Abstract
Congestive heart failure (CHF) has a high rate of morbidity and mortality. It is often accompanied by other medical and psychosocial comorbidities that complicate treatment and adherence. We conducted a proof of concept pilot project to determine the feasibility of providing integrative group medical visits plus mindfulness training for patients recently discharged with CHF. Patients were eligible if they had been discharged from an inpatient stay for CHF within the 12 months prior to the new program. The Compassionate Approach to Lifestyle and Mind–Body (CALM) Skills for Patients with CHF consisted of 8 weekly visits focusing on patient education about medications, diet, exercise, sleep, and stress management; group support; and training in mind–body skills such as mindfulness, self-compassion, and loving-kindness. Over two 8-week sessions, 8/11 (73%) patients completed at least 4 visits. The patients had an average age of 57 years. The most common comorbidities were weight gain, sleep problems, and fatigue. After the sessions, 100% of patients planned to make changes to their diet, exercise, and stress management practices. Over half of the patients who met with a pharmacist had a medication-related problem. Improvements were observed in depression, fatigue, and satisfaction with life. Integrative group visits focusing on healthy lifestyle, support, and skill-building are feasible even among CHF patients and should be evaluated in controlled trials as a patient-centered approach to improving outcomes related to improving medication management, depression, fatigue, and quality of life.
Heart failure is one of the leading causes of morbidity and mortality in the United States. 1 It is the most common hospital discharge diagnosis for patients over the age of 65 years and is often accompanied by multiple comorbid conditions. 2,3 As such, it is a major driver of health care costs. Despite advances in its treatment, the 50%, 5-year mortality rate for patients newly diagnosed with heart failure has not changed for at least 20 years. 4 The national 30-day readmission rate remains at 25% with a 40% to 50% six-month readmission rate. 5,6 Given these numbers, there remains a significant opportunity for improvement in the treatment for this disease.
Fatigue is a major component of the heart failure symptom complex. Fatigue is a persistent impediment to usual daily activities even when medical regimens are optimized and have maximal benefit on cardiac function. 7,8 Fatigue is also among the factors that contribute to reduced satisfaction with life and the capacity to engage in activities of daily living. 9,10 Improvement in quality of life has assumed major importance in evaluating the effect of pharmacologic and other therapeutic interventions. Despite improvements, the best medical therapies often fall short of restoring the highest quality of life and minimizing fatigue.
Depression, anxiety, and social isolation also commonly occur in individuals with heart failure and are associated with poor outcomes. 11 –18 Notably, psychosocial and behavioral factors have an impact on symptom perception, behavior, quality of life, and health care use, and they contribute to increased stress related to the self-management of a chronic medical condition. 19,20 For example, depression and anxiety can interfere with dietary adherence. 21 However, treatments that focus on just one behavior, such as exercise, may improve performance on one outcome, such as exercise capacity, without affecting overall quality of life. 22,23 Novel approaches are needed to improve overall self-care and thereby improve the psychosocial factors and behaviors that affect quality of life in patients with congestive heart failure (CHF). 24
Furthermore, medication nonadherence adversely affects patients’ symptoms and health outcomes, such as mortality, and adds $290 billion on cost to the health care system. 25 –27 However, medical regimens for patients with CHF are often complex and this complexity is compounded by common comorbid conditions in this population. 27 Limited adherence to the complex medical and behavioral regimens required to treat heart failure contributes to hospital readmission and health care cost. 28 Patient-centered instructions can improve patients’ understanding and use of medications, 29 but the availability of individualized medication counseling on busy clinical services is limited.
Self-care behaviors include not only medication management but also attention to diet, exercise, and sleep. 30 –32 Salt and fluid restriction, for example, can improve both signs and symptoms of CHF, as well as quality of life. 33 Increased awareness of the need for comprehensive lifestyle programs to support CHF programs has led to an expansion of cardiac rehabilitation programs and improved insurance coverage for these services. 34 Although programs that include a broad focus on medications, education and symptoms, and exercise have successfully improved quality of life and depression, 35 it is unclear whether additional counseling components can be feasibly included.
