Abstract
Animal-assisted activity is the use of trained animals for the therapeutic, motivational, or educational benefit of patients. Subjects of this study were 218 patients hospitalized on the mental health unit of a community hospital with an existing, complementary animal-assisted activity program. Half of the patients participated in a 1-hour session of animal-assisted activity. The other half, who served as a comparison group, participated in a 1-hour stress management program. It was hypothesized that an animal-assisted activity program would improve ratings of depression, anxiety, and pain and the associated physiological measures of stress and discomfort. Self-report ratings of depression, anxiety, and pain were collected before and after treatment sessions, and blood pressure, pulse, and salivary cortisol were measured. There were significant decreases in depression (P < .0001), anxiety (P < .0001), pain (P < .0001), and pulse (P < .04) after animal-assisted activity program, comparable to those in the more traditional stress management group.
Introduction
It is thought that prehistoric man forged a bond with the tamest wild wolves, leading to the evolution of Canis lupus familiaris, the domesticated dog. 1 Domesticated animals have been integrated into the treatment of illness for over a hundred years. 2 Due to the rising demand for complementary and alternative medicine services, many hospitals, psychiatric facilities, nursing homes, and rehabilitation centers are including trained animals, especially dogs, for socialization as well as therapeutic activities. 3 Such dogs complete both obedience and specific therapy training under the auspices of organizations such as Pet Partners, formerly the Delta Society, which set standards and maintains registries. Training topics include understanding the needs of specific client groups, client confidentiality, and interpersonal skills. 4 One survey found such activities to be the most common complementary and alternative medicine approach offered to hospitalized patients. 5
Although the terms are often used interchangeably, animal-assisted activity refers to any use of trained animals for the therapeutic, motivational, or educational benefit of patients, 6 while animal-assisted therapy is technically defined as the use of trained animals by trained health professionals to facilitate specific, measureable goals for individual patients for whom there is documentation of progress. 7 This differs from the task-oriented training of service animals (eg, Seeing Eye dogs that are trained to scan for oncoming traffic before the owner crosses a street). For example, an animal-assisted therapy dog may be used as an adjunct to physical therapy for a patient working on increasing range of motion by having the patient throw a ball, which the dog retrieves. Goals in mental health settings are often not so concrete. At times, the dogs’ benefit in such settings may be that of a more general “social lubricant” enabling the patient to feel more at ease and consequently, better able to develop a therapeutic rapport with the therapist. 8 Holcomb and Meacham 9 found that more patients attended group therapy on an inpatient psychiatric unit when therapy dogs were present. Such interventions have also been shown to facilitate more specific mental health goals such as getting resistant patients to engage in counseling, trusting others, and expressing emotion. 10 A psychotherapist’s dog may provide a shared interest, creating a bond that encourages conversation with a patient, or a patient may learn to identify and talk about emotions by being asked to describe what the dog may be feeling. 11
Animal-assisted activity (and therapy) programs have been associated with positive effects in many studies although poor designs and small sample sizes have limited conclusions. 12 A comprehensive literature search conducted by Nimer and Lundahl 13 reviewed 250 studies, of which only 49 met their criteria for inclusion in a meta-analysis. Only 23 of the 49 used a control group, and the mean number of subjects receiving the animal-assisted activity in those studies was only 18. They reported finding treatment effects in studies in which the dependent variables were improvements in the symptoms of autism-spectrum disorders (high effects), medical and behavior disorders (moderate effects), and problems with emotional well-being (low effects). Souter and Miller 14 also performed a meta-analysis of studies that used animal-assisted activities with depressed patients and found a statistically significant mean effect size in the 5 best studies. In one small, but randomized and controlled study, Villata-Gil et al 15 showed improvement in the social interactions of hospitalized schizophrenic patients after 25 group sessions with a therapy dog, which were comparable to those seen in participants in a group session without a dog.
Psychological variables can be challenging to operationalize. When psychological variables are assessed in animal-assisted activity studies, it is often done by self-report, without measuring physiological correlates of those variables. Studies that have addressed physiological variables have often used nonpsychiatric patients. Cole et al 16 showed that hospitalized heart failure patients who received a 12-minute visit from an animal-assisted activity dog and its handler had lower cardiopulmonary pressure and neurohormone levels and lower anxiety scores than did patients who were either left alone or had a human visitor. Measurement of physiological variables is important in order to corroborate self-report and to assess the impact of emotional distress on physical health. This may be especially important given that animal-assisted activity, like many complementary and alternative medicine therapies, may be less likely to be seen to have quantifiable benefits.
