Abstract
Introduction
Patellar stability is the result of the complex interplay between several anatomical and biomechanical factors including overall limb alignment, femoral valgus, trochlear dysplasia and dynamic balancing of forces acting at the patellofemoral interface. 1 When one or more risk factors are present patellofemoral kinematics may be altered and patellar maltracking or instability may result, possibly leading to anterior knee pain or lateral patellar dislocation.2,3 In this context, despite the debate concerning its clinical utility, the fundamental principle of an altered force vector acting on the patella influenced the development of surgical strategies to improve patellar tracking. 4 Based on the assumption that the correction of an excessive Q-angle in genu valgum could reduce the lateral vector applied to the patella, 5 distal femur varus-producing osteotomy was postulated to be an effective option in the treatment of patellar instability associated with a valgus deformity.6,7 Several recent studies reported on patients with valgus malalignment and patellofemoral symptoms and showed reliable patellar stabilization after distal femoral varus osteotomy.1,4,6,8–11
While distal femur varus osteotomy seems to be clinically effective in the management of patellofemoral instability associated with genu valgum, the exact mechanisms for this are unclear and detailed biomechanical implications of femoral osteotomy on the patellofemoral biomechanics are just starting to be elucidated.12,13 Moreover, literature on this subject remains scarce and consists mostly of small case series. The aim of the present study is to pool the evidence from the existing studies in order to elucidate the biomechanical implications and clinical outcomes of distal femur varus osteotomy for patellar instability in the setting of genu valgum.
Data source and studies selection
An extended research on PubMed, Google Scholar, and Embase was performed by two independent authors (FMG and GR) using various combinations of the following keywords: “Femoral distal osteotomy”, “Valgus correction”, “Varus osteotomy”, and “Femoral osteotomy”. A total of 167 related articles were identified through databases searching. After title screening and abstract reading 39 studies were included based on the following inclusion criteria: the osteotomy was performed at the level of the distal femur, bone alignment by a varus-producing osteotomy as surgical indication, English language, and clearly reported outcomes. Ultimately, a total of 16 studies published from 2005 to 2020 dealing with distal femur osteotomy and its femoropatellar implications were included in the present review.
Surgical indications
The studies included in this review had very heterogeneous objectives to evaluate the efficacy of femoral osteotomy. Seven studies14–18 were conducted to evaluate the efficacy of femoral osteotomy on patellar tracking and clinical improvement in patellar instability.
Four studies were carried out to evaluate the clinical efficacy of the treatment: two of these studies18,19 were carried out in young patients on non-arthritic knees, one study 15 was carried out to evaluate clinical efficacy and pain relief in arthritic knees, one study 13 instead considered a more heterogeneous cohort of patients. The aim of two studies20,21 was to evaluate patellofemoral symptoms and the implication of femoropatellar osteoarthritis following DFO. One study 21 performed an analysis of changes in patella height following DFO, while another retrospectively evaluated postoperative axis changes without correlating to clinical outcomes. The correlation between osteotomy correction angle and its influence on Q-angle was instead investigated in another study. 22 Details of the inclusion and exclusion criteria are described in Table 1.
The details about the inclusion and exclusion criteria of the studies in the present review.
