Abstract
This case presents a discussion of a frail 98-year-old woman in hospice care, with a history of dementia, previous hip fracture, and anemia, who is admitted with a left intertrochanteric fracture. Care is coordinated and expedited by an interdisciplinary team to optimize her outcome, in the context of her goals of care.
Initial Presentation
The patient is a 98-year-old woman with past medical history of dementia and a previous right hip fracture who lives in a nursing home. She sustains her third fall in 3 weeks while ambulating to the bathroom. She is unable to stand or bear weight and complains of left hip pain. There are no other injuries noted. Her history is notable for progressive fatigue over the past month, but she still ambulates without assist around the room and uses a wheelchair to get around the facility. Due to dementia, most of the history is obtained from the patient's daughter.
Comments on Initial Presentation
Susan Bukata, MD (Orthopaedic Surgery, Metabolic Bone Disease)—In the geriatric population almost all fractures of the hip occur with a fall. The low-energy trauma of the fall from standing height or less combined with weakened bone from osteoporosis results in the fracture. Falls are extremely common in the nursing home setting, especially in patients with dementia. These patients commonly need assistive devices for walking but often forget or refuse to use them. Patients with prior hip fractures have an increased risk of future fragility fracture, including an almost 9% chance of fracturing the second hip within 2 years, 1 emphasizing the importance of osteoporosis and fall prevention care, particularly after a hip fracture has already occurred. Major risk factors for fragility fracture in this patient include advancing age, history of prior fracture, dementia, and history of falls.
Joe Nicholas, MD (Geriatrics, Palliative Care)—Increasing falls in geriatric patients are of high clinical significance, both in terms of immediate morbidity and a marker for underlying pathology and prognosis. 2 In this patient with dementia, significant baseline dependency, and greatly diminished physiologic reserve, an increasing pattern of falls may be the result of relatively minor changes in her strength, environment, or cognition or may represent a more easily identifiable medical etiology. Common medical issues that may relate to progressive fatigue and falls include anemia, polypharmacy, renal failure, dehydration, or volume overload. She needs a complete history and medical evaluation to identify any correctable medical issues that relate to her fitness for surgery and her anticipated recovery as well as attempts to intervene to reduce her future likelihood of falls.
Nathan Clark, MD (Anesthesiology)—Anesthesiologists are beginning to view themselves as perioperative physicians. We are studying how our preoperative, intraoperative, and postoperative actions interface with one another in order to maximize patient outcomes. For geriatric patients with fracture, morbidity and mortality are minimized when definitive surgical care occurs within 24 to 36 hours of the injury. 3 Thus, as a perioperative physician my goal is to eliminate or minimize any unnecessary obstacles in this patient’s path to the operating room, thus maximizing her chance for a successful recovery. One of the major obstacles is preoperative testing. We limit testing and workup to focus on information that can be obtained quickly and easily, and will be likely to alter the course of patient care.
History
The patient’s past medical history is significant for colon cancer, for which she underwent resection 20 years prior to admission. Three years prior to admission, while still a resident in an assisted living facility, she sustained a right intertrochanteric fracture and C2 fracture in the setting of possible alcohol use. She underwent a dynamic helical hip screw, with a course that was uncomplicated except for transfusion of 3 units of packed red blood cells (PRBCs) for acute blood loss anemia. She has chronic obstructive pulmonary disease (COPD) for which she occasionally uses supplemental oxygen. She has anemia, hyperlipidemia, coronary artery disease, hypertension, depression, and macular degeneration.
Medications on admission are citalopram, metoprolol, bupropion, omeprazole, and sorbitol. She takes lorazepam as needed for anxiety and restlessness, oral morphine as needed for pain, and albuterol as needed for shortness of breath.
