Abstract
Study Design:
Scoping review.
Objectives:
To identify a practical and reproducible approach to organize Quality of Care Indicators (QoCI) in individuals with traumatic spinal cord injury (TSCI).
Methods:
A comprehensive literature review was conducted in the Cochrane Central Register of Controlled Trials (CENTRAL) (Date: May 2018), MEDLINE (1946 to May 2018), and EMBASE (1974 to May 2018). Two independent reviewers screened 6092 records and included 262 full texts, among which 60 studies were included for qualitative analysis. We included studies, with no language restriction, containing at least 1 quality of care indicator for individuals with traumatic spinal cord injury. Each potential indicator was evaluated in an online, focused group discussion to define its categorization (healthcare system structure, medical process, and individuals with Traumatic Spinal Cord Injury related outcomes), definition, survey options, and scale.
Results:
A total of 87 indicators were identified from 60 studies screened using our eligibility criteria. We defined each indicator. Out of 87 indicators, 37 appraised the healthcare system structure, 30 evaluated medical processes, and 20 included individuals with TSCI related outcomes. The healthcare system structure included the impact of the cost of hospitalization and rehabilitation, as well as staff and patient perception of treatment. The medical processes included targeting physical activities for improvement of health-related outcomes and complications. Changes in motor score, functional independence, and readmission rates were reported as individuals with TSCI-related outcomes indicators.
Conclusion:
Indicators of quality of care in the management of individuals with TSCI are important for health policy strategists to standardize healthcare assessment, for clinicians to improve care, and for data collection efforts including registries.
Keywords
Introduction
Traumatic spinal cord injury (TSCI) has an annual incidence of 40-80 per million people. About 90% of these cases in under-developed countries are caused by external factors such as motor vehicle accidents, falls, or sports-related activities. 1 An individual with TSCI can experience a variety of acute and chronic complications affecting their quality of life. To improve quality of care, healthcare systems have recently attempted to broaden access to care in addition to improving the care delivered. Studies identifying the quality of care for individuals with TSCI are rare and most of them are based on national registries.
To maximize outcomes following TSCI, timely access to a specialized, patient-centered, and evidence-based care is mandatory. A review of the World Health Organization 2 and other national and international databases demonstrate large differences across countries in the TSCI supply-demand relationship. 1 Interestingly, low- and middle-income countries tended to report less availability of all kinds of resources despite greater need. 3 To address this challenge, the WHO and the International Spinal Cord Society (ISCoS), in a collaborative effort to comprehensively map healthcare, social services, and policy requirements, developed evidence-based recommendations to address these needs based on income level. 4 However, we do not have evidence regarding the current adherence of different countries to these recommendations or improvement by different healthcare system interventions. The former is ongoing by the recent Learning Health System-International SCI Survey (LHS-InSCI) initiative, 5 but the latter requires a robust tool to monitor SCI care in different parts of the world.
Well-defined and validated Quality of Care Indicators (QoCI) can help improve TSCI care by establishing parameters that clinicians, healthcare managers and policymakers can monitor and report. These indicators must be based on evidence and experiences reflecting the standard of care. 6 In the present study, we reviewed the literature to summarize QoCI in individuals with TSCI into 3 groups: 1) healthcare system structure, 2) medical processes, and 3) individuals with traumatic spinal cord injury (TSCI)-related outcomes.
Method
Protocol and Registration
Our protocol included the Preferred Reporting Items for Systematic Reviews and Meta-Analysis protocol for scoping reviews.7,8 The PRISMA chart of this study is also available in Figure 1.
