Abstract
Study Design:
Retrospective survey.
Objectives:
Purpose of this study was to explore whether bowel and bladder management can be influenced by locomotion therapy with HAL Robot Suit.
Methods:
35 subjects with acute (< one year since injury, n = 13) or chronic (> one year since injury, n = 22) incomplete paraplegia (American Spinal Injury Association Impairment Scale (AIS) B, n = 1 / AIS C, n = 22 / AIS D, n = 7) or complete paraplegia (AIS A, n = 5) with zones of partial preservation (ZPP) participated. A retrospective survey was carried out asking for bowel incontinence (Wexner Score), constipation (Cleveland Clinic Constipation Scoring System (CCCS)) and bladder function (self-developed questionnaire) before and after completing a training period of 12 weeks with HAL.
Results:
Wexner Score over all patients and for group of chronic patients decreased significantly. For group of acute patients Wexner Score decreased insignificantly. Patients from both groups with higher baseline scores could decrease significantly. CCCS was insignificantly reduced for all patients, group of acute and group of chronic patients. For subgroup of chronic patients with higher baseline scores, CCCS decreased at end of training period missing out significance. The self-developed questionnaire showed an improvement in bladder function in 28.24% of all patients, 31.43% of chronic patients, and 23.08% of acute patients.
Conclusions:
Our findings show trends of enhanced bladder and bowel function following exoskeleton training. Patients with higher baseline scores in Wexner Score and CCCS seem to benefit more than those with mild to moderate scores.
Introduction
Spinal cord injury (SCI) affected people experience a drastic incursion in their lives. Loss of mobility and independency, pain and spasticity represent only a couple of possible consequences they may have to deal with.1,2 However, bladder and bowel dysfunctions are a common problem in SCI patients, not only physically but also psychologically challenging and associated with depression and decreased quality of life (QoL).1,3-6 As persons concerned tend to self-isolate, it has a disastrous impact on their social life. 3
Locomotor training after SCI is known to be effective regarding motor outcomes and showed signs of positive effects on bowel and bladder function.7,8 In recent years locomotor training with exoskeleton systems was used for rehabilitation of SCI patients and provided efficiency in terms of functional improvements. Amendments in bladder and bowel functions received less attention; however, they were reported for some devices.1,9-13
The Hybrid Assistive Limb (HAL) Robot Suit (Cyberdyne Inc., Ibaraki, Japan) is a wearable cyborg that is controlled using remaining muscle impulses of the lower extremities. 14 Acute and chronic SCI patients benefits in regard to walking ability while wearing the device on treadmill (walking time, distance, speed) as well as without wearing it (10-Meter-Walk-Test (10MWT), Timed-Up-and-Go-Test (TUG), 6-Minutes-Walk-Test (6MWT)) were published previously.9,15-21 Patients included in those studies partially reported about changes in their bladder and bowel dysfunctions subsequently, which were not assessed in the course of the study. The objective of the present study was therefore to explore the influence of locomotion therapy with HAL on bladder and bowel function retrospectively.
Methods
Study Design
A retrospective survey was carried out using 2 standardized and established gastroenterological questionnaires (Cleveland Clinic Constipation Scoring System (CCCS), Wexner Score) for bowel function and a self-developed questionnaire asking for bladder function before and after completing a training period of 12 weeks with wearable cyborg HAL. Questionnaires were handed out and completed within 2 weeks after completing the training period asking for condition prior and condition immediately after the training period.
