Abstract
Negative change occurring during psychotherapy is relatively underresearched and current theories take little account of social context. Eight clients and four therapists were interviewed about their therapy experience when reliable score deterioration on an outcome measure was observed, with the aim of generating a Grounded Theory model of negative change. The emerging model identified three major themes: a context of adversity, the therapeutic experience, and help withdrawn (within the context of positive outcomes). Difficulties included wanting therapy to provide more advice, talking about distressing issues, relationship difficulties, ambivalence, and a wish for support instead of change. Client context merits increased attention. Changes in outcome measures used, more diverse supervision models, training to use outcome measures constructively, and sensitive, routine analysis of negative change are indicated. Increased availability of therapies able to address clients’ interpersonal and social context and a wider choice of therapy type would allow interventions to better fit the individual in context.
Introduction
Any intervention seeking to induce change may result in both positive and negative outcomes. Although there is good evidence for the efficacy of psychotherapy, a small proportion of individuals consistently show evidence of a negative outcome following therapeutic input (Lambert, 2013). It is therefore important that outcome studies report negative outcomes alongside positive impact. Psychotherapy outcome research has frequently failed to do this. Negative change occurring during therapy may go unreported, or if reported, be subject to little discussion or analysis (Jonsson et al., 2014; Nutt & Sharpe, 2008). This represents a missed opportunity to learn about negative change, the circumstances in which it is likely to occur, and actions that might prevent such outcomes.
Definition
For the purposes of this study, negative change is defined as a process occurring during therapy, where a client’s “symptoms” appear to increase or worsen. Reliable change looks at whether change was sufficient so as not to be due to measurement unreliability and is calculated using the standard deviation of the measure and its reliability. Clinically significant change concerns the progression from a score typical of a treatment-seeking population to a score typical of the rest of the population. Researchers often consider a change of two standard deviations on an outcome measure score to represent a reliable change in symptoms (Jacobson et al., 1984). It is important to note that this study’s definition of negative outcomes is restricted by the use of outcome measures, whereas the issue of negative experiences associated with therapy is complex. Mays and Franks (1985) who coined the term negative outcome believed that any significant decline in functioning during therapy should be seen as a negative outcome, not only an increase in certain measured symptoms.
Prevalence
Recent estimates of the prevalence of negative change state that approximately 3% to 15% of patients receiving psychotherapy may experience negative outcomes (Linden, 2013). However, not all services collect data consistently. In the United Kingdom, around 6% of clients receiving therapy from Improving Access to Psychological Therapies (IAPT) services show evidence of reliable deterioration on outcome measures (Gyami et al., 2013). IAPT services aim to administer outcome measures before every therapy session, collecting vast quantities of outcome data. Interestingly, despite this, there is little research analyzing negative outcomes in this setting.
Earlier Research
The potential for negative outcomes in psychotherapy has been recorded for many years (Bergin, 1963; Masserman & Carmichael, 1938). Historically, therapists were taught to expect negative change as a potential outcome in their practice; however, it is reportedly no longer emphasized during clinical training (Barlow, 2010; Curran et al., 2019). Authors have suggested correlates that might be associated with negative change, including client, therapist, and process factors (Lambert et al., 1977; Mohr, 1995). Suggested client correlates include factors such as a “Borderline Personality Organisation” (Horwitz, 1974), “Obsessive-Compulsive traits” (Vaughan & Beech, 1985), expecting therapy to be painless (Foa & Steketee, 1977), severe interpersonal problems, poor motivation (Strupp, 1980), initial high symptom severity (Kernberg et al., 1972), chronic conditions, and hostility (Stone, 1985). Suggested therapist factors include low levels of empathy and warmth (Truax, 1963), underestimating client issues, poor technique (Ricks, 1974), frequent transference interpretations (Piper et al., 1991), and disagreement with the client (Llewelyn, 1988).
However, early studies often had methodological limitations and were conducted at a time when therapy might have differed from more current interventions and been less regulated. For example, in the United Kingdom, the U.K. Council for Psychotherapy only began regulating therapists in 1985 (Antrican, 2009), 8 years after Lambert et al.’s (1977) review. Psychotherapy is also now more frequently carried out by psychologists, counselors, and psychotherapists as opposed to psychiatrists. Within the U.K. National Health Service, therapists tend to provide evidence-based therapies given recommendations from NICE (The National Institute for Health and Care Excellence). For psychologists working within these settings, there has been a shift from being trained in multiple models to increased specialization and the use of protocolized therapies, leaving less space for individual differences in how therapy is delivered. It is therefore important to consider whether correlates already identified remain relevant in explaining negative change and whether the findings of previous research can be substantiated.
Differing Client and Therapist Perceptions of Negative Change
Lambert and colleagues have written extensively about negative change, in terms of how best to detect and measure it, alongside proposing methods that may help reduce its occurrence (Lambert et al., 2001, 2002). A call for clinicians to obtain feedback by routinely monitoring patient outcome (Lambert et al., 2003) came from research suggesting that therapists are poor at detecting negative change in their clients, perhaps due to an overly positive bias about their work (Walfish et al., 2012).
Hatfield et al. (2010) investigated therapists’ ability to notice negative change and base treatment decisions on this, in two linked studies. When clients showed evidence of reliable deterioration according to the Outcome Questionnaire (OQ-45), the authors examined case notes from the same time point, looking for mentions of worsening. Only 21% of therapists referred to negative change. Even when there were significant signs of deterioration during consecutive sessions, this was not mentioned in the notes around 70% of the time. In terms of responses, 23.8% of therapists continued treatment as usual, 19% changed treatment implementation, and 23.8% made a referral for medication. In 33.3% of cases, it was unclear whether the therapist made any changes, as notes merely referred to session content. This contrasted with results from their second study, a survey of therapists asking about client deterioration and action they would take. Half of therapists mentioned a medication referral and approximately a third said they would discuss deterioration with the client, increase the number of sessions, modify treatment, or consult with peers. It is not possible to know whether therapists consulted with peers and difficult to agree what level of detail would be expected in clinical notes, as this varies between clinicians and services. However, a mention of deterioration would be expected, and in two cases, therapists noted that clients appeared to have improved, which is concerning.
