Abstract
Background:
Despite being deemed essential non-healthcare workers, agricultural workers were excluded from COVID-19 vaccine prioritization in Texas. This professional practice report describes the multifaceted worker health and safety approaches to protecting agricultural workers and their families during the COVID-19 pandemic.
Methods:
Between March 2020 and January 2025, several outreach, education, and training grants from various funding agencies were leveraged to deliver training, personal protective equipment, vaccines, and economic relief to agricultural workers in partnership with community-based organizations, industry, local public health departments, and academic institutions.
Findings:
Timely funding efforts led to the distribution of 1,000 PPE kits, with more than 3,000 in-person and virtual trainings, 80 on-farm clinics hosted with over 2,200 vaccinations, 4,500 door-to-door education visits in 31 rural counties and 61 zip codes, exceeding 4,600 relief payments distributed, and 30,000 rural county resource lists disseminated across rural agricultural communities in Texas. These collaborative efforts gave rise to Sembrando el Sueño—a program that provided social services to agricultural workers in the Texas Panhandle.
Conclusion/Application to Practice:
Over $4.5 million in grant monies were leveraged to help advocate for agricultural worker health, safety, and well-being as well as their multigenerational households in rural Texas. This report underscores the challenges and the collaborative multifaceted approach needed among various partners to ensure that essential workers are adequately protected from exposure to infectious agents while on the job.
Keywords
Background
In the United States (U.S.), over two-thirds of undocumented immigrants were deemed essential healthcare or non-healthcare workers during the COVID-19 global pandemic declared on March 11, 2020 (CDC, 2023; Conniff, 2022; Texas Economic Development & Tourism Office, 2025). In 2020, over 40% of agricultural workers in the U.S. originated from Mexico, Guatemala, and other Latin American countries, having unknown work authorization status (Castillo & Simnitt, 2023). Deemed non-healthcare essential, many agricultural workers and their families continued to work during peak periods of community spread to provide fresh fruits and vegetables, meats, and dairy products during national stay-at-home orders (Boggess et al., 2023; Conniff, 2022). Yet, essential agricultural workers expressed that they felt olvidados y descuidados (forgotten and neglected) regarding access to personal protective equipment (PPE) supplies, workplace and informational resources to mitigate spread inside the home, testing, and clinical resources between March and June 2020 (CDC, 2020). The pandemic exposed years of historical neglect and exclusion of agricultural workers from public health literacy and practices, unwavering growth of economic inequalities, healthcare and vaccination access, social support, and other occupational health, safety, and well-being initiatives (Bonotti & Zech, 2021; Chicas et al., 2022; Crudo Blackburn & Azurdia Sierra, 2021; Keeney et al., 2022; Olayo-Méndez et al., 2021).
The health inequities became apparent among these workers when the first two authorized COVID-19 vaccines became available in the U.S. on December 14, 2020 (CDC, 2023) and individual states were allowed to prioritize populations using the guidance of the Centers for Disease Control and Prevention (CDC) Advisory Committee on Immunization Practices (ACIP; Dooling et al., 2021). Despite being deemed essential non-healthcare workers by the U.S. Department of Homeland Security (DHS) and mapped to the ACIP vaccination Phase 1B (CDC, 2021), Texas agricultural workers were not eligible for vaccination until Phase 2, alongside 22 million adults (Texas Department of State Health Services, 2021). Broad eligibility, previous dose shortages, and high vaccination demand in Texas led to limited vaccine appointments and disparities in vaccine access for ethnic and racial minoritized groups and people living in rural farming communities (Bauer et al., 2021; Fernández-Sánchez et al., 2023; Freeman Anderson & Ray-Warren, 2022). The purpose of this work is to describe the multifaceted health and safety strategies we implemented in collaboration with community and industry partners to protect agricultural workers and their families during the COVID-19 pandemic.
The study team was composed of public health academics, graduate students, and Community Health Worker (CHWs) contractors across Texas. Collaborators varied from producers, growers, industry associations, dairy extension, farm labor contractors (FLCs), local and regional public health departments, agricultural worker health advocacy groups, legal aid organizations, federally qualified health centers (FQHCs), and other academic institutions. These collaborations were established throughout a decade of field research and outreach conducted across rural farming communities in Texas. In March 2020, this collaborative network started a “Texas Panhandle Immediate Response” group, which met virtually each month to share resource availability, outreach events, address challenges, and general updates of how the pandemic was affecting workers and their families. Over time, this group evolved into the “Texas Farmworker Coalition” expanding its resources and outreach to rural farming communities across Texas. Our team leveraged this network to organize, deliver, and evaluate our outreach and training efforts among agricultural workers and their families (Figure 1).