Participants
The survey involved 35 participants who received HAL training between September 2013 and March 2015. 13 patients (male n = 9, female n = 4) were in acute state (< one year since injury, average 3.85 ± 2.58 months) with an average age of 46.85 ± 13.98 years, an average height of 177.38 ± 12.65 cm and a mean body weight of 76.62 ± 12.47 kg. 22 patients (male n = 17, female n = 5) were in chronic state (> one year since injury, average 71.73 ± 60.71 months) and showed an average age of 48.95 ± 13.81 years, an average height of 177.14 ± 9.15 cm and a mean body weight of 77.95 ± 12.39 kg. The inclusion criteria were an acute or chronic incomplete paraplegia (American Spinal Injury Association Impairment Scale (AIS) B / C / D) or complete paraplegia (AIS A) with zones of partial preservation (ZPP). The participants had to have motor functions of flexor and extensor muscles of the hips and knees to be able to control the exoskeleton (Frankel and Janda Grade 1/5 or 2/5 22 ). Exclusion criteria included cardiopulmonary comorbidities, lower extremity decubitus, infections, osteoporosis, past thrombosis / embolism, contractures or severe spasticity of the lower limb, epilepsy, the presence of electronic medical devices that cannot be removed (e.g. pacemakers), and a body weight over 100 kg. The study was approved by the Ethics Committee of the medical faculty of the Ruhr-University of Bochum (Register No. 4733-13) and strictly follows the Declaration of Helsinki. The subjects were instructed about the objectives and the course of the study and provided written consent Alexis Brinkemper and Dennis Grasmücke shared first authorship.
Intervention
All patients underwent a body-weight-supported treadmill (WOODWAY USA Inc.) training of 30 minutes 5 times a week over 12 weeks using HAL as described previously. 15 At the outset, the harness system supported roughly 50% of each patient’s body weight and was reduced as tolerated within process of training. The speed could be aligned from 0km/h up to 4.5km/h. The velocity of the treadmill was settled individually among comfortable and maximum speed tolerated by the patients. Rest periods were taken as needed. Training was performed in the “Zentrum für Neurorobotales Bewegungstraining” (ZNB) in Bochum, Germany. All training sessions were observed by qualified physiotherapists. No adverse events occurred during the intervention. The mean number of training sessions was 58.54 ± 4.19. Nutrition and medication were not changed during training period.
HAL Robot Suit
The HAL system consists of a back module, a hip frame, an upper and lower leg frame on the right and left side as well as own sensor shoes (Figure 1). All components can be individually sized to suit the individual user. Servo motors at the hip and knee joints provide the necessary torque support. Bioelectric signals (BES) are detected via electrodes applied to the skin surface directly above the flexion and extension muscles of the hips and knees and a connection between patients and the exoskeleton is established via cable. Using these BES HAL generates torque support, which allows a voluntary robotic-supported movement. Settings of torque support at each joint are adjusted by a trained therapist using multiple pieces of information provided from HAL such as BES, joint angle and plantar pressure, visualized on a controller. Over the course of the training, these settings are optimized and adapted as needed. During training with HAL, no assistive devices are used. To support balance, patient can use handrails from treadmill.

HAL® - Hybrid assistive limb exoskeleton (Cyberdyne Inc.).
Questionnaires
Wexner Score
All patients completed the Wexner incontinence questionnaire to assess the severity of fecal incontinence. This score uses a scale from 0 – 20, with 0 = perfect and 20 = complete incontinence. 3 The following subdivision can be made: 1 – 7 = good continence, 8 – 14 = moderate incontinence, 15 - 20 = severe incontinence. 23
Cleveland Clinic Constipation Scoring System
The CCCS is a questionnaire presented by Agachan et al 24 in 1996 to assess the severity of constipation and thus to obtain a universally applicable and objective definition of the term constipation. The scoring system consists of eight individual questions. The total number of points results from the addition of the point values of the individual questions and covers a range from 0 to 30 points, where 0 means normal bowel function and 30 means severe constipation. From a score of more than 15, the authors speak of constipation. 24
Ad-hoc Developed Questionnaire
In order to inquire about the influence of locomotion training on bladder function, a separate questionnaire was designed at BG University Hospital Bergmannsheil Bochum (Figure 2). Questions were about bladder sensitivity (1), the type of urinary bladder emptying (2) and its frequency using external catheterization, if necessary (3). In addition, questions were asked about the presence of urinary incontinence (4), the use of incontinence pads (5), and the circumstances under which incontinence occurs (6). Furthermore, the feeling of incomplete emptying after micturition (7) and finally to what extent there was a urinary tract infection that had to be treated with antibiotics within the past 3 months (8) was interrogated. The questions offer Likert scales with 5-7 items as answer options, whereby a multiple selection is only possible when asked about the circumstances of incontinence.

