Abstract
Introduction
In 2020, the COVID-19 pandemic forced medical educators and trainees to find alternative methods of granting exposure to surgical residency programs in Canada. 1 With limited electives and shadowing opportunities, programs began organizing virtual information sessions, social events, and the Canadian Resident Matching Service (CaRMS) interviewing process shifted from traditional in-person interviews to an online format. 2 This shift brought about new challenges for both medical students and program directors alike.
Since medical trainees represent the future of medicine and surgery, it remains critical to evaluate and improve upon the recruitment methods used. Since the CaRMS process was newly made virtual as of the 2021 application cycle, there exist a paucity of data with regard to optimal factors affecting virtual engagement and Canadian surgical applicant selection. Although some of these factors have been studied in the United States, to the authors’ knowledge, this has not yet been studied in Canada. 3
In the present study, the authors aim to analyze the perspectives of both applicants and program directors who had participated in the first iteration of the virtual CaRMS surgical residency selection process, with the overarching goal of providing guidelines and recommendations for its sustainable adoption in future years.
Methods
This study was designed as a cross-sectional survey study sent to trainees and program directors (PDs) who participated in the 2021 CaRMS surgical program application cycle. All surgical subspecialties were included. PD contact information was available publicly through the Royal College of Physicians and Surgeons of Canada website, and recent medical school graduates were reached through their program directors, postgraduate medical education administrators, or medical school council representatives. Institutional Review Board ethics approval was obtained (review number A07-E38-21B 21-07-078) prior to study commencement. Participation was voluntary and anonymous; all participants signed an informed consent form at the questionnaire offset. Questionnaire details are provided in Supplemental materials (Supplemental Digital Content 1-3).
Results
Program Director Feedback
Demographics
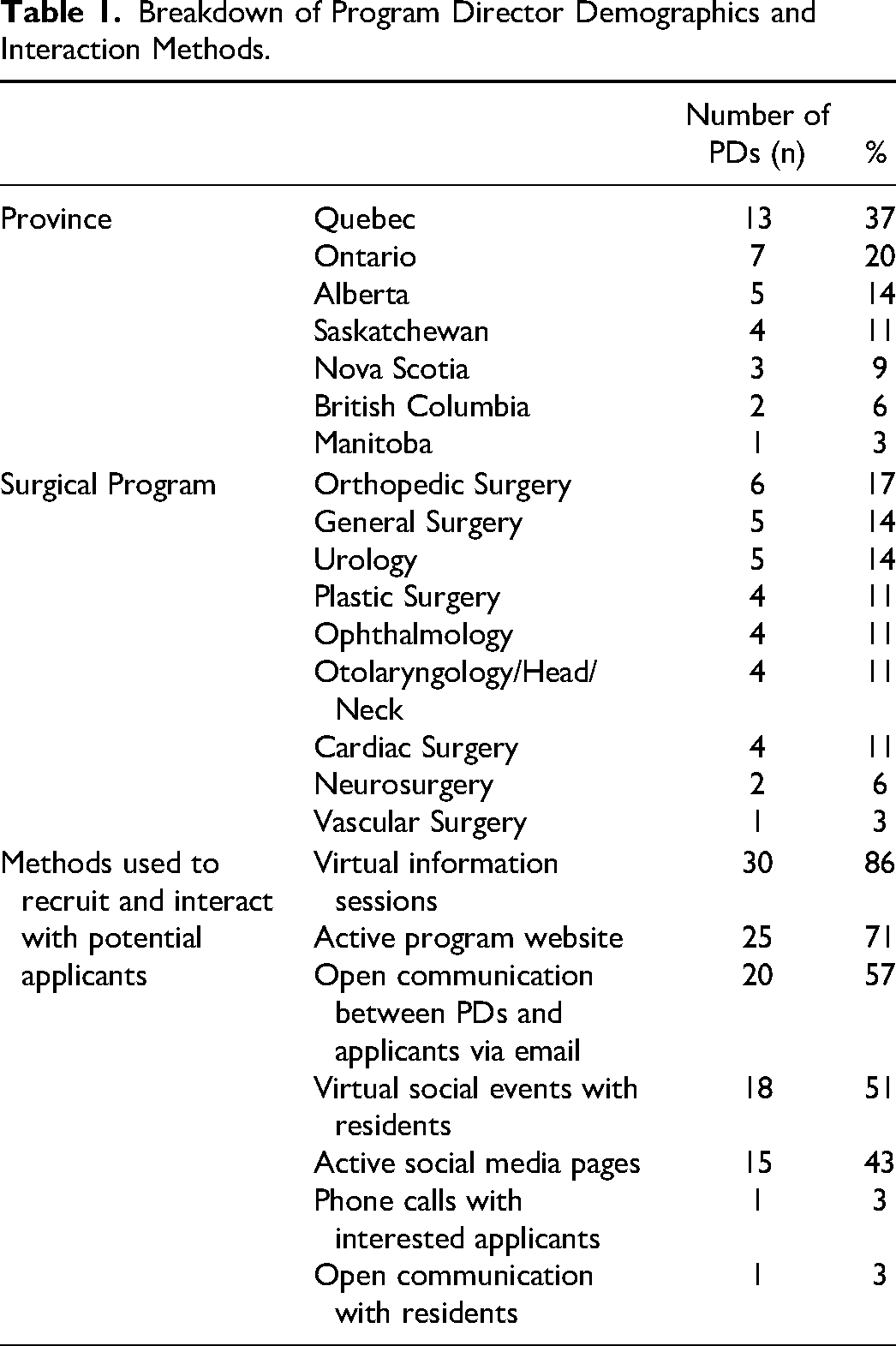
Thirty-five out of 128 Canadian surgical program directors (27%) responded to the survey, the majority of which from Quebec (n = 13, 37%) and Ontario (n = 7, 20%). The majority of PDs were from orthopedic surgery programs (n = 6, 17%), followed by general surgery (n = 5, 14%), urology (n = 5, 14%), plastic surgery (n = 4, 11%), ophthalmology (n = 4, 11%), otolaryngology (n = 4, 11%), cardiac surgery (n = 4, 11%), neurosurgery (n = 2, 6%), and vascular surgery (n = 1, 3%); complete demographic data is presented in Table 1. A percentage comparison of program directors who responded to the survey, relative to the total number of surgical program directors per province, is presented as Supplemental Digital Content 4.
Breakdown of Program Director Demographics and Interaction Methods.
Perceived advantages
