Abstract
This study compared the possible protective effects of silymarin and melatonin against gentamicin (GEN)-induced nephrotoxicity in rats. Rats were allocated to 6 groups: Group I, control group; Groups II and III, administered with silymarin or melatonin; Group IV, injected with GEN; and Groups V and VI, administered with silymarin or melatonin, and then injected with GEN. Compared with the rats in the control group, all rats injected with GEN significantly presented elevated levels of serum creatinine and urea that was accompanied by an increase in relative kidney weight, increase in renal reactive oxygen species (ROS) and malondialdehyde (MDA) levels, and reduction in renal glutathione (GSH) level and superoxide dismutase (SOD) activity. Silymarin and melatonin pretreatment significantly lowered the elevated serum urea and creatinine concentration, kidney weight, and renal ROS and MDA levels. In addition, silymarin and melatonin significantly enhanced renal GSH level and SOD activity. This study indicates that silymarin and melatonin can attenuate renal injury in rats treated with GEN possibly by reducing the ROS level.
Gentamicin (GEN), an antibiotic of the aminoglycoside group, is still an important drug against life-threatening Gram-negative infections. Despite the introduction of newer and less toxic antibiotics against Gram-negative microorganisms, its broad-spectrum activity, rapid bactericidal action, postantibiotic effects, chemical stability, low cost, and efficacy against germs insensitive to other antibiotics have made it a first-line drug in a variety of clinical situations. 1,2 However, due to the risk of ototoxicity and nephrotoxicity (serious side effects of GEN), its usefulness is limited. The major adverse effect of this drug is nephrotoxicity. GEN nephrotoxicity accounts for 10% to 30% of acute renal failure that markedly limits its clinical use. 3 –5 It has been suggested that GEN nephrotoxicity may be related to its accumulation in renal proximal convoluted tubules, reaching a concentration of 5 to 50 times higher than the plasma level in the tubular renal cell, leading to the loss of brush border integrity. 6 GEN nephrotoxicity is characterized functionally by markedly increased levels of serum creatinine, blood urea concentration, and significant decrease in glomerular filtration and morphologically characterized by extensive tubular epithelial cell vacuolation and desquamation, tubular fibrosis, epithelial edema, glomerular hypertrophy, and severe proximal renal tubular necrosis, linked to renal failure. The exact mechanism of GEN nephrotoxicity is not well elucidated; however, several studies demonstrated that the nephrotoxic effect of GEN can be mediated by increased generation of reactive oxygen species (ROS) and reactive nitrogen species (RNS) and the reduction of efficiency of kidney antioxidant enzymes like superoxide dismutase (SOD), catalase (CAT), glutathione peroxidase (GPX), and glutathione (GSH). 7 –9 Lipid peroxidation, protein denaturation, DNA damage, and upregulation of caspase family of proteases with subsequent apoptotic cell death and the increase of monocyte/macrophages infiltration mediated by ROS are proximal events in the cascade of GEN nephrotoxicity. 10,11
Silymarin is a flavonoid complex isolated from the seeds of milk thistle (
The present investigation was carried out to evaluate the protective effects of silymarin and melatonin against GEN-induced nephrotoxicity in Wistar albino rats.
Methods
Drugs and Chemicals
Gentamicin, silymarin, and melatonin were purchased from Sigma (St Louis, MO).
Test Animals
The experimental protocols used in this study were approved by the Ethics and Animal Care Committee of Zahedan University of Medical Sciences and were performed in accordance with the National Institute of Health Guidelines for the Care and Use of Laboratory Animals. Male Wistar rats with an initial body weight of 230 to 260 g were used in this study. The animals were kept in groups and housed in stainless steel cages under standard environmental conditions at a temperature of 23 ± 3°C, with 12-hour light/dark cycles. Standard commercial diet and water were available ad libitum. The study was conducted in accordance with the European Communities Council Directive in such a way to minimize the number of animals used and their suffering.
Ethics
This study was performed according to the guidelines of the US National Institute of Health (NIH Publication No. 85.23, revised 1985) guides for the care of laboratory animals.
Experimental Design
Thirty-six male Wistar albino rats were randomly divided into 6 groups each containing 6 rats.
