Abstract
Orthopaedic undergraduate teaching in Hong Kong largely consists of didactic teaching and ward-based bedside teaching, despite being a ‘surgical’ specialty. With newer teaching activities introduced by teachers to enhance learning, students’ perception of these newer learning modalities may not be in sync with teachers’ expectation. In particular, the practical procedural aspect remains unsatisfactory with large proportion of students expressing lack of confidence in performing procedures that teachers deemed to be core skills. Aligning students’ and teachers’ expectation and perception could improve the overall satisfaction and competency in orthopaedic teaching.
Dear editor,
Musculoskeletal health has become more widely valued by the public. Locally trained medical graduates are expected to have proficient knowledge in managing musculoskeletal diseases, whether they work as primary care physicians, emergency physicians or orthopaedic surgeons. The local undergraduate orthopaedic curriculum is designed to cover common musculoskeletal diseases and those that should not be missed. This is delivered over 6 to 8 weeks of contact time in both medical schools in Hong Kong, with stepwise exposure provided from Year 4 to Year 6 via clinical rotations. Despite orthopaedics being a ‘surgical’ specialty, knowledge is largely conveyed through didactic lectures and ward-based bedside teaching, mostly within university hospitals by academic staff but also in regional hospitals by honorary teachers. Assessment is also largely knowledge-based via written examination and clinical skill stations, without any in orthopaedically related procedural skills. The recently revamped clinical curriculum sees more innovative forms of teaching activities aimed at increasing learning efficiency and improving students’ engagement during the process of acquiring knowledge, 1 with problem-based small group learning, team-based clinical attachment and sessions in the operating theatre. However, whether teachers’ expectation and goals align with students’ perception is often undetermined.
We therefore designed a single-institution cross-sectional survey targeted at a single cohort of students to investigate students’ perception on efficacy of current orthopaedic undergraduate teaching activities and how confident they are in the primary learning outcomes by the end of orthopaedic rotation in final year. An online anonymous questionnaire was distributed in January 2022 to all 229 final-year medical students, with 84 responses eventually received. All study participants had already completed their orthopaedic specialty clerkship by the time of recruitment. Students were asked to rate on Likert scale of 1 to 5 on helpfulness of current clerkship teaching activities and how confident they were in selected clinical scenarios. Quantitative parameters were analysed using standard descriptive statistics.