Cost reduction was the most commonly reported benefit of online interviewing perceived by PDs (n = 30, 85%), followed by efficiency (n = 25, 71%), enhanced resource management and planning (n = 15, 49%), as well as ability to conduct a greater number of interviews than usual (n = 8, 23%). Three PDs added that virtual interviews allowed the inclusion of faculty that may have otherwise been out of the country or physically unavailable, while one other PD (3%) reported on the benefit for applicants as it pertains to less travel.
Perceived disadvantages
The most commonly reported disadvantages of the virtual interview process included the inability to show applicants the program and facilities, as well as the inability to socialize with applicants to gauge their interpersonal traits (n = 24 each, 69%). Six PDs (17%) reported that they found themselves interviewing more applicants than truly necessary, while 2 other PDs reported on the difficulty of virtual event planning, and difficult applicant–interviewer interactions in the virtual setting (3% each). Overall, 54.3% of PDs (n = 19) felt that the benefits of online interviewing outweighed its disadvantages.
Program director outlook
Overall, 31% of PDs felt that they were very capable of representing their programs using virtual methods. When queried about their confidence in the fit of incoming residents to their programs, 49% responded that they were “very” confident, and 41% responded that they were “somewhat” confident. When queried about whether they would prefer virtual or in-person interviews for future cohorts, results were equivocal; 18 PDs (51%) preferred a virtual format and 17 (49%) preferred in-person. Seven PDs further elaborated that regardless of the interview format, nothing could replace the value of an in-person elective as a major factor in gauging applicant suitability, and ultimately, resident selection (n = 7, 20%). It remained unclear whether the lack of clinical electives specifically, or the overall virtual process, had the most impact on PD-perceived satisfaction presented herein.
When queried about factors that made applicants from outside schools appealing given the absence of visiting electives, the majority of PDs reported that “strong letters” (n = 28, 80%) and “strong interviews” (n = 26, 74%) were the most significant factors. Extracurriculars outside of medicine (n = 15, 43%), leadership positions (n = 14, 40%), and research experience (n = 12, 34%) were also highly valued. The majority of PDs (n = 24, 69%) reported that attendance to virtual information sessions did not increase the likelihood of an applicant being invited to an interview. Two PDs (6%) further emphasized the importance of interacting well with the interview panel and treating the virtual interview as though it was in-person. Four PDs (11%) suggested that applicants reach out to their programs (through residents, coordinators, or directly to PDs themselves) in order to demonstrate interest and learn about their programs prior to interviews. With regard to external factors such as lighting, clothing choice, and background during the virtual information sessions, socials, or interviews themselves, the majority of PDs reported that they did not play a significant role in applicant selection. Specifically, 19 PDs (54%) reported that these factors played no role at all, while 11 PDs (31%) reported them playing a minor role.