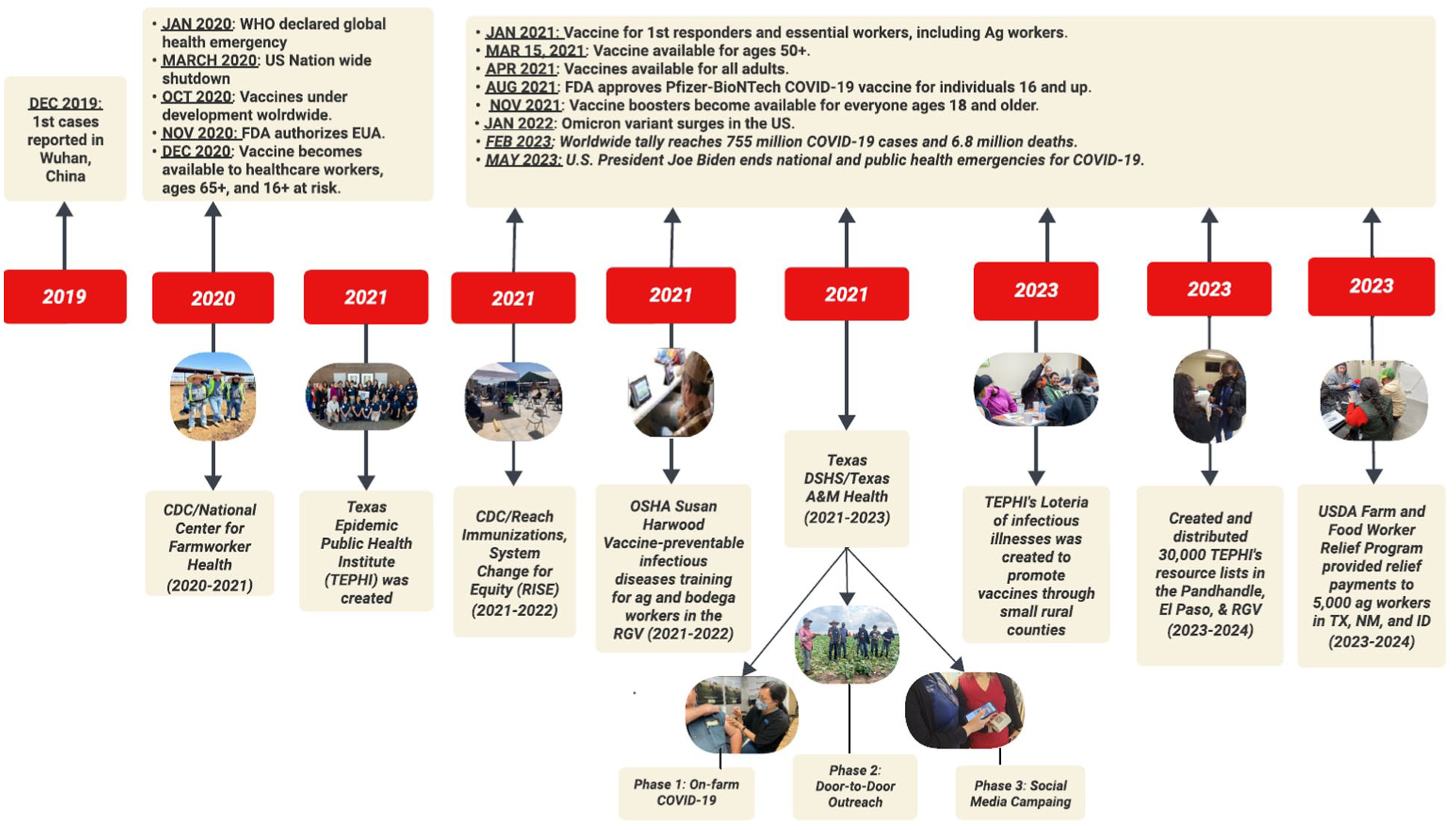
Vaccine outreach timeline (2019–2023).
Essential Non-Healthcare Working Populations Served
This report describes efforts to serve two cohorts of agricultural workers: (1) dairy farm workers in the Texas Panhandle and (2) farmworkers and bodega workers in the Rio Grande Valley. Crop, bodega, and dairy farm workers perform distinct roles within agriculture, each with unique responsibilities and work environments. Crop workers focus on planting, cultivating, and harvesting fruits, vegetables, grains, and other plant-based products. Their tasks often involve operating machinery, irrigating fields, applying fertilizers and pesticides, and monitoring plant and orchard health (Tonozzi & Layne, 2016). Bodega or packhouse workers focus on sorting, grading, and packing fresh produce ready for distribution (Rodriguez et al., 2024). In contrast, dairy farm workers care for cattle raised for food. Their duties include feeding, cleaning, monitoring animal health, assisting with births, and milking dairy cows (Douphrate et al., 2013; Rovai et al., 2016). While crop work is typically seasonal and heavily influenced by weather patterns, livestock work tends to be more consistent year-round, requiring daily attention to animal welfare. The physical demands and risks also differ, with crop workers often exposed to chemicals and extreme weather, and livestock workers facing hazards related to animal handling and zoonotic diseases (Nguyen et al., 2018).
Texas Panhandle Dairy Farm Workers
Dairy workers are predominantly immigrant (Passel et al., 2014), Hispanic males (Adock et al., 2015), of approximately 30 years of age (Roman-Muniz et al., 2006), with limited English proficiency and formal education (Jenkins et al., 2009). Most agricultural workers are of Mexican descent (88.5%–97.1%; Jenkins et al., 2009; Liebman et al., 2016; Roman-Muniz et al., 2006) although in recent years there has been an increase in agricultural workers from the Quiché department in Guatemala (Rodriguez et al., 2018, 2020). Most immigrants find low-wage jobs in prominent dairy, farming, animal husbandry, and meatpacking industries, with little to no social support (Ramos et al., 2020). The modern U.S. dairy farm is a highly integrated agricultural system (Rotz et al., 2012). Whereas crop harvest is seasonal, dairy production is year-round, producing milk 24 hours a day, 7 days a week, and 365 days a year (USDA, 2013).
Texas Rio Grande Valley Bodega and Farmworkers
The Rio Grande Valley (RGV) is located in a rural and underserved U.S.-Mexico border region and home to 25,000 citrus acres, 5,000 onion acres, and 5,000 watermelon acres, as well as leafy greens, beets, carrots, and herbs among its major production items (International Fresh Produce Association, 2020). Similar to dairy workers, farmworkers and bodega workers residing in the RGV are predominantly immigrant, Hispanic middle-aged males (Rodriguez et al., 2024) with limited English proficiency (apart from Spanish, speaking indigenous languages such as Tzotzil, Tzeltal, or Nahuatl), limited opportunity for formal education attainment, and living in poverty (NCFH, 2021; Shrider et al., 2020; United States Census Bureau, 2021).