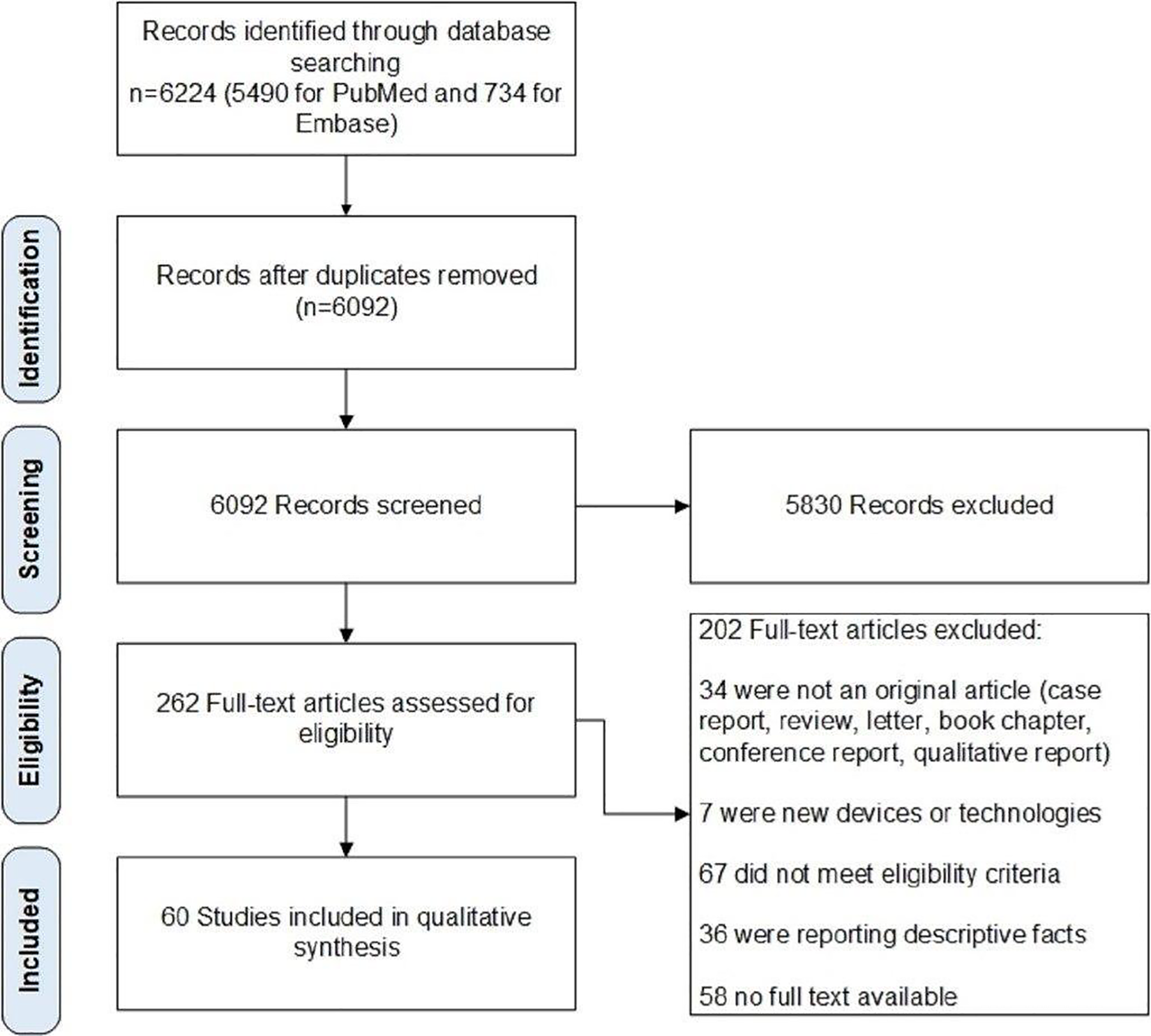
Flowchart of studies excluded and included for this study.
Eligibility Criteria
We included studies with at least 1 QoC indicator to evaluate patients with TSCI without time and language limitations. We excluded case series with less than 10 cases, as well as animal studies. We excluded studies with new technologic instruments and devices (such as robotic-assistance devices or novel types of wheelchairs), as it was difficult to measure their impact and impractical for worldwide application.
Data Sources
To identify relevant studies, a search was done through the following databases: Cochrane Central Registry of Controlled Trials (CENTRAL) (Date: May 2018), MEDLINE (1946 to May 2018) and EMBASE (1974 to May 2018).
Selection of Sources of Evidence
In the first phase of screening, 2 authors independently screened related study titles and abstracts. After examining the discrepancies between the 2 teams, the second phase included full text screening of the included studies. The third stage resolved any potential discrepancy regarding the eligibility of studies through discussion and by the decision of a third review author. Then, based on the nature of indicators, we developed 3 categories: healthcare system structure, medical processes, and individuals with TSCI related outcomes. The same categorization was used in another national study. 9
Data Charting Process and Data Items
Four review authors independently proceeded with data extraction from included studies and entered the data in standardized data collection forms. Each potential indicator was evaluated in an online, focused group discussion to define its categorization (healthcare system structure, medical process, and individuals with Traumatic Spinal Cord Injury (TSCI) related outcomes), definition, survey options (e.g. types of questionnaire, data registries, etc.), and scale (e.g. percentage, day, hour, dollar, etc.), as well as reproducibility across various healthcare systems.