Self-developed questionnaire regarding urinary bladder dysfunction.
Statistical Analysis
Results were evaluated after completion of the study using the statistical analysis program PSPP 1.2.0 (GNU Project, Free Software Foundation, Inc.). Mean values and standard deviations (SD) were calculated. Kolmogorov-Smirnov test for normality distribution was performed prior to paired t-test for acute and chronic patients separately as well as for subgroups within these separations to identify significant changes between pre-post conditions. Statistical significance was set at P ≤ .05. Results of our self-developed questionnaire are only presented descriptively and no statistical tests were performed as it is not a validated questionnaire yet.
Results
Comparisons were made for all patients (n = 35) and the group was divided into subgroups of acute (n = 13) and chronic patients (n = 22). Within these subgroups, further subgroups were formed according to baseline scores as described below (Table 1). 2.86% of the participants represent AIS B, 62.86% AIS C, 20.0% AIS D, and 14.29% AIS A.
Measurement Descriptives and Statistical Outcome of Wexner Score and Cleveland Clinic Constipation Scoring System.
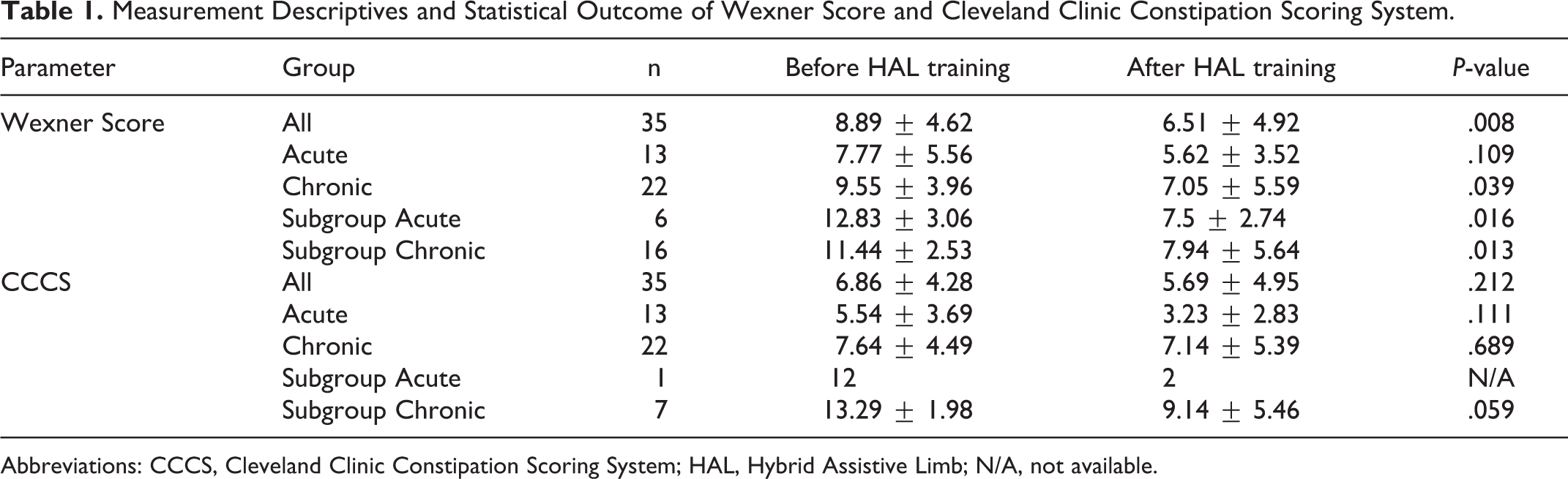
Abbreviations: CCCS, Cleveland Clinic Constipation Scoring System; HAL, Hybrid Assistive Limb; N/A, not available.