Mindfulness-Based Stress Reduction and mindfulness-based training in self-care are attractive additions to cardiac rehabilitation programs because they have demonstrated a positive effect on quality of life as well as on symptom improvement in patients with chronic conditions, including patients with depression and heart failure. 36 –39 Mindfulness interventions are generally delivered in group settings over several weeks, providing opportunities for increased social support as well as improved self-efficacy and psychological functioning. 40 –42 Enhanced self-efficacy and group support could contribute to increased adherence with behavioral and medication recommendations, leading to improvements in symptoms and overall satisfaction with life. 43
Group medical visits offer an intriguing opportunity to deliver comprehensive cardiac rehabilitation training including mindfulness. Group visits have been used since the early 1980s for pediatric health supervision as a way of enhancing group support, providing more intensive patient and family education, and improving psychosocial outcomes. 44 –46 This model has been successfully applied to prenatal care (the centering pregnancy model), 47 diabetes, 48 and other chronic conditions. 49 Starting in 1983, intensive group dietary counseling, yoga, and group support have been available to patients with ischemic heart disease, 50 but we were unable to find any published trials evaluating the impact of weekly integrative group medical visits combined with mind–body training for patients with CHF.
The commonsense appeal of an intervention combining education in self-care behaviors and medication management with group support and mind–body skills (see Figure 1 for conceptual model underlying the intervention) is counterbalanced by concerns that such an intervention may be too burdensome to be of practical value to fragile patients confronted with CHF. Therefore, we designed a proof of concept project to test an innovative model of care combining integrative group visits providing in-depth training about medications, nutrition, exercise, stress, and sleep, with weekly training in mindfulness and self-compassion. We wished to answer 3 questions:
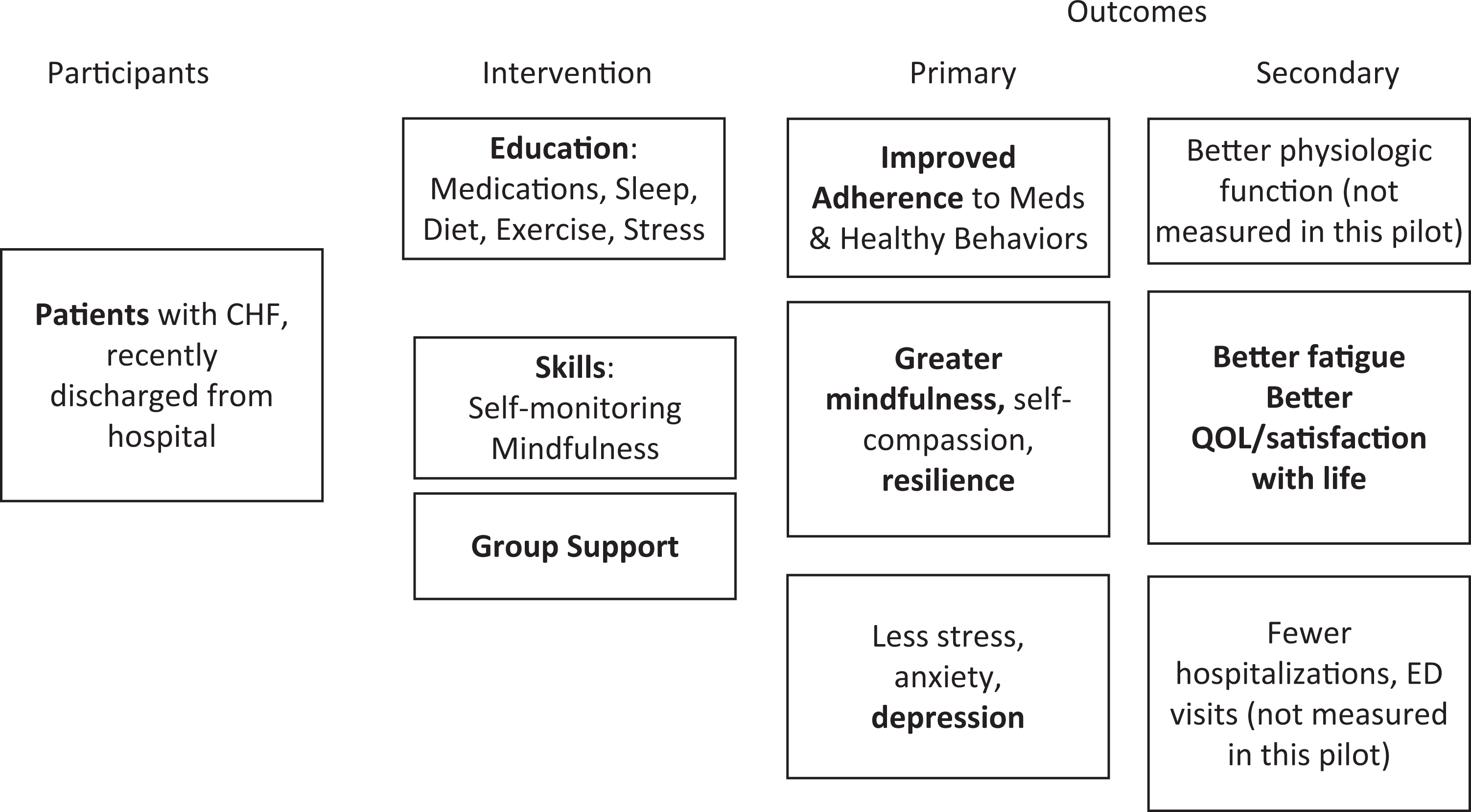
Conceptual model.