Therapists and clients may have different views about what change is desired. For example, Watzlawick et al. (1974) suggested that long-term therapy aims to achieve unattainable or utopian goals, valued by the therapist more than the client and potentially leading to client resistance. Fago (1980) found that therapists tended to rate clients receiving long-term therapy as improved, whereas clients’ scores showed the opposite pattern, suggesting that therapists’ and clients’ views about desirable change may differ. Werbart et al. (2019) identified differences in perceptions of therapy between therapists and clients when therapy ended in no change. These studies highlight the importance of obtaining the client’s viewpoint when investigating negative change.
Prior research has informed us about correlates of negative change occurring during routine clinical practice, implicating problems with the therapeutic alliance, social support, and negative life events (Probst et al., 2015; White et al., 2015). Some studies have also collected data about therapist explanations of negative change (Bystedt et al., 2014; Maggio et al., 2019; Shepherd et al., 2012). However, clients’ experiences are also crucial.
Client Experiences
Some studies have explored clients’ experiences beyond using outcome measures (e.g., De Smet et al., 2019; Von Below, 2020) and one has compared directly the experiences of clients and therapists of the same therapy (Werbart et al., 2019). Werbart et al. (2015) interviewed 20 patients who received psychoanalytic therapy and were defined as “non-improved,” including both those who had experienced no change and those who experienced score deterioration according to outcome measures. Although participants reported some positive experiences, a core category named “spinning one’s wheels” emerged from the data, which described therapy as an ongoing process that resulted in no movement toward goals. Participants described concerns around not understanding the therapeutic method, therapy being too short, experiencing distance in the relationship, and a focus on past experiences, when focussing on the present or future would have been valued more. Werbart et al. (2019) reported experiences of three therapists, each of whom talked about two clients with contrasting outcome. They also interviewed the clients. Where there was clinically significant change on outcomes, client and therapist appeared to have similar perceptions of therapy goals, and therapists were able to adjust their technique to meet needs. By contrast, in cases with no change, perceptions of therapist and client differed, and therapists appeared to attribute lack of change to client difficulties.
Existing studies are illuminating but most were carried out outside the United Kingdom. Furthermore, the main focus in most studies has been within the therapeutic relationship, with relatively little attention to the client’s current life context or the social determinants of well-being. “Contextual factors” and “pre-therapy factors” are important components of the theory derived by Curran et al. (2019, p. 7) in their synthesis from qualitative studies, but the main focus is on the therapeutic relationship rather than interactions between this and the life context.
Probst et al. (2015) examined expected recovery curves according to the Outcome Questionnaire Analyst (Lambert, 2012) and identified clients showing extreme positive (EPD) or extreme negative (END) deviations. The researchers looked for correlates and found that negative life events and less social support were associated with negative change. These results suggest that interventions should include some focus on the social structure and support around clients if possible. However, the authors only examined four potential correlates: motivation, therapeutic alliance, social support, and life events. Perhaps other factors would have correlated with negative outcomes had more been included.
Arguably, Lambert’s Clinical Support Tools (CSTs; Lambert et al., 2015) provide the most helpful contribution yet toward identifying a theory of negative change, as he devised an outcome measure (Assessment for Signal Cases, ASC), for use in the event of any deterioration, which looks for problems in the four key areas mentioned above: the therapeutic alliance, social support, motivation, and stressful life events. The CST manual provides advice for action in each area. For example, if therapeutic alliance is indicated, the therapist should aim to ensure they have the same goals or ask for client feedback, whereas if motivation is implicated, questions based on Miller and Rollnick’s (2002) motivational interviewing techniques are advised. Although research into CSTs is still in process, they appear to have been devised based on evidence related to positive change or outdated research on negative change, however. Increasing knowledge of negative change in various clinical settings could help to improve such tools.
Only one previous study has investigated correlates of negative change within an IAPT service. Branson et al. (2015) conducted a naturalistic study of trainee therapists delivering a cognitive behavioral therapy (CBT) intervention within an IAPT training service. However, they only looked for a correlation between therapist competence and client outcome. They found no correlation, but when therapists were divided into three groups according to competence, clients treated by the least competent therapists showed a higher-than-expected rate of deterioration in symptoms. Although this is useful for clinician training, it does little to inform us about negative change in routine clinical practice.
Rationale for the Current Study
The present study aimed to generate a model of factors contributing to negative change in brief therapy. When negative change is indicated by measures, what aspects of the client’s or therapist’s experience might help to explain this? As the hope was to inform a general explanation of negative change rather than a modality specific one, all individual therapies occurring within the relevant service were of interest. The study explored how both clients and therapists experienced the process of therapy in the context of negative change. De Smet et al. (2019) called for more attention to client perspectives. Therapists’ perspectives may also be important to build a more complete theory. Given the relative paucity of U.K.-based research into negative outcomes following therapy, and the lack of this in IAPT services, it was timely to explore this issue, with the hope of providing recommendations to improve client care in these services.
Method
Participants
Twenty-seven clients of a metropolitan IAPT service were identified as having reliably deteriorated according to scores on the Generalized Anxiety Disorder measure (GAD-7, Spitzer et al., 2006), the Patient Health Questionnaire (PHQ-9, Kroenke et al., 2001), or both, following psychological input in 2014–2015. Fifteen had received CBT and 12 had received counseling. Ten therapists, all female, provided CBT. Nine counselors, of which three were male and six females, provided counseling. Clients had received between five and 25 sessions, with a mean of 10 sessions. Eight of these clients and four of the therapists took part in the study (Table 1). It was not possible to ensure that both parties of any specific client–therapist pairing would be interviewed.
Participant Information.

M = Male; F = Female; GAD = Generalized Anxiety Disorder; PHQ-9 = Patient Health Questionnaire; CBT = cognitive behavioral therapy.
Design
Individual interviews were analyzed using a grounded theory (GT) methodology (Corbin & Strauss, 2008) to construct a model of negative change. The authors took the view that the Corbin and Strauss approach more easily accommodates perceptions from different sides of a social interaction than does more constructionist GT, as the aim was to triangulate different data sources for theory-building purposes. The first stage involved line-by-line coding, followed by axial coding and diagramming to elaborate the properties and dimensions of major categories and to hypothesize about their interaction based on the data.