Applicant Feedback
Demographics
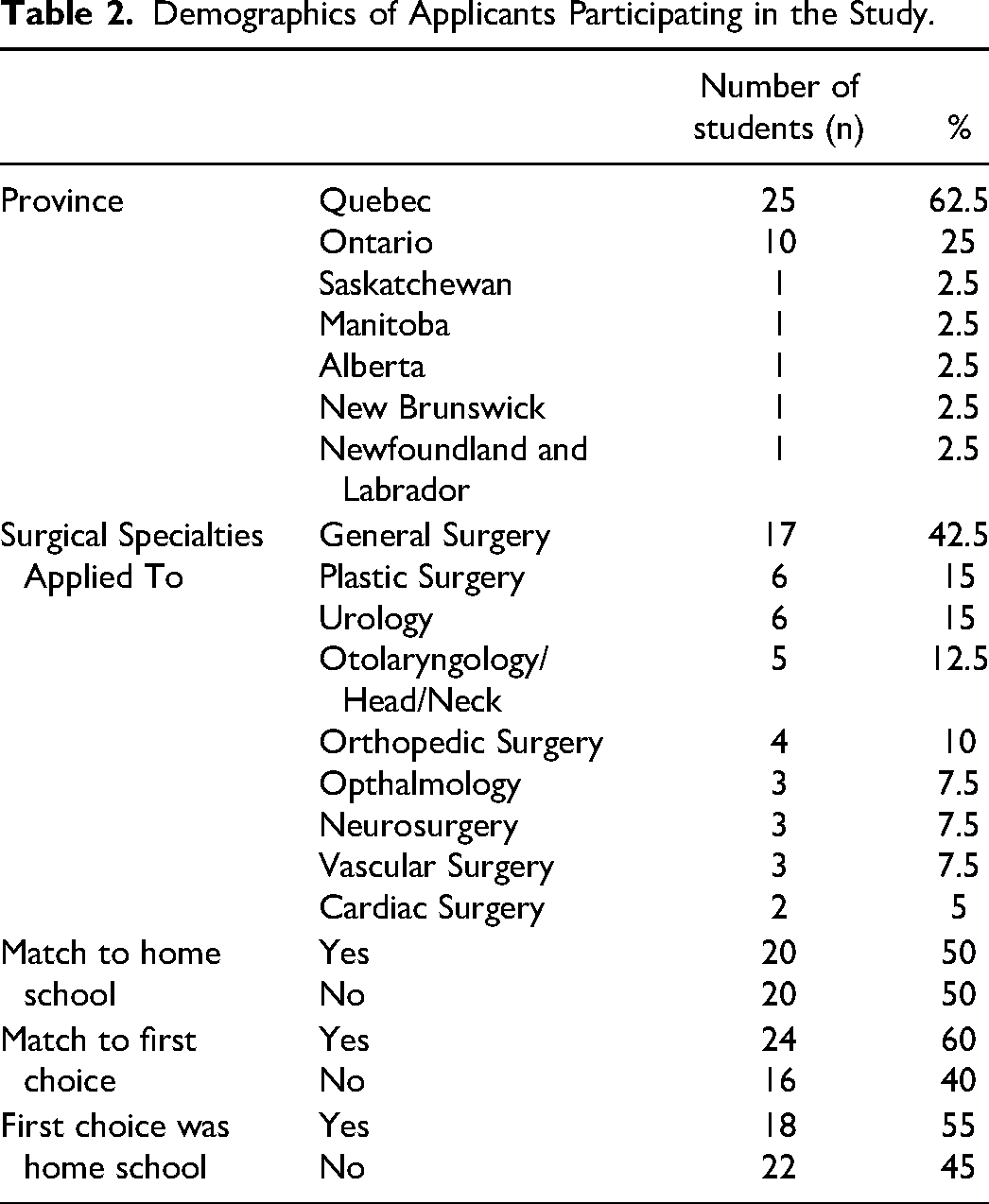
Forty medical trainees out of 284 (14%) who applied in the 2020 to 2021 CaRMS process and successfully matched into a Canadian surgical residency program responded to the survey: 25 were from Quebec (62.5%), 10 from Ontario (25%), and 1 from Manitoba, Saskatchewan, Alberta, New Brunswick, and Newfoundland and Labrador (2.5% each). The most common specialty applied to was general surgery (n = 17, 43% of all programs applied to by respondents), followed by plastic surgery (n = 6, 15%) and urology (n = 6, 15%). Eighteen respondents (45%) ranked their home school first, and 24 (60% of all participants) matched to their first choice. A detailed breakdown of demographic data is presented in Table 2.
Demographics of Applicants Participating in the Study.
Among applicants whose first choices were their home schools (n = 18, 45%), the most commonly reported reasons included geographic preference (n = 14, 74%) and personal life-related matters (family, partner, etc; n = 14, 74%). Elective experience subsequently followed, (n = 13, 68%), as well as “preference to stay in same location” and “institutional reputation” (n = 11, 58% each). For those whose first choices were not their home schools (n = 22, 55%), geographic reasons remained the most common reason for their submitted rankings (n = 14, 64%). This was followed by available clinical opportunities (n = 10, 46%) and perceived work environment (n = 8, 36%). A breakdown of all reported reasons for first-choice ranking by applicants is presented in Supplemental Digital Content 5.