It can also be argued that the important endpoints in animal-assisted activity research need to be relevant to the population being studied, 12 which in mental health settings involves assessment of things like mood and anxiety. Barker and Dawson, 17 for example, found statistically significant reductions in anxiety using the (self-report) State-Trait Anxiety Inventory with hospitalized psychiatric patients who participated in either animal-assisted activity or another recreational therapy program, but no differences in effectiveness between the 2 types of sessions. Physiological variables were not measured, but they were in a later study by one of the same authors 18 using 20 health care professionals as participants. Salivary and serum cortisol dropped after a 20-minute interaction with a therapy dog, but not any more than they did for participants in a group that simply rested. This illustrates the often-contradictory findings in animal-assisted activity research when both physical and psychological variables are measured. As pointed out by Palley et al, 12 if animal-assisted activity is to become part of standard medical therapy, more convincing studies are needed that demonstrate its efficacy and explain the underlying mechanisms of the human response.
The purpose of this study was to assess the effects of an existing animal-assisted activity program on psychological as well as physiological variables in an inpatient mental health population, using measures of depression and anxiety as well as measures of blood pressure, pulse, salivary cortisol, and pain. This study also compared these effects to those of a stress management program that was part of the treatment programming at the same site.
Methods
The protocol for the study was submitted to the hospital’s institutional review board to ensure the ethical treatment of participants, and approval was granted. This board does not review animal welfare issues. The dogs were, however, the personal pets of the handlers and the sessions were only 1-hour long, reducing the likelihood of the dogs being maltreated.
This study was carried out on the mental health inpatient unit of a community hospital over a 1-activity-year period (July 2008-August 2009). The animal-assisted activity program had been in existence for several years prior to the study. Hospital regulations did not allow the dogs to enter patient rooms, so sessions were held in a group format in a common area. This limited the amount of individual goal setting described in the formal definition of animal-assisted therapy. The treatments consisted of group sessions of animal-assisted activity and of the stress management program. Both occurred once a week, on different days, but in the same room at the same time of day. This study assessed the immediate impact of a single, hour-long session.
For the animal-assisted activity condition, participants met in a large room with the dog and its owners. For the majority (80%) of the sessions, the therapy dog was Jesse, a female Border Collie. Jesse’s owners were experienced volunteers at the hospital, who used specific animal-assisted therapy strategies in the sessions. 19 To improve social interaction skills, the owners encouraged participants to ask questions about the dog and to speak about their own experiences with pets and animals. The dog’s feelings and responses to human emotions were discussed to encourage emotional expression. Patients were asked to try commands such as “sit” and “fetch” with the dog in order to enhance their self-efficacy. The comparison group watched a video-based stress management program using a DVD presentation called The Joy of Stress, 20 which was designed to teach coping through cognitive restructuring and humor. A trained facilitator managed that program, although no effort was made to encourage discussion. This design controlled for treatment consistency across participants.
All patients hospitalized on the mental health unit during the study period were encouraged to attend both types of sessions as part of their treatment. Participation in the study, however, was voluntary. Patients could participate in as many sessions of both treatments as they wished, but each patient could only participate in the study (ie, have their psychological and physiological measurements done before and after the session) once, and in only one treatment condition or the other. For example, if a patient came to a session of animal-assisted activity on Day 1 of his hospitalization and agreed to be part of the study, he could attend as many future animal-assisted activity or stress management sessions as he wished, but would not be measured again. For this reason, some participants may have had additional sessions of one or both treatments. Every effort was made, however, to recruit participants as early as possible in their hospitalization. Given that the mean length of stay on the unit was only 7.13 days, it is unlikely that many patients would have had the opportunity to attend repeatedly.
A total of 218 participants were studied. Over that 1 year, patients volunteered to participate in 43 animal-assisted therapy sessions (mean = 2.49 participants) and 41 stress management sessions (mean = 2.71). There were slightly more women (61.7%) in the animal-assisted activity group and more men (52.2%) in the stress management group (χ2 P = .039). The mean age of participants was 39.3 years. Further demographic or diagnostic data were not collected to maintain greater privacy for these patients (for whom these groups were part of their treatment) and to increase acceptability of the study to staff and patients. As the setting was an acute care unit, most patients were in crisis and carried diagnoses associated with significant mental illness (major depressive disorder, bipolar disorder, schizophrenia).