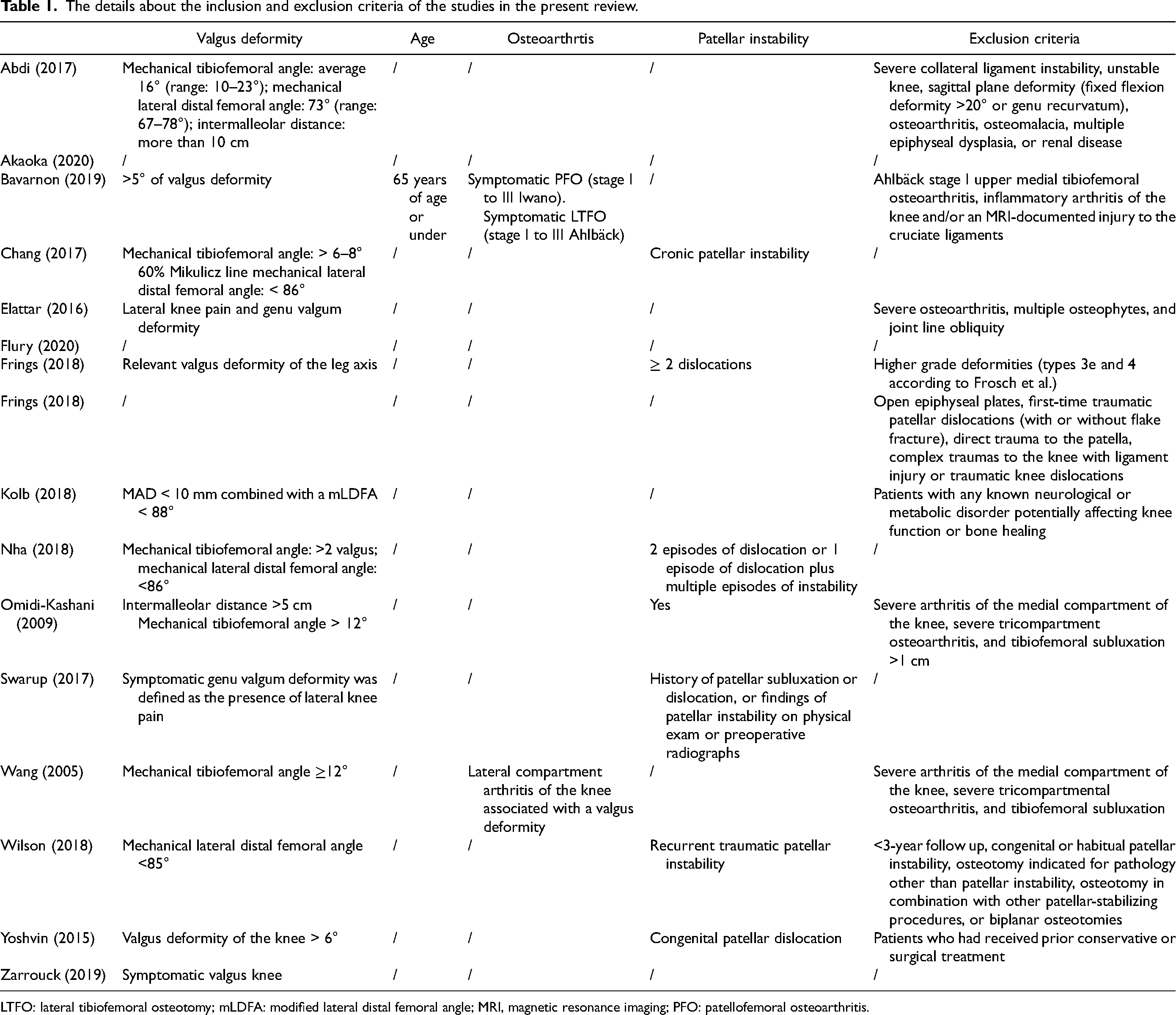
LTFO: lateral tibiofemoral osteotomy; mLDFA: modified lateral distal femoral angle; MRI, magnetic resonance imaging; PFO: patellofemoral osteoarthritis.
Surgical techniques
Concerning the surgical technique, the studies have reported different methods.
Seven studies14–18 reported a medial closing wedge as surgical technique associated or not with a medial reefing and a lateral release.
Five studies1,9,10,13,15 described a lateral opening wedge as a method to restore the desired axis. Also, in this case a lateral release was described in cases where this procedure was deemed necessary. One study 22 described a single-cut distal femoral osteotomy that enables concurrent correction of angulation and translation. Another study 3 used three-dimensional models obtained using patient computed tomography data and subsequently biplanar supracondylar osteotomies were simulated with different degrees of varus correction (from 1° to 15°) in one-degree steps beginning from the preoperative valgus deformity, resulting in a total of 150 simulations in order to evaluate the association between Q-angle and femoral osteotomy. Details concerning the surgical techniques are described in Table 2.
The different techniques employed.
