Abstract
Background
Obesity is a recognized risk factor for work-related injuries (WRI). Despite the inherent safety hazards associated with farm work, research on obesity among farmers is limited giving little guidance to occupational health providers on obesity as a risk factor in farm WRI. This study evaluated the association between obesity and farm WRI.
Methods
Cross-sectional data were collected from farmers (n = 100) in Kentucky, Tennessee, and West Virginia. Data included a survey (demographic data, farm factors, health indicators, occurrences of work-related injuries consistent with the definition of Occupational Safety and Health Administration [OSHA] recordable injuries) and direct anthropometric measures (height, weight, and waist circumference). Logistic regression was used to model any work-related injury, injuries consistent with the definition of OSHA recordables (herein called OSHA-recordable injuries), and recurrent injuries occurring during farm work performance on body mass index (BMI) and waist circumference.
Findings
Twenty-five percent of the participants reported any injuries, and 18% reported OSHA-recordable injuries. Farmers with a BMI ≥30 kg/m2 had 3 times the risk for OSHA-recordable injuries and 5 times the risk for recurrent injuries. No significant relationship was identified between waist circumference and farm WRI.
Conclusion
This study provides evidence that increased BMI is a safety risk for farmers. Prospective studies with a larger sample are needed. Occupational health nurses and providers should educate farmers on the potential safety risk of obesity and implement weight management programs addressing obesity in farmers.
Background
Farming remains one of the most dangerous occupations in the United States. In 2019, crop and animal production resulted in 410 fatal injuries (Bureau of Labor Statistics [BLS], 2020b). In addition, crop and animal production workers have higher incidence rates of nonfatal injuries (5.3 and 5.6/100 full-time equivalent [FTE] workers, respectively) compared with the incident rates of all U.S. workers (3.0/100 FTE workers) (BLS, 2020a). However, Leigh et al. (2014) estimate that 73.7% of crop production injuries and 81.9% of animal production injuries are unreported due to small and family-owned farm reporting exemptions. The economic cost of farm work-related injuries (WRI) is unknown, but Landsteiner et al. (2016) estimated the cost as $21 to $31 million in Minnesota alone.
Obesity has been identified as a risk factor for WRI across industries (Gu et al., 2016; Rommel et al., 2016). Obesity prevalence among U.S. farmers has doubled since 1960 (Gu et al., 2014). However, articles in two systematic reviews with meta-analyses (Jadhav et al., 2015, 2016) identifying risk factors and emerging risk factors for agriculture injuries did not include obesity as a risk factor. King et al. (2016), using data from the Saskatchewan Farm Injury Cohort, reported an increase in farm WRI in women farmers who were overweight (n = 280), but not if they were obese (n = 190). Obesity was identified as a protective factor in women, limiting the duration, intensity, and type of farm work performed.
Interventions to prevent farm WRI need to address both modifiable personal risk factors and job factors that are most likely to result in severe and costly injuries that affect farmers’ health, economic well-being, and quality of life (Bradley et al., 2016). In addition, recurrent injuries are also valuable indicators of a need for preventive interventions (Jadhav et al., 2016; Pietila et al., 2018). Evaluating injuries from these varying perspectives can add additional information for designing programs for injury prevention.
Current research on obesity and WRI in U.S. workers has focused primarily on obesity as increased body mass index (BMI). However, central or abdominal obesity, even with normal BMIs, has also been associated with adverse health effects, including increased mortality, decreased physical activity, decreased functional ability, and increased disability (Batsis et al., 2015). Research on central obesity and WRI in firefighters (McGill et al., 2013) supports a potential risk of injury in occupations with higher physical demands. With the increase in central obesity associated with aging, the increasing age of farmers, and the physical demands of farming, assessing the relationship between central obesity and farm WRI is important.
Limited evidence is available to guide practice related to obesity’s role in farm WRI and needed interventions. The purpose of this study was to examine the relationship between obesity and farm-related work injuries by (a) identifying the relationship between obesity and farm-related work injuries, injuries consistent with the definition of Occupational Safety and Health Administration (OSHA)-recordable WRI and recurrent injuries among farmers; and (b) determining the pattern of obesity, general or central, most associated with farm WRI.
