Abstract
Background:
A gap in the literature is the associations between longitudinal changes in food insecurity (FI) with parental feeding behaviors (PFB) and child weight status.
Methods:
Secondary analysis of data from the Greenlight trial. Exposure was FI at 2 and 24 months, categorized as: no FI, food insecure to food secure (resolved FI), food secure to food insecure (new FI), or persistent FI. Outcomes included PFB, measured by the Child Feeding Questionnaire, and child weight outcomes. Adjusted linear models were used to estimate predicted means; pairwise comparisons were conducted with the no FI group as the referent group.
Results:
Analysis included 496 parent-child dyads: 45% no FI, 11% new FI, 19% resolved FI, and 25% persistent FI. New and resolved FI had lower mean monitoring scores (p < 0.001 and p = 0.02, respectively). New FI and persistent FI had higher mean pressuring scores (p = 0.03 and p = 0.03, respectively). No difference in restrictive scores was observed. The persistent FI group was more concerned about their child becoming overweight, p = 0.03. Persistent FI had the highest body mass index z-score point estimate (p = 0.07).
Conclusions:
Persistent food insecurity during the first 24 months of life were associated with differences in PFB that may contribute to obesity.
Clinical Trials Registration:
NCT01040897.
Introduction
Food insecurity (FI) can have a detrimental impact on the nutrition and growth of children. FI is defined as a “household-level economic and social condition of limited or uncertain access to adequate nutrition.” 1 FI has been linked to iron deficiency, poor diet quality in children, infant adiposity, and, although findings are mixed, obesity among children and adolescents.2–10 In 2023, 17.9% of households in the United States with children reported FI. 11
Overall, 20.9% of children in the United States have obesity based on NHANES data from 2021 to 2023. 12 Understanding the relationship between FI and obesity is an important area of research. 13 Experiencing FI during childhood can alter a child’s risk for obesity and related chronic diseases through three potential pathways. One pathway is the nutritional pathway in which children who experience FI have poor dietary quality and nutrition.2–5,14,15 Another pathway is through stress,16,17 which can be detrimental to the mental health of parents and lead to parental feeding patterns that influence a child’s risk for obesity.4,18–21 A third potential pathway is that FI may be linked to obesity through parental feeding behaviors (PFB), i.e., the way parents feed their children. PFB can be categorized into distinct domains such as monitoring, where parents carefully watch what their child is eating, restriction, where parents may limit certain types of foods, and pressuring, where parents encourage their child to eat past satiety. 22 PFB that are “non-responsive”, such as pressuring or restricting, are associated with a higher child weight status, whereas monitoring PFB may be associated with a lower child weight status.23,24 Prior cross-sectional work among infants and toddlers demonstrated that FI is associated with non-responsive PFBs and may increase a child’s risk of pediatric obesity.25–27 Cross-sectional work also suggests households that experience FI have a greater concern for their child becoming overweight. 26 A limitation of this prior work was the cross-sectional study design and single measurement of FI. FI can be dynamic for families and the impact of changes over time on pediatric growth, nutrition, and concern for a child’s future weight status are not well understood.4,28
The objective of this study is to examine how the timing of FI over the first 2 years of life is associated with PFB and child weight status in a racially and ethnically diverse cohort. We hypothesized that, compared to households that do not experience FI, a lower monitoring score, and higher restrictive and pressuring PFB scores, would be observed among the groups that experienced FI. Further, we anticipated that PFB scores would vary with the timing of FI. We also hypothesized that compared to children from households that do not experience FI, those who experience FI would have a higher mean body mass index (BMI) at 2 years of age.
