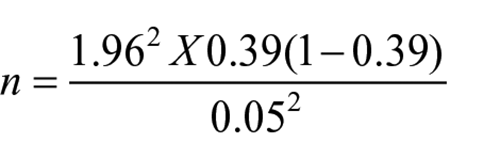Abstract
Background:
Human milk bank is a sustainable source of donor human milk (DHM) which is an acceptable alternative to the mother’s milk and it is not routinely available in Nigeria, a multi-ethnically diverse country.
The study aimed to assess the willingness to donate or accept human milk among pregnant women and mothers attending the antenatal, immunization, outpatient, under-five, and neonatal follow-up clinics in selected health facilities in Ekiti State, Southwest Nigeria.
Study Design and Methods:
A descriptive cross-sectional, mixed methods study design was used to collect data in selected health facilities in Ekiti State. Questionnaires and focus group discussions were used to collect quantitative and qualitative data respectively while data analysis was done using the IBM® Statistical Package for Social Science SPSS version 26® and thematic analysis respectively.
Results:
Of the 798 respondents, 529 (66.3%) and 626 (78.4%) did not know about wet nursing or human milk banking (HMB) respectively and 139 (17.4%) were willing to donate their breastmilk for a stipend. In the focus group discussion, 50% had heard about wet nursing but none heard about HMB. Maternal educational level had a significant impact on their willingness to donate or accept DHM (p < 0.00). Wholesomeness, cultural, and religious biases were major reasons affecting HMB acceptability.
Conclusions:
Awareness and perception of HMB are poor. Appropriate information, education, and counselling on HMB are needed to drive the adoption and establishment of HMB in Nigeria.
Introduction
Mothers’ own milk (MOM) is the best nutrition option for infants, but when unavailable, donor human milk (DHM) can be a suitable alternative. Donor human milk is collected, screened, pasteurized, and stored breast milk from a human milk bank. Although widely accepted in developed countries, DHM’s acceptability and uptake in sub-Saharan Africa, including South Africa and Kenya, remain low.1,2 The American Academy of Pediatrics (AAP) and the World Health Organization (WHO) recognize DHM as an acceptable alternative to MOM.3,4
Fear of disease transmission, cultural, and religious prohibitions as well as concerns about the inadequacy of MOM for the babies of donors, affect the acceptability of human milk banking (HMB).5–7 In addition, the variance between the willingness to donate compared with the willingness to accept with a preponderance towards donating has been reported. 5
Human milk banking has been shown to improve breastfeeding rates in settings where it is practiced and decrease rates of necrotizing enterocolitis (NEC). However, in Nigeria, where exclusive breastfeeding rates are low, knowledge about HMB remains low, and the practice is not yet available for routine use.8–11 A study conducted in the country over two decades ago found a wide gap in the willingness to donate or accept donor human milk (DHM), and more recent research revealed that knowledge about HMB remains low.5,12 To improve the breastfeeding rates in Nigeria and increase the availability of DHM, surveys should be conducted in all geopolitical zones of the country to understand the factors that affect the acceptability of HMB.
This study aims to assess the willingness to donate or accept human milk and knowledge about human milk banking among pregnant women and mothers attending clinics in Ekiti State, Nigeria. The results will guide policies towards establishing human milk banks in the Southwestern region of the country.
Methods
Inclusion criteria
Women at least 18 years of age
Pregnant women attending antenatal clinics in these facilities
Mothers attending immunization, or under-five clinics
Mothers at the Postnatal and Neonatal units
Exclusion criteria
Pregnant women whose foetus are not viable or with doubtful viability.
Women with postpartum haemorrhage or severe complications that were too ill to participate in the study.
Women with postpartum depression or severe mental health conditions.
Women who do not consent to the study.
Sample size
Sample size was calculated using the formula 14 :
where n = minimum sample size,
Z = standard normal variate at 95% CI is 1.96.
P = expected prevalence [39%], 12
d = precision, allowable error margin of 5%.
The qualitative data obtained from the FGDs were transcribed verbatim, translated into English as needed and analysed based on the themes.