Overall applicant confidence in the virtual selection process
Applicants reported an average score of 6.9/10 regarding their perceived confidence in the virtual selection process, with an average score of 7.7/10 regarding their perceived suitability to their first choice-ranked program. A significant association was demonstrated between confidence in suitability with first-choice programs, as well as knowledge of matched programs, with applicants who ranked their home programs first (
Virtual information sessions
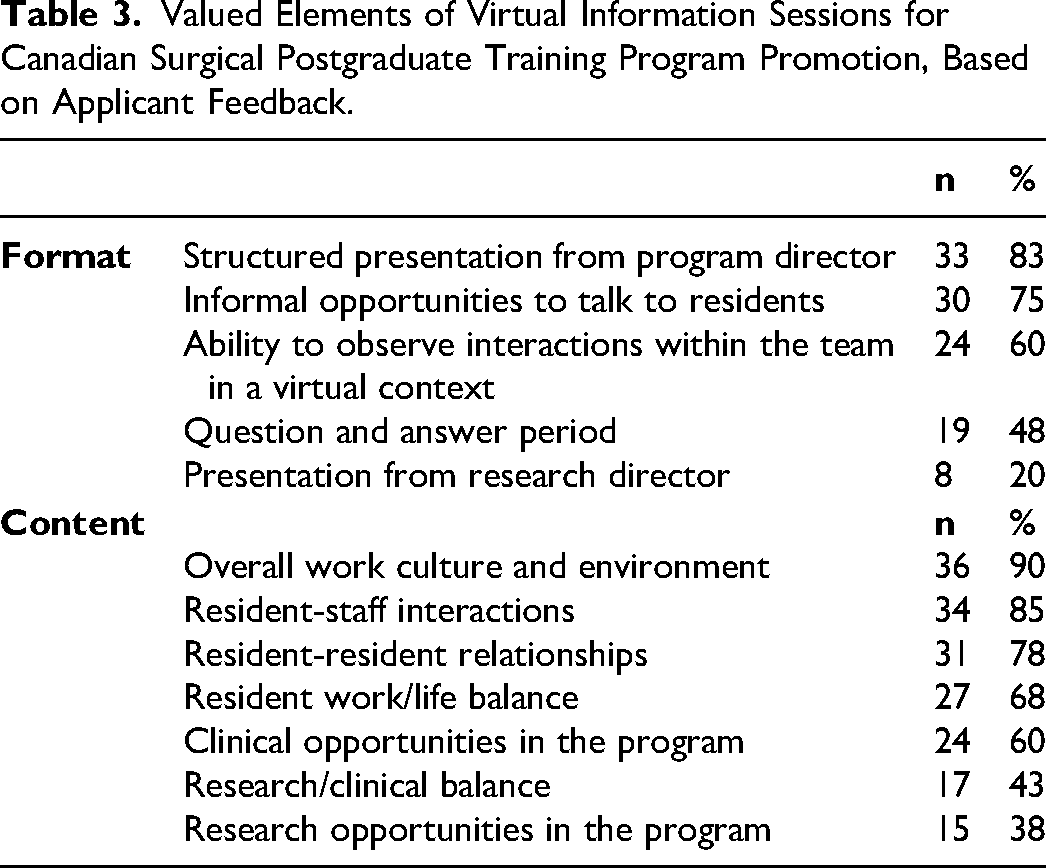
All applicants (n = 40, 100%) reported having attended virtual information sessions or virtual events hosted by programs they were interested in. Applicants reported an average score of 7.0/10 regarding the ability of virtual information sessions to increase their interest in programs they may have otherwise not been interested in. Structured presentations from program directors (n = 33, 85%) and informal opportunities to speak with residents (n = 30, 77%) were aspects of the virtual information sessions most appreciated by applicants. When asked about what they would have liked to hear more about during these sessions, 90% of applicants (n = 36) reported an interest in learning more about the work culture and environment, while 34 (85%) were interested in learning about social relationships between residents and staff (Table 3).
Valued Elements of Virtual Information Sessions for Canadian Surgical Postgraduate Training Program Promotion, Based on Applicant Feedback.
Preinterview socials
When asked about whether preinterview socials helped applicants get to know programs better, n = 34 (86%) responded either “a little bit” or “somewhat.” With regard to suggestions for content and format for these events, applicants overwhelmingly suggested that resident/resident and resident/staff relationships be discussed (n = 38, 95%), followed by discussions about work culture and environment (n = 36, 95%), as seen with virtual information sessions (Supplemental Digital Content 6). With regard to format, casual interactions with residents and staff (n = 33, 83%) were preferred, in addition to icebreaker games and “get-to-know you” activities (n = 23, 58%). Applicants mainly suggested socials be held the day before interviews (n = 29, 76%).
