Abstract
High prevalence of undiagnosed cases of diabetes mellitus and poor knowledge, awareness, and practice has increased premature death, costly complications, and financial burden. A cross-sectional survey was conducted in November 2014 on 273 diabetics and 355 nondiabetics in 3 government homeopathic hospitals in West Bengal, India. A self-administered questionnaire assessing knowledge, awareness, and practice related to diabetes was used. A total of 17.5% to 29.3% of the participants were aware of the normal blood sugar level. Lack of insulin, frequent urination, hypertension, and poor wound healing were identified most frequently as the cause, symptom, association, and complications. A total of 35.5% to 46.5% said that diabetes was preventable; 14.1% to 31.9% knew that diabetes was controllable rather than curable. Consumption of planned diet, avoiding sugar, and testing blood sugar were the most frequently identified components of healthy lifestyle, diabetic diet, and diagnostic domain. Diabetics had higher knowledge and awareness than nondiabetics (P < .0001); still the latter need to be made aware and knowledgeable to curtail the ever-increasing burden of diabetes.
Diabetes mellitus is rapidly gaining a potential epidemic state all over the world. In 2014, about 387 million people (8.3% prevalence and 46.3% undiagnosed) were suffering from diabetes mellitus globally, of which 75 million people are from southeast Asia (prevalence 8.3% and undiagnosed 52.8%), and it is projected to be 592 million by 2035. 1,2 Among the diabetic population, 77% are living in low- and middle-income countries. 1 For every 12 people, one is diabetic; in every 2 diabetics one does not know that he or she has it; and every 7 seconds one person dies from diabetes mellitus, thereby amounting to 4.9 million deaths already in 2014. 1,3 Globally, more than 21 million live births have been affected by diabetes mellitus during pregnancy in 2013. 2 It not only poses a grave threat to the health of a mother and her child, but evidence shows that this can lead to an increased risk of type 2 diabetes mellitus later in life for the child. 2 Among those 20 to 79 years of age, 66 846 million people have been diagnosed with diabetes mellitus 3 ; 35 495 million people remained undiagnosed; 8.63 is the national prevalence; 9.11 is the diabetes comparative prevalence; and 1 039 980 million deaths have occurred, of which 54% are under the age of 60, and the per person cost is US$95. 1
Very recent studies conducted among diabetics and the general population in India found meager levels of knowledge and awareness related to diabetes mellitus and poor self-care practices. 4 –7 Similar community and hospital surveys in developing countries also unfolded unsatisfactory knowledge, awareness, and practices of the diabetic patients. 8 –12 Thus, the high prevalence of undiagnosed cases, and consequently poor knowledge, awareness, and practices, has directly increased premature deaths, costly complications, and financial burdens. The high cost of diabetes mellitus management and treatment indirectly provoke patients to choose complementary and alternative medicine therapies. 13 –18 Recent studies in India revealed that 1.5% of the diabetic population underwent homeopathic treatment for diabetes 19 and a considerable number of diabetics report at homeopathy hospitals 20,21 ; still the effectiveness of homeopathy has not yet rigorously been evaluated and the research evidence base has remained miniscule. 22
Evidence has showed that increasing knowledge regarding diabetes and its complications has significant benefits in management and treatment. 23,24 This study was intended, for the first time, to be conducted on the diabetic and nondiabetic patients visiting the homeopathic hospitals in West Bengal, India, to disclose their levels of knowledge and awareness of diabetes mellitus and practices of diabetics to manage and prevent complications. It would also reveal the differences between the responses and would identify the reasons for such differences.
Methods
A cross-sectional survey was conducted in November 2014 on patients (diabetics and nondiabetics/control) visiting as outpatients in 3 government homeopathic medical colleges of West Bengal.
The survey sample size was calculated to be 643 (margin of error 5%, confidence level 99%, population size 20 000, and response distribution unknown, estimated to be 50%). However, as we obtained 628 total responses (97.7% response rate), the confidence level was slightly reduced to 98.9%. The diabetics were selected by simple random method and nondiabetics by convenience sampling.