Method
Design and Sample
This cross-sectional secondary data analysis examined BMI and waist circumference’s (WC) impact on the frequency and severity of WRI. One hundred farmers (owner/operator/managers) who were actively engaged in farm production were surveyed. Inclusion criteria included adults (≥18 years of age) who reported doing farm work, spoke and read English, and were able to complete the questionnaire. We designed recruitment strategies to encourage the participation of female and racially diverse farmers. Data collection was conducted from February through November 2014 at farm shows, farm association conferences, and farm supply stores in Kentucky, West Virginia, and Tennessee. Written informed consent was obtained from each participant. Each recipient received a $10.00 gift card for participating. The University of Kentucky Institutional Review Board approved this study.
Measures
Data collection consisted of a written questionnaire and anthropometric measurements, including height in centimeters, weight in kilograms, and waist circumference in centimeters. A questionnaire adapted from the Kentucky Farm Health and Hazard Surveillance Project Survey included (a) demographic data (age, gender, ethnicity, education, and income); (b) farm information (number of hours of farm work, hours off-farm work, farm commodities, acreage, household income from farm work); and (c) general health information (perceived health status, hours of sleep, tobacco and alcohol use, and current diseases) (Browning et al., 1998). Height and weight were directly measured using a portable Seca 213 stadiometer and Healthometer 844KL High-Capacity Digital scale. We performed device calibrations and participant measurements following the manufacture’s recommended procedures. Shoes and outerwear were removed for measurements. BMI was calculated using the formula: weight (kilograms)/height (centimeters)2. Standard World Health Organization (1995) categories were used to dichotomize BMI into obese (≥30 kg/m2) and non-obese (<30 kg/m2). Based on the U.S. National Institute of Health (NIH, 2000) guidelines, we defined central obesity as a waist circumference greater than or equal to 102 cm in males and 88 cm in females. Measurements were obtained following NIH (2000) guidelines using a Sammons Preston Gulick Anthropometric Tape Measure.
The outcome variables included (a) any work-related injures defined as the number of WRI occurring in the last 12 months; (b) injuries consistent with OSHA-recordable injuries defined as injuries resulting in a loss of consciousness, medical attention beyond first aid, a medical diagnosis by a health provider, missed time from farm work, or restricted farm work more than 4 hours (OSHA, 2001); and (c) recurrent injuries defined as two or more injuries sustained in the last 12 months.
Data Analysis
Statistical analyses were performed using IBM SPSS Version 22. Frequency distributions were used to describe the sample demographics and covariables. Bivariate analyses, including t-test and chi-square, were conducted to evaluate the relationship between the predictor and outcome variables and evaluate potential confounding variables. We conducted logistic regressions modeling the predictor variables BMI, referent non-obese (<30 kg/m2) and WC, referent non-obese (<102 cm in males and 88 cm in females) on the three WRI outcome variables. Examinations of predictors for multicollinearity revealed acceptable tolerance (0.689–0.913) and variance inflation factors (0.95–1.45).
Result
Table 1 presents a description of the sample demographic and study variables by BMI and central obesity status. Descriptive analysis revealed the participants (n = 100) were predominantly White (83%), male (69%), and greater than 55 years of age (46%). The majority were college-educated (69%), and nearly one third (31%) reported an income exceeding $80,000. Fifty-eight percent of the participants met the WC criteria for central obesity, and 39.4% exceeded 30 kg/m2 BMI. Males and females had equal rates of central obesity (58%), but males had a higher percentage of general obesity (42%) than females (32.3%). Central obesity increased with age ranging from 42.3% (18–34 years old) to 71.7% (>55 years of age); however, general obesity was more prominent (46.4%) in the 35 to 54 years age group. Non-White farmers exhibited higher rates of general (52.9%) and central obesity (82.4%) than White farmers (36.1% and 53%, respectively). Twenty-six percent of farmers reported an injury in the last 12 months, with 16% reporting multiple injuries. A total of 47 injuries were reported, with 18 of the injuries meeting the OSHA-recordable standard.