Wexner Score
Over all patients (n = 35), the Wexner Score changed from 8.89 ± 4.62 points to 6.51 ± 4.92 points (P = .008).
Acute Patients
Patients who were in the acute stage of paraplegia (n = 13) showed an average Wexner Score of 7.77 ± 5.56 points before training (Figure 3). After exoskeleton training was finished, the average score was reduced to 5.62 ± 3.52 points (P = 0.109), remaining insignificant. In this group, 10 of the 13 patients showed a 1-10 point reduction in the overall Wexner Score. One study participant indicated no change in his stool habits in the Wexner Score; this participant had a score of 0 already before training. In 2 patients, the Wexner Score worsened by 4 and 6 points, respectively.
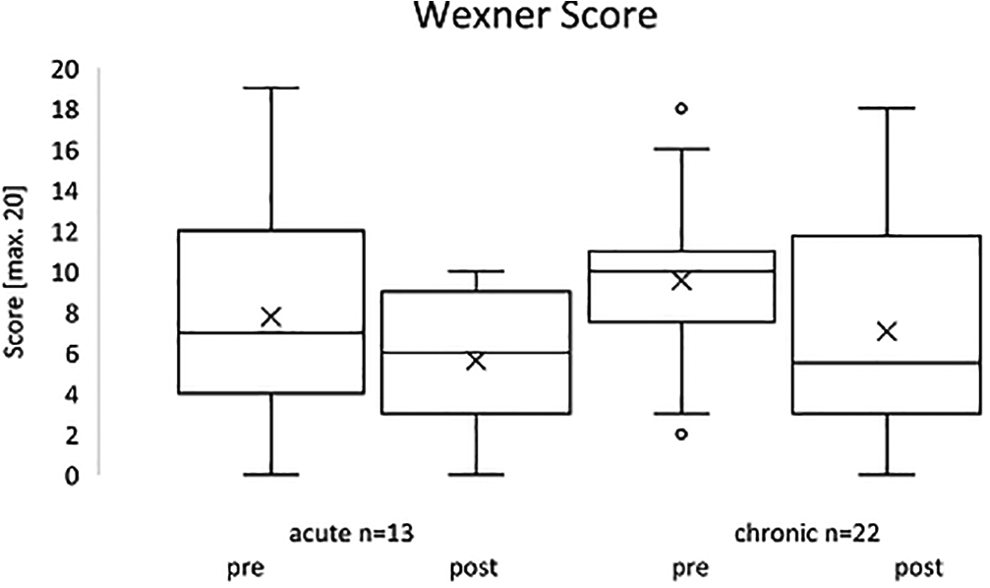
Wexner Score of all involved patients.
Excluding patients who already had a good continence (score ≤ 7) at baseline, 6 acute patients were analyzed separately showing a significant change of Wexner Score from 12.83 ± 3.06 points before training to 7.5 ± 2.74 points after training (P = .016) (Figure 4).