Overview of Projects
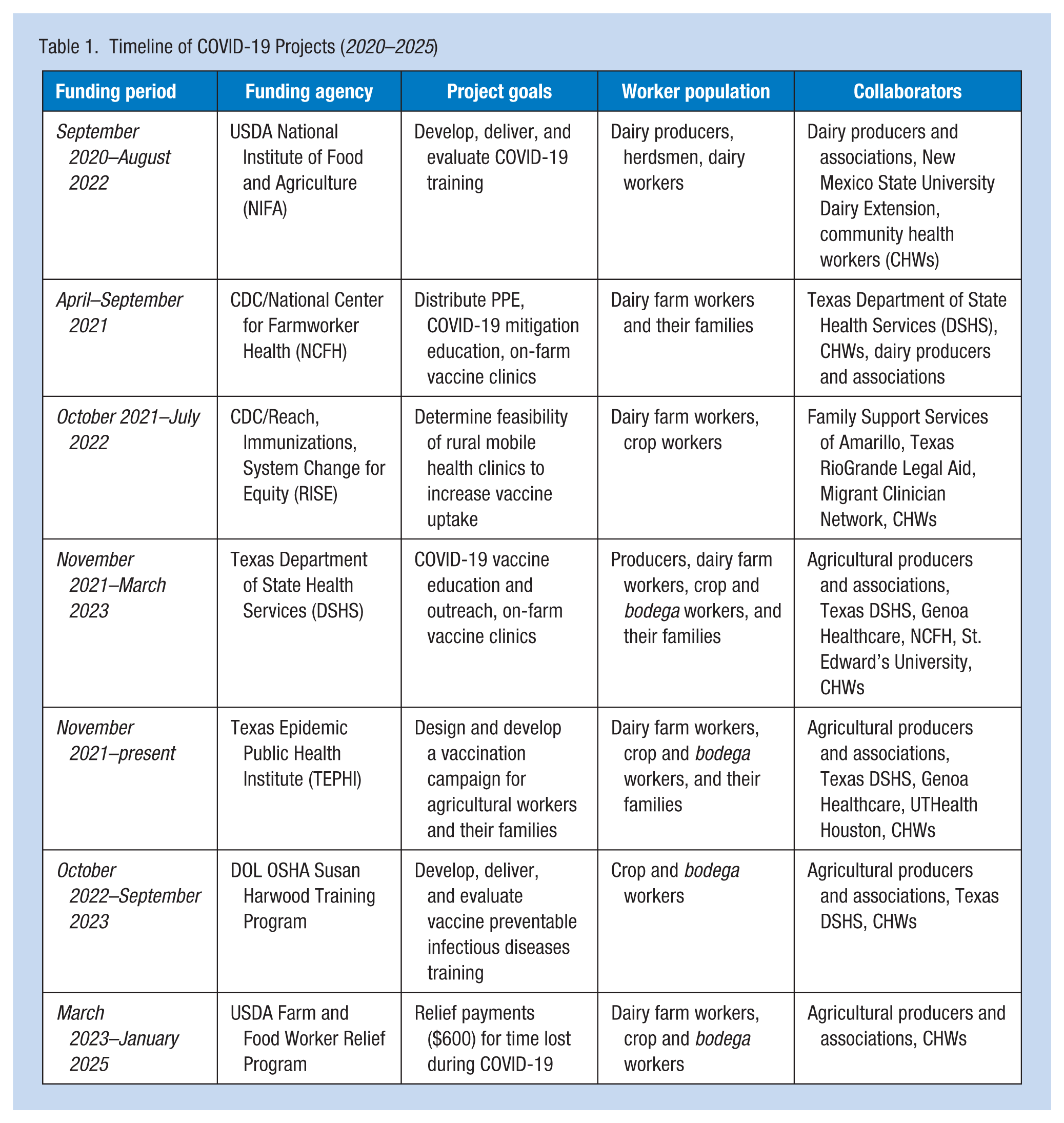
As outlined in Table 1, we sought funding from various state and federal agencies to employ COVID-19 pandemic responses among agricultural workers which included mitigation communication to the agricultural industry, PPE education and distribution, access to vaccinations, economic relief programs, and continued agricultural worker community support. This table also provides details about the goals of the project, funding source, worker populations, and our collaborators.
Timeline of COVID-19 Projects (2020–2025)
Early Mitigation Communications
Early in the COVID-19 pandemic (February 2020), our team studied current information and transmission mitigation strategies that could be applied in agriculture production working environments. This work resulted in an industry publication entitled, “What dairy farms must know about COVID-19” which was published in Hoard’s Dairyman, one of the largest trade magazines for the dairy industry, including dairy producers. This publication was followed by numerous efforts aimed at protecting the health, safety, and well-being of agricultural workers and their families as well as overcoming systemic barriers to healthcare access encountered by workers in rural agriculture communities located in health deserts.
PPE Education and Distribution
During the early stages of the pandemic, federal and state public health campaigns emphasized the importance of wearing masks in certain settings, such as crowded spaces or when illnesses were increasing in the community. Agricultural work practices, including both livestock and crop production, are often in open air settings where the wearing of masks may not be as necessary as compared to indoor work environments. However, our efforts in the arena of PPE usage concentrated on the selection of proper PPE and why masks are particularly effective in reducing the spread of the virus to others as well as protecting wearers from inhaling infectious particles, particularly in settings where agricultural workers may be in close proximity to others, such as carpooling to and from work, or living conditions where many workers share the same residence. This effort was funded by the CDC through the National Center for Farmworker Health (April–September 2021). Our outreach team distributed 1,000 PPE kits, delivered in-person education to nearly 950 agricultural workers, and facilitated on-farm vaccination events for 1,029 agricultural workers and their multigenerational household members.
COVID-19 Training Programs
Texas Panhandle Dairy Farm Workers
We developed training programs for dairy workers, herdsmen or supervisors, and producers to address concerns and reduce anxieties by providing accurate and up to date information about the coronavirus. Our team developed and evaluated two videos focused on: (1) COVID-19 health and safety transmission prevention at work and at home environments and (2) COVID-19 Vaccine Frequently Asked Questions (FAQs) answered by a bilingual a board-certified occupational medicine physician. All videos were available in English, Spanish, and translated and voiced into Guatemalan K’iche. In the past decade, our team has documented an increase in dairy farm workers working in the Texas Panhandle and Eastern New Mexico from the department or state of Quiché in Guatemala (Rodriguez et al., 2018, 2020). These training efforts were funded by the United States Department of Agriculture (USDA) National Institute of Food and Agriculture (NIFA) to develop, deliver, and evaluate these COVID-19 training resources among 237 dairy farm workers in Texas (September 2020–August 2022).
