Abstract
Osteopathy in the cranial field is an approach used by manual and physical therapists. However, there is minimal information in the literature about patient experiences of this treatment. The present study was undertaken to explore patients’ experiences of osteopathy in the cranial field. Patients completed the Patient Perception Measure–Osteopathy in the Cranial Field and identified sensations they experienced during treatment. Additional measures of anxiety, depression, Satisfaction With Life, and Meaningfulness of Daily Activity were completed. The Patient Perception Measure–Osteopathy in the Cranial Field was internally consistent (Cronbach’s α = .85). The most frequently experienced sensations of osteopathy in the cranial field patients were “relaxed,” “releasing,” and “unwinding.” Satisfaction With Life and Meaningfulness of Daily Activity were positively associated with Patient Perception Measure–Osteopathy in the Cranial Field scores. Negative associations were observed between the Patient Perception Measure–Osteopathy in the Cranial Field and depression. Psychometric properties of the Patient Perception Measure–Osteopathy in the Cranial Field require further testing. The observed associations of Satisfaction With Life and depression with patients’ perceptions of osteopathy in the cranial field treatment needs to be tested in larger clinical manual therapy cohorts.
Introduction
Osteopathy is a manual therapy used by less than 4% of the Australian population, and of those who use osteopathy, only 6% of patients receive cranial osteopathic treatment. 1 Consequently, there is little evidence in the research literature about osteopathy in the cranial field treatment outcomes. 2,3
Osteopathy in the cranial field as a technique cannot readily be measured by observers or accessed via organic measures of change such as pathology or radiology. Also, the underlying theory of the osteopathy in the cranial field technique has been questioned, including the reliability of palpating the cranial rhythmic impulse. 4 –6
Of those studies that have reported on the outcomes of osteopathy in the cranial field, they are typically small clinical samples or individual case studies, 7,8 and they do not use a standardized self-report measure of what the patient perceives actually happens during osteopathy in the cranial field treatment. Outcomes of a specific treatment cannot be determined unless the patients are asked about their perception of the treatment or intervention. 9 –11 Subsequently, the Patient Perception Measure–Osteopathy in the Cranial Field was developed to investigate patients’ experiences of osteopathy in the cranial field treatment. In a previous article, the development of items for inclusion in the Patient Perception Measure–Osteopathy in the Cranial Field was reported. 12 Subsequent articles by the same authors are currently being written with 2 additional osteopathic (non–osteopathy in the cranial field) clinical populations to establish the psychometric properties of a revised measure of Patient Perception Measure–Osteopathy.
There are individual patient characteristics such as age, gender, education, employment status, chronic illness, and comorbid illnesses that have previously been found to influence the use of complementary and alternative medicines. 13,14 Previous studies have also observed a relationship between mental health (anxiety and depression), Satisfaction With Life, Meaningfulness of Daily Activity, and perceived treatment outcomes, particularly for patients with chronic pain. 15 –20 The presence of depression or anxiety has been associated with decreased treatment satisfaction and poorer patient outcomes. 21,22 Conversely, Satisfaction With Life and Meaningfulness of Daily Activity have been associated with more favorable health behaviors and treatment outcomes. 23 –27 When considering patients’ experience of osteopathy in the cranial field treatment, the relationship between patients’ individual health and social factors and their experience of osteopathy in the cranial field must be taken into consideration.
The specific aim of the present study was to identify what osteopathy in the cranial field patients experienced during their treatment. Secondary aims were to explore the affect of depression, anxiety, Satisfaction With Life, and Meaningfulness of Daily Activity on patients’ perception of their osteopathy in the cranial field treatment.
Methods
Ethics approval was obtained from the Victoria University Human Research Ethics Committee.
Participants
Two groups of participants were recruited: registered osteopaths in Australia and New Zealand who used osteopathy in the cranial field as their principal treatment approach, or as a substantial part of their treatment, and patients who attended osteopathy in the cranial field practitioners.
Osteopaths were recruited from a list of practitioners who had completed postregistration training in osteopathy in the cranial field, provided by the Sutherland Cranial Teaching Foundation of Australia and New Zealand. The research packages were sent to osteopaths in Australia (N = 5) and New Zealand (N = 4) who agreed to be participants in the study. Osteopathy in the cranial field patients were recruited by the osteopaths, because not all patients that the osteopaths were treating received osteopathy in the cranial field treatment at a consultation. Osteopathy in the cranial field is used often in conjunction with other osteopathic techniques. Therefore, the patients were recruited via a convenience sample by their treating osteopath.
Osteopaths invited 61 patients who satisfied the research criteria (adult, able to read and write English, able to give informed consent to participate) to complete the research package after their usual osteopathy in the cranial field treatment. Osteopathy in the cranial field patients who volunteered for the study completed the research package including: consent form, patient demographic survey, Patient Perception Measure–Osteopathy in the Cranial Field, and Hospital Anxiety and Depression Scale. 28 Forty-two completed research packages were returned via prepaid post to the researchers at Victoria University, equivalent to a response rate of 68.9%.
Measures
Patient Demographic Survey
The patient demographic survey recorded the following demographics: sex, age, education, employment status, marital status, religion observation, past medical history and medication history, and duration of their currently presenting condition. Additional data collected included the conditions currently being treated with osteopathy in the cranial field and whether or not patients used other treatments in combination with osteopathy in the cranial field, such as acupuncture, chiropractic, exercise, homeopathy, hospitalization, hydrotherapy, massage, medication, myotherapy, naturopathy, occupational therapy, osteopathy, physiotherapy, pilates, and surgery. Patients were also asked whether or not each of the additional treatments they used was helpful in managing their condition(s).