Results
The database search resulted in 6092 records. After screening relevant titles and abstracts, 262 records were included for further assessment. Full-text review resulted in 60 studies for evidence synthesis. Out of 60 studies, the main source of data collection of the 2 studies was national data registries. There were 21,574 cases from 60 studies. We identified 87 indicators from 60 studies, among which 37 indicators were associated with healthcare system structure (Table 1).
Healthcare System Structure Indicators.
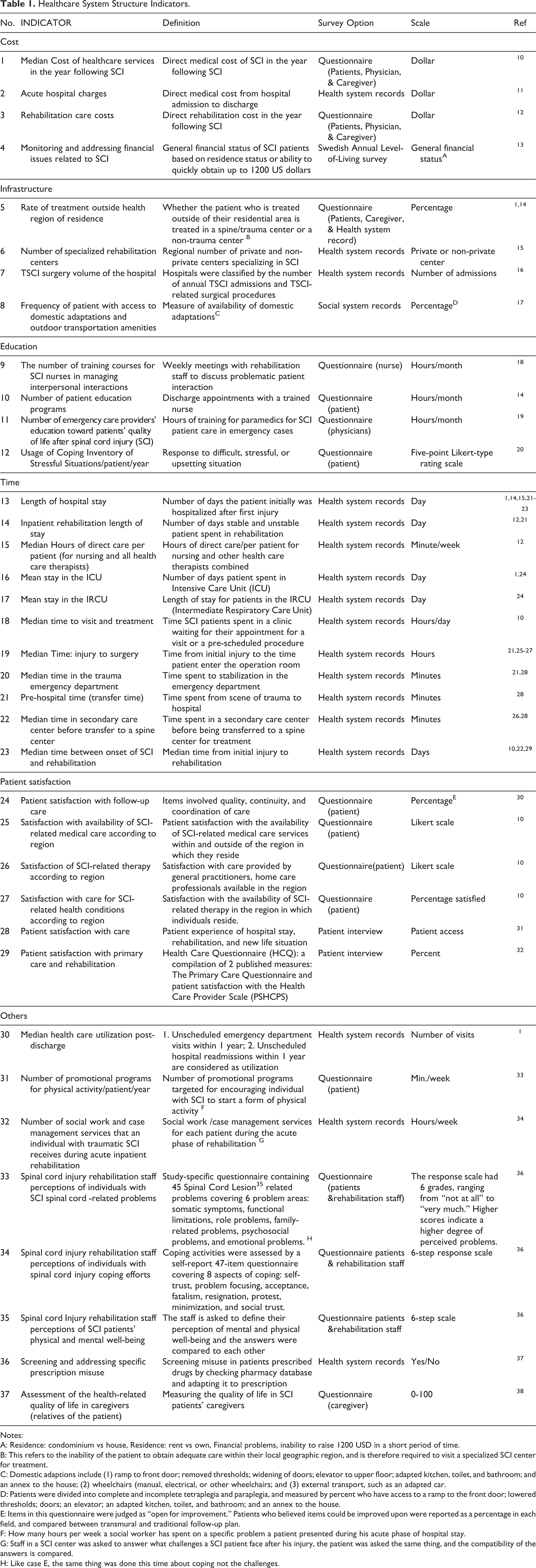
Notes:
A: Residence: condominium vs house, Residence: rent vs own, Financial problems, inability to raise 1200 USD in a short period of time.
B: This refers to the inability of the patient to obtain adequate care within their local geographic region, and is therefore required to visit a specialized SCI center for treatment.
C: Domestic adaptions include (1) ramp to front door; removed thresholds; widening of doors; elevator to upper floor; adapted kitchen, toilet, and bathroom; and an annex to the house; (2) wheelchairs (manual, electrical, or other wheelchairs; and (3) external transport, such as an adapted car.
D: Patients were divided into complete and incomplete tetraplegia and paraplegia, and measured by percent who have access to a ramp to the front door; lowered thresholds; doors; an elevator; an adapted kitchen, toilet, and bathroom; and an annex to the house.
E: Items in this questionnaire were judged as “open for improvement.” Patients who believed items could be improved upon were reported as a percentage in each field, and compared between transmural and traditional follow-up plan.