Measures
Two different semi-structured interview schedules were used with clients and therapists. The client interview schedule contained four question categories that asked how they found out about the service, experienced therapy, experienced the therapist, and how the treatment affected their life. Clients were not asked directly about negative change to avoid any unnecessary distress. The therapist interview schedule contained four question categories that asked how the client came to the IAPT service, about their experience of therapy, and of working with the client and about therapy outcome. Therapists were aware that the study was investigating negative change. Each question category contained a number of prompt questions to use if necessary. As this was a GT design, the interviewer was responsive to participants’ answers to interview questions, rather than using the schedule in a rigid way, and some prompts were modified as the study progressed. For example, in later interviews, the interviewer focused more on issues that some participants mentioned in relation to having wanted to continue therapy.
Score deterioration was calculated on the basis of GAD-7 or PHQ-9 scores. The GAD-7 is a seven-item self-report measure that screens for anxiety (Spitzer et al., 2006). The PHQ-9 is a nine-item self-report measure that screens for depression (Kroenke et al., 2001). Both use 4-point Likert-type scales and ask patients to rate how much they have experienced symptoms in the past 2 weeks. For the purpose of this study, reliable deterioration was defined, according to the method of Jacobson and Truax (1991), as an increase of at least four points on the GAD-7 or at least six points on the PHQ-9.
Procedure
Twenty-six clients identified as having experienced score deterioration were sent written information inviting them to participate in the study (see Figure 1). All had been discharged from the service and one was excluded as she remained in therapy. If clients consented to participate, they were offered an appointment at a local IAPT base or their home. Therapists received a separate information sheet. If consent was given, interviews lasted up to 1 hr. All 12 individual interviews were audio-recorded, transcribed, and coded with the aid of MAXQDA, a tool that assists the researcher in organizing pieces of data and the assigned codes (VERBI, 2020).

Flowchart of sampling process.
Data Analysis
Analysis was carried out according to the Corbin and Strauss’s (2008) method of GT, based on a positivist epistemology. This was thought appropriate as this study attempted to identify a theory of negative change that would inform research and clinical practice concerning potential correlates and ways to prevent or minimize its occurrence. Transcribing and coding of interview data were carried out alongside interviewing as far as was possible. Memo-writing was used to stimulate the researcher’s thinking process around analysis and to have a record of these processes. Process notes were recorded after interviews and, as the study progressed, used to brainstorm about salient impressions of participants and reflect on these in relation to personal biases or prior knowledge. After coding five interviews on a line-by-line basis, an initial spider diagram of all emerging categories was drawn out. This helped to identify categories that needed confirmation or further information, which informed additions to the interview. After all interviews had been transcribed, diagrams were drawn for each person, highlighting key categories relating to their experience of therapy and their interaction, and in particular, categories that might help to explain negative change. Diagramming helped generate hypotheses about negative change that had been identified on the outcome measures in terms of each participant’s individual perceptions as recounted. Following diagramming, transcripts were recoded and analyzed to clarify themes and concepts by “continuous dialogue” with the data (Becker, 1998).
Quality Assurance
Guest et al. (2006) proposed that 12 interviews are often adequate to reach theory saturation, so this study aimed to recruit 12 participants. No new themes central to the model emerged at the 12th interview. A bracketing interview (Rolls & Relf, 2006) that lasted around 40 min was carried out by a colleague of the principal investigator. This explored the principal investigator’s preconceived ideas, predictions, and expectations about the project. The principal investigator had a general sense that IAPT could be positive in making therapy more available to people, but was aware of mixed views by other clinical psychology trainees in her cohort at the time of the research, including its potential (with people who are on welfare benefits and not working) for focusing too much on returning them to work. Four of the other authors work as psychotherapists, one as a trainer of IAPT workers and another as a clinical lead of an IAPT service. The third author is a researcher in applied psychology and has substantial experience of receiving mental health services in both primary and secondary care. At the time of writing, the third author has a view that therapy in IAPT can be too short, and too much focused on the individual and too little on their surrounding context.
Verbatim quotes were used in support of the final model. Supervision and meetings with supervisors were used concurrently with data collection to discuss coding and interpretation of the interview data. A section of one interview was cross-coded by a colleague of the principal investigator to validate emerging themes. In most instances, coding was agreed. Whenever disagreement occurred, there was discussion and subsequent improvement of the coding system.
Results
Analysis identified 635 coded segments and major categories emerged, offering potential explanations for the phenomenon of negative change seen in this sample. The three major categories (Figure 2 moving left to right) were the following:
Therapy in the context of adversity: descriptions of negative life events or hardships which are proposed to have reduced the effectiveness of therapy.
Negative change related to the therapeutic experience: aspects of therapy that clients or therapists found difficult or did not seem effective.
Help withdrawn: therapy described as a positive experience overall, raising questions around whether therapy had ended well, or before the client had fully benefited.
The model indicates first that clients might be living within a context of adversity (left side in Figure 2). Participants spoke about returning to this context after therapy: going back to difficult relationships, unjust situations, and struggling with the benefit system. However, there were also clear examples of clients experiencing increased adversity or negative life events during the course of therapy. This context was described as affecting how well people could engage with therapy. It influenced mood, potentially leading to increased levels of depression and anxiety and seemed to be associated with the aim of just wanting support—not seeing change as possible. The therapeutic experience (middle section in Figure 2) included negative experiences that could help to explain negative change. However, positive experiences or outcomes were also noted (right side in Figure 2), suggesting that the client did not always or only feel worse, or perhaps only experienced feeling worse as a result of therapy ending too soon, or the ending not being appropriately addressed (Help withdrawn).