The inclusion criteria were patients aged 18 to 70 years, both sexes, literate, and willing to participate in the survey. Those patients who were illiterate, unwilling to participate in the survey, or unwilling to stay after the doctor consultation were excluded from the study. Before participation in survey, an information sheet was provided in local vernacular Bengali and written informed consent was obtained from each participant. Following that, a self-administered questionnaire in Bengali was distributed.
The questionnaire was divided into 4 sections (see supplementary material, available online at http://chp.sagepub.com/content/by/supplemental-data). Sections A, B, and C were for both diabetics and nondiabetics, and section D was for diabetics only. Section A sought data on sociodemographic details; questions were either open-ended or close-ended and provided options allowing to choose the appropriate ones. Section B consisted of 16 close-ended questions assessing the knowledge of diabetes. Section C had 4 questions gauging the awareness about diabetes. Section D contained 6 questions about self-care practices among diabetics. Patients were allowed to choose multiple alternatives, if they desired, among the options provided with regard to the knowledge and awareness questions. One mark was attributed to each selected option and finally summarized to calculate the total knowledge and awareness scores.
No universally accepted standardized questionnaire in local vernacular Bengali was available for the purpose. The questionnaire was developed by extracting items from previously validated questionnaires, 4,7 –10,12 along with little modifications as per patients’ perspective. It was translated and back-translated in standard procedure independently by 2 translators. The face and content validity of the study questionnaire was already established in earlier studies. The questionnaire was piloted on 5 patients in each setting before widespread distribution to check for the appropriateness of wording. After little modifications as per the feedback from the pilot sample, the questionnaire was finalized. It was easy and took only 5 to 10 minutes to complete. The questionnaire was explained verbally to the patients by research assistants. After completing the questionnaire, the sheets were collected and subjected to data analysis.
Various computational websites were used for sample size calculation and statistical analysis. Descriptive statistics were presented through frequencies and percentages for categorical data and mean ± standard deviation for continuous data. Independent t tests were used to analyze the difference between knowledge and awareness scores of diabetics and nondiabetics. Univariate (1-way analysis of variance and independent t tests) and multivariate analyses were conducted to examine the influence of different potential predictors on knowledge and awareness scores. P < .05 (2-tailed) was taken as statistically significant.
Results
Table 1 shows he sociodemographic details of the survey respondents. Mean age of the study participants was 53.8 (standard deviation [SD] 11.5) and 39.3 (SD 15.6), and body mass index was 23.6 (SD 5.3) and 22.2 (SD 3.7), for diabetics and nondiabetics, respectively. Majority of diabetics belonged to the age group of 46 to 60 years (49.8%), male gender (58.9%), resided at rural areas (38.8%), had education of 10th standard or less (44.3%), were married (89.4%), were dependent (42.1%), and had a monthly family income of less than INR 10 000 (49.1%). Majority of the nondiabetics belonged to the age group of 18 to 45 years (67.6%), male gender (57.2%), resided at urban areas (43.4%), had education of 10th standard or less (38.3%), were married (63.1%), were dependent (34.4%), and had a monthly family income of less than INR 10 000 (60.6%). A total of 98.9% diabetic participants and 92.1% nondiabetic participants had heard about diabetes. Among diabetics, 67.8% participants were suffering from diabetes for past 5 years or less and 29.3% were suffering from diabetes for more than 5 years. Source of diabetic education among diabetics were doctor (79.1%), friend (34.4%), and family member (31.5%), and among nondiabetics it was family member (56.0%), friend (51.3%), and doctor (50.2%).
Sociodemographics of The study Population: Diabetics (n = 273) and Nondiabetics (n = 355).

Abbreviations: CI, confidence interval; DM, diabetes mellitus.
aContinuous data presented as mean ± standard deviation.
bCategorical data presented as n (%).
