Abstract
Traditional Indian medicine—ayurveda—could be the oldest medical system in which leech therapy was adopted for treating specific disease conditions of patients. Some of the indications in which leeches are used are in tumors, hemorrhoids, abscess and boils, skin disorders, ulcers, gout, diseases of the eye, headache, herpes zoster, thrombosis, and wounds. The saliva of the leech consists of anesthetic agents, anticoagulant, antiplatelet aggregation factor, antibiotic, anti-inflammatory substances, and gelatinous substances. Leeches suck the excess blood, reduce the swelling in the tissues, and promote healing by allowing fresh oxygenated blood to reach the area until normal circulation can be restored. Clinical studies have been conducted in different parts of the world to observe the scientific action of leech therapy. Studies with leeches have been carried out to observe the healing of complicated varicose veins, pain reduction in osteoarthritis, and other disorders.
Leech therapy is becoming increasingly popular among practitioners of complementary and alternative medicine. Many studies are currently under way to evaluate its effects, mainly in the treatment of pain. 1 In Europe and the United States, thousands of patients have been healed using leech therapy. 2 Many traditional medical systems, for example, the Greek, Arab, and Russian, mention leech usage. 3 The origins of traditional Indian medicine—–ayurveda—remain unclear, but it is said to date back some 3000 years. Leech therapy has been an active part of traditional Indian medicine throughout its history.
Types of Leeches
In traditional Indian medicine, leeches are classified into poisonous and nonpoisonous types, depending on their toxicity. The application of poisonous leeches can cause swelling and itching in the bitten area, as well as fainting, fever, burning sensations, vomiting, intoxication, and myalgia. 4 The use of nonpoisonous leeches causes no complications during bloodletting (Figure 1). In India, Phylum-Annelida, class-Hirudinea, Hirudo medicinalis are used for bloodletting. These leeches are dark in color and marked with 6 longitudinal stripes. Their bodies are 2 to 3 inches long, convex and wrinkled transversely, 5(p167) tapering at each end. These leeches are classified into 12 types, with each type bearing Sanskrit names 6 –8 (Table 1).

Leech.
Types of Leeches.

Rearing of Leeches
Leeches are best collected during the autumn or rainy season. They should be kept in fresh water, in a big jar, and fed on algae and powdered dried meat of aquatic animals. Placing straw and aquatic plants in these jars helps create an appropriate environment. The water should be changed, and the food residue cleaned, every 3 days. Transferring the leeches to another jar, once a week, also appears beneficial. 9
Indications for Leech Therapy 10 ,11
Benign tumors
Hemorrhoids
Abscesses and boils
Skin disorders—such as dermatitis, psoriasis, vitiligo, alopecia, ulcers
Gout
Diseases of the throat
Diseases of the eye
Cysts
Headaches
Herpes zoster
Thrombosis
Wound management—such as diabetic, pyogenic wounds
Bloodletting is undertaken according to the stage of the dosha—the condition of the patient and his or her blood. Blood vitiated due to Pitta can be effectively removed by leeches. Leeches live in water in cold environments and are seen as “sweet” in nature, according to ayurvedic principles—all properties seen to be opposite of Pitta. 12 In addition, blood vitiated due to tumors and abscesses can be effectively treated with leeches. 13,14 Leeches are also used to treat acute inflammation of glands, including the mammary and parotid glands, as well as bruises, sprains, and inflammation of the serous membranes, skin, and bones. In severe headaches, leeches are placed on the temples to alleviate pain. In menstrual disorders, leeches are applied to the inner thighs. 5(p169) Figures 2 and 3 show the methods of applying leeches to different types of wound.

Leech treatment in a Thrombo Angiitis Obliterans or Buerger's disease patient.
