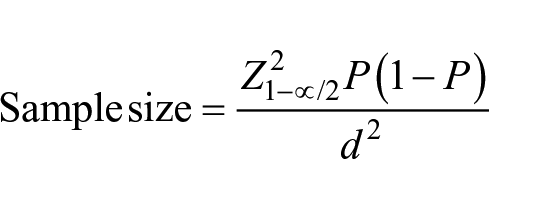Abstract
Introduction:
Psoriasis is a chronic non-contagious inflammatory skin disorder, which might impair patient’s social relationships, limit leisure activities, and lower self-esteem. Psoriasis patients might be stigmatized leading to psychological disorders such as anxiety and depression.
Objectives:
This study aimed to outline the clinical features of psoriasis and its effects on quality of life, and the feeling of stigmatization among psoriasis patients.
Methods:
This cross-sectional questionnaire-based study was conducted on 109 adult psoriasis patients in Arar City, Saudi Arabia. The study collected data on socio-demographic and clinical characteristics of psoriasis patients, self-reported psoriasis severity using the self-assessment Simplified Psoriasis Index (sa-SPI-s), patients’ quality of life using the dermatological life quality index (DLQI), and the feeling of stigmatization using the six-items stigmatization scale.
Results:
The mean age of psoriasis onset in studied patients was 20 (±7.65) years, females represented 58.72%, and 22% were unemployed. Joint and nail affection were reported in 46.79% and 51.38%, respectively. One third of patients had positive family history of psoriasis. Seasonal variation, life stressors, smoking and skin injuries were frequent provocative factors for psoriasis lesions. The average sa-SPI-s was 10.08 (±10.41), which was correlated with patients’ ages, disease duration, obesity, and pruritis. The average DLQI and six-items stigmatization scale for psoriasis patients were 8.95 (±5.77) and 7.61 (±4.5), respectively that were correlated with sa-SPI-s.
Conclusion:
The clinical manifestations and chronicity of psoriasis impaired patients’ quality of life and accompanied with social stigma due to skin disfigurement. These effects need to be addressed for better care of patients.
Introduction
Psoriasis is a chronic non-contagious inflammatory skin disorder characterized by remission and exacerbation. Psoriasis is a multifactorial immune-mediated disorder induced by the interaction between immunogenic, genetic, and environmental factors. It is due to the accelerated multiplication of skin cells resulting in elevated skin lesions with erythema and silvery scales. Lesions vary in shape and size from localized plaques to whole-body affection. Psoriasis can affect nails, which become thickened, laminated, and brittle. Joints can be affected as well and become swollen, painful, and stiff.1–3
Psoriasis affects both sexes at any age, however it is more frequent in adult age, its prevalence ranged between 0.51% and 11.43% compared to 0% to 1.37% in children worldwide. 4 In Saudi Arabia, the prevalence of psoriasis ranged between 2.47% and 5.3% and is common before the age of 30 years.5,6
In 2014, psoriasis was declared a serious disease by the World Health Organization (WHO). 7 The burden of psoriasis lasts a lifetime resulting in impaired patients’ health, reduced work productivity, and economic loss. 8 Psoriasis is a systemic disease associated with psychological, metabolic, and cardiovascular impairments that may cause premature death. 9
Patients with skin diseases, such as psoriasis, not only suffer from illnesses but also negative reactions from others, which might impair their social relationships, limit leisure activities, and lower self-esteem. Psoriasis patients might be stigmatized leading to psychological disorders such as anxiety and depression. Thus, the severity of psoriasis is estimated not only by the extent of skin lesion but also by the quality of life of psoriasis patients. 1
Limited data on the characteristics of psoriasis are available. 4 In addition, a lack of knowledge and awareness was recorded among Saudi people. 10 The rationale for this study was to fill this gap.
Aims and objectives: This study aimed to outline the clinical features of psoriasis and its effects on the quality of life and feeling of stigmatization in patients in the Northern Border Province.