Methods
This is a secondary analysis of data from the Greenlight Study. The methods for the Greenlight Study have been previously described. 29 Briefly, the Greenlight Study was a cluster randomized trial conducted at four academic medical centers to prevent childhood obesity using a low health literacy intervention. 29 Inclusion criteria for the study were an infant presenting for a well-child check (WCC) appointment between 6 and 16 weeks of age, a caregiver who speaks English or Spanish, and who had no plans to leave the clinic during the study years. Exclusion criteria were: gestational age < 34 weeks, birth weight < 1500 g, weight < 3rd percentile per the World Health Organization (WHO), 30 or any chronic medical condition that influenced weight. 29 The study received IRB approval at each of the four participating institutions and was registered on the national clinical trials registry (clinicaltrials.gov), study no. NCT01040897.
Exposure
The exposure of interest for this analysis was household food security status as measured by a 2-item validated screen. 31 Participants were asked: “Within the past 12 months we worried whether our food would run our before we got money to buy more” and “Within the past 12 months the food we bought just didn’t last and we didn’t have money to get more.” 31 Respondents with an affirmative response to at least one of the questions were categorized as experiencing FI. Data on household food security status were collected at two timepoints: baseline (when the child was 2 months old) and when the child was 24 months old. Based on food security responses at 2 and 24 months of age, four categories of food security status were created. Participants who did not report experiencing FI at 2 and 24 months were categorized as the no FI group. Participants whose food security changed between the two time points were classified as new FI (no FI at 2-month to FI at 24-months), or resolved FI (FI at 2 months to no FI at 24 months). The persistent FI group were participants who reported FI at both time points.
Outcomes
Parental feeding behaviors
PFB at 24 months were measured using the Child Feeding Questionnaire (CFQ). The CFQ is comprised of 31 questions that load onto 8 domains. 22 The factors in the CFQ include parental feeding behavior domains: (monitoring, pressuring, and restriction) and parent perception domains (concern about child weight, perceived parent responsibility, perceived parent weight, perceived child weight, and concern about child weight). 22 Responses are measured on a 5-point Likert scale ranging from 1 to 5 with 1 indicating never/markedly underweight/unconcerned/disagree, and 5 indicating always/markedly overweight/very concerned/agree/always. The CFQ has been studied in populations with lower socioeconomic status and in racially and ethnically diverse populations.22,32 To test our hypotheses we included the monitoring, restricting, and pressuring domains as outcomes in our analysis. We also included the “concern about child weight” perception domain in our analysis.
Child weight status
Data on child height and weight were collected at routine well-child visits by clinical staff who were trained on proper approaches to collect child weight and length according to the U.S. Department of Health and Human Services guidelines. 29 Child weight outcomes included the WHO BMI percentile z-score, adjusting for age and sex per WHO.30,33 WHO BMI growth curves were used because a number of children presented for their 24-month routine well child visit prior to being 24 months of age and were unable to have BMI plotted on the Centers for Disease Control (CDC) growth chart since CDC BMI standards are available beginning at 24 months. 33 Both BMI percentile and z-scores were examined because BMI percentiles facilitate clinical interpretation, while BMI z-score is advantageous for research and statistical analysis as it is continuous and more effective for extreme values. 34
Covariates
Two separate models were developed for the outcomes of interest. For the model examining the relationship of change in food security between 2 and 24 months to PFB at 24 months, the following covariates were selected a priori: child sex, participation in the Special Supplemental Nutrition Program for Women, Infants, and Children (WIC), caregiver educational attainment, and child health insurance type. A site variable was included in the model to adjust for variations at the clinic level and the effect of randomization at the clinic level. Self-reported caregiver race and ethnicity were also included in the model because parental feeding behaviors may vary by race and ethnicity.15,27 Categories for race and ethnicity included: non-Hispanic Black, non-Hispanic White, Hispanic, and Other, which included multiple races and ethnicities.