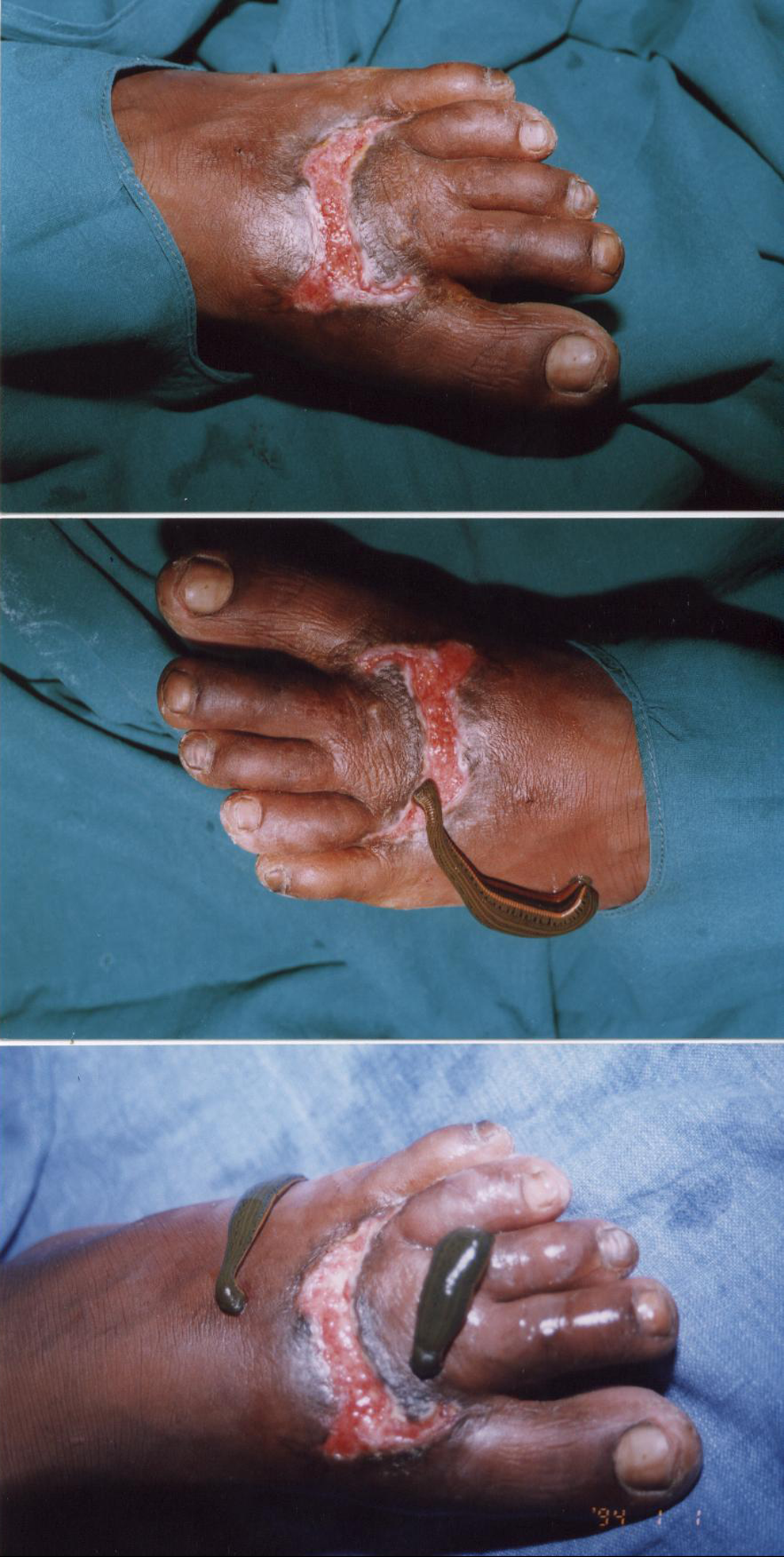
Leeches applied in wounds.