A list of 22 sensations and responses was included in the demographic survey, and patients were required to tick whether or not they experienced any of the sensations or responses during their osteopathy in the cranial field treatment. The sensations included Apathetic, Balancing, Centered, Cold, Depressed, Emotional, Energetic, Happy, Hardening, No Change, Nothing, Numb, Relaxed, Releasing, Restless, Sad, Softening, Straining, Tingling, Uncomfortable, Unwinding, and Warmth.
Two single-item Likert-type scale measures were included to assess the patient’s overall global Meaningfulness of Daily Activity and their current Satisfaction With Life. These items were “Overall how meaningful are your daily activities?” and “Overall how satisfied are you with your life?” Both the measures were 7-point Likert-type scales ranging from 0 (not at all meaningful, not at all satisfied) to 6 (extremely meaningful, extremely satisfied), as depicted in the rating scales. The Meaningfulness of Daily Activity Flesch-Kincaid Grade reading level was 10.8, and the Flesch reading ease 40.7. The Satisfaction With Life Flesch-Kincaid Grade reading level was 7.6, and Flesch reading ease 62.1, as assessed through Microsoft Word (Microsoft Corp, Redmond, WA). 27
Patient Perception Measure–Osteopathy in the Cranial Field
The Patient Perception Measure–Osteopathy in the Cranial Field 12 is a 33-item self-report measure developed to identify patient perceptions of osteopathy in the cranial field treatment. Items were allocated to 1 of 6 theoretically constructed domains: Education and Information (5 items), Efficacy/Satisfaction with Treatment (5 items), Physical Perception of Treatment (9 items), Therapeutic Relationship (2 items), Emotion/Mood (9 items), and Cognition (3 items). Examples of the responses and scoring of individual Patient Perception Measure–Osteopathy in the Cranial Field items are provided in Figure 1. The psychometric properties have been investigated previously (unpublished data), and modifications to the measure are currently being undertaken and tested in a non–osteopathy in the cranial field clinical population.

Sample items and scoring methods from the Patient Perception Measure–Osteopathy in the Cranial Field.
Hospital Anxiety and Depression Scale
The Hospital Anxiety and Depression Scale is a brief self-report screening measure to identify possible cases of clinical anxiety and/or depression in a medical outpatient clinic, and it takes the patient approximately 10 minutes to complete. The form consists of 7 depression items and 7 anxiety items, and these items are presented as alternative anxiety and depression questions. Each of the 14 Hospital Anxiety and Depression Scale items is scored from 0 to 3, and the total scores for the anxiety and depression subscales range from 0 to 21. Test authors report that the Hospital Anxiety and Depression Scale is internally consistent, and Cronbach’s α for Hospital Anxiety and Depression Scale Depression and Anxiety was .90 and .93, respectively. The measure requires the patient to select from 4 possible alternatives in response to each of the 14 questions. 28 The scores obtained from the Hospital Anxiety and Depression Scale have also been used to determine the presence and/or severity of clinical disorders (Anxiety or Depression), where scores ranging from 0 to 7 indicate No Disorder (Normal), 8 to 10 a Mild Disorder, 11 to 14 a Moderate Disorder, and scores above 15 indicate there is a Severe Disorder.
Data Analysis
Data were entered into and analyzed using SPSS 20 (IBM Corp, Armonk, NY). Descriptive data were compiled from the patient demographic survey as well as duration of treatment, sensations experienced during osteopathy in the cranial field treatment, comorbid conditions, and treatments used apart from osteopathy in the cranial field.
The Satisfaction With Life, Meaningfulness of Daily Activity, and Hospital Anxiety and Depression Scale were scored as recommended by the authors, 27,28 providing a measure of anxiety and depression, Satisfaction With Life, and Meaningfulness of Daily Activity. Patient Perception Measure–Osteopathy in the Cranial Field item and total scores were calculated for each of the 6 domains: (a) Education/Information; (b) Satisfaction with Treatment; (c) Physical Perception of Treatment; (d) Therapeutic Relationship; (e) Emotion and Mood; and (f) Cognitive Functioning.
Data were not normally distributed; therefore, nonparametric inferential and correlation statistics were used for the analysis. The Patient Perception Measure–Osteopathy in the Cranial Field total and domain scores were correlated with the Meaningfulness of Daily Activity, Satisfaction With Life, and scores obtained on the Hospital Anxiety and Depression Scale Depression and Anxiety subscales using Spearman’s ρ. Number of pain sites, duration of pain, number of comorbid health conditions, number of treatments used, and number of sensations experienced during osteopathy in the cranial field treatment affected Patient Perception Measure–Osteopathy in the Cranial Field scores were also correlated with the total Patient Perception Measure–Osteopathy in the Cranial Field score using Spearman’s ρ. The effect of demographic variables and sensations experienced during osteopathy in the cranial field treatment were tested with Mann–Whitney U tests or Kruskal–Wallis tests. Alpha was set at P < .05. Internal consistency of the Patient Perception Measure–Osteopathy in the Cranial Field and the Hospital Anxiety and Depression Scale was calculated using Cronbach’s α.