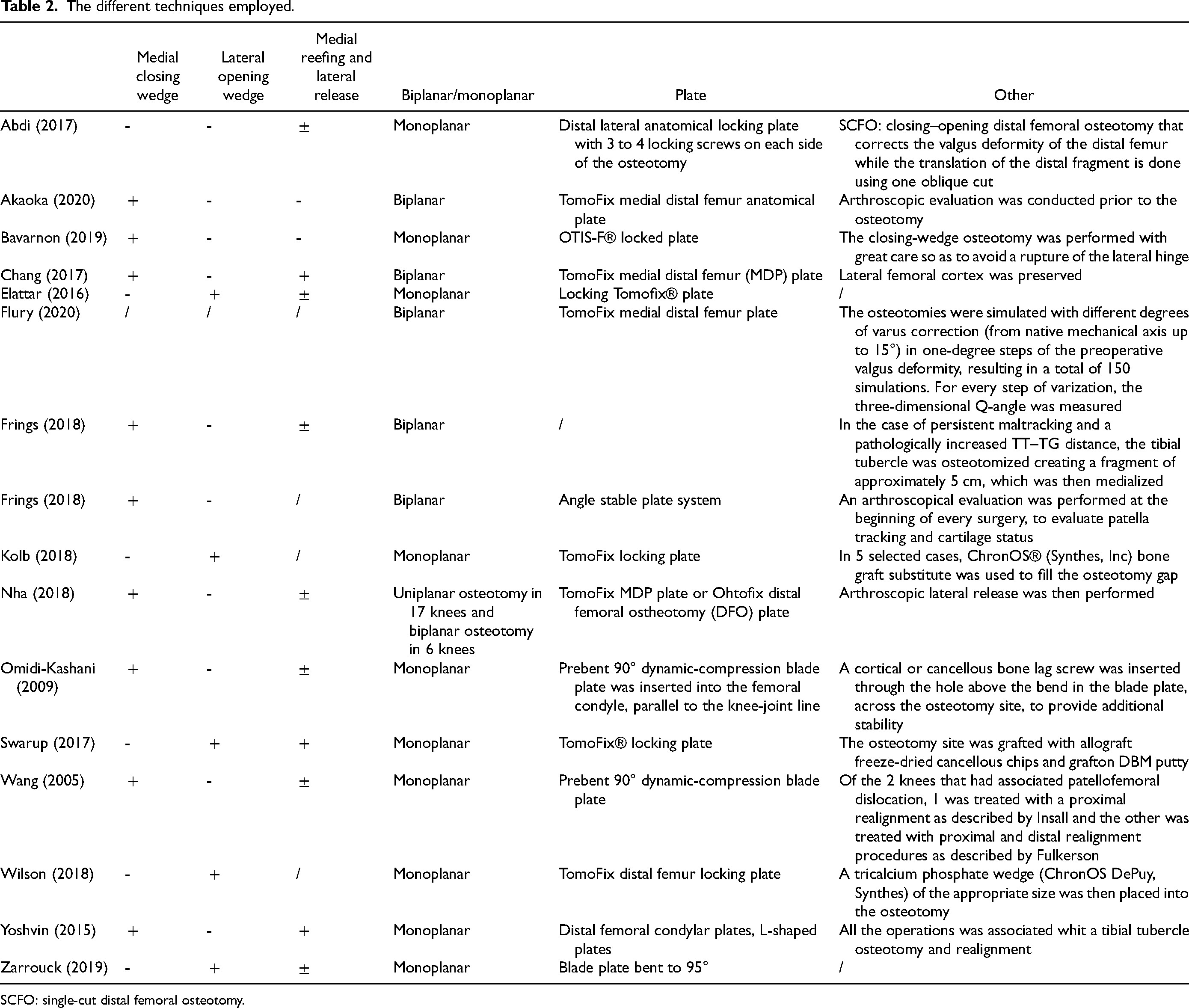
SCFO: single-cut distal femoral osteotomy.
The main results and conclusions of the included studies.