Is it feasible to recruit and retain patients with moderately severe CHF or do the sickest patients drop out?
Is it feasible to collect pre/post intervention measures?
If feasible, which measures appear to be most useful for future studies evaluating the effectiveness of this integrative approach?
Methods
To answer these questions, we conducted a small prospective cohort proof of concept project to assess the feasibility of combining integrative medical group visits with mind–body training in mindfulness, loving-kindness, and self-compassion.
Participants
Participants were eligible if they received care at our academic medical center’s Cardiomyopathy Clinic and had been discharged from hospital within the past 12 months for symptoms of heart failure. Nurse practitioners and physicians in the clinic provided patients brochures describing the intervention and invited them to participate if they spoke English, had a life expectancy of at least 3 months, lived within reasonable driving distance of the groups (less than 1 hour drive), had transportation, and were willing to attend 2-hour group sessions weekly for 8 weeks. Participants who agreed to participate were scheduled for the 8 weekly sessions and received packets by mail containing the intake questionnaire, directions to clinic, and a description of the group visit format.
Interventions
The group mindfulness training sessions were led by a licensed clinical psychologist who had 5 years of experience in teaching mindfulness meditation. The group medical visits were led or co-led by a family physician who reviewed all patient records and saw all patients weekly (Table 1). Additional presenters included a dietitian, a pharmacy faculty member and trainee, an exercise physiologist, and a clinical nurse specialist with expertise in sleep, stress management, and advance planning. At each visit, patients were encouraged to weigh themselves and take their own blood pressure with guidance from a medical assistant. Patients’ whose blood pressure was high or whose weight varied markedly week to week were encouraged to monitor weight and blood pressure at home and assisted in obtaining appropriate devices. All visits were recorded in the electronic medical record shared by the hospital and outpatient clinics in our academic health system.
Schedule of Group Integrative Medicine + Mindfulness Visits.

The mindfulness training portion of the visits was based on the widely used Mindfulness-Based Stress Reduction program developed at the University of Massachusetts. The first session defined mindfulness, introduced the mindful body scan, and provided a link to a free recording for participants to practice daily for 20 minutes. At each subsequent session, participants discussed their practice and learned a new mindfulness practice; for most sessions, these practices were paired with the general medical topic, for example, mindful eating for the session with the dietitian, mindful movement for the session with the exercise physiologist. The final sessions focused on mindful self-compassion for self, loved ones, and others.
Assessments
The 15-page baseline assessment used in the fall (reduced to 13 pages for spring session) included typical demographic information; it also asked patients to prioritize their top health concerns and health goals. In addition, a complete review of systems indicated additional health concerns to fully characterize the range of comorbid symptoms and conditions. A family medical history was included in the fall, but not the spring versions of the baseline assessment.
The baseline assessment also asked patients to list all medications and dietary supplements used in the past 30 days; any medication allergies or side effects; and encouraged patients to bring all medications to the third and seventh group visits to discuss with the pharmacist.