Results
Participants
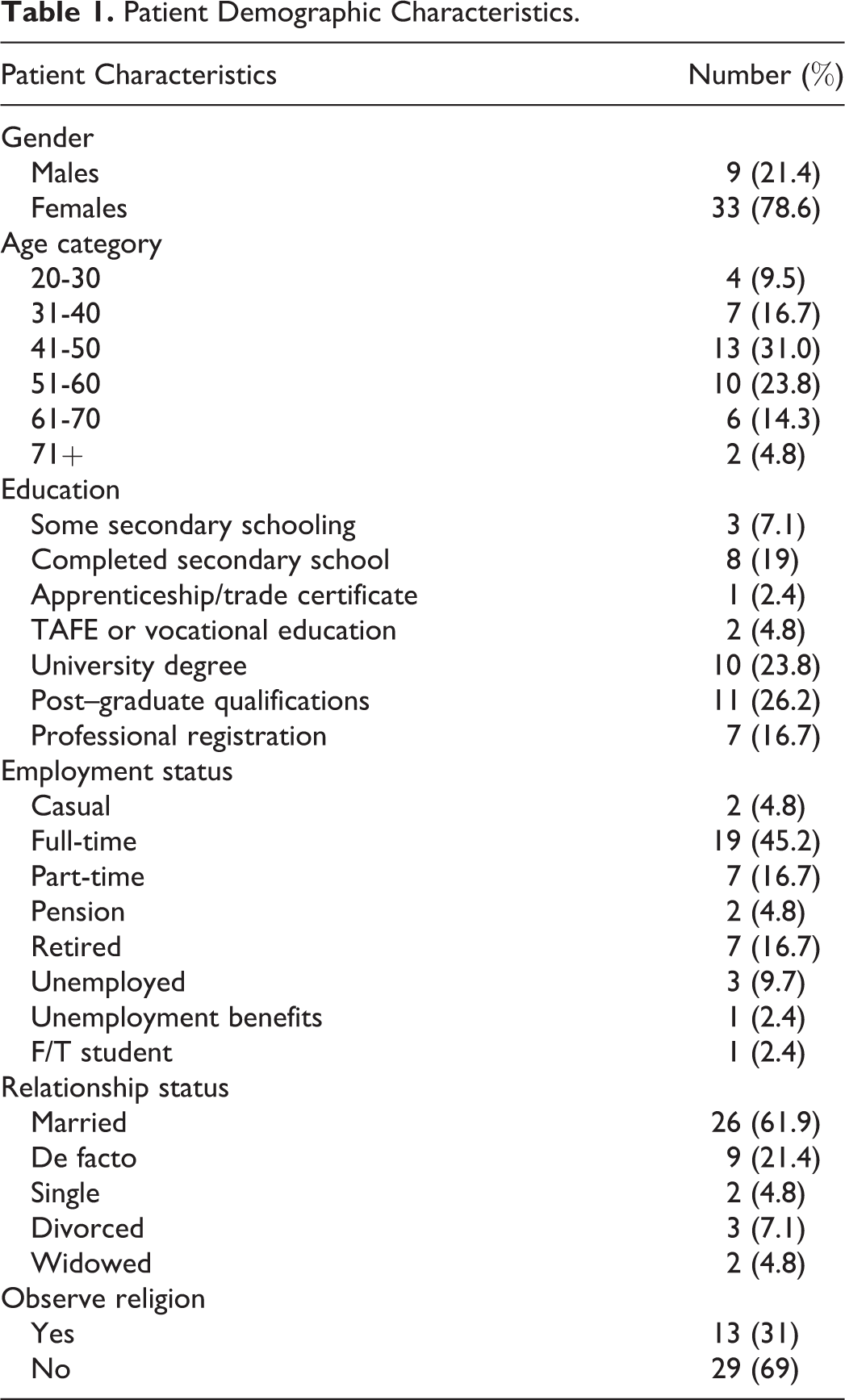
The demographic characteristics of patients who participated in this study are summarized in Table 1. There were no statistically significant differences in the total Patient Perception Measure–Osteopathy in the Cranial Field score for gender, age, education, employment status, relationship status, observance of a religion, and pain duration. Females demonstrated a statistically significant higher mean score for Domain 2 Satisfaction with Treatment. A Mann–Whitney U test revealed a significant difference in the Satisfaction With Treatment (Males: median = 20.50, n = 8; females: median = 23.00, n = 33; U = 70.00, z = −2.058, P = .04, r = −.32).
Patient Demographic Characteristics.

Reason for Attending Osteopathy in the Cranial Field Practitioner
The most common reasons for attending for osteopathy in the cranial field treatment were neck and shoulder pain (21.4%) and lower back pain (14.3%). The number of pain sites identified by participants ranged from 1 (11.9%) to 7 (2.4%) sites. Most participants experienced either 3 (23.8%) or 4 (28.6%) pain sites. There were no significant correlations between the number of pain sites and Patient Perception Measure–Osteopathy in the Cranial Field scores.
The chronicity of the disorders being treated was reflected in the duration of the condition that the patient was receiving osteopathy in the cranial field treatment for. There were 21.4% of patients with pain duration of 0 to 6 months, 14.2% for 6 to 12 months, 2.4% for 12 to 18 months, and 61.9% of patients had pain duration of longer than 18 months. This chronicity may in part be attributed to the age of patients being predominantly over the age of 40 (73.81%) and being more likely to have either illnesses or injuries that require long-term management. However, there were no significant correlations identified between pain duration and Patient Perception Measure–Osteopathy in the Cranial Field scores.
Additional Health Issues Reported by Osteopathy in the Cranial Field Patients
Of the major illnesses identified in Australia, both chronic and acute, the comorbid conditions that were reported most often in the current sample were psychological distress (anxiety and depression; Table 2). Of note was the higher prevalence in the current sample of patients who experienced anxiety than reported in the general Australian population. There was no correlation between the number of comorbid health conditions and Patient Perception Measure–Osteopathy in the Cranial Field scores.