F: How many hours per week a social worker has spent on a specific problem a patient presented during his acute phase of hospital stay.
G: Staff in a SCI center was asked to answer what challenges a SCI patient face after his injury, the patient was asked the same thing, and the compatibility of the answers is compared.
H: Like case E, the same thing was done this time about coping not the challenges.
Healthcare system structure indicators assessed 6 main domains including: Cost: which evaluates 2 classes: Medical care cost, including healthcare service, acute hospitalization charge, and rehabilitation care cost. Financial ramifications for the patient related to SCI, e.g. loss of income, etc. Infrastructure: which evaluates infrastructure specialized for SCI care, such as number of SCI rehabilitation centers, availability and access to domestic adaptations and outdoor transportation amenities, etc. Education: which evaluates educational programs for physicians, patients, and caregivers. Time: which evaluates 2 main classes including: Length of stay in the hospital, ICU, IRCU, rehabilitation unit. Time cost for different processes: pre-hospital transfer time, Emergency Department (ED) arrival to first visit, injury to surgery, etc. Patient Satisfaction: which evaluates patient-centered point of view in the SCI care process. Others: not classified into other categories.
The number of indicators for the medical process and individuals with TSCI related outcomes were 30 and 20, respectively. The healthcare system structure indicators included: the effects of cost of the acute phase hospitalization and rehabilitation, facility costs (including MRI, CT scan, and staff- and patient-perception of treatment). The medical process indicators included physical activity and rehabilitation, complication rates, and overall treatment including every healthcare professional involved in the patient treatment. Furthermore, telemedicine was identified as a new form of care and a potential indicator (Table 2).
Medical Process Indicators.
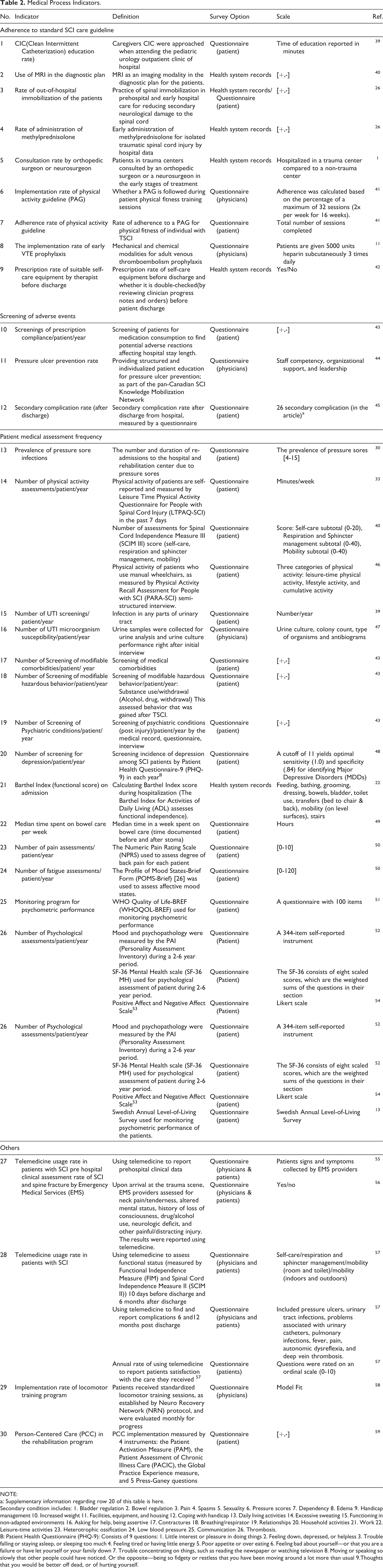
NOTE:
a: Supplementary information regarding row 20 of this table is here.
Secondary condition includes: 1. Bladder regulation 2. Bowel regulation 3. Pain 4. Spasms 5. Sexuality 6. Pressure scores 7. Dependency 8. Edema 9. Handicap management 10. Increased weight 11. Facilities, equipment, and housing 12. Coping with handicap 13. Daily living activities 14. Excessive sweating 15. Functioning in non-adapted environments 16. Asking for help, being assertive 17. Contractures 18. Breathing/respirator 19. Relationships 20. Household activities 21. Work 22. Leisure-time activities 23. Heterotrophic ossification 24. Low blood pressure 25. Communication 26. Thrombosis.