In order to help the clinicians plan visits to meet individual patient needs and to help patients reflect on their lifestyle, the assessment also asked about the following: Typical diet (breakfast, lunch, dinner, snacks; favorite foods; food intolerances); daily servings of fruits, vegetables, fish, meat, type of cooking oil, soda and juice intake; water intake; fast food intake; meals eaten with others; and whether or not they monitored salt intake. The intake form also asked about nutritional goals and challenges to meeting those goals. Activity (organized sports, teams, or dancing; unstructured activity such as biking, walking, or swimming); favorite physical activity; fun activities as a family; typical weekly activity Stressful life events including domestic violence, death in family, divorce, financial problems, serious illness in family member, and stress management strategies (eg, watching TV, listening to music, talking with a loved one, eating, and 10 other options) Sleep (bedtime, wake up time; napping patterns; trouble sleeping through the night; snoring; diagnosis of obstructive sleep apnea) Miscellaneous items (smokers in household, family strengths, time spent watching TV or on computer, and social support; goals for the group visits)
In addition, we used standard instruments to assess patient-reported factors.
Psychosocial Factors
These factors were assessed with the 29-item Patient-Reported Outcome Measurement Information System (PROMIS) questionnaire, which includes standardized, validated subscales for anxiety, depression, sleep, and fatigue. 51,52 We used Cohen’s widely used, 10-item Perceived Stress Scale to assess stress. 53 Diener’s Satisfaction with Life Scale was included as an overall measure of well-being, consistent with our focus on promoting progress toward positive health goals. 54
We also measured 2 factors hypothesized as being significant intermediaries in improving fatigue and satisfaction with life: mindfulness and resilience.
Mindfulness
Mindfulness was measured in 2 ways. For the fall group, we used Freiburg Mindfulness Inventory (FMI); the FMI contains 14 items and each item is ranked for how often (rarely = 1, 4 = almost always) the participant experiences each item 55 ; for example, “I am open to the experience of the present moment”; “I am able to appreciate myself”; “I experience moments of inner peace and ease, even when things get hectic and stressful.” Because patients asked for shorter questionnaires, for the second session, we switched to the 10-item Cognitive and Affective Mindfulness Scale–Revised (CAMS-R), which has a similar 4-point rating system for each item (1 = rarely or not at all; 4 = almost always) 56 ; for example, “It is easy for me to concentrate on what I am doing”; “I am able to accept the thoughts and feelings I have”; “I am able to focus on the present moment.”
Resilience
We used 2 measures, Smith’s Brief Resilience Scale 57 and Malarkey’s 22-item Ohio State University scale, which assesses resilience in 5 domains: Relational Engagement, Emotional sensibility, Meaningful action, Awareness of self and others, and Physical health behaviors (REMAP scale; see the appendix for the 22 items). This measure has a test–retest reliability of r = .80, good internal reliability (Cronbach’s α = .85), and excellent convergent validity in terms of correlations with other measures including Ego Resilience (r = .55), Brief Resilience Scale (r = .48), and the Mindful Attention Awareness Scale (r = .49) as well as negative correlations with depression (CES-D, r = −.36), loneliness (UCLA Loneliness Scale, r = −.62), and poor sleep (Pittsburgh Sleep Quality Index, r = −.37, unpublished data).
Analysis
Data were described using simple means, standard deviations, and percentages. No statistical comparison testing was done since there was no control group, and the sample size for pre/post measures precludes meaningful analyses. This was a proof of concept study.
This project was approved by the Ohio State University Office of Research Biomedical Institutional Review Board, 2014H0356.
Results
Subjects
Five patients enrolled in the 2013 session and 6 enrolled in the 2014 session; overall, 3 dropped out for a 73% completion rate. Of the 10 patients who completed baseline questionnaires, 5 (50%) also completed follow-up questionnaires. Several patients mentioned the length of the questionnaires (particularly for the first session) as a barrier to completing them.
Baseline Measures
At enrollment, patients’ average age was 57 years. In addition to CHF, other health conditions reported by 50% or more of patients included recent weight gain, sleep problems, decreased appetite, frequent urination, numbness or tingling in fingers or toes, diabetes, sleep apnea, back pain, fatigue, and medication side effects. Those who completed both pre- and postsession questionnaires did not report fewer health problems than those who completed only the baseline assessment (see Table 2). The average symptom severity on a 0 (none) to 10 (severe) numeric rating scale was 6.8 among those who completed all questionnaires compared with 5.5 among those who completed only the baseline assessments.