Rats in Group I served as the control group and were consecutively was injected intraperitoneally (ip) with physiological saline (1 mL/kg/day) for 8 consecutive days. Rats in Groups II and III were administered with silymarin (50 mg/kg/day, ip) or melatonin (15 mg/kg/day, ip) for 7 consecutive days. Rats in Group IV were injected with gentamicin sulfate (100 mg/kg/day, ip) for 8 consecutive days. Rats in Groups V and VI were administered with silymarin (50 mg/kg/day, ip) or melatonin (15 mg/kg/day, ip) for 7 consecutive days and then received injections of gentamicin sulfate (100 mg/kg/day, ip) for 8 consecutive days.
Serum and Tissue Collection
After 8 days, the weight of animals was measured; then, they were anesthetized by intraperitoneal injection of ketamine (30 mg/kg). Blood samples (4-6 mL) were taken by cardiac puncture after which the animals were sacrificed by cervical dislocation, kidneys quickly removed, washed with ice-cold physiological saline, and the absolute and relative (organ to body weight ratio) weights of the kidney measured for all rats. Kidneys were shock-frozen in liquid nitrogen and were kept in −80°C for lipid peroxidation and ROS assay.
Serum Biochemical Assays
To obtain serum, blood samples were centrifuged at 1500 ×
Estimation of Lipid Peroxidation
Malondialdehyde (MDA) concentrations were measured in kidney tissues as a marker of lipid peroxidation. Kidney tissues were homogenized in ice-cold tamponade containing 150 mM KCl for the determination of MDA. MDA, referred to as thiobarbituric acid reactive substance (TBARS), was determined by the absorbance of 535 nm wavelength, and the results were expressed as malondialdehyde equivalents (nmol/mg protein). 21
Assay of Superoxide Dismutase Activity
SOD activity was determined by using a commercially available SOD assay kit (Sigma) according to the manufacturer’s instructions.
Dichlorofluorescein Assay for the Determination of ROS Levels
ROS levels in kidney were determined by using the 2′,7′-dichlorofluorescein diacetate (DCF-DA) fluorescence method. The fluorescence intensity of DCF was measured by a fluorescence plate reader using excitation at 485 nm and emission detection at 528 nm, and the results were expressed as percentage change in fluorescence, where the control group was taken as 100%.
Determination of GSH Level
Renal GSH level was determined according to a previously published method 22 with little modifications. The method is based on the reduction of 5,5-dithiobis-2-nitrobenzoicacid by GSH to yield a yellow component. The absorbance of this yellow component was measured at 412 nm and compared with the standard curve to determine GSH concentration.
Statistical Analysis
The results are reported as mean ± SEM. The statistical analyses were performed using one-way analysis of variance (ANOVA) by SPSS software (version 20). Group differences were calculated by post hoc analysis using Tukey test.
Results
Effects of Silymarin and Melatonin Treatments on Kidney and Body Weight in GEN-Treated Rats
No deaths or remarkable signs of external toxicity were observed in the groups of animals that were given GEN, melatonin, or silymarin. Relative kidney weight significantly increased (
Effects of GEN-Induced Alterations in the Body Weight Changes and Kidney Weights*.

Abbreviations: GEN, gentamicin; SEM, standard error of the mean; ANOVA, analysis of variance.
*The data are expressed as mean ± SEM (n = 6). The data were analyzed by one-way ANOVA followed by Tukey test.
a
b
Effects of Silymarin and Melatonin on Serum Creatinine and Urea Levels in GEN-Treated Rats
Table 2 shows the serum urea and creatinine levels in control and experimental groups of rats. In control animals, serum creatinine and urea concentration were 0.63 ± 0.01 and 20.4 ± 1.71 mg/dL, respectively. They significantly increased to about 2-fold (
Effects of Melatonin and Silymarin on GEN-Induced Alterations in the Serum Biochemical Parameters*.
