Abstract
Study Design
Retrospective database study.
Objectives
The goal of this study was to assess the influence of weekend admission on patients undergoing elective thoracolumbar spinal fusion by investigating hospital readmission outcomes and analyzing differences in demographics, comorbidities, and postoperative factors.
Methods
The 2016-2018 Nationwide Readmission Database was used to identify adult patients who underwent elective thoracolumbar spinal fusion. The sample was divided into weekday and weekend admission patients. Demographics, comorbidities, complications, and discharge status data were compiled. The primary outcomes were 30-day and 90-day readmission. Univariate logistic regression analyzed the relationship between weekday or weekend admission and 30- or 90-day readmission, and multivariate regression determined the impact of covariates.
Results
177,847 patients were identified in total, with 176,842 in the weekday cohort and 1005 in the weekend cohort. Multivariate regression analysis found that 30-day readmissions were significantly greater for the weekend cohort after adjusting for sex, age, Medicare or Medicaid status, and comorbidity status (OR 2.00, 95% CI: 1.60-2.48; P < .001), and 90-day readmissions were also greater for the weekend cohort after adjustment (OR 2.01, 95% CI: 1.68-2.40, P < .001).
Conclusions
Patients undergoing elective thoracolumbar spinal fusion surgery who are initially admitted on weekends are more likely to experience hospital readmission. These patients have increased incidence of deep vein thrombosis, postoperative infection, and non-routine discharge status. These factors are potential areas of focus for reducing the impact of the “weekend effect” and improving outcomes for elective thoracolumbar spinal fusion.
Introduction
Globally, there is increasing incidence of age-related spinal degeneration and a growing need for the elective thoracolumbar spinal fusions used to treat these degenerative conditions.1,2 The number of patients undergoing anterior lumbar interbody fusion (ALIF) and posterior lumbar fusion (PLF), 2 common lumbar fusion techniques, is estimated to rise by 12.9% and 16.7% by the year 2040, respectively, surpassing the predicted growth rate for the U.S. population overall. 3 Thus, analyzing the risk factors associated with worse outcomes for thoracolumbar spinal fusion procedures, especially as they are more frequently utilized, is critical in improving the patient experience.
Many previous studies have investigated the impact of weekend admissions on clinical outcomes. One study confirmed the presence of a “weekend effect” causing increased mortality rates in a meta-analysis of hospital patients admitted on weekends, even after adjusting for potentially confounding differences in staffing, procedure rates and delays, and illness severity. 4 However, such an effect as it pertains to spine surgery, and moreso, thoracolumbar spine surgery, is not well represented in the literature. Previous literature regarding the weekend effect in spine surgery provides insight into the association between weekend admission and hospital acquired conditions (HAC) and length of stay (LOS).5-7 However, results vary and these papers do not consider readmission and several comorbidities and complications. Therefore, further analysis of the “weekend effect” in thoracolumbar spinal fusion patients is needed to confirm its impact on patient outcomes and facilitate identification of risk factors for this patient population.
Hospital readmission rates are a particularly useful outcome measure because readmission directly results in added costs for hospitals and presents an unfavorable experience for patients. 8 More specifically, for elective revision lumbar fusions in 2014, readmissions within 90 days resulted in an average cost increase of $96,152 per patient. 9 The importance of readmission rates is further justified by the fact that the Centers for Medicare and Medicaid Services uses hospital readmissions as a quality-based reimbursement metric and a measure of hospital performance. 10
Thus, the objectives of this study are to analyze the “weekend effect” by (1) comparing 30- and 90-day hospital readmission rates of weekday and weekend admission patients undergoing elective thoracolumbar spinal fusions and (2) identifying disparities in demographic characteristics, comorbidities, postoperative complications, and discharge status between the weekday and weekend admission cohorts.
Methods
We queried the 2016-2018 versions of the Nationwide Readmissions Database (NRD), which contains data on millions of hospital discharges in the U.S. every year. Institutional review board exemption was obtained from our institution for this retrospective analysis. The 2016-2018 datasets use the International Classification of Diseases, Ninth Revision (ICD-9) and International Classification of Diseases, Tenth Revision (ICD-10) diagnosis and procedural codes to identify specific medical conditions and surgical procedures. The NRD contains data from 30 state inpatient databases (SID). Sampling discharge weights are provided by the Healthcare Cost and Utilization Project (HCUP) to allow for national estimates from the NRD. The NRD discharge data includes patient demographics, hospital characteristics, payer status, total hospital charges to patient, readmission information, and patient diagnoses and procedures.