B: Patient Health Questionnaire (PHQ-9): Consists of 9 questions: 1. Little interest or pleasure in doing things 2. Feeling down, depressed, or helpless 3. Trouble falling or staying asleep, or sleeping too much 4. Feeling tired or having little energy 5. Poor appetite or over eating 6. Feeling bad about yourself—or that you are a failure or have let yourself or your family down 7. Trouble concentrating on things, such as reading the newspaper or watching television 8. Moving or speaking so slowly that other people could have noticed. Or the opposite—being so fidgety or restless that you have been moving around a lot more than usual 9.Thoughts that you would be better off dead, or of hurting yourself.
Medical process indicators assessed 4 main domains, which are: Adherence to standard SCI care guideline: Venous Thromboembolism (VTE) prophylaxis, prehospital immobilization, use of MRI, use of steroid, CIC training, etc. Screening of adverse events: which evaluates 2 main classes: ˆ Medical process complications, such as prescription complications ˆ SCI complications, such as bed sores Patient medical assessment frequency: including physical activity, urinary tract infection (UTI) screening, etc. Others: not classified into other categories.
The third table reports the indicators of individuals with TSCI-related outcomes. Measuring tools such as American Spinal Injury Association (ASIA) score, functional independence Measure (FIM), Oswestry disability index (ODI), Spinal Cord Independence Measure II (SCIM II), Self-efficacy improvement rate by Moorong Self-Efficacy Scale (MSES), Canadian Occupational Performance Measure (COPM), and Barthel Index were used to report functional independence outcomes. Discharge efficiency and readmission rate are also part of outcome measuring tools for individuals with TSCI (Table 3).
Individuals With TSCI-Related Outcomes.
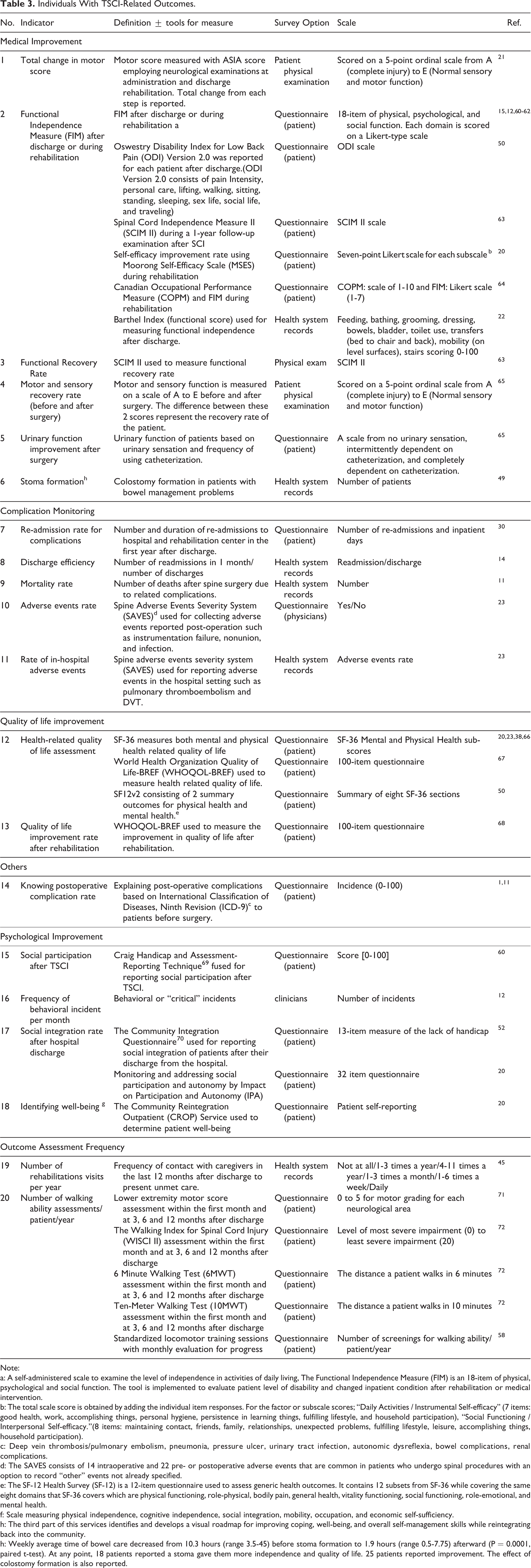
Note:
a: A self-administered scale to examine the level of independence in activities of daily living, The Functional Independence Measure (FIM) is an 18-item of physical, psychological and social function. The tool is implemented to evaluate patient level of disability and changed inpatient condition after rehabilitation or medical intervention.