Results
Of the 820 questionnaires administered to the mothers, 798 had complete responses and were analysed giving a response rate of 97.3%. The majority (73.6%) were aged 20–34 years, of the Christian religion (91.1%), from the Yoruba tribe (86.7%), had post-secondary education (62.8%), and were married (93.9%). Two-thirds and a third of the respondents patronized the infant welfare/immunization clinic and antenatal clinic respectively. Other socio-demographic characteristics of the respondents are shown in Table 1.
Sociodemographic characteristics of the respondents and Health Services Patronized.

Divorced/cohabiting.
Some individuals used multiple facilities.
Table 2 shows the obstetrics and breastfeeding history. Seven hundred and sixty (95.2%) of the mothers had at least a parous experience. Of these, 719 (94.6%) had antenatal care (ANC) in the immediate past pregnancy and the majority 641 (89.2%) had adequate ANC visits, had last delivery in a healthcare facility 608 (80.0%), and were counselled on breastfeeding 631 (87.8%). Most of the mothers 621 (81.7%) delivered per vagina but only 327 (43.0%) had postnatal clinic attendance which was inadequate in over 80% of this population but the majority of them had breastfeeding counselling. Exclusive breastfeeding was practiced by 560 (73.7%) of the participants while only 388 (69.3%) claimed to have breastfed exclusively for 6 months and 648 (85.3%) were still breastfeeding at the time of the study. Of the women who had patronized the different paediatrics-related health services, breastfeeding counselling was offered at the outpatient department and immunization clinic to 115 (75.2%) and 585 (77.0%) of the participants respectively. Of the 760 mothers, 391 (51.4%) had previous breastfeeding challenges; with delayed milk flow 171 (43.7%) and ‘not enough milk’ 138 (35.3%) being the most common challenges. Of those with ‘not enough milk’, alternative ‘feeds’ given were infant formula 41 (29.7%), corn gruel 30 (21.5%), water 21 (15.2%), adult milk 8 (5.8%), and other preparations including juice and herbal concoction 38 (27.5%). Among the women with breastfeeding challenges, about half 189 (48.2%) did not consult anyone for advice on how to solve the challenge, and about a quarter 97 (24.8%) consulted relatives including the baby’s grandmothers and friends, 90 (23.0%) consulted healthcare workers while the remaining 15 (3.8%) sourced for solutions from other sources.
Obstetrics and breastfeeding history of the respondents.

ANC: Antenatal Clinic; PNC: Postnatal Clinic; COPD: Children outpatient department.
Nulliparous women were excluded.
Multiple responses.
Awareness about HMB
Knowledge of wet nursing was observed to be poor among the 798 study participants as 529 (66.3%) of them did not know about wet nursing and a higher percentage (78.4%) had never heard about HMB. Of the 172 respondents who had heard about HMB, 37.8% and 47.5% heard from the electronic media and healthcare workers (HCW) respectively (Doctors – 10%; Nurses – 12%; Nutritionists/Dietician – 7%; Other HCW – 28%).
Almost all the participants in the FGDs had not heard about HMB, however, about half of them knew about wet nursing. A 24-year-old mother replied ‘You people have come again o. What do you mean by breast milk banking? I have never heard about it. I only know that in the olden days, women used to breastfeed another child in the family if the mother is not around. Which one is breast milk banking again?’ Interactions with the mothers during the FGDs revealed that the practice of wet nursing was no longer widely practiced or acceptable by the mothers.
Opinions and concerns about HMB
More than half of the participants of the quantitative survey felt that HMB was not a good idea. More than half (58.5%) of the respondents felt that HMB is not a good idea, only 24.2% believe it is a good idea while 17.3% don’t know.
Most of the participants of the FGDs did not like the idea of HMB. One of the participants asked – ‘How will you collect breastmilk from a woman and store it? Will she express from home? How are you sure it is her milk? Will it not get spoilt? How will it be preserved? For how long can it be stored?’ ‘It looks odd/ strange to me’, said another 24-year-old mother of one.” ‘Another mother retorted, with the incessant power outages, how will the milk be preserved without it getting spoilt?’