She is a nursing home resident. She ambulates with a walker with supervision at baseline, and occasionally uses a wheelchair. She is a retired dental hygienist. She has a history of heavy alcohol use and previous tobacco use, but has quit. Her daughter is her health care agent. She is on hospice care and has an advance directive that says do not resuscitate (DNR)/do not intubate (DNI)/no feeding tube and do not send to the hospital unless pain or severe symptoms cannot be controlled.
Review of systems is negative except for fatigue as above.
Comments on History
Susan Bukata, MD (Orthopaedic Surgery, Metabolic Bone Disease)—Her history demonstrates additional risk factors for osteoporosis including a history of smoking, alcohol use, prior fracture, yet her medication list does not include calcium, vitamin D, or any osteoporosis medication. Alcoholics are at a particular risk of low vitamin D levels, which in itself affects bone strength and fracture risk. 4 It is not uncommon for chronic alcoholics to have both osteomalacia and osteoporosis. It is also common for patients in skilled nursing facilities to have issues with low vitamin D levels. Even if she is no longer drinking, these issues have certainly contributed to her fracture risk. Her complex medical history certainly obligates a good medical evaluation prior to surgery and stabilization of her acute medical issues. It is important to remember that many of her medical issues are chronic and will not be improved. These should not delay the surgery. It is extremely important in patients like this who are medically fragile to undergo acute optimization of their medical issues and then get to the operating room as quickly as possible to prevent additional medical decline due to bed rest and pain associated with the fracture. Ideally, these patients should proceed to surgery within 24 hours of admission to the hospital. Her history of needing significant blood transfusion of 3 units after her prior hip fracture surgery should signal to the care team that similar bleeding issues may complicate her current surgery. The team needs to be prepared to have blood available for the operating room and to give it during surgery if needed.
Joe Nicholas, MD (Geriatrics, Palliative Care)—She certainly has a number of common clinical conditions that are likely to impact her prognosis and care. Her history of alcohol abuse places her at high risk of underlying cirrhosis, cardiomyopathy, autonomic neuropathy, and dementia, all of which may complicate her perioperative course, primarily through risks of hypotension, volume overload, and delirium. If she is drinking regularly in her nursing home, she is at significant risk of alcohol withdrawal. She appears to have advanced chronic lung disease and is at risk of hypoxemia and hypercarbia following anesthesia and analgesia. A careful medication history is essential. Opiates, benzodiazepines, and antidepressants should not be stopped or tapered abruptly as this may precipitate withdrawal; if she is taking opiates regularly, she may need higher doses of as-needed opiates to achieve satisfactory pain control. Similarly, metoprolol should be continued in this setting. Omeprazole can place the patient at risk of pneumonia, 5 Clostridium difficile colitis, 6 and osteoporosis 7 ; if there is no recent history of active peptic ulcer disease or symptoms of severe reflux, this can likely be discontinued. Hospice care is not a contraindication to fracture repair; it is often a necessary palliative intervention to help keep patients with fracture comfortable, prevent pressure ulcers, and deliver personal care.