A second model examined the relationship of change in food security between 2 and 24 months and child weight status at 24 months. Covariates included in the weight model included birth weight, due to its association with subsequent weight status,35,36 child sex, clinic site, child health insurance status, parental educational attainment, participation in WIC, history of any breastfeeding, and self-reported race and ethnicity. Race and ethnicity were included in the model due to the known differences in infant growth and prevalence of pediatric obesity by race and ethnicity.37,38
Analysis
Participants were included in the current analysis if they completed the CFQ survey and provided data on household food security status at 2 and 24 months. Descriptive statistics using percentages, frequencies, and means were used to describe the analytical sample. Parametric and non-parametric measures of bivariate association were used as appropriate to examine the association between food security status and demographic characteristics and outcomes of interest. For each outcome, we used linear models to estimate the adjusted means and their 95% confidence intervals (CIs). The adjusted predicted means reflected the expected outcome value within each FI change group, with other covariates held constant at their reference levels (for categorical variables) or the population mean (for continuous variables). We tested whether FI change was associated with each outcome of interest after adjusting for covariates, and reported pairwise comparisons with the no FI group as the referent. Full model outputs provided in Supplementary Table S1.
Additionally, we compared the distribution of demographic variables of the analytical sample and the distribution of these variables among participants who were excluded from the analysis due to missing data (Supplementary Table S2). Compared with the full study sample, the analytical sample had fewer White and Hispanic children, more children that were breastfed, and fewer children from the Miami site. As a sensitivity analysis, inverse probability weighting was used to address missing data using the “any breastfeeding” and “site” variables. Specifically, we modeled the probability of inclusion in the analytical sample as a function of the two variables. Race/ethnicity was not included as a covariate in the weighting model due to missingness in these data. We estimated inclusion probabilities using logistic regression, with inclusion in the analytical sample (yes/no) as the outcome and breastfeeding and site as predictors. The inverse of the estimated probabilities was then used as weights for each participant in the analytical sample (Supplementary Table S3). All primary analyses were subsequently repeated using these weights, providing estimates that are adjusted for differential inclusion related to breastfeeding and site.
Results
Of the 865 children enrolled in the Greenlight study, 23 were missing baseline food security status, 346 were lost to follow-up or had missing food security status at 24 months (Supplementary Table S2). Participants were included in the sample if CFQ data and food security data were available at 2- and 24-months. A total of 496 parent-infant dyads were included in the analysis (Table 1). The sample of infants was 51% female and racially and ethnically diverse, with 51% of the sample identified as Hispanic, 29% Black, and 15% White, non-Hispanic. Fifty-eight percent of caregivers reported having less than a high school education. A majority of children were insured by Medicaid and participated in WIC. Almost 60% of the sample reported their child received any breastmilk during the first 2 months of life.
Sample Demographics (N

BMI, body mass index; WHO, World Health Organization; WIC, Special Supplemental Nutrition Program for Women, Infants, and Children.
Food Insecurity
Forty-three percent of participants experienced FI at 2 months, and 37% experienced FI at 24 months. Twenty-six percent of the sample had persistent FI from the time their children were 2–24 months of age. Overall, 30% changed food security status over the first 2 years of life; 19% reported resolved FI at 24 months, whereas 11% reported new FI at 24 months. Forty-five percent of the sample reported no FI throughout the time when their child was 2–24 months of age.