Methods
Study design
This is a cross-sectional questionnaire-based study.
Study setting
This study was conducted on psoriasis patients attending the Dermatological Clinics at the North Medical Tower and Prince Abdulaziz bin Musaed Hospital, Arar City, Northern Border Province, Saudi Arabia.
Sampling method
A purposive sampling technique.
Study sample
The minimal sample size for the study (109) was calculated according to the equation:
Where, (Z1−α/2) is the standard normal variate at 5% type 1 error (1.96); (P) is the expected proportion of psoriasis in Saudi Arabia (5.3%) 5 ; and (d) is the absolute error (0.04).
Inclusion criteria
Adult male and female psoriasis patients attending the above-mentioned clinics who accepted to participate in the study and fulfilled the following criteria:
Age: ≥18 years old
Had a definite diagnosis of psoriasis confirmed by a dermatologist
The duration of psoriasis was more than 1 year.
Absence of uncontrolled illnesses (e.g., hypertension, diabetes mellitus, heart diseases, etc.) and other skin diseases over the past 3 months.
Data collection procedure
After necessary approval from LCBE, administrative authorities of health affairs, and defined clinical settings, the data collection process was carried out from May to August 2021. Eligible patients were identified and communicated by the principal and coinvestigators and briefed about the study and requested for their willingness to participate in this study through written informed consent. An electronic Google questionnaire was used to collect data.
Tools for data collection
An electronic structured questionnaire in the Arabic language was used to collect data. An electronic format of the questionnaire was used instead of the paper format due to the circumstances of the new coronavirus 11 epidemic to prevent the transmission of infection. This is an open-source and validated questionnaire based on an extensive review of relevant literature and consists of four parts:
Part I: This collects data on socio-demographic and clinical characteristics. It includes questions on socio-demographic characteristics of studied patients such as age, sex, educational level, occupation, and family history of psoriasis. Participants were asked to report their body weight and height. Data were collected on clinical characteristics of studied patients such as affected area, triggering factors, pruritis, arthritis, nail affection, onset of diseases, and treatments received.
Part II: This assesses Psoriasis severity using the self-assessment Simplified Psoriasis Index (sa-SPI-s). This tool has been translated and validated for use among Arab patients in previous studies.12,13 First, the patient was asked to score the severity of psoriatic lesions in 10 body areas as 0 (clear or minor), 0.5 (obvious), or 1 (widespread). Second, the patient was asked to give an average score for his/her psoriasis lesions as 0 (clear or just slight redness of staining), 1 (mild redness or scaling with no more than slight thickening), 2 (definite redness, scaling, or thickening), 3 (moderately severe with obvious redness, scaling, or thickening), 4 (very red and inflamed, very scaly, or very thick), or 5 (intensely inflamed skin with or without pustules). The product of the first and second scores produced the sa-SPI-s index, which was then subdivided into mild (<10), moderate (10–20), or severe (>20) psoriasis.
Part III: Dermatological Life Quality Index (DLQI): The 10-items self-assessment tool aims to assess the effects of dermatological diseases on quality of life of patients. They include items related to symptoms and feelings (items 1 and 2), daily activities (items 3 and 4), leisure (items 5 and 6), work and school (item 7), personal relationships (items 8 and 9), and treatment. 14 Patients were asked to rate their responses as 0, 1, 2, and 3 corresponding to “not at all/irrelevant,” “a little,” “a lot,” and “very much,” respectively. Responses were then summed to give the DLQI score, the higher the score, the poorer the quality of life. The score was categorized into five subgroups: 0–1, 2–5, 6–10, 11–20, and 21–30 corresponding to “no effect at all on patient’s life,” “small effect on patient’s life,” “moderate effect on patient’s life,” “very large effect on patient’s life,” and extremely large effect on patient’s life,” respectively.