Nathan Clark, MD (Anesthesiology)—Delays in surgical care significantly increase risks of geriatric fracture morbidity and mortality. Therefore, generally speaking, unless there is an acute exacerbation of a chronic condition, further workup of most chronic conditions can be avoided preoperatively. Extensive workup of a chronic medical condition should only delay surgery if the results of that workup are expected to significantly alter either surgical or anesthetic management. This elderly patient has multiple serious medical comorbidities, but they all appear to be stable. A detailed history and physical examination with corroboration by the patient's caregivers and family is a must and will further clarify her medical issues. First, the extent of her lorazepam, morphine, and alcohol use must be determined. Abrupt discontinuation of any of these agents may precipitate withdrawal. Second, she has known coronary artery disease. As long as they are appropriately titrated, β-blockers are cardioprotective perioperatively. Her metoprolol should be adjusted toward a target heart rate of 60 to 70 bpm. 8 Further cardiac workup is not necessary because it will delay her surgery and is unlikely to significantly alter her anesthetic management. There are 4 cardiac conditions that require a delay in surgery and cardiology consult per the American College of Cardiology/American Heart Association guidelines. 9 They are acute coronary syndrome, severe valvular abnormalities, uncompensated congestive heart failure, and severe arrhythmias. Third, her age and COPD place her at high risk of perioperative hypoxia and hypercarbia. A detailed discussion with her caregivers is a must to find out her baseline oxygenation. In the absence of clinical findings of acute pulmonary compromise—that is, worsening wheezing, infection, and so forth—further pulmonary workup is not necessary. Finally, she is a hospice/DNR/DNI patient. A discussion with her health care agent is needed to determine the extent of perioperative resuscitation allowed. Typically, DNR/DNI orders are suspended for the immediate perioperative period, but this is always adjusted per the patient’s wishes. 10
Initial Examination
On initial examination, she is a thin, frail older woman in no acute distress. Weight is 91.2 lbs (41.4 kg), and height is 63 in (1.6 m). Body mass index (BMI) is 16.2 kg/m2. Blood pressure is 133/71, heart rate 81, respiratory rate 14, temperature 36.1°C, and oxygen saturation of 90% in room air. Her chest is clear to auscultation bilaterally. Heart sounds are regular rate and rhythm. Lung examination shows poor air movement. Abdomen is benign. She has tenderness to palpation over her left thigh. Her skin is intact anterior and laterally. She is able to move her ankle dorsiflexors, plantar flexors, and extensor hallucis longis. Sensation is intact to light touch over the medial, lateral, dorsal, plantar, and first dorsal webspaces. She has a palpable 2+ dorsalis pedis (DP) pulse, and she has pain with any attempted hip motion. Several skin tears are noted on both upper extremities.
Comments on Initial Examination
Susan Bukata, MD (Orthopaedic Surgery, Metabolic Bone Disease)—Her examination shows her to be frail. Great care must be taken to protect the integrity of her skin, providing another reason to take her to the operating room as soon as possible. The examination is highly suspicious for hip fracture and consistent with her history; however, radiographs must confirm the diagnosis because occasionally similar symptoms are seen with pelvic fracture, although the thigh pain would be unusual with a pelvic fracture. It is tempting during the examination to move the hip extensively, as would be done in a normal test of range of motion for that joint. This is extremely painful for the patient and can trap muscle in the fracture site, complicating surgery and fracture reduction. A simple observation of limb shortening, limb external rotation, and pain with minimal rotational motion of an extended leg is sufficient to suspect hip fracture. A gentle tap to the heel of the extended leg (known as heel percussion) that elicits pain is also highly suggestive of fracture.
Joe Nicholas, MD (Geriatrics, Palliative Care)—Her general appearance and BMI suggest frailty and malnutrition and certainly predict diminished physiologic and functional reserve. Despite a normal blood pressure, she is still extremely likely to become hypotensive with anesthesia, blood loss, or pain medications. Her oxygen saturation is likely to drop with pain medications, anesthesia, or atelectasis, and supplemental oxygen is reasonable. She does not have any historical features or examination findings that are a contraindication to early surgery, and no further perioperative testing beyond basic labs and electrocardiogram (ECG) are likely to impact her outcome.
Nathan Clark, MD (Anesthesiology)—The initial examination does not suggest any acute exacerbations of her known chronic conditions. Her oxygen saturation is expected, to give her known COPD and age. Supplemental oxygen is indicated, as she will receive opioids, undergo anesthesia, and be on bed rest, which all cause respiratory compromise. There is no sign of acute coronary syndrome. However, she has a normal blood pressure and heart rate, 2 things that we would not expect in someone her age, with known hypertension, painful acute hip fracture, and severe anemia. Resuscitation with PRBCs and intravenous (IV) fluids are indicated to stabilize intraoperative hemodynamics. The best treatment for this patient is early surgery after she is resuscitated. Further workup is very unlikely to change anesthetic management.