b: The total scale score is obtained by adding the individual item responses. For the factor or subscale scores; “Daily Activities / Instrumental Self-efficacy” (7 items: good health, work, accomplishing things, personal hygiene, persistence in learning things, fulfilling lifestyle, and household participation), “Social Functioning / Interpersonal Self-efficacy.”(8 items: maintaining contact, friends, family, relationships, unexpected problems, fulfilling lifestyle, leisure, accomplishing things, household participation).
c: Deep vein thrombosis/pulmonary embolism, pneumonia, pressure ulcer, urinary tract infection, autonomic dysreflexia, bowel complications, renal complications.
d: The SAVES consists of 14 intraoperative and 22 pre- or postoperative adverse events that are common in patients who undergo spinal procedures with an option to record “other” events not already specified.
e: The SF-12 Health Survey (SF-12) is a 12-item questionnaire used to assess generic health outcomes. It contains 12 subsets from SF-36 while covering the same eight domains that SF-36 covers which are physical functioning, role-physical, bodily pain, general health, vitality functioning, social functioning, role-emotional, and mental health.
f: Scale measuring physical independence, cognitive independence, social integration, mobility, occupation, and economic self-sufficiency.
h: The third part of this services identifies and develops a visual roadmap for improving coping, well-being, and overall self-management skills while reintegrating back into the community.
h: Weekly average time of bowel care decreased from 10.3 hours (range 3.5-45) before stoma formation to 1.9 hours (range 0.5-7.75) afterward (P = 0.0001, paired t-test). At any point, 18 patients reported a stoma gave them more independence and quality of life. 25 patients reported improvement. The effect of colostomy formation is also reported.
Indicators involving individuals with TSCI-related outcomes evaluated 6 main domains: Medical Improvement: Functional Independence Measure, motor improvement, etc. Complication Monitoring, e.g. mortality, readmission rate, and discharge efficiency. Quality of Life Improvement, e.g. health-related quality of life assessment and quality of life improvement rate after rehabilitation. Psychological Improvement, e.g. social participation after TSCI Outcome Assessment Frequency: number of rehabilitation visits/year and number of walking ability assessments/patient/year.
Other
Discussion
In the present study, we summarized important QoCI indicators in individuals with TSCI. In the current literature, the main focus has been on developing QoCI by finding gaps in care in different phases of the care continuum and designing solutions for the healthcare system, whereas this study focuses on factors affecting the patients care across the TSCI continuum (i.e. from the time of injury through to the community). Examining care in 3 stages is a unique way to report indicators that to our knowledge has not been previously used. We assessed QoCI in terms of access to care and quality of care.
TSCI QoC indicators must cover the TSCI continuum to assist healthcare policymakers, clinicians, and health managers monitor and enhance care. Our study categorized QoC indicators into 3 groups to assist healthcare policymakers with understanding their relevance to care delivery. These groups were healthcare system structure indicators, medical process indicators, and indicators involving individuals with TSCI-related outcomes. Not only were these indicators important for finding gaps in current knowledge, but they also assisted in data collection and designing data registries.1,73 This study is a scoping review; therefore, the main focus was to identify key concepts of care for individuals with TSCI and provide evidence to inform clinicians, healthcare managers, and policymakers.
Healthcare System Structure
Cost of care as a healthcare system structure is a challenging indicator to assess accurately. Cost of care has been mentioned as an indicator for QoC, however hospital care is directly affected by hospital length of stay. 12 If cost of in-hospital care is solely considered as a QoC indicator, many inconsistencies may therefore arise. For instance, certain medications prescribed in the setting of TSCI can be costly compared to other alternatives. In these cases, the incremental cost-effectiveness ratio 74 should be used in cost-effectiveness analysis. This ratio can measure how effective a costly intervention can be in certain patient-specific situations.