All adult patients (>18 years of age) who underwent elective thoracolumbar spine fusion surgery were identified using ICD-9 procedure codes and ICD-10 procedure codes (see Supplementary Table 1). Patients who underwent non-elective procedures were excluded. Patients were then separated into 2 sub-groups based on whether or not their index admission was on a weekday vs weekend; the NRD uses the binary variable “AWEEKEND” to identify whether an admission is on a weekend (=1) vs weekday (=0). Patient characteristics were obtained from the NRD database including demographic information (sex, age, payer type), diagnoses, postoperative complications, and discharge status. Postoperative complications were obtained by reviewing diagnosis codes associated with the initial hospitalization and selecting those representative of surgical complications. Diagnoses at readmission were determined by tabulating the diagnosis codes associated with 30-day and 90-day readmission events. The total charge for each patient represents the cost of the first hospital admission and is reported by the NRD in dollar amount; we then adjusted each charge for inflation using the consumer price index. Length of stay represented the length of the first hospital admission in days; this was obtained from the NRD using the variable “LOS”. Preoperative comorbidities were identified using ICD-9 and ICD-10 diagnosis codes and the R Comorbidity package. 11 This package allows for the calculation of Elixhauser comorbidity scores as well as incidence of specific comorbidities among the patient population.
Statistical Analyses
The NRD allows for the longitudinal tracking of patients and their care as they are readmitted throughout a specific year via patient-specific identifiers within the database. However, the data is specific to year and state, so if a patient is readmitted to a different facility in a different state or if their readmission occurs after the calendar year ends, the readmission is unaccounted for and could be coded as an initial admission. In order to capture 90- day readmissions, patients discharged during the last quarter of the calendar year were excluded using the variable identifying the month associated with the discharge, “DMONTH”. We were then able to quantify the incidence of 30- and 90- day readmissions for both the weekend-admit and weekday-admit subgroups using the relative date variable, “NRD_DaysToEvent”, to calculate readmission windows since the NRD does not specify exact dates to protect patient privacy.
SciPy version 1.6.1 was used for all statistical analyses conducted. SciPy is an open-source Python library that provides functions for scientific analysis and computation. 12 Univariate regression analyses and chi-squared tests were performed to compare the weekday admission and weekend admission cohorts, analyzing for differences in demographic information, comorbidities, postoperative complications, and discharge status. Univariate regression was also performed to analyze differences in mean total charges and mean length of stay between the cohorts. Multivariate logistic regression was performed to analyze the association between weekend admission and both 30- and 90-day readmission, adjusted for demographic data (sex, age, and Medicaid or Medicare status) and Elixhauser comorbidity scores. A significance level of .05 was used.
Results
General Patient Data
A total of 177,847 patients undergoing elective thoracolumbar spine fusion surgery were identified, with 176,842 in the weekday cohort and 1005 in the weekend cohort. The cohorts were well-matched in age (P = .18) and payer type (P = .06). The cohorts were significantly different in sex, as the weekday cohort contained significantly more female patients (P = .008).
Comparison of Demographic and Admission Characteristics Between Weekday Admission and Weekend Admission Cohorts. Chi-Squared Analysis was used to Compare Represented Rates Between Cohorts. Univariate Regression Analysis was Used to Compare Length of Stay and Total Charges Between Cohorts.
