Abstract
Background
Physical activity is a critical component of health.
Objective
We implemented a pilot project to determine feasibility of embedding activity tracker data within routine primary care visits among family medicine residency patients. This study also examined whether physician monitoring of and feedback concerning tracker improves exercise compliance and overall health.
Methods
Twenty-six participants received the FitBit Charge HR and were randomized into the self-monitoring (control) or intervention group for 12 weeks. The intervention group received weekly electronic health record (EHR) messages from their physician with feedback. The control group self-monitored activity.
Results
Data demonstrates patient interest in sharing exercise data with primary providers, patient-generated exercise data can be embedded within visits to personalize recommendations, and patient-physician data sharing is logistically feasible via the EHR.
Conclusion
Physicians can utilize activity trackers to potentially positively influence patients’ exercise. This research supports the shift toward personalized medicine by facilitating conversations and additional studies about fitness data.
Keywords
Background
Approximately 70 percent of U.S. adults are overweight or obese, posing a challenging public health dilemma. 1 These adults are at increased risk for developing heart disease, stroke, diabetes, and other serious health problems. The Centers for Disease Control & Prevention, American Heart Association, and American College of Cardiology all endorse physical activity as a critical component of weight-loss therapy, weight maintenance, and reduction of the aforementioned risks. 2 While studies have shown fitness-tracking devices and physician counseling can modify physical activity, no studies have examined the impact of physician monitoring of such data.3–6 Utilization of such data may allow physicians to provide personalized, data-driven fitness recommendations.
We implemented a pilot project to determine the feasibility of embedding activity tracker data within routine primary care visits among family medicine residency patients. 7 Additionally, we collected short-term health outcomes data, including compliance to daily recommended physical activity, patient-physician communication and quality of life measures. These measures were selected to determine whether physician monitoring of tracker data to the extent that was conducted in this study made a positive impact in addition to being feasible. 7
Methods
Participants
Inclusion criteria included patients attending the Family Medicine clinic who were 18 or older. Exclusion criteria were not having access to a computer or smartphone and pregnancy. There were no criteria related to amount of physical activity or body mass index (BMI).
Data Collection
Process metric data was collected to determine the overall feasibility of the intervention, and included: enrollment and attrition rates, patient communication logs, and participant feedback. 7 Feasibility was defined using several criteria (e.g. willingness of patients to enroll, follow-up rates, adherence/compliance rates, time needed to collect data, etc.), following the framework of Eldridge et al. 7 Additionally, health assessment data was collected using the Perceived Stress Scale (PSS, Supplement 1), 8 Medical Outcomes Survey (MOS), 9 and the Exercise Motivations Inventory (EMI, Supplement 2). 10 Participants received a FitBit Charge HR, a wearable activity and heart rate tracking device, at no charge for the 12 week duration of the study. We used the SmartTrack™ feature to automatically recognize and select continuous movement activities as exercise. The FitBit Charge HR has been shown to have approximately 84% bpm (beats per minute) concordance with an EKG. 11
Procedures
This study was approved by the Northwestern University Institutional Review Board. Patient participants were assigned a username and password to synchronize device data to their computer or smartphone. During the initial visit, participating patients were counseled by 2 primary physicians regarding CDC exercise and heart rate goals (150 minutes per week with a target heart rate of 50-70% of maximum heart rate, calculated for each participant), as well as provided with a handout. 12 At the initial and final 12 week visit, subjects completed the Perceived Stress Scale, Exercise Motivations Inventory, and Medical Outcome Survey.
In total, 26 patients were randomized by arbitrary computer sorting of participant number into either the Intervention (13) or Control (13) group (Figure 1). 13 Recruitment size was limited by time available in the resident clinic. FitBit data is automatically uploaded from the device to an online portal. Participant Fitbit data for both groups was analyzed weekly by the primary physicians, who then sent a standardized message to participants of the intervention group through the secure EHR patient portal system indicating whether they achieved CDC exercise goals for minutes and/or heart rate. Control group participants did not receive any message.

CONSORT Flow Diagram of Study Participants.