Baseline Age and Health of Entire Group Versus Those Who Completed Outcome Measures.
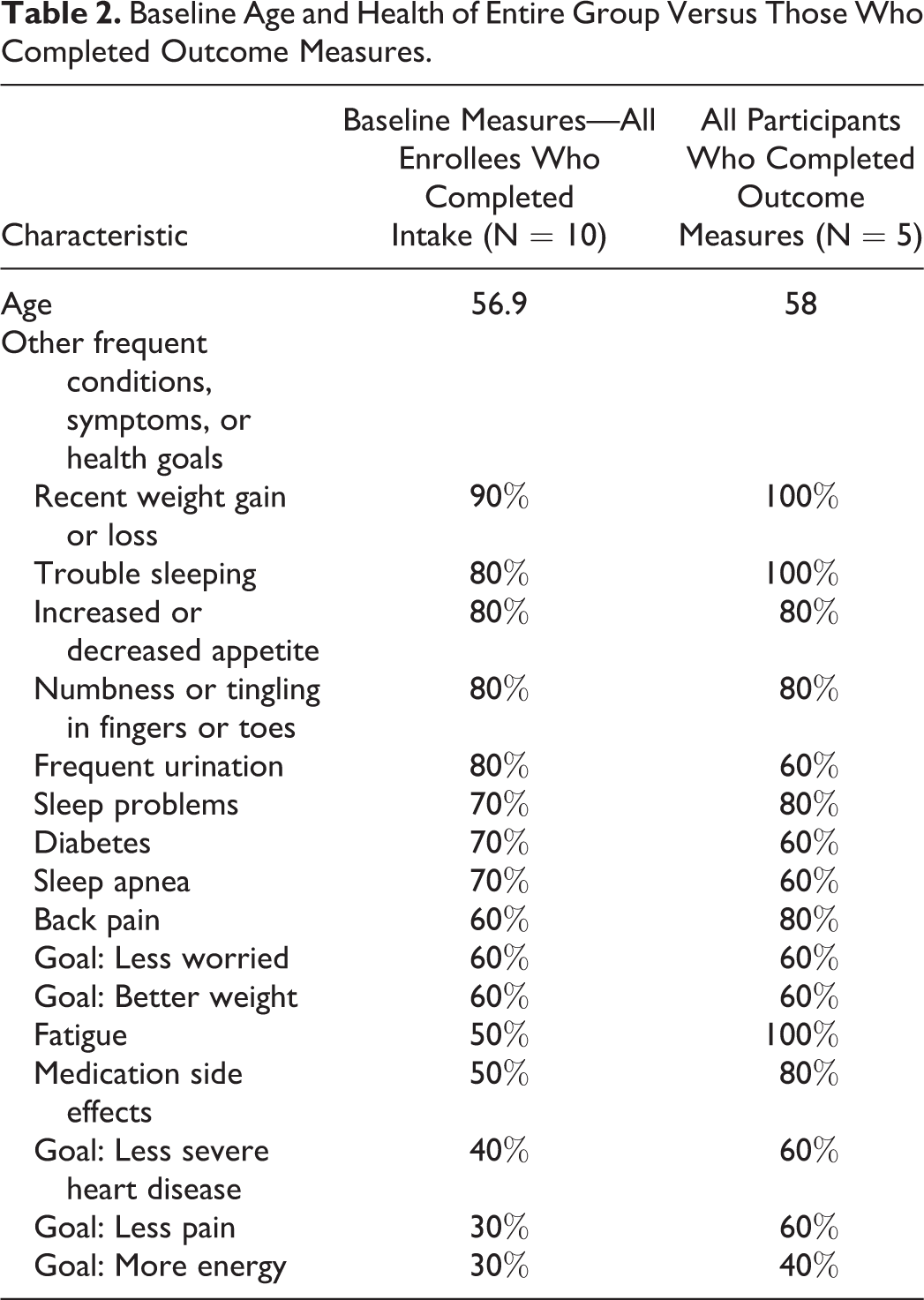
In addition to multiple comorbid conditions, participants reported additional health risks. Forty percent of participants reported living with a smoker. Two thirds reported a recent stressful life event other than their hospitalization, and one third served as the primary caretaker for someone else at home. No problems were reported less often by those who completed the follow-up questionnaires than those who did not.