Part IV: Six-items stigmatization scale: This includes six questions that participants answered as 0, 1, 2, or 3 corresponding to “not at all,” “sometimes,” “very often,” and “always,” respectively. The sum of the answers gives the stigmatization score, the higher the score, the more feeling of stigmatization (range 0–18). 15
Statistical analysis
Data were described as frequency and percentage for qualitative data and mean ± standard deviation (SD) and range for quantitative data. The distribution of quantitative data was examined using the Shapiro-Wilk test for normality. The Spearman correlation coefficient (ρ) was used to test the correlation between psoriasis severity and patients “ages, age of marriage, age of onset of psoriasis, duration of psoriasis, Body Mass Index (BMI), DQLI, and six-items stigmatization scores.” The Chi-square test and the Fisher exact test were used to compare psoriasis grades by the different categorical variables as appropriate. Two-sided p values <0.05 were considered as statistically significant. The Microsoft Excel and the STATA/SE version 11.2 for Windows (STATA Corporation, College Station, Texas) were used for data entry and analysis.
Results
A total number of 109 psoriasis patients were involved in this study. Their ages ranged between 18 and 66 years with an average of 35.39 (±12.11) years and females comprised 58.72% of studied patients. Detailed demographic and clinical data of the study participants are shown in Table 1.
Demographic and clinical characteristics of the studied psoriasis patients.

For only married, divorced, and widows (n = 83).
For patients with psoriasis arthritis (n = 51).
Regarding the triggering factors for psoriasis lesions, 33.94% of patients reported that changes in seasons cause their lesions to inflame, while life stresses, smoking, and skin injuries were reported by 16.51%, 11.93%, and 10.09%, respectively. Weight gain, steroid withdrawal, and lithium (a psychiatric medication) were reported as provocative factors in 6.42%. Infections, calcium, and ACI inhibitors were reported by 5.5%, 1.83%, and 0.91%, respectively.
Figure 1 shows the frequency distribution of patients’ responses to sa-SPI-s items (Panel A), their average psoriasis severity (Panel B), and the grades of psoriasis (Pabel C). The average sa-SPI-s was 10.08 (±10.41). Most patients had mild psoriasis (60.55%), while moderate and severe psoriasis was reported in 22.94% and 16.51%, respectively.

Self-assessment Simplified Psoriasis Index-severity (sa-SPI-s)a response (Panel A), average psoriasis severity (Panel B), and grades (Panel C) for the studied psoriasis patients.
Table 2 shows the DLQI and the six-items stigmatization scale among studied psoriasis patients. The average DLQI was 8.95 (±5.77) with 41.28%, 21.1%, 22.94%, and 14.68% had a very large effect, moderate effect, small effect, and no effect were, respectively. The average stigmatization scale was 7.61 (±4.5). Ten patients (9.17%) had no stigmatization (0 point) and seven patients (6.42%) had only minimal feeling of stigmatization (1–2 points).
Categorical data were presented as number (%).
Basra et al. 14
Evers et al. 15
The Spearman correlation coefficient (ρ) was used to examine correlations between sa-SPI-s in studied patients and their quantitative data. There were significant positive correlations between sa-SPI-s and DLQI (ρ = 0.45; p < 0.001), six-items stigmatization scale (ρ = 0.31; p = 0.001), patients’ ages (ρ = 0.27; p = 0.004), duration of psoriasis (ρ = 0.25; p = 0.01), and BMI (ρ = 0.31; p = 0.0009) as demonstrated in Figure 2. There were no significant correlations between sa-SPI-s and age at marriage and age when first diagnosed with psoriasis.

Correlation between self-assessment Simplified Psoriasis Index-severity (sa-SPI-s)a and Dermatology Life Quality Index (DLQI)b (Panel A), six-items stigmatization scalec (Panel B), patients’ ages (Panel C), duration of psoriasis (Panel D), and Body Mass Index (BMI) (Panel E) in psoriasis patients.