Demographic, Farm, and Health Characteristics Among a Sample of U.S. Farmers by Obesity Status (n = 100)
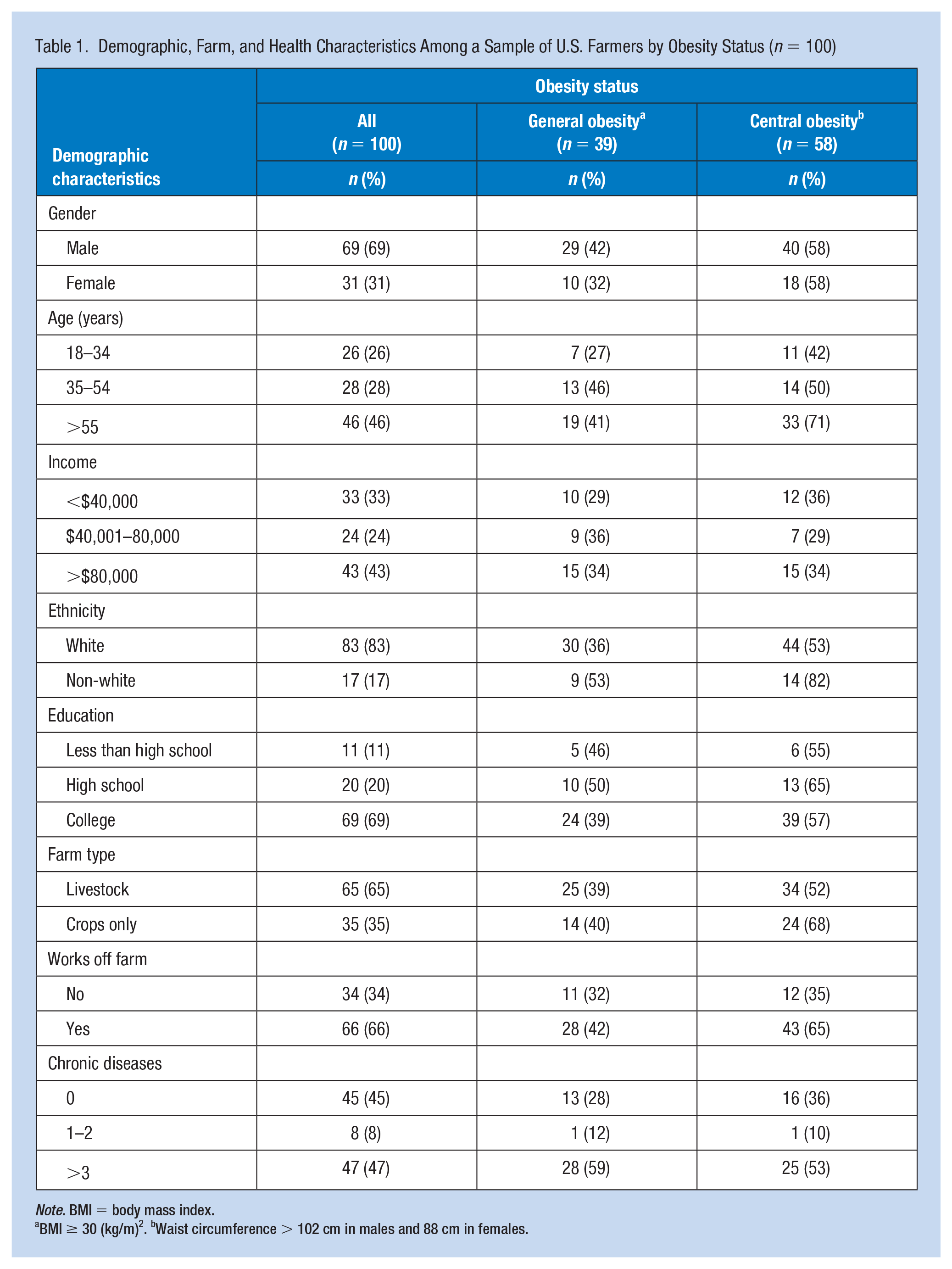
Note. BMI = body mass index.