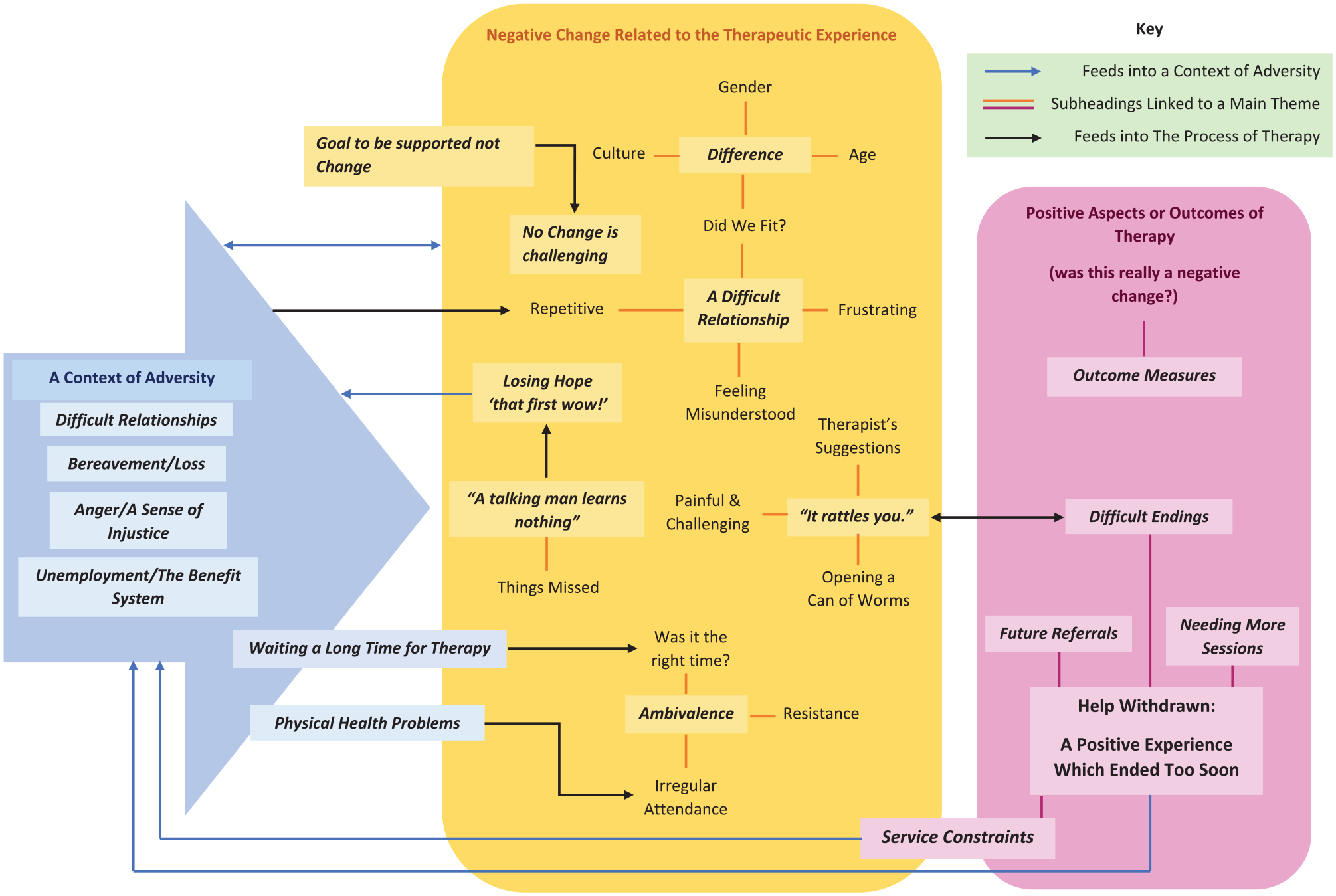
A theory of negative change.
Major Categories
The following section outlines the three major categories thought to contribute to a theory of negative change, with verbatim quotes. (Quotes are ascribed to substituted names to protect participant identities.)
Therapy in the Context of Adversity
Such contexts (left side in Figure 2) include negative life events occurring during therapy and negative circumstances that impacted therapy. Negative life events included bereavements, family conflict, and being made homeless. Negative circumstances included factors such as chronic pain, grief, a sense of injustice, and anger or circumstances around the individual such as family conflict, difficult relationships or unemployment, and the way people were treated by the benefit system. This sense of adversity could have increased due to the feeling of needing further support, addressed later in the theme “help withdrawn.” It also may feed into the therapeutic process, influencing the loss of hope and contributing to irregular attendance. The challenge of no change being observed during therapy was also thought to link to a loss of hope and associated feelings of adversity.
Bereavement/Loss
Some bereavements occurred alongside therapy, whereas other clients seemed to be experiencing unresolved grief: After the first session her mother in law . . . had gone into hospital for lung cancer . . . and then . . . I can’t remember if it was the second or third session, she actually died. (Rosie, therapist)
Quotes such as the above seemed to provide an intuitive explanation for an increase in distress.
Difficult Relationships
There were many descriptions of difficult relationships outside therapy, most often with family members, particularly when clients were in a caring role. However, sometimes they referred to friends or employees. In the model, difficult relationships are proposed to link into process issues (middle section in Figure 2) in that clients often described therapy as not able to help with these issues because they seemed to be beyond their control: My girlfriend . . . she’s been hiding so many stuff . . . from me, and I found out . . . and then when I wanted . . . to finish with her, she said to me to kill herself. And she tried this, in front of me, she cut her vein . . . (Mehmet)
Physical Health Problems
Physical health problems such as those related to pregnancy, chronic pain, and memory were described as affecting the ability to attend, engage with, and benefit from therapy: I was missing a lot of the sessions . . . I was ill all the time . . . I was in hospital; in and out, in and out . . . (Amy)
In relation to a participant who experienced ongoing cognitive difficulties, Interviewer: Was it (the therapy) helpful? Constance: No I wouldn’t say . . . because right now I be talking to you and if, things that I want to say . . . I forget . . . I do forget it now and . . . later . . . it just come to me.
Anger/a Sense of Injustice
Some clients described high levels of anger, which could seem justified in view of events experienced. Therapists sometimes described this anger as keeping the person stuck and unable to move on or change: There’s only so much that could’ve shifted because . . . he wanted an apology . . . a resolution, he wanted someone to say . . . it’s not your fault . . . I had a strong feeling that, if he had got that . . . he could’ve moved on. (Katrina, therapist)
Unemployment/the Benefit System
Being unemployed could be depressing in itself, but some participants described an additional layer of distress attributed to the benefit system: You have to go to this work programme thing where instead of looking for jobs at home . . . you have to go and sit . . . with a load of other people and you got to sign in and out 3 times a day and you can’t go home cos if you do you get sanctioned . . . they treat you like . . . naughty schoolchildren and . . . as if you’re all benefit scroungers and . . . I find it, firstly very offensive . . . The way they treat you when you’re on benefits could be calculated to drive somebody into depression. (Sandy)
In this model, the context of adversity meant that while therapy aimed to improve functioning, circumstances often resulted in increased levels of distress. Negative life events such as bereavement could explain an increase in symptoms, whereas ongoing negative circumstances could lead to hopelessness and the belief that things could not change.