Parental Feeding Behaviors
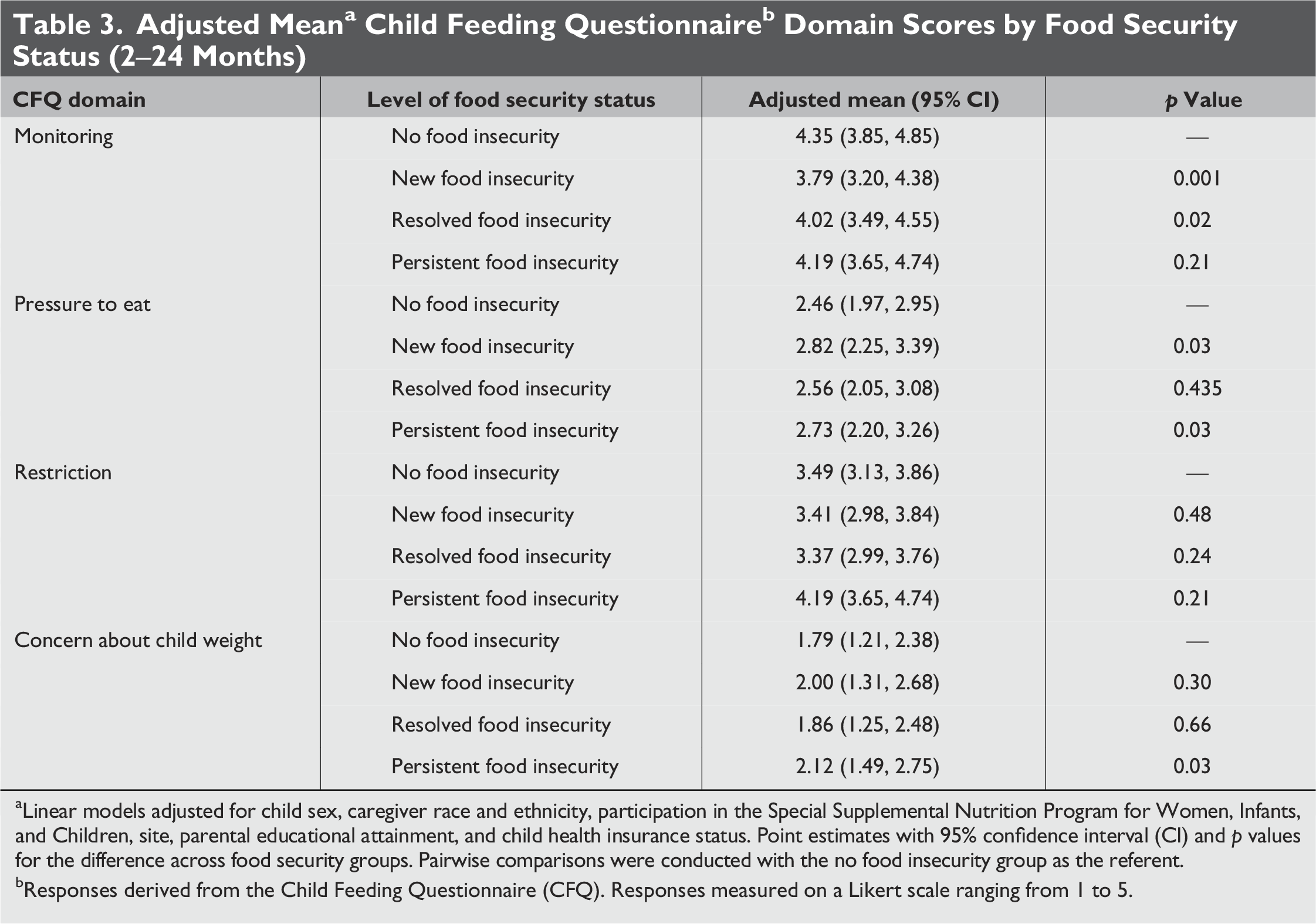
The results of the unadjusted and adjusted mean CFQ PFB domains are shown in Tables 2 and 3. For the monitoring PFB domain, the no FI group had the highest adjusted predicted mean of 4.35. Compared to the no FI group, statistically significant differences in adjusted predicted mean monitoring scores were observed for the new FI group (predicted mean monitoring score 3.79; p = 0.001) and resolved FI (predicted mean monitoring score 4.02; p = 0.02). Statistically significant differences in pressuring PFB domain were seen between the no FI group with an adjusted predicted mean score of 2.46 compared to an adjusted predicted mean score of 2.82 (p = 0.028) for the new FI and 2.73 (p = 0.03) for the persistent FI group. No statistically significant differences were observed in the restrictive domain. The no FI group reported a lower concern about their child becoming overweight compared to the persistent FI group (p = 0.03).