Initial Evaluation
Initial evaluation includes plain radiographs of the left lower extremity, which show an intertrochanteric hip fracture with fracture through the base of the lesser trochanter. See attached film (Figure 1).

Preoperative proximal femur x-ray.
Original ECG shows a wandering atrial pacemaker with 2 premature ventricular contractions and a rate of 97 as well as probable left ventricular hypertrophy with repolarization abnormalities.
Chest radiograph is a poor quality film that shows prominent interstitial markings bilaterally (see Figure 2).
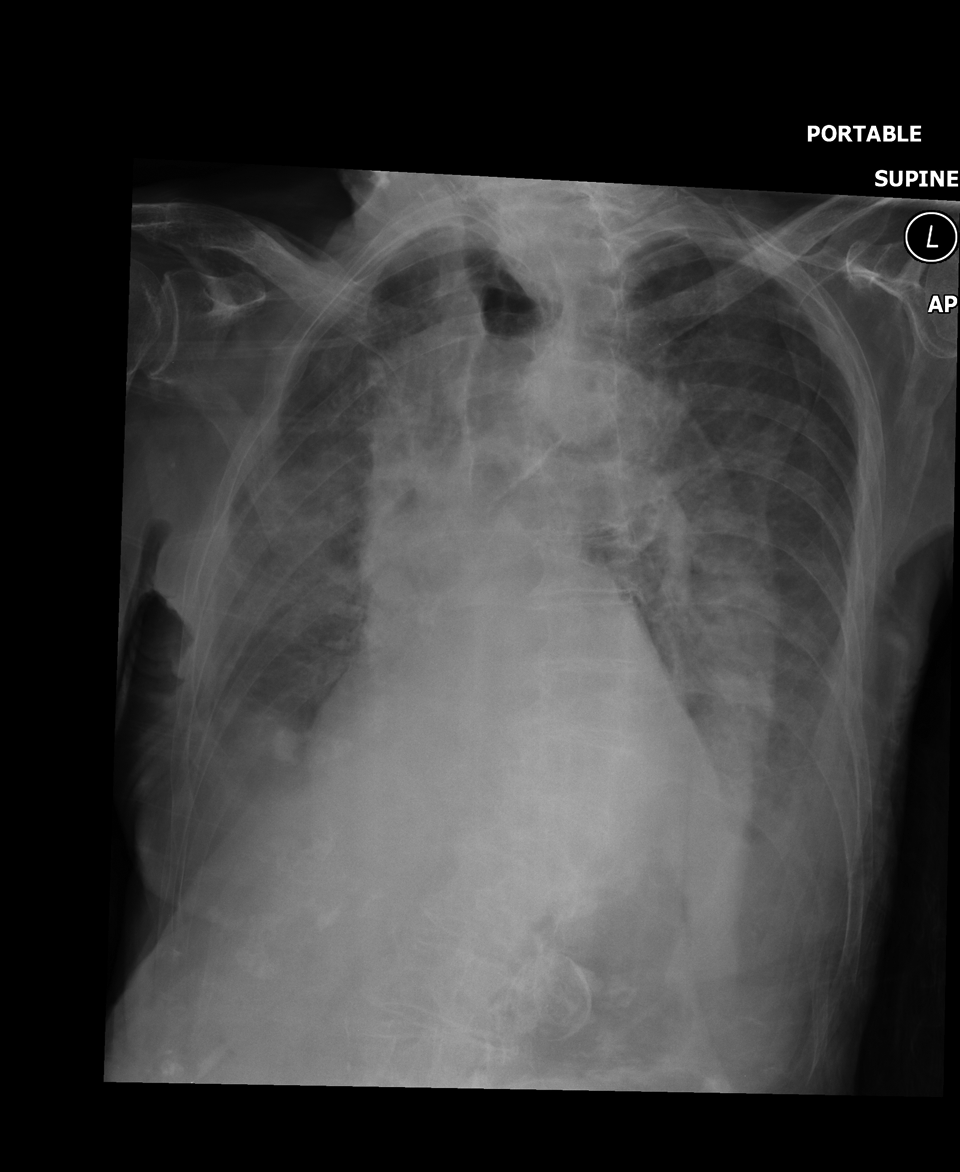
Preoperative chest x-ray.