Goal to Be Supported
The subcategory “goal to be supported not change” is subsumed within the overarching category of “negative change related to the therapeutic experience” but is shown straddling the major categories “context of adversity” and “negative change” because the experience of adversity seemed linked to support-seeking more than change goals. For some, adversity may have affected their motivation and decreased the likelihood of measurable change occurring: It (the therapy) was support—it wasn’t anything changing my life . . . there was too much going on to change anything. (Amy)
Waiting a Long Time for Therapy
“Waiting a long time” is a subcategory of “context of adversity,” but again straddles two major categories, as it might contribute to the experience of adversity. However, while some clients may have felt worse due to this, others described it as meaning that they already felt better by the time therapy started. This may well have had an impact on the direction of change seen on the measures and potentially given less chance of seeing clinically significant positive change.
“A Talking Man Learns Nothing”
This subcategory of the major category “Negative change related to the therapeutic experience” emerged strongly, from six of the interviews. Participants spoke about feeling like talking could not help, expecting to get more input or coping “tools” from the therapist or therapy raising more questions than answers. One person felt that he needed something more than counseling and would have liked to speak to someone “more professional”: A talking man learns nothing. . . If I’m listening then I’m learning, if I’m talking, I’m not learning and who’s the one that’s learning? (Patrick) He was listening yeah but . . . he didn’t give me any tools to even . . . give me anything to fight with. (Mehmet)
These expectations were postulated to lead to a loss of hope and disappointment with therapy as described in the next theme.
Losing Hope—“That First Wow!”
Three participants described experiencing an initial boost, moments of insight, and hope, followed by disappointment: If she can change my way of thinking, then . . . this is gonna be amazing . . . And that was the one and only time that she said something . . . that made a lot of sense and it never came again . . . At the end of the day the experience as a whole was a bit of a disappointment. (Patrick)
Or not being able to maintain changes: The first week I did really well on it and I thought, “this is it, I’m sorted” and then it. . . slipped back and I did get very despondent. (Sandy)
“It Rattles You”
Eight interviews described challenges related to therapy being difficult, although most thought this did not make it less useful. Participants described difficulties with being honest, feeling vulnerable, bringing up issues from the past, and therapy leaving them feeling less able to function. Some participants reported that therapy could also uncover or expose problems to clients, leaving them feeling distressed after the sessions: It rattles you doesn’t it . . . I’d maybe go there in quite a good mood and then I’d leave and I was, my day was kind of . . . dead . . . Cos you do uncover a lot of things and you talk about things that are probably more sensitive than you realise. (James) It was difficult yeah because . . . I was bringing things up, from years ago and, I was thinking, god, I’m opening a can of worms! (Olive) It’s . . . overwhelming and . . . very, very hurt . . . it hurts when you talk about it. (Mehmet)
Difference
Some clients and therapists mentioned issues of difference between them, related to age, gender, and culture, which may have affected the outcome of therapy. The quote below provides an example of an issue around age difference: She was much younger than me, I’d sooner somebody . . . that’s older . . . cos when we are younger we do not understand much . . . when we mature, we understand. (Constance)
A Difficult Relationship
Some difficulties with the therapeutic relationship were noted. Clients sometimes felt misunderstood, or therapists described feeling a lack of empathy: Intellectually, I had . . . roughly the same understanding, but emotionally I couldn’t get to grips with what the issues were. (Rachel, therapist)
Sometimes there were feelings of hopelessness: I wondered whether I was feeling a little bit hopeless for him and. . . I hope he didn’t pick up on that. (Katrina, therapist)
Or feelings that the therapist was critical, too directive or repetitive: She was giving me . . . lots of answers back, I didn’t really like; “this is what . . . you should do” or “do that.” (Amy) She mentioned it quite a few times in quite a few of the sessions, she always said the same things. (Patrick)
Ambivalence
Sometimes clients seemed unsure what they wanted in terms of goals or type of therapy. Irregular attendance was also mentioned as something that might have indicated ambivalence and therapists sometimes wondered whether it had been the right time for therapy: I couldn’t understand how therapy was gonna change things. (Patrick) Towards the end of the therapy there were . . . patterns of irregular attendance, cancellations . . . I did . . . wonder what was happening . . . I thought is there anything that I’m not . . . contributing? What is he trying to communicate? (Katrina, therapist)
No Change Is Challenging
This theme often emerged when discussing change. Participants might report that there had been neither positive nor negative change. Some described feeling stuck or trapped, whereas others suggested that change might not have happened until sometime after therapy: He openly acknowledged his anger . . . his depression, he just felt that he couldn’t move on and I, think I felt a little bit like that with him. (Katrina, therapist) It took a while to sink in . . . cos you gotta remember . . . you’re talking about how many years, you’re blaming yourself and everything. (Olive)
The latter quote suggests that, if followed up after therapy, some clients’ scores may have shown improvement.
Positive Aspects or Outcomes of Therapy
This major category (right side of Figure 2) contains six subcategories representing 127 lower level concepts, as clients listed many aspects that they found useful about therapy. Coded sections describe having a positive relationship with the therapist, receiving practical advice and an appreciation of having somewhere to talk which felt confidential, nonjudgmental, and impartial. Many clients also appreciated the input they received and the changes it helped them to make. The emergence of so many positive aspects seemed paradoxical in the context of an investigation of negative change. Due to this, outcome measures were discussed in the interviews.
Outcome Measures
Outcome measures were described as useful but were sometimes criticized for not picking up on the whole story or being less important than what was spoken about in therapy. One therapist felt that outcome measures caused clients to be reminded of previous symptoms rather than looking to the future or thinking about positive change. One client also described finding it difficult to rate levels of symptoms on the measures. These descriptions suggest that the measures used were viewed as limited. Therapists described avoiding looking at scores and one said she had not discussed scores with a client because they were showing negative change and she felt this might be unhelpful. Two therapists raised concerns about being too driven by outcome measure scores and “looking for a nice decline.”