BMI ≥ 30 (kg/m)2. bWaist circumference > 102 cm in males and 88 cm in females.
The bivariate analysis between BMI and the three dependent variables supported a significant association between BMI and OSHA-recordable farm injury occurrences (p = .034) and recurrent injuries (p = .007) (Table 2). There was no significant relationship between general obesity and any farm work-related injury occurrences (p = .071). Similarly, there was no significant relationship between central obesity and any farm WRI (p = .167), OSHA-recordable farm WRI (ρ = .768), or recurrent injuries (ρ = .272).
Bivariate Analysis of Demographic Characteristics, Farm and Health Predictors With Three Types of Farm Work–Related Injuries (n = 100)
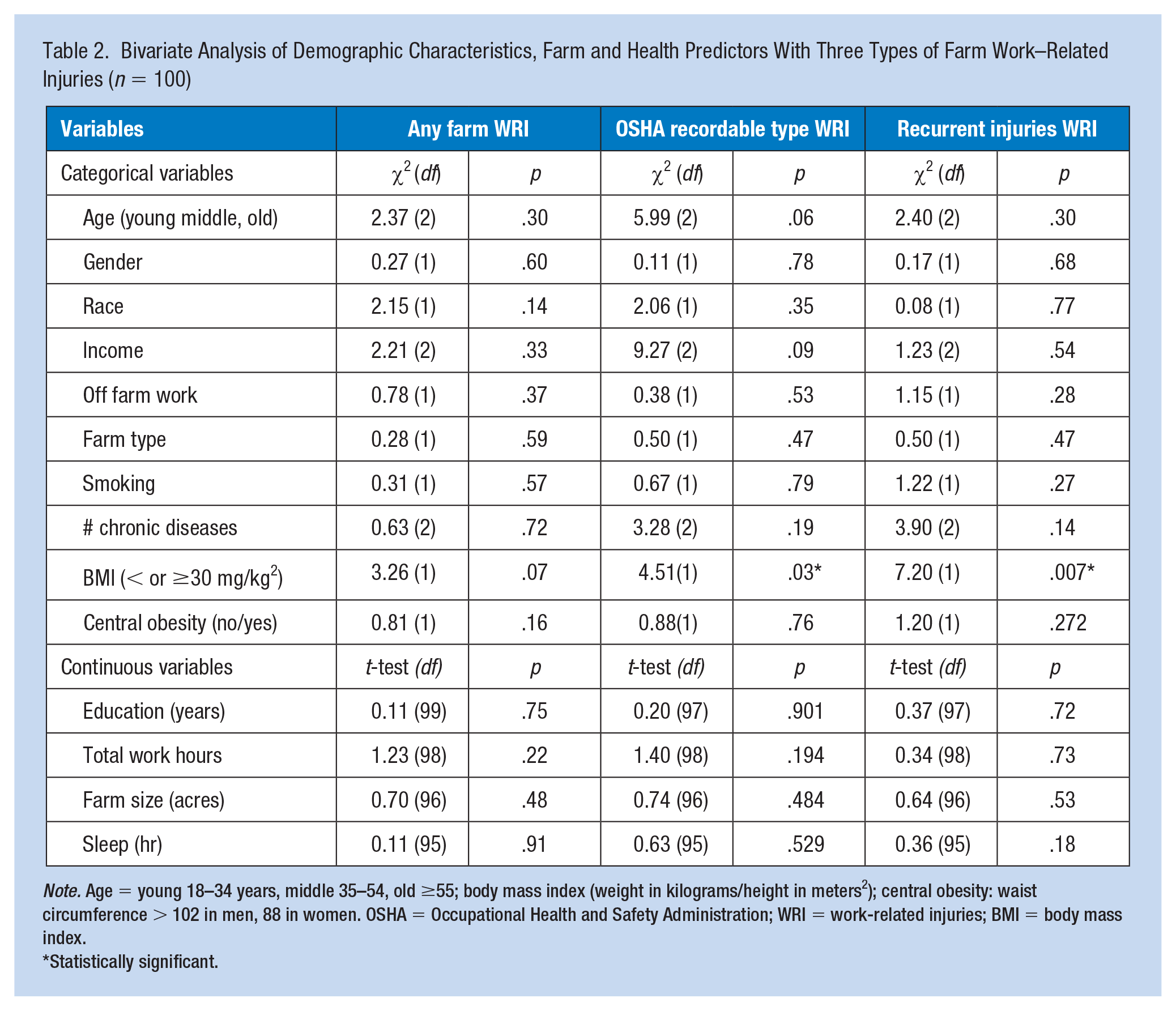
Note. Age = young 18–34 years, middle 35–54, old ≥55; body mass index (weight in kilograms/height in meters2); central obesity: waist circumference > 102 in men, 88 in women. OSHA = Occupational Health and Safety Administration; WRI = work-related injuries; BMI = body mass index.