Our findings indicated that the mean age of training participants was 38.1 (SD 12.3) years, with a wide range of 18 to 78 years, and 83.5% were males identifying as Hispanic (92.8%; Table 2). The majority reported Mexico (75.1%) as their country of origin from the states of Chihuahua (17.3%) and Hidalgo (16.2%). Spanish (80.2%) was the primary language spoken, with 42.6% of participants reporting a middle school education at most. Participants lived in the U.S. for a mean of 13.0 (SD 11.4) years, ranging from 3 months in the country to 50 years of residency. Most reported working as a milker (34.6%) or conducting other general duties (33.3%) around the dairy farm, with a mean of 8.3 (SD 8.9) years of dairy work experience ranging from 1 month of experience to 50 years.
Demographic, Occupational Characteristics, and COVID-19 Experiences Among Dairy Workers in Texas (n = 237)
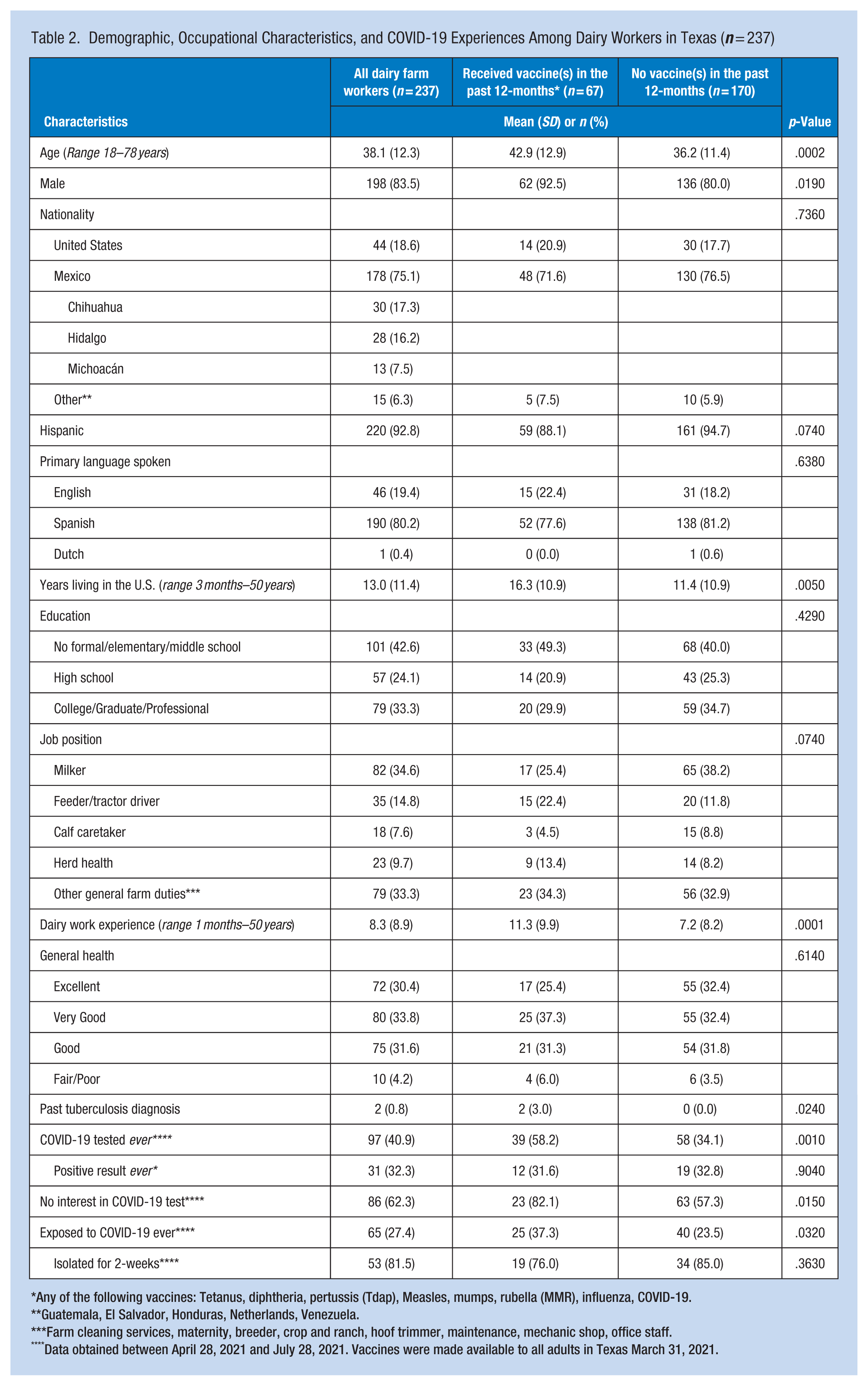
Any of the following vaccines: Tetanus, diphtheria, pertussis (Tdap), Measles, mumps, rubella (MMR), influenza, COVID-19.
Guatemala, El Salvador, Honduras, Netherlands, Venezuela.
Farm cleaning services, maternity, breeder, crop and ranch, hoof trimmer, maintenance, mechanic shop, office staff.
Data obtained between April 28, 2021 and July 28, 2021. Vaccines were made available to all adults in Texas March 31, 2021.
Both groups of dairy workers who reported receiving and not receiving any vaccines in the past 12 months had statistically significant knowledge mean scores (p < .05). Of note, on average, the group reporting no vaccines increased their scores (pre- to post-test) 9.3 points, whereas the group reporting vaccines increased to a lesser extent, by 7.3 points. There were some differences between the groups. The group who reported receiving vaccine(s) in the past 12 months were more likely to be older males with longer residencies in the U.S., more years of dairy farm work experience, reported interest in COVID-19 testing (survey administered between April and July 2021), and were more likely to report having been exposed to COVID-19 on the farm.
Among participating dairy farm workers, the mean score on the pretest given before training was 77.0% (SD 15.2), and the mean score on the same test given immediately after the video training was 85.3% (SD 15.1; p < .05; Table 3), resulting in an effect size estimate of 0.55, indicative of a medium learning effect. There were differences (p < .05) between and within pre- and post-test scores across individuals with no formal/elementary/middle school and high school education levels, individuals who reported no vaccine(s) received in the past 12 months, workers with less than 3 years and more than 5 years of dairy farm work experience, and all job positions, except herd health.
