Abstract
Racial and ethnic disparities in utilization of chiropractic services have been described at the state level, but little is known about such local disparities. We analyzed Medicare data for the year 2008 to evaluate by ZIP code for utilization of chiropractic services among older adults in Los Angeles County, California. We evaluated for availability and use of chiropractic services by racial/ethnic category, quantified geographic variations by coefficient of variation, and mapped utilization by selected racial/ethnic categories. Among 7502 beneficiaries who used chiropractic services, 72% were white, 12% Asian, 1% black, 1% Hispanic, and 14% other/unknown. Variation in the number of beneficiaries per ZIP code who used chiropractic services was highest among Hispanics, blacks, and Asians. We found evidence of racial disparities in use of chiropractic services at the local level in Los Angeles County. Older blacks and Hispanics in Los Angeles County may be underserved with regard to chiropractic care.
Keywords
Racial and ethnic disparities in access to health care services are well documented and significant concerns in the delivery of health care in the United States. Racial and ethnic minorities are commonly confronted both with decreased access to care as well as poorer quality care. 1 –3 According to the 2012 US Department of Health and Human Services National Healthcare Disparities Report, although the overall quality of health care is improving nationally, access to care is declining, and disparities are not improving. 3 Manifold disparities have been documented across a broad range of medical conditions, including acute and chronic pain. 4 –8
Chiropractic physicians are complementary and integrative health care providers whose scope of practice includes pain complaints. Back and neck pain are the most common conditions for which patients seek chiropractic services. Several studies have analyzed data from the National Health Interview Survey and found that minorities are less likely than whites to use complementary and integrative health care in general and chiropractic in particular. Graham et al reported that, in 2002, chiropractic use was 8.8% among whites, 3.8% among Hispanics, and 2.7% among blacks. 9 They also reported that even after controlling for sociodemographic factors that influence complementary and integrative health care use, blacks were 29% and Hispanics 22% less likely to use complementary and integrative health care than whites. Su and Li reported similar rates of use of chiropractic services among minorities in 2002, and additionally reported that in 2007, 10.7% of whites, 3.1% of African Americans, 3.8% of Hispanics, and 4.4% of Asians used chiropractic care. 10 Barnes and colleagues reported that in 2007, complementary and integrative health care use was more prevalent among women, adults aged 30 to 69 years, adults with higher levels of education, and adults who were not poor. 11 They further found that in 2002 and 2007, adults were more likely to use complementary and integrative health care than when the cost of conventional care was unaffordable. 11
Other investigations have reported fewer significant differences in chiropractic use across ethnic groups. In a 2003 study, Carey and Garrett found that blacks with acute low back pain were only slightly less likely to see a chiropractor than a medical doctor as their initial provider for the episode, 8 and Carey et al found the proportions of black and white chronic back and neck pain sufferers who sought chiropractic care were not significantly different at 23.6% and 21.7%, respectively, while 33.9% of Latinos with chronic back and neck pain sought chiropractic care. 12
With regard to chiropractic utilization among older adults, multiple studies have reported increased rates of use among whites and females. 13 –17 Arcury et al’s analysis of National Health Interview Survey data for adults over age 65 demonstrated that in 2002, chiropractic use was 6.6% among whites, 3.1% among Hispanics, 1.5% among blacks, and 0.6% among Asians. 18 Other studies of older adults have uncovered similar patterns of greater chiropractic use in whites and lesser but varying use in other ethnic/racial groups. 15,19 –21 Variability in use reported among other ethnic/racial groups, especially Hispanic, may have been due to these studies not being designed to be nationally representative with regard to racial composition. A study of the practices of minority chiropractors in Erie County, New York, found smaller proportions of chiropractors and chiropractic patients in areas with relatively high minority populations. 22 Whedon and Song studied a national sample of Medicare claims data from 2002 to 2007 and reported that whites had the highest rate of chiropractic use, comprising 96% to 97% of users, followed by blacks at 1% to 2%, and all other minorities with 1% or less. 17 Rates of chiropractic use among racial minorities showed greater geographic variation than did rates for whites. Racial disparities were found to be independent of the racial composition of state populations, and varied little over time.
In a 2012 study, Whedon and colleagues reported that increased chiropractic supply was strongly correlated with increased chiropractic use under Medicare. 23 The use of chiropractic services, patterns of use by minorities, and supply of chiropractic physicians under Medicare have been described nationally by state and hospital referral region, 17,23,24 but regional averages may smooth over local effects, 25 and little is known about local variations and disparities in use and availability of chiropractic services. The purpose of this study is to evaluate for racial disparities in use of chiropractic services at the local level by zooming in on a single US metropolitan area and evaluating patterns of chiropractic use by ZIP code. For this purpose, we chose Los Angeles County, California, owing to the area’s dense population and racial and ethnic diversity.