Statistically significant.
Regression models were conducted to test the hypothesis that increased BMI and increased central obesity would increase the risk for WRI (Table 3). The model supported BMI as a significant predictor of OSHA-recordable injuries. This model classified 82% of the cases correctly and indicated that obese farmers had 3 times the risk of OSHA-recordable injuries as non-obese farmers (odds ratio [OR] = 3.03, confidence interval [CI] = [1.06, 8.68]). Based on Nagelkerke R2, BMI independently explained approximately 7% of the variance in OSHA-reportable injuries among farmers. The model also supported BMI as a predictor of recurrent injuries. Obese farmers were nearly 5 times more likely to sustain two or more injuries than non-obese farmers (OR = 4.91, CI = [1.42, 17.03]). BMI was not a significant predictor of any work-related injuries (OR = 2.287, CI = [0.921, 5.68]).
Unadjusted Regression Models Examining WRI in Farmers by BMI and Central Obesity (n = 100)
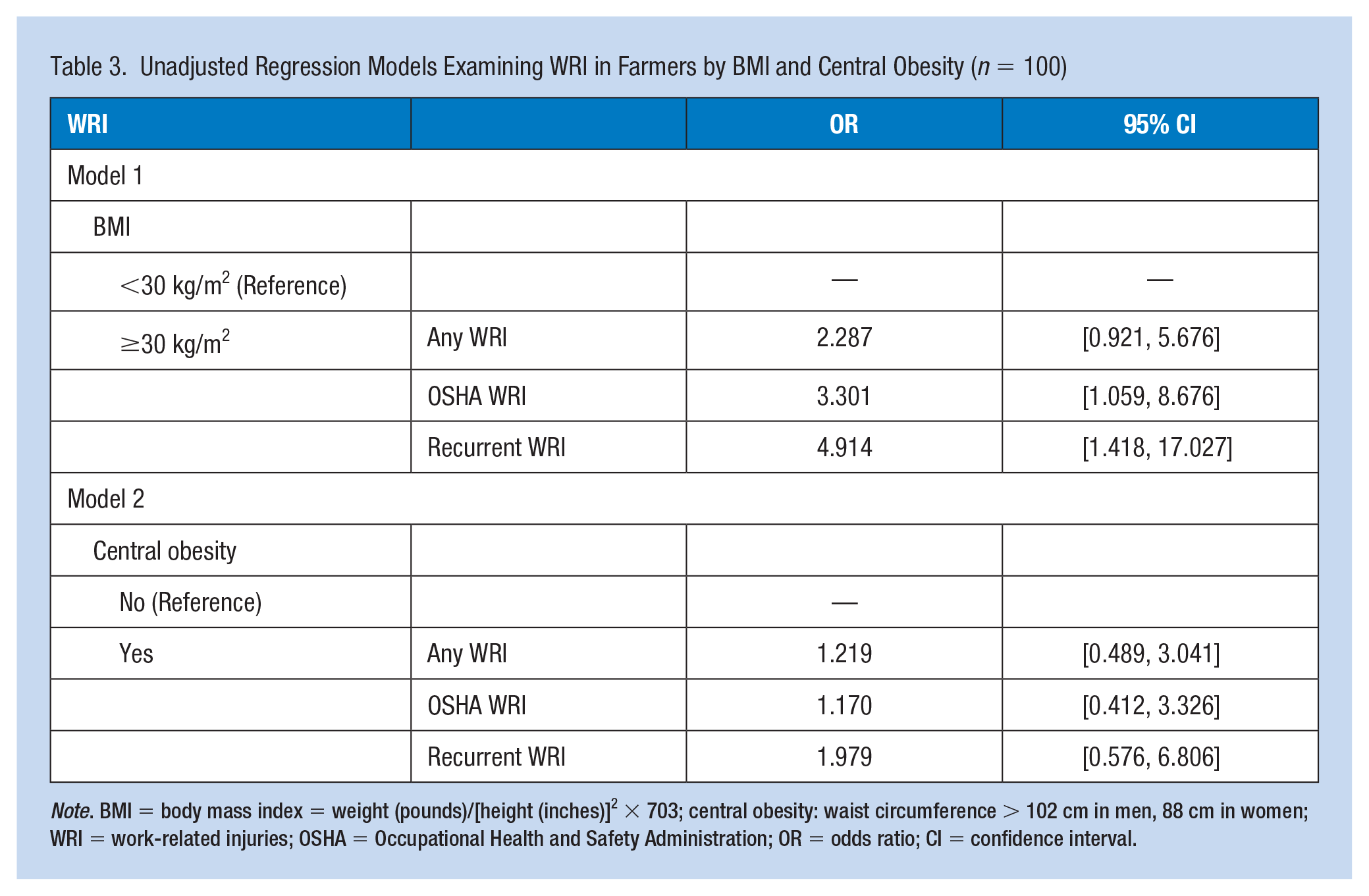
Note. BMI = body mass index = weight (pounds)/[height (inches)]2 × 703; central obesity: waist circumference > 102 cm in men, 88 cm in women; WRI = work-related injuries; OSHA = Occupational Health and Safety Administration; OR = odds ratio; CI = confidence interval.
Following the evaluation of BMI as a predictor of WRI, we conducted a binary logistic regression analysis of WC as a predictor of farm WRI, OSHA-recordable injuries, and recurrent injuries. Consistent with the bivariate analysis, findings did not support WC as a significant predictor of any farm WRI, OSHA-related injuries, or recurrent injuries.
Discussion