Leeches’ Modes of Action 15
Leeches act by secreting biologically active substances in their saliva. This saliva, which contains a hundred or so different substances, includes an antiplatelet aggregation factor, anesthetic, and anti-inflammatory and antibiotic agents. Leech saliva also contains an anticoagulant, hirudin, which stops blood clotting and dissolves thrombi, clearing partial and complete blockages in distal arteries. When leeches bite, chemicals in their saliva dilate hosts’ blood vessels and thin their blood. Simultaneously secreting a local anesthetic masks any pain from the bite, rendering hosts unaware of leeches’ presence. By ingesting excess blood, leeches reduce tissue swelling and promote healing. These microcirculatory actions enable fresh oxygenated blood to reach hosts’ affected areas prior to the restoration of the normal circulation. Table 2 shows the major constituents of leech saliva. 16
Composition of Leech Saliva.

Method of Leech Application
Leech application is done as follows:
Pre-Application Procedures
Patient examination and preparation: Patients’ general health is first examined, before providing appropriate information about the use of leeches and their actions. Mornings are the preferred time to apply leeches as the leeches will be fresh and not hyperactive. The leeches are applied with patients sitting or supine, in a way that exposes the affected part comfortably. The previous day, oil and/or sweating treatments are given, depending on the patients’ conditions.
Leech disinfection: Before use, leeches are smeared with a paste of mustard and turmeric, which acts as a disinfectant and increases their appetite and blood-sucking ability. The disinfected leeches are kept in a fresh jar of water for half an hour prior to use. 17
Leech Application Procedures
The area to which a leech is to be applied must first be cleaned thoroughly with sterile water. Disinfectant or soap should be avoided, as this can irritate the leech and prevent it from attaching. The leech should be taken from its jar and its mouth placed precisely over the spot where the blood is to be removed. The leech’s tail should be held until it begins to draw blood, at which time it can be gently released. The leech should be lightly covered with moist cotton (cotton material or cotton wool) while it works. This should be kept wet until the end of the process by applying a few drops of water, as needed. If a leech refuses to bite, then a drop of milk or ghee can be applied to the skin in the affected area, to encourage it. A small puncture made through the skin can also help by giving a reluctant leech a drop of blood to initiate sucking. If a given leech still fails to suck, despite these measures, it should be replaced by another. 18,19 A leech can be made to bite in a particular area by placing a piece of paper in which there is a small hole over the desired spot and placing the leech’s mouth over the hole. This will automatically direct the leech to suck blood from the desired location. 5(p169) Leeches normally absorb about 5 mL of blood.
Ayurvedic medicine offers the following advice about the timing of leech removal:
Leeches should suck only impure blood. Symptoms such as pricking pain and itching at the site of the bite occur when leeches start to suck pure blood. If such symptoms appear, the leech should be removed gently by sprinkling powdered rock salt (sainthava) or turmeric around its mouth. 20 These mild substances are disliked by leeches, causing them to stop sucking in a comfortable way. These substances are chosen because they are nonirritant to the host and do not stimulate the leeches. They are also antiseptic and antitoxic.
If pricking pain and itching at the site of the bite do not occur, then the leeches should be allowed to finish on their own.
The maximum amount of blood to be removed from an individual patient depends on the strength of the patient and the nature of the disease.
Postapplication Procedures 21,22
Aftercare of the patient: After the removal of the leech, blood should be allowed to flow from the wound for a few minutes. Satadhauta ghritha, a classical ayurvedic herbal ghee preparation with antiseptic and antibacterial properties, can then be applied to promote healing. The wound is then lightly bandaged for 6 to 12 hours. 23 Turmeric powder can also be applied for its antiseptic, antibacterial, and anti-inflammatory effects. 24
Care of the leech: The same leeches can be used with the same patients more than once, but the leeches must be purified after each application. After having drawn blood, the leeches are sprinkled with rice flour and their mouth parts smeared with oil and rock salt. Massaging the leeches’ body from the tail toward the mouth helps them to regurgitate the ingested blood. Keeping leeches in turmeric water also helps them to vomit the blood without force. This simple method is widely practiced in India today. Once the leeches are emptied of blood, they are kept in dilute saline, turmeric water, and plain water in sequence. If the leeches move actively in the saline, it is a sign that they have regurgitated all the blood ingested. Leeches that stay at the bottom of the jar, without much movement, should be removed and made to regurgitate again. If this process is not followed properly, the leeches can get sick and die.