Help Withdrawn
This subcategory may explain why so many positive aspects of therapy were described in a study of negative change. Participants talked about difficult endings, future referrals, and the need for more sessions. The subcategory title comes directly from a client’s words (Sandy). Except in cases referred onward, help withdrawn too early may have fed back into an experience of adversity.
Difficult Endings
Both session endings and the end of therapy were sometimes described as difficult. In some cases, it seemed like endings could have been discussed or addressed more fully and, in this way, might link back into the therapeutic process factors in the model: It was a tricky conversation and he . . . didn’t want to leave, so it’s one of those . . . “right, well . . . you take care and good luck and . . . bye!” and . . . he was just still sitting in the chair, so having to try and physically get him up. (Rachel, therapist)
In other cases, clients reported the ending coming too soon: You’re not properly better, it’s like stopping the tablets when you’re still poorly, I mean . . . it was very helpful . . . but, it would have been so much more helpful if we could have continued or, I was at a stage that I could carry on better. (Sandy)
Service Constraints
Therapists sometimes said they felt restricted and unable to offer more sessions even when thought to be useful in view of the severity or chronicity of a client’s issues. As seen in Figure 2, these constraints fed back into the experience of therapy.
The service has some really rigid, well I think it’s rigid; had they not had those requirements I think I would’ve extended the sessions . . . I probably would have offered him 16-20 sessions. (Katrina, therapist)
Future Referrals
Some clients were referred on for other input or were told about other services with the option to self-refer, but this did not always end successfully: I did refer him on . . . the CMHT (Community Mental Health Team) . . . ultimately wouldn’t accept him . . . he didn’t get any further support but he wasn’t in a place where he could use an IAPT intervention either. (Rachel, therapist) She didn’t leave me out in the cold which she could have . . . she was good to refer me on. (Amy)
Needing More Sessions
The subcategory concerning needing more input emerged from seven of the interviews and was mentioned by clients and therapists: It wasn’t enough . . . she would have benefitted from . . . longer term therapy. (Carl, therapist) I mean this . . . 8 weeks is . . . is not enough . . . Between 8 weeks and err something for, 25 years . . . or more than that. (Mehmet)
In this model, “help withdrawn” contributes to the explanation of negative change by presenting aspects of the experience of therapy which felt unfinished. The disappointment or distress felt in the context of a positive experience ending before the client is ready could potentially account for “symptom” increases seen on measures at the last session.
Responses to Negative Change
Some peripheral themes emerged describing responses to negative change as opposed to explanations. Therapists described feeling disappointed or sad when they observed negative change. However, it was also thought to be something natural and expected at times. All therapists felt it was an important issue to investigate, although concerns were raised around the political context meaning that findings could be used to reduce funding or deny some people therapy. Other concerns raised included the temptation to falsify data if services were commissioned according to outcome scores and therapists feeling judged, criticized, or inadequate.
Discussion
This study explored client and therapist experiences of therapy within an IAPT service, when there was evidence of negative change on at least one outcome measure. The following section discusses the emerging model, keeping in mind previous research and how findings might be applied to current practice, alongside implications for future research.
Therapy in the Context of Adversity
When clients described at interview the adversity they had experienced and with which they were still coping, the expectation that short-term therapy could achieve positive change sometimes seemed optimistic. In the context of ongoing difficulties, therapy for those who were angry with a strong sense of injustice seemed to pose a particular challenge. This sense of injustice seemed understandable given events experienced, including disability, loss, injustice, divorce after infidelity, and losing contact with children. Therapists spoke about how acceptance, or perhaps adjustment, would be necessary for the client to move on, but this seemed impossible to achieve at the time of therapy. These results tie in with previous research (Curran et al., 2019; Probst et al., 2015), suggesting that negative outcomes were associated with client circumstances and not necessarily a consequence of therapy itself. However, it could also be argued that therapy needs to be differently focused. Psychological therapy aimed at individual change may not be the best intervention when clients are dealing with particularly difficult life circumstances: Harper and Speed (2012) have suggested that it locates problems too much within the individual and takes too little account of their context.
It is important to consider clients’ expectations of what therapy can achieve, especially considering some difficult contexts. Some participants were referred via their general practitioner (GP) with little explanation about the process. It is possible that some clients were unaware of the effort therapy would demand and hoped it would provide a ‘ready made’ solution. Clients facing severe adversity might have benefited from a different type of intervention, targeting social support and the structures around them, such as systemic therapy (Stratton, 2016), group work with others in similar circumstances (Thoits et al., 1986) or a service working assertively to address social circumstances. However, as one therapist pointed out, due to cuts to services, it can be difficult or impossible to provide this, reflecting additional adversity within the professional system.
Cited issues with the benefit system and associated feelings of guilt and further depression also merit consideration when thinking about context. Some have criticized IAPT’s agenda of supporting people to return to work, as interfering with the formation of a good therapeutic alliance (Wesson & Gould, 2010), stating that the relationship may not be genuinely collaborative if the therapist is unduly influenced by these service expectations. The experience of these expectations may also risk the client feeling guilty and worthless if they remain on benefits. As one participant stated, the current benefit system could be “calculated to drive people into depression,” and if therapeutic services are perceived to be aligned with this, it could be unhelpful. However, this is speculative and was not specifically referred to by participants in this study. In some cases, when a return to work is facilitated sensitively, this could be hugely therapeutic.
Negative Change Related to the Therapeutic Experience
Factors emerging in this part of the model varied greatly between participants. Some felt that talking did not help, whereas others had only wanted support and found interventions designed to help them make changes unhelpful. Some found the relationship difficult and others found it challenging to raise past issues or to be honest with the therapist. Others may have held unrealistic expectations of therapy or described an initial boost which was not maintained. Difficulties in the therapeutic relationship were also cited, perhaps influencing or indicating how understood the client felt.
Although the theme “A talking man learns nothing” arose from interviews with both male and female participants, it was often cited by men as something they struggled with. It could be that the process of talking about emotions is more difficult for men (Pollack & Levant, 1998/2008), although one study has found that men show an equal preference for psychotherapy over medication when compared with women (Sierra Hernandez et al., 2014). One male participant subsequently joined a group called “Men in sheds” that seemed to offer more favorable input for him. However, it was not only a problem for men; one female participant also found it difficult to see how she could benefit from just “her alone talking.” As she also mentioned the problem of an age difference though, she may have felt the therapist was not knowledgeable or experienced enough. In her words, “when we are young, we do not know much.”