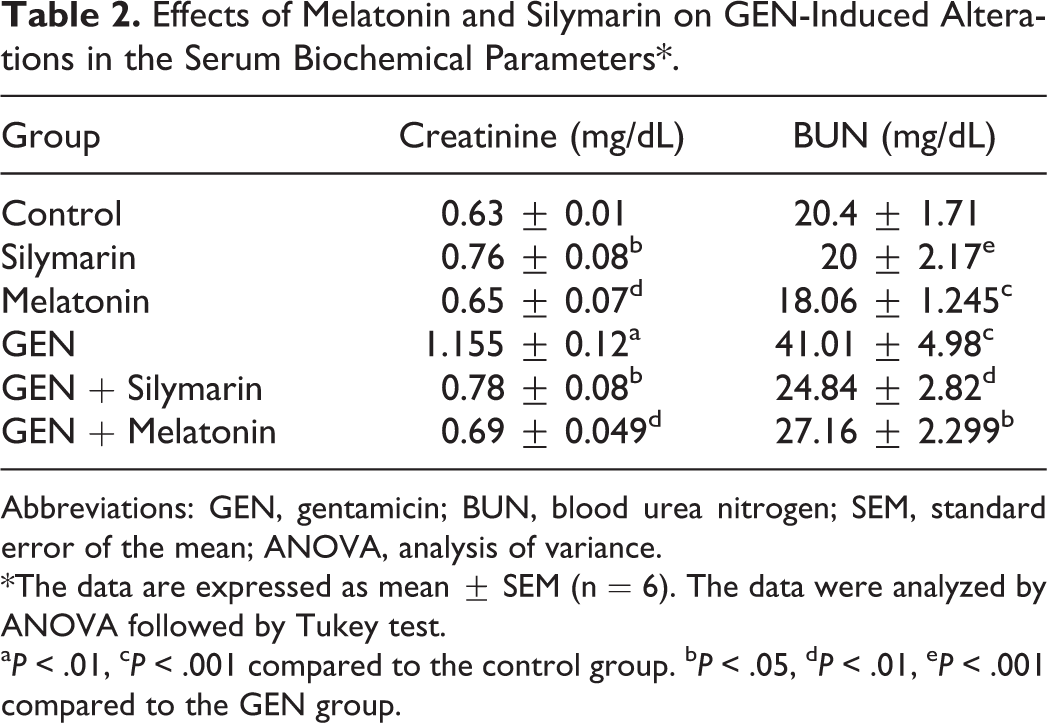
Abbreviations: GEN, gentamicin; BUN, blood urea nitrogen; SEM, standard error of the mean; ANOVA, analysis of variance.
*The data are expressed as mean ± SEM (n = 6). The data were analyzed by ANOVA followed by Tukey test.
a
Effects of Silymarin and Melatonin on Renal ROS and MDA Levels in GEN-Treated Rats
A highly significant elevation was observed in MDA and ROS levels in the kidneys of GEN-intoxicated rats when compared with the control group (
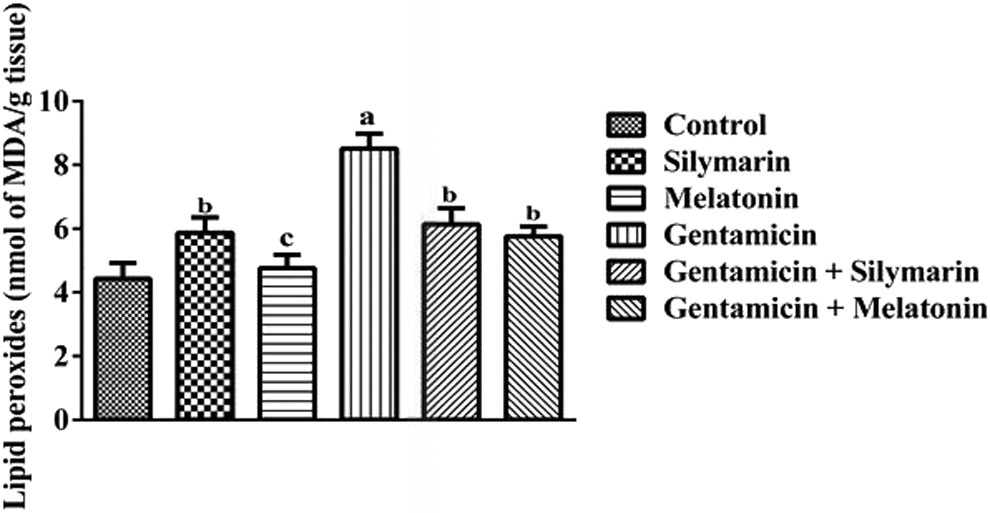
Levels of lipid peroxidation in the kidneys of control and experimental animals.

Levels of reactive oxygen species (ROS; % of control) in the kidneys of control and experimental animals.