Levels 1 and 2 Training Effectiveness Evaluations Among Dairy Farm Workers in Texas
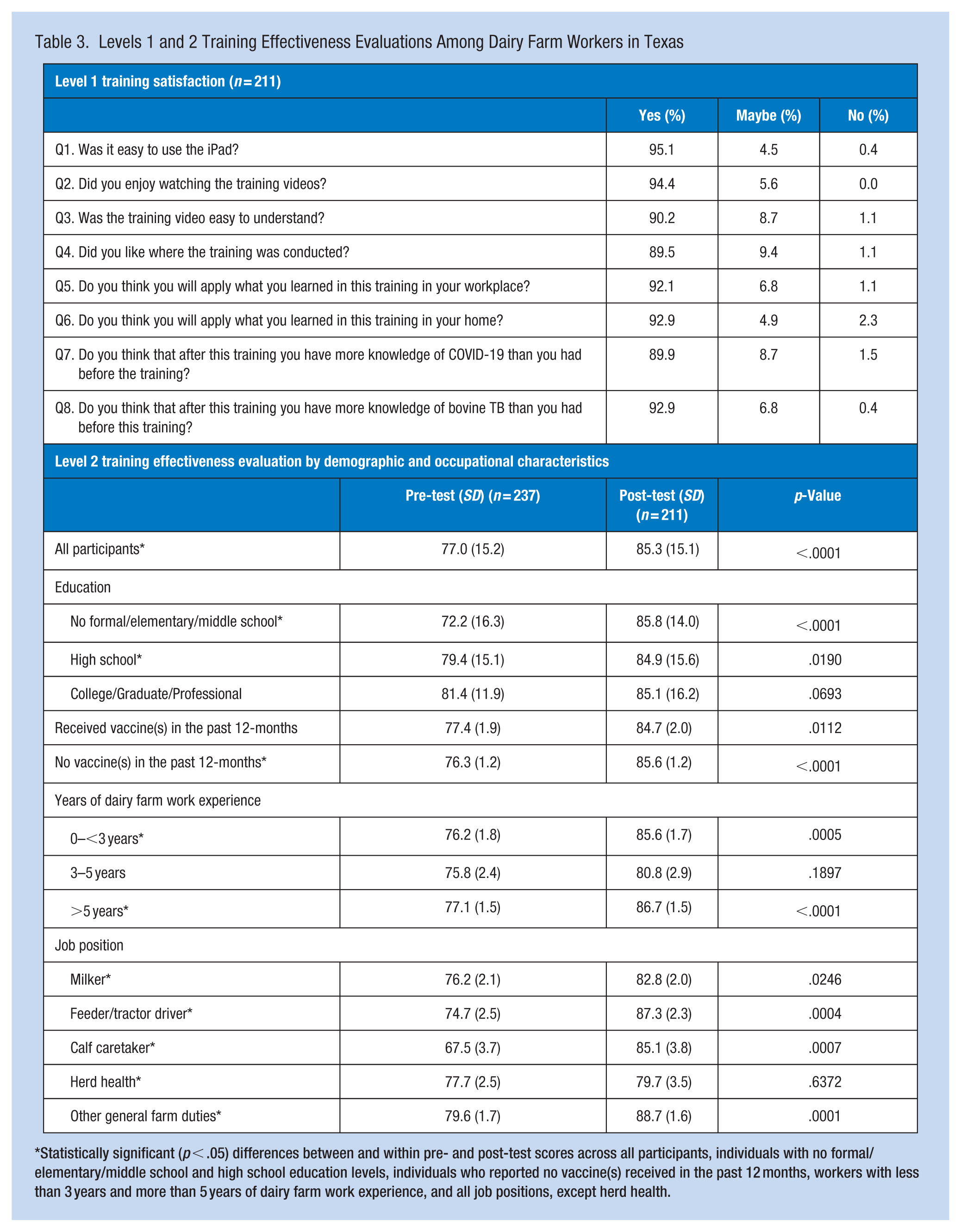
Statistically significant (p < .05) differences between and within pre- and post-test scores across all participants, individuals with no formal/elementary/middle school and high school education levels, individuals who reported no vaccine(s) received in the past 12 months, workers with less than 3 years and more than 5 years of dairy farm work experience, and all job positions, except herd health.
Texas Rio Grande Valley Bodega and Farmworkers
As we navigated the pandemic, we recognized that other vaccine-preventable infectious diseases were being overlooked, and as public health professionals, we were missing critical opportunities to advocate for vaccines and boosters. As a result, we leveraged funds from the U.S. Department of Labor (DOL) Occupational Safety and Health Administration (OSHA) Susan Harwood Training Program (October 2022–September 2023) to create, deliver, and evaluate a 1-hour culturally, linguistically (English, Spanish, Nahuatl), and literacy-appropriate training vignette focused on transmission prevention of influenza, tetanus, tuberculosis, hepatitis A, hepatitis B, and COVID-19 for crop and bodega workers and employers in the Rio Grande Valley (RGV). A non-random sample of 1,043 (1,006 agricultural workers and 37 production managers) were recruited and trained at farms and bodegas in the RGV. For crop and bodega workers, the mean score on the 10-item pretest before training was 67.8% (SD 17.5), and the mean score on the same test immediately after the video training was 77.2% (SD 17.9; p < .05), resulting in an effect size estimate of 0.53, indicative of a medium learning effect. There were differences (p < .05) between and within pre and post-test scores across gender, all education levels (except “No education”), language, ethnicity, and ever diagnosed with COVID-19 (Rodriguez et al., 2024).