With 4 or above on a helpfulness scale of 1–5 (meaning quite helpful or very helpful), highest ratings were received in bedside teaching (96%), seminars (80%) and assistant intern week (75%), where lowest ratings were found in grand rounds (38%) and case conferences (27%), with similar trend seen in mean scores (Table 1). Traditional teaching modalities with didactic seminars and bedside teaching seemed to withstand the test of time and consistently achieved highest ratings among students. This reflects that despite the trend of reducing didactic teaching load, these remain to be gold standard in clinical teaching, both from teachers’ and students’ point of view. These modalities are proven effective and should be continued. Students also valued small group activities, efficacy of which has been well established 2 and consistent with our institution's effort in increasing small group teaching to enhance learning.
Student rating on existing teaching activities and confidence in managing common clinical scenarios in orthopaedics.
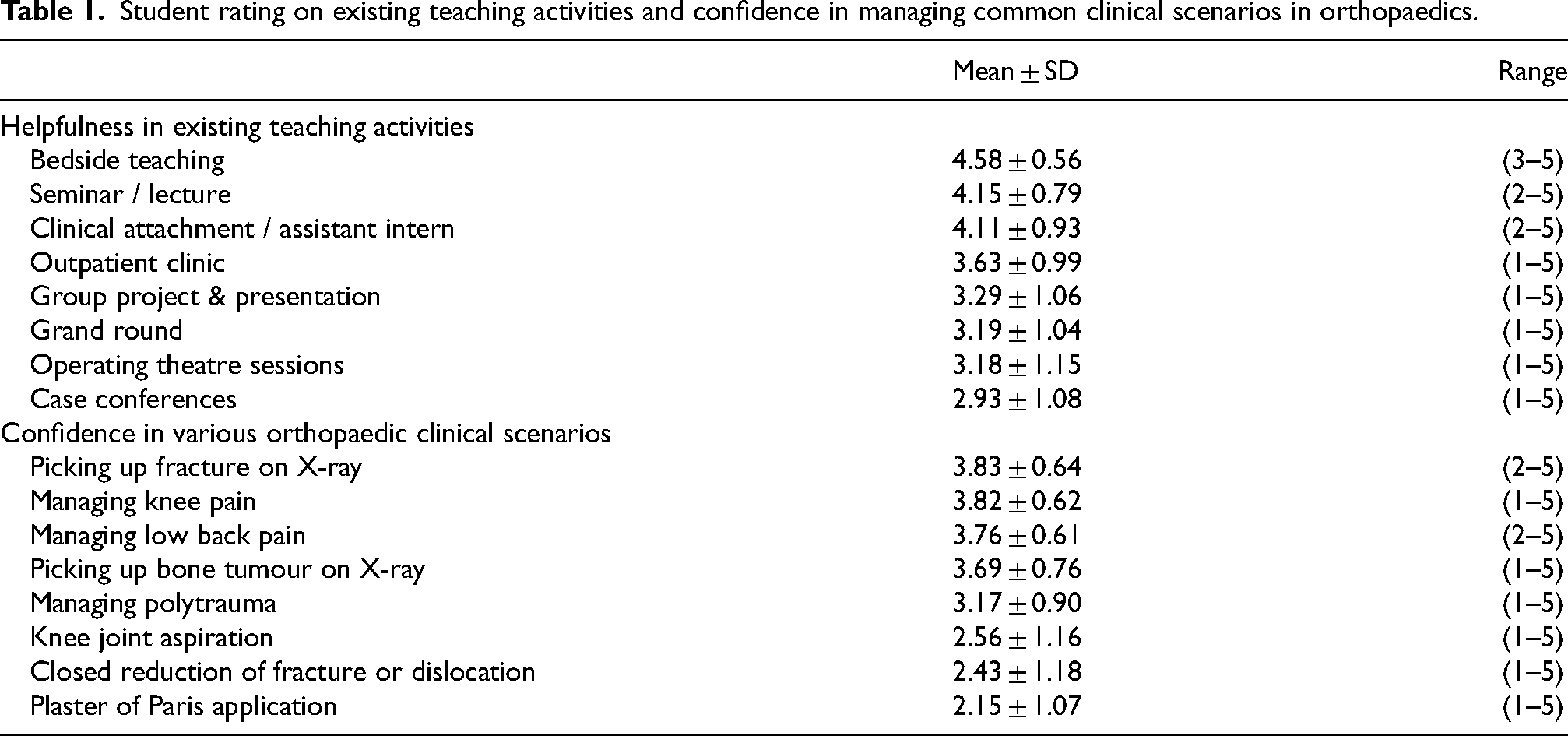
Teaching activities that were introduced recently in the curriculum, such as clinical attachment in the form of assistant intern week and new case outpatient clinics, were also rated highly in terms of helpfulness in students’ learning. However, observing surgery in operating theatre, participation in grand rounds and attendance in clinical case conferences were rated low scores. This suggests that routine clinical service may not be the best learning activities from students’ perspective, as these are often service-based rather than educationally focussed activities. Potential room for improvement includes incorporation of active learning and participation modalities within these teaching activities, such as handpicking several cases where students would participate actively by case presentation or offering consultations under supervision – in other words, ‘practice-based learning’ or ‘experience-based learning’ which was shown to be an effective pedagogy in improving students’ capability and competency in offering clinical care. 3