Pertinent labs include a white blood cell (WBC) count of 11 600, hematocrit of 18% with a mean corpuscular volume of 66 (baseline 4 months prior is 28 and 89, respectively), and platelets of 280 000. Blood urea nitrogen and creatinine (Cr) are 24 and 0.85, respectively. Sodium is 138, potassium is 3.4, chloride 100, and bicarbonate 28, albumin is 3.0, and calcium 8.1. Initial international normalized ratio is 1.2. Urinalysis shows a specific gravity of 1.025, 6 to 10 WBC, 3 + bacteria and is negative for leukocyte esterase and nitrites.
Comments on Initial Evaluation
Susan Bukata, MD (Orthopaedic Surgery, Metabolic Bone Disease)—The patient has a classic low-energy fragility fracture of the hip that has an excellent chance of healing with fixation. This intertrochanteric fracture can be fixed with either a sliding hip screw or a intramedullary nail. Her anemia is very concerning as she will certainly have blood loss during the surgery, which can easily be a few hundred cubic centimeters regardless of the type of fixation used. Dealing with preoperative anemia and intraoperative blood loss will be very important for this patient.
Joe Nicholas, MD (Geriatrics, Palliative Care)—Most striking is her profound microcytic anemia that likely represents severe iron deficiency from slow ongoing blood loss and poor nutritional intake. She will require preoperative red blood cell (RBC) transfusion of at least 2 to 3 units. Since this anemia appears to have developed slowly, and she has expanded her intravascular volume as compensation, she is at risk of acute pulmonary edema with RBC transfusion and needs to be monitored for increasing dyspnea. In general, her surgery is likely to be better tolerated with high intravascular volume, and I would reserve diuresis for symptomatic dyspnea. Interstitial markings on chest x-ray are nonspecific, and the consequences of overdiuresis are more problematic than mild pulmonary edema in the perioperative setting. As is common in many frail older women, she has bacteriuria without symptoms of clinical infection; she is unlikely to benefit from empiric antibiotics at this time. 11 Her ECG findings also suggest a cardiomyopathy, but cardiology consultation or echocardiography are unlikely to change our management and often result in a harmful delay to surgery. 12
Nathan Clark, MD (Anesthesiology)—From a preoperative standpoint, several things can be done immediately to prepare this patient for the operating room. First, blood transfusions are required. I agree that she will need to be transfused 2 or 3 units PRBCs preoperatively in order to raise her hematocrit to the 30% range—the exact target HCT is a matter of personal preference. It should be noted that since she has ongoing blood loss from her fracture, she is by definition an unstable patient, and the typical transfusion “targets & triggers” are not necessarily appropriate. Second, no diuresis is indicated. Yes, her renal function is significantly impaired, with an estimated Cr clearance of approximately 24. Although the transfusions will place her at risk of acute pulmonary edema, her intraoperative hemodynamic course is likely to be much more stable if she is relatively volume overloaded versus intravascularly volume depleted. Therefore, I would not diurese her preoperatively unless she displayed significant acute pulmonary edema from her transfusions. Also, her medications will need to be adjusted to accommodate her renal function. Third, I would avoid a cardiology consult at this time. Although abnormal, her ECG by itself does not warrant the surgical delay that a cardiology consult would cause.
Preoperative Course
The patient is evaluated by Geriatrics and determined to be at intermediate-to-high risk of surgery, which is addressed with her family. The family thinks that the benefits of improved pain control and possibility for increased mobility and not requiring high-dose opioids for pain control are consistent with the patient’s values. Surgery is planned for palliation of fracture-induced pain.
