Abstract
Study Design
Prospective cohort study.
Objectives
In this study we aim to assess the difference in triggered EMG readings throughout different depths in the psoas muscle during the lateral approach to the lumbar spine and their effect on surgeon decision making.
Methods
Three surgeons, practicing at different institutions, assessed triggered EMG readings during the trans psoas approach at the level of the disc and 5,10 and 15 millimeters into the psoas muscle with sequential dilators. Measurement of distance into the psoas muscle was done with a specially designed instrument. Results of anterior and posterior directed stimulation as well as the delta value between these were recorded and underwent statistical analysis. Patients who had partial readings were excluded from the study.
Results
A total of 40 levels in 35 patients were included in the study. There was no significant difference found between means of anterior or posterior threshold readings along the different distance groups. A significant difference was found (P = .024) in the mean difference between the distance groups with a decrease in the difference between anterior and posterior threshold values found as the distance from the disc space increased. None of the surgeons reported a decision to abort the fusion of a spinal level.
Conclusions
In the trans-psoas approach to the lumbar spine, the assessment of the location of the femoral nerve using directional neuromonitoring when advancing in the psoas muscle shows no clear benefit as opposed to stimulating solely when adjacent to the disc space.
Introduction
Since its introduction in 2006, the lateral trans-psoas approach for lumbar fusion has been adopted by many surgeons due to its effectiveness in indirect decompression, deformity correction and facilitation of fusion.1–4 In this technique, a minimally invasive, trans-psoas approach is utilized to instrument the lumbar spine intervertebral discs. Due to concerns of injury to the lumbar plexus, and the resulting neurologic deficits, it is necessary to identify a neurologically safe corridor during the approach to the disc space through the psoas muscle. Identifying the neurologically safe corridor may be challenging due to the anatomical variation of the lumbar plexus between individual patients.5,6 Neuromonitoring with directional triggered electromyography (EMG) has become an essential tool for localization of the lumbar plexus during the trans-psoas approach to the lumbar spine. To accomplish this, a specially designed dilator allows the surgeon to stimulate the lumbar plexus in discreet directions following docking on the surface of the disc to determine the threshold necessary to cause EMG activity in the appropriate muscle group. A difference in excitation thresholds following stimulation in different directions can approximate the location of major motor branches within the plexus with relation to the dilator and assists the surgeon in the assessment of the safety of the surgical corridor. Due to the variable course of the lumbar plexus within the psoas, it is unknown whether it is necessary to stimulate at several depths within the psoas relative to the surface of the disc during dilation to establish the safe working corridor.7,8 Stimulation at multiple depths within the psoas can be time consuming and potentially provide misleading data due to different EMG threshold values at various depths. To address this important clinical question, in this study, we assessed the triggered EMG thresholds at different depths within the psoas muscle and the effect of this additional data on surgical decision making. We Hypothesize that stimulating at multiple depths does not produce significantly different information with regards to the proximity to the lumbar plexus and therefore will have no effect on intraoperative surgical decision making.