Participants reported that the number of sessions was “about right,” and most wanted to continue to meet together after the 8 planned sessions had concluded. No sessions were identified as being superfluous, and no additional topics for discussion were identified.
The sample of 5 patients who completed both sets of questionnaires was too small for formal significance testing. Nevertheless, the responses provide important proof of concept information that motivates further exploration of this program. For example, as a result of participating in the program, 100% of patients planned to make changes in their diet, sleep, and stress management practices. The 9 patients seen by pharmacists had between 16 and 22 prescribed medications; 5 patients were identified as having a total of 14 medication-related problems. These concerns included concerns about adherence, medications listed in the medical record without a medical indication, ineffective dosages, and potential drug interactions. One patient was referred to the pharmacist for a separate comprehensive medication review. Pharmacists provided general group education regarding medications commonly used to treat CHF and products that should be used cautiously by patients with CHF, including prescription and over-the-counter medications and dietary supplements.
In addition, the questionnaires that appeared to show the most improvements from before to after the intervention (and most likely to be useful for a future adequately powered study) were the following: PROMIS subscales for fatigue (falling from 15.2 to 7.5) and depression (falling from 11.8 to 8.8), Diener’s Satisfaction with Life Scale (improving from 46 to 57); Malarkey’s REMAP measure of resilience (increasing from 43 to 54), and the Freiburg Mindfulness Scale (increasing from 14 to 34; Table 3).
Changes From Intake to Final Group Visit.

Most participants requested that the groups continue to meet after the 8 scheduled sessions were completed.
Discussion
To our knowledge, this is the first proof of concept project testing the feasibility of delivering a multimodal integrative medicine group visit plus mind–body skills training for patients with CHF. The proof of concept study supports the notion that such groups are feasible in terms of recruitment and retention. It is feasible to retain even patients who are quite sick with multiple symptoms and concerns in addition to CHF; those who drop out or decline to complete follow-up assessments do not appear to be sicker at baseline than those who continue to participate. However, participants found the length of the questionnaires burdensome, and it would be prudent in the future to reduce the length of the assessments to less than 10 pages. Future studies will need to focus on the most promising outcomes: fatigue, depression, satisfaction with life, resilience, and possibly mindfulness. Additional sessions may be added to complete questionnaires together or to transition to a more conventional rehabilitation program since participants seemed to enjoy the groups and asked for additional sessions.
Our patients reported high stress levels (average scores >20) on the Perceived Stress Scale compared with population normative values of 12 to 14 for healthy adults. 58 On the other hand, their scores were comparable to patients with severe CHF in a study evaluating the impact of transcendental meditation. 59 The high level of stress in these patients indicates that CHF is a condition that may be highly amenable to interventions that alleviate stress, such as training in mindfulness. It is known that the neurohormonal mediators of stress can lead directly to further clinical decompensation and increase mortality risk in this population. 60 Thus far, pharmacologic interventions have had at best incomplete impact on the stress and depression that are so common in this condition. Accordingly, nonpharmacologic interventions that can interrupt the cycle of stress and neurohormonal activation hold promise for improving survival and quality of life. It is also possible that psychosocial interventions addressing concerns with depression, anxiety, and perceived stress may require longer than 8 weeks to demonstrate significant benefits.
The group visits in this project differed from traditional hospital-based, home-based, or smartphone-based cardiac rehabilitation for patients with coronary artery disease in terms of having a strong explicit focus on mindfulness training as well as medications, nutrition, and exercise. 61 They also differed from the Ornish program, particularly in terms of our stronger emphasis on medications; time self-monitoring weight and blood pressure; a less restrictive Mediterranean, low-salt diet; and a greater focus on mindfulness, loving-kindness, and compassion meditation rather than yoga. 50,62 Our mind–body approach also differed somewhat from the Benson-Henry cardiac rehabilitation program, which focuses more on the Relaxation Response for patients with coronary artery disease than on mindfulness for patients with CHF. 63 However, like traditional programs, participants attended an average of 5 sessions (slightly more than half of the available). 64
Our group visits also differed from conventional mindfulness-based stress reduction programs in that we had a strong emphasis on biomedical and behavioral factors thought to be important for patients with CHF. Patients were seen by a physician at every visit and had weight and blood pressure measured. Pharmacists led 2 of the 8 visits in order to ensure that patients’ complex medical regimens (often managed by multiple specialists) were optimized and that patients understood what each of their medications were used to achieve. Given the large number of medications that patients were taking, pharmacists were able to identify and make suggestions to resolve a number of medication-related problems. Through this pilot project, work flow issues such as how to communicate and resolve medication-related problems were identified and resolved. A key element was the utility of the electronic health record in facilitating interprofessional communication. Patients were also counseled and had opportunities for questions and answers with a dietitian and an exercise physiologist, which were associated with planned changes in diet and exercise in all participants.