OCF Patients’ Prevalence of Medical Conditions Compared With Australian General Population Prevalence (2011-2012).

Abbreviation: OCF, osteopathy in the cranial field.
a Australian Bureau of Statistics (2013) Australians Health Survey. 39 Note: prevalence of arthritis, diabetes, heart disease, hypertension, high blood pressure, and osteoporosis increased with age.
b Australian Institute of Health and Welfare (2012) Australia’s Health. 37
Complementary and Alternative Medicine and Treatment Modalities
The number of treatments patients used ranged from 1 to 9 (mean 4.43 = treatments), and the most frequently associated treatments with osteopathy were exercise (61.9%), massage (45.2%), and pilates (45.2%). Individual patients used 14 different treatments apart from osteopathy in the cranial field (osteopathy) to manage their comorbid conditions and presenting conditions. The use of each allopathic and complementary and alternative medicine treatment is summarized in Figure 2. The combinations of treatments varied according to the comorbid conditions individual patients had been diagnosed with and their personal characteristics. Spearman’s ρ failed to identify any significant relationship between the number of treatments used and Patient Perception Measure–Osteopathy in the Cranial Field scores, and there were no statistically significant differences in the total Patient Perception Measure–Osteopathy in the Cranial Field score between those patients who did and did not undertake a particular treatment. Mann–Whitney tests did not reveal any significant differences between any of the treatments used in conjunction with osteopathy in the cranial field and scores on the Patient Perception Measure–Osteopathy in the Cranial Field (P > .05).
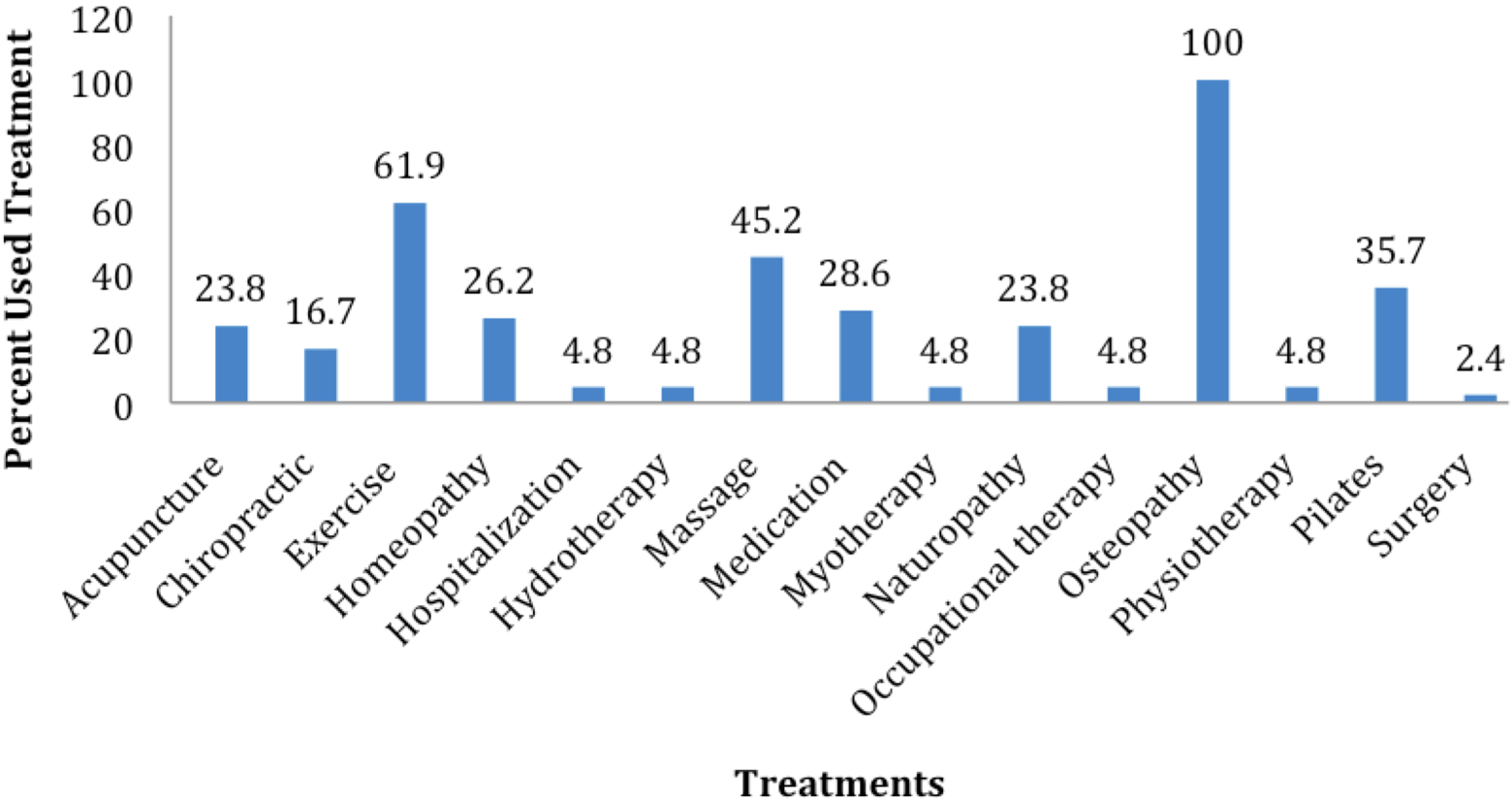
Percentage of osteopathy in the cranial field patients who used other treatments.