Virtual interview
With regard to the virtual interview, 26 respondents (65%) said they appreciated closer interactions with program directors and staff members, and n = 25 (62.5%) reported appreciating a preamble and/or presentation by PDs. With regard to confidence in their ability to properly present their strengths and candidature in the online interview, applicants gave an average answer of 7.45/10, whereas a score of 7.3/10 was given for confidence in ranking programs following virtual interviews. Applicants were asked about aspects of their experiences with the virtual residency selection process that they believe may have contributed to their successful match and were queried for recommendations for future applicants. A summary of key points is synthesized and presented in Figure 1.
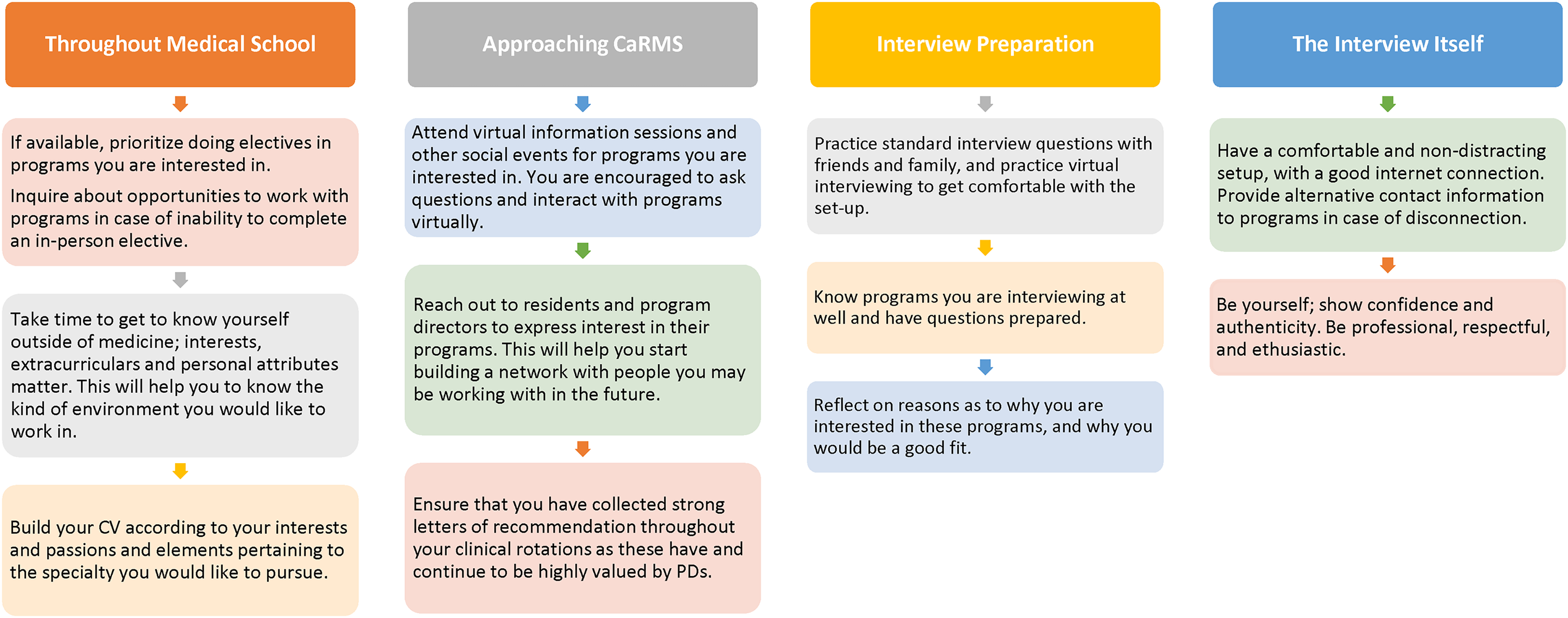
Longitudinal recommendations for medical students applying to Canadian surgical subspecialty programs based on collected feedback from applicants and program directors.