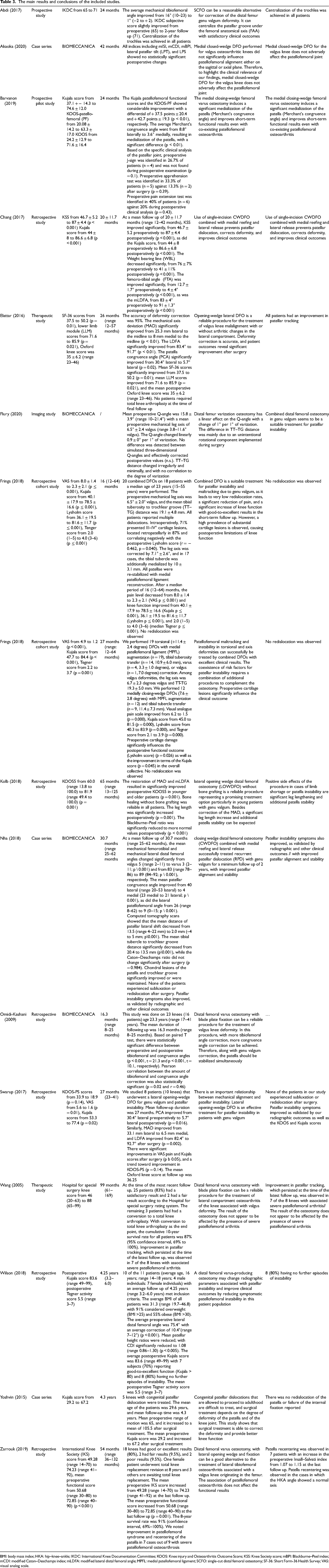
BMI: body mass index; HKA: hip–knee–ankle; IKDC: International Knee Documentation Committee; KOOS: Knee injury and Osteoarthritis Outcome Score; KSS: Knee Society score; mBPI: Blackburne–Peel index; mCDI: modified Caton–Deschamps index; mLDFA: modified lateral distal femoral angle; MPFL: medial patellofemoral ligament; SCFO: single-cut distal femoral osteotomy; SF-36: Short Form-36 Health Survey; VAS: visual analog scale.
Results
Patients demographics
Sixteen studies involving a total of 235 patients and 276 knees who performed a femoral distal osteotomy for valgus deformity of the lower limb have been included in this review. All 16 studies are case series with level of evidence of IV. Concerning the patients’ demographic of the latter studies, of the 227 patients 146 were females and 81 males, the mean age was 37.5 (range: 21–63.5) and the mean body mass index 27.6. Patients were followed up for a mean of 37.9 months after surgery (range: 16–99).
Radiological outcomes
Of the 16 trials, 4 studies1,3,13,18 analyzed only radiological outcomes, the others also considered functional outcomes. The radiological outcomes taken into consideration were both related to alignment of the entire lower limb as the hip–knee–ankle angle (HKA), the lateral distal femoral angle (LDFA), femoral shortening (FS), and to the patellar alignment as the modified Insall–Salvati index (mSI), modified Caton–Deschamps index (CDI), and modified Blackburne–Peel index (BPI). Ten studies investigated the HKA, described in Figure 1, reporting an average preoperative value of 12.02° of deviation from the mechanical axis, and a mean postoperative value of 0.22°, hence an improvement of 11.80° in the HKA axis. Ten studies reported the LDFA, describing an average preoperative value of 83.4°, and a mean postoperative value of 88.3°, hence an improvement of 4.9° in the LDFA. Five studies investigated the FS, reporting an average postoperative value of 4.3 mm of FS. Concerning the patellar radiological outcomes, three studies reported the mSI (Figure 2), describing an average preoperative value of 1.11°, and a mean postoperative value of 1.13°, hence a change of 0.02° in the mSI. Three studies reported the CDI, describing an average preoperative value of 1.02°, and a mean postoperative value of 0.87°, hence a change of 0.15° in the CDI. Three studies reported the BPI, describing an average preoperative value of 0.89°, and a mean postoperative value of 0.8°, hence a change of 0.09° in the BPI.