Unadjusted Association Between Food Security Status and Parental Feeding Behavior and Child Weight Status (N
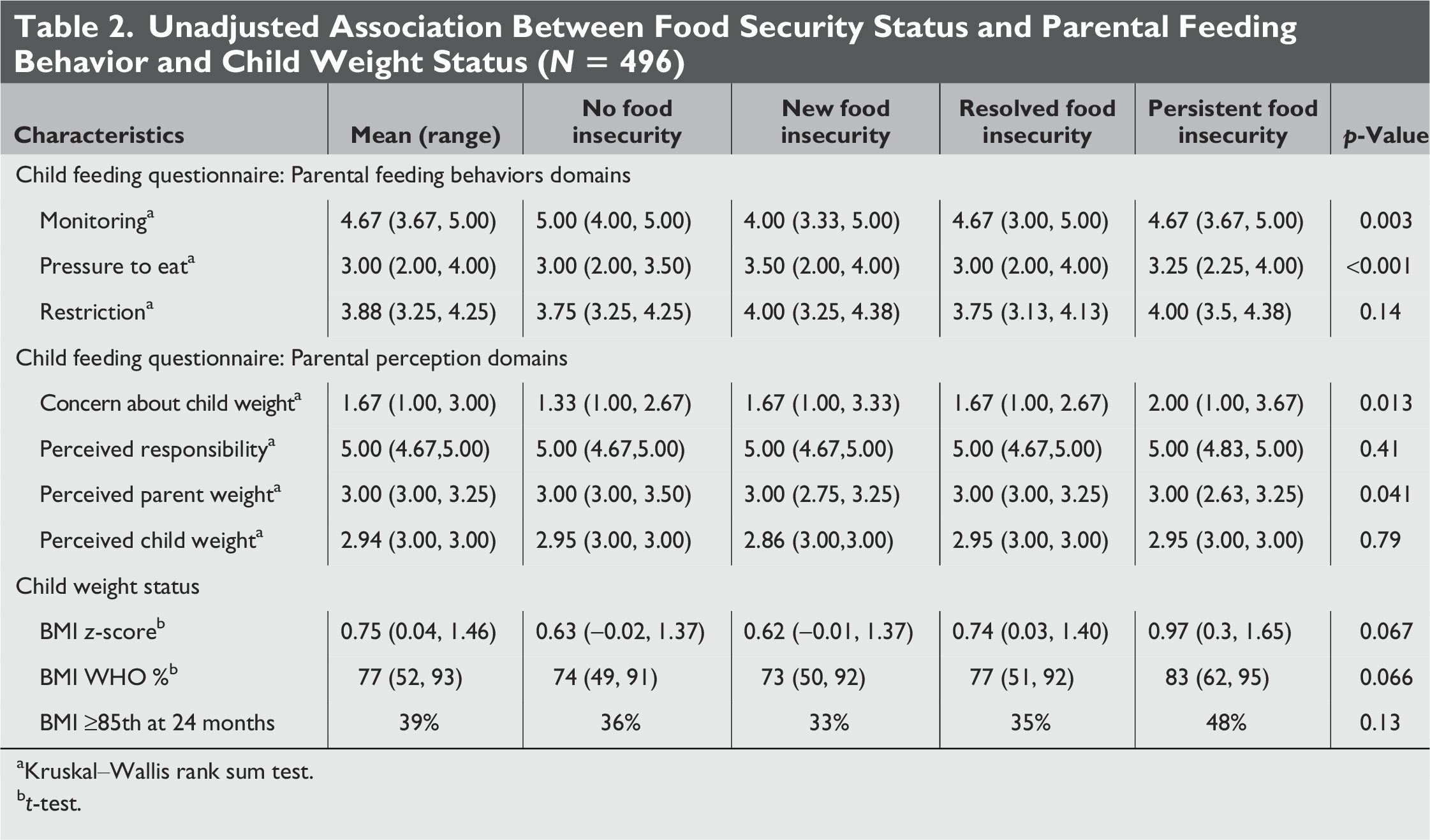
Kruskal–Wallis rank sum test.
t-test.