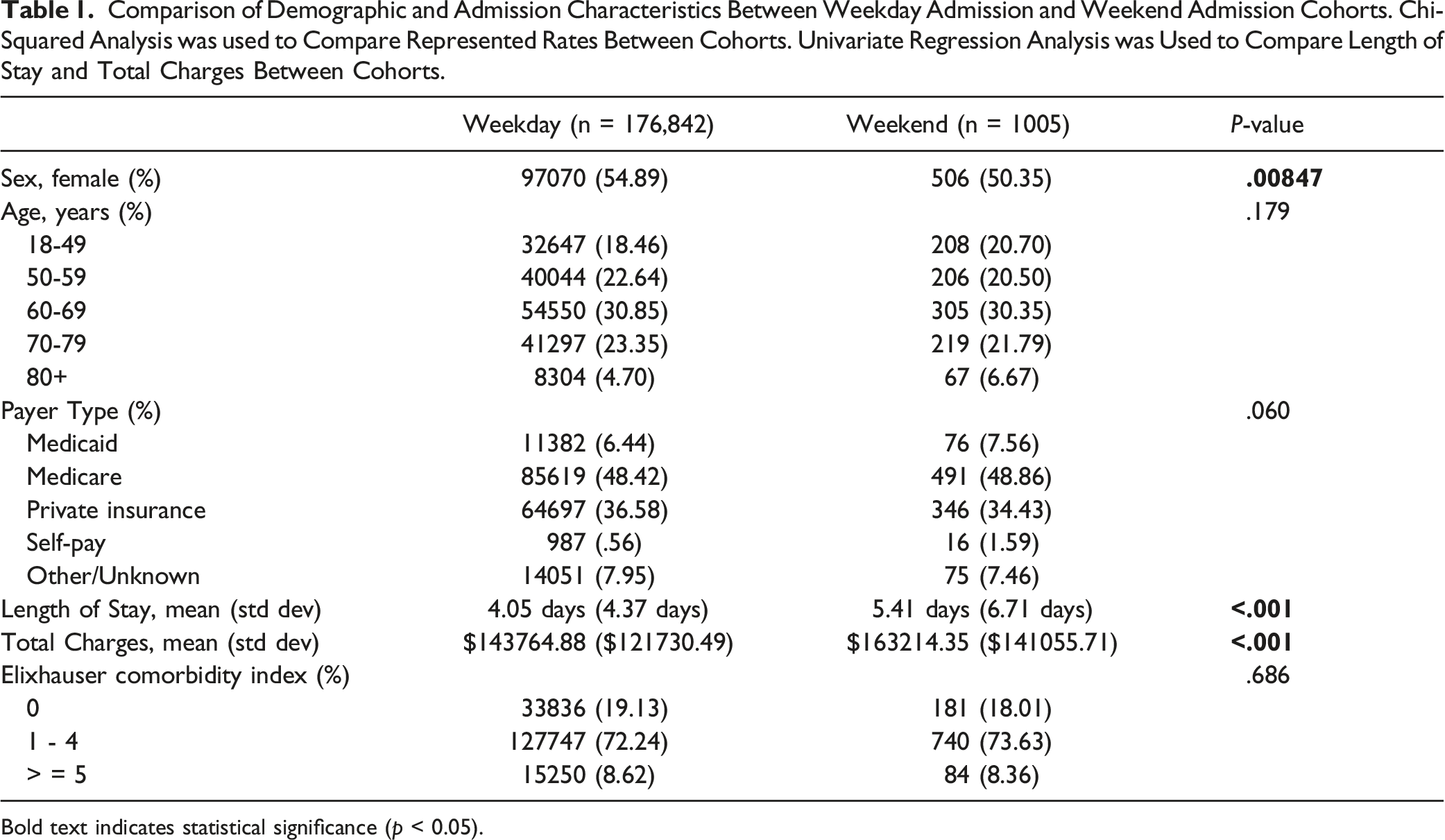
Bold text indicates statistical significance (p < 0.05).
Comorbidity Analysis
Frequency of Elixhauser Defined Comorbidities for Weekend and Weekday Admission Cohorts. Chi-Squared Analysis was used to Compare Comorbidity Rates Between Cohorts.
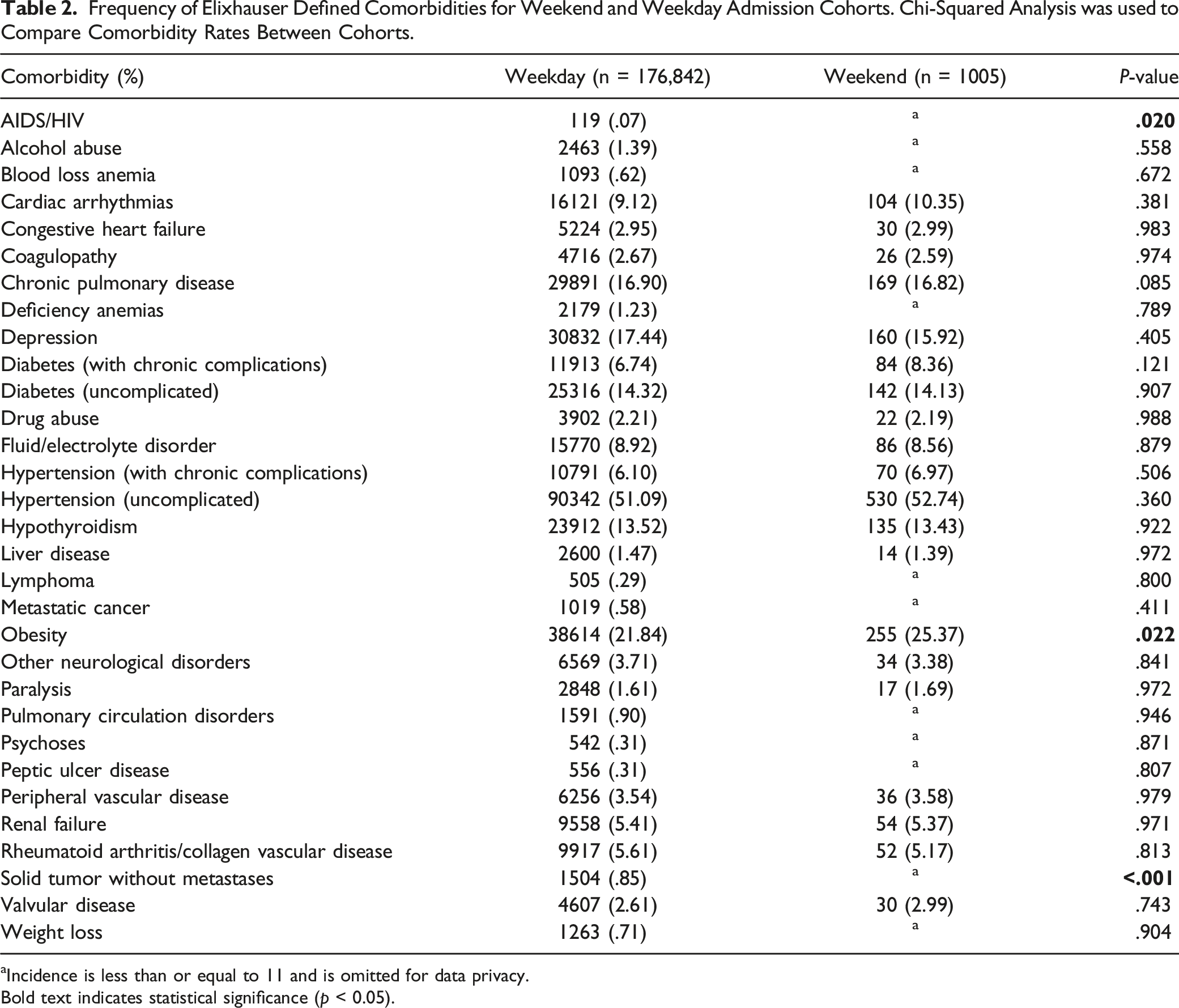
aIncidence is less than or equal to 11 and is omitted for data privacy.
Bold text indicates statistical significance (p < 0.05).
Readmission Rates and Causes
30-day and 90-day Readmission Rate Comparison Between Weekday Admission and Weekend Admission Cohorts. Chi-Squared Analysis was used to Compare Readmission Rates Between Cohorts.

Bold text indicates statistical significance (p < 0.05).
Odds ratios for 30-day readmission following weekend admission.

Bold text indicates statistical significance (p < 0.05).
Odds Ratios for 90-day Readmission Following Weekend Admission.

Bold text indicates statistical significance (p < 0.05).
After adjusting for sex, age, Medicare or Medicaid status, and Elixhauser comorbidity index using multivariate logistic regression, 30-day readmissions remained higher for members of the weekend admission cohort (OR 2.00, 95% CI 1.60-2.48, P < .001). 90-day readmission rates also remained higher for members of the weekend admission cohort after adjustment (OR 2.01, 95% CI: 1.68-2.40, P < .001) (Tables 4 and 5).For both the weekday admission and weekend admission cohorts, the most frequent diagnosis associated with 30 and 90 day readmission was infection following a procedure (Supplementary Table 2 and 3).
Complication Rates
Frequency of Postoperative Complications for Weekday Admission and Weekend Admissions Cohorts. Chi-Squared Analysis was used to Compare Complication Rates Between Cohorts.