Table 3 shows relationships between the grades of psoriasis and demographic and clinical characteristics of psoriasis patients. Mild psoriasis was more likely among patients who were below 30 (p = 0.005) and those with <10 years duration (p = 0.001). Pruritis was reported more by patients with severe and moderate psoriasis than those with mild psoriasis (83.33%, 80.0%, and 54.55%, respectively; p = 0.016). The proportions of obese patients were higher among those with moderate and severe psoriasis compared to mild psoriasis (44.0%, 38.89%, and 19.7%, respectively; p = 0.03). There were significant differences between psoriasis patients as regards their occupations (p = 0.009) and treatment received (p < 0.001).
Relationship between self-assessment Simplified Psoriasis Index-severity (sa-SPI-s) grades a and demographic and clinical characteristics of psoriasis patients.

χ2: the Chi-square test; FET: Fisher Exact test; P: probability.
For patients with psoriasis arthritis (n = 51)
There were significant differences between patients with different grades of psoriasis severity and their quality of life (Figure 3). The proportion of patients with a very large effect on DLQI was higher among patients with severe and moderate psoriasis compared to mild psoriasis (77.78%, 48.0%, and 28.79%, respectively; p < 0.001).

Relationship between self-assessment Simplified Psoriasis Index-severity (sa-SPI-s)a and Dermatology Life Quality Index (DLQI)b (p < 0.001 using the Fisher exact test) among psoriasis patients.
Discussion
This study was conducted to determine the clinical features of psoriasis and its implications for quality of life among adult patients in Northern Saudi Arabia.
The mean age of psoriasis onset in this study was 20 (±7.65) years, with 52.29% of patients first diagnosed with psoriasis under 20 years of age, 33.03% between 20 and 30 years, and 14.68% were diagnosed ≥30 years of age.
It has been demonstrated psoriasis has a bimodal pattern. The incidence increases in late teens and 20s and again in 50s and 60s with slightly later ages in males than females.16–18 In our study, this bimodality was not evident since patients under 45 years of age represented 75% of the study population with a higher proportion of female than male patients, which increased the frequency of early-onset psoriasis while the next psoriasis wave was absent. By agreement, 72.9% of patients enrolled in the Psoriasis Longitudinal Assessment and Registry (PSOLAR) had early-onset psoriasis. 19 However, in Denmark, the peak incidence of psoriasis was recorded among individuals over 50 years of age and the least psoriasis incidence was in the 0–19 year age group. 20 Also in the UK, the peak incidence of psoriasis was in the 60–69 age group. 21
The average age of psoriasis onset in adults has been recorded in the USA, 22 Pakistan, 23 and Malaysia 24 around the 30s (32.8 ± 24.1 years, 30.48 ± 14.37 years, and 35.14 ± 16.16 years, respectively) and males were more likely to have a later age of onset than females in the latter two studies. Whereas, the average age of psoriasis incidence ranged between 47.7 and 49 years in Denmark 20 and the UK. 21
Previous studies have shown no fixed sex differences in psoriasis patients. 18 Some studies showed a higher percentage of male patients that ranged from 56.6% to 76.9% such as Mohd Affandi et al., 24 Soliman, 13 and Ejaz et al. 23 Similarly, Ding et al. 25 reported a higher prevalence of psoriasis among males compared to females (0.54% vs 0.44%). In Malaysia, there was no sex difference in young patients, as with age, male patients constituted higher proportions. 26 However, in the current study females represented 58.72% of psoriasis patients. In agreement with our results, female patients were slightly higher than males (1.62% vs 1.53%) in the USA National Health and Nutrition Examination Survey. 27 In addition, females accounted for 54% of psoriasis patients in Denmark. 20 In the UK, psoriasis incidence was higher in women than men 9 with a female predominance in early-onset psoriasis while a male predominance was noticed in late-onset psoriasis. 21 Nonetheless, no significant differences were detected in the prevalence of psoriasis in the USA between males and females (2.8% vs 3.2%, respectively). 22