Table 2 shows the percentages of correct knowledge responses, which were significantly higher (χ2 tests; P < .05 two-tailed) for diabetics than nondiabetics in most of the occasions. A total of 84.9% of diabetics and 91.8% of nondiabetics identified diabetes correctly as a noninfectious disease; 76.2% of diabetics and 58.0% of nondiabetics recognized diabetes as a chronic disease. Although suffering from diabetes, only 29.3% of diabetics knew the normal blood sugar level; and in nondiabetics, it was only 17.5%. The most frequently identified causes of diabetes were lack of insulin (47.6% diabetics and 59.7% nondiabetics), lots of sugar consumption (46.9% diabetics, 40% nondiabetics), heredity (59.3% diabetics, 43.7% nondiabetics), and mental stress (31.1% diabetics, 22.5% nondiabetics). Frequent urination was the most frequently identified symptom of diabetes (75.8% diabetics, 77.5% nondiabetics). A total of 47.3% diabetics and 40.6% nondiabetics recognized hypertension as the most frequently associated disease with hypertension. Among complications of diabetes mellitus, the respondents most frequently made out poor wound healing (52.4% diabetics, 43.7% nondiabetics), loss of vision (44.7% diabetics, 27.3% nondiabetics), and kidney failure (36.6% diabetics, 26.5% nondiabetics); 46.5% of diabetics and 35.5% of nondiabetics believed that diabetes was preventable; 31.9% of diabetics and 14.1% of nondiabetics knew that diabetes could be controlled rather than cured; 35.9% of diabetics and 49.3% of nondiabetics were unaware of hypoglycemic symptoms; and 42.5% of diabetics and 25.4% of nondiabetics knew how to manage this life-threatening condition.
Comparison of Correct Responses of Knowledge Questions Between Diabetics and Nondiabetics.

Abbreviations: CI, confidence interval; DM, diabetes mellitus.
*Chi-square test applied; P < .05 two-tailed considered as statistically significant.
Table 3 shows the levels of awareness that were significantly higher in diabetics than nondiabetics in most of the occasions (χ2 tests; P < .05 two-tailed). A total of 82.4% diabetics and 61.4% nondiabetics knew that antidiabetic medication should be continued lifelong. Consumption of healthy and planned diet was the most frequently identified healthy lifestyle (80.9% diabetics, 76.1% nondiabetics); avoiding sugar as the most frequently recognized component of diabetic diet (72.2% diabetics, 66.8% nondiabetics); and blood sugar test as the most well-known diagnostic domain for diabetes mellitus (91.2% diabetics, 92.4% nondiabetics).