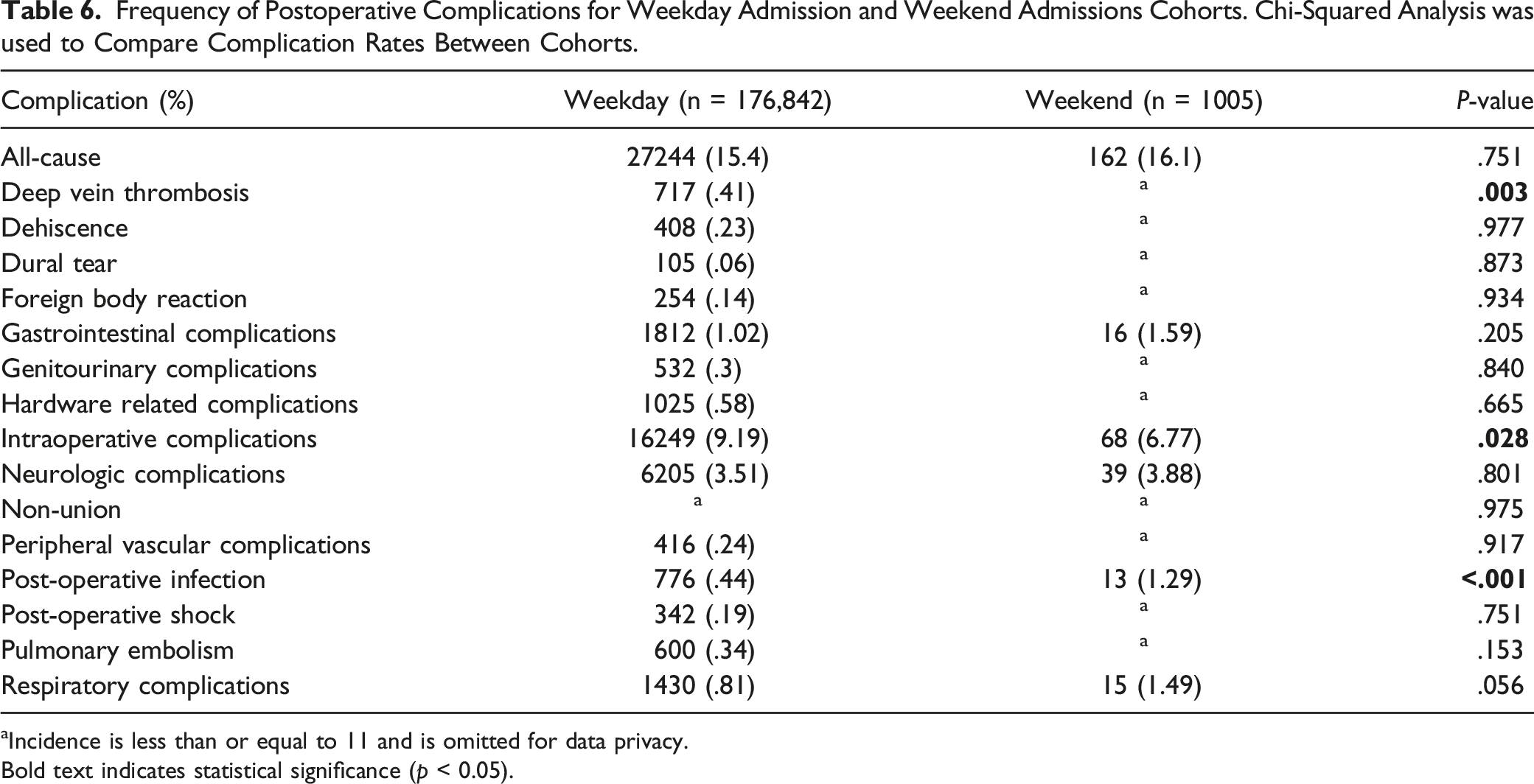
aIncidence is less than or equal to 11 and is omitted for data privacy.
Bold text indicates statistical significance (p < 0.05).
Discharge Status
Discharge status after first admission for weekday admission and weekend admission cohorts. Chi-squared analysis was used to compare discharge status rates between cohorts.
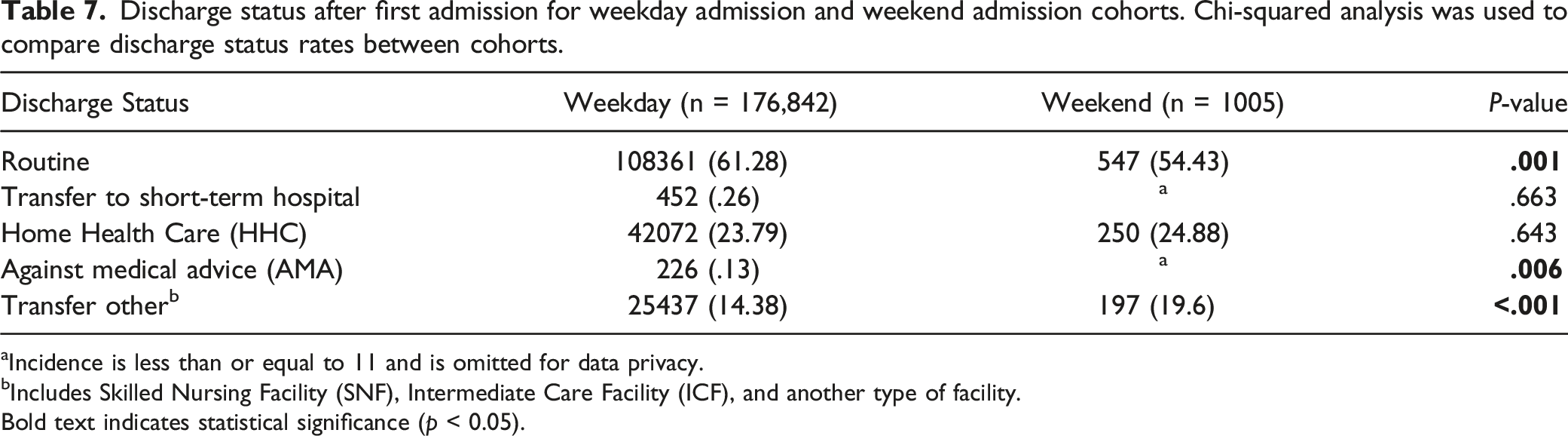
aIncidence is less than or equal to 11 and is omitted for data privacy.