Effects of Silymarin and Melatonin Treatments on Renal GSH Level and SOD Activity in GEN-Treated Rats
GSH level and SOD activity significantly decreased in the GEN-treated group when compared with the control group (

Levels of superoxide dismutase (SOD) in the kidneys of control and experimental animals.

Levels of glutathione (GSH) in the kidneys of control and experimental animals.
Discussion
Aminoglycoside antibiotics, and specially GEN, are well known to cause serious nephrotoxicity and this toxic effect limits their clinical usefulness. In this study, GEN was injected consecutively at the dose of 100 mg/kg (ip) for 8 days. As expected, all rats injected with GEN alone presented reduced renal function, which was correlated with elevated levels of serum urea and creatinine. In the present study, it was shown that the impairment of renal function was accompanied by an increase in kidney weight, increase in renal ROS and MDA levels, and reduction in renal GSH level and SOD activity. The data obtained from the present work showed that pretreatment of rats with melatonin (15 mg/kg/day, ip) for 7 days was able to attenuate GEN-induced nephrotoxicity, and similar to melatonin, silymarin (50 mg/kg/day, ip) also could prevent nephrotoxicity induced by GEN in rats.
The exact GEN nephrotoxicity mechanism is unknown, but according to experimental data, oxygen free radicals are considered to be important mediators of GEN-mediated nephrotoxicity. 23 Some authors reported that GEN can stimulate free radical formation by releasing iron from renal cortical mitochondria and forming iron-GEN complexes by iron chelation, which can be the initial step in GEN-induced ROS formation. 24 This viewpoint is supported by an increase in serum urea and creatinine levels, MDA level, an index of LPO, depletion of kidney reduced GSH content, and low activity of antioxidant enzymes such as SOD and CAT. 25,26 Inactivation of these antioxidant enzymes could be the result of increased production of ROS, which could aggravate the oxidative damage. However, the results of our study showed that pretreatment with melatonin (15 mg/kg/day, ip) induced a significant decrease in kidney weight and serum urea and creatinine levels and improved the GEN-induced suppression of GSH level, SOD activity, and elevation of ROS and MDA levels in kidney tissue efficiently. It has been well documented that melatonin (a pineal gland hormone) has antioxidant properties in addition to its other biological functions. Numerous reports have demonstrated that the antioxidant effect of melatonin may result from its direct ability to scavenge free radicals or its indirect antioxidant activity by increasing the activity and expression of the antioxidative enzymes. 15,16
Melatonin is an effective scavenger of ROS and RNS including singlet oxygen (1O2), superoxide radical (O2 • −), hydroxyl radical (•OH), hydrogen peroxide (H2O2), nitric oxide (NO), and peroxynitrite anion (ONOO−). In addition, melatonin can inhibit the catalytic activity of nitric oxide synthase (NOS) and expression of inducible nitric oxide synthase (iNOS) at the transcriptional level that reduces the amount of NO produced. 27 Besides direct scavenger activity, melatonin can stimulate gene expression and activities of several antioxidative enzymes including GRd, GPX, CAT, and SOD, and this indirect antioxidant activity of melatonin is related to its interaction with either membrane or nuclear receptors. These antioxidative enzymes can metabolize free radicals to less reactive species and thereby decrease the formation of highly toxic by-products. For example, SOD can reduce free radical–mediated cellular damage as a result of producing H2O2 by dismutasing O2 • −; CAT converts H2O2 to water and oxygen; GPX, by oxidizing GSH to glutathione disulfide (GSSG) can metabolize peroxides such as H2O2 to water, and then GRd reduces GSSG to GSH. It has been shown that melatonin by stimulating its rate-limiting enzyme, γ-glutamylcysteine synthase, increases the synthesis of GSH. Experimental studies show that administration of melatonin for long periods increases mitochondrial number in cells. Furthermore, it has been shown that there are mitochondrial binding sites for melatonin. Additionally, treatment of mitochondria with melatonin improved the efficiency of the oxidative phosphorylation metabolic pathway and consequently reduced the leakage of electrons and formation of free radicals. Also, melatonin upregulates the production of ATP, which is vital for cellular functions including the repair of molecular damage created by ROS and RNS. 28 –31 Previous studies indicate that melatonin can protect kidneys against pathological conditions. It has been shown that melatonin is able to prevent renal functional impairment induced by oxygen free radicals resulting from cyclosporine in rats without any alteration in cyclosporine plasma levels. 