Linear models adjusted for child sex, caregiver race and ethnicity, participation in the Special Supplemental Nutrition Program for Women, Infants, and Children, site, parental educational attainment, and child health insurance status. Point estimates with 95% confidence interval (CI) and p values for the difference across food security groups. Pairwise comparisons were conducted with the no food insecurity group as the referent.
bResponses derived from the Child Feeding Questionnaire (CFQ). Responses measured on a Likert scale ranging from 1 to 5.
Child Weight Outcomes
The results of adjusted predicted child WHO BMI percentile and z-score are presented in Table 4. A statistically significant difference in WHO BMI percentile was observed for the no FI group and the persistent FI (p = 0.04). A trend toward a higher BMI z-score was seen between the no FI and persistent FI group (p = 0.07).
Adjusted Child Weight Outcomes at 24 Months by Food Security Status a
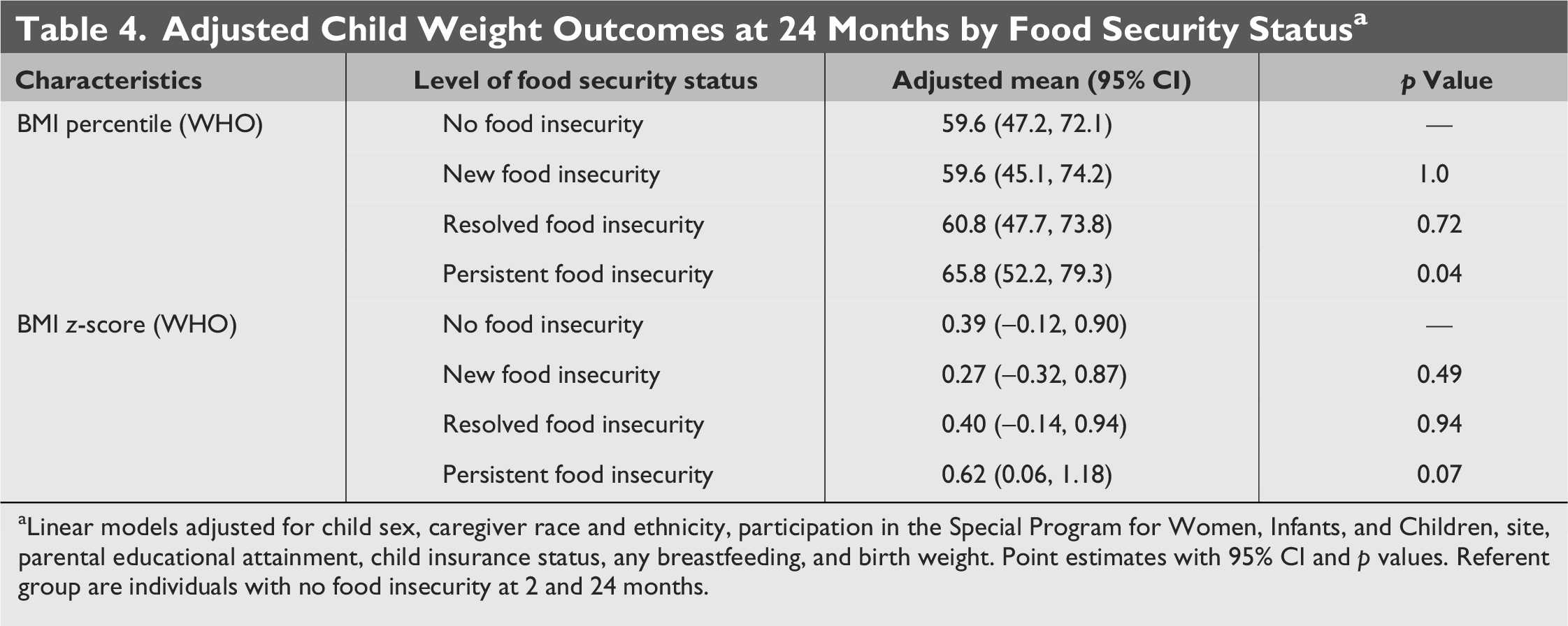
Linear models adjusted for child sex, caregiver race and ethnicity, participation in the Special Program for Women, Infants, and Children, site, parental educational attainment, child insurance status, any breastfeeding, and birth weight. Point estimates with 95% CI and p values. Referent group are individuals with no food insecurity at 2 and 24 months.