bIncludes Skilled Nursing Facility (SNF), Intermediate Care Facility (ICF), and another type of facility.Bold text indicates statistical significance (p < 0.05).
Discussion
Though the “weekend effect” has been described in the literature as it pertains to the medical field as a whole, its influence on spine surgery has been minimally explored. Additionally, even less is described in the literature regarding the effect of weekend admission vs weekday admission on patient outcomes following thoracolumbar surgery. This study is the first to describe differences in readmission rates between patients who underwent thoracolumbar surgery admitted on weekends and weekdays.
Our study found that patients undergoing elective thoracolumbar spinal fusion surgery who are initially admitted on the weekend are significantly more likely to be readmitted to the hospital than weekday admit patients.This was true even after adjusting for patient sex, age, Medicare or Medicaid status, and Elixhauser combordity score. Furthermore, analysis of the most frequent diagnoses at readmission confirmed a likely relationship between 30-day and 90-day readmission and previous thoracolumbar surgery, with infection following a procedure, sepsis, displacement of internal fixation device of vertebrae, and disruption of surgical wound among the most common diagnoses at readmission. Weekend admission patients also have significantly longer length of hospital stay, greater total hospital charges, increased rates of discharge against medical advice and to additional care facilities, and increased rates of DVT and post-operative infections.
Hospital readmission presents a significant financial burden to the American healthcare system. In 2011, 3.3 million 30-day all-cause hospital readmissions in the United States resulted in hospital costs amounting to $41.3 billion. 13 Lumbar spine surgery patients are also subject to readmission and increased healthcare costs. Hydrick et al. found 90-day readmission following elective revision lumbar fusion surgery was associated with an average increase of $96,152 per patient, compared to those who were not readmitted. Describing the relationship between weekend admission and future readmission can help providers address differences in weekend care and therefore minimize the sources of increased costs associated with patients admitted on weekends.
We found that weekend admission patients were approximately twice as likely to be readmitted to the hospital both within 30 days and 90 days of their initial admission when compared with patients admitted on weekdays. Similarly, an analysis of readmission rates in patients undergoing elective posterior cervical surgery for degenerative conditions found that weekend admission at index hospitalization was a significant risk factor for 30-day readmission. 14 Hospital readmission after spine surgery presents an undesirable experience for patients because of the hardships directly associated with additional time spent in the hospital. Associated financial hardships are notable, with patients who were readmitted to hospitals after posterior cervical fusion or posterior decompression paying an additional $12,495 with 30-day readmission and an additional $14,391 with 90-day readmission on top of the mean index hospitalization cost of $24,647. 14 Our analysis found that weekend admission thoracolumbar fusion patients faced total hospital charges of $163,214.35 for their first admission, which was significantly higher than the amount for weekday admission patients, $143,764.88. This increase in cost does not take the cost of readmission into account and is solely attributed to the increased length of initial hospital stay. Thus, weekend admission patients are more likely to experience an even greater total cost due to their initial length of stay and the charges associated with readmission, which is more likely to occur.
In addition to confirming the presence of a “weekend effect” using hospital readmission rates, our analysis goes further to specifically identify the differences in discharge status, postoperative complications, demographic characteristics, and comorbidities between the weekday and weekend admission cohorts for elective thoracolumbar spinal fusion. The weekend cohort had fewer female patients and increased incidence of obesity and AIDS/HIV. Although the increase in AIDS/HIV incidence was statistically significant, it is unclear if this difference is clinically significant. However, adjusting for these factors still resulted in significantly increased hospital readmission rates for the weekend admission cohort.