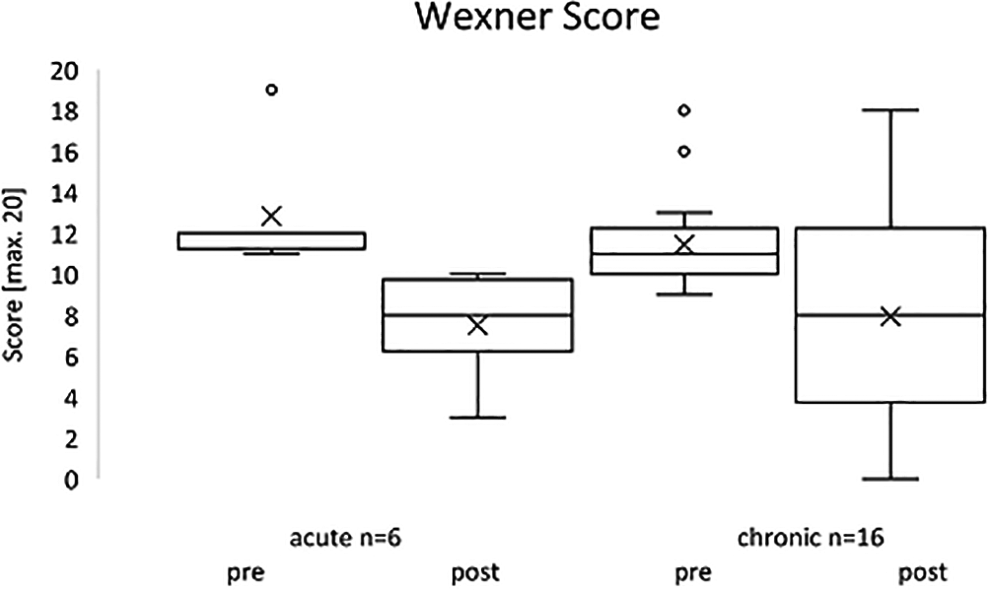
Wexner score of acute and chronic patients with a baseline score above 7.
Looking at the individual questions, 5 patients indicated that they were able to hold solid stool better after exoskeletal training than before. When asked about stool continence in liquid stool, 5 previously incontinent test persons stated that they were always or mostly able to hold it. In particular, when asked about the number of incontinence pads used, 7 of the 13 patients who used incontinence pads before the locomotion training indicated a clear improvement. Five of these 7 patients no longer required any incontinence pads after the intervention. Furthermore, 6 out of 13 study participants reported an improvement in their quality of life.
Chronic Patients
The chronically paraplegic patients (n = 22) showed an average value of 9.55 ± 3.96 points before the 3-month training. After the intervention, the average score was reduced to 7.05 ± 5.59 points (P = .039) and thus showed a significant improvement (Figure 3). 15 study participants showed an improvement of 1-11 points in the overall score, 3 patients indicated the same point value, 4 showed a deterioration.
A separate analysis of patients with a baseline score above 7 (n = 16) showed a significant improvement from 11.44 ± 2.53 points before to 7.94 ± 5.64 points after locomotion training (P = .013) (Figure 4).
In detail, the analysis of the individual questions showed that 7 study participants noticed an improvement in continence with solid stool. When asked about stool continence in liquid stool, 7 patients also reported an improvement. When asked about the impairment of lifestyle, 12 patients said that it had improved after the intervention.
Cleveland Clinic Constipation Scoring System
Over all patients (n = 35), the CCCS changed from 6.86 ± 4.28 points to 5.69 ± 4.95 points (P = 0.212).
Acute Patients
In the CCCS, the total score in acute paraplegic patients reduced from averaged 5.54 ± 3.69 points prior to training to 3.23 ± 2.83 points afterward (P = 0.111) (Figure 5). Of the 13 patients interviewed here, 8 showed an improvement in symptoms. In 2 patients the same point value is available before and after the training intervention. Three patients worsened in the overall score. Having a look into the individual questions, it shows that especially frequency of bowel movement improved and pain during evacuation decreased.
One participant out of the acute patients group had a baseline score above 10 and was therefore considered individually. This patient improved from 12 points to 2 points.