Methods
Three surgeons, practicing at different institutions, assessed triggered EMG thresholds during the direct lateral trans psoas approach to L3-4 and L4-5. The side of the approach was chosen at the surgeon’s discretion based on the patient’s pathology and anatomical features. Thresholds were assessed with sequential dilators at the level of the disc (0 mm) and at a distance of 5, 10 and 15 mm from the surface of the disc space into the psoas muscle. Measurement of distance from the disc space was done with a specially designed device (Figure 1). The minimum threshold for muscle EMG response at each depth was determined using the SafeOp system (ATEC, Carlsbad, CA) and using standard three-stage sequential dilators. Results of anterior and posterior directed stimulation at each depth using the secondary dilator were recorded. Individual disc levels without complete data sets were excluded from the study. Differences in measurements with regards to the laterality of the surgical approach were not assessed. Patients were followed up by their attending surgeon per protocol at the specific institution where they underwent their procedure. This study was exempt from institutional review board approval and informed consent due to the nature of the study. Custom designed dilator-disc distance measuring device.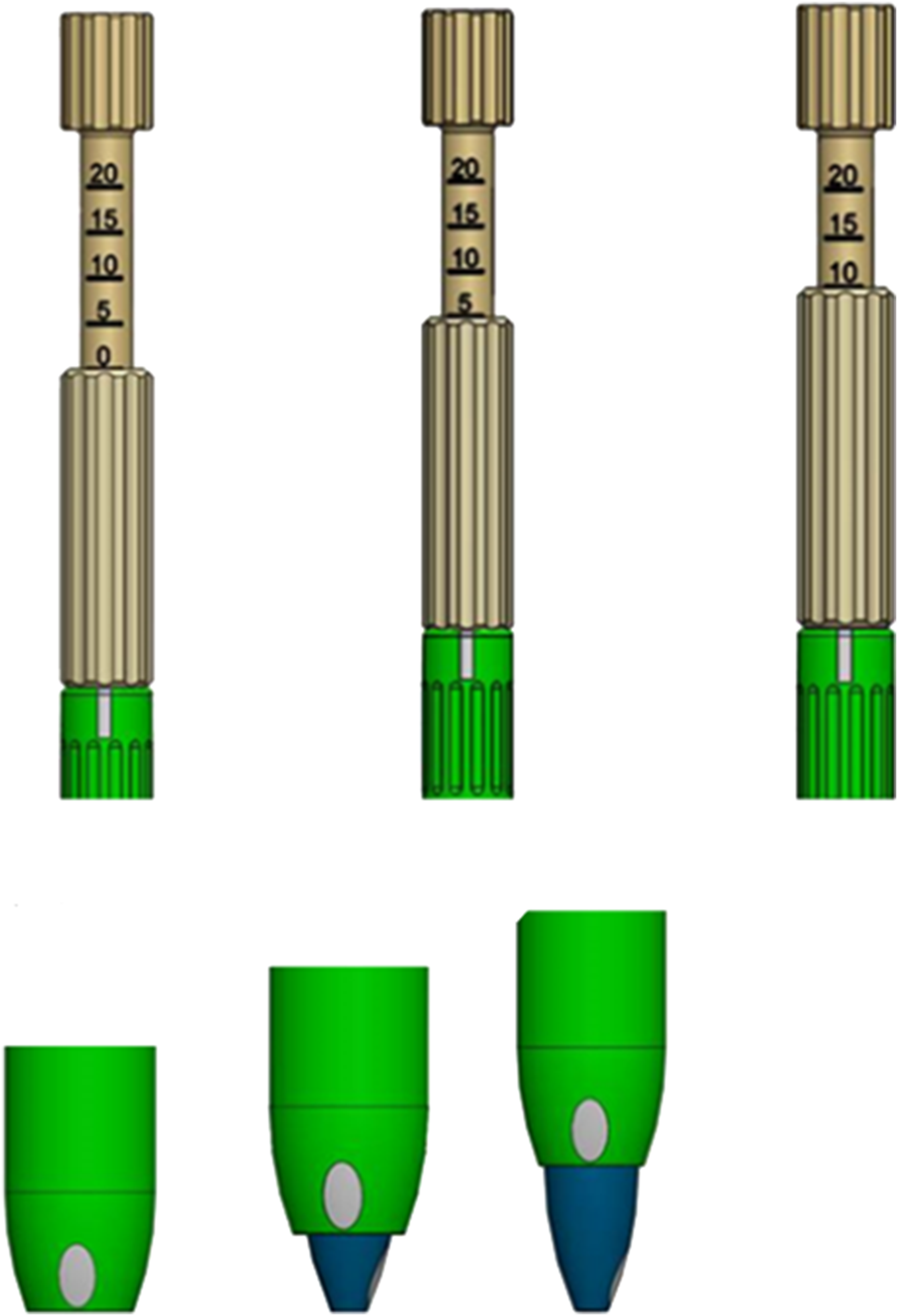
The statistical analysis was conducted to compare threshold levels across the 4 distance groups for each of anterior and posterior directions, as well as the differences between anterior and posterior measurements. We used one-way analysis of variance (ANOVA) to compare threshold levels across the 4 distance groups. When the assumptions of ANOVA were not satisfied, we used non-parametric Kruskal-Wallis rank sum test to perform the comparisons. To quantitively examine the relationships between distances and threshold levels, we used linear regression analysis to calculate differences and 95% confidence intervals (95% CI) in threshold levels for each distance group using the 0 mm group as the reference group. All statistical tests were 2-sided and were conducted using the R software.