The cost of care in this review identified 3 types: acute care costs, cost in the first year following TSCI, and cost of rehabilitation. The effect of costs on the quality of care is not straightforward and there is a need for further research as highlighted by this review. Length of stay is acquainted with better care, including better emotional and social support and also more improvement in FIM, in patients who have suffered from TSCI.15,22 Shortening the length of stay in acute phase could have positive impact on patient outcome while longer stay in a center specialized for TSCI rehabilitation have been shown to improve FIM of individuals to a greater degree.12,22 In other words, the patient benefit the most when staying less in the acute phase of hospitalization and spending more time in a center specialized for TSCI rehabilitation. SCI centers have facilities and specialized services for patients who have sustained a TSCI. In the post-traumatic setting, these rehabilitation centers are equipped to manage the patient from arrival to the emergency room until discharge. Education of patients and staff regarding the challenges and concerns of individuals with TSCI is also an indicator that can often be taken for granted. Patient satisfaction with their care is also an indicator measured at multiple phases and has different measures. These QoC measures help us assess the current situation of healthcare systems in responding adequately to TSCI and provide avenues for future improvements in patient outcomes.
Medical Processes
Medical process indicators mainly focused on screening common postoperative complications such as urinary tract infection, VTE, pressure injuries, and depression. Previous studies reported that urinary tract infections are the most common postoperative complication in patients with TSCI. Clean intermittent catheterization has been proven to reduce the incidence of UTIs and its further complications, such as sepsis in individuals with TSCI. 39 Physical activity and rehabilitation are also considered an essential part of a patient’s care. The use of telemedicine for managing complications and subsequent consultation is also reported to have an impact on a patient care. Patient functional score and psychomotor performance have been measured using a variety of different scales and performance scores.16,34,51,52 VTE prophylaxis at an early stage is an important indicator as well. Evidence-based medicine argues aggressive, early prophylaxis leads to reduced rates of VTE and pulmonary thromboembolism without an increased risk of an epidural hematoma. 11 Early consultation with a neurosurgeon and orthopedic surgeon for spinal cord decompression and spine stabilization was also suggested to increase the quality of care. 1
Individuals With TSCI-Related Outcomes
For measuring individuals with TSCI-related outcomes, the indicators mainly focused on the changes in motor score and functional recovery from initial visit to discharge. Characterizing patient well-being was captured through questionnaires and surveys. 20 An interesting indicator is the number of physician visits per year after discharge to evaluate outcome. Readmission after discharge, reoperation rates, and discharge efficiency (measured as the number of visits in the following month after discharge) were also considered as independent indicators.23,30,45
Future Directions
The identification of QoCI in patients with TSCI will help identify pitfalls in clinical data collection and data inclusion in SCI registries. Some of these indicators require resources to monitor over the long term, but the utility in improving future health care delivery outweighs these costs. Globally, developed and developing countries have healthcare systems that significantly differ from one another. Identifying QoCI could help standardize healthcare assessments for each country. Furthermore, these indicators could provide baseline elements for comprehensive QoC questionnaires to compare healthcare systems across the world. In areas where indicators measure similar concepts, a consensus process such as the Delphi method would help establish standards that can be used by all SCI centers.
Conclusion
This scoping review maps current literature and provides key concepts in the care of individuals with TSCI. These indicators are helpful in improving QoL of individuals with TSCI by providing improved care and enhanced clinical practice. The classification used in this study (healthcare system structure, medical process, and individuals with TSCI related outcomes) models the SCI continuum of care, and may be useful in further data collection efforts.
Supplemental Material
Supplemental Material, sj-docx-1-gsj-10.1177_2192568220981988 - Indicators of Quality of Care in Individuals With Traumatic Spinal Cord Injury: A Scoping Review
Supplemental Material, sj-docx-1-gsj-10.1177_2192568220981988 for Indicators of Quality of Care in Individuals With Traumatic Spinal Cord Injury: A Scoping Review by Sepehr Khosravi, Amirmahdi Khayyamfar, Milad Shemshadi, Masoud Pourghahramani Koltapeh, Mohsen Sadeghi-Naini, Zahra Ghodsi, Farhad Shokraneh, Mohadeseh Sarbaz Bardsiri, Pegah Derakhshan, Khalil Komlakh, Alex R. Vaccaro, Michael G. Fehlings, James D. Guest, Vanessa Noonan and Vafa Rahimi-Movaghar in Global Spine Journal
Footnotes
Competing Interest
None declared except Alex R Vaccaro (file attached).
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval Number Is 97-02-38-323.
Scoping reviews do not directly access patient data, nor do they intervene in medical treatment course, but rather reviews other studies performed in this field. Hence, the ethical consideration is in the minimal risk category.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded and supported by Sina Trauma and Surgery Research Center, Tehran University of Medical Science (TUMS); Grant no. 97-02-38-39121 and approved by National Institute for Medical Research Development (NIMAD).
ORCID iD
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