Discussion
The Canadian Resident Matching Service (CaRMS) process has been consistently described as a great source of stress for medical students applying for surgical subspecialties, especially given the growing limitations on available positions. 4 From its initiation in 1969, until just before the COVID-19 pandemic, Canadian medical graduates applying to a residency program have been traditionally required to perform in-person electives at programs in which they were interested, and to travel across the country for interviews. Despite its institution over these years, this process had become veiled with challenges for both applicants and program directors alike. Previous initiatives have been ascribed on behalf of residency programs to reduce interview burden on Canadian applicants; for example, in 2003, Grober et al described a unified urology fair for information about individual programs and interviews on the same day in the same Canadian city. 5 The economic impact on applicants, time required for travel, and environmental implication of thousands of applicants traveling for interviews represented just a few reasons that the CaRMS process could have transformed into a virtual format earlier on. However, with the advent of the COVID-19 pandemic, the 2021 CaRMS selection process was forced to become virtual, and a paradigm shift for resident selection in Canada began. 6
The present study provides both applicants and program directors participating in future iterations of the virtual residency selection process with the perspectives of successful applicants and PDs from the 2021 match, as well as feedback and advice for the improvement of the experience for both applicants and PDs. In addition to the fundamental benefits of curbing COVID-19 spread, the present study demonstrates that there exist several advantages to a virtual format in surgical resident selection. Reduction in stress for applicants and the convenience of being able to interview from the comfort of their homes represent notable advantages. This also serves to increase applicant access to their wellness resources, whether spending quality time with family/friends during the interview period, having access to their traditional facilities for physical activity, or university wellness advisors. With the associated reduction in time required for travel, applicants also reported on the ability to attend more interviews which otherwise may have conflicted by overlapping across different cities. Additionally, the estimated environmental impact of travel during the traditional CaRMS process is nonnegligible, with the virtual switch representing a 100% reduction in greenhouse gas emissions related to this process. 7 At a time when climate change remains of increasing concern, this itself calls into question whether the travel component for interviews was, at all previously truly warranted.
Among the 40 successful applicants surveyed, a mean response of 7.6/10 and a mode of 9/10 were reported regarding applicant confidence in the knowledge of their matched programs. Although control data from previous years during the traditional match process is not available for the purpose of comparison, these findings demonstrate that overall, despite the virtual format, applicants were still beginning their postgraduate training with significant confidence and knowledge of their programs. Applicant confidence in this context was demonstrated to be statistically correlated with instances of matches to home schools, which may further reinforce the importance of elective opportunities and in-person program exposure, regardless of the interview format, as highlighted by feedback from program directors surveyed in this study. These findings are in line with additional studies from the United States, including on nonsurgical training programs. When asked about preferences regarding future recruitment strategies to pediatric neurology programs, American program directors reported a preference for combined experiences that include in-person social activities or program visits, with continuing online interviews. 8 Another study on American surgical oncology programs found that most PDs (83%) and candidates (79%) were comfortable making their rank lists following virtual interviews, in line with the remarkably high PD and applicant confidence in ranking and match outcomes following virtual interviews in the present study. 9 In contrast, a similar study surveying American plastic surgery program directors found that most PDs (76.3%) would not prefer to have virtual interviews in future years, whereas in the present study, findings were rather split regarding PD and student preference. 10 Ultimately, this accentuates the importance of ongoing discussion regarding the future of residency interviewing and selection in order to leverage the benefits of virtual interviewing and selection, all while minimizing its limitations.
Despite its notable advantages, the virtual residency selection process is not without its limitations. Technological difficulties arising from poor internet connection, accidental disconnection, breakout room confusion, and overall virtual applicant and interviewer coordination were stated as marked disadvantages. Indeed, computer proficiency, literacy, and technological difficulties were cited as notable challenges in recent studies, along with a compromised element of social interaction and loss of opportunity for applicants to observe program environments.11,12 Although these limitations may be unique to the virtual applicant process of 2021; reinstitution of in-person visiting electives as part of the virtual residency selection process may circumvent most of these challenges. Although this study did not query the specific impact of the lack of visiting electives on satisfaction with match outcomes among PDs and applicants, the significance of clinical electives for applicant selection was noted by several PDs. Many PDs felt that regardless of selection process format, virtual or in-person, nothing could replace the value of in-person electives; and while 90% felt either “very” or “somewhat” confident in the fit of their selected residents, it remains unclear to what extent the absence of electives impacts this perceived confidence and overall PD satisfaction. In contrast, given that all applicant respondents were those who had matched, naturally, most felt that the absence of electives and virtual format didn't have any impact on their chances of matching to their top programs. The impact of absent clinical electives on perceived satisfaction in surgical candidate selection among PDs remains an interesting consideration for our group, which we hope to address in future studies. Nonetheless, taken together with the ability to increase the flexibility for scheduling, reduced cost for applicants and programs, increased participation of multiple faculty members, and reduced travel for applicants, the advantages of virtual interviewing and applicant recruitment may significantly outweighing limitations of the virtual process presented herein.11,13
Recommendations for applicants
Strong letters and interviews remain the most significant factors in applicant selection, consistent with practices prior to virtual resident selection. 14 Although attendance to virtual information sessions was not reported by PDs to increase likelihood of being offered an interview, many applicants in the 2021 CaRMS cycle found that attendance helped their ability to get to know programs better and make informed decisions on program suitability. Applicants are encouraged by some PDs to reach out to programs in which they are interested, in order to learn more about them, get involved in research, and perform visiting electives, if and when possible. During the interviews themselves, applicants are encouraged to interact with the entire interview panel and treat virtual interviews as though they were in-person. Although interview setup, lighting, and background choice were not significant factors in applicant selection from the perspective of PDs, choice of a quiet, nondistracting, and professional environment, as well as professional attire, can help better-simulate the traditional interview experience (Figure 1).