Willingness to donate breast milk
Only 223 (27.9%) of the 798 participants were willing to donate their breastmilk for another baby’s use while 575 (72.1%) were not willing to donate their milk.
Most of the participants in the FGDs, 14 (77.8%), were also not willing to donate their breast milk while the remaining four (22.2%) do not mind if they had more than enough. A 27-year-old woman said, ‘I cannot donate my breast milk even if I have more than enough. The world is dangerous now, in this age of money-making rituals, why should I donate my milk, it can be used for money rituals. I will rather prefer to breastfeed the child if they bring him/ her but I cannot donate my milk for someone to take it away’. Another 26-year-old mother said: ‘I can donate my breastmilk to assist another baby if I have more than enough for my baby, however, I don’t think I have enough for my own baby’.
Reasons for willingness to donate breast milk
Of those who were willing to donate, reasons for willingness to donate were to help other babies in need (52.5%), for health promotion and disease prevention 28.3% (Table 3). The mothers who indicated their willingness to donate their breast milk during the FGDs said it is in their bid to help another baby in need. One of the mothers said, ‘breastmilk is good for every baby, hence her reason for her willingness to donate her milk if she has excess’. Another mother said, ‘breast milk has lots of benefits to babies and infant formula is very expensive, so for these reasons I will be willing to be of help to babies who need such help provided I have excess milk that my baby does not need’.
Reasons for willingness/unwillingness to donate breast milk.

Reasons for being unwilling to donate breastmilk
Among those unwilling to donate their milk, 359 (62.4%) did not like the idea of milk donation and felt it was not right, 82 (14.3%) believed they did not have enough, 79 (13.7%) believed that their family or spouse would not support it while 4.2% felt that it is unhygienic and could transmit diseases (Table 3).
Most of the participants during the FGDs gave reasons similar to the findings of the quantitative survey for being unwilling to donate their breast milk. A 30-year-old woman said, ‘that it is not hygienic and that any disease that runs in the family could affect the child who takes such milk’. A 32-year-old woman gave religious reasons for being unwilling to donate her breast milk or accept her baby to be fed with DHM. She said that it is not allowed in the Islamic religion. She said that the children who take milk from the same source must not marry each other. ‘The two families must know each other and inform the children. It is forbidden in Islam for the children to marry later on in life’ she retorted.
Willingness to accept DHM
When asked if they will allow their baby to be fed with donated human milk (DHM) if the need arises, 677 (84.8%) declined while only 121 (15.2%) of the participants said they may agree.
Only 201 (25.2%) of the study participants said that they may accept DHM if given more information.
Findings from the FGDs were not particularly different as most of the participants were not in support of feeding their baby with DHM.
Reasons for willingness/unwillingness to accept/use DHM for infant feeding
Sixty-seven (55.4%) of the respondents will be willing to use DHM to feed their infant because they know that breast milk is the best for every child, 17 (14.0%) will accept it because it improves the immunity of the child and prevents infections, while 13 (10.7%) will accept it if the doctor advises them to use it. A sizeable number of participants 438 (64.7%) in the quantitative survey did not like the idea, 67 (9.9%) prefer to use of breastmilk substitute, 91 (13.4%) believed the collection and use of human milk is unhygienic and can transmit infections while 28 (4.1%) feared genetic diseases transmission. Table 4 shows the reasons for willingness/Unwillingness to accept/use DHM.
Reasons for willingness/unwillingness to accept/use DHM.

In one of the FGD sessions, there was a 28-year-old mother who also said that she does not mind giving her baby DHM as long as it was recommended by the Doctor. She said that the doctor knows that it is good for my baby, then I have to follow the advice.