Patients admitted on weekends for elective thoracolumbar spinal fusion experienced a significantly higher risk of non-routine discharge compared to weekday admission patients, including discharge against medical advice and discharge to skilled nursing facilities, intermediate care facilities, or other types of facilities. The increased rate of discharge against medical advice is particularly concerning for several reasons. First, in comparison with planned discharges, discharge against medical advice reduces the length of admissions, resulting in incomplete inpatient treatment. 15 Incomplete inpatient treatment after thoracolumbar spinal fusion could exacerbate postoperative complications, necessitating hospital readmission. Notably, an analysis of discharges against medical advice found that those most at risk were patients with Medicaid, Latino patients, patients with higher acute physiology scores, and patients cared for by residents. 15 This suggests a potential lack of adequate communication regarding the risk of discharge against medical advice, possibly due to language barriers or provider inexperience, as well as substandard follow-up care for Medicaid patients. 15 This assessment is bolstered by the fact that a survey of provider attitudes towards discharge against medical advice revealed a common theme of poor patient-physician communication, indicating a need for deeper analysis of discharge outcomes in thoracolumbar spinal fusion patients. 16
The cost of hospital readmission has also been described specifically in patients with non-routine discharge status. Tan et al. found 30-day readmissions that specifically occurred after discharge against medical advice were associated with over $800 million in hospital costs. 17 Furthermore, in a study examining discharge outcomes for patients undergoing 1- or 2-level lumbar fusion, increased LOS was a major driver of increased total hospital costs for patients discharged to nonhome facilities, and the increased LOS was attributed to the lengthy precertification process required for nonhome discharge. 18 More specifically, total hospital costs for patients discharged to nonhome facilities was $21,204 compared to $17,518 for patients discharged home. 18
Non-routine discharge is not only fiscally problematic but also directly associated with negative health outcomes for patients. Southern et al. found a significantly higher risk of 30-day mortality amongst patients discharged against medical advice when compared with planned discharges, even after adjusting for sociodemographic and clinical characteristics. 15 Additionally, in a review of discharge outcomes after anterior lumbar interbody fusion, it was found that discharge to inpatient care facilities was correlated with increased risk of postdischarge wound and sepsis complications. 19 An analysis of nonhome discharge after elective 1- to 2-level posterior lumbar fusions (PLF) found an association between discharge to skilled care or rehabilitation facilities and higher odds of unplanned reoperations and hospital readmission following discharge. 20 Moreover, discharge to skilled care or rehabilitation facilities after PLF was also related to increased risk of any complication, wound complication, sepsis related complication, DVT/pulmonary embolism complications, and urinary tract infections. 20 Thus, the increased incidence of non-routine discharge noted in our weekend cohort could be a contributing factor to the elevated risk of hospital readmission, so highlighting differences in discharge status is crucial in our analysis of the “weekend effect” in outcomes for elective thoracolumbar spinal fusion.
As previously discussed, increased LOS experienced by patients in the weekend admission cohort may be a result of prolonged precertification required to be discharged to advanced care facilities. However, several papers using the National Inpatient Sample (NIS) that found weekend admission prior to cervical and thoracolumbar surgery to be a risk factor of prolonged length of stay attribute LOS in this population to be a result of postoperative complications.5-7 We postulate that extended LOS of the weekend admission cohort in our study is a combination of both postoperative complications and time needed for approval to be admitted into advanced care facilities. Ultimately, we cannot determine whether the increased LOS consists mainly of preoperative days or postoperative because we do not know the timing of the surgery itself within the initial hospitalization period. However, because we selected for elective thoracolumbar spinal fusion surgery, we suspect that surgery date is likely the same as or close to the date of admission due to the scheduled nature of elective procedures, further supporting that the postoperative period is likely the driver of increased LOS.
Differences in postoperative complications following thoracolumbar fusion between weekend and weekday admission patients is minimally represented in the literature. Attenello et al. identified a higher frequency of hospital acquired conditions (HAC) following thoracolumbar surgery in the weekend cohort after adjusting for patient and hospital covariates. The most common HACs for both cohorts overall were falls/trauma and surgical site infection. 5 In our study, rates of DVT and postoperative infection were significantly increased in the weekend admission cohort when compared to the weekday admission cohort. Increased postoperative infection could be explained by a recent study examining decreased quality of support services on weekends demonstrated through accuracy of blood culture diagnostics. 21 A decrease in blood culture positivity rates on weekends compared with weekdays was attributed to sample mishandling, leading to delayed diagnosis of sepsis and antibiotic administration. 21 Previous studies have noted the incidence of symptomatic DVT in patients who underwent posterior lumbar spinal surgery, documenting various risk factors including advanced age, higher preoperative serum D-dimer level, and lower serum potassium level. 22 However, DVT has not been previously associated with the “weekend effect.” These adverse outcomes indicate a need to consider the factors impacting the quality of surgical care on weekends for elective thoracolumbar spinal fusion.