Comparison of Correct Responses of Awareness Questions Between Diabetics and Nondiabetics.

Abbreviations: CI, confidence interval; DM, diabetes mellitus.
*Chi-square test applied; P < .05 two-tailed considered as statistically significant.
Table 4 describes the self-care practices of diabetics. A total of 77.3% diabetics regularly checked their blood sugar, 80.6% regularly visited their physician, 47.6% regularly took exercise, and 90.1% took their medicine without missing doses.
Self-Care Practices of Diabetics (n = 273).

Abbreviations: CI, confidence interval; BP, blood pressure.
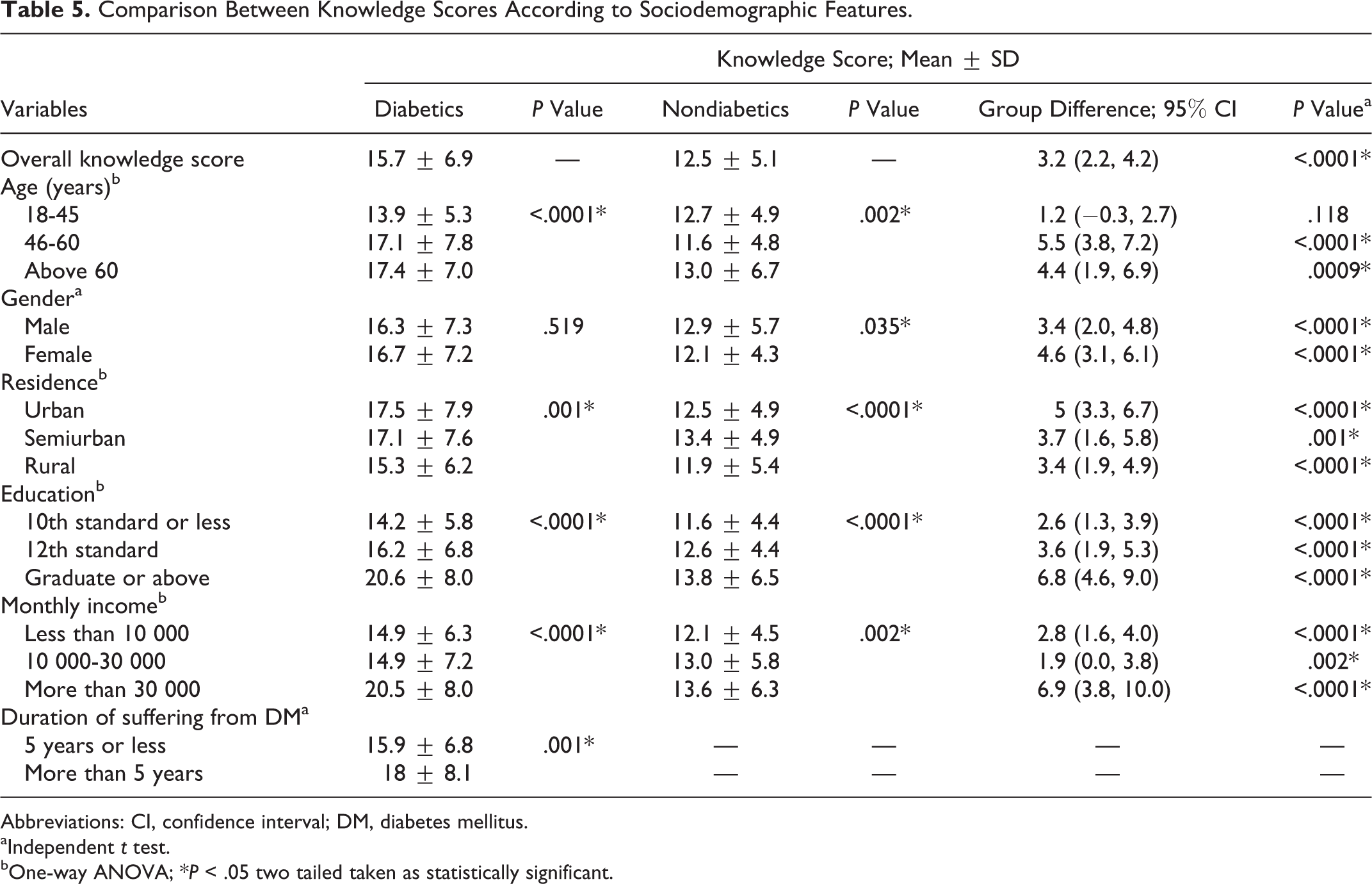
Table 5 shows the comparison of mean knowledge scores between diabetics and nondiabetics according to the suspected sociodemographic predictors. Overall knowledge score of diabetics was significantly higher than nondiabetics (15.7 ± 6.9 vs 12.5 ± 5.1; group difference 3.2; 95% confidence interval = 2.2-4.2; t = 6.430; P < .0001). Knowledge score of diabetics was influenced significantly by age (F = 22.346; P < .0001), residence (F = 7.091; P = .001), education (F = 61.021; P < .0001), monthly household income (F = 55.046; P < .0001), and duration of suffering from diabetes mellitus (t = −3.281; P = .001). Multiple regression retained only age (P = .023) and education (P = .0003) as the influencing variables of knowledge scores among the diabetics (adjusted model R2 = .097). Apart from age (F = 6.294; P = .002), residence (F = 7.865; P < .0001), education (F = 15.959; P < .0001), and income (F = 6.487; P = .002), gender (t = 2.111; P = .035) was also found to influence knowledge score of nondiabetics significantly; however, multiple regression retained only education (P = .019) as the influencing factor of knowledge scores among the nondiabetics (adjusted model R2 = .018). Overall, except the 18 to 45 age group (t = 1.581, P = .118), diabetics had significantly higher knowledge scores than nondiabetics across all the strata of the variables studied: age (46-60 years [t = 5.648; P < .0001], above 60 years [t = 3.427; P = .0009]), sex (male [t = 4.448, P < .0001], female [t = 6.017, P < .0001]), residence (urban [t = 4.729; P < 001], semiurban [t = 3.388; P = .001], and rural [t = 4.383; P < .0001]), education (10th standard or less [t = 4.010; P < .0001], 12th standard [t = 4.132; P < .0001], and graduate or above [t = 4.947; P < .0001]), and income (less than 10 000 [t = 4.481; P < .0001], 10 000 to 30 000 [t = 3.134; P = .002], and more than 30 000 [t = 4.354, P < .0001]).