For Item 16 on the patient demographic survey, “Have you noticed any difference since receiving osteopathy in the cranial field as part of your usual osteopathy treatment?” 78% responded yes, 19% responded maybe, and no osteopathy in the cranial field patients reported that their treatment had not made a difference. The majority of osteopathy in the cranial field patients would appear to have been satisfied with their treatment as 39/42 (92.9%) indicated they would recommend osteopathy in the cranial field to friends or family.
There were 23/42 (54.8%) of participants who reported they were taking medication prescribed by their doctor. Of the participants taking medication 54.7% took 1 medication only, 31% took 2 medications, 14.3% took 3 medications, 11.9% took 4 medications, and only 4.8% (2 persons) took 5 medications. Pain medications had the highest incidence of use (21.4%). Other medications used by participants were prescribed for respiratory conditions (11.9%), cardiac conditions (9.5%), hypertension (9.5%), high cholesterol (7.1%), hormone replacement therapy (7.1%), depression (7.1%), and cancer (4.8%). Less commonly used medications (2.4%) included antipsychotics, anti-anxiety medications, and thyroid medications. There was no statistically significant difference in the Patient Perception Measure–Osteopathy in the Cranial Field total score between patients who reported using a medication and those who did not.
Association Between Measures
Associations between the Patient Perception Measure–Osteopathy in the Cranial Field score and the other measures used in the study are summarized in Table 3.
Associations Between SWL, MDA, Anxiety, Depression, and PPM-OCF.

Abbreviations: SWL, Satisfaction with Life; MDA, Meaningfulness of Daily Activities; HADS, Hospital Anxiety and Depression Scale; HADSa, HADS Anxiety Score; HADSd, HADS Depression Score; PPM-OCF, Patient Perception Measure–Osteopathy in the Cranial Field.
**Correlation is significant at the .01 level (2-tailed). *Correlation is significant at the .05 level (2-tailed).
Positive Relationships
The 6 domains of the Patient Perception Measure–Osteopathy in the Cranial Field were developed from the published literature pertaining to patient perception of physical therapies, including osteopathy. 12 In the current study, the sample was small and it was not appropriate to perform any factor analysis on the data.
Correlation of the measures, including the Patient Perception Measure–Osteopathy in the Cranial Field, confirmed that all of the 6 domains in the Patient Perception Measure–Osteopathy in the Cranial Field were positively and significantly associated with the total Patient Perception Measure–Osteopathy in the Cranial Field score. Table 3 also demonstrates there were positive and significant associations between Satisfaction With Life and Education and Information (P < .05), Satisfaction With Treatment (P < .05), Therapeutic Relationship (P < .05), Emotion and Mood (P < .01), Cognitive Functioning (P < .05), and the total Patient Perception Measure–Osteopathy in the Cranial Field score (P < .05). There was also a significant positive association between Meaningfulness of Daily Activity and Patient Perception Measure–Osteopathy in the Cranial Field Satisfaction with Treatment (P < .05) and Emotion and Mood (P < .05), where higher scores on Meaningfulness of Daily Activity were associated with higher scores on Satisfaction with Treatment and Emotion and Mood.
Negative Relationships
Patient Perception Measure–Osteopathy in the Cranial Field Satisfaction With Treatment, Physical Perception of Treatment, Emotion and Mood, and the total Patient Perception Measure–Osteopathy in the Cranial Field score were negatively associated with Hospital Anxiety and Depression Scale Depression (Table 3). Higher scores on Depression were significantly associated with lower scores of patient perception of osteopathy in the cranial field. Education and Information, Therapeutic Relationship, and Cognitive Functioning were negatively associated with Depression, but these associations were not significant. Anxiety was not significantly associated with any of the Patient Perception Measure–Osteopathy in the Cranial Field scores.
Sensations and Symptoms Experienced During Osteopathy in the Cranial Field Treatment
The mean number of sensations experienced by participants during treatment was 4.5 (range = 1-12). On the patient demographic survey there were 22 sensations to select from. Fifteen sensations were experienced during treatment by at least 2 participants, and 20 of the 22 were selected by at least 1 participant. Figure 3 depicts 15 sensations participants experienced during osteopathy in the cranial field treatment (sensations with less than 2% of participants reporting the sensations were not included in Figure 3). Fifteen sensations that patients experienced were analyzed to ascertain whether the Patient Perception Measure–Osteopathy in the Cranial Field score or domain scores were significantly different for those patients who experienced the sensation versus those who did not. Domains 4 and 6 did not demonstrate any significant difference between those who experienced a sensation versus those who did not.

Sensations experienced by osteopathy in the cranial field patients during their treatment.
Patients who indicated that they experienced the Releasing sensation had significantly higher scores for Domains 1, 3, and 5 as well as the total Patient Perception Measure–Osteopathy in the Cranial Field score. Mann–Whitney U tests revealed significant differences. In Domain 1, Education and Information, where patients who experienced a releasing sensation had higher scores than those who did not (median = 23.00, n = 31, vs median = 19.00, n = 11; U = 82.50, z = −2.53, P = .011, r = −.39). In Domain 3, Physical Perception, patients who experienced a releasing sensation had higher scores than those who did not (median = 32.00, n = 31, vs median = 27.00, n = 11; U = 73.00, z = −2.79, P = .005, r = −.43). Patients who experienced a releasing sensation also had higher scores on Domain 5, Emotion and Mood, than those who did not (median = 39.00, n = 29, vs median = 37.00, n = 11; U = 91.50, z = −2.07, P = .0038, r = −.33). While for the total Patient Perception Measure–Osteopathy in the Cranial Field score patients who experienced a releasing sensation had higher scores than those who did not (median = 131.50, n = 28, vs median = 124.00, n = 11; U = 63.00, z = −2.84, P = .004, r = −.45).