The average age at marriage among the studied psoriasis patients was 24.34 (±3.84) years, which is not different from the average age of marriage in the KSA according to 2016 demographic survey, which reported the average age of first marriage was 26.3 and 21.8 years for males and females, respectively. 28 Similarly, there were no differences in the prevalence of psoriasis by marital status among US adults. 22 However, it has been reported that the probability of marriage was reduced in Swedish patients with psoriasis over time. 29
Our results revealed that the higher the educational level of psoriasis patients, the more likely they were to have mild disease, however this was at a borderline p = 0.05. This is consistent with the findings of a previous study among Arab psoriasis patients, and was explained by the lack of acceptance of the disease by the less educated, which made them overestimate their illness.13,30 The unemployment rate in this study was 22% with a higher frequency in patients with moderate and severe psoriasis. Moreover, in Sweden, psoriasis patients were unlikely employed over time. 29
Psoriasis arthritis is arthritis associated with psoriasis, which increases the burden of psoriasis on the healthcare system and can interfere with patients’ daily activities and lower the quality of life. The prevalence of psoriasis arthritis has shown geographical and ethnic variability with higher prevalence in Western countries compared to Asian countries, which was also related to the different diagnostic tools used. 31 In this study, 46.79% of patients reported psoriatic arthritis, with more than half having coincident joint and skin lesions and about a quarter having arthritis after skin lesion. Peripheral joints were affected in a third of patients and axial joints were slightly more affected (35.29%).
However, psoriasis arthritis was less frequently reported by the international PSOLAR study (38.5%). 19 In addition, joint affection was reported in 13.7% of registered Malaysian psoriatic patients with a higher frequency in female patients than males (16.3% vs 11.8%). 24 Moreover, psoriasis arthritis was reported by 11% of patients in the USA 32 and only 8% of newly diagnosed psoriasis cases in Italy. 33 Mohd Affandi et al. 24 found that oligoarthritic was the most frequent type followed by bilateral polyarthritis, distal hand arthritis, spondylitis/sacroiliitis, and arthritis mutilans (37.3%, 30.6%, 29.6%, 7.4%, and 2.8%, respectively). Meanwhile, Mishra et al. 31 reported that bilateral symmetrical polyarthritis followed by oligoarthritic were the most frequent forms of psoriasis arthritis (46% and 44%, respectively). The higher prevalence of psoriasis arthritis in our study could be because arthritis was identified based on self-reported data rather than more specific clinical examination and exclusion criteria of other forms of arthritis.
Nail affection was reported by more than half of psoriasis patients in our study. Similar results were reported in Malaysia, where 57.1% of psoriasis patients had nail affection with more prevalence in male than female patients (62.0% vs 50.6%). 24
In the present study, local treatment was the most frequent treatment received by psoriasis patients (46.79%), particularly those with mild disease, followed by systemic treatment (34.86%), and phototherapy (18.35%). By agreement, local treatment was the most frequently used by Italian psoriasis patients (45.3% and 47.2% for local non-steroidal and corticosteroids preparations, respectively) followed by systemic immunosuppressants and vitamin A (7.5%). 33 Similarly, local steroids were the first-line treatment in 75.3% of psoriasis patients while systemic treatment and phototherapy were prescribed in 18.4% and 2.8%, respectively. 24 Furthermore, local treatment was used by 94% of patients versus 4% systemic treatment and 2% did not receive treatment during 1-year follow-up. 34 In agreement with these results, local corticosteroids were more frequently used by psoriasis patients compared to controls. 29
Systemic treatment has been frequently consumed by psoriasis patients with more severe disease and longer duration while mild to moderate cases have been adequately treated with topical corticosteroids, vitamin D analogs, keratolytics, tar preparation, or phototherapy.16,19,35
Psoriasis results from the interaction between immune, genetic, and environmental factors. A positive family history of psoriasis was found in 47.5% of patients with early-onset psoriasis and 36.9% of those with late-onset psoriasis. 19 In the present study, about one-third of patients had a positive family history of psoriasis. By agreement, 23.1% of psoriasis patients reported positive family history, which was more frequent in female patients. 24