Access to COVID-19 Vaccine
Texas agricultural workers were not eligible for COVID-19 vaccination until Phase 2 (March 31, 2021; Texas Department of State Health Services, 2021). We anticipated that broad eligibility and early dose shortages, combined with historical barriers to healthcare faced by agricultural workers in rural areas, would complicate access. We recognized that vaccine education needed to be paired with vaccine availability and access. One significant barrier we identified was transportation to and from vaccination sites. Our team leveraged funds from the CDC through Reach, Immunizations, System Change for Equity (RISE; October 2021–July 2022), in collaboration with Family Support Services of Amarillo and Texas RioGrande Legal Aid, to determine the feasibility of rural mobile health clinics in increasing vaccine uptake among agricultural workers in the Texas Panhandle. Certified Community Health Workers (CHWs) administered surveys to 118 dairy farm workers and crop workers to assess social support, living conditions, occupational exposures, vaccination status, and preferred methods for receiving health services. Our findings indicate that economic hardship is a significant barrier to having a primary care provider, which in turn limits vaccine access (p < .001). This initiative led to the creation of Sembrando el Sueño. Although the program was discontinued in 2024 due to funding cuts, it provided essential services to agricultural workers in the Panhandle, including transportation to and from clinics and pharmacies, emergency medical funds, and healthcare advocacy and navigation.
Our team continued to advocate for improved vaccine access for agricultural workers and their families, recognizing the need to remain flexible and adapt to evolving circumstances throughout the pandemic. Funding from the Texas Department of State Health Services (DSHS) enabled us to implement on-farm vaccine clinics for workers and their families, conduct door-to-door vaccine education, and launch a social media campaign promoting vaccine awareness (November 2021–March 2023). This outreach effort was delivered in three complimentary phases.
Phase 1 (November 2021–August 2022)
Our team facilitated on-farm COVID-19 vaccine clinics (1st dose, 2nd dose, 55+ boosters, bivalent boosters) for 1,200 agricultural workers and their families in the RGV and Panhandle. As new community needs were recognized, we began including pediatric COVID-19 vaccines, influenza, pneumonia (65+ as well as high-risk individuals), tetanus, diphtheria, pertussis (Tdap), measles, mumps, and rubella (MMR), hepatitis A, hepatitis B, as well as basic preventative health screenings (weight, height, blood pressure checks, at-home COVID-19 tests, distribution of PPE, and information regarding local low-cost health services).
In addition, brief surveys were administered throughout various COVID-19 education and vaccine clinic events on farms: (1) among dairy farm workers in the Panhandle (September 2020–March 2021) and (2) among citrus farmworkers in the RGV (December 2021–January 2022). Compared to citrus farmworkers in the RGV, dairy farm workers in the Panhandle were younger males originating from Mexico under an H-2A temporary agricultural guest visa and less likely to be COVID-19 vaccinated (Table 4). In the Texas Panhandle, 70.6% of dairy workers who received on-farm COVID-19 prevention and vaccine education indicated they were “Extremely likely” to get the COVID-19 vaccine. While there is no comparison data for citrus farmworkers in the RGV, most surveyed workers indicated no vaccine hesitancy (78.6%). However, a small group of surveyed workers listed side effects, fear of getting COVID-19 disease from the COVID-19 vaccine, distrust in the government, perceived ineffectiveness of the vaccine, and conflicting work schedules as barriers to receiving the COVID-19 vaccine.
Demographic and Occupational Characteristics and Vaccine Insight of Dairy Farm Workers in the Texas Panhandle (September 2020–March 2021; n = 199) and Citrus Farmworkers in the Rio Grande Valley (December 2021–January 2022; n = 109)
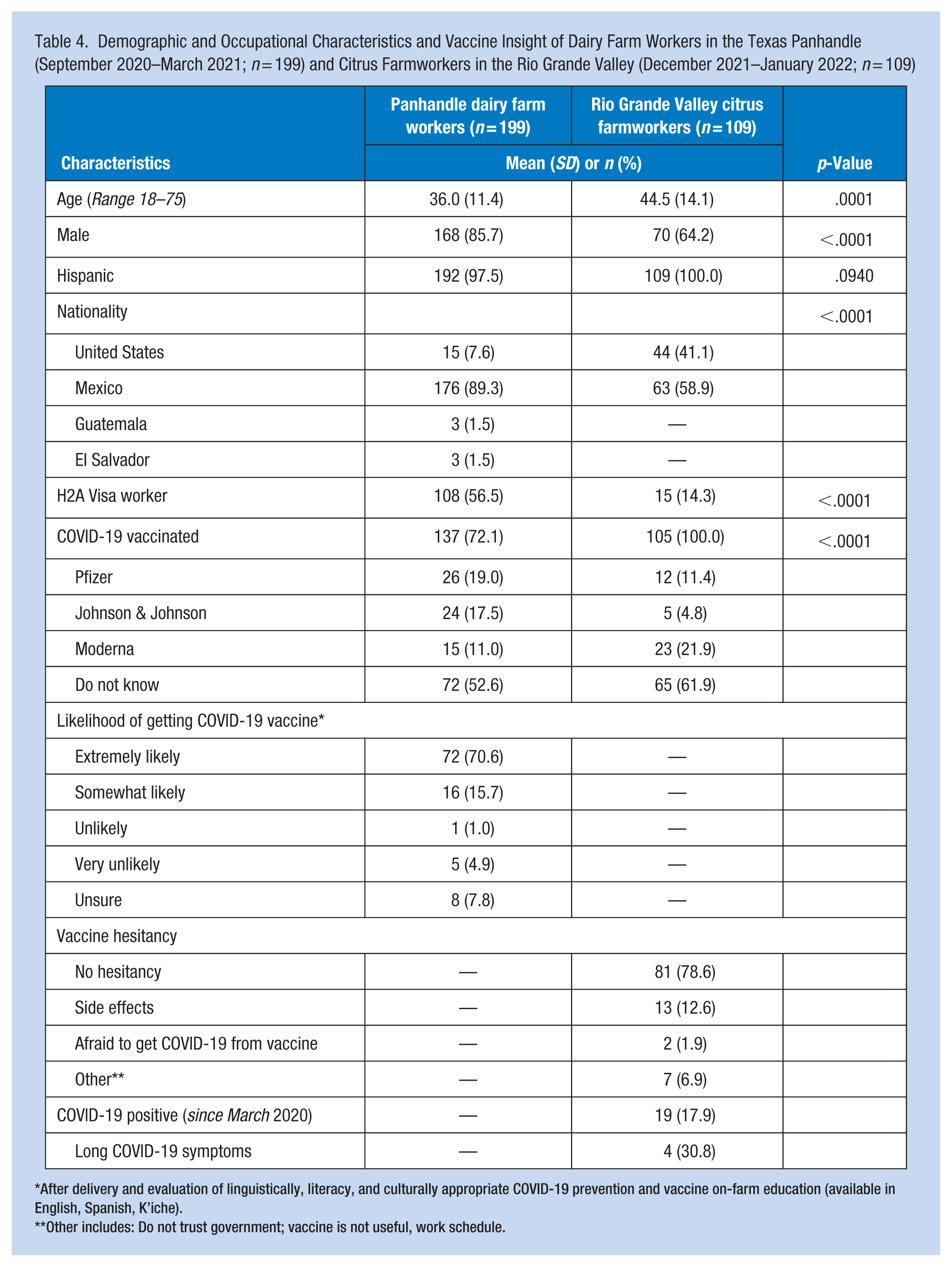
After delivery and evaluation of linguistically, literacy, and culturally appropriate COVID-19 prevention and vaccine on-farm education (available in English, Spanish, K’iche).