Purified leeches should be placed in a jar similar to the one previously used. The water in the jar should be changed every third day to remove any toxins. If this is not done, the leeches can become toxic and unsuitable for further use. 25 Once applied, leeches are not fit for use for at least 7 days. 26
Contraindications in Leech Therapy
Leeches should not be applied directly over large, prominent veins or to the eyelids, breasts, or genital organs. Care should be taken in using leeches with children, as bleeding can be severe (intense) or prolonged. Applying leeches at midday or during the evening or night is also inadvisable, as this can lead to complications such as hemorrhage. 5(p169) In addition, leech therapy is contraindicated in patients who are immunocompromised or taking anticoagulants; those who have endoprostheses, anemia, diabetes, or an allergy to leeches; as well as those with bleeding disorders such as hemophilia and arterial insufficiency. It is also inadvisable to apply them during pregnancy.
Research
Leech Therapy for Complicated Varicose Veins 27
A 2-year prospective nonrandomized study evaluated the effectiveness of medicinal leech therapy for venous decongestion, reversing edema, and hyperpigmentation and healing varicose ulcers.
Twenty male patients with varicose vein complications participated. All were treated with leeches applied around their varicose ulcers. The number of leeches used per patient depended on the size of the leeches, the area of the affected part, and the number of affected sites. The leeches were applied every 3 days. Patients were assessed weekly for a range of changes. First, the extent of their edema and hyperpigmentation was scored on a subjective visual analogue scale that ranged from 0 (representing normal) to 3+ (representing severe edema and pigmentation). These results were analyzed statistically using the Wilcoxon sign rank test. Second, limb girth measurements were taken at calf, ankle, and foot levels. Third, patients’ ulcers were assessed for healing, using parameters such as largest diameter, area, and appearance of a healing margin and the extent of any granulation tissue or epithelization. Finally, blood obtained from the leeches’ coelomic cavities within 5 minutes of their attachment was analyzed for its partial pressure of oxygen using an IL 1321 analyzer. Individual patient’s partial pressure of oxygen levels were compared with each of their last 7 arterial and venous blood samples.
Results
Patients’ mean age was 43 years. All had varying degrees of edema and hyperpigmentation, and 19 had venous ulcers. The number of leeches applied at each session ranged from 1 to 4, with 2 to 20 applications being required per patient. Applications were continued until ulcer healing or significant reduction in edema occurred. On completion, all patients’ ulcers showed complete epithelization. Nineteen patients (95%) showed a significant decrease in the extent of the edema in their involved limbs (P < .05). The same number (95%) also experienced a decreased ankle girth of up to 4.5 cm. Fifteen participants (75%) also showed a significant decrease in hyperpigmentation of their limbs (P < .05).
Leech Therapy in Osteoarthritis of the Knee 1
Methods
Fifty-one participants with osteoarthritis of the knee were randomly assigned to either leech or topical diclofenac gel therapy. On study day 0, patients attended the Essen clinic, and 4 to 6 medicinal leeches were applied to the periarticular soft tissue of one of their knees. Preference was given to points found maximally painful on examination and palpation. The leeches were left in place until they detached themselves—a mean duration of 70 minutes. Patients’ knees were then bandaged and patients asked not to be physically active for the next 12 hours. They returned on study day 1 for a change of bandage and a repeated blood count. Control group patients were given 300 g of diclofenac gel and a demonstration of its proper use. During subsequent clinic visits on study days 3, 7, 28, and 91, each of the study outcomes was assessed, except for quality of life, which was assessed only on days 28 and 91. Patients were asked to record their use of any additional “rescue” medication and their application of the study gel, as well as the appearance of any adverse treatment effects.