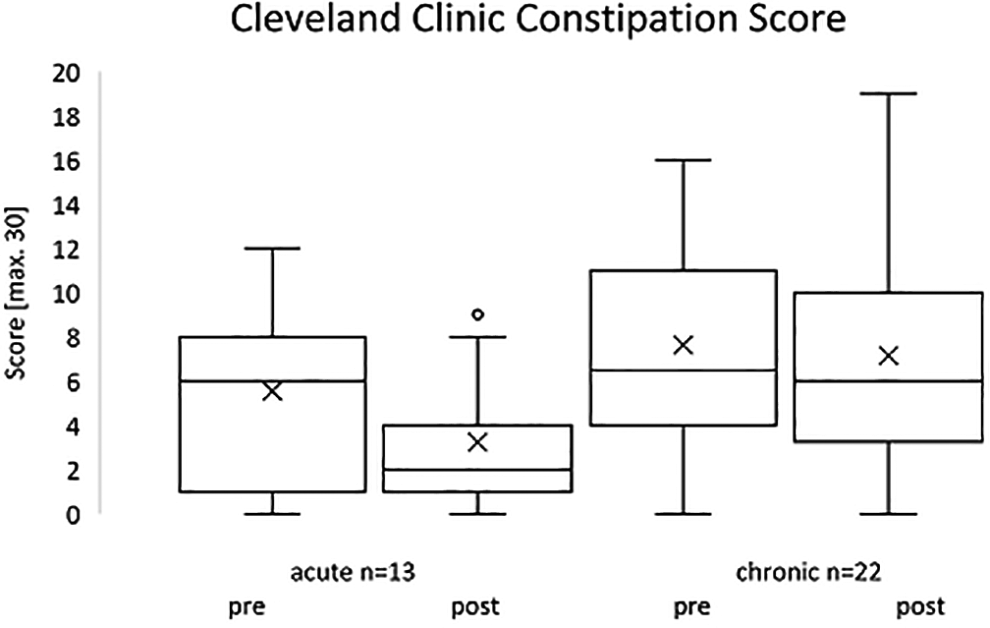
CCCS of all involved patients.
Chronic Patients
The average result in the CCCS for chronic paraplegic patients was slightly reduced from 7.64 ± 4.49 points before training to 7.14 ± 5.39 points after intervention (P = 0.689) (Figure 5). A total of 10 patients out of 22 showed an improvement in the point value in the range of 1-8 points. The point value did not change in 4 patients. In 8 patients, the evaluation of the questionnaires showed a deterioration of the overall score by 1-15 points.
Seven patients out of 22 had a baseline score above 10 and therefore were analyzed separately showing an improved score from 13.29 ± 1.98 points to 9.14 ± 5.46 points (P = .059) (Figure 6).
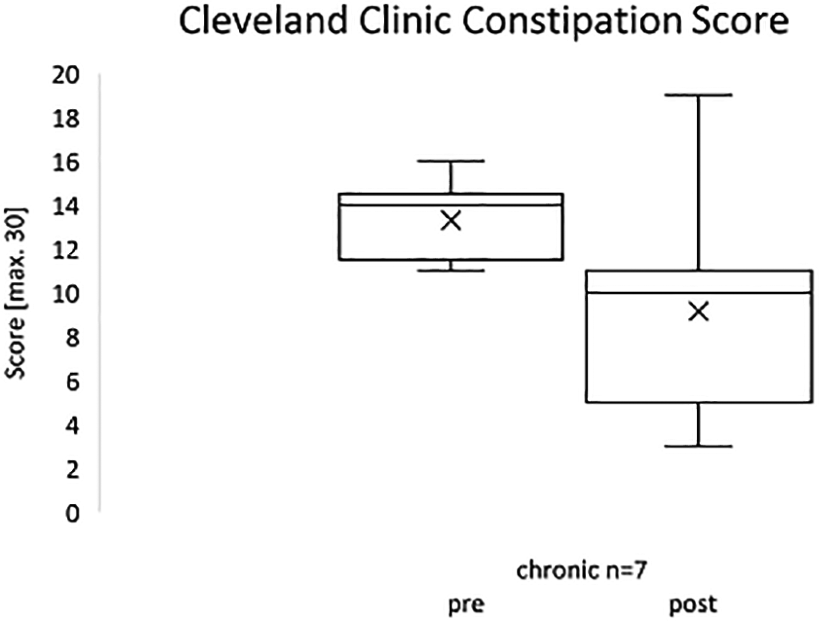
CCCS of chronic patients with a baseline score above 10.