Conceptual Model
Our underlying conceptual model (Figure 1) was supported in part by this project, but we did not test some elements or find support for others. For example, we saw no changes in anxiety, sleep, perceived stress, or in the shorter scales measuring resilience or mindfulness. Larger sample sizes will be necessary to test the model with adequate statistical power. Because of the limited sample size, we cannot determine whether the apparent differences observed between the 2 sessions in measured mindfulness were due to random variability, differences in the sensitivity of the 2 instruments to detect changes in mindfulness, or differences between the participants in the 2 groups.
Limitations
As a proof of concept project, this study suffers from a small sample size, and use of changing measures to assess key outcomes as we adapted the assessment based on participant feedback. The project was carried out at a single academic institution and included only short-term self-reported outcome measures; future studies could include multiple sites, objective measures of exercise tolerance, and health care utilization, and include a longer follow-up period. In future studies, cost data would be useful in comparing the cost-effectiveness of this program to other programs. Future studies should include objective measures of medication and behavioral adherence and physiologic and clinical measures (eg, autonomic balance, baroreflex function, and sleep) as well as self-report measures.
Conclusion
Despite these limitations, this proof of concept project suggests that group integrative medical visits combined with mindfulness training are feasible for patients with CHF. Aside from the burden of completing lengthy questionnaires, patients enjoyed the sessions and expressed interest in ongoing group support. Future studies can focus on a few self-report outcome measures and may be able to add objective measures of medication adherence and physiologic measures of autonomic and baroreflex function, functional status, and ultimately of the rates of emergency room use and hospital readmission. These and other measures can be used to test the efficacy of novel interventions to address the considerable remaining unmet psychosocial and medical needs in the treatment of heart failure to reduce the morbidity, mortality, and high health care cost of this disease.
Footnotes
Appendix
REMAP Scale Itemsa.

| I feel supported by friends |
| I attend social functions |
| I talk with family members |
| I laugh |
| I like myself |
| I am peaceful |
| I am optimistic |
| I relax |
| I use my mental ability at work |
| I feel satisfied by my work |
| I feel my life has meaning |
| I feel in control of my life |
| I am learning |
| I reflect on my life |
| I am a good listener |
| I pray or meditate |
| I appreciate nature |
| I give to or serve others |
| I eat properly |
| I exercise |
| I abstain from smoking |
| I get refreshing sleep |
aRatings are made on a 4-point scale (1 = rarely, 4 = very frequently). No items are reverse scored.
Acknowledgments
We are grateful to Dr Ruslana Kurpita for leading the integrative medical visits and Dr Lisa Thornton for teaching the mindfulness meditation part of the visits. We are grateful to the clinicians and staff who assisted in referring and caring for the patients, creating and collecting the baseline and evaluation forms, and entering and managing the data.
Author Contributions
KK conceived of the project, oversaw data collection and analysis, organized the study team, drafted and revised the manuscript. CC assisted in the interpretation of the psychosocial data, and in writing and revising the manuscript. BM led the sessions on medication management, and assisted in collecting and interpreting the data on medication management and adherence, and in writing and revising the manuscript. PH assisted in planning the group medical visits, assisted in identifying eligibility criteria and recruiting patients, interpreting the data, and writing and revising the manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project was funded in part by in-kind contributions and in part by a gift from the Ross Heart Hospital at the Ohio State University Wexner Medical Center.
Ethical Approval
This project was approved by the Ohio State University Office of Research Biomedical Institutional Review Board, IRB #2014H0356.