The client who cited a “lack of tools” as an issue was someone who received counseling and was helped to re-refer to IAPT. The problems experienced by this man could perhaps have been avoided at the initial referral stage by a clearer explanation of the therapeutic options available to him. This man appeared distressed at interview and perhaps the severity of his difficulties had been missed at initial assessment.
Difficulty with the therapeutic relationship is something already postulated as influencing the process of negative change and has been attributed to low levels of therapist empathy or an interaction of this with certain client characteristics (Curran et al., 2019; Lambert et al., 1977; Truax, 1963). Difference of opinion with the therapist over the process of therapy has also been implicated (Mohr, 1995; Von Below, 2020; Werbart et al., 2019). Issues raised in this study related to feeling misunderstood, feeling that the therapist was repetitive, not getting on, things being missed, and frustration on behalf of both client and therapist. One therapist spoke about difficulty in finding an emotional connection with a client who appeared stuck. These findings seem consistent with the therapeutic alliance factor on Lambert’s CSTs, deemed as important for therapeutic outcome.
The subcategory “It rattles you” often referred to distress caused by talking about difficult subjects. The theme arose predominantly from those who received counseling as opposed to CBT, perhaps an indication that more structured support could have suited them better, potentially CBT or input from other services. However, most participants seemed to recognize that this would be an integral part of therapy. One client also raised the issue of his counselor suggesting problems that he had never considered. Relating this to negative change, this client may have left with additional worries as opposed to feeling existing distress had improved. This finding may tie in with past research, related to issues with therapists interpreting the transference too much or suggesting problems (Piper et al., 1991) but it may also reflect appropriate links and challenges made as part of any therapy.
Therapists sometimes questioned whether it was the right time for therapy, which echoed previous research (Shepherd et al., 2012). However, clients never mentioned this, perhaps feeling that therapy should provide support at difficult times, as reflected in the theme “the goal to be supported not change,” which first emerged from a participant who had received CBT. This might suggest different ideas between clients and therapists about what therapy should provide, which could be addressed more fully at assessment or the outset of treatment. In the case of clients who received CBT, it may be that the initial referral should have been for counseling, or vice versa. However, clients who received both types of intervention raised the theme of just wanting support or a space to offload. As with other psychological therapies, counseling aims to help people to change, although this is often misunderstood. As general social support is what all people need for good mental health, ideally provided via mutually rewarding relationships in social contexts, which raises the question as to whether therapists should more often train to work systemically with couples, families, and social networks. This would be consistent with Probst et al.’s (2015) study, which found that less social support was correlated with negative change and that interventions should target the social structure and support around clients if possible.
It is important that experiences such as a “Boost followed by disappointment” are identified during therapy. Measures used before every session might be helpful in this regard but only if therapists attend to them and perhaps discuss scores with the client. The disappointment felt might have been linked to a drop in motivation, which would be expected to reduce the chances of positive change (Prochaska & DiClemente, 1984). Some therapists reported finding it difficult to pay attention to the outcome measures. Within a payment-by-results and austerity-oriented context, even a temporary worsening of scores may be anxiety-provoking for therapists, but ignoring them is a form of avoidance that will not address the problem. Some therapists talked about a wish to have more supervision, which could be important to address negative change when noted. Shepherd et al. (2012) reported that therapists experienced case reviews of “score deteriorators,” which aimed to aid supervision, as useful and they did not raise excessive anxiety, but it is important to state they were carefully introduced in the context of a “no blame” culture.
Positive Experiences: Help Withdrawn
Many clients reported having a positive experience of therapy. Some stated that they had volunteered for the study to give positive feedback. This did not seem to fit with negative change as seen on the outcome measures, but was consistent with statements about helpful input being withdrawn too soon. Both clients and therapists talked about whether it could have been useful to have more sessions and this seemed to be a dilemma for therapists given service constraints. This finding echoes those of Falkenstrom et al. (2007), where clients who did not benefit from therapy seemed to view it as “abruptly terminated” or unfinished. This sense of premature ending has also been postulated as a factor that mediates poor results with trainee therapists (Callahan et al., 2009).
The IAPT service offers time-limited therapy and attempts to be cost-effective, but sometimes the use of such brief interventions has been questioned (Salyer, 2002). It can be difficult to justify providing more sessions if an intervention is not thought to be working though, and Waller (2009) cautions about persisting with therapy in these cases. However, if negative change is due to social adversity or life events, it might seem inappropriate to withdraw support, although different or additional input might be advisable (Lambert et al., 2015). If clients only sought support and were not expecting to change, this calls into question the service’s rationale in looking for score decreases on outcome measures that focus on “symptoms.” Not all clients wanted more sessions, but those who did had often experienced chronic problems, ongoing for many years. In addition to help being withdrawn, some felt they needed “something more in-depth than counseling,” as if other types of therapy would explore their issues more deeply. Client perceptions about the intensity of different types of therapeutic intervention might have been clarified at assessment.
Study Limitations
There was a relatively short data collection time period, which limited the opportunity to implement theoretical sampling or to analyze each interview in full before proceeding to the next one. Ethical approval also limited the ability to change items on the interview schedule much, as specific schedules were approved. However, some theoretical sampling was applied, particularly in seeking out male counselors, so that their perspectives could be included.
The model of negative change was potentially limited by the complexity in defining it, and only deterioration on at least one self-report outcome measure was required. It would be difficult to find an objective measure, although analyzing therapy transcripts or gathering data from additional measures could be helpful for future research. The model is also solely based on one-off interviews, so it is not possible to know whether negative change was the outcome or cause of certain process factors. For example, therapeutic alliance may have suffered as a result of negative change, rather than being problematic from the outset. There are also limitations associated with applying the results of a small qualitative study to a broader population. Sampling was opportunistic and there may be bias inherent in terms of those who were willing to respond and talk about their experiences.