The agricultural industry’s injury rates rank among the highest in the United States, nearly double the average OSHA incident rate of 3.0/100 FTE workers across sectors (BLS, 2020a). However, very few family farms are required to report injuries to OSHA; therefore, farmer’s injuries are estimated to be much higher than reported. Findings in this study of farm owners, operators, and managers support high rates of injuries (n = 47) and recordable injuries (n = 18) despite the small sample size (n = 100). The study’s findings suggest general obesity, but not central obesity, may be a factor in these high rates.
Research on the impact of obesity on injuries in the farm sector is limited. However, past research supports an increased risk of injuries related to obesity among farmers, craftsmen, and tradespeople (Chau et al., 2009); public sector workers (Kouvonen et al., 2013); firefighters (Kuehl et al., 2012); and manufacturing workers (Pollack et al., 2007). Research exploring increased BMI’s effects on body biomechanics identifies altered functional abilities that could augment injury risk, including altered balance (Del Porto et al., 2012), limited mobility (Stenholm et al., 2010), and decreased flexibility, endurance, range of motion, muscle strength, and capacity to hold fixed positions (Capodaglio et al., 2010).
Specific to female farmers, King et al. (2016) identified falls, work performed in close proximity to hazards, repetitive manual tasks, and assisting in tasks where being overweight could contribute to injuries. Further research to identify the specific impact of weight on injuries is needed to identify work modifications to prevent and guide health care providers in assessing for injuries in overweight and obese workers. With the high physical work demands and risk exposures associated with farming, these alterations in function make obese farmers more susceptible to injury in the high-risk environment related to farm work.