32 It has also reduced renal oxidative damage induced by aluminum, lead, ochratoxin, mechlorethamine, spinal cord and thermal injury and has been able to improve early glomerulopathy mediated by oxidative stress in diabetic rats’ kidneys. 33 –40 In another study, it has been shown that melatonin had protective effect against hamster kidney model of estradiol-induced DNA damage. 41 In our previous study, we showed melatonin is able to enhance the beneficial effects of atorvastatin against GEN-induced nephrotoxicity. 42 Also, there are other studies about the protective effects of melatonin in GEN-induced nephrotoxicity, and our results are entirely consistent with the other studies. 27,43 –46 Our results also showed that pretreatment with silymarin at a dose higher than melatonin (50 mg/kg/day, ip) had protective effects against nephrotoxicity induced by GEN in rats. Silymarin was significantly able to decrease kidney weight and serum urea and creatinine levels and efficiently improved the suppression of GSH level and SOD activity and elevated levels of ROS and MDA induced by GEN in kidney tissue. According to experimental and human studies, silymarin has good antioxidant activity, and this property may be due to the inhibition of the initiation step in auto-oxidation by silymarin and its free radical scavenger activity. 47,48 It has probable antagonizing effects against the depletion of endogenous antioxidant defenses, such as those mediated by SOD or the GSH system through free radical load decrease, upregulation of GSH levels, and stimulation of SOD activity. 49
A number of studies have demonstrated that silymarin has a regulatory action on cellular membrane permeability and improves the membranes’ stability against xenobiotic-induced damage. Furthermore, silymarin has nuclear expression regulatory capacity. It is appeared that silymarin stimulates RNA polymerase I and the transcription of rRNA by which it increases the synthesis of ribosomal RNA (rRNA) species. The loss or functional impairment of transporters and enzymes occur in many pathological conditions and the stimulation of protein synthesis is an important step for counteracting it. 17,31 It has also been shown that silymarin by effective induction of antioxidant related genes, including the transcription factor NF-E2-related factor-2 (Nrf2), can act as a potent cytoprotective effector. The transcription factor Nrf2 can regulate the expression of a variety of cytoprotective and phase II detoxifying enzymes, such as glutathione S-transferase (GST) and SOD. 50 Also it has been reported that silymarin and its biologically active component, silybin, are powerful iron chelators that reduce serum iron and ferritin and thus they are able to inhibit Fe2+ salts catalyzing linoleic acid oxidation. These data suggest that iron chelating activity can be one of the protective mechanisms of silymarin against GEN-induced oxidative damage. 51 Maybe this property of silymarin inhibits the formation of iron-GEN complex and its renal accumulation. Renoprotective effects of silymarin have been reported in several studies. It has been shown silymarin is able to increase antioxidant enzymes and a number of protection mechanisms against free radical damage in alloxan-induced pancreatic damage in rats and also antagonize cisplatin- and ifosfamide-induced renal toxicity without reducing their antitumor efficacy. It has also been reported that treatment with silymarin or vitamin E in GEN-treated dogs improved alteration in serum creatinine and MDA concentrations, which may be due to its antioxidant activity. 52 –54
From the results of the present study, it could be inferred that the pretreatment of rats with melatonin and silymarin inhibits GEN-induced nephrotoxicity, and it seems that melatonin can induce this effect at a dose lesser than silymarin. Administration of silymarin and melatonin prior to GEN exposure resulted in a marked decline in kidney weight and serum urea and creatinine concentrations, renal ROS and MDA levels, and also significant elevation in renal GSH level and SOD activity. These results suggest that the protective effect of silymarin and melatonin may be caused by their antioxidant properties.
Footnotes
Authors’ Note
Habib Ghaznavi and Saeed Mehrzadi equally contributed to this work.
Author Contributions
The work presented in this article was carried out through collaboration between all authors. BD and HG made the initial hypothesis. All authors participated in defining the research theme and provided the proposal. SM, SMTHT, HV, HRPT, and AH performed the experiments, collected the data, analyzed the data, and wrote the article. BD, HG, and AR conceptualized the study, critically analyzed and discussed the data, and corrected and reviewed the article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by a grant from the Zahedan University of Medical Sciences.
Ethical Approval
This study was performed according to the guidelines of the US National Institute of Health (NIH Publication No. 85.23, revised 1985) guides for the care of laboratory animals.
