Abstract
Background:
Family physician advice and follow-up may be important to reduce the negative aspects of locally marketed herbal remedies and improve the patient outcome. There is a lack of studies assessing the preference of Saudi patients for the integration of herbal medicine into primary care services.
Objectives:
To examine the knowledge, attitudes, and practice of Saudi patients toward herbal medicine and its integration into primary care services.
Methods:
A cross-sectional study was conducted between February and March 2013 among adult patients attending the family medicine clinics at a primary care center in Riyadh, Saudi Arabia. A self-administered questionnaire (27 items) was developed and administered to all patients.
Results:
A total of 240 patients were included in the current analysis. The average age was 33.5 ± 9.9 years, and 61% of the patients were women. Approximately 60% of the patients were aware of herbal medicine use and its possible side effects. More than 85% of the patients believed that herbal containers should be labeled with safety information. Approximately 71% of the patients had a favorable attitude toward integrated services. Approximately 65% of the patients used herbal remedies for themselves, and 42% used them for their children. Preference for integrated services was significantly associated with female sex, better knowledge, positive attitudes toward safety and regulations, and higher level of practice.
Conclusions:
A good knowledge and a very favorable attitude toward integrating herbal medicine into primary care services were found among a group of patients attending a primary care center in Saudi Arabia.
The term complementary and alternative medicine (CAM) is used interchangeably with traditional medicine. 1 It includes herbal medicine, several mind and body practices, and other complementary health approaches. 1 The growing popularity of CAM resulted in an ongoing debate on integrating such therapies into the mainstream health care. 2 The World Health Organization encourages integration of CAM into national health care systems to ensure its rational use. 3 Integrative medicine has a client-centered approach to therapy and a holistic focus on health care instead of a disease-centered approach of conventional medicine. 4 Integration of CAM in primary care services was reported in a number of studies from the United States, Germany, Israel, Australia, Italy, and Iran. 5 –10 However, there are several challenges for the integration of CAM services within the conventional health care services. 11 These include, among others, physician concern, utilization issues, and system adjustment.
The prevalence of herbal use in Saudi populations was high but variable in different studies. 12 –17 The commonest herbal remedies used were myrrh (oleoresin oil containing natural gum), black seed (of Nigella sativa), helteet (ferula assa-foetida), fenugreek (Trigonella foenum-graecum) and aloes (plant family Xanthorrhoeaceae and subfamily Asphodeloideae). 12,13 However, a considerable proportion of locally marketed herbal remedies are unsafe and sometimes toxic. 18 Family physician advice and follow-up may be important to reduce the negative aspects of herbal use and improve the patient outcome. 19 Attitudes toward integrative medicine were examined among patients 20 and physicians 6,21 in different parts of the world, with generally favorable attitudes. There is a lack of studies assessing the preference of Saudi patients for the integration of herbal medicine or other types of CAM into primary care services. The objective of the current study was to examine the knowledge, attitudes, and practice of Saudi patients toward herbal medicine as well as to assess their preference for integration of herbal medicine practices into primary care services.
Methods
Population
The current study was conducted among patients attending a family medicine clinic at Al-Wazarat Health Care Center, the largest primary care center that belongs to Military Hospital, located in Riyadh, Saudi Arabia. The center has 32 general clinics and 6 chronic disease clinics, with about a thousand visits per day. The center was accredited by the Joint Commission International in 2010. The current study targeted adult Saudi patients of both sexes, above the age of 18 years. As it was self-administered questionnaire, illiterate patients were excluded.
Study Design
A cross-sectional study was carried between February and March 2013. The study obtained all required ethical approvals from the institutional review board at Military Hospital, Riyadh, Saudi Arabia.
Sample Size
It was estimated that 208 patients are required to detect a 20% difference (eg, 50% vs 30%) in a knowledge or practice characteristic with 80% power and 95% confidence.
Questionnaire
A self-administrated questionnaire was developed and administered to all patients. It included 2 sections: sociodemographic information and 27 questions assessing the patient’s knowledge, attitudes, and practice of herbal medicine and its integration into the primary care services. Sociodemographic data included age, sex, marital status, number of children, educational level, and monthly income. The knowledge part included 7 questions about herbal medicine use, side effects, interactions, local and international governing regulations, and awareness of a Western model of integration. The attitude part included 14 questions divided into 2 groups: 9 questions about the regulations and the safety of herbal medicine and 5 questions about the preference for integrated services. The practice part included 6 questions about one’s experience using herbal medicine and its integration. The content of the study questionnaire was validated by experts in family and community medicine and translated into Arabic by a professional translator. The questionnaire was then piloted on a small number of patients (n = 10) before widespread distribution. The wording of some questions was modified per the feedback from the pilot sample. The questionnaire had a high reliability, with an overall Cronbach alpha of 0.81.