Methods
Design and Data Handling
We used a cross-sectional design to retrospectively analyze Medicare administrative data for the year 2008. The study was conducted under the terms of a data user agreement with the Centers for Medicare and Medicaid Services. The primary author’s institutional review board reviewed and approved the research plan. We performed data analyses with SAS, and data mapping with SAS Visual Analytics Hub 6.4M1 (SAS Institute Inc, Cary, NC).
Data Sources and Sampling
The analytic data file used in this study was sourced from Medicare administrative files for the year 2008. We merged—on unique beneficiary identifiers—Medicare Part B claims data from the Carrier File with beneficiary demographic data from the Denominator File. The Carrier File provided Medicare Part B claims. The Denominator File provided beneficiary demographic and enrollment information, including self-reported race/ethnicity. We restricted the analytic file to beneficiaries aged 65 to 99 years; living as of January 1, 2008; and residing in 124 ZIP codes that overlap with Los Angeles County, California, as defined by the Centers for Medicare and Medicaid Services. We excluded disallowed claims and duplicate claims for the same patient, provider, procedure, and date of service. To reduce the likelihood of individual patient identification, we excluded beneficiaries older than 99 years, and in accordance with the Centers for Medicare and Medicaid Services’ rules for protection of human subjects we suppressed any data fields with 1 to 10 observations.
Analyses
We used ZIP code of beneficiary residence as the unit of geographic analysis. We aggregated the data by ZIP code and evaluated for use of chiropractic services (defined as at least one allowed claim in 2008 associated with provider specialty code 35) by beneficiary race/ethnicity category (white, black, Hispanic, Asian, or other/unknown). We evaluated for Medicare-active chiropractic physicians, defined as Medicare providers with at least one allowed claim in 2008 associated with provider specialty code 35. We quantified geographic variations in Medicare-active chiropractic physicians, Medicare beneficiaries, and Medicare beneficiaries who used chiropractic (chiropractic users) by coefficient of variation. We defined chiropractic use as chiropractic users per 1000 beneficiaries, and chiropractic availability as Medicare-active chiropractic physicians per ZIP code. We used Fisher’s exact test to analyze for differences in chiropractic use among minorities as compared with Whites. We used Spearman’s rank correlation coefficient to correlate chiropractic use with chiropractic availability, by race/ethnicity of chiropractic user. To illustrate geographic variations, we mapped counts of beneficiaries and chiropractic users by selected racial/ethnic categories.
Results
Racial Disparities in Chiropractic Availability and Chiropractic Use
We found 377 Medicare-active chiropractic physicians in Los Angeles County. They provided chiropractic care to 7502 patients, out of a total of 248 116 Medicare beneficiaries aged 65 to 99 who resided in Los Angeles County in 2008 (Tables 1 and 2). Thus, the proportion of beneficiaries who used chiropractic services was 3%, and the ratio of patients to chiropractors was 20:1. Medicare beneficiaries of other/unknown race/ethnicity had the highest rate of chiropractic use (75.4) followed by whites (36.2), Asians (25.9), blacks (3.4), and Hispanics (1.7). For each minority category, rates of chiropractic use differed significantly as compared with Whites (Table 2). Correlation between chiropractic availability and chiropractic use was moderately positive, both overall (Spearman’s ρ 0.49; P < .0001) and for white beneficiaries (Spearman’s ρ 0.56, P < .0001); the same correlations for other racial/ethnic categories were weak and statistically insignificant (Table 3).
Geographic Variation in Race/Ethnicity of Medicare Beneficiaries in Los Angeles County, 2008a.

aData are summarized by ZIP Code.
Chiropractic Use in Los Angeles County, by Race/Ethnicitya.