Patients who experienced a Centered sensation had significantly higher scores for Domain 1 and the total Patient Perception Measure–Osteopathy in the Cranial Field score. Mann–Whitney U tests revealed significant differences in Domain 1, Education and Information, where patients who experienced a Centered sensation had higher scores than those who did not (median = 25.00, n = 5, vs median = 20.50, n = 36; U = 22.00, z = −2.72, P = .004, r = −.44). However, for the total Patient Perception Measure–Osteopathy in the Cranial Field score patients who experienced a Centered sensation had higher scores than those who did not (median = 139.00, n = 5, vs median = 129.00, n = 33; U = 33.00, z = −2.14, P = .032, r = −.33).
Those patients who experienced a balancing sensation had significantly higher scores for Domain 2 and 5. Mann–Whitney U tests revealed significant differences in Domain 2, Satisfaction with Treatment, where patients who experienced a balancing sensation had higher scores than those who did not (median = 23.50, n = 16, vs median = 22.00, n = 24; U = 113.00, z = −2.20, P = .028, r = −.35. However, for Domain 5, Emotion and Mood, patients who experienced a balancing sensation had higher scores than those who did not (median = 40.00, n = 16, vs median = 138.00, n = 23; U = 114.00, z = −2.01, P = .044, r = −.32.
Satisfaction With Life and Meaningfulness of Daily Activities
Descriptive statistics for the Satisfaction With Life and Meaningfulness of Daily Activity are presented in Table 4. The majority of participants (99.9%) rated their Satisfaction With Life between “Occasionally satisfied” (3) to “Extremely satisfied” (6). No participants reported feeling less than “Occasionally satisfied with their life.” On the Meaningfulness of Daily Activity 88.1% of participants rated their Meaningfulness of Daily Activity as being between (3) “Occasionally meaningful” and (6) “Extremely meaningful”; 2 participants did not find their daily activities to be “At all meaningful.”
Descriptive Statistics and Internal Reliability of the Outcome Measures Used.

Abbreviations: HADS, Hospital Anxiety and Depression Scale; PPM-OCF, Patient Perception Measure–Osteopathy in the Cranial Field; SD, standard deviation; α, Cronbach’s α.
a If Item 22 deleted, α = .595.
b Two items only in this domain; α reliability not appropriate.
c If Item 29 deleted, α = .739.
d Three items only in this domain; α reliability not appropriate.
Patient Perception Measure–Osteopathy in the Cranial Field
Descriptive statistics for each of the Patient Perception Measure–Osteopathy in the Cranial Field subscales and total Patient Perception Measure–Osteopathy in the Cranial Field score are summarized in Table 4. Internal consistency (α) of the Patient Perception Measure–Osteopathy in the Cranial Field 33-item measure was .847, and the subscales ranged from .780 to .016. While the subscales may not reach acceptable levels of reliability, the overall measure is reliable. The measure requires modifications prior to further testing of the psychometric properties.
Hospital Anxiety and Depression Scale
Descriptive statistics for the Hospital Anxiety and Depression Scale are presented in Table 4. The majority of participants were within the normal ranges (0-7) for anxiety (73.2%) and depression (90.2%) as assessed on the Hospital and Anxiety and Depression subscales. There were 11 participants (26.8%) who were anxious and 4 participants (9.8%) who were depressed. One person did not complete an item related to anxiety, and 1 person did not complete an item related to depression. These questionnaires were not included in the analysis. Mann–Whitney U tests revealed a significant difference in Domain 5, Emotion and Mood, scores of depressed persons compared with those who were not depressed (median = 34.00, n = 4, vs median = 39.00, n = 35; U = 28.00, z = −1.96, P = .05, r = −0.31). Mildly depressed patients had a lower score on Emotion and Mood (median = 34.00) than patients within the normal range for depression (median = 39.00).
Discussion
The present study reports on the perceptions of 42 patients presenting to osteopaths for osteopathy in the cranial field treatment. Patients displayed a similar profile to previous research into Australian osteopathic practice. The Patient Perception Measure–Osteopathy in the Cranial Field was used in the present study to assess what patients believed happened during treatment. Patients were also asked what sensations they experienced during treatment. The internal consistency of the measure was acceptable overall; however, it requires modifications prior to testing on a larger clinical sample. Sensations experienced, gender, depression, Satisfaction With Life, and Meaningfulness of Daily Activity affected the patients’ perception of their osteopathy in the cranial field treatment, as measured on the Patient Perception Measure–Osteopathy in the Cranial Field. These factors need to be taken into consideration in clinical settings when patients’ manual treatment outcomes are being evaluated.
A study on the complementary and alternative medicine use in Australia, stated females, aged 18 to 43, who were employed, well educated, with private health insurance coverage, and with higher than average incomes tend to use more complementary and alternative medicine. 29 The patient cohort in the present study is predominantly female (78.6%), aged between 18 and 50 years of age (56.1%), educated to a tertiary degree level or higher (66.7%), and who were currently employed (66.7%). Therefore, it can be deduced that the sample population in the present study represents on average, well-educated people who are consequently more likely to be on higher levels of income and as a result are likely to use more complementary and alternative medicine. Consequently, the current clinical sample, albeit small, is representative of the patients who use complementary and alternative medicine, including manual therapy in Australia. 10,29,30 Consistent with previous research into Australian osteopathic practice, 1,31 the condition(s) being treated were predominantly back pain (33.3%), neck pain (19.5%), and headaches (19.5%).