A wide range of provocative factors for psoriasis has been identified. Exposure to environmental and daily stressors can flare up psoriasis lesions mainly through hypothalamic-pituitary-adrenal pathway, sympathetic-adrenal-medullary pathway, peripheral nerves, and immune system. 36 In our study, seasonal variations were reported by a third of patients followed by life stresses, smoking, and skin injuries (16.51%, 11.93%, and 10.09%, respectively). Other factors such as weight gain, steroid withdrawal, certain medications, and infections have been reported by smaller proportions. Stress, sunlight, and infections were the most common triggering factors by Malaysian patients (48.3%, 24.9%, and 9.1%, respectively). 24
The average sa-SPI-s in this study was 10.08 (±10.41). Most patients had mild psoriasis (60.55%), while moderate and severe psoriasis were reported in 22.94% and 16.51%, respectively. Comparable results have been reported among186 psoriasis patients from 15 different countries, the average sa-SPI-s was 9.6(±8.6), 37 and 221 Arab psoriasis patients with a mean (95% CI) sa-SPI-s of 10.9 (9.6–12.2). 13
In this study, sa-SPI-s was correlated with patients’ ages and disease duration with mild psoriasis was more frequent in patients <30 years of age and disease duration <10 years. Consistent with our results, higher sa-SPI-s was recorded among patients aged 31–40 years and among those with early-onset psoriasis <10 years of age. 13
Pruritis is the most frequent and troublesome manifestation of psoriasis. In this study, the prevalence of pruritis was 65.14% with higher frequency in patients with severe and moderate psoriasis than in mild psoriasis (83.33%, 80.0%, and 54.55%, respectively). In Australia, more than 80% of psoriasis patients had pruritis varying from all the time to occasional itching, which has been associated with severe psoriasis (PASI > 10). 38
The prevalence of obesity in the studied psoriasis patients was 28.44% with a significant positive correlation between psoriasis severity and BMI. The link between psoriasis and obesity has been reported by previous studies. In Malaysia, the prevalence of obesity in psoriasis patients was 24.3%. 24 In addition, the likelihood of obesity was more than 50% higher in psoriasis patients compared to the general population and obese patients were more likely to have moderate to severe psoriasis than mild disease. 39 By agreement, psoriasis patients were more likely obese than non-diseased (42.3% vs 33.7%). 40
Psoriasis manifestations have adverse effects on patients’ quality of life. However, these effects have not been adequately addressed in developing countries in Africa and the Middle East due to the brief time of consultation. 41 In our study, the average DLQI for psoriasis patients was 8.95 (±5.77) with 41.28%, 21.1%, 22.94%, and 14.68% of patients having very large effect, moderate effect, small effect, and no effect, respectively. DLQI for studied psoriasis patients was positively correlated with their disease severity. Soliman 13 scored an average (95% CI) DLQI for Arab psoriasis patients of 11.3 (10.2–12.3) that was moderately correlated (ρ = 0.34, p = 0.0001) with psoriasis severity. The average DLQI for 176 Moroccan psoriatic patients was 11.8 (±7.9), which was associated with disease severity and older age. 42 In Malaysia, the mean DLQI ranged between 7 and 8.5.24,43
In Kuwait, more than 50% of psoriasis patients had impairment in their physical activities and social relationships, and a third of them had their sexual activities adversely affected because of psoriasis. In addition, physical activities and psychological feelings were significantly worse with increased psoriasis severity. 44 Moreover, psoriasis patients had a worse quality of life compared to patients with vitiligo and onychomycosis, particularly for those with lesions in exposed skin areas. 45 In the USA, 39% of psoriasis patients reported that their disease was a large problem in everyday life. 32 Psoriasis has been also claimed to reduce work productivity and increase sick leave and loss of working days. 46