Sensitivity Analysis
A sensitivity analysis was conducted to examine the effect of missing data using inverse probability weighting. For the CFQ outcomes, the findings were consistent between the analytical and the weighted group (data not shown). For the weight outcomes, the magnitude and directions of results were similar between the analytical and weighted samples.
Discussion
In our analysis, we found that the timing of FI was associated with differences in PFB. Our study contributes evidence to the growing literature that examines the longitudinal effect of changes in food security status on child nutrition and growth outcomes. The timing of FI on child weight outcomes in our study was mixed with a statistically significant difference between the no FI group compared with the persistent FI group in WHO BMI percentile but not in WHO BMI z-score; however, the difference in BMI-z score between the groups approached statistical significance.
Understanding the effects of change in food security status on child growth and nutrition is an understudied and important area of research. 28 Given the rapid changes in the growth, nutrition, development, and a child’s interaction with their food environment in early childhood, it is important to understand not only the longitudinal effects of FI on child health, but the effects of the timing of FI at different points in early childhood. A previous study reported that FI during pregnancy and infancy was positively associated with pressuring, indulgent, and laissez-faire PFB. 39 Building upon this work, others found that prolonged FI in the same cohort was positively associated with use of food as a reward, restricting food to control weight, and use of food for emotional regulation at later points in infancy and toddlerhood. 40 The study also found that a higher frequency of reported FI was associated with less monitoring of healthy food options. 40 Our study extends this prior work by demonstrating the association between the timing of FI during infancy and toddlerhood with parental feeding behaviors of toddlers.
Consistent with prior work and our hypothesis, our study found statistically significant differences in the monitoring, pressuring, and concern about child weight domains of the CFQ, by timing of food security status. The no FI group had the highest score in the monitoring domain of the CFQ with the second-highest score seen among the persistent FI group. The groups with a changing food security status, i.e., new or resolved FI status, had statistically lower scores compared to the no FI group. Higher parental monitoring and feeding behaviors are of long-term significance because they may be associated with a lower child and adolescent weight status.24,41 In contrast, we did not observe a difference in mean monitoring scores between the no FI and persistent FI groups. This could occur if the groups conceptualize monitoring behaviors differently. For example, monitoring in the no FI group could consist of ensuring nutritional quality and appropriate portion sizes, while in the persistent FI group, monitoring might focus on ensuring that the child is consuming adequate calories regardless of nutritional value when food is available. Future qualitative research could address this observation of no differences in the monitoring domain between the two groups.
Contrary to our hypothesis, we did not find an association between change in FI and parental report of restrictive parental feeding behaviors. Our findings are consistent with prior work that explored the association between FI and restrictive feeding behaviors among WIC-eligible toddlers. 42 This suggests that FI may not operate on restrictive parental feeding behaviors and may influence child weight through other non-responsive parental feeding behaviors. 42
Consistent with cross-sectional work, we found that FI was associated with pressuring feeding behaviors when FI was reported at 24 months. These differences in parental feeding behaviors by timing of FI may represent modifiable factors that contribute to disparities in the risk of pediatric obesity.
Prior work found that child feeding practices can be modified to be more responsive through a targeted intervention; however, this was implemented in a predominantly White, college educated cohort where a majority of the sample reported an annual household income of greater than $50,000–$74,999.43,44 While such interventions are promising, interventions to address PFB among caregivers who experience FI might need to be tailored to address the pathways that contribute to parental feeding behaviors among households that experience FI, such as parental mental health, stress, 19 and access to food. Research is needed to identify best practices to support healthy parental feeding behaviors among families who experience barriers to consistent access to healthy food options.