After a complete description of the study was given to participants, written and informed consent was obtained. Before and after each session, participants filled out a questionnaire that assessed depression, anxiety and pain. The Burns Depression Checklist (Brief Version, Revised) and the Burns Anxiety Inventory (Brief Version, Revised) developed by David Burns 21 were used to assess depression and anxiety. The Burns Scales are measures that each consist of 5 symptoms and use a Likert-type format. Participants rate each on a of 0 to 3 scale, with 3 indicating “It bothers me a lot” and 0 indicating, “I am not bothered at all.” Total scores for each scale can range from 0 to 15, with lower scores indicating less distress. Some symptoms on the depression scale are “sadness” and “loss of interest in life.” The anxiety scale includes items such as “feeling stressed, uptight or on edge” and “frightening thoughts, feelings, and daydreams.” According to Brittain, 22 Burns’ anxiety scale has been shown to have good internal consistency and concurrent validity (r = .85, P < .01), with the more widely used Beck Anxiety Inventory.
Pain was measured using the 0 to 10 Pain Scale, 23 also a Likert-type format in which 0 represents “no pain” and 10 represents the “worst pain possible.” This scale has been shown in numerous studies to be valid, reliable, and easy to use. 24 –26 The participants had their blood pressure and pulse measured before and after the sessions by trained staff who also collected saliva samples for cortisol analysis. Cortisol is a corticosteroid hormone produced by the adrenal cortex that becomes elevated as part of the human stress response. Saliva samples were frozen and later analyzed by Salimetrics, LLC, in State College, Pennsylvania.
With the help of a trained statistician, basic descriptive statistics were calculated for each factor with means and standard deviations for continuous variables and proportions for categorical variables. Bivariate tests using t tests and χ2 were done where appropriate to assess unadjusted associations.
To assess the effect of the intervention, a general linear model with a random intercept (to account for repeated measures of subjects) was employed. An interaction term was included in the model to determine if there was any difference in the intervention from the premeasure to the postmeasure. These measures were also analyzed with adjustments made for age and gender. For any statistical tests, a probability level not to exceed P < .05 was considered statistically significant.
Results
The baseline measures are summarized in Table 1 showing that prior to treatment, there were no significant differences between the 2 groups on any of the dependent variables.
Baseline Measures.

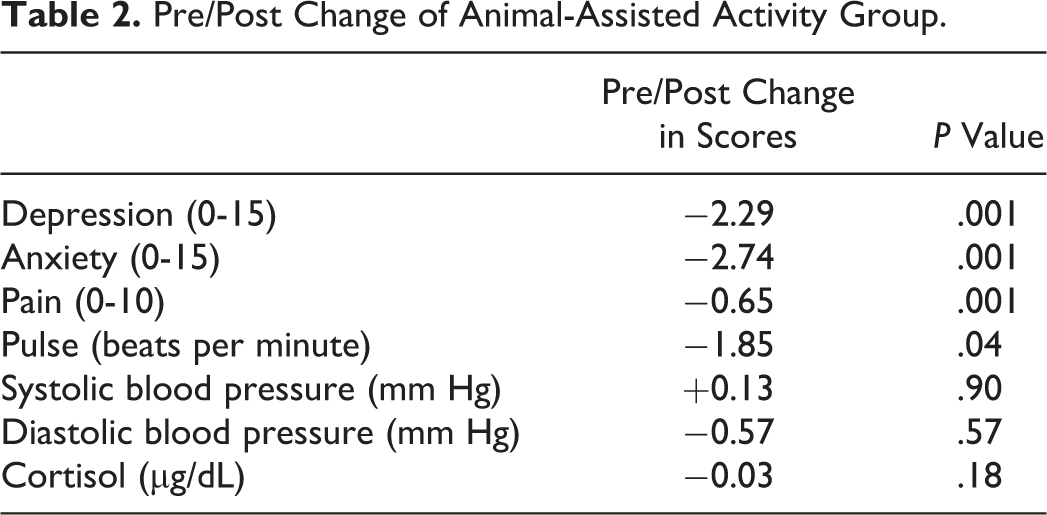
After participating in animal-assisted activity, patients showed significant improvement on some psychological as well as physiological measures. Postmeasures for this group showed decreases in depression (P < .001), anxiety (P < .001), pain (P < .001), and pulse (P < .04). Hypothesized changes in systolic blood pressure, diastolic blood pressure, and cortisol were not observed (Table 2).
Pre/Post Change of Animal-Assisted Activity Group.
Participants in the stress management program showed similar reductions in depression, anxiety, pain, and pulse, although neither program was significantly better than the other. When analyzed by gender, women in both groups, as compared to men, had lower blood pressure at both pretest (systolic, P < .001; diastolic, P < .002) and posttest (systolic, P < .002; diastolic, P < .014), which created a significant interactive effect.
It was observed that the animal-assisted activity sessions were the most well attended of all therapeutic activities offered on the unit. There were also instances in which the session served as a clinical bridge, with patients revealing significant issues or, in one case, speaking for the first time in days, while interacting with the dog and her owners.