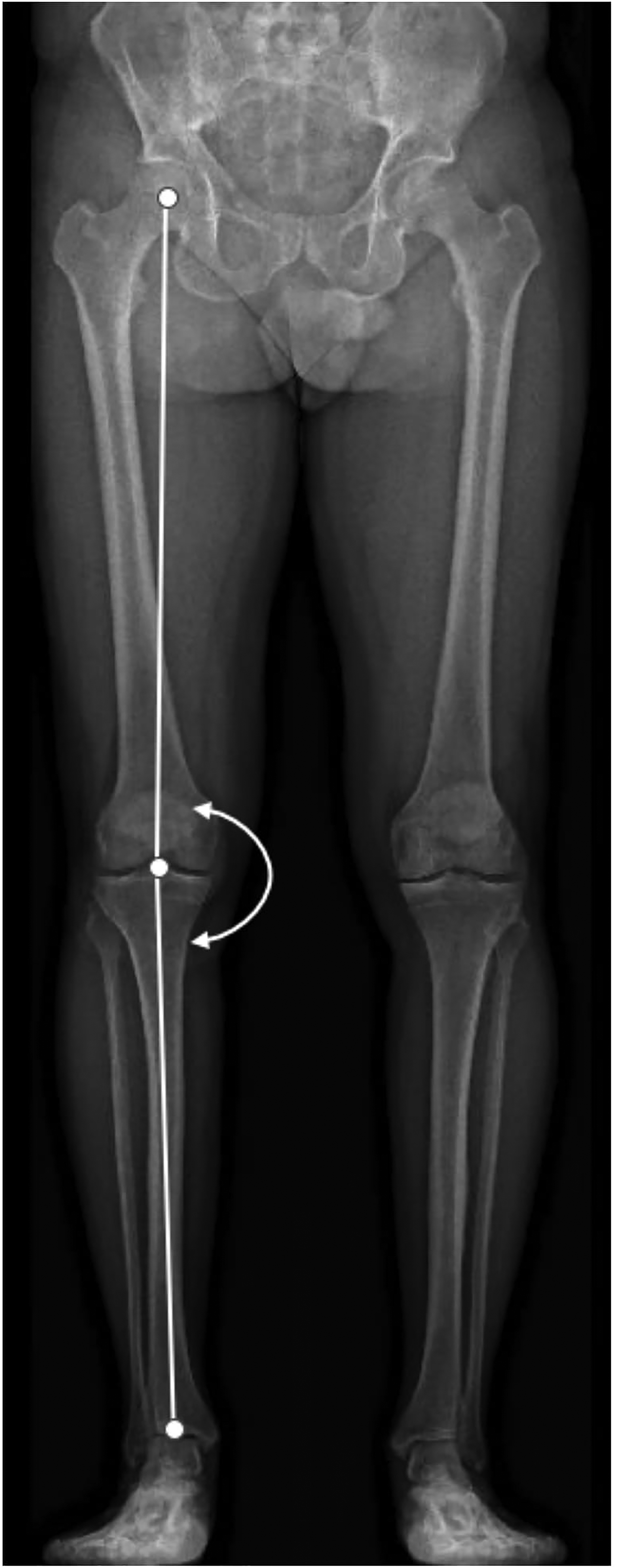
Describes how to measure the hip–knee–ankle (HKA) angle. Is the angle formed by two axes (white lines). The first axis runs from the center of the femoral head to the middle of the femoral notch, and the second axis from the middle of the tibial notch to the middle of the talar head of the tibia.
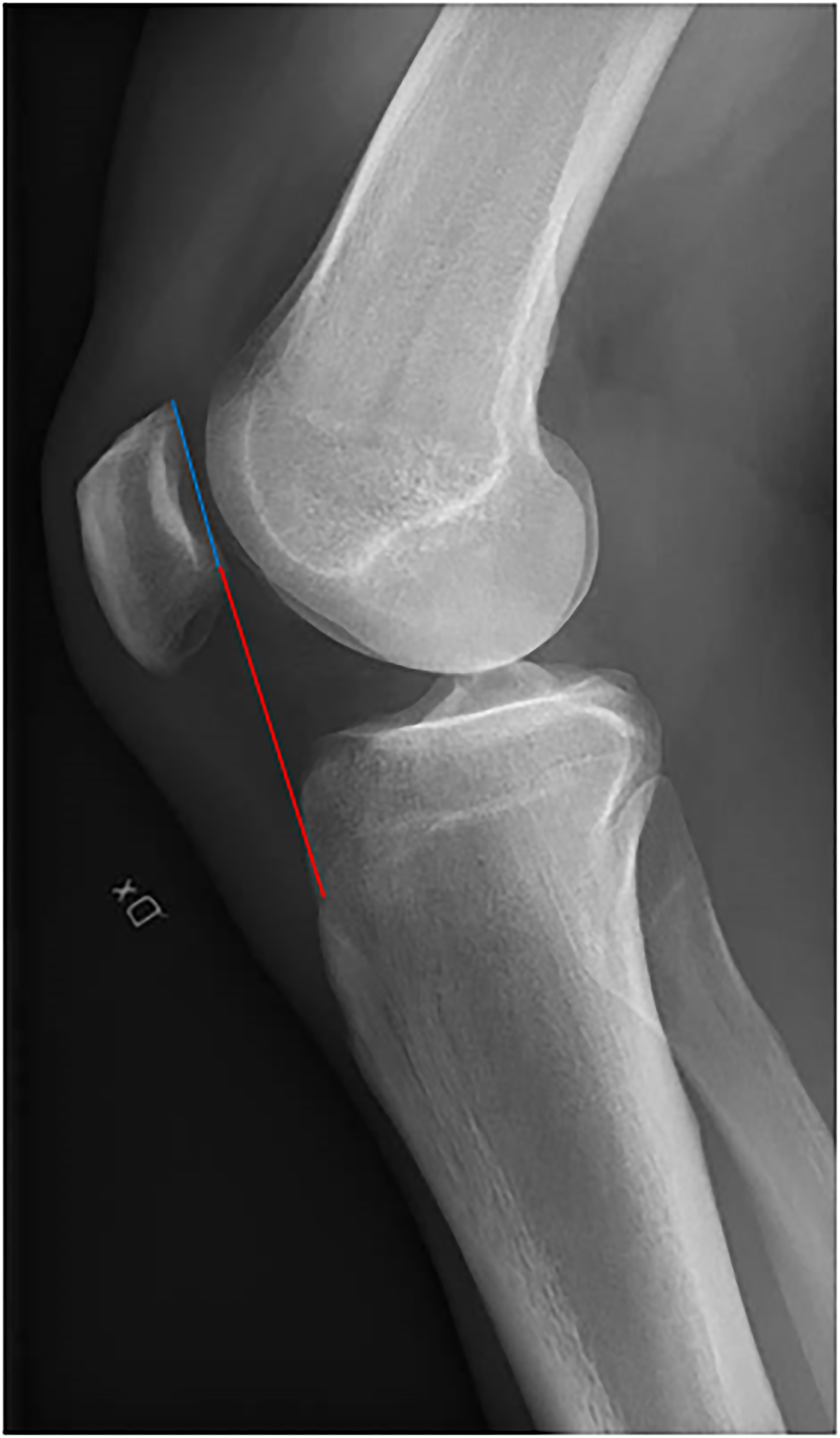
The modified Insall–Salvati ratio (mSI).
Clinical outcomes
Knee function was evaluated using the following items: the Kujala score and the Knee injury and Osteoarthritis Outcome Score (KOOS). Indeed, 5 studies investigated the Kujala score, describing an average preoperative value of 47.08, and a mean postoperative value of 82.84, hence a change of 35.76 in the Kujala score. Four studies reported the KOOS, describing an average preoperative value of 58.17, and a mean postoperative value of 86.4°, hence a change of 28.23 in the KOOS. Of the 16 trials, 4 studies131813 analyzed only radiological outcomes, the others also considered functional outcomes. The details of the study design and patient population of all the studies are reported in Table 1. Knee pain was evaluated using visual analog scale (VAS). Knee function was evaluated using the following items: KOOS, Tegner activity scale, Lysholm knee function score, Oxford knee score, Short Form-36 Health Survey, the International Knee Documentation Committee (IKDC), Kujala score, the Knee Society score, American Academy of Orthopedic Surgeons LLM, Hospital for special surgery knee score. The radiological outcomes taken into consideration were both related to alignment of the entire lower limb as the