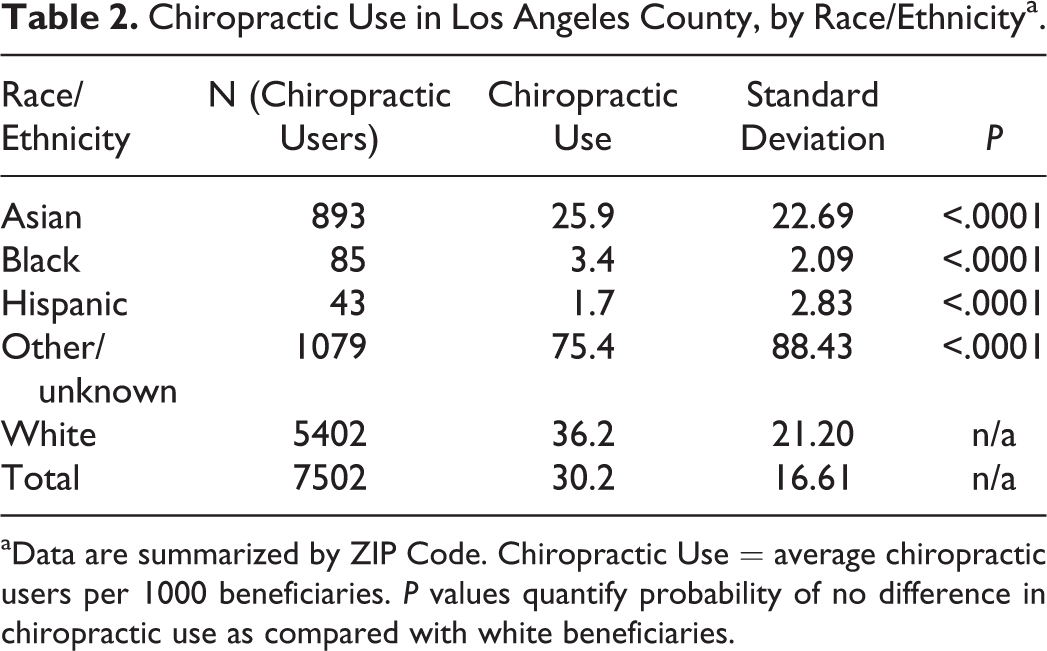
aData are summarized by ZIP Code. Chiropractic Use = average chiropractic users per 1000 beneficiaries. P values quantify probability of no difference in chiropractic use as compared with white beneficiaries.
Correlation Between Chiropractic Availability and Chiropractic Use, by Racial/Ethnic Category, Medicare Beneficiaries in Los Angeles County, 2008a.

aData are summarized by ZIP Code.
Table 4 illustrates disparities in the use of chiropractic services. The racial/ethnic composition of the Medicare B population was 60% white, with a relatively even distribution among the remaining race/ethnicity categories, and the other/unknown category accounting for the fewest beneficiaries. Among chiropractic users, the proportions of blacks and Hispanics were low, comprising only 1% each of all chiropractic users
Racial/Ethnic Composition of Medicare Beneficiaries and Chiropractic Users in Los Angeles County, 2008.

Small Area Variations in Chiropractic Users by Race/Ethnicity
We found variations by ZIP code in the number of beneficiaries who used chiropractic services. In many of the 124 ZIP codes in Los Angeles County, values of summary statistics were less than 11 and therefore suppressed. Overall variation by ZIP code among chiropractic users was relatively low (mean 66, standard deviation 42, coefficient of variation 0.64). Variation by ZIP code in the number of Asian chiropractic users was high (coefficient of variation 1.38); variation among whites was relatively low (coefficient of variation 0.69). Mean numbers of chiropractic users by ZIP code were too small to report for beneficiaries of black, Hispanic, or other/unknown race/ethnicity. As noted above, Asians and Hispanics had the highest and lowest rates, respectively, of chiropractic use among minorities. The map in Figure 1 depicts geographic variations in use of chiropractic services among Asian Medicare beneficiaries, and Figure 2 illustrates variations in use of chiropractic services among Hispanic beneficiaries.

Use of chiropractic services by Asian Medicare beneficiaries in Los Angeles County, 2008.

Use of chiropractic services by Hispanic Medicare beneficiaries in Los Angeles County, 2008.
Discussion
Utilization of chiropractic services under Medicare in Los Angeles County differed from national patterns The correlation between chiropractic physician availability and chiropractic use in Los Angeles County was weaker than that observed at the national level by Whedon and colleagues 23 (Spearman’s ρ 0.40 vs 0.68). Rates of use of chiropractic services were lower than the national average for all beneficiaries and for white beneficiaries (3% vs 7%, and 3.6% vs 8.0%, respectively), 24 and consistent with rates previously reported for whites in California statewide. 17 Among Asians and blacks, rates of use were slightly below the ranges previously reported for California statewide 17 (2.6% vs 3.4-8%, and 0.3% vs 1.2-1.5%, respectively); rates of use for Hispanics fell within the previously reported range (0.2% vs 0-2.1%). The racial/ethnic composition of chiropractic users reflected the greater diversity of Los Angeles County as compared with national statistics, which were reported as 96.4% white, 1.7% black, and other categories 1% or less. 17 We find it striking that the proportion of white Medicare beneficiaries who use chiropractic services in Los Angeles County (as well as California overall) is less than half the national average, given the general popularity of complementary and integrative health services in California. It is possible that the chiropractic profession’s historic roots among whites in the rural Midwest may present a cultural barrier to chiropractic use among older adults in an urban, multiethnic environment. Regional cultural differences may also account for strong differences in utilization rates between some Midwestern states (over 20% in North Dakota 17 ) and the West Coast.