Discussion
The results of the study support the hypothesis that animal-assisted activity can improve ratings of depression, anxiety, pulse, and pain, doing so as well as a more traditional stress management program. These findings are consistent with the equivalent reductions in anxiety found by Barker and Dawson 17 in both animal-assisted activity and a comparison group, although the current study expanded on that work with the inclusion of physiological variables and assessment of depression.
There were possible confounding variables and alternate explanations for the findings. The small (P < .004) change in pulse could have been an artifact of sitting in the session, although changes in blood pressure and cortisol were not observed in either group. Many medications, including psychotropic ones, can affect blood pressure response, so the lack of change in blood pressure also found in other hospital studies 16 may be due, at least in part, to such effects. Gender differences in group composition may also have influenced results. As noted, female subjects in both groups had lower blood pressure before and after the sessions, and there were more women in the animal-assisted activity group than the stress management group. The sessions may not have been long enough to reveal a measureable change in salivary cortisol. Considering, however, that all of the participants were psychiatric patients, depression and anxiety, where significant changes were seen, may actually be the more meaningful endpoints.
This study cannot be regarded as a traditional experiment in which participants are randomly assigned to treatment conditions, because the patients were free to elect which mode of therapy they would receive. Several factors made random assignment impractical. This was a clinical outcomes study of an existing program that was already an important component of treatment. Excluding some patients from it was not acceptable to the staff. Also, there were patients who disliked or feared dogs, and such patients could not ethically be assigned to animal-assisted therapy.
A large sample size was used to try to adequately power the study and maximize the chances of detecting real differences. Efforts were made to have the treatment be as consistent as possible over the year of data collection. The programs occurred at the same time of day and in the same room and were standardized by having the animal-assisted activity sessions done by the same dog/handler team 80% of the time, and by presenting the stress management program in a DVD format, with a trained facilitator. Both programs, however, were administered by humans (although the facilitator’s role in the comparison group was minimal), and it is possible that those persons (rather than the dog) were the therapeutic factor. It would not be possible for the dog to interact with patients without its handler, for the safety and welfare of the dog as well as the patients. To control for the human factor in their study done on a cardiac unit, Cole et al 16 included a human visitor without a dog (which was not as effective as the animal-assisted activity condition), but that was not clinically feasible in this setting. Additional factors include the likelihood that the dog (and her owners) may not have been equally energetic or engaged every day, and that the participants (who provided much of the discussion in the animal-assisted activity sessions) were obviously different from session to session. The experience was, therefore, not identical for different participants over the course of the study. Such issues can be hard to avoid in clinical settings such like this. An ongoing challenge to researchers working in animal-assisted therapy and other types of complementary and alternative medicine is the appropriateness and feasibility of conventional research methods, especially in health care settings. 27
Further research with a nontreatment control group could clarify whether observed changes in both groups were truly treatment effects versus placebo effects. Results cannot necessarily be generalized to nonpsychiatric patients or to those significantly different in age or culture than those in this sample. This program would not be expected to be effective for patients who disliked or feared dogs, but those patients were unlikely to have agreed to participate.
The program was safe and extremely cost-effective because animal-assisted activity teams are all volunteers. It was efficient in that it was delivered in a group format. For patients who like animals, this may be a more acceptable alternative to the typical therapeutic programs on an inpatient mental health unit. It is also a way to satisfy health consumers’ increasing interest in complementary and integrative approaches to care.
Further research is needed to evaluate how long the positive effects of animal-assisted activity last, the amount needed to produce a durable effect, and ways to extend the benefits beyond the hospital and to other types of patients. There are also unanswered questions about the conditions under which it has the most benefit.
Conclusions
Animal-assisted activity can improve ratings of depression, anxiety, pulse, and pain, doing so as well as a more traditional stress management program.
Footnotes
Authors’ Note
Results were presented at the 2010 annual meeting of the Pennsylvania Psychological Association. A previous version of this article was published in the Journal of Lancaster General Hospital and is used with permission.
Acknowledgments
The project was carried out at Lancaster General Hospital, Lancaster, Pennsylvania, and would not have been possible without the assistance of the staff and patients and the volunteer team of Dorothy and Aaron Rowe and their dog, Jesse. Michael Horst, PhD, provided invaluable help with data analysis, interpretation of results, and creation of charts and graphs. Elizabeth Lynn provided assistance with data collection.
Author Contributions
PN, CNS, and SRB are first authors who contributed equally to this work.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project was funded by a grant from the Lancaster General Health Foundation.
Ethical Approval
This project was reviewed and approved by the Institutional Review Board of Lancaster General Hospital.