Self-Developed Questionnaire
Acute Patients
In the self-developed bladder questionnaire, 6 of the 13 patients in the acute stage stated that they felt the urinary bladder filling better after the intervention. Five of these 6 reported that they always felt the urinary bladder filling after 3 months of training. Six patients felt no change. One study participant rated bladder sensitivity slightly worse after training than before. When asked how the bladder was emptied, 3 patients reported being able to empty the bladder spontaneously without aids after training, although they had previously been dependent on aids such as intermittent self-catheterization (n = 2) or intermittent external catheterization (n = 1). In 6 patients, the method of emptying the bladder did not change, 4 others again changed the type of device. When asked about the extent of urinary incontinence, 3 patients reported an improvement in continence, 4 reported deterioration and 6 reported constant bladder continence level. One study participant stated that he no longer used incontinence pads after training, although he needed them before therapy. Three test persons required more incontinence pads after the training than before (Figure 7).

Selected questions from bladder questionnaire of acute patients.
Chronic Patients
One chronic patient did not fill out the self-developed questionnaire, which is why only 21 questionnaires were evaluated here. Regarding bladder function, 8 of the 21 patients here report that they felt the urinary bladder filling better after the intervention than before. They stated that they could now always (n = 6) or mostly (n = 2) feel the filling, which was not the case before. When asked how the urinary bladder was emptied, 4 patients stated that this was possible spontaneously after training without aids or catheter, although they had previously been dependent on them. In addition, 7 study participants needed fewer incontinence pads after the training than before, 5 of which no longer needed any pads at all. In response to this question, 11 patients stated that they used the same number of incontinence pads; 3 needed more than before. Six subjects indicated that there was less of a feeling of incomplete emptying than before training. With 3 of them, this feeling no longer exists (Figure 8).

Selected questions from bladder questionnaire of chronic patients.
Discussion
Bladder and bowel dysfunction following SCI is a physical and psychological problem negatively affecting the QoL and is ranked as one the highest priorities for functional recovery in SCI population.2,7,25. Tate et al 26 state that bladder and bowel dysfunction interferes with activities of daily living in 40 - 60% of SCI patients and creates barriers to social interaction and social integration. Therefore it deserves attention as the outcome from rehabilitation programs. Hence we wanted to explore the influence of locomotion therapy with HAL on bladder and bowel function in people with acute and chronic SCI. Our findings demonstrate an overall benefit regarding Wexner Score (P = .008) in 35 involved patients. However, separated by acute and chronic patients, we found no statistical evidence for the group of acute injured patients (P = .109) while the group of chronic patients improved significantly (P = .039). Our group of acute patients had an average time between injury and baseline measurements of 3.85 ± 2.58 months. It is known that recovery of bladder and bowel function is one of the last mechanisms to become better after SCI and therefore comprehensible to not find a significant change in this group. In contrast to our findings, Baunsgaard et al 1 found signs of improvement in bowel function in a group of recently injured patients but not for chronically ones after 24 robotic exoskeleton gait training sessions. Other studies using exoskeletons equally reported about positive change, if any, in bowel function after training in a group of chronic patients 11 and in a collective disregard whether in acute or chronic state. 12 It might be that different training protocols including number of sessions per week and in total as well as usage of different data gathering methods lead to these differentiated outcomes.
Because 13 out of 35 patients presented in this study had a baseline Wexner Score with good continence (score ≤ 7) we excluded those to analyze change in the group of more severely affected patients. Six acute and 16 chronic patients then showed significant results (acute P = .016, chronic P = .013) between baseline and after training, suggesting that treatment has more influence on bowel incontinence for patients with higher values in Wexner Score as for patients with just moderate to low scores. However, without consideration of significance 76.92% of acute and 68.18% of chronic patients improved in Wexner Score.