Recommendations for program directors
Virtual information sessions remain highly valued by applicants as useful tools to get to know programs they are unable to visit; ensuring their sustainability, regardless of interview format in future years, can help promote your program. Applicants are interested in learning about the work environment, resident work–life balance, and resident–staff relationships, in addition to academic and clinical highlights of your program. Given the Association of Faculties of Medicine of Canada (AFMC) elective diversification policy that limits electives within one particular specialty to a maximum of 8 weeks, applicants may no longer count on the ability to perform visiting electives at programs in which they are interested, regardless of waning pandemic restrictions.15,16 Programs may thus need to reconsider policies in which in-person electives represent a major requirement for offering interviews to applicants. Although programs may consider the option of offering an in-person interview in order to better-interact with these applicants, the potential selection bias that may arise toward applicants afforded in-person interviews cannot be ignored. Opportunities for direct faculty and resident interactions with applicants remain highly valued, whether during the virtual information sessions, social events, or interviews themselves (Figure 2).
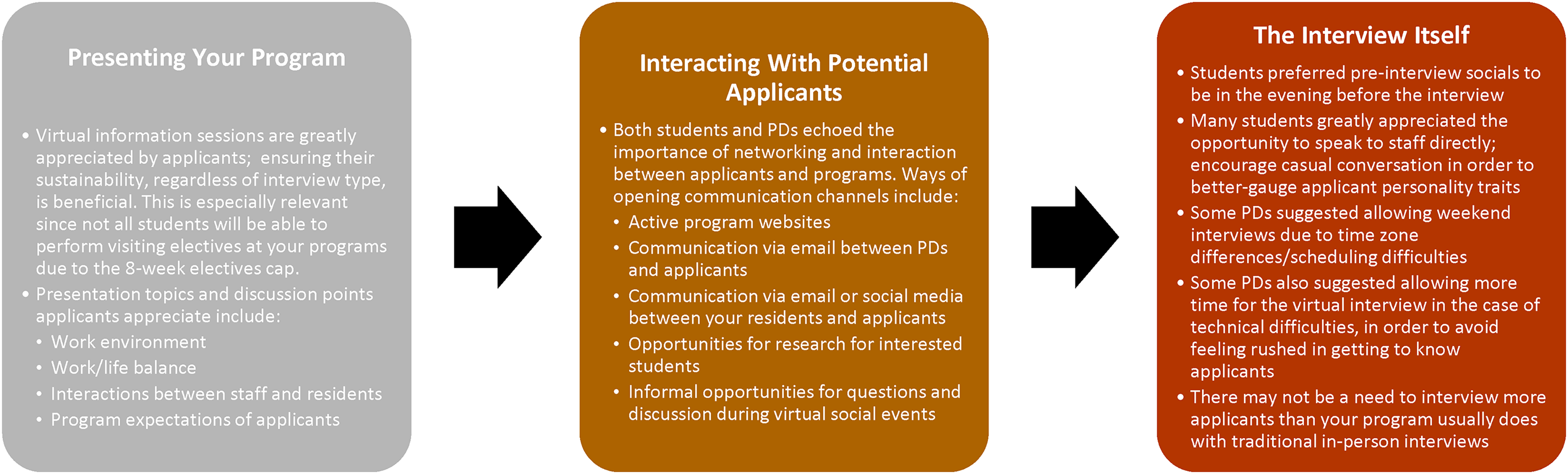
Recommendations for Canadian surgical program directors navigating the Canadian surgical subspecialty resident selection process, based on collected feedback from applicants and program directors.
Limitations
This study is not without its limitations. The cross-sectional nature of this study and lack of follow-up, to better understand the longitudinal impact of the 2021 virtual selection process, cannot be ignored. Additionally, a limited sample size of participants was analyzed, with data captured from 35/128 (27%) of Canadian surgical program directors, 17 and 40/284 (14%) of successful surgical applicants. 18 Overrepresentation of Quebec applicants in the survey process, given affiliation of study organizers to Quebec home programs, may represent an added limitation. Given that the study captured data from only successful applicants, perceptions of the 2021 CaRMS process may be biased in a positive fashion. Lack of control data from earlier cohorts who participated in the traditional CaRMS process precludes strong comparative conclusions. Nonetheless, the conclusions and advice presented herein remain useful as a guide for both applicants and PDs on ways to better-navigate upcoming virtual surgical residency selection processes, during the time of COVID-19, and beyond.