Results
Means ± SDs of Thresholds by Different Distances (n = 40).
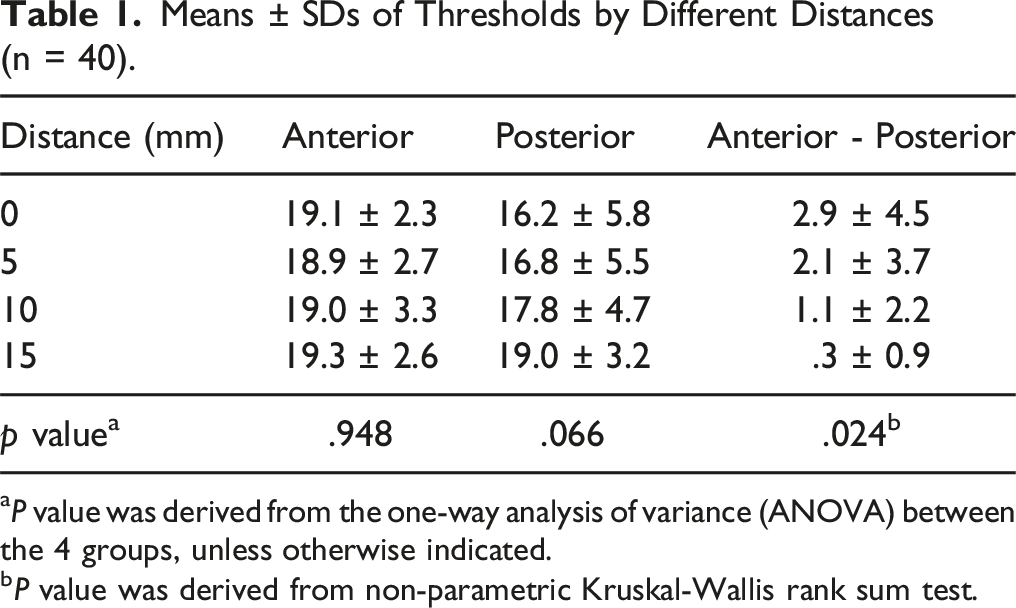
aP value was derived from the one-way analysis of variance (ANOVA) between the 4 groups, unless otherwise indicated.
bP value was derived from non-parametric Kruskal-Wallis rank sum test.
Differences (95% CIs) in Threshold Values for the Groups of 5 mm, 10 mm, and 15 mm Compared With the Group of 0 mm (n = 40).
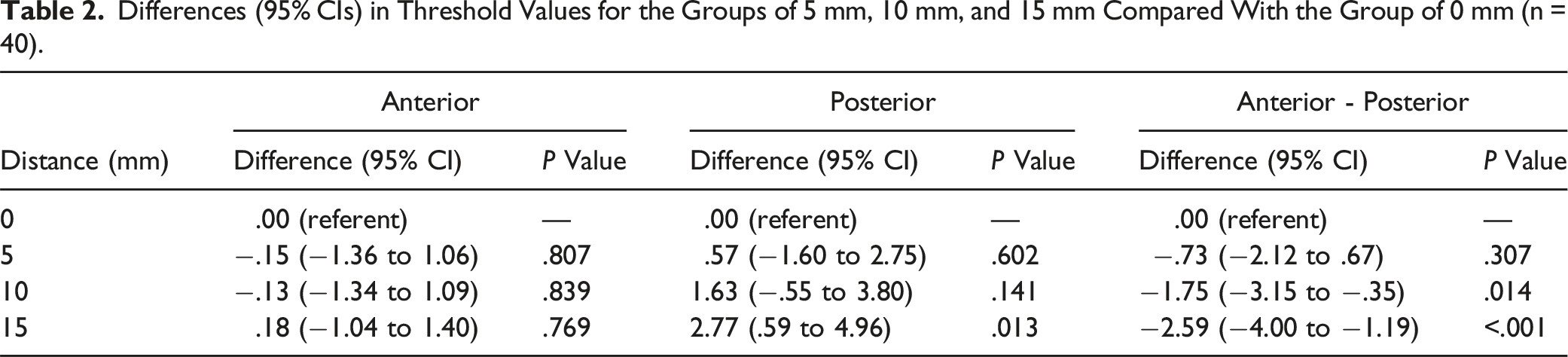
Differences (95% CIs) in Threshold Values for the Groups of 5 mm, 10 mm, and 15 mm Compared With the Group of 0 mm, Stratified by Disc Space Levels.