Comparison Between Knowledge Scores According to Sociodemographic Features.
Abbreviations: CI, confidence interval; DM, diabetes mellitus.
aIndependent t test.
bOne-way ANOVA; *P < .05 two tailed taken as statistically significant.
Table 6 shows the comparison of mean awareness scores between diabetics and nondiabetics according to the potential predictors. Overall awareness score of diabetics was significantly higher than nondiabetics (6.5 ± 3.2 vs 4.9 ± 2.4; group difference 1.6; 95% confidence interval = 1.2-2.1; t = 6.902; P < .0001). Among diabetics, higher awareness scores were found to be associated with increasing age (F = 16.906; P < .0001), higher education (F = 7.599, P = .001), and higher duration of suffering (t = −3.709; P < .0001), but not influenced significantly by gender (t = −0.383; P = .702), residence (F = 0.647; P = .524), and income (F = 1.205; P = .300). Multiple regression retained only age (P = .006) as the influencing variable of awareness scores among the diabetics (adjusted model R2 = .019). On the other hand, higher awareness scores among nondiabetics was associated lower age group (F = 4.761; P = .009) and semiurban residence (F = 5.538; P = .004), but not influenced significantly by gender (t = 0; P > .999), education (F = 0.582; P = .559), and income (F = 2.256; P = .105); however, multiple regression could not identify a single variable to influence awareness score among the nondiabetics (adjusted model R2 = −.004). Except the 18 to 45 age group (t = 1.373, P = .174), diabetics had significantly higher awareness scores than nondiabetics across all strata of the variables: age (46-60 years [t = 5.913; P < .0001], above 60 years [t = 5.235; P < .0001]), gender (male [t = 5.461; P < .0001], female (t = 5.429; P < .0001]), residence (urban [t = 4.168; P < .0001], semiurban [t = 3.001; P = .003], and rural [t = 5.885; P < .0001]), education (10th standard or less [t = 3.948; P = .0001], 12th standard [t = 4.494; P < .0001], and graduate or above [t = 5.073; P < .0001]), and income (less than 10 000 [t = 4.511; P < .0001], 10 000 to 30 000 [t = 4.954; P < .0001], and more than 30 000 [t = 3.109; P = .0028]).
Comparison Between Awareness Scores According to Sociodemographic Features.

Abbreviations: CI, confidence interval; DM, diabetes mellitus.
aIndependent t test.
bOne-way ANOVA; *P < .05 two-tailed taken as statistically significant.
Discussion
Few similar community-based and hospital-based surveys have been conducted in India in recent times. A survey conducted in 4 states (Chandigarh, Maharashtra, Tamil Nadu, and Jharkhand) of India by Deepa et al in 2014 showed that only 41.6% of the general participants knew about the condition of diabetes, 56.3% knew that diabetes was preventable, and 51.4% knew about diabetic complications. Among diabetic participants, only 63.4% were aware that diabetes could be prevented, and 72.7% knew about diabetic complications. Knowledge of risk factors for diabetes was better among the diabetic subjects. 4 In 2013, a survey in central Delhi by Singh et al showed that 85.9% had basic knowledge regarding diabetes, 28.2% knew about the normal blood sugar level, and 17.2% used to do their routine investigation. 5 Another survey in Andhra Pradesh by Karam et al in 2012 showed that 66.67% of diabetic participants correctly answer the nature of disease, 75.21% knew that diabetes medication should be continued even after control of blood sugar, and 63.25% knew that diabetes cannot be cured. 6 In 2010, a household survey in Tamaka village, Kolar, by Muninarayana et al showed that among diabetic patients, 16% did not know about the risk factors of diabetes, 74% knew that diabetes had some complications, and 75% of the participants did not know about the long-term effects of diabetes. Among diabetics, only 54.8% were exercising regularly, 87.1% used footwear, 38.7% monitored blood sugar, and 9.7% visited doctors regularly. 7 The CURES-9 study by Mohan et al 24 in 2005 reported that, in Chennai, 75.5% people knew about a condition called diabetes; 60.2% to 76.7% knew that the prevalence of diabetes was increasing in India; and 22.2% to 41% were aware that diabetes could be prevented. Knowledge of the role of obesity and physical inactivity in producing diabetes was 11.9%; 19% to 40.6% knew that diabetes could cause complications.
