interventions would allow for apt identification and immediate streamlined resource referral to appropriate psychological for symptom management. 11
Future studies may involve conducting a prospective study to strengthen the evidence and minimize bias, which would allow standardization of the time from injury to evaluation to ensure consistent data collection. Collaborating with other trauma clinics would not only increase sample size and statistical power but would also broaden the scope to include mandible fractures, which would offer a more comprehensive analysis of facial injuries and concussions. Furthermore, an extension of the study to collaborate with EDs to track initial assessments and interventions for head injuries in facial trauma patients would provide more detailed baseline patient information. Lastly, collaboration with allied health services such as psychologists and occupational therapists would allow for assessment of long-term functional impairments and quality of life measures to enhance the relevance of our findings.
Conclusion
In summary, concussion symptoms post-facial injuries are common and can lead to long-term functional impairment. Facial trauma is related to clinically significant concussion symptoms that affect quality of life. The severity of concussion scores increased significantly with fractures, particularly with zygoma/zygomatic arch fractures in facial trauma patients. Early detection and management of concussions are critical for better outcomes; yet as seen in this study, many patients in an acute facial trauma clinic had symptoms suggestive of concussion which did not warrant any formal specialist management for head injury. The results from this study support a structured screening program for all patients attending facial trauma clinics to be screened for concussions. Future efforts should focus on developing simple objective screening tools for use in clinics to guide patients to appropriate concussion management and resources.
Footnotes
Contribution of Authors
PO was responsible for the study design and data collection. Both RX and PO contributed to the writing, editing, data analysis and submission of this study.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethics
This retrospective chart review did not require ethics approval. Fraser Health Authority allows for practice review/patient quality of care improvement to be exempt from ethics review. In this circumstance, the addition of the questionnaire was done for all patients as a quality improvement initiative and not originally done as a research initiative. The questionnaire has been continued for all patients since the original group was reviewed.
Informed Patient Consent Statement
Patient consent was obtained.