She receives 2 units of PRBCs in preparation for the surgery. Geriatrics recommends albuterol nebulizers and notes that she is at high risk of pneumonia. They also note poor nutritional status and recommend a nutrition consult.
Comments
Susan Bukata, MD (Orthopaedic Surgery, Metabolic Bone Disease)—Her significant anemia needs to be addressed prior to proceeding to the operating room. Blood loss during fixation of intertrochanteric fractures can be significant and her anemia and frailty require the surgeon to be honest with medicine and anesthesia colleagues about their anticipated blood loss during the case. Fixation can be done with a sliding hip screw and side plate or a trochanteric nail. Patients of this age and medical frailty often have significant comminution of their fractures. If the lateral wall is compromised at the level of the hip screw or if a reverse obliquity pattern is present in the fracture, a trochanteric nail must be used. If these issues are not present either fixation device will be effective, but the dynamic hip screw costs significantly less that the intertrochanteric nail.
Joe Nicholas, MD (Geriatrics, Palliative Care)—This appears to be a well-reasoned and appropriate assessment and plan. She is at high risk of surgery for a number of reasons, but without surgery it will be near impossible to keep her comfortable. With close medical and surgical attention to intravascular volume status and pain control, her perioperative risk of mortality is still likely under 10%. Other than preoperative transfusion and pulmonary toilet, there are no further tests, consultations, or interventions that are likely to improve her outcome, and she will be optimized for surgery following blood transfusion.
Nathan Clark, MD (Anesthesiology)—I agree with the recommendation of the geriatrician. Ideally, surgery can be performed under regional anesthesia, either with spinal or epidural anesthesia. This would maximize her intraoperative and postoperative analgesia, minimize her pulmonary compromise, and minimize her perioperative delirium risk. However, it is important to keep in mind that she still may require some postoperative benzodiazepines and opioids to minimize withdrawal risk, depending upon her baseline usage.
Surgery
The patient is brought to surgery 23 hours after admission, where a dynamic helical hip screw is placed under general anesthesia. There are no complications, and estimated blood loss is less than 50 mL. After a short time in the postanesthesia care unit, the patient is transferred to the orthopedics floor for further monitoring.
Comments
Susan Bukata, MD (Orthopaedic Surgery, Metabolic Bone Disease)—Postoperative orders must allow for early mobilization and weight bearing as tolerated. Elderly patients cannot maintain a limited weight-bearing status. Early mobilization is essential to prevent skin pressure ulcers. Patients with hip fracture often take a step down in mobility status, and frail nursing home patients who do not mobilize soon after surgery may not regain their ambulatory status.
Joe Nicholas, MD (Geriatrics, Palliative Care)—Early surgery has been shown to be superior for a number of important outcomes, including mortality, pressure ulcers, delirium, and pain control. 13 The medical team will need to continue to assess her postoperative volume status, pain control, and medications and watch for signs of alcohol withdrawal (agitation, delirium, and tachycardia).
Nathan Clark, MD (Anesthesiology)—General anesthesia is an acceptable alternative to regional anesthesia. Her pulmonary status will need to be closely monitored, and an aggressive pulmonary toilet is indicated. A peripheral nerve block, such as a femoral 3 in 1 nerve block or lumbar plexus block can be placed to optimize analgesia while minimizing opioid-induced respiratory depression. She may still require additional IV fluids and blood products depending upon her postoperative vital signs and laboratory tests. Diuresis is rarely indicated in the acute postoperative period. It is important to note that one of the reasons this patient did so well intraoperatively was that she was adequately volume resuscitated and transfused preoperatively.