Based on prior cross-sectional work, 26 we hypothesized that parents with persistent FI would be more concerned about their child becoming overweight, given that FI can be a stressful state 16 for families, leading to high-calorie, unhealthy foods. 3 In our study, we found that persistent FI was associated with higher mean scores for concern about child weight status (child becoming overweight) compared to the no FI group. We did not observe differences between the no FI and new and resolved FI groups. This suggests that timing (single or multiple exposures) may influence parents’ concern about a child becoming overweight. Reducing the number of episodes of FI experienced by a family may influence a family’s concern about a child becoming overweight.
Previous literature is mixed with some studies finding statistically significant associations between food security status and obesity and others finding no association.6,7,9,10,26,45,46 This may reflect the complex mechanisms between food security status and child weight status, which can vary by a child’s sex and number of exposures to FI.4,45,47 We were able to identify a statistically significant difference in WHO BMI percentile, but not WHO BMI z-score, between the no FI and persistent FI groups. While the two measures of child weight status are highly correlated, differences can exist at the extremes of weight. The point estimates of the WHO BMI z-score suggest that children who experience persistent FI may have a higher weight status compared to children who do not experience FI. Prospective studies are needed to clarify the relationship between timing of FI and child weight status.
Our study has several limitations. Missing data could potentially bias this analysis; to address this limitation, inverse probability weighting was conducted with similar findings between the analytical sample and the imputed sample. Measures of parental feeding behaviors were collected via self-report, which is subject to the potential for social desirability. The measure of FI had a 12-month lookback window, which can introduce recall bias and potentially not capture all participants who experienced FI or desire for connection to resources.48,49 Additionally, the use of the 2-item FI screen is not sufficiently granular to identify various levels of severity of FI. There is also the potential for unmeasured confounders.
Conclusions
Persistent FI and changes in FI status during the first 24 months of life were associated with differences in PFB that may contribute to obesity. Our study also suggests that compared to children who are never food insecure, children who experience persistent FI may have a higher BMI status. Addressing food security and strengthening parental feeding practices may improve the weight status of toddlers whose households experience FI.
Authors’ Contributions
C.J.O. and K.B.F. contributed to the study design, analytical plan, data interpretation, and writing of the article. Y.Y. and F.-C.L. contributed to the analytical plan, conducted the analysis, and critically revised and edited the article. E.M.P., W.J.H., R.L.R., L.M.S., S.Y., C.T.W., and A.M.D. contributed the study design, data collection, and grant funding of the original study. The authors contributed to the analysis of the current study and provided critical feedback and revisions. All the authors agree to the submission of the article.
Footnotes
Author Disclosure Statement
No competing financial interests exist.
Funding Information
Supported by National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) (K23 5K23DK132513 PI [C.J.O]). Supported by the Eunice Kennedy Shriver Institute for Child Health and Development, National Institute of Child Health and Human Development (grant R01 HD049794), with supplemental funding from Centers for Disease Control and Prevention and Office of Behavioral and Social Sciences Research (grant R01HD059794-04S1, R01HD059794-04S2). Parts of the study were supported the National Institutes of Health’s National Center for Advancing Translational Sciences through its Clinical and Translational Science Awards Program (grants 1UL1RR029893, UL1TR000445, and UL1RR025747). During the time the study was conducted, Dr Yin was supported by a grant under the Robert Wood Johnson Foundation Physician Faculty Scholars Program and Health Resources and Services Administration (12-191-1077-Academic Administrative Units in Primary Care) and by funding from the KiDS of NYU Langone Foundation.
Impact Statement
Our study contributes to the field by examining how the timing and persistence of food insecurity is associated with parental feeding behaviors and obesity.
Supplemental Material
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.