The skin is the mirror that reflects us to the outside community. Unhealthy skin makes patients unconfident about their image and makes them feel that other people are uncomfortable seeing their skin lesions. This stigma has been linked to psoriasis patients and can lead to withdrawal, anxiety, depression, and even suicide attempts. 47 In this study, the average six-item stigmatization scale was 7.61 (±4.5) and the most frequent disturbing feelings were thinking others stare at my skin disease (1.4 ± 0.94) and others avoid me due to my skin disease (1.37 ± 1.03). Only 9.17% and 6.42% had none (0 point) or minimal (1–2 points) feelings of stigmatization, and the remaining patients reported higher levels of stigmatization. Our results revealed a positive correlation between psoriasis severity and six-items stigmatization scale. The mean six-item stigmatization scale for Arab psoriasis patients ranged between 5.6 and 7.48,49 Soliman 49 reported that only 4.0% (n = 8) of psoriasis patients had no feeling of stigmatization and the common disturbing feelings were others stare at my skin disease 83.4%, people are not attracted to me because of my skin disease 78.9%, and people are avoiding me due to my skin disease 53.8%. In the United Arab Emirates, 12.0% (n = 13) and 16.7% (n = 18) had none and minimal feelings of stigmatization and the most troublesome feeling were others think that my skin disease is contagious and others stare at my skin disease. 48 By agreement, 73% of Dutch psoriasis patients experienced stigmata on at least one of the six-items stigmatization scale and the common troublesome feelings were others stare at my skin disease (61.9%), people think my skin disease is contagious (44.9%), and being unattractive due to my skin disease (38.1%). 50
This study is by far the first study to demonstrate the clinical features of psoriasis and its implications for the quality of life in Arar City, the largest city of Northern Saudi Arabia. The cross-sectional design of this study was easy, rapid, and convenient for online self-reported data tools with minimal cost. Self-reported data collection tools were helpful to assess patients remotely within the era of the COVID-19 pandemic, which is also in line with the development of telemedicine and remote management of patients away from the health facilities. 11 In addition, the employed tools have been widely used as valid and reliable tools to assess psoriasis severity. 12
The main drawbacks of the present study were selection bias due to the inability of illiterate patients and those who were unfamiliar with online participation to complete the electronic self-reported questionnaire. In addition, the way patients perceive their illness would influence their responses, which could misestimate the disease conditions. Besides, the study design did not enable the assessment of impacts of psoriasis on patients’ quality of life over time. It is therefore recommended that further large-scale prospective studies be conducted to assess the extent to which psoriasis can affect patients’ lives.
Conclusion
In conclusion, the onset of psoriasis was commonly below the age of 30 with a higher frequency for females with a positive family history of psoriasis. Significant proportions of psoriasis patients participating in this study had joint and nail problems and were unemployed. Seasonal variation, life stressors, smoking, and trauma were the common provoking factors for psoriasis lesion. Moderate to severe psoriasis was reported by 40% of patients and was associated with longer disease duration, pruritis, and obesity. Psoriasis has reduced the quality of life of patients and associated with social stigma due to skin disfigurement. The results of this study will help to better understand the problem of psoriasis and its impact on patients’ quality of life, improve patients’ healthcare and provide support to reduce stigma and enjoy a satisfactory life quality.
Footnotes
Author contributions
All authors contributed equally to this work.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics approval
This study was approved by the Local Committee of Bioethics (HAP-09-A-043) at the Northern Border University, which has issued decision no. (25/42/H) dated on 26/04/2021, during its 12th meeting for the academic year 2020–2021.
Consent to participate
An informed consent was given by all participants. includes all details about the study (title, objectives, methods, expected benefits and risks, and confidentiality of data).
Availability of data and material
Data will be available on reasonable request from the corresponding author.