It was recognized that talking about therapy that may not have been effective might be distressing and some participants did become upset at interview. One client appeared distressed and requested help to re-refer. When applying for ethical approval, these concerns were raised and prevented the researcher from speaking about negative change observed with clients, in case this caused further upset. However, there is no evidence that discussing negative change in therapy is harmful and, in fact, it may have the opposite effect (Delgadillo et al., 2017) although this evidence is in the context of therapy, where a plan can be implemented and negative change addressed. In a research capacity, it is less clear what the impact might be, particularly if the person had to wait a long time for further input. It would have been interesting to see if clients would have spoken more openly about problems if they knew about this finding. Some seemed reluctant to mention difficulties and perhaps they were concerned that it would make the therapist look bad or be fed back to them. This may also reflect a general reluctance to complain, particularly as clients had been offered input for which most seemed very grateful. Clients were potentially aware of austerity’s impact on the NHS (National Health Service) and may have felt lucky to be offered therapy at all. This ethical concern also prevented the researcher seeking validation of the draft model from study participants, which could have been valuable.
Clinical Recommendations
As mentioned previously, IAPT services use outcome measures routinely to track progress. However, as the measures are symptom-focussed and do not ask about life events, social adversity, or interpersonal relationships, it may be difficult to detect negative change due solely to therapeutic process, or to assess the relationship between these contexts and the progress of therapy. If information was collected using a measure such as the Outcome Questionnaire (Lambert et al., 2004), more factors would be taken into account that may also help to identify clients for whom intervention is advisable, using CSTs to guide therapist decision-making. Alternatively, the CORE-OM (Clinical Outcomes in Routine Evaluation, Evans et al., 2002) includes interpersonal items, which might give a more rounded measure of functioning than symptom-specific measures.
Therapist interviews highlighted structural issues within the NHS, whereby primary care services can only be effective if they are supported by secondary care mental health services: It is often difficult to transfer clients to secondary care, and there may be a gap between primary and secondary care. This means that IAPT often see people who are not at the appropriate service tier and clients may receive interventions that do not fit their needs. Themes such as aiming for support and not change, and needing further input might relate to this issue. However, preparing clients for therapy, so they are aware of the focus and do not arrive with unrealistic expectations does not address the lack of appropriate services. This issue is highlighted by Curran et al. (2019) in terms of clients feeling that there was a lack of choice.
As many clients in this study stated that they would have liked further input, it might be helpful for the IAPT service to review procedures concerning extending therapy, when indicated or possible to provide. Some aspects of the service appear to be driven by outcome scores and the same measures are used for every client. In view of differing goals, it may be useful to fit outcome measures to the client or to measure movement toward the client’s specific goals rather than using a “one size fits all” approach (Donnelly et al., 2011). For example, using the PSYCHLOPS (Psychological Outcome Profiles; Ashworth et al., 2012) measure could address this issue as it rates the client’s own stated goals rather than items provided by professionals.
Reported issues around the therapeutic process (relating to the therapeutic relationship and issues around the therapy ending) and clients’ levels of social support or the structure around them could have implications for training. Although practitioners such as Gilbert and Leahy (2009) show that cognitive behavioral approaches are focusing more on process and relational issues than previously, they do not typically emphasize issues occurring in the therapeutic relationship or clients’ interpersonal relationships. Therefore, continued professional development (CPD) highlighting such issues might be provided for staff working within the service. One therapist spoke about finding psychodynamic supervision useful, suggesting that she could have benefited from more of this kind of input. She also talked about wanting more group supervision and a space to discuss individual cases. This might fit with the idea of regular case reviews of “score deteriorators” discussed in supervision and in meetings as reported by Shepherd et al. (2012). Although regular supervision is provided for therapists working within IAPT services, the type, orientation, and amount provided could be reviewed. Psychodynamic and systemically orientated supervision may be helpful to complement CBT and counseling supervision, which is more commonly available.
Therapists raised issues about outcome measures more than clients did. If therapists believe outcome measures are not useful, this may affect how useful they can be as a clinical tool. As mentioned previously, without the assistance of such measures, therapists often fail to identify negative change (Walfish et al., 2012). This might be predicted to lead to worse outcomes, but awareness of negative change could permit a modification in therapeutic approach. Perhaps the introduction of measures better tailored to individual need might facilitate their use by therapists.
Further Research
Many aspects of the final model could warrant further investigation. For example, the interesting subcategory “A talking man learns nothing” could be examined in more depth, establishing when and for which clients it is most relevant and what interventions may be more useful. While NICE guidance identifies interventions with the strongest evidence base, these are nomothetic and diagnosis-specific and might not always suit individual presentations that do not fit neatly within a diagnostic description. Perhaps future research could help to identify individuals for whom alternative approaches might be more appropriate. Individual trajectories through different therapies and other forms of social engagement (such as the example of Men in Sheds) could cast light on what people gain from different options at different times, and why. As some clients noted, positive change may have been something that took time to develop so it would have been useful to administer outcome measures at follow-up, to track change over a longer time. Indeed, a recent trial of psychoanalytic psychotherapy found evidence of delayed therapeutic benefit at 2-year follow-up, which was not evident immediately following therapy (Fonagy et al., 2015).
Conclusion
The emerging model provides a useful overview of experiences of therapy in a U.K. IAPT service context, which may contribute to the process of negative change, highlighting the importance of paying attention to context and life events, alongside what clients expect from therapy. Issues around wanting further input arose frequently as therapy often felt too brief. This reflects the study’s focus on IAPT services, which offer brief therapy and rely for their effectiveness on appropriate referrals and good links with secondary care services. Clients did not always seem well prepared for the focus on personal change in therapy; however, arguably this was an overly optimistic goal in light of the clients’ ongoing adverse circumstances. Therapists did not always seem to use outcome measures to help them address negative change and were working in high-pressure contexts. Such contexts can raise anxiety about deterioration, and therapists need effective support systems to explore it constructively. Service-level changes in supervision and training would be useful alongside the introduction of sensitive, routine analysis of negative change by, for example, case reviews in a “no blame” culture. Increased availability of therapies able to address clients’ interpersonal and social context is indicated.
It is important to note that some clients did not think there had been a negative outcome and some noted that change could take time. Difficulties raised were different for different participants, for example, some clients did not like the emphasis on their talking, whereas others felt that the therapist advised them too much. This echoes a recent study (Swift et al., 2017) which found that the events or therapist actions associated with clients’ perceptions of helpfulness were sometimes the same as those associated with hindrance. This highlights the need to adjust interventions to fit with individual clients and their goals, which would also fit with NHS’ aims to offer patient choice in all settings.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported and funded by the Salomons Institute for Applied Psychology, Canterbury Christ Church University.