Other includes: Do not trust government; vaccine is not useful, work schedule.
Phase 2 (August 2022–March 2023)
In Phase 2, CHWs conducted door-to-door visits aimed to educate entire families and assist them in scheduling vaccine appointments at local clinics and pharmacies. A total of 4,778 door-to-door vaccine education visits across 31 rural counties and 61 rural zip codes in Texas.
Phase 3 Social Media Content (December 2022–March 2023)
By this stage of the pandemic, most individuals willing to be vaccinated had already received their doses. Our team was aware of misinformation and disinformation circulating on social media platforms commonly used and trusted by agricultural workers and their families. To counter these inaccuracies, we partnered with students and faculty from the Department of Visual Studies at St. Edward’s University in Austin, Texas, to develop bilingual training vignettes in English and Spanish. These short videos addressed vaccine concepts, debunked myths such as microchips, magnets, altered DNA, fertility concerns, and provided information on other infectious diseases, including influenza, tetanus, tuberculosis, hepatitis A, hepatitis B, and monkeypox. The resulting educational campaign, Café con Comunidad, was disseminated using QR codes printed on coffee mugs and hydration bottles distributed to workers during outreach events.
COVID-19 Economic Relief Program
Agricultural workers faced significant economic challenges during the pandemic, including job insecurity, loss of income due to unpaid sick leave, and the ripple effect of supply chain disruptions. Our team leveraged funds from the United States Department of Agriculture (USDA) Farm and Food Worker Relief Program to provide agricultural workers with a one-time $600 relief payment for any wages and time lost during the COVID-19 pandemic (March 2023–September 2024). Our team was able to mobilize quickly and reach over 4,600 agricultural workers across the RGV, Panhandle, and Eastern New Mexico. To complement these efforts, our communications team produced a short documentary that highlighted the lives and struggles of agricultural workers and their families during the pandemic, as well as the impact of community outreach initiatives, including the USDA economic relief program.
Continued Agricultural Worker Community Support
Our team continued supporting producers, growers, agricultural workers, and their multigenerational families as pandemic efforts wound down and funding ended. Although this is an extremely resilient community, we aimed to ensure they had access to resources during this recovery period. The Texas Epidemic Public Health Institute (TEPHI) is an institute funded by the State of Texas legislature (established on November 7, 2021) headquartered at UTHealth Houston School of Public Health. Multidisciplinary collaborations were formed across three “Readiness” TEPHI Working Groups: (1) Rural and Border Communities, (2) Small Rural Healthcare Systems, and (3) Food Chain Preparedness. One objective guiding the Small Rural Healthcare Systems working group was to create rural county resource lists aimed to guide agricultural workers and their families seeking access to limited and valuable resources, such as testing sites, vaccination sites, food pantries, social services, transportation services, childcare, and economic relief, and funeral assistance, among others. CHWs in rural farming counties highly impacted by COVID-19 disseminated >30,000 resource lists in the RGV, El Paso, and the Panhandle. On March 1, 2024, Juntos en Salud working group was formed to design and develop a vaccination campaign for agricultural workers and their families in the RGV, Panhandle, El Paso; and implement social media educational components of the developed campaign. The campaign promotes recommended vaccines for all family members, including standard childhood vaccines (e.g., MMR, DTaP, Varicella, Hepatitis A and B), adult vaccines for agricultural workers (e.g., Td/Tdap, MMR booster), vaccines for special populations, such as pregnant women (i.e., Tdap, RSV, flu) and seniors (i.e., RSV, flu, pneumococcal polysaccharide [PPSV23], pneumococcal conjugate [PCV13], shingles). Juntos en Salud continues to provide on-farm vaccinations, promote vaccine education through social media, and expand into other health initiatives for agricultural workers such as point-of-care testing and early skin cancer detection.
Discussion
During the pandemic, worker health, safety, and well-being became paramount for food supply sustainability. Farming operations in the U.S. remain and will continue to make a vital economic contribution and source of food security (Adock et al., 2015; Dimitri et al., 2005). A threat to the future of agriculture, including the health, safety, and well-being of workers and their families, threatens a nation’s security. Farming operations have seen a fair share of threats in the past, from the most recent pandemic to economic recessions, constant tariff revisions, zoonotic diseases (e.g., bovine tuberculosis, highly pathogenic avian influenza A H5N1), climate change and subsequent extreme weather events, and immigration enforcement and deportations disrupting labor supply (Dimitri et al., 2005; USDA, 2016). This professional practice report summarized lessons learned from field outreach and training activities, emphasizing the cognitive dissonance between public health responsibilities and actual responses among agricultural workers. To address this gap, we must prioritize building relationships, strengthening capacity, and improving delivery methods before the next public health emergency.