There are several hospital factors that could potentially contribute to the “weekend effect.” Gallego et al. referenced several studies analyzing the weekend effect in their review of temporal patterns affecting patient safety. Important factors that defined weekend care included a smaller percentage of administrative and clinical teams with fewer specialists and significantly lower nurse-to-patient ratios. 23 Additionally, interventional procedures were delayed in weekend patients, and this delay was associated with increased infection complications, length of stay, and mortality. 23 With these documented differences in quality of weekend hospital care, there is a clear need for further investigation into the factors driving the “weekend effect” and improvement of hospital standards of care for weekend admission patients.
In conclusion, our study adds to the literature supporting the existence of the “weekend effect,” providing evidence for the impact of weekend admission on patients undergoing elective thoracolumbar spinal fusion. This is demonstrated via increased risk of hospital readmission for weekend admission patients. These patients were also more likely to experience non-routine discharge, which has been shown in the literature to increase likelihood of readmission, as well as increased length of hospital stay and increased risk of postoperative infection and deep vein thrombosis. Addressing the factors associated with the “weekend effect”—and if possible avoiding weekend admission—will ultimately lead to more positive outcomes for patients and decreased healthcare costs.
A limiting factor with this study is the inherent inaccuracies in ICD-9 and ICD-10 coding, affecting accurate documentation of patients with multiple comorbidities and possibly causing postoperative complications to be underreported. The study is also limited by the retrospective nature of the NRD, which could result in selection bias between the cohorts. Additionally, we did not have access to the patient’s date of surgery, so we did not know which days within the total length of stay were preoperative days or postoperative days. Future analyses could include analyzing the impact of patient race and the “July effect” on readmission outcomes for elective spinal fusion.
Conclusion
This study has demonstrated that there is evidence of a ‘weekend effect’ for patients undergoing thoracolumbar spinal fusion surgery, with patients who are initially admitted on the weekend experiencing higher rates of 30- and 90-day readmissions. Furthermore, patients admitted on weekend days experience increased rates of DVT and postoperative infection, prolonged length of stay, and non-routine discharge. Therefore, these risk factors are all potential areas of focus for guiding preoperative counseling and postoperative care management in order to reduce readmissions and improve outcomes for elective thoracolumbar spinal fusion.
Supplemental Material
Supplemental Material - Weekend Admission Increases Risk of Readmissions Following Elective Thoracolumbar Spinal Fusion
Supplemental Material for Weekend Admission Increases Risk of Readmissions Following Elective Thoracolumbar Spinal Fusion by Ashley Rosenberg, BS, Calista Dominy, BS, Brian T. Bueno, BS, Sara Pasik, BA, Brandon Yeshoua, BS, MHA, Brian Cho, BS, Varun Arvind, PhD, Aly A. Valliani, BA, Jonathan Markowitz, MD, and Jun S. Kim, MD, Samuel K. Cho, MD in Global Spine Journal
Supplemental Material
Supplemental Material - Weekend Admission Increases Risk of Readmissions Following Elective Thoracolumbar Spinal Fusion
Supplemental Material for Weekend Admission Increases Risk of Readmissions Following Elective Thoracolumbar Spinal Fusion by Ashley Rosenberg, BS, Calista Dominy, BS, Brian T. Bueno, BS, SaraE Pasik, BA, Brandon Yeshoua, BS, MHA, Brian Cho, BS, Varun Arvind, PhD, Aly A. Valliani, BA, Jonathan Markow tz, MD, and Jun S. Kim, MD, Samuel K. Cho, MD in Global Spine Journal
Supplemental Material
Supplemental Material - Weekend Admission Increases Risk of Readmissions Following Elective Thoracolumbar Spinal Fusion
Supplemental Material for Weekend Admission Increases Risk of Readmissions Following Elective Thoracolumbar Spinal Fusion by Ashley Rosenberg, BS, Calista Dominy, BS, Brian T. Bueno, BS, Sara Pasik, BA, Brandon Yeshoua, BS, MHA, Brian Cho, BS, Varun Arvind, PhD, Aly A. Valliani, BA, Jonathan Markowitz, MD, and Jun S. Kim, MD, Samuel K. Cho, MD in Global Spine Journal
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