Age, education, employment status, and marital status did not affect patients’ perceptions of osteopathy in the cranial field treatment. There has been previous research that would refute this finding in that these demographic variables have been found to be related to the patient’s satisfaction with manual and physical therapies. 32,33 Female osteopathy in the cranial field patients were however more satisfied with their treatment than males; females had significantly higher scores than males on Domain 2, Satisfaction with Treatment (mean = 22.15, standard deviation = 2.32, vs mean = 20.50, standard deviation = 1.93, respectively). This finding is in contrast to the review by Sitzia and Wood, 34 who reported that gender does not impact patient satisfaction. It may be that there is a link between the gender of the practitioner and gender of the patient, as has previously been described. 35,36 However, this finding requires further testing in manual therapy samples.
The construct validity for the Patient Perception Measure–Osteopathy in the Cranial Field is enhanced by the fact that the total Patient Perception Measure–Osteopathy in the Cranial Field score was not influenced by the patient’s current or previous use of other health care services. This is important to establish, as the patients in the present study were utilizing other health care services beyond osteopathic treatment, potentially for the same presenting complaint. The results suggest that the patients are providing an isolated response to the Patient Perception Measure–Osteopathy in the Cranial Field based on their experience with the osteopathic treatment.
Musculoskeletal pain and other major illnesses are common conditions. 37 In Australia, persons who had a musculoskeletal disorder were 1.5 times as likely to report that they had a mental health disorder than those who did not have a musculoskeletal condition. 38 In the present study, 26.2% of patients reported having an anxiety disorder compared to an overall prevalence rate of 3.8% in the Australian community. Whereas the prevalence for depression was 9.4% compared with a population prevalence of 9.7%. It has previously been identified 39 that 12% of Australians have coexisting mental health disorders and a physical condition, and the most common mental health disorder coexisting with a physical condition is anxiety, affecting 1.4 million Australians. 40 The prevalence of anxiety in the present study is still much higher than would have been anticipated and could be due to factors apart from musculoskeletal pain including chronicity of pain, cause of pain, effectiveness of pain management treatments and regimens, and life circumstances. It is not possible to determine the reason for the higher than anticipated prevalence of anxiety in this population of osteopathy in the cranial field patients, although it is an important consideration for osteopathy in the cranial field practitioners. To date there have been no studies in the osteopathy in the cranial field literature that address the possible causes of higher prevalence of mental health problems in patients attending osteopathy in the cranial field; therefore, the current observations cannot be compared with previous osteopathy in the cranial field clinical samples. However, these observations have been replicated in chronic pain samples 41 –43 and will require further testing on larger osteopathy samples.
Anxiety was not associated with Patient Perception Measure–Osteopathy in the Cranial Field scores, and persons who were anxious did not significantly differ from those who were not anxious on the Patient Perception Measure–Osteopathy in the Cranial Field. However depression was associated with Patient Perception Measure–Osteopathy in the Cranial Field scores, and patients who experienced mild depression had significantly lower scores on the Patient Perception Measure–Osteopathy in the Cranial Field domain Emotion and Mood. This finding would tend to support the validity of Domain 5 as a measure of Emotion and Mood, and being distinct from the other domains of the Patient Perception Measure–Osteopathy in the Cranial Field.
The sensations that patients most often reported experiencing during their osteopathy in the cranial field treatment were positive and included the following: Relaxed (83.3%), Releasing (73.8%), Unwinding (57.1%), Warmth (45.2%), Balancing (40.5%), and Softening (40.5%). All these sensations may be seen to be favorable, in that the outcomes for osteopathy in the cranial field patients who experienced these sensations would generally improve patients’ symptoms and increase their sense of well-being. Patients who reported the sensation of Releasing had statistically significant higher total Patient Perception Measure–Osteopathy in the Cranial Field scores when compared with those that did not. Anecdotally, this sensation is one that is described by osteopathy in the cranial field practitioners, and it would be of interest to determine if the clinician providing the osteopathy in the cranial field treatment had actually used these, or similar, terms to describe the goals and/or effect of the treatment.
Negative sensations were experienced far less by osteopathy in the cranial field patients and included the following: Anxious (4.8%), Emotional (4.8%), Sad (4.8%), Uncomfortable (4.8%), and Restless (4.8%); and on further examination of the data, these sensations were experienced by patients who also had a comorbid psychological disorder such as depression or anxiety. These negative sensations would not be perceived by patients as being consistent with an improvement in symptoms and well-being 44 and also have a negative relationship with emotional well-being and psychological health. Therefore, there may have been a bias in patients not choosing these sensations due to the negative connotations associated with these terms. It cannot be substantiated that osteopathy in the cranial field patients commonly experience these sensations, because no studies describing the sensations experienced by osteopathy in the cranial field patients could be located. However, these sensations may be experienced in other manual therapy patients. Future studies should investigate whether these sensations are experienced with the application of other manual therapy techniques or whether they are only experienced by patients with comorbid anxiety or depression.