Recruitment
The questionnaire was distributed to patients attending the family medicine clinic at time of the study (ie, convenience sampling). The questionnaire was distributed just before or after the clinic visit. Informed consent was obtained from all patients after explanation of the study objectives. The participation rate was 98% of all contacted patients (n = 240 of 244).
Statistical Analysis
Data were presented through frequencies and percentages for categorical data and mean ± SD for continuous data. Scores were calculated from the knowledge, attitudes, and practice questions. A point was given for the yes answer and a zero for the no and not sure answers. Patients who answered yes to all 5 preference questions (questions 17-21; see Table 1) were considered demanding the integration. Significant differences in sociodemographic characteristics and scores between the study groups (those who preferred and did not prefer integration of herbal medicine into the primary care services) were tested through the chi-square test or Fisher exact test (as appropriate) for categorical data and Student t test or Mann-Whitney test (as appropriate) for continuous data. To detect predictors of the preference for the integration, we ran univariate (individual potential predictors) and multivariate (all potential predictors together) regression models. All P values were 2-tailed. P < .05 was considered significant. SPSS 20.0 (SPSS Inc, Chicago, IL) was used for all statistical analyses.
Patients’ Knowledge, Attitudes, and Practice Toward Herbal Medicine Practice and Its Integration Within the Primary Care Setting.
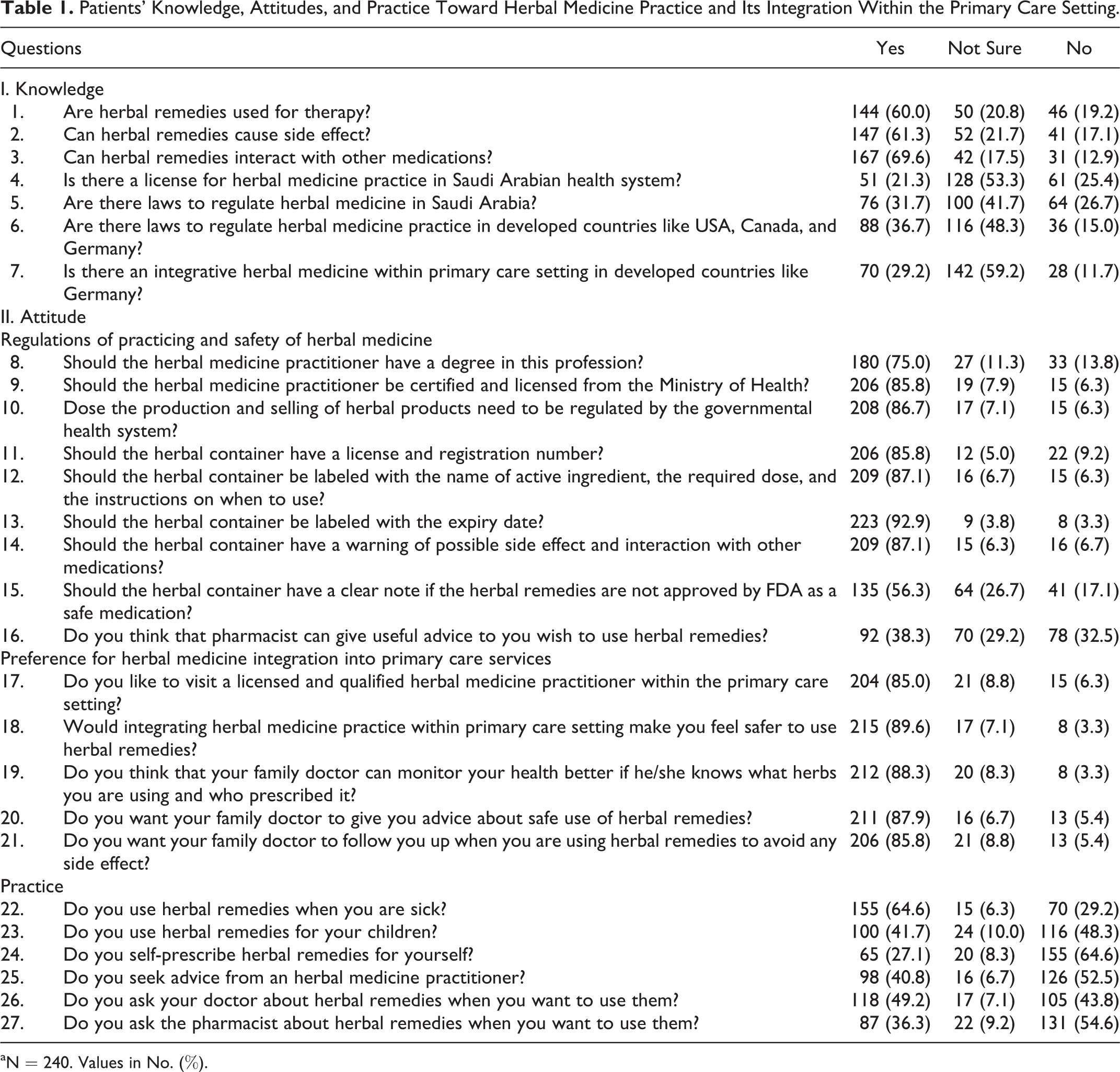
aN = 240. Values in No. (%).
Results