The reasons given by the participants of the FGDs were not different from the quantitative survey findings. Most of them were afraid of the transmission of genetic diseases and infections. Three hundred and fifty-eight respondents (62.9%) prefer their relatives to donate milk for their baby if the need arises, 174 (30.6%) will opt for banked human milk while 37 (6.5%) will accept milk from their friends. Close to half (46%) of the participants were not interested in accepting DHM even if they were given more information about it, about a third (28.8%) claimed not to be interested in receiving more information about it while about a quarter (25.2%) claimed that they may likely accept DHM if they were given more information about it. Of the maternal socio-demographic characteristics relating to human milk acceptance and donation (Table 5); more women within the age group of 20–34 were willing to accept DHM while more women above the age of 35 years were more willing to donate compared with other age groups (p > 0.05). Higher proportion of women of the Islamic religion were willing to accept DHM (p < 0.05) and donate human milk (p > 0.05) when compared with their Christian counterparts. Also, higher proportion of married women were willing to accept DHM (p > 0.05) and donate human milk (p < 0.05) when compared with unmarried women. A significantly higher proportion of women who had secondary and post-secondary education were not willing to accept DHM (p < 0.05) and also not willing to donate human milk (p < 0.05).
Relationship between sociodemographic factors and respondents’ attitude towards human milk donation and use.

Among the obstetrics factors (Table 6), it was noted that more women who had breastfeeding counselling during antenatal care were willing to donate their breastmilk or accept DHM but the effect was not significant. However, many of the respondents were not willing to donate or accept DHM despite receiving counselling on breastfeeding during the antenatal period.
Relationship between obstetric factors and willingness to donate or accept DHM for infant feeding.

ANC: antenatal clinic; PNC: postnatal clinic; TBA: traditional birth attendant; SVD: spontaneous vaginal delivery.
More women who delivered via caesarean section 51 (36.7%) compared to those who had SVD (25.4%) were willing to donate their breastmilk or accept DHM. Overall, the majority of the respondents were not willing to donate or accept DHM irrespective of the mode of delivery. It is also important to note that post-natal care and breastfeeding counselling during postnatal care did not improve the respondents’ views or ideas about human milk donation. Though more than 70% of the respondents claimed to have practiced exclusive breastfeeding in their last pregnancy, this did not have any effect on their willingness to accept or donate human milk.
Discussion
The benefits of human milk have been widely reported and propagated. Despite this, MOM may not be available or sufficient in some special situations. Such conditions would include maternal unavailability from perinatal morbidities or illnesses such as HIV infection, medications or demise, multiple births. Such situations will warrant the use of alternatives to MOM and the closest is the DHM which is screened and pasteurized to ensure its safety and wholesomeness. 17 This study conducted in the Southwestern part of Nigeria revealed poor knowledge about human milk banking (HMB), with only 21.6% of respondents having heard of it. This is comparable to the 25.8% reported in South-south Nigeria but lower than the 39% reported in south-east Nigeria.12,18 The suboptimal knowledge is not likely related to maternal education as the majority of participants had post-secondary school education. The lack of HMB practice in Nigeria and neighbouring countries may contribute to the low awareness. The authors suggest that policy interventions are needed to promote and establish HMB in Nigeria.
The willingness to donate milk was slightly lower in this study than that reported in other Nigerian studies but comparable to a study in South-south Nigeria by Iloh et al. 12 In Ethiopia, a lower proportion of mothers were willing to donate, while in Southern Australia, all breastfeeding mothers were willing to donate.7,19 Cultural differences and access to information about HMB could explain this difference. Less than 50% of participants in this study received information about HMB from healthcare workers, similar to what was reported in a study in Benin. 18
Participants in the study expressed unwillingness to donate breastmilk due to concerns about transmission of diseases or infections and feeling that it was not the right thing to do. This is consistent with similar reports from other countries, such as Kenya. 17 Lack of appropriate information about HMB and its processes may contribute to these concerns, indicating a need for public enlightenment on HMB.
The study found that despite receiving information about HMB from healthcare workers, most participants were not willing to donate or accept DHM, indicating the need for healthcare workers to acquire more education about HMB. The proportion of respondents who heard about HMB from electronic and print media is lower than what was reported in Turkey. 20 This finding highlights the potential of electronic media in increasing awareness and disseminating information about HMB.