Conclusions
Trainees are entering residency with confidence following virtual interviews, and PDs feel confident in their selections. Although no clear consensus exists regarding preference for a virtual or in-person interview, several advantages for virtual selection exist. The influence of an in-person elective may be difficult to replace, regardless of interview type. The importance of applicant engagement with programs prior to interviews is highlighted and discussed, with guidelines for best practices presented. With surgical residency interviews remaining online despite waning COVID-19 restrictions, PDs and applicants must continuously adapt recruitment and engagement methods in order to optimize their match outcomes.
Supplemental Material
sj-docx-1-psg-10.1177_22925503221108468 - Supplemental material for Successful Applicant and Program Director Perspectives on the Virtual Residency Selection Process for Canadian Surgical Subspecialties
Supplemental material, sj-docx-1-psg-10.1177_22925503221108468 for Successful Applicant and Program Director Perspectives on the Virtual Residency Selection Process for Canadian Surgical Subspecialties by Jad Abi-Rafeh, Victoria Sebag and Hassan ElHawary, Dino Zammit, Mirko S. Gilardino in Plastic Surgery
Supplemental Material
sj-pdf-2-psg-10.1177_22925503221108468 - Supplemental material for Successful Applicant and Program Director Perspectives on the Virtual Residency Selection Process for Canadian Surgical Subspecialties
Supplemental material, sj-pdf-2-psg-10.1177_22925503221108468 for Successful Applicant and Program Director Perspectives on the Virtual Residency Selection Process for Canadian Surgical Subspecialties by Jad Abi-Rafeh, Victoria Sebag and Hassan ElHawary, Dino Zammit, Mirko S. Gilardino in Plastic Surgery
Supplemental Material
sj-pdf-3-psg-10.1177_22925503221108468 - Supplemental material for Successful Applicant and Program Director Perspectives on the Virtual Residency Selection Process for Canadian Surgical Subspecialties
Supplemental material, sj-pdf-3-psg-10.1177_22925503221108468 for Successful Applicant and Program Director Perspectives on the Virtual Residency Selection Process for Canadian Surgical Subspecialties by Jad Abi-Rafeh, Victoria Sebag and Hassan ElHawary, Dino Zammit, Mirko S. Gilardino in Plastic Surgery
Supplemental Material
sj-pdf-4-psg-10.1177_22925503221108468 - Supplemental material for Successful Applicant and Program Director Perspectives on the Virtual Residency Selection Process for Canadian Surgical Subspecialties
Supplemental material, sj-pdf-4-psg-10.1177_22925503221108468 for Successful Applicant and Program Director Perspectives on the Virtual Residency Selection Process for Canadian Surgical Subspecialties by Jad Abi-Rafeh, Victoria Sebag and Hassan ElHawary, Dino Zammit, Mirko S. Gilardino in Plastic Surgery
Supplemental Material
sj-pdf-5-psg-10.1177_22925503221108468 - Supplemental material for Successful Applicant and Program Director Perspectives on the Virtual Residency Selection Process for Canadian Surgical Subspecialties
Supplemental material, sj-pdf-5-psg-10.1177_22925503221108468 for Successful Applicant and Program Director Perspectives on the Virtual Residency Selection Process for Canadian Surgical Subspecialties by Jad Abi-Rafeh, Victoria Sebag and Hassan ElHawary, Dino Zammit, Mirko S. Gilardino in Plastic Surgery
Supplemental Material
sj-pdf-6-psg-10.1177_22925503221108468 - Supplemental material for Successful Applicant and Program Director Perspectives on the Virtual Residency Selection Process for Canadian Surgical Subspecialties
Supplemental material, sj-pdf-6-psg-10.1177_22925503221108468 for Successful Applicant and Program Director Perspectives on the Virtual Residency Selection Process for Canadian Surgical Subspecialties by Jad Abi-Rafeh, Victoria Sebag and Hassan ElHawary, Dino Zammit, Mirko S. Gilardino in Plastic Surgery
Supplemental Material
sj-pdf-7-psg-10.1177_22925503221108468 - Supplemental material for Successful Applicant and Program Director Perspectives on the Virtual Residency Selection Process for Canadian Surgical Subspecialties
Supplemental material, sj-pdf-7-psg-10.1177_22925503221108468 for Successful Applicant and Program Director Perspectives on the Virtual Residency Selection Process for Canadian Surgical Subspecialties by Jad Abi-Rafeh, Victoria Sebag and Hassan ElHawary, Dino Zammit, Mirko S. Gilardino in Plastic Surgery
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