A total 240 patients completed the study questionnaire. The sociodemographic characteristics of the study patients are described in Table 2. The average age was 33.5 ± 9.9 years, and 61% of the patients were women. Three-quarters (75%) of the patients were married. Married patients had 3.5 ± 2.6 children. All patients but 1 were living in an urban community. The majority (61%) had lower than a university education; 32% had a university degree and 7% a postgraduate education. Almost three-quarters (74%) of the patients had a family monthly income of 10 000 SR or less.
Demographic Characteristics and Scores Among Study Patients by Preference for Integrating Herbal Medicine Practice Within Primary Care Services.a

aValues in mean ± SD or No. (%).
Table 1 shows their knowledge, attitudes, and practice of herbal medicine. Approximately 60% to 70% of the patients were aware of herbal medicine use, possible side effects, and possible interactions with other medications. However, a much smaller proportions (21%-32%) were aware of the presence of an official license or governing regulations in Saudi Arabia. Similarly, only 37% of the patients were aware of the presence of such regulations, and 29% were aware of herbal medicine integration within primary care services in Western countries. Approximately 44% of the patients positively answered the knowledge questions (Figure 1).
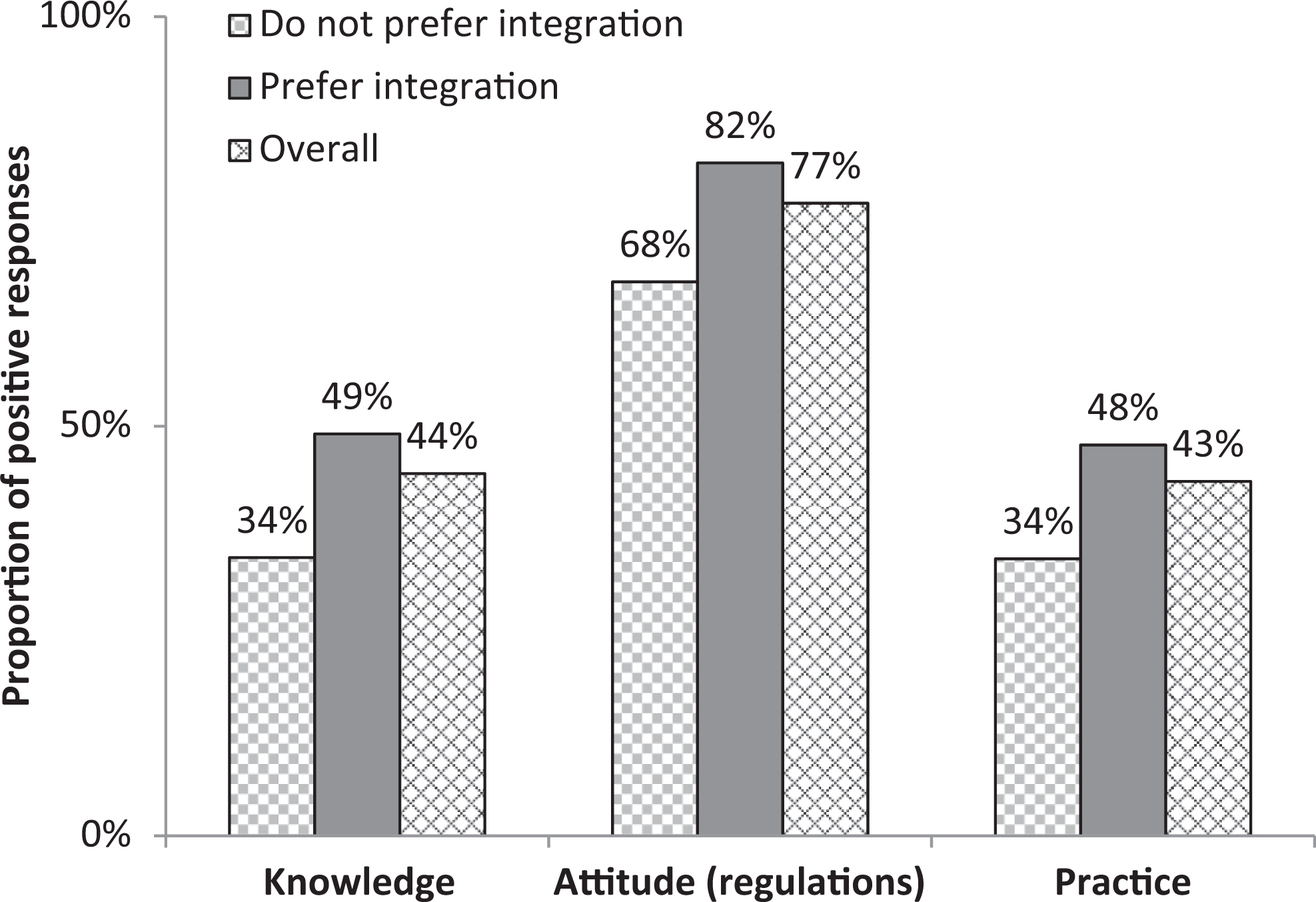
Mean proportions of positive knowledge, attitudes, and practice responses by preference for integrated herbal medicine practice within primary care services (N = 240).
The majority (75%-87%) of the patients believed that an herbal medicine practitioner should have a degree and official license as well as local governing regulations (Table 1). More than 85% of the patients believed that herbal containers should be labeled with safety information, such as active ingredient, indications, dose, side effects, interactions, and expiry date. A relatively small proportion (38%) of patients believed that pharmacists can give useful advice about herbal remedies. The majority of the patients held a positive attitude toward the integration of herbal medicine into primary care services. Between 85% and 90% answered yes to 1 or more of the 5 preference