Our study findings were similar to the results of other studies in India. 4 –7,25 The sample size of our study was large enough to generalize to the whole population availing homeopathic treatment in West Bengal. However, such a study was conducted for the first time in India on this specific cohort. Though the study findings showed diabetics had higher knowledge and awareness than nondiabetics, still the overall percentages were compromised. Policy makers should concentrate on the strategies promoting regular health education for patients in all health care setups—conventional, AYUSH (Ayurveda, Yoga, Unani, Siddha, Homeopathy, and Amchi/“Sowa Rigpa”/Tibetan Medicine), or integrated health care. Making the patients more aware and knowledgeable regarding the disease and encouraging self-care and self-management during treatment can reduce complications and health care burden, and thereby can help achieve optimal control of the disease. This target may not be very stiff, especially in the context when patient activation is not really deficient among the patients visiting Indian homeopathy hospitals. 26 Lower knowledge of nondiabetics is also worrisome and should be another target area for policy makers to curtail the conversion rate to diabetes mellitus. Scarcity of display in the premises of government homeopathic hospitals in West Bengal has already been identified in a recent study. 27 This may substantially contribute to the compromised knowledge score of the patients. Along with communicable diseases, noncommunicable and lifestyle disorders also need to be highlighted.
In Chennai, the Prevention, Awareness, Counseling and Evaluation Diabetes Project has been implemented to control diabetes. 28 National programs on noncommunicable diseases have already been undertaken by the Government of India and development of integrated models are being planned; still such initiatives suffer from lack of transparent policies. 29 To train physicians, 2 major education programs—Certificate Course in Evidence-Based Diabetes Management and diabetes educators National Diabetes Educator’s Program [NDEP]—have been started that can help build manpower to tackle the situation. 30,31
Further studies on different cohorts, on larger samples, and in different geographic areas are needed to identify the severity of the problem. Conducting similar studies a few years later may also prove fruitful to assess the effectiveness of patient education programs.
Conclusion
The study findings showed that though the major national project was implemented in India, the overall percentages of knowledge, awareness, and self-care practices were compromised. The findings showed diabetics had higher knowledge and awareness than nondiabetics. Further rigorous education programs need to be implemented on an urgent basis. Apart from the suffering population, the healthy population also needs to be made aware and knowledgeable to curtail the ever-increasing burden of diabetes in India.
Footnotes
Acknowledgments
The authors would like to acknowledge Dr Nikhil Saha, Acting Principal, Mahesh Bhattacharyya Homeopathic Medical College and Hospital; Dr Chapal Kanti Bhattacharyya, Principal-in-Charge, Midnapore Homeopathic Medical College and Hospital; and Dr Kajal Bhattacharyya, Principal-in-Charge, The Calcutta Homeopathic Medical College and Hospital, for permitting us to conduct the study in their institutions. The authors are also grateful to Dr Poulami Sen, Dr Rashidul Hakim, and Dr Debobroto Chatterjee for their sincere efforts in data collection. The authors are also thankful to the patients for their participation in this study.
Author Contributions
SS, MK, JSA, GC: concept, design, literature search, data interpretation, statistical analysis, manuscript preparation. SG, RC, KDD, AG, HH, RM, TB: clinical study and data acquisition. All the authors edited, reviewed, and approved the final article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
The institutional ethics committees of respective institutions approved the study prior to its initiation.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