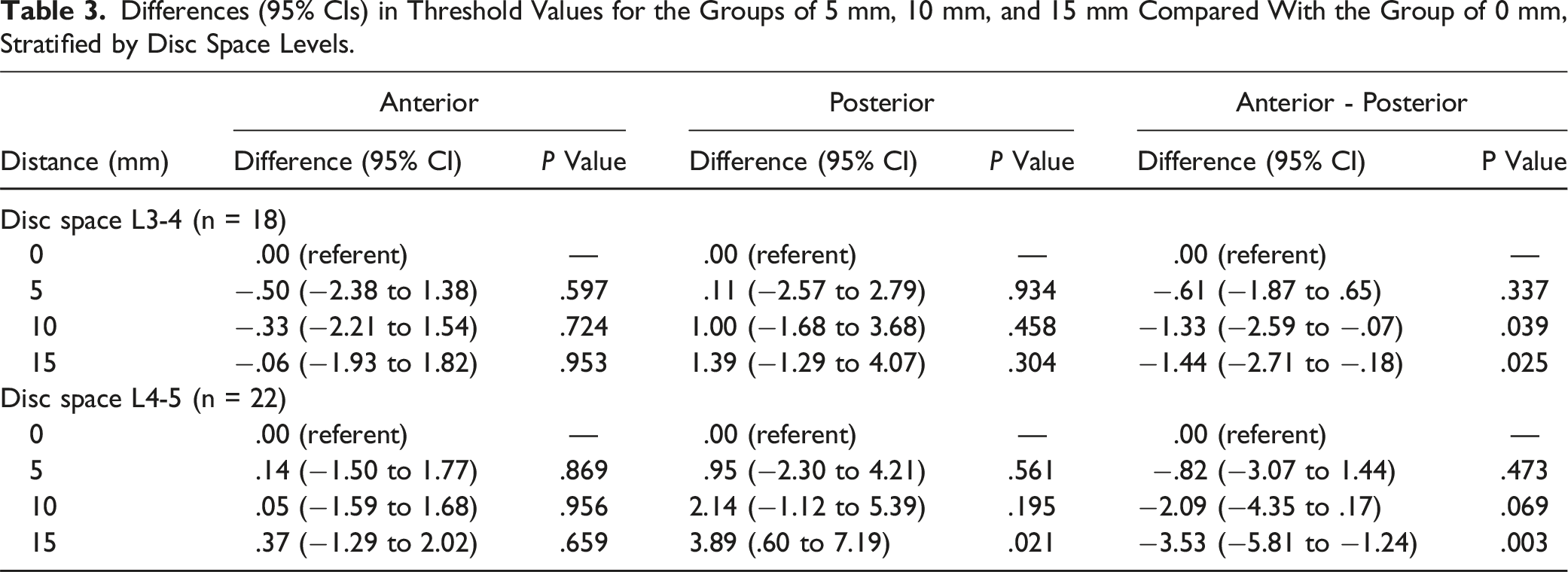
Discussion
Injury to the lumbar plexus is an important concern during the trans-psoas approach to the lumbar spine with studies demonstrating rates of 8%–46% for post-operative sensory deficits and up to 7% for motor deficits. 9 These complications are thought to come about from the retraction of the lumbar plexus as well as from direct trauma to nerves during dissection through the psoas muscle.10–12 Although the majority of neurological deficits are transient in nature, additional methods of establishing a safe lateral corridor to the lumbar spine have been explored in an effort to reduce the rate of lumbar plexus injury. The oblique, anterior to psoas, approach, for example, has shown similar radiographic and functional outcomes as the trans-psoas approach with less injury to the lumbar plexus, however there is greater risk of vascular complications as well as sympathetic chain injuries13-15 which deter many. “Shallow docking” is an alternative method for creating a trans-psoas corridor where the retractor is initially docked on the surface of the psoas muscle rather than on the disc space followed by sequential dilation. The psoas and lumbar plexus are then dissected under direct visualization until the surface of the disc space is reached. Although this could theoretically minimize injury to the lumbar plexus as well as the psoas itself, studies have shown no significant decrease in neurologic complications using this method.16,17 Sequential dilation of the psoas muscle with utilization of directional triggered EMG remains the mainstay of the direct lateral approach. The notion that sequentially stimulating at different depths within the psoas could provide a better approximation of the lumbar plexus and possibly impact intra-operative surgical decision making has been scarcely studied. In a porcine model, Sarwahi et al 8 gradually stimulated in 2 mm intervals from adjacent to the nerve until a distance of 10 mm. They found that the threshold for stimulus increased when further from the nerve, but this was not significantly proportional to the distance, suggesting limitations for nerve mapping. In a multicenter study of 102 patients undergoing direct lateral fusion at L3-4 and L4-5, Tohmeh et al 7 evaluated nerve stimulation thresholds on the psoas surface, mid psoas and on the surface of the spine using 3 sequential dilators with stimulation directed anteriorly, posteriorly, superiorly and inferiorly. They report that on average, triggered EMG thresholds at L4-5 decreased from the psoas surface to mid-psoas then slightly increased as they approached the disc space. This could suggest that at the L4-5 level the nerves are closer in proximity to the dilator when mid-psoas than when on the surface of the spine. At L3-4 they describe a different threshold trend with values steadily decreasing as the dilator descended within the muscle with lowest overall thresholds found when stimulating posteriorly. However, they did not report the significance of these findings. Our findings further aid in the understanding of triggered EMG neuromonitoring when traversing the psoas muscle. We found a nonsignificant trend of decreasing posterior