Lessons Learned for Professional Practice
Vaccine Delivery On-Farms
At the time of vaccine delivery, on-farm clinics documented overcoming well-known systemic barriers to healthcare access like transportation to-and-from medical service facilities, conflicting work-life schedules (working from dawn-to-dusk and following the harvest), lack of childcare, cost of vaccines or health services, lack of health insurance coverage, as well as linguistic and cultural challenges associated with health literacy (Rodriguez et al., 2023). However, on-farm events hosted with large teams of nurses, public health practitioners, and academics did not eliminate barriers to healthcare access. Still, they stressed that barriers, like lack of trust in medical and governmental officials and fear of law and deportation agencies continue to exist. Based on anecdotal observations from these events, some workers failed to show, some left the event without getting vaccinated, and others were reluctant to complete vaccine in-take forms and provide physical addresses, telephone numbers, and dates of birth. Barriers to vaccine administration were exacerbated when identification cards were required, and densely worded, time-consuming intake forms were available in English only. As a result, protocols were expeditiously modified by local public health officials to no longer require identification cards, condense the intake form, make all forms available in Spanish, and leverage support from bilingual community partners and certified Community Health Workers (CHWs) to help workers and their families correctly complete intake forms. “Taking the pulse” of fieldwork methods, collecting information on participant comfort and barriers, as well as setbacks in worker access and perceived benefits of research and outreach interventions, is vital. This, in turn, built trust, acceptance, and open dialogue between all parties. Informed preparation for on-farm events can impact overall care and make-or-break success of interventions.
Vaccine Hesitancy and Education
On-farm vaccine education was met by workers with both endorsement and reservations. Gaps in infectious disease awareness and education among agricultural workers became especially apparent during the pandemic and were exacerbated by mis- and disinformation acquired from trusted social media platforms like Facebook and WhatsApp (Goldsmith et al., 2022; Suarez-Lledo & Alvarez-Galvez, 2021). Anecdotal observations from training sessions suggested that workers had considerable health concerns regarding vaccine safety among children, their elderly parents, pregnant women, and individuals with underlying health conditions like diabetes and heart issues. A subset had questions about the vaccine’s ability to “change their DNA” or to “introduce magnetism and microchips,” as well as questions associated with religious beliefs such as vaccines carrying “the mark of the beast,” the end of times vaccine, and questions concerning the ethical use of fetal cells in vaccine manufacturing. Leaning on field experience from a decade of research, outreach, and training initiatives among agricultural workers, our team was able to meet workers where they were not just physically but in terms of their deeply rooted cultural beliefs, health literacy, language(s), and familismo (loyalty to family). Most importantly, training and enabling culturally competent CHWs to serve their own agricultural communities was a vital approach to successfully rolling-out all outreach and training activities. Despite the high levels of uncertainty the pandemic created, these community members were able to bring comfort, familiarity, consistency, and empathy, all while delivering data-driven vaccine education.
Industry Support
Securing agreement from participating agricultural producers to host was crucial. The effectiveness of on-farm vaccine education and clinics facilitated by outreach personnel can be attributed to transparent communication, intentional collaborations, and active inclusion of agricultural producers and their management team. Access to agricultural workers and their families is delicate, strenuous, and a privileged experience. This access comes with higher responsibilities of respect for workers and their private place of employment. Additionally, having common goals, clear communication, and resource support from local public health departments that serve agricultural communities can make or break public health emergency initiatives like the COVID-19 pandemic. Partnerships with regional/local health departments should be established and maintained before trauma informed and culturally responsive approaches to emergency vaccination, testing, or surveillance efforts are needed to allow for a faster, organized, and trusted centralized response during time-sensitive health emergency events.
Applications to Professional Practice
Agriculture producers, workers, and their families play an essential role in our society and are entitled to participate actively in our public health research, outreach, and training initiatives. We must draw on lessons learned from past health emergency responses among agricultural workers to prevent repeating the same mistakes during future epidemics or pandemics. As a nation, we strengthen our food supply security by prioritizing and investing in agricultural workers’ health, safety, and well-being. Preparation must include building genuine and transparent relationships with agricultural producers, workers, their families, and their rural communities to promptly address critical public health needs and inequities. The recent detection of avian influenza among cattle on dairy farms and the confirmed transmission to dairy farm workers clearly demonstrate the urgent nature of building relationships. Public health departments should receive the necessary resources to strengthen community preparedness and response in rural regions, leveraging collaborative partnerships with community-based organizations, academic institutions, and rural clinicians. Future efforts and investments should prioritize building resilience and preparedness through comprehensive training programs, PPE stockpiling, mobile units for health and vaccine delivery, research and education, equitable health services, and outreach to agricultural workers and their multigenerational families in rural communities. This, in turn, strengthens the community’s ability to respond effectively to future public health emergencies.
Footnotes
Acknowledgements
The authors thank the Texas International Produce Association in Mission, Texas, for their encouragement and support in every step of these programs and initiatives. The authors would also like to thank the leadership at all the farms and bodegas who graciously hosted our team to deliver these programs as well as all the community coordinators in the Panhandle, RGV, and El Paso and public health students who helped make all these initiatives a reality. Truly this work could not have been accomplished without them. Most importantly, the authors thank the agricultural workers and their families who sacrificed their health, safety, and well-being to feed the world and, simultaneously, keep our economy strong through unprecedented times. Last, the corresponding author would like to thank her partner, Grady Young, and her fur-kids, Shiner and Tejas, for their love, encouragement, and patience throughout multiple work trips and long hours of work away from home during highly uncertain times.
Conflict of Interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This material was produced under grant number 6 NU50CK000567 Center for Disease Control and Prevention/National Center for Farmworker Health; HSS001043100001 from the Texas Department of State Health Services/Texas A&M University Health Science Center; United States Department of Agriculture/National Center for Farmworker Health; S.B. 1780, 87th Legislature, 2021 Reg. Sess.; SH-38960-22-60-F-48 from the Occupational Safety and Health Administration (OSHA), U.S. Department of Labor. It does not necessarily reflect the views or policies of the U.S. Department of Labor, nor does mention of trade name, commercial products, or organizations imply endorsement by the U.S. Government or the Southwest Center for Occupational and Environmental Health (SWCOEH), the Centers for Disease Control and Prevention (CDC) National Institute for Occupational Safety and Health (NIOSH) Education and Research Center (grant #T42OH008421) at The University of Texas Health Science Center at Houston (UTHealth Houston) School of Public Health.
Ethical Approval
All human subjects research and outreach were approved by The University of Texas Health and Science Center at Houston Committee for the Protection of Human Subjects (CPHS).