HKA, LDFA, medial proximal tibial angle (MPTA), tibial posterior slope (TPS), but also related to the patellar alignment as the mSI, CDI, and BPI. Only 3 studies4,15,23 reported clinical data concerning pain on the VAS and a decrease from a mean preoperative value of 4.7 to 2.1 was observed. Kujala score was reported by 7 studies4,14,15,16,17,19,23 reporting an average increase of 35.8 points from a preoperative mean value of 47.1 to 82.8 postoperatively. Only the study by Abdi et al. 20 uses the IKDC and reports an improvement of 6 points from 65 to 71. KOOS was used by three authors10,15,29 with a mean improvement of 16.7 points, from 60 to 76.5. Regarding patellar outcomes, the literature is not homogeneous in its evaluation and therefore this review is limited to a descriptive analysis of the various outcomes. Akaoka et al. 1 reported that medial closed-wedge DFO for the valgus knee does not adversely affect the patellofemoral joint. Few studies17,19,20 shows that distal femoral varus osteotomy is a valid treatment to obtain a centralization of the trochlea and a medialization of the patella. Several studies10,18,19,21 reported the postoperative clinical outcomes of the knee without, however, specifying the recurrence rate of patellar dislocation, highlighting an improvement in the clinical parameters taken into consideration. Other studies have analyzed the recurrence rate of postoperative patellar dislocation: Frings et al., 4 Swarup et al., 15 and Yoshvin et al.17 did not observe redislocation of patella after surgery while Wilson et al. 16 reported that 80% of the treated patients have no further episode of instability.