threshold values when approaching the spine, although a similar trend was not identified with threshold values found when stimulating anteriorly. Our significant finding of a difference in the mean delta value at the various psoas depths could suggest the distance between the dilator and the nerve decreases as we move from 15 mm off of the disc towards the disc space. This being said, a delta of stimulation thresholds within the substance of the psoas, as opposed to on the disc space, is not unidirectional due to the 3 dimensional shape of the psoas and therefore not helpful in understanding the relative location of the nerve. Although our data demonstrates that stimulation at multiple depths within the psoas is not useful for neural mapping when establishing a safe corridor to the disc space, our findings corroborate with those of Tomeh et al in that the nerve could be different distances from the dilator as it progresses throughout the psoas. This could lead some to believe that even when favorable directional EMG thresholds are found, post-operative neurologic deficits are still possible due to retraction of an undetected nerve during the procedure. Although this cannot be avoided by sequential stimulation when traversing the psoas, this thesis suggests that there is utility of concomitant use of additional neuromonitoring techniques that could monitor nerve integrity during retraction such as somatosensory evoked potentials (SSEP) and motor evoked potentials (MEP) which have been shown to increase rates of intraoperative detection of neural insult.18-20
This study is not without limitations. Our choice of distances from the disc space to be tested is arbitrary. In a heterogenous patient population, the absolute distance of the lumbar plexus from the disc space could relate to the relative size and shape of the psoas arguing that a relative measurement could be more appropriate. This however was not feasible when designing the study protocol, and unlikely to have real-world clinical utility due to the difficulty in applying such a measurement system. From a clinical standpoint, although no postoperative motor deficits were recorded, additional clinical follow-up of patient outcomes including sensory deficits and hip pain related symptoms may have provided additional context to our findings.
In conclusion, when utilizing directional triggered EMG to localize the lumbar plexus during the trans-psoas approach to the lumbar spine, there is no clear benefit to stimulating at multiple depths within the psoas as compared to stimulating on the surface of the disc space alone. Adjunct neuromonitoring techniques such as SSEP and MEP should be further studied to determine their utility in avoiding neurologic complications in trans-psoas lumbar fusion procedures.
Footnotes
Author Contributions
I.M. ATEC- Consultant, Royalties. Biedermann Motech- Consultant. Orthozon- shareholder, Spinal Simplicity- Shareholder, Spinewave- Consultant, Stryker spine- Consultant. R.O. ATEC- Consultant, teaching and royalties. Providence Medical technologies-consultant, teaching. J.O. Nuvasive, Cerapedics- Consultant. G.B. No disclosures. W.Q. No disclosures.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