Blacks and Hispanics in Los Angeles County may be underserved with regard to chiropractic care, and given the weak, statistically insignificant correlation between utilization and chiropractic physician availability, supply does not appear to be the sole causative factor. Reasons for these marked racial/ethnic disparities in chiropractic use remain uncertain, but may pertain to barriers to care, patients’ preferences, beliefs and reasons for seeking care, and the demographics and beliefs of chiropractic physicians. Racial/ethnic data for Medicare-active chiropractic physicians in Los Angeles County was not obtained as part of this study; however, in 2002, Cherkin et al reported that only 5% of complementary and integrative health care providers (licensed acupuncturists, chiropractors, massage therapists, and naturopathic physicians) were nonwhite. 26 In 2010, the National Board of Chiropractic Examiners reported that in 2009, the racial composition of US chiropractors was 85% white, 2.6% Asian/Pacific Islander, 1% Hispanic, 0.9% black, 0.4% Native American, and 10.2% other/mixed race. 27 In 2013, the US Bureau of Labor reported that US chiropractors were 95.8% white, 2.3% Asian, 2.3% Hispanic/Latino, and close to 0% black/African American. 28
It is possible that a preference for a same-race chiropractic physician and disproportionately small minority supply of such contributes to the racial/ethnic disparities demonstrated in this study. Malat and Hamilton explored this theme in their analysis of the 1999 “Americans’ Perceptions of Racial Disparities in Health Care” survey and concluded that the degree of preference for same-race health care providers among black patients is associated with perceptions of interpersonal racial discrimination in health care. 29 Their analysis suggests that there are many factors that contribute to same-race, difference-race, or no preference attitudes, which in turn implies that proportionate supply of minority chiropractic physicians alone would not be sufficient to counteract racial/ethnic disparities. Thorburn et al also studied discrimination in health care in relation to complementary and integrative health care use and reported that discrimination in health care was significantly related to use of herbal medicines alone, but not significantly associated with use of practitioner-provided complementary and integrative health care, specifically acupuncture, chiropractic, traditional healers, or herbalists, possibly due to a desire to self-treat in order to avoid interacting with a potentially discriminatory health care provider. 30 In other words, patients who report having experienced discrimination from any health care professional may be reticent to visit all health care professionals in general. Another reason for low use of chiropractic services among minorities may be poorer general health status. Persons with greater comorbidity may be more likely to seek care from medical doctors than chiropractors. The beliefs and attitudes of medical providers may also contribute to the observed racial/ethnic disparities and variations because they likely advise patients with regard to what type of practitioner or type of care to seek. Further research incorporating predictive modeling is needed to identify factors affecting racial and ethnic disparities such as perceived discrimination and cultural/immigration factors in utilization of chiropractic services.
Limitations
Inferences drawn from the results cannot be generalized to populations that are younger, outside the Unites States, or not covered by Medicare Part B. However, with 7502 subjects, statistical power was more than adequate. The US Census Bureau’s definition of Los Angeles County contains approximately 10 ZIP codes that are not included among the 124 ZIP codes identified by the Centers for Medicare and Medicaid Services as being located within Los Angeles County. Native American beneficiaries, who were sparsely distributed throughout the Los Angeles area, were included in the other/unknown category rather than a separate category. We analyzed for the year 2008 only; therefore, it is not possible to determine from this study whether utilization rates are changing over time, although on a national level the demographics of chiropractic utilization under Medicare have been slow to change. Finally, we were unable to account for unknown factors that likely influenced the choice whether or not to use chiropractic services.
Conclusion
Even in the highly diverse environment of Los Angeles County, striking disparities in the use of chiropractic services are evident. Consistent with national patterns of utilization, users of chiropractic services among Medicare beneficiaries in Los Angeles County were predominately white. Very low proportions of black and Hispanic beneficiaries used chiropractic services, and these groups are likely underserved with regard to chiropractic care. Because chiropractic care is an effective and low-cost option for the primary care of patients with spine-related conditions, the needs of patients with such conditions would be served by greater availability and utilization of chiropractic services within minority communities in Los Angeles County, particularly for low- and fixed-income older adults. Improved access to chiropractic services for minority populations will require better understanding of the possible causes of disparities, such as perceived discrimination and cultural/immigration factors within the black and Hispanic communities.
Footnotes
Acknowledgments
This research was performed at The Dartmouth Institute for Health Policy and Clinical Practice and Southern California University of Health Sciences.
Authors’ Note
The research described in this article was presented as a poster at the World Federation of Chiropractic 13th Biennial Congress; May 13-16, 2015; Athens, Greece.
Author Contributions
Dr Whedon was responsible for design, analysis, interpretation, writing the first draft, and final approval of the manuscript. Dr Kimura was responsible for critical revision and final approval of the manuscript. Dr Phillips was responsible for critical revision and final approval of the manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the National Center for Complementary and Integrative Health (Grant Number K01AT005092).
Ethical Approval
This study was approved by The Committee for Protection of Human Subjects (CPHS), Dartmouth College (Research Study No. 21613).