Leech therapy provided a greater benefit for study patients than topical diclofenac on the primary study outcome measure: a change in knee pain after 1 week. In the leech therapy group, patients’ mean Western Ontario and McMaster Universities Arthritis Index pain scores were reduced from 53.5 ± 13.7 (n = 24) to 19.3 ± 12.2 (n = 24), after 1 week, compared with a reduction from 51.5 ± 16.8 (n = 27) to 42.4 ± 19.7 (n = 26) in the diclofenac group. After inputting multiple missing values, a highly statistically significant estimated between-group difference was found (−23.9 [confidence interval = −32.8 to −15.1]; P < .001, repeated-measures analysis of variance). The estimated group difference for pain relief in favor of leech therapy was most pronounced at day 3 (−29.5 [confidence interval = −36.3 to −22.6]; P < .001). It diminished over time, with a nonsignificant group difference of −9.9 (confidence interval = −20.3 to 0.5; P = .061) found at day 28 and −9.4 (confidence interval = −20.0 to 1.3; P = .084) at day 91. In addition, joint function improved and stiffness decreased more rapidly, and statistically significantly, with leech therapy. The effects were maintained until day 91, resulting in significant group differences favoring the leech therapy group, including the groups’ Western Ontario and McMaster Universities Arthritis Index total scores. The physical dimension of quality of life improved only for the leech therapy group on day 28 (group difference = 0.49 [confidence interval = 0.07 to 0.91]; P = .023). By day 91, these group differences were no longer detectable (difference = 0.13 [confidence interval = 0.31 to 0.56]; P > .2). Patients’ calculated physical activity also increased, but nonsignificantly, in the leech therapy group when compared with the diclofenac group. Neither group experienced any serious adverse effects. A common minor adverse effect of leech therapy was mild to moderate itching at the leech bite sites, which lasted for a mean of 4 days. None of the patients in the leech group rated the pain associated with leeching as severe.
Study of Leeches’ Salivary Gland Secretions 28
This study revealed the relative location, size, and morphology of the proteins and lipids in particles in medicinal leeches’ salivary gland secretions for the first time, using scanning electron and transmission electron microscopy. The picture is further supported by confocal laser scanning microscopy of salivary gland secretion preparations treated with fluorescein isothiocyanate. After incubation with nonionic detergents (Brij 35 and Tween 20), transmission electron microscopy revealed the dissociation of fragments composed of protein-lipid particles, with an increase in free protein concentration using a modified Lowry method. Cholesterol was detected during salivary gland secretions probing using cholesteryl-Bodipy (hydrophobic fluorescent analog of cholesterol) on surface sections during confocal analysis of electron microphotographs of salivary gland secretions.
Side Effects
Local itching proved a common minor side-effect of leech therapy about which patients should be informed. Theoretically, leech therapy carries an infection risk because of the colonization of Hirudo medicinalis with Aeromonas hydrophila bacteria. 29 Infection and septicemia with A hydrophila have been reported where leeches have been used in very ill patients or applied to malperfused tissue in reconstructive or plastic surgery. 30 –32
Conclusion
All medical systems aim to restore those who are ill to health. Leech therapy is a good example of a medical treatment valued in both complementary and conventional medicine. In this article, maximum available literature related to leech therapy in ayurveda is included, ranging from classical texts to modern clinical trials. Traditional medicine, including traditional Indian medicine (ayurveda), has particular strengths and much to offer conventional medicine. It is hoped that many traditional medical treatments will find their way into the integrated medical systems of the future. Where traditional medicine is practiced to high standards, with in-depth understanding of its strengths, the aforementioned studies suggest that it can contribute significantly to integrated medical care, to the benefit of humanity.
Footnotes
Acknowledgments
The article was written at the office of Syal Kumar with the guidance of Prof Gustav J. Dobos and Dr Thomas Rampp.
Author Contributions
SK collected the data, references, tables, pictures, and wrote the article. GJD and TR verified the article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
As this is an article, our institution policy does not require an ethical review.