questions, and 71% answered yes to all the questions. For example, approximately 85% of the patients expressed their wish to visit a qualified herbal medicine practitioner within the primary care setting, and 90% of the patients believed that integrating herbal medicine within primary care services would make them feel safer to use herbal remedies. Approximately 77% of the patients positively answered the attitude questions (Figure 1).
Approximately 65% of the patients used herbal remedies for themselves, and 42% used them for their children (Table 1). Approximately 41% of the patients sought advice from an herbal medicine practitioner, and 27% self-prescribed herbal remedies for themselves. Almost half the patients discussed the use of herbal remedies with their doctors, and 36% did the same with their pharmacists. Approximately 43% of the patients positively answered the practice questions (Figure 1).
Sex was significantly associated with the preference for integrating herbal medicine within primary care services (Table 2). Such preference was 78% among women and 60% among men (P = .003). Similarly, those with lower income showed slightly higher preference than those with higher income (73% vs 64%); however, the difference did not reach statistical significance. Those who preferred the integration had significantly higher knowledge, attitude (excluding the preference part), and practice scores compared with those who did not prefer such integration. Adding sex, income, and the 3 scores to a multivariate regression model showed that knowledge, attitude, and practice scores were the only independent positive predictors of the patients’ preference for the integration (Table 3). Yet, the sex effect that was shown in univariate analysis was lost in multivariate regression model.
Predictors of Preference for Integrating Herbal Medicine Practice Within Primary Care Services Among Study Patients (n = 237).

Abbreviations: CI, confidence interval; OR, odds ratio.