Results
Process Data
1 participant discontinued participation due to an allergic reaction, while over the course of 12 weeks 9 Control group members were lost to follow up (Figure 1), and 5 Intervention group members (Figure 1). It took approximately 5 minutes per week to review one participant’s activity data and send the standardized message. This is less than the average 15-30 minute in-person appointment.
Health Assessment Data
To explore potential baseline differences between the control and intervention groups, a battery of health assessment data (MOS, EMI, and PSS) were analyzed. The study is not powered for efficacy; no statistically significant differences between groups were detected at baseline or follow up (Table 1). Exercise Motivations Inventory data indicate the top motivators for exercise are weight loss and to improve appearance, while social factors including competition and recognition ranked at the bottom (Figure 2). Among those who exceeded CDC exercise guidelines for all 12 weeks of the study, all were in the Intervention Group but one (Figure 3). On a scale of 0 to 8, participants in the Intervention group increased in motivation to exercise (5.5 to 6) from start to completion of the study, while those in the Control group started with higher motivation for unclear reasons, but dropped in motivation (6.75 to 6). Among those who exceeded CDC exercise guidelines throughout the duration of the study, all were in the Intervention Group but one. By the end of the study, compared to the control group the Intervention group experienced less average stress (5.1 vs. 7.2) & more average energy (6 vs. 5.1). We did not detect statistically significant improvements in health outcomes. The only adverse outcome was one case of mild skin irritation in the area of the device of unclear causation, suggesting overall patient safety.
Differences in Perceived Stress Scale Scores Among Control and Intervention Group Participants.


Exercise Motivations of Study Participants as Assessed by the Exercise Motivations Inventory.
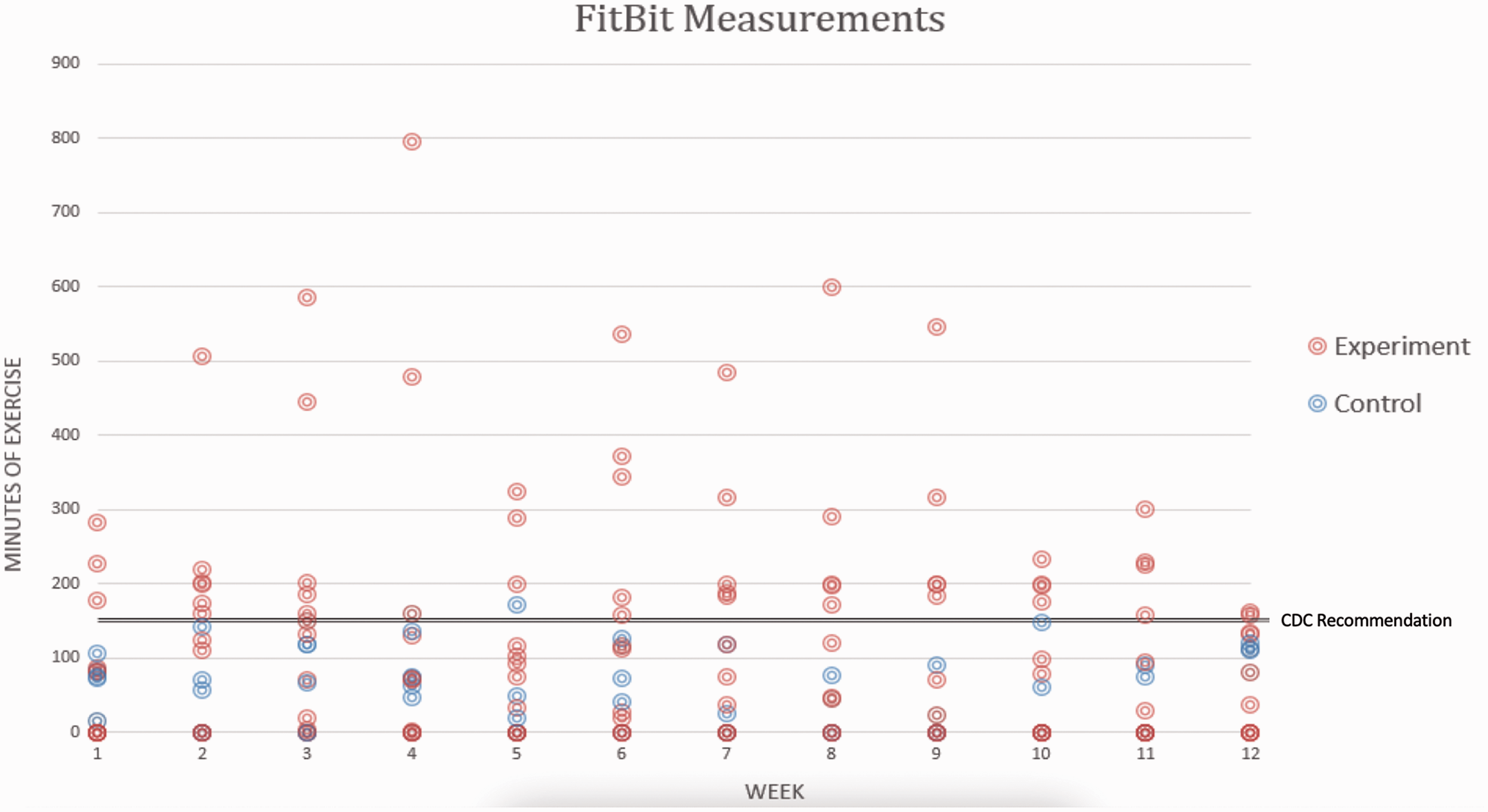
FitBit Measurements of Detected Participant Exercise Time, in Relation to CDC Exercise Time Recommendations.
Conclusions
This study demonstrates the feasibility of monitoring activity tracker data within routine primary care. Wearable activity trackers are a promising tool to facilitate patient-physician communication around exercise goals, though infrastructure and resources are needed to support this process. Though not significant, health assessment data show possible beneficial effects on motivation, energy & stress level amongst intervention participants. Physicians may be able to utilize activity trackers to positively influence patients’ exercise habits.