CCCS showed no significant change for whole group (P = .212), for group of acute patients (P = .111) or group of chronic patients (P = .689). As the overall average score at baseline were 6.86 points and the authors states that only a score of more than 15 points represents a constipation, 24 it could be argued that no positive impact of training could show because no real constipation was present even before training. Only 2 patients (both out of the chronic group) had a baseline score ≥15 points. One improved from 16 points to 10 points whereas the other increased in score from 15 points to 19 points. However, 61.54% of acute and 45.45% of chronic patients improved in CCCS and even though not statistically significant, this could be clinically significant for patients as having an impact on their QoL. 12 To analyze whether patients with a higher CCCS at baseline and therefore more likely to have problems with constipation improved more than those one with lower scores, we excluded patients with a baseline score ≤ 10. One acute patient and 7 chronic patients remained. The acute patient improved clearly from 12 points to 2 points while the 7 chronic patients showed a change from 13.29 ± 1.98 points to 9.14 ± 5.46 points narrowly missing the significance threshold (P = .059). These results may lead to the interpretation that patients with low or without constipation do not experience changes in function after training while patients with moderate to higher constipation may benefit from such training.
Beside bowel function, bladder function is of interest for SCI population. Juszczak et al 12 reported in their study with acute and chronic SCI patients 91% who have not experienced a change in bladder management after exoskeleton training. Indeed, from the 9% who reported about change, all assessed a positive change. Hubscher et al 7 examined bladder function after locomotor training in chronic SCI, finding significantly increased bladder capacity after training and decreased urinary incontinence in some participants. For this survey, we developed an own questionnaire asking for SCI-relevant topics such as frequency of bladder incontinence or bladder sensitivity. The questionnaire included 5 questions with clear assignment as to whether the condition is better or worse and 3 questions with open-ended answers. In those 5 clear assigned questions, 28.24% indicated an improvement, 23.53% worsened, and 48.24% were unchanged in score. In the group of chronic patients, 31.43% improved, 21.9% worsened, and 46.67% were unchanged while in the group of acute patients 23.08% improved, 26.15% worsened and 50.77% did not change. Patients who worsened mostly reported about episodes of incontinence and increased number of used incontinence pads after training. Our questionnaire shows signs that training with HAL somehow influences the bladder function, although in some cases in the form of temporary deterioration possibly due to unusual strain and exertion.
Limitations of this study include the small sample size as well as the fact that the survey was carried out retrospectively. Furthermore, we used a not validated, self-developed questionnaire for bladder function with inconsistent Likert scale precluding a statistically evaluation. Evaluation of acute injured patient can be questioned as regeneration of bowel and bladder function occurs still months after SCI and therefore status of acute patients cannot be seen as constant before training. Other limitations are the varying lesion levels of our patients, the absence of a control group and a missing follow up evaluation to observe how long the effects last.
Despite these limitations, findings of our survey are consistent with those from Baunsgaard et al 1 , Hubscher et al 7 , Juszczak et al 12 and Chun et al 13 showing trends of enhanced bowel incontinence, constipation and bladder function following exoskeleton training and locomotor training, respectively. Patients with SCI even in a chronic state could potentially benefit from this method of high repetitive and movement-supporting gait training not only in gait-associated parameters as reported previously9,15-21 but also in secondary health conditions and therefore contribute to an increased QoL. Further Studies with larger sample size are needed to confirm this assumption. For this, multi-center approaches should be considered, especially since therapy with exoskeletons has also spread in outpatient therapy centers in recent years.
Footnotes
Authors’ Note
The study was approved by the Ethics Committee of the medical faculty of the Ruhr-University of Bochum (Register No. 4733-13). The subjects were instructed about the objectives and the course of the study and provided written consent.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The authors confirm that the data supporting the findings of this study is available within the article or its supplementary materials.