Discussion
We assessed the knowledge, attitudes, and practice of a group of Saudi patients attending a primary care center in Riyadh, Saudi Arabia. The study is considered the first local study to assess patients’ demand of integrated medical services. The majority of our patients were knowledgeable about herbal medicine use, possible side effects, and possible interactions with other medications. It is difficult to compare such findings with local data. Previous local studies assessing herbal medicine knowledge among Saudi populations examined health care professionals or traditional healers 22 –24 or the knowledge of herbal medicine combined with many other CAM modalities. 17 In a local household survey, 89% of people living in Riyadh had some knowledge of CAM, and 59% already used herbal remedies. The authors reported that different forms of media as well as family, relatives, and friends represented the main sources of CAM knowledge. 17
Our patients expressed a strong concern about the safety of marketed herbal remedies and a strong positive attitude toward the need of official regulations. However, the majority of our patients were unaware of the presence of an official license or any governing regulations for herbal medicine in Saudi Arabia. These 2 findings may may indicate a failure in the implementation of local regulations. 3 The Ministry of Health in Saudi Arabia is responsible for the licensing of some CAM practices, such as acupuncture and chiropractic services, as well as approving or disapproving all marketed products with health concerns including herbal preparations. 3 Reflecting the minimal governmental control on the safety of marketed remedies on traditional herbal stores, a recent laboratory study showed that about 30% of locally used herbal medications were unsafe for human use due to high heavy metal content, bacterial contamination, or presence of toxic organic substances. 18 Additionally, a case report from Saudi Arabia showed serious complications following treatments given by traditional healers that caused death after ingestion of herbal medicine (ricin poisoning). 25
Our patients had a very favorable attitude toward integrating herbal medicine into primary care services. The observed trust in family physician advice in both conventional and CAM therapies has been similarly reported in other studies. For example, a study in the Netherlands showed that the majority of patients with joint diseases wanted their general practitioners to listen, inquire about used CAM therapies, and, if necessary, refer to or collaborate with CAM practitioners. 20 In another study in Israel, patients suggested that family physicians play a central role in CAM referral; they also expected their family physicians themselves to provide CAM treatments when needed. 26
Almost two-thirds of our population reported the use of herbal remedies. Although it is difficult to compare the finding with local data due to different methodology and population, the current prevalence may be slightly higher than reported before. Previous local studies estimated the prevalence of herbal medicine use among patients with chronic diseases (eg, diabetes, asthma, and liver diseases) between 8% and 32%. 12 –16 Additionally, herbal use was estimated at 59% in a community sample. 17 Since Saudi women were reported to be associated with much higher herbal use when compared with men, 12 the higher female proportion in the current study (61%) may contribute to the observed high herbal use.
Preference for integration of herbal medicine into primary care services in our population was associated with female sex, better knowledge, positive attitude toward safety and regulations, and higher level of practice. Several studies showed that female patients have better knowledge and more favorable attitudes toward the use of CAM modalities and integrated medical services. 17,27 –29 Being more safety-oriented may enhance the preference of having physicians involved in the referral process and posttreatment follow-up of herbal therapies to reduce the possibility of developing side effects. Additionally, almost half our patients reported discussing the use of herbal remedies with their doctors, a probable sign of favoring integration of herbal medicine into primary care services. However, the percentage of those who preferred integrated services was higher than that of those who actually used herbal remedies. This may reflect more trust in herbal medicine when prescribed by physicians rather than by laypeople or herbal practitioners. Although the questionnaire was carefully designed, we cannot exclude the possibility that the phrasing of some of our questions might encourage a positive response.
The current study had several advantages. It is considered the first local study to assess patients’ demand of integrated medical services and its predictors. The study also was done in a primary care setting, where proposed integrations should be initiated. Nevertheless, we acknowledge a number of limitations. Since the patients were recruited from a single center through a convenience sampling, the generalizability of the findings should be limited to urban primary care centers with a similar population. The lack of a universally accepted questionnaire to assess patients’ attitudes about herbal medicine and integrated services may limit future comparability of the current findings. Since illiterate patients were excluded because of their inability to fill the questionnaire, the observed knowledge score in the current study may be overestimated.
In conclusion, a good knowledge and a very favorable attitude toward integrating herbal medicine into primary care services were found among a group of patients attending a primary care center in Saudi Arabia. Further research may be required to assess the knowledge and attitudes of family physicians and herbal medicine practitioners on the possibility of integrated services and the best way to assign responsibilities and the logistics of such integration.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