This study’s findings did not support WC as a statistically significant predictor of increased risk for farm WRI. Multiple factors may have led to this outcome. While WC is associated with chronic illnesses, BMI is more highly associated with musculoskeletal problems, which alter functional ability and increase the risk of injury (Capodaglio et al., 2010; King et al., 2016; Stenholm et al., 2010). Research supporting the impact of central obesity on functional limitations is scant and primarily focused on elderly adults (Batsis et al., 2014; Germaine et al., 2015). However, Houston et al. (2005), in a prospective study of middle-aged adults (45–64 years), identified an increase in severe functional limitations and disability over 9 years in a biracial cohort with increased WC. The average age of participants in this study was 49 years, and an impact of WC may become apparent with aging and a longer duration of abdominal obesity. Also, physical activity may decrease the physical and functional limitations in older adults with central obesity (Germaine et al., 2015). The increased physical activity associated with farming may also contribute to a decreased effect on farmers. Future research, including prospective studies evaluating the temporal relationship between work injuries and the development of obesity over time among farmers, is needed.
The obesity rate in this sample of farmers (39.4%) was much higher than the 29.17% rate reported by Gu et al. (2014) among U.S. farmers. This finding may reflect response bias in the Gu study due to self-reported data. In addition, this study’s setting was Kentucky, Tennessee, and West Virginia, all states with historically higher rates of obesity (Centers for Disease Control and Prevention, 2020). Further research is needed using measured heights and weights to clarify the extent of the obesity problem among U.S. farmers and to evaluate variations in obesity rates among farmers in different regions and states.
Limitations of this study decrease the ability to generalize the findings. The potential for selection bias is high due to the lack of random sampling and self-selection into the study. Investigators observed potential participants who were obese avoiding the data collection booth. Respondent and recall bias could result from using written questionnaires and asking participants to report injuries over the last year. In addition, the use of a cross-sectional design with obesity and injury data collected simultaneously negates the ability to infer causality. Large prospective studies are needed to clarify the role of obesity and interactions between obesity and other risk factors in farm WRI.
Implications for Occupational Health Practice
This study’s findings add to the evidence for addressing obesity in farmers through workplace programming and thus have implications for occupational health practice. Health care providers for the high-risk farming population need to be aware of and educate farmers about the need for weight reduction to improve overall health and the potential for increased injury related to their occupation which may be exacerbated by obesity. Providers should recommend work modifications and safety instruction to decrease associated risk. Treatment and care plans should include interventions to promote weight loss and improve overall physical fitness. Farmers’ desire and tendency to continue farming long past retirement age can serve as a motivational factor for behavioral and lifestyle changes to address obesity. Occupational health nurses can assume leadership roles in developing education programs to increase awareness and knowledge of the impact of obesity on farmers’ safety. In addition, they should collaborate with farm associations, extension agencies, and occupational public health providers to directly provide education and interventions.
Applying Research to Occupational Health Practice
This research identifies general obesity as a potential risk factor for injuries among farmers. In addition, this study suggests that both general and central obesity may be more prevalent among farmers than past research has reported. Occupational health nurses should increase their focus on health promotion and injury prevention in this population through education of farmers on the potential role for obesity to increase work-related injuries, methods to prevent these injuries, and weight management techniques to decrease the risk. Developing coalitions with local farmer’s associations and extension agencies can promote outreach to this population.
Footnotes
Acknowledgements
The authors would gratefully acknowledge the technical support of Gail Spake, MA, Writing Support Specialist at Frontier Nursing University. In addition, they would like to acknowledge the guidance of the National League of Nursing’s Scholarly Writing Retreats in the preparation of this manuscript.
Conflict of Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Grants from the Vice President of Research Fund, University of Kentucky and NOISH Southeast Center for Agricultural Health, Injury Prevention supported this study. The contents of this paper have not been reviewed or endorsed by the funding agencies. The contents are the sole responsibility of the authors.
Author Biographies
Sharon Hunsucker, PhD, APRN, FNP-BC, is faculty at Frontier Nursing University. She contributed to the study’s design, data collection, and analysis, drafting of the original manuscript, and revisions based on the co-author’s recommendations.
Deborah B. Reed, MSPH, PhD, RN, FAAOHN, FAAN, is professor emeritus at the University of Kentucky College of Nursing. She contributed to the study’s design, data analysis, and editing all sections of the paper.