Discussion
This study shows that distal femoral osteotomy can be used as a reliable tool in addressing patellofemoral instability in the setting of genu valgum, as it can be demonstrated by an improvement in clinical outcome scores as well as in patellar tracking and in patellofemoral symptoms (Table 3). Also, a reduction in recurrence of dislocation and in pain scores was noted in most of the studies. While historically distal femur varus-producing osteotomy (DFVO) was intended essentially to treat early-stage lateral compartment osteoarthritis, better knowledge of patellofemoral kinematics in recent years led to the expansion of the indications for DFVO and to the extension of its use for the treatment of patellar instability under the assumption that a reduction in the Q-angle could reduce the lateral translational vector applied to the patella. However, the literature on the subject remains scarce and consists mostly of small case series. Thus, with this study, we aimed to recollect the evidence from these studies in order to review and evaluate the clinical implications of DFVO for the patellofemoral joint. With the present review, we could demonstrate that DFVO allows to obtain a reliable correction of femoral valgus which in turn improved patellofemoral tracking and stability. Clinically, this translated into improved functional scores (Kujala score and KOOS), diminished pain (VAS) and reduction of instability (mSI and CDI). Remarkably, an improvement was observed for both medial closing-wedge and lateral opening-wedge osteotomies. As a sidenote, as femoral opening-wedge osteotomy is known to normalize the patellar height while correcting the genu valgum of the patient, 24 it should be observed that patients with patella alta, which is a known risk factor for patellofemoral instability, would most likely benefit from an opening-wedge osteotomy. Similarly, closing-wedge osteotomy would be most indicated in patients with a low to normal patellar height in order to prevent the inadvertent occurrence of patella baja that could occur with an opening osteotomy. Among the 16 included studies, an average mechanical axis correction of 11.8° was noted, with 7 studies reporting undercorrection (range from 4° to 0.2°) and 3 studies reporting overcorrection (range from −0.6 to −3). Interestingly, the clinical and radiological outcomes did not differ when overcorrection was performed. Moreover, in one study the Merchant congruence angle was adequately restored and patella was medialized with a significant improvement of short-term functional results even with co-existing patellofemoral osteoarthritis. In another study, centralization on the trochlea was achieved in all patients. 24 In the study by Elattar et al. 21 all patients showed an improvement in patellar tracking. In the studies by Frings et al.4,23 no recurrence of dislocation was observed after femoral osteotomy.
It is also relevant to note that while the patient population of the analyzed studies was highly heterogenous, with varying degrees of preoperative deformity and patellofemoral instability, DFVO seemed to be effective regardless of preoperative patient status. Even if the clinical and radiological results of the procedure looks promising, it should be noted that other additional procedures were concomitantly performed in several studied, including medial reefing or lateral release. This review, while being one of the only reviews performed on this subject, has some limitations: first, preoperative patient characteristics are extremely variable, making the drawing of generalized conclusion more hazardous despite the encouraging results hereby displayed. Second, in many of the considered studied DFVO was associated with other procedures including medial reefing or lateral release, making it difficult to adequately analyze the relative contributions of each of these procedures to the final clinical outcome. Third, as the use of DFVO to address patellofemoral instability is not widespread, the actual sample size analyzed is relatively small. Also, as most of the studies considered are probably lacking adequate power, and the level of evidence of the current review is thus probably limited.
Conclusions
According to the encouraging results showing a reduction in patellar redislocation rate and an improvement in postoperative outcome scores, DFVO should be considered as a promising alternative to more classical procedures in the treatment of patellofemoral instability in the setting of genu valgum, and should be taken into account as one of the surgical options to address the issue of altered patellofemoral kinematics.
In the next few years, more studies should investigate the clinical and radiological outcomes distal femoral varus osteotomy with a longer follow up in order to better understand the long-term consequences of this surgery.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