Limitations of this study include a small sample size, and short term follow up period. Recruitment and feasibility were limited due to time restrictions with patients during resident clinic. A small sample size limits our ability to draw conclusions about health outcomes. Implementation of a similar physician tracking study or program may be easier in settings with greater flexibility. A longer study would allow a more robust analysis of the health benefits of the intervention.
This study shows possible feasibility and resource benefits of incorporating FitBit data into patient visits, such as time saved on counseling as previously mentioned. The intervention has the opportunity to improve patient-provider communication between visits while saving both patient and physician resources spent on an in person visit, such as support staff in the clinic for the physician, and transportation for the patient. For physicians interested in incorporating activity tracker implementation into their practices, we advise a coordinated system of enrollment and survey completion involving pre-visit planning, and a system for data review and feedback. As the capacity evolves to continuously collect data outside the clinic, physicians have the opportunity to capitalize on a wealth of patient data.
Physician monitoring of FitBit data has potential to contribute numerous health benefits for patients, including maintaining motivation to exercise, and achieving compliance with CDC exercise and heart rate recommendations. This research supports the shift toward personalized medicine by facilitating conversations and additional studies about fitness data.
Ethics
This study was approved by the Northwestern University Institutional Review Board on 6/10/2016 (STU00202313).
ORCID iD
Anna Shannahan https://orcid.org/0000-0001-8468-497X
Supplemental Material
sj-pdf-1-gam-10.1177_21649561211018999 - Supplemental material for Physician Monitoring of FitBit Use for Patient Health
Supplemental material, sj-pdf-1-gam-10.1177_21649561211018999 for Physician Monitoring of FitBit Use for Patient Health by Anna Shannahan, MD, Aditya Shah, MD, Katherine Wright, PhD and Deborah S Clements, MD in Global Advances in Health and Medicine
Supplemental Material
sj-pdf-2-gam-10.1177_21649561211018999 - Supplemental material for Physician Monitoring of FitBit Use for Patient Health
Supplemental material, sj-pdf-2-gam-10.1177_21649561211018999 for Physician Monitoring of FitBit Use for Patient Health by Anna Shannahan, MD, Aditya Shah, MD, Katherine Wright, PhD and Deborah S Clements, MD in Global Advances in Health and Medicine
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project is supported by a grant from the Northwestern Medicine Lake Forest Hospital Women’s Board.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