It is also noteworthy that four out of every five participants in this study were unwilling to allow their babies to be fed with DHM, which agrees with the findings of Abhulimhen et al. 18 in Benin. Many of the participants claimed they just didn’t like the idea while a few will reject the offer because they believe it is unhygienic and that it can increase the risk of infection transmission. In climes where HMB is practiced, facilities for bacteriological testing and treatment are available to ensure that banked milk is wholesome and rid of infection. 21 About a 10th of this category of mothers prefers the use of breastmilk substitutes to DHM. Studies have reported the superiority of DHM compared with breastmilk substitutes in terms of better tolerability by preterm neonates, effectiveness in reducing the risks of late-onset sepsis, and significantly reducing the risks of NEC in newborns especially preterm babies22–24 as well as significantly reducing the length of hospital stay for sick infants and saving on the cost of healthcare.8,25 Very few hinged their reason on cultural beliefs while some mothers rejected the offer based on religious belief. While culture and religion have been reported to affect human lifestyle, it has also been reported to have a negative influence on health-related choices. 26 Most of the reasons given for the rejection of HMB are still evidence of inadequate and inappropriate information about HMB which can be corrected through enlightenment campaigns. These reasons are not different from what has been documented in previous studies.2,7,17,18
Most of the study participants were counselled about breastfeeding during antenatal, outpatient clinic visits, and immunization visits; these counselling sessions did not improve the acceptance of this infant feeding option among our study participants. This may reflect the content of information given during such sessions. There may be a need to encourage healthcare workers to include information about HMB in their counselling sessions. Censored information, education, and counselling materials should be made available with reference to further access to information that the participant can read on their own.
Nigeria has not adopted this WHO-recommended method of alternative infant feeding. Hence the need for multiple stakeholders’ meetings to establish the use of DHM as an alternative infant feeding method. Previous studies conducted in other regions have also reported that various challenges, including cultural and religious beliefs, inadequate information, and poverty, hinder the success of HMB establishment. The involvement of opinion leaders in the community, religious leaders, traditional leaders, media practitioners, and healthcare workers is essential in tackling these challenges and ensuring that the interests of different groups are taken care of. However, this study found that about half of the participants were still unwilling to use DHM even with more information, highlighting the need for continued education and advocacy.
Concerning the choice of donor, of those willing to feed their children with DHM, most of them prefer to use milk from their relatives, this is different from the findings of Kimani-Murage et al. 17 where most of the participants (63%) were only interested in accepting DHM from any healthy mother. Notably, in settings where HMB is practiced, pooled milk sources are usually in place, and donors are usually de-identified.
This study highlights the need for increased awareness of human milk banking (HMB) in Nigeria as a recommended alternative infant feeding option. Healthcare workers should provide adequate information, education, and counselling to mothers about the steps involved in HMB. Policymakers and stakeholders should collaborate with religious leaders to establish HMB in Nigeria and dispel myths and wrong information about the practice.
Footnotes
Acknowledgements
The authors acknowledge all the study participants, the research assistants and the resident doctors who assisted with the data collection.
Authors’ contributions
The study was conceived and designed by EOO and IOD. EOO, AOB, ATA, ABA, OAL, ABT. OAF and AEA assisted with data collection. EOO, IOD and OAF analysed the data. EOO wrote the initial draft. IOD, AOB, ABA, ATA, OAL, OAF, ABT, OBB, AEA and OOS critically reviewed the manuscript. All authors read and approved the final draft of the manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Significance for public health
Are nursing mothers in the southwestern part of Nigeria open to donor human milk (DHM) as an alternative to mother’s own milk since previous studies in other regions of Nigeria revealed a low level of acceptability?
● This study showed that DHM from human milk bank is still not an acceptable alternative to the mother’s milk amongst nursing mothers and pregnant women in Ekiti State, Southwest Nigeria. ● There is a lack of awareness about this method of infant feeding which will affect the level of acceptance of this alternative feeding option. ● There is a need for public enlightenment campaigns about human milk banking in order to improve the knowledge of mothers and hence the acceptability of this method of infant feeding.