Satisfaction With Life and Meaningful Daily Activity as possible factors affecting patients outcomes of treatment have been previously reported in chronic pain samples 23,45,46 but not in the manual therapy literature. Patients’ reported levels of Satisfaction with Life and Meaningfulness of Daily Activity were positively associated with their perception of osteopathy in the cranial field treatment. Also, depression and anxiety were negatively associated with Satisfaction With Life, and depression was negatively associated with Meaningfulness of Daily Activity. Higher scores on Satisfaction With Life were significantly related to higher scores on all of the Patient Perception Measure–Osteopathy in the Cranial Field subscales and total score, except for Physical Perception of Treatment. These findings would appear to be consistent with positive attitudes, expectations, and beliefs of patients being related to better outcomes and perceptions about therapeutic interventions for various illnesses. 47 –50 These associations cannot be refuted or confirmed in the manual therapy literature and warrant further testing.
Of note was that Physical Perception of Treatment was not significantly associated with either Education and Information or Satisfaction with Treatment. These findings suggest that physical aspects of a osteopathy in the cranial field consultation are independent of education and satisfaction with treatment. However, Physical Perception of Treatment positively influenced the patient’s overall perception of their treatment, including the Therapeutic Relationship, Emotion and Mood, and Cognitive Functioning. Physical Perception of Treatment was also significantly and positively associated with experiencing the sensation of releasing during osteopathy in the cranial field treatment and negatively associated with depression. Persons who were depressed had lower scores on the Physical Perception of Treatment domain. This is not atypical of chronic pain patients who are depressed as they tend to have elevated scores on measures of pain and interference than those who are not depressed. 41,51,52
Further investigation is required to explore the positive associations of Satisfaction With Life with perceived outcomes of osteopathy in the cranial field treatment and the negative associations of depression on manual therapy outcomes. 14,53 Currently, there is no published manual therapy evidence to refute or support these associations. However, on the basis of current observations, it would appear that manual therapy practitioners should consider the routine screening of patients for depressive disorders and access patients’ satisfaction with life.
For the present study, the primary limitation was the small sample size. The main reason was the small number of osteopaths who regularly use osteopathy in the cranial field as a technique. 1 Another reason for small sample size was that our study excluded patients under the age of 18 years. Many osteopathy in the cranial field practitioners treat children and these patients were excluded from our study. Furthermore, as the study was implemented in 2 countries, communication due to the time differences between Australia and New Zealand was a significant limitation. The issue of bias in osteopathy in the cranial field practitioners inviting patients who are favorably disposed toward osteopathy in the cranial field treatment and most likely to positively respond to the Patient Perception Measure–Osteopathy in the Cranial Field is possible. The desire to favorably respond to items on the Hospital Anxiety and Depression Scale and Patient Perception Measure–Osteopathy in the Cranial Field is possible in a clinical sample, 54,55 and patients may have also responded favorably to items on the Patient Perception Measure–Osteopathy in the Cranial Field to please their treating practitioner. However, the conditions most often treated in the current study are consistent with other manual therapy samples and may be representative of manual therapy patients.
Despite the sampling limitations of the study, overall the Patient Perception Measure–Osteopathy in the Cranial Field was reliable and appears to tap patient experiences of osteopathy in the cranial field that to date have not been reported in the manual therapy literature. The associations between sensations experienced, gender, positive and negative affect (depression, Satisfaction With Life, and Meaningfulness of Daily Activity), and patient perception of osteopathy in the cranial field has also been identified in this study and has implications for clinical practice.
Conclusion
In a clinical osteopathy in the cranial field sample, sensations that patients have reported they experienced during osteopathy in the cranial field treatment affected the patients’ perceived outcome of their treatment. This is particularly the case for those patients who reported they experienced a Releasing sensation during treatment. In that, Patient Perception Measure–Osteopathy in the Cranial Field Education and Information, Physical Perception of Treatment, Emotion and Mood, and the total Patient Perception Measure–Osteopathy in the Cranial Field score were all significantly higher for patients who reported they experienced a Releasing sensation during treatment. Patients who experienced a Balancing sensation during treatment had higher scores on the Patient Perception Measure–Osteopathy in the Cranial Field domain Satisfaction with Treatment. Female patients also reported higher levels of satisfaction with osteopathy in the cranial field treatment than male patients, but given the small sample in the current study and inconsistency with the patient satisfaction literature, this finding warrants further investigation.
An important outcome of this study is that the Patient Perception Measure–Osteopathy in the Cranial Field is potentially a useful outcome measures for therapists to assess patients’ perceptions of their respective osteopathy in the cranial field treatments. The information obtained from the Patient Perception Measure–Osteopathy in the Cranial Field may be used to refine the clinician’s skills and attributes and provide evidence for practice, in that patients’ perception of their treatment outcomes may be assessed and monitored with the Patient Perception Measure–Osteopathy in the Cranial Field.
The observed association between depression, Satisfaction With Life, Meaningfulness of Daily Activity, and patients perception of their osteopathy in the cranial field treatment was an important finding and has clinical relevance for managing patients, particularly those patients who are depressed, not satisfied with life, or do not perform meaningful daily activities. These findings warrants further exploration in manual therapy regardless of the therapeutic techniques employed.
Footnotes
Acknowledgments
Thanks are extended to the osteopaths who agreed to participate in the study. Thanks are also extended to Pilar Munoz for her assistance in recruiting and distributing the survey to osteopaths in New Zealand. Also, thanks are extended to Denise Cornall for her assistance in developing items for the Patient Perception Measure–Osteopathy in the Cranial Field and providing contacts for osteopaths who practice osteopathy in the cranial field in Australia and New Zealand. The authors would also like to acknowledge the assistance of Jane Boadle who assisted with data entry.
Author Contributions
Both authors were involved in the literature review. JM conducted the data analysis. Both authors contributed to the development of the article and approved the final version.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
The study was approved by the Victoria University Human Research Ethics Committee (HRETH 11-226).