As for the outcome of achieving primary learning objectives, majority of students expressed confidence (with score of 4 or 5) in management of knee pain (81%) and recognizing fracture on X-ray (75%), but only a small proportion reported confidence in knee joint aspiration (24%) and cast application (15%) (Figure 1). These results showed that students are generally confident in offering consultation, reading radiographs and formulating treatment plan in core knowledge taught in the curriculum, indicating that teachers were effective in delivering core knowledge in orthopaedics. However, less than 40% were confident in managing polytrauma patients despite seminars on polytrauma, reflecting the need for increased exposure and hands-on simulation training in particular. On a related note, most medical students exhibited uncertainty in common practical skills such as cast application for immobilization of fracture and dislocations, and knee joint aspiration for diagnosis and treatment of knee effusion. These simple procedures were useful not just in orthopaedic surgery, but also in general internal medicine, family practice and emergency care, where proficiency should be expected in all medical graduates. Overall, students looked forward to receiving teaching in active clinical skills and procedures, but these were not addressed adequately in the current orthopaedic teaching arrangement. While there are medicolegal implications in procedures performed by medical students who have yet to obtain medical license, which limits the opportunities in practical procedures, this could be supplemented by man-made models, simulation tools, or even virtual reality. 4
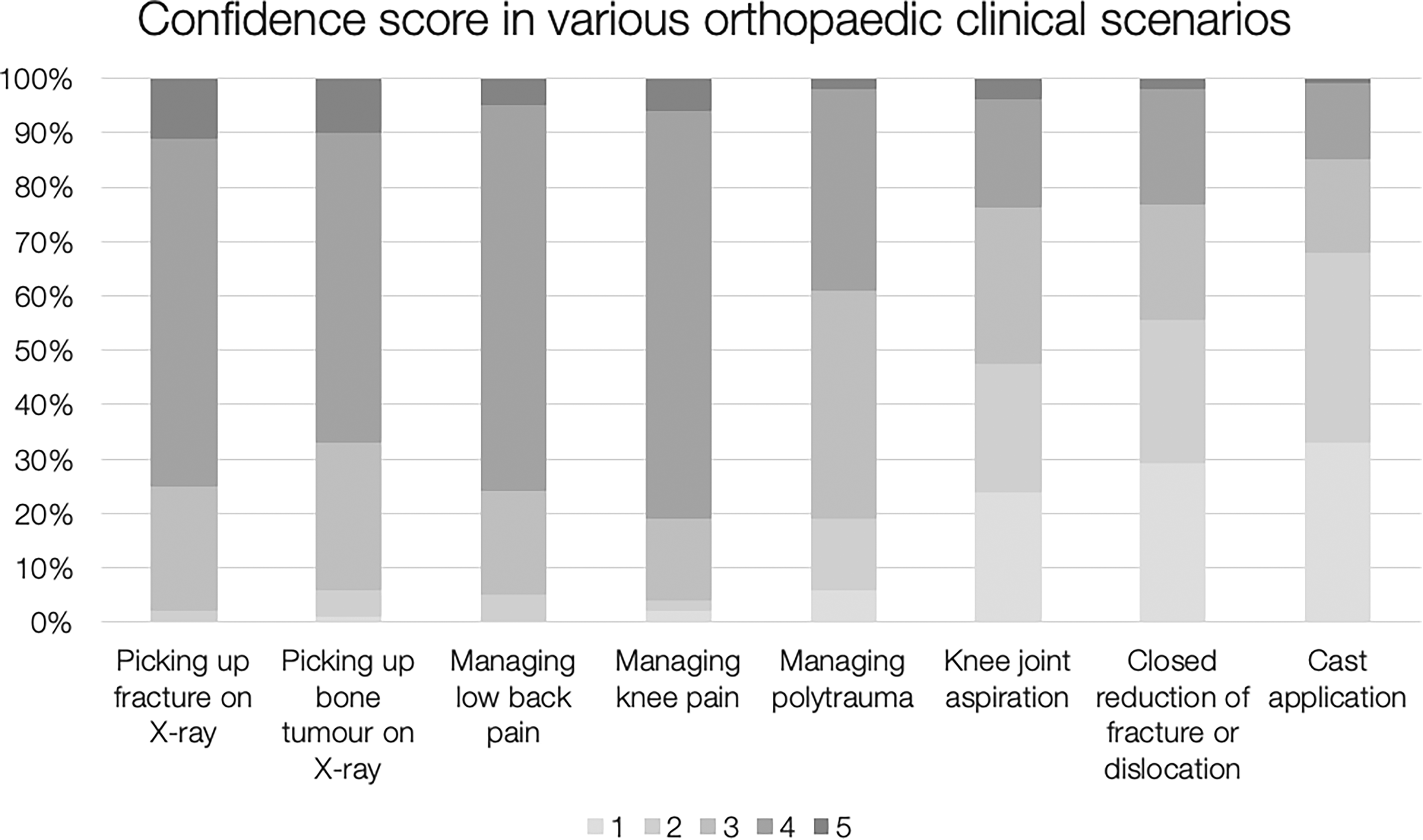
Confidence score in various orthopaedic clinical scenarios.
Apart from maintaining core competency that should be achieved in every medical graduate, we should also cater to students’ wants as student-centred teachers to enhance intrinsic motivation, 5 which does not contradict with upholding professional standards. Students’ perception in newer modalities of teaching activities varied and did not always align with teachers’ goals and objectives. There is still room for improvement in enhancing student experience and student-centred learning in Hong Kong, but results of this survey can be extrapolated to any institution and region around the world.
Footnotes
Declaration of conflicting interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Results in this study were presented at the Tripartite Medical Education Conference Hong Kong 2023 (14–15 January 2023). The author declares no conflict of interest otherwise.
Funding
The author received no financial support for the research, authorship, and/or publication of this article.