Postoperative Course
The hospice team remains involved throughout her hospital course, making daily visits. The patient is noted to have low urine output on postoperative day 1, which responds to fluid boluses. Her hematocrit is stable at 31. Her pain is well controlled on oral pain medications. Physical therapy, occupational therapy, and social work are all consulted in preparation for discharge. She is recommended to receive daily physical therapy at the nursing home.
On postoperative day 2, the dressing on her left hip is changed. The incision is clean, dry, and intact. She is able to dorsiflex and plantar flex her ankle and flex and extend her toes. Sensation is intact to light touch over her entire foot, and she has a 2+ DP pulse. Pain is well controlled on oral pain medications. The COPD is controlled with albuterol as needed. Urine output is 530 cm3 in 24 hours. Hematocrit is 29, and she is given another unit of blood due to poor urine output. Postoperative films are seen in Figure 3.
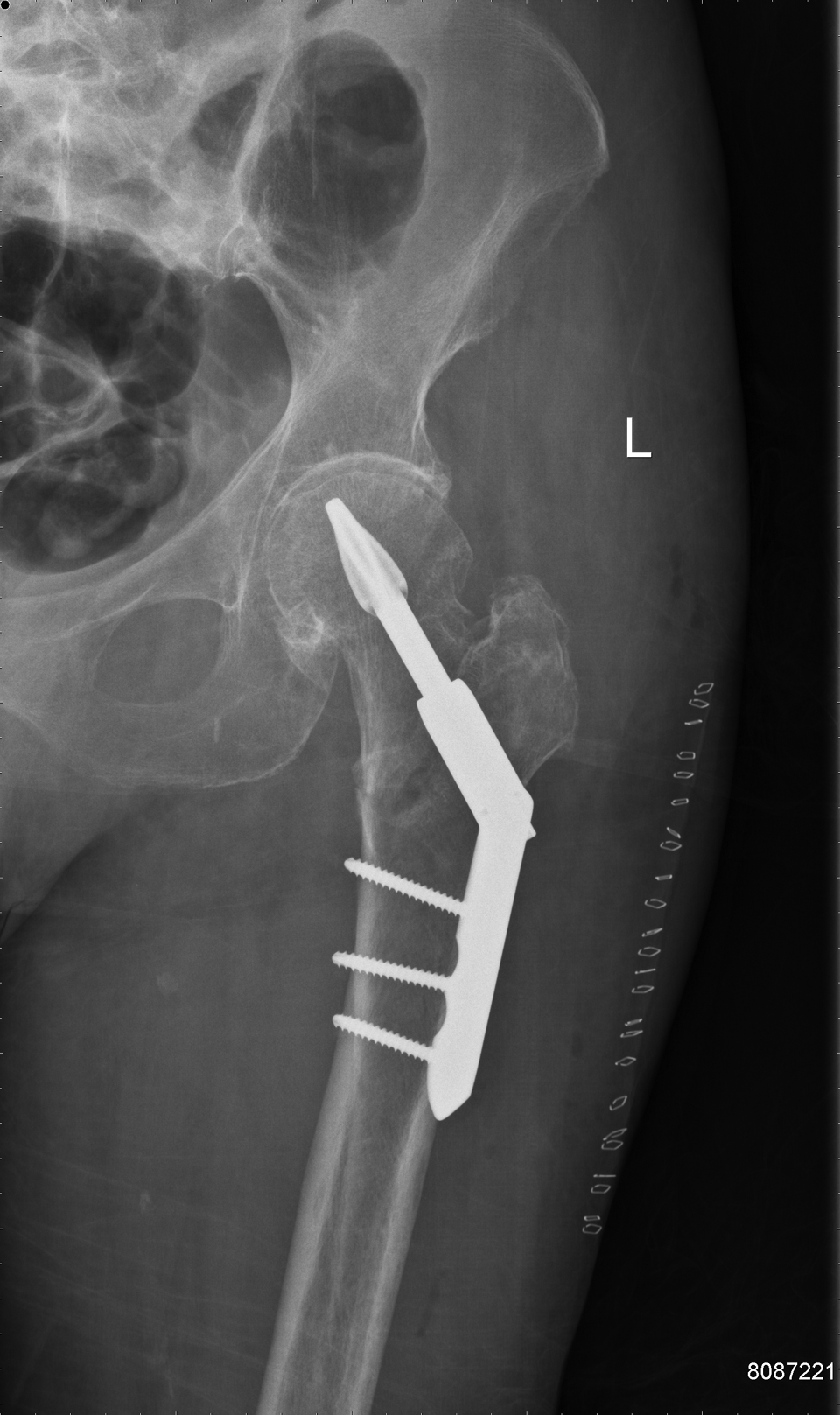
Postoperative proximal femur x-ray.
On postoperative day 3, her hematocrit is 33. Her urine output improves. She is eating. Her mental status is felt to be at baseline. She is discharged back to the nursing home.
Comments
Susan Bukata, MD (Orthopaedic Surgery, Metabolic Bone Disease) —She has done well postoperatively. Her urinary catheter would normally be removed on postoperative day #1, but her low urine output warrants continued use of the catheter to assist with patient monitoring. Discuss this issue with her medical team and do not automatically follow protocol orders if a particular care issue arises such as low urine output. Consider with the medical team discharge plans for both her osteoporosis and her orthopedic care. Make sure that calcium and vitamin D are a part of the discharge orders unless there is a significant contraindication for them, such as hypercalcemia or severe kidney disease that requires dialysis. This patient is at high risk of recurrent fracture, but her prognosis of less than 6 months (based on qualifying for hospice) may preclude more aggressive approaches to secondary prevention.
Joe Nicholas, MD (Geriatrics, Palliative Care)—Despite the identification of multiple preoperative risk factors and comorbidities, she has had an uncomplicated perioperative and postoperative course. This is a typical experience at many geriatric fracture centers. Attention to pain control, volume status, and constipation prevention are essential for a stable postoperative course. Early postoperative oliguria often represents intravascular volume depletion; ongoing oliguria may represent renal failure, urinary retention, or diuretic dependence. Considering the patient’s prognosis and wishes, workup and treatment for underlying osteoporosis can be considered; for patients on hospice, treatment of vitamin D and calcium deficiencies is appropriate to help in bone healing and musculoskeletal symptoms. Iron replacement is reasonable, but no further workup for the source of her iron deficiency is warranted. Careful medication reconciliation on discharge is essential to avoid the resumption of medications that are not indicated in this setting.
Nathan Clark, MD (Anesthesiology)—This patient has done very well despite her multiple serious comorbidities. Early surgery minimized further decreases to her already diminished physiologic reserve. Aggressive preoperative hydration and transfusions allowed for a very stable intraoperative course. However, she still required additional intravascular fluid volume postoperatively. This is a frequent occurrence in this patient population, and close attention to volume status is critical to preventing acute renal injury due to intravascular volume depletion and resultant hypoperfusion.
Teaching points
An increasing pattern of falls may represent a nonspecific finding of one or more acute or subacute issues, including anemia, polypharmacy, renal failure, dehydration, or volume overload. Hospice is not a contraindication to hip fracture repair and may be indicated for pain control and care management as well as prevention of other morbid events that may reduce the quality of life. In patients with a significant alcohol history, it is necessary to consider both acute (eg, cause of fall and withdrawal) and chronic (eg, cirrhosis, cardiomyopathy, autonomic neuropathy, dementia, and vitamin D deficiency) consequences in the management of patients with fracture. In patients who present with severe anemia, the chronicity should be considered in its evaluation and management. Patients should be transfused for volume repletion prior to surgery. Patients who present with fragility hip fractures are at high risk of recurrent fracture, and efforts to reduce risk through osteoporosis management and falls reduction should be addressed. These need to be tempered by considerations of life